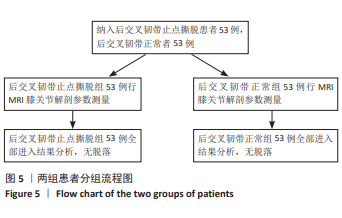
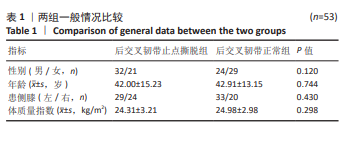
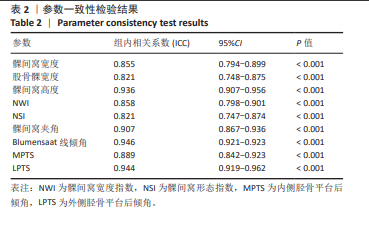
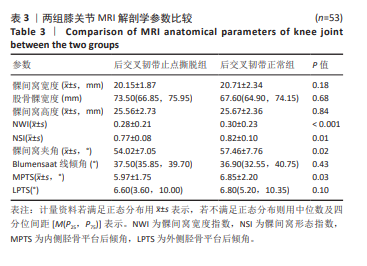
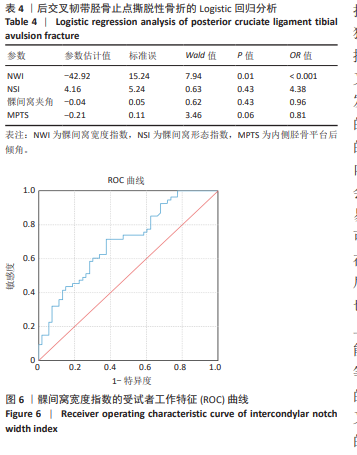
[1] XIN W, GAO Y, ZHENG L, et al. Posterior cruciate ligament tibial attachment sacrifice percentage is higher in cruciate-retaining total knee arthroplasty in patients with discoid lateral meniscus. Arthroplasty. 2024;6(1):19.
[2] AKPINAR B, DECLOUETTE B, GONZALEZ-LOMAS G, et al. Posterior Cruciate Ligament Reconstruction Current Concepts Review. Bull Hosp Jt Dis (2013). 2024;82(1):4-9.
[3] ZSIDAI B, HORVATH A, WINKLER PW, et al. Different injury patterns exist among patients undergoing operative treatment of isolated PCL, combined PCL/ACL, and isolated ACL injuries: a study from the Swedish National Knee Ligament Registry. Knee Surg Sports Traumatol Arthrosc. 2022;30(10):3451-3460.
[4] ZHOU Z, WANG S, XIAO J, et al. The degree of fracture reduction does not compromise the clinical efficacy of arthroscopic reduction and fixation of tibial posterior cruciate ligament avulsion fractures: A retrospective study. Medicine (Baltimore). 2023;102(39):e35356.
[5] VAN KUIJK KSR, REIJMAN M, BIERMA-ZEINSTRA SMA, et al. Posterior cruciate ligament injury is influenced by intercondylar shape and size of tibial eminence. Bone Joint J. 2019;101-B(9):1058-1062.
[6] NEDAIE S, VIVEKANANTHA P, O’HARA K, et al. Decreased posterior tibial slope is a risk factor for primary posterior cruciate ligament rupture and posterior cruciate ligament reconstruction failure: A systematic review. Knee Surg Sports Traumatol Arthrosc. 2024;32(1):167-180.
[7] OWESEN C, SANDVEN-THRANE S, LIND M, et al. Epidemiolgy of surgically treated posterior cruciate ligament injuries in Scandinavia. Knee Surg Sports Traumatol Arthrosc. 2017;25(8):2384-2391.
[8] SONIN AH, FITZGERALD SW, HOFF FL, et al. MR imaging of the posterior cruciate ligament: normal, abnormal, and associated injury patterns. Radiographics. 1995;15(3):551-561.
[9] LIU F, ZHANG S, XIAO Y, et al. Stenotic intercondylar notch is not a risk factor for posterior cruciate ligament rupture: a morphological analyses using magnetic resonance imaging. Knee Surg Sports Traumatol Arthrosc. 2022;30(5):1711-1717.
[10] HODEL S, KABELITZ M, TONDELLI T, et al. Introducing the Lateral Femoral Condyle Index as a Risk Factor for Anterior Cruciate Ligament Injury. Am J Sports Med. 2019;47(10):2420-2426.
[11] KIZILGÖZ V, SIVRIOĞLU AK, AYDIN H, et al. The Combined Effect of Body Mass Index and Tibial Slope Angles on Anterior Cruciate Ligament Injury Risk in Male Knees: A Case-Control Study. Clin Med Insights Arthritis Musculoskelet Disord. 2019;12:1179544119867922.
[12] BERNHARDSON AS, DEPHILLIPO NN, AMAN ZS, et al. Decreased Posterior Tibial Slope Does Not Affect Postoperative Posterior Knee Laxity After Double-Bundle Posterior Cruciate Ligament Reconstruction. Am J Sports Med. 2019;47(2):318-323.
[13] LAPRADE CM, CIVITARESE DM, RASMUSSEN MT, et al. Emerging Updates on the Posterior Cruciate Ligament: A Review of the Current Literature. Am J Sports Med. 2015;43(12):3077-3092.
[14] GWINNER C, WEILER A, ROIDER M, et al. Tibial Slope Strongly Influences Knee Stability After Posterior Cruciate Ligament Reconstruction: A Prospective 5- to 15-Year Follow-up. Am J Sports Med. 2017;45(2):355-361.
[15] OWESEN C, SANDVEN-THRANE S, LIND M, et al. Epidemiology of surgically treated posterior cruciate ligament injuries in Scandinavia. Knee Surg Sports Traumatol Arthrosc. 2017;25(8):2384-2391.
[16] BAYER S, MEREDITH SJ, WILSON KW, et al. Knee Morphological Risk Factors for Anterior Cruciate Ligament Injury: A Systematic Review [published correction appears in J Bone Joint Surg Am. 2020;102(14):e85. doi: 10.2106/JBJS.ER.19.00535]. J Bone Joint Surg Am. 2020;102(8):703-718.
[17] JHA V, PANDIT A. Notch Volume Measured on Magnetic Resonance Imaging Is Better Than 2-Dimensional Notch Parameters for Predicting Noncontact Anterior Cruciate Ligament Injury in Males. Arthroscopy. 2021;37(5): 1534-1543.e1.
[18] SHEN X, XIAO J, YANG Y, et al. Multivariable analysis of anatomic risk factors for anterior cruciate ligament injury in active individuals. Arch Orthop Trauma Surg. 2019;139(9):1277-1285.
[19] HUDEK R, SCHMUTZ S, REGENFELDER F, et al. Novel measurement technique of the tibial slope on conventional MRI. Clin Orthop Relat Res. 2009;467(8):2066-2072.
[20] HUANG WT, KANG K, WANG J, et al. Morphological Risk Factors for Posterior Cruciate Ligament Tear and Tibial Avulsion Injuries of the Tibial Plateau and Femoral Condyle. Am J Sports Med. 2023;51(1):129-140.
[21] FAN N, ZHENG YC, ZANG L, et al. What is the impact of knee morphology on posterior cruciate ligament avulsion fracture in men and women: a case control study. BMC Musculoskelet Disord. 2021;22(1):100.
[22] SOURYAL TO, FREEMAN TR. Intercondylar notch size and anterior cruciate ligament injuries in athletes. A prospective study. Am J Sports Med. 1993; 21(4):535-539.
[23] DOMZALSKI M, GRZELAK P, GABOS P. Risk factors for Anterior Cruciate Ligament injury in skeletally immature patients: analysis of intercondylar notch width using Magnetic Resonance Imaging. Int Orthop. 2010;34(5): 703-707.
[24] BOURAS T, FENNEMA P, BURKE S, et al. Stenotic intercondylar notch type is correlated with anterior cruciate ligament injury in female patients using magnetic resonance imaging. Knee Surg Sports Traumatol Arthrosc. 2018;26(4):1252-1257.
[25] EVERHART JS, FLANIGAN DC, SIMON RA, et al. Association of noncontact anterior cruciate ligament injury with presence and thickness of a bony ridge on the anteromedial aspect of the femoral intercondylar notch. Am J Sports Med. 2010;38(8):1667-1673.
[26] FUNG DT, HENDRIX RW, KOH JL, et al. ACL impingement prediction based on MRI scans of individual knees. Clin Orthop Relat Res. 2007;460:210-218.
[27] DAVIS TJ, SHELBOURNE KD, KLOOTWYK TE. Correlation of the intercondylar notch width of the femur to the width of the anterior and posterior cruciate ligaments. Knee Surg Sports Traumatol Arthrosc. 1999;7(4):209-214.
[28] DIENST M, SCHNEIDER G, ALTMEYER K, et al. Correlation of intercondylar notch cross sections to the ACL size: a high resolution MR tomographic in vivo analysis. Arch Orthop Trauma Surg. 2007;127(4):253-260.
[29] ALENTORN-GELI E, PELFORT X, MINGO F, et al. An Evaluation of the Association Between Radiographic Intercondylar Notch Narrowing and Anterior Cruciate Ligament Injury in Men: The Notch Angle Is a Better Parameter Than Notch Width. Arthroscopy. 2015;31(10):2004-2013.
[30] AL-SAEED O, BROWN M, ATHYAL R, et al. Association of femoral intercondylar notch morphology, width index and the risk of anterior cruciate ligament injury. Knee Surg Sports Traumatol Arthrosc. 2013;21(3):678-682.
[31] MA S, TIAN XD, TAN YT, et al. [Clinical study of intercondylar fossa formation to prevent intercondylar fossa impingement after high tibia osteotomy]. Zhongguo Gu Shang. 2023;36(10):943-948.
[32] KOH JRD, LOH SYJ. All-inside posterior cruciate ligament reconstruction-A systematic review of current practice. J Orthop. 2024;55:1-10.
[33] BERNHARDSON AS, DEPHILLIPO NN, DANEY BT, et al. Posterior Tibial Slope and Risk of Posterior Cruciate Ligament Injury. Am J Sports Med. 2019;47(2):312-317.
[34] YIN B, ZHAO P, CHEN J, et al. Decreased lateral posterior tibial slope and medial tibial depth are underlying anatomic risk factors for posterior cruciate ligament injury: a case-control study. BMC Musculoskelet Disord. 2022;23(1):689.
[35] YOON KH, LEE JH, KIM SG, et al. Effect of Posterior Tibial Slopes on Graft Survival Rates at 10 Years After Primary Single-Bundle Posterior Cruciate Ligament Reconstruction. Am J Sports Med. 2023;51(5):1194-1201.
[36] SHELBURNE KB, KIM HJ, STERETT WI, et al. Effect of posterior tibial slope on knee biomechanics during functional activity. J Orthop Res. 2011;29(2): 223-231.
[37] BERNHARDSON AS, AMAN ZS, DEPHILLIPO NN, et al. Tibial Slope and Its Effect on Graft Force in Posterior Cruciate Ligament Reconstructions. Am J Sports Med. 2019;47(5):1168-1174.
[38] GIFFIN JR, STABILE KJ, ZANTOP T, et al. Importance of tibial slope for stability of the posterior cruciate ligament deficient knee. Am J Sports Med. 2007;35(9):1443-1449.
[39] AGNESKIRCHNER JD, HURSCHLER C, STUKENBORG-COLSMAN C, et al. Effect of high tibial flexion osteotomy on cartilage pressure and joint kinematics: a biomechanical study in human cadaveric knees. Winner of the AGA-DonJoy Award 2004. Arch Orthop Trauma Surg. 2004;124(9):575-584.
[40] WINKLER PW, WAGALA NN, CARROZZI S, et al. Low posterior tibial slope is associated with increased risk of PCL graft failure. Knee Surg Sports Traumatol Arthrosc. 2022;30(10):3277-3286.
[41] STURNICK DR, VACEK PM, DESARNO MJ, et al. Combined anatomic factors predicting risk of anterior cruciate ligament injury for males and females. Am J Sports Med. 2015;43(4):839-847.
[42] HUANG YL, JUNG J, MULLIGAN CMS, et al. A Majority of Anterior Cruciate Ligament Injuries Can Be Prevented by Injury Prevention Programs: A Systematic Review of Randomized Controlled Trials and Cluster-Randomized Controlled Trials With Meta-analysis. Am J Sports Med. 2020;48(6): 1505-1515. |