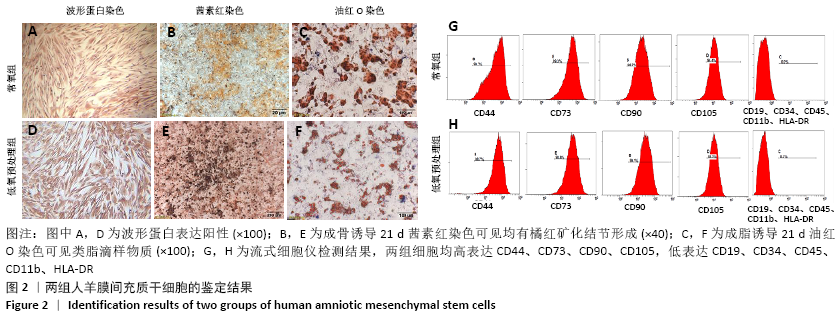
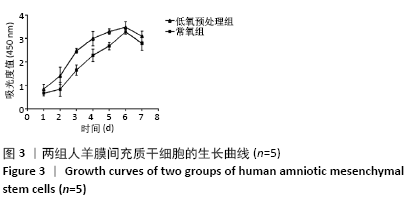
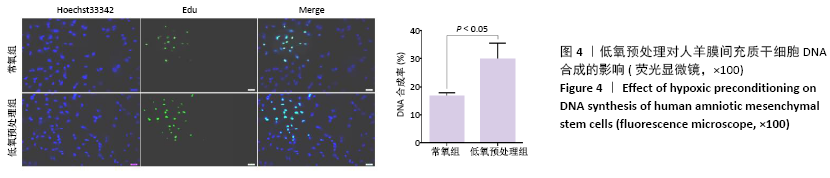
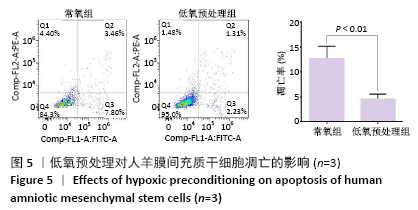
[1] WEI L, WEI ZZ, JIANG MQ, et al. Stem cell transplantation therapy for multifaceted therapeutic benefits after stroke. Prog Neurobiol. 2017;157:49-78.
[2] LIU Y, GUO LB, XU JK. Amniotic stem cell transplantation therapy for type 2 diabetes: 3 years’ follow-up report. Eur Rev Med Pharmacol Sci. 2016;20(18): 3877-3885.
[3] HUANG GL, ZHANG NN, WANG JS, et al. Transdifferentiation of human amniotic epithelial cells into acinar cells using a double-chamber system. Cell Reprogram. 2012;14(4):377-383.
[4] AMIRI F, JAHANIAN-NAJAFABADI A, ROUDKENAR MH. In vitro augmentation of mesenchymal stem cells viability in stressful microenvironments : In vitro augmentation of mesenchymal stem cells viability. Cell Stress Chaperones. 2015; 20(2):237-251.
[5] YU SP, WEI Z, WEI L. Preconditioning strategy in stem cell transplantation therapy. Transl Stroke Res. 2013;4(1):76-88.
[6] 莫壁伶,黄子祥,黄帅,等.低氧预处理脂肪间充质干细胞移植对小鼠心肌梗死后心肌细胞凋亡及血管新生的影响[J].山东医药,2018,58(33):28-31.
[7] WANG JW, QIU YR, FU Y, et al. Transplantation with hypoxia-preconditioned mesenchymal stem cells suppresses brain injury caused by cardiac arrest-induced global cerebral ischemia in rats. J Neurosci Res. 2017;95(10):2059-2070.
[8] SYVA SH, AMPON K, LASIMBANG H, et al. Microenvironmental factors involved in human amnion mesenchymal stem cells fate decisions. J Tissue Eng Regen Med. 2017;11(2):311-320.
[9] INSAUSTI CL, BLANQUER M, BLEDA P, et al. The amniotic membrane as a source of stem cells. Histol Histopathol. 2010;25(1):91-98.
[10] DÍAZ-PRADO S, MUIÑOS-LÓPEZ E, HERMIDA-GÓMEZ T, et al. Human amniotic membrane as an alternative source of stem cells for regenerative medicine. Differentiation. 2011;81(3):162-171.
[11] GRZYWOCZ Z, PIUS-SADOWSKA E, KLOS P, et al. Growth factors and their receptors derived from human amniotic cells in vitro. Folia Histochem Cytobiol. 2014;52(3):163-170.
[12] 肖建辉. 人羊膜干细胞:再生医学的理想种子细胞资源[J]. 遵义医学院学报, 2015,38(5):439-449.
[13] KIM SW, ZHANG HZ, KIM CE, et al. Amniotic mesenchymal stem cells with robust chemotactic properties are effective in the treatment of a myocardial infarction model. Int J Cardiol. 2013;168(2):1062-1069.
[14] KIM SW, ZHANG HZ, GUO L, et al. Amniotic mesenchymal stem cells enhance wound healing in diabetic NOD/SCID mice through high angiogenic and engraftment capabilities. PLoS One. 2012;7(7):e41105.
[15] MASTRI M, LIN H, LEE T. Enhancing the efficacy of mesenchymal stem cell therapy. World J Stem Cells. 2014;6(2):82-93.
[16] WANG X, ZHAO T, HUANG W, et al. Hsp20-engineered mesenchymal stem cells are resistant to oxidative stress via enhanced activation of Akt and increased secretion of growth factors. Stem Cells. 2009;27(12):3021-3031.
[17] XUE J, LI X, LU Y, et al. Gene-modified mesenchymal stem cells protect against radiation-induced lung injury. Mol Ther. 2013;21(2):456-465.
[18] LEE JH, YOON YM, LEE SH. Hypoxic Preconditioning Promotes the Bioactivities of Mesenchymal Stem Cells via the HIF-1α-GRP78-Akt Axis. Int J Mol Sci. 2017; 18(6):1320.
[19] 姚舜,靳安民,张辉,等.低氧预处理对脐带间充质干细胞表型、增殖及神经营养因子分泌功能的影响[J].山东医药,2017,57(32):25-28.
[20] KUMAR S, VAIDYA M. Hypoxia inhibits mesenchymal stem cell proliferation through HIF1α-dependent regulation of P27. Mol Cell Biochem. 2016;415(1-2): 29-38.
[21] XU R, GREENING DW, ZHU HJ, et al. Extracellular vesicle isolation and characterization: toward clinical application. J Clin Invest. 2016;126(4):1152-1162.
[22] AN HY, SHIN HS, CHOI JS, et al. Adipose Mesenchymal Stem Cell Secretome Modulated in Hypoxia for Remodeling of Radiation-Induced Salivary Gland Damage. PLoS One. 2015;10(11):e0141862.
[23] TRAN SD, LIU Y, XIA D, et al. Paracrine effects of bone marrow soup restore organ function, regeneration, and repair in salivary glands damaged by irradiation. PLoS One. 2013;8(4):e61632.
[24] LOMBAERT I, MOVAHEDNIA MM, ADINE C, et al. Concise Review: Salivary Gland Regeneration: Therapeutic Approaches from Stem Cells to Tissue Organoids. Stem Cells. 2017;35(1):97-105.
[25] MAUMUS M, JORGENSEN C, NOËL D. Mesenchymal stem cells in regenerative medicine applied to rheumatic diseases: role of secretome and exosomes. Biochimie. 2013;95(12):2229-2234.
[26] YAMADA PM, LEE KW. Perspectives in mammalian IGFBP-3 biology: local vs. systemic action. Am J Physiol Cell Physiol. 2009;296(5):C954-976.
[27] LAWLER PR, LAWLER J. Molecular basis for the regulation of angiogenesis by thrombospondin-1 and -2. Cold Spring Harb Perspect Med. 2012;2(5):a006627. |