Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (18): 2911-2918.doi: 10.3969/j.issn.2095-4344.2635
Previous Articles Next Articles
Selection and discussion of the best treatment strategy for different
types of rotator cuff injury
Zhao Di, Han Yanhong, Pan Jianke, Zhao Jinlong, Lin Jiongtong, Huang Hetao, Liu Jun
- Department of Orthopedics, the Second Affiliated Hospital of Guangzhou University of Chinese Medicine (Guangdong Provincial Hospital of Chinese Medicine), Guangzhou 510120, Guangdong Province, China
-
Received:2019-10-11Revised:2019-10-14Accepted:2019-12-13Online:2020-06-28Published:2020-04-03 -
Contact:Liu Jun, Chief physician, Professor, Doctoral supervisor, Department of Orthopedics, the Second Affiliated Hospital of Guangzhou University of Chinese Medicine (Guangdong Provincial Hospital of Chinese Medicine), Guangzhou 510120, Guangdong Province, China -
About author:Zhao Di, Master candidate, Department of Orthopedics, the Second Affiliated Hospital of Guangzhou University of Chinese Medicine (Guangdong Provincial Hospital of Chinese Medicine), Guangzhou 510120, Guangdong Province, China -
Supported by:the Project of Guangdong Provincial Department of Finance, No. [2014]157; the Project of Administration of Traditional Chinese Medicine of Guangdong Province, No. 20181119; the Research Project of TCM Science and Technology in Guangdong Provincial Hospital of Chinese Medicine, No. YK2013B2N19 and YN2015MS15
CLC Number:
Cite this article
Zhao Di, Han Yanhong, Pan Jianke, Zhao Jinlong, Lin Jiongtong, Huang Hetao, Liu Jun.
Selection and discussion of the best treatment strategy for different
types of rotator cuff injury
share this article
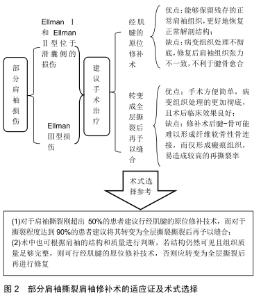
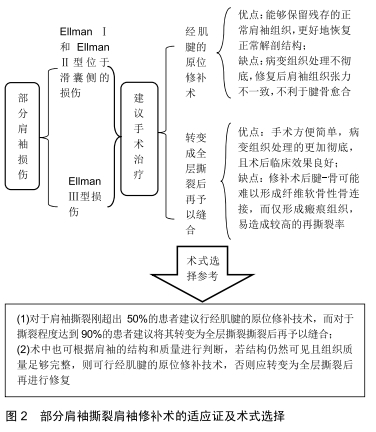
2.1 保守治疗 目前保守治疗仍被作为肩袖损伤的常规治疗方式,保守治疗的方式有很多,包括患肢固定、药物治疗、中医治疗和康复治疗等。目前认为保守治疗的适应证主要集中在以下几个方面:①全层肩袖撕裂程度小于1 cm的患者;②无创性或无症状的全层撕裂患者;③部分肩袖损伤患者(更适用于肌腱撕裂厚度小于50%的患者);④慢性撕裂或对功能要求不高的老年患者(大于65或70岁)。其中对于部分肩袖损伤患者,一项研究中发现,在76例诊断为部分肩袖损伤的患者中,对其中的37例患者采取保守治疗,最终有91%的患者获得了满意的效果[4]。该作者还发现对于部分肩袖损伤肌腱撕裂厚度小于50%的患者,保守治疗的效果相比于肌腱撕裂厚度大于50%的患者效果更好。PETRI等[5]认为保守治疗适用于慢性撕裂的老年患者(大于65或70岁),TASHJIAN等[6]在文章中提出任何年龄的全层肩袖撕裂的小撕裂患者(小于1 cm),也可采取积极的保守治疗。对于全层肩袖撕裂的患者,BOORMAN等[7]认为保守治疗对于全层肩袖损伤的患者效果良好,在5年的随访研究中,保守治疗在肩袖全层撕裂的病例中有效率约75%。他在文章中提到对于保守治疗的过程中要关注以下2点:①患者对于保守治疗的效果如何;②症状是否会复发或加重。如果患者对于保守治疗的反应较差或出现疼痛症状的复发或加重,应尽早进行手术干预。在一项多中心前瞻性队列研究中,共纳入了452例患者,进行为期2年的随访发现,有75%的无创性全层肩袖撕裂患者的症状得到了改善,说明保守治疗能够达到良好的效果[8]。但应警惕无症状的全层肩袖损伤患者,其有可能发展为有症状的或肩袖撕裂进一步扩大[9-10],需告知患者定期随访,以便及时调整治疗策略。 2.2 手术治疗 在保守治疗中,对于部分肩袖损伤患者,如果出现症状的加重,应提高警惕,尽快手术治疗;对于肩袖全层撕裂患者,可先予保守治疗6-8周,若症状未见好转或出现急性加重者,应积极采取手术治疗;而对于有创性或急性肩袖损伤患者,此时肌腱仍然强健有力且移动性良好,应尽早行手术治疗。对于肌力恢复要求高的患者,如军人、运动员,也应提倡手术治疗[11-12]。目前的手术类型分为开放性手术和关节镜下手术,其中关节镜下手术又分为关节镜辅助下的小切口治疗以及全关节镜治疗。手术方式则更加多样化,主要包括肩袖清创术、修补术、上关节囊重建术、肌腱移位术、反肩置换术以及最新的肩峰下球囊间隔术等。 2.2.1 关节镜下肩袖清创术及肱二头肌长头键的切断或固定 关节镜下清创术主要包括对一些病变的滑囊、滑膜、关节囊部分予以清理,以缓解疼痛为主。目前认为单纯进行关节镜下清创术可用于部分肩袖撕裂厚度< 50%或EllmanⅠ或Ⅱ型[13-14]。REYNOLDS等[15]对部分小型肩袖撕裂运动员进行了相关研究发现单纯行关节镜下清创术能够很好地恢复肩关节功能,但可能要比伤前功能弱。而对于是否需要同时行肩峰下减压成形术尚存在争议。BUDOFF等[16]在长期的随访中发现单纯关节镜下清创术而不进行肩峰减压成形术对于非全层撕裂的肩袖损伤患者具有很好的疗效,并且能最大限度降低手术所带来的创伤。但有学者认为导致滑囊侧部分撕裂的主要原因是由于肩峰下撞击引起的,且与关节侧相比,其有创伤病史的比率明显较低[13,17]。有研究将滑囊侧的部分撕裂与关节侧进行了对比,发现滑囊侧肩峰的病理变化更明显,而肌腱退变程度较轻[18]。因此对于滑囊侧撕裂若术前X射线片提示为Ⅱ型或Ⅲ型肩峰,同时术中发现有肩峰撞击的表现,则应行肩峰成形术;而对于关节侧损伤,则可单纯行关节镜下清理术。但需注意这种治疗方式虽然能减轻患者疼痛,但并不能阻止病程的进展[19],仍有部分患者最终会发展为全层肩袖撕裂,所以同保守治疗一样,需定期随访。 对于全层撕裂患者,一项随机对照试验发现,非肩峰成形术组具有更高的再手术率[20]。ABRAMS等[21]在为期2年的随访研究中得出全层撕裂而未进行肩峰成形组与肩峰成形组相比差异没有显著性意义,但在未行肩峰成形组中要求二次手术的概率更大。作者认为行肩峰下减压成形术有利于解决肩峰下撞击的因素,从而在更大程度上缓解患者疼痛,降低再手术率的风险。 同时也不能忽略,肩袖撕裂通常也会伴有肱二头肌长头肌腱的损伤,因此肱二头肌长头肌腱磨损所引发的炎症也是造成肩关节疼痛的原因之一。尤其在巨大肩袖撕裂时,其压制肱骨头的力量减弱,会导致肱骨头上移,致使肩袖间隙变窄,更加重了肌腱的磨损。目前临床上主要采取肱二头肌长头肌腱切断或固定术来减轻患者症状,2种术式在改善患者功能和缓解疼痛方面没有明显差异[22]。但2种手术方均存在不良的手术并发症:肩关节镜下肱二头肌长头腱单纯切断术可能会使部分患者出现Popeye畸形(大力水手征)、肌力减弱(肘关节屈曲、前臂旋后功能)、肱骨头上移等并发症[23];而肩关节镜下肱二头肌长头腱单纯保留术虽然可以很好的解决上述问题,但可能会引起疼痛残留、感染等风险的增加[24]。因此2种手术方式的选择仍存在一定争议。对于合并有肱二头肌长头肌腱损伤的患者,联合肱二头肌长头键切断或固定术,可以有效减轻患者疼痛症状,有利于后期康复治疗,提高患者满意度,但对于其并发症的发生仍然不可忽视。 2.2.2 肩袖修补术 (1)部分肩袖撕裂:随着对关节镜手术认识的不断加深,肩袖修补术已经由原来的开放手术转变为关节镜辅助下小切口手术和全关节镜下手术。由于镜下修补技术能很大程度恢复肩关节的生物力学特性,保留肩袖的完整性,因此已经逐渐成为首选方案。目前对于部分撕裂的肩袖修补术分为2种:经肌腱的原位修补术和转变成全层撕裂后再予以缝合。这2种手术方式均存在各自的优缺点,经肌腱修补技术的优势在于当重建撕裂肌腱的同时,能够保留残存的正常肩袖组织,从而能更好地恢复正常的解剖结构,但由于其处理的病变组织不彻底,易导致修复后肩袖组织的张力不一致,不利于腱骨愈合[25];而转变成全层撕裂后再予以缝合的优势在于手术更加方便简单,病变组织处理的更加彻底,且术后临床效果良好,但由于其修补术后腱-骨可能难以形成纤维软骨性骨连接,而仅形成了瘢痕组织,所以容易造成较高的撕裂率[26-27]。有学者则提出对于肩袖撕裂刚超出50%的患者建议行经肌腱的原位修补技术,而对于撕裂程度达到90%的患者建议将其转变为全层撕裂撕裂后再予以缝合[28]。术中也可根据肩袖的结构和质量进行判断,若结构仍然可见且组织质量足够完整,则可行经肌腱的原位修补技术,否则应转变为全层撕裂后再进行修复。 在镜下修补术的适应证方面,多数学者认为对于EllmanⅢ型的患者应行肩袖修补术。而对于EllmanⅠ和EllmanⅡ型损伤,CORDASCO等[29]在进行10年的随访中发现,对于撕裂程度小于50%的滑囊侧的部分撕裂,仅行清创术和肩峰下减压术,要比关节侧具有更高的手术失败率(38% vs. 5%)。MCCONVILLE等[30]认为滑囊侧的肩袖组织分布有较多的神经和血管组织,仅行清创术和肩峰下减压术而不做缝合处理并不能减轻患者疼痛。并且有报道称对于滑囊侧撕裂仅行清创术和肩峰下减压术具有更高的手术失败率和再撕裂率[25,31]。所以应当引起足够重视。因此对于小于50%的滑囊侧部分撕裂的患者建议行肩袖修补术,详见图2。 "

(2)全层肩袖撕裂:对于肩袖全层撕裂的修复,讨论更多的是肩袖的修复技术,目前常用的方法包括单排固定、双排固定和缝线桥固定技术。其中双排固定和缝线桥固定能增加肌腱与足印区的接触面积,同时提供了更大的拉力负荷,增强了初始生物力学强度,更利于腱骨愈合,降低再撕裂率[32]。在一项系统评价中发现,当肩袖撕裂长度<3 cm时,使用单排、双排技术对于术后功能评分上没有明显差别,但>3 cm的肩袖撕裂,使用双排技术可以明显改善术后评分[33]。而对于缝线桥技术,KIM等[34]认为其在>1 cm的肩袖撕裂患者中应用可取得满意结果,但<1 cm的肩袖撕裂使用单排效果更好[35]。因此双排缝合及缝线桥技术可能更适用于中型和大型肩袖损伤。 目前单排、双排以及双排缝线桥技术,在中小型及部分大型肩袖撕裂中的效果得到了肯定,但在巨大肩袖撕裂中,由于其撕裂范围广,回缩明显,修复难度大以及再撕裂率高,普通的缝合方式很难达到良好的修复效果,因此很多学者总结出了其他的固定缝合技术,如部分修复术、肩袖间隙滑移术或结合肌腱止点内移术、边对边缝合技术等可用于巨大肩袖损伤的修复。不过尽管通过上述修复方式的改良,能使巨大肩袖的撕裂缘重新固定于肱骨大结节,从而改善肩关节功能,增加肌肉力量,缓解疼痛。但巨大肩袖撕裂在修复术后,由于其张力过大,再撕裂率可达34%-94%[36]。因此,为了能够更好的解决类似问题,对新的技术和材料开展了广泛的研究,并逐步应用于临床。 2.2.3 上关节囊重建术 肩关节囊在稳定盂肱关节稳定方面起着重要的作用,有研究表明,上关节囊的缺损会引起盂肱关节的不稳,导致其在各个方向的滑动度增加[37-38],而经过重建修补后,其可以改善力学平衡,稳定盂肱关节,并且能够封闭关节腔,使关节液正常分泌。但该技术需要与补片技术相结合。MIHATA等[39]采用自体阔筋膜对巨大肩袖损伤患者的上方关节囊进行了重建,其外侧折叠后使用双排技术固定于肱骨大结节,内侧则与冈上和冈下肌腱的前部或肩胛下肌腱进行缝合,术后随访发现在临床疗效评分和肩部力量上均有提高和改善。但作者指出该项技术的应用需排除肱骨头的严重上移、颈神经麻痹、腋神经麻痹、三角肌功能障碍和感染。MIHATA等[40]在一项队列研究中,使用该技术对100例巨大不修复性肩袖撕裂患者进行了观察,其中60例患者术前曾参加了体育运动或锻炼,最终随访发现上关节囊重建技术可以使大部分患者恢复到原有的活动状态,并认为该技术尤其适用于喜欢体育运动或从事重体力劳动的患者。有部分研究者报道,使用脱细胞真皮补片作为修补材料对巨大肩袖撕裂患者的上关节囊进行重建修补,最后所得出的结果也令人满意[41-42]。对于上关节囊重建术的选择,PENNINGTON等[43]认为保守治疗效果不好的巨大肩袖撕裂,同时盂肱关节没有明显退变的患者,可以选择上关节囊重建术。HIRAHARA等[44]认为上关节囊重建术的适应证为巨大的、不可修复的冈上肌和(或)冈下肌撕裂,三角肌功能正常,最好不伴有关节炎的患者。因此存在巨大或不可修复性冈上肌和(或)冈下肌撕裂,三角肌功能正常,被动活动良好,主动功能受限,不伴有明显盂肱关节退变、严重肱骨头上移、颈神经及腋神经麻痹,同时最好不伴有关节炎的患者,经保守或姑息治疗后症状加重者,则可以选择上关节囊重建术,尤其对于喜欢体育运动或从事重体力劳动的患者。 2.2.4 肌腱移位术 肌腱转位术是巨大肩袖损伤的一种治疗方式,目前常采用的肌腱转位主要包括背阔肌、胸大肌、斜方肌等。其主要是改变部分肌腱的止点,替代原有肩袖的功能,重建盂肱关节水平或垂直方向的力偶,并起到缓解疼痛的作用。背阔肌移位主要用于巨大肩袖损伤的后上部撕裂。在转位后,背阔肌对肩关节起到外旋的作用,并具有下压肱骨头的功能[45-46]。EI-AZAB等[47]对86例背阔肌移位术患者进行了随访研究,随访平均时间为9.3年。平均美国肩肘外科指数从30分提高到70分,平均目测类比评分从7.8分降低到2.4分,肩袖撕裂关节病的平均Hamada分级由术前的1.7(0-2级)提高到2.2级(1-5级)。并发现患者越年轻,愈后结果越好。GERBER等[48]在一项长期随访中也得出了背阔肌肌腱移位术是一种治疗肩袖后损伤的有效方法,肩部功能和疼痛得到了实质性和持久的改善。而在该项研究中作者发现对伴有小圆肌脂肪浸润和肩胛下肌功能不全的患者,术后结果较差。目前随着关节镜技术的不断发展,镜下行背阔肌转位术也得到了良好的效果,并且在短期疗效上与传统切开术相比没有明显差异[49]。因此对于年轻、活动能力较强、存在后上侧巨大肩袖撕裂、并且仅存在轻微盂肱关节炎、同时肩胛下肌和小圆肌功能良好的患者,行背阔肌移位手术并结合关节镜技术是理想的手术方案。 而对于前上部巨大或不可修复肩袖撕裂(冈上肌或肩胛下肌),胸大肌转位术则成为了一种理想治疗方案的选择。MORODER等[50]在一项长期研究中,对27例前上部不可修复肩袖撕裂进行了喙突下胸大肌转位术,术后平均随访10年发现,尽管有2/3的患者存在影像学上的肩袖撕裂关节病的进展,但仍有77%的患者对手术表示非常满意。在一项系统评价中,共纳入了8篇文献(共195例),平均随访了33.4个月后,术后肩功能、力量和疼痛均有改善,且术后出现神经麻痹的发生率较低[51]。并且该研究还发现在喙突下行胸大肌转位术的Constant评分要明显高于喙突上转位。因此胸大肌转位术适用于不可修复的前上部肩袖撕裂,尤其对于单纯性的肩胛下肌撕裂,术后结果最佳[52]。 斜方肌移位也是治疗巨大肩袖损伤的一种肌腱移位方式。OMID等[53]在一项生物力学的研究比较中发现,相比于背阔肌转位术,斜方肌转位术在恢复肱骨原有生物力学、重建前后力偶方面要更理想,并且能够更好的限制患者肱骨的过度内旋,但由于斜方肌的肌腱部分较短,通常需要与自体或异体肌腱相结合的方式进行手术。ELHASSAN等[54]采用斜方肌移位和同种异体跟腱加强的方式对33例不可修复性后上部巨大肩袖撕裂的患者进行了治疗,在平均47个月的随访后发现,其中32例患者的肩关节疼痛、活动度有了明显的改善,尤其对于术前能够屈曲大于60°的患者,效果更加显著。除了上述肌腱转位方式外,也有学者报道使用三角肌肌瓣转位术、胸小肌转位术和大圆肌转位术来治疗不可修复肩袖损伤[55-57],也得到了较好的临床结果,但三角肌肌瓣转位术远期的效果并不理想[58-59]。 2.2.5 反肩置换 反肩关节置换是指在肩胛骨关节盂侧放置半球型关节面,在肱骨近端侧放置盂杯的半限制性人工全肩关节置换。反肩关节置换通过内移盂肱关节的旋转中心,减少了肩胛盂之间的剪切力,增加了肩关节外展时三角肌的力臂,同时在肱骨侧近端的假体下移,增加了肩肱间距,使得三角肌的张力增高,发挥了三角肌在肩袖缺损的情况下稳定肩关节的作用。ERNSTBRUNNER等[60]在一项系统回顾中纳入了8项研究(365例),在手术后20年内,患者主客观评分均有显著改善,并在平均9.5年的随访期间,肩关节功能和预后评分均没有明显恶化的表现,但有42%的患者出现了Ⅲ级或Ⅳ级肩胛盂切迹。ERNSTBRUNNER等[60]所纳入的部分文章认为肩胛骨盂切迹的形成与术前较差的肩关节功能有关,并且有文章认为肩胛骨盂切迹形成会出现较差的预后。GERBER等[61]对22例反肩关节置换手术进行15年的随访研究,发现尽管在术后所有患者的肩关节功能和主观评分都有了实质性改善,但仍有59%的患者出现了一种或多种并发症,并有27%的患者手术失败。不过,该研究发现如果并发症在不取出假体的情况下可以得到治疗,那么最终结果就不会受到影响。并且有学者认为目前的手术技术和材料与之前相比有了很大的改进和提高,因此术后出现的并发症问题也会随之减少[60]。三角肌在反肩关节置换中起着重要的作用,保证三角肌功能的正常是决定手术的关键。有研究者也发现小圆肌损伤对反肩关节之后术后的影响也很大,其可能导致术后主动外旋功能的下降[62]。 在年龄的选择方面,ERNSTBRUNNER等[63]进行了一项长期随访研究,研究者对60岁以下患有不可修复性肩袖撕裂的患者进行了反肩关节置换术,在随访10年后发现,患者的主观感受和肩关节功能均有改善,但术后并发症发生率可达39%。EK等[64]也对年轻患者进行长期的随访发现反肩置换术并发症的发生率高达37.5%,尽管这些并发症大多可以成功治疗而不影响临床结果,但作者认为术前术者也应清楚、仔细地考虑手术所带来的风险与效益,并与患者和家属详细沟通。有学者发现尽管反肩关节置换术在10年后的翻修率较低[65],但随着时间的推移,影像学表现和临床效果都在逐渐恶化,因此对年轻患者使用反肩置换应该谨慎[66]。 患有肩袖的巨大撕裂难以修复并且合并有继发性盂肱关节炎时,反肩置换是其主要的手术适应证。但随着其适应证的扩大,对于没有合并盂肱关节炎的巨大肩袖撕裂所致的肩关节假性麻痹,也可行反肩置换治 疗[67]。尽管反肩置换术的确有良好的术后效果,但也应严格把握其适应证。对患有巨大不可修复性肩袖撕裂所致的假性麻痹,伴或不伴有盂肱关节炎且功能要求低的老年患者是反肩置换的理想适应证;但对于存在三角肌和腋神经损伤的患者则不应行反肩置换术。鉴于目前反肩置换手术长期的效果并不理想,因此对于小于60岁的年轻患者不推荐使用,可通过肌腱移位等其他治疗方式延后关节的置换。 2.2.6 肩峰下球囊间隔术 肩峰下球囊间隔术是一种新的治疗方案,它利用一种可生物降解的垫片(球囊状),予关节镜下清理后,放入肩峰下间隙,并注入生理盐水,允许肱骨头在肩峰下无摩擦的滑动,并且起到下压肱骨头的作用[68]。这种材料在动物实验研究表明其具有良好的生物相容性和安全性,可在体内使用,而不会引起局部或全身反应[69]。SINGH等[70]进行了一项生物力学研究对比,在尸体上比较了不可修复性肩袖损伤在使用肩峰下球囊间隔术和上关节囊重建术后与正常肩部的对比,分别测量在肩关节外展0°,30°,60°和90°时肱骨头的上移距离,并同时测量的肩关节的外展能力。最终发现这2种技术均可以很好的改善肩关节的功能和下压肱骨头的作用,并且2种手术方式相比没有明显差异。在一项临床研究中,研究者对37例患者(39个肩)随访至少1年后发现,所有患者的肩关节活动范围和临床功能评分均有所改善,除1例患者对垫片的进行翻修外,其余患者未见明显的术中或术后并发症[71]。并且在其他临床研究中,也得出了较理想的结果[72-73]。但有学者得出了不同的结论,该研究者对16例存在后上侧巨大肩袖撕裂的患者进行了肩峰下球囊间隔术,术后2年随访发现仅有40%(6例)的患者取得了良好的效果,其余患者均未见好转,其中5例患者由于缺乏临床改善或症状的恶化,在研究期间进行了反肩置换手术。作者认为手术失败的原因可能是垫片在肩峰下间隙的早起移动所致,或因垫片在短期内出现断裂和再吸收,导致了其早期机械作用的失效[74]。因此对于这项技术的可行度存在一定争议,仍需大量的临床研究去证实。 2.3 辅助治疗技术 目前使用的辅助治疗技术主要有肩袖补片技术、细胞种植支架技术、生长因子、富血小板血浆技术、干细胞技术等,这些技术的应用为肩袖损伤的治疗提供了新的前景。目前辅助治疗领域的相关研究也在不断创新和发展,但由于缺乏高质量的临床研究,多数实验研究存在一定的局限性,其研究的成果不能直接在临床得以应用。目前在临床中使用较广泛的是补片技术和富血小板血浆技术,尽管这2种技术相对成熟,但仍存在着许多问题急需解决,如生物相容性、可降解性、力学强度、制备标准、临床应用经验等,每一问题的解决都需要大量的实验研究和探索。不过随着对生长因子、干细胞注射等组织工程技术的不断钻研和探 讨[75-77],在未来对肩袖损伤腱-骨愈合方面的改善也会有很大的提升,尤其对于巨大肩袖撕裂的治疗,不仅包括使撕裂的肩袖闭合,恢复肩关节功能,同时也要考虑肩袖修复后的愈合问题。其中对肩袖愈合起重要作用的是腱-骨之间的正常组织,也称腱-骨复合体。肌腱和骨属于2种组织,而2种不同组织的相连处最容易引起应力的集中,导致腱-骨不愈合或再次撕裂的可能。但腱-骨复合体能够很好的转移2种不同组织之间的应力作用,从而增加了肌腱和骨之间的牢固作用,降低肩袖的再撕裂率。辅助治疗技术便能够提高和改善腱-骨之间的愈合能力,已经成为目前肩袖损伤研究的热点。 "

| [1] ALEEM AW, BROPHY RH. Outcomes of rotator cuff surgery: what does the evidence tell us? Clin Sports Med. 2012;31(4):665-674. [2] TEMPELHOF S, RUPP S, SEIL R. Age-related prevalence of rotator cuff tears in asymptomatic shoulders. J Shoulder Elbow Surg. 1999;8(4):296-299. [3] TEUNIS T, LUBBERTS B, REILLY BT, et al. A systematic review and pooled analysis of the prevalence of rotator cuff disease with increasing age. J Shoulder Elbow Surg. 2014;23(12):1913-1921. [4] LO IK, DENKERS MR, MORE KD, et al. Partial-thickness rotator cuff tears: clinical and imaging outcomes and prognostic factors of successful nonoperative treatment. Open Access J Sports Med. 2018;9:191-197. [5] PETRI M, ETTINGER M, BRAND S, et al. Non-Operative Management of Rotator Cuff Tears. Open Orthop J.2016;10: 349-356. [6] TASHJIAN RZ. Epidemiology, natural history, and indications for treatment of rotator cuff tears. Clin Sports Med.2012;31(4):589-604. [7] BOORMAN RS, MORE KD, HOLLINSHEAD RM, et al. What happens to patients when we do not repair their cuff tears? Five-year rotator cuff quality-of-life index outcomes following nonoperative treatment of patients with full-thickness rotator cuff tears. J Shoulder Elbow Surg.2018;27(3):444-448. [8] KUHN JE, DUNN WR, SANDERS R, et al. Effectiveness of physical therapy in treating atraumatic full-thickness rotator cuff tears: a multicenter prospective cohort study. J Shoulder Elbow Surg.2013;22(10):1371-1379. [9] YAMAGUCHI K, TETRO AM, BLAM O, et al. Natural history of asymptomatic rotator cuff tears: a longitudinal analysis of asymptomatic tears detected sonographically. J Shoulder Elbow Surg.2001;10(3):199-203. [10] RAMME AJ, ROBBINS CB, PATEL KA, et al. Surgical versus nonsurgical management of rotator cuff tears: a matched-pair analysis. J Bone Joint Surg Am. 2019;101(19):1775-1782. [11] WOLF BR, DUNN WR, WRIGHT RW. Indications for repair of full-thickness rotator cuff tears. Am J Sports Med.2007;35(6): 1007-1016. [12] PARNES N, BARTOSZEWSKI NR, DEFRANCO MJ. Arthroscopic repair of full-thickness rotator cuff tears in active patients younger than 40 years: 2- to 5-year clinical outcomes. Orthopedics. 2018; 41(1): e52-e57. [13] SAMBANDAM SN, KHANNA V, GUL A, et al. Rotator cuff tears: An evidence based approach. World J Orthop.2015;6(11): 902-918. [14] LIU JN, GARCIA GH, GOWD AK, et al. Treatment of partial thickness rotator cuff tears in overhead athletes. Curr Rev Musculoskelet Med.2018;11(1):55-62. [15] REYNOLDS SB, DUGAS JR, CAIN EL, et al. Debridement of small partial-thickness rotator cuff tears in elite overhead throwers. Clin Orthop Relat Res.2008;466(3):614-621. [16] BUDOFF JE, RODIN D, OCHIAI D, et al. Arthroscopic rotator cuff debridement without decompression for the treatment of tendinosis. Arthroscopy.2005;21(9):1081-1089. [17] FUKUDA H. The management of partial-thickness tears of the rotator cuff. J Bone Joint Surg Br.2003;85(1):3-11. [18] KO JY, HUANG CC, CHEN WJ, et al. Pathogenesis of partial tear of the rotator cuff: a clinical and pathologic study. J Shoulder Elbow Surg.2006;15(3):271-278. [19] MATTHEWSON G, BEACH CJ, NELSON AA, et al. Partial thickness rotator cuff tears: current concepts. Adv Orthop.2015; 2015:458786. [20] MACDONALD P, MCRAE S, LEITER J, et al. Arthroscopic rotator cuff repair with and without acromioplasty in the treatment of full-thickness rotator cuff tears: a multicenter, randomized controlled trial. J Bone Joint Surg Am.2011;93(21):1953-1960. [21] ABRAMS GD, GUPTA AK, HUSSEY KE, et al. Arthroscopic Repair of Full-Thickness Rotator Cuff Tears With and Without Acromioplasty: Randomized Prospective Trial With 2-Year Follow-up. Am J Sports Med.2014;42(6):1296-1303. [22] SHANG X, CHEN J, CHEN S. A meta-analysis comparing tenotomy and tenodesis for treating rotator cuff tears combined with long head of the biceps tendon lesions. PLoS One.2017; 12(10): e185788. [23] VIRK MS, NICHOLSON GP. Complications of Proximal Biceps Tenotomy and Tenodesis. Clin Sports Med.2016;35(1):181-188. [24] FRANCESCHI F, LONGO UG, RUZZINI L, et al. To detach the long head of the biceps tendon after tenodesis or not: outcome analysis at the 4-year follow-up of two different techniques. Int Orthop.2007;31(4):537-545. [25] KIM KC, SHIN HD, CHA SM, et al. Repair integrity and functional outcome after arthroscopic conversion to a full-thickness rotator cuff tear: articular- versus bursal-side partial tears. Am J Sports Med.2014;42(2):451-456. [26] BROCKMEIER SF, DODSON CC, GAMRADT SC, et al. Arthroscopic intratendinous repair of the delaminated partial-thickness rotator cuff tear in overhead athletes. Arthroscopy.2008;24(8):961-965. [27] KIM YS, LEE HJ, BAE SH, et al. Outcome Comparison Between in Situ Repair Versus Tear Completion Repair for Partial Thickness Rotator Cuff Tears. Arthroscopy.2015;31(11): 2191-2198. [28] PARK JY, CHUNG KT, YOO MJ. A serial comparison of arthroscopic repairs for partial- and full-thickness rotator cuff tears. Arthroscopy.2004;20(7):705-711. [29] CORDASCO FA, BACKER M, CRAIG EV, et al. The partial-thickness rotator cuff tear: is acromioplasty without repair sufficient?. Am J Sports Med.2002;30(2):257-260. [30] MCCONVILLE OR, IANNOTTI JP. Partial-thickness tears of the rotator cuff: evaluation and management. J Am Acad Orthop Surg. 1999;7(1):32-43. [31] CHUNG SW, KIM JY, YOON JP, et al. Arthroscopic repair of partial-thickness and small full-thickness rotator cuff tears: tendon quality as a prognostic factor for repair integrity. Am J Sports Med. 2015;43(3):588-596. [32] BAUMS MH, SCHMINKE B, POSMYK A, et al. Effect of single- and double-row rotator cuff repair at the tendon-to-bone interface: preliminary results using an in vivo sheep model. Arch Orthop Trauma Surg.2015;135(1):111-118. [33] CHEN M, XU W, DONG Q, et al. Outcomes of single-row versus double-row arthroscopic rotator cuff repair: a systematic review and meta-analysis of current evidence. Arthroscopy.2013; 29(8): 1437-1449. [34] KIM YK, MOON SH, CHO SH. Treatment outcomes of single- versus double-row repair for larger than medium-sized rotator cuff tears: the effect of preoperative remnant tendon length. Am J Sports Med.2013;41(10):2270-2277. [35] AYDIN N, KARAISMAILOGLU B, GURCAN M, et al. Arthroscopic double-row rotator cuff repair: a comprehensive review of the literature. SICOT J.2018;4:57. [36] NERI BR, CHAN KW, KWON YW. Management of massive and irreparable rotator cuff tears. J Shoulder Elbow Surg.2009; 18(5): 808-818. [37] ISHIHARA Y, MIHATA T, TAMBOLI M, et al. Role of the superior shoulder capsule in passive stability of the glenohumeral joint. J Shoulder Elbow Surg.2014;23(5):642-648. [38] SHEEAN AJ, HARTZLER RU, BURKHART SS. Rotator cuff repair: single row repair versus double row repair and superior capsular reconstruction. Sports Med Arthrosc Rev.2018;26(4):171-175. [39] MIHATA T, LEE TQ, WATANABE C, et al. Clinical results of arthroscopic superior capsule reconstruction for irreparable rotator cuff tears. Arthroscopy.2013;29(3):459-470. [40] MIHATA T, LEE TQ, FUKUNISHI K, et al. Return to sports and physical work after arthroscopic superior capsule reconstruction among patients with irreparable rotator cuff tears. Am J Sports Med.2018;46(5):1077-1083. [41] PETRI M, GREENSPOON JA, MOULTON SG, et al. Patch-augmented rotator cuff repair and superior capsule reconstruction. Open Orthop J.2016;10:315-323. [42] BURKHART SS, DENARD PJ, ADAMS CR, et al. Arthroscopic superior capsular reconstruction for massive irreparable rotator cuff repair. Arthrosc Tech.2016;5(6):e1407-e1418. [43] PENNINGTON WT, BARTZ BA, PAULI JM, et al. Arthroscopic superior capsular reconstruction with acellular dermal allograft for the treatment of massive irreparable rotator cuff tears: short-term clinical outcomes and the radiographic parameter of superior capsular distance. Arthroscopy.2018;34(6):1764-1773. [44] HIRAHARA AM, ADAMS CR. Arthroscopic superior capsular reconstruction for treatment of massive irreparable rotator cuff tears. Arthrosc Tech.2015;4(6):e637-e641. [45] HENSELER JF, NAGELS J, NELISSEN RG, et al. Does the latissimus dorsi tendon transfer for massive rotator cuff tears remain active postoperatively and restore active external rotation? J Shoulder Elbow Surg.2014;23(4):553-560. [46] ANASTASOPOULOS PP, ALEXIADIS G, SPYRIDONOS S, et al. Latissimus dorsi transfer in posterior irreparable rotator cuff tears. Open Orthop J.2017;11:77-94. [47] EL-AZAB HM, ROTT O, IRLENBUSCH U. Long-term follow-up after latissimus dorsi transfer for irreparable posterosuperior rotator cuff tears. J Bone Joint Surg Am.2015;97(6):462-469. [48] GERBER C, RAHM SA, CATANZARO S, et al. Latissimus dorsi tendon transfer for treatment of irreparable posterosuperior rotator cuff tears: long-term results at a minimum follow-up of ten years. J Bone Joint Surg Am.2013;95(21):1920-1926. [49] KANATLI U, OZER M, ATAOGLU MB, et al. Arthroscopic-assisted latissimus dorsi tendon transfer for massive, irreparable rotator cuff tears: technique and short-term follow-up of patients with pseudoparalysis. Arthroscopy.2017;33(5):929-937. [50] MORODER P, SCHULZ E, MITTERER M, et al. Long-term outcome after pectoralis major transfer for irreparable anterosuperior rotator cuff tears. J Bone Joint Surg Am.2017; 99(3):239-245. [51] SHIN JJ, SACCOMANNO MF, COLE BJ, et al. Pectoralis major transfer for treatment of irreparable subscapularis tear: a systematic review. Knee Surg Sports Traumatol Arthrosc.2016; 24(6):1951-1960. [52] OMID R, STONE MA, LIN CC, et al. Biomechanical analysis of anterior capsule reconstruction and latissimus dorsi transfer for irreparable subscapularis tears. J Shoulder Elbow Surg. 2019. [53] OMID R, HECKMANN N, WANG L, et al. Biomechanical comparison between the trapezius transfer and latissimus transfer for irreparable posterosuperior rotator cuff tears. J Shoulder Elbow Surg.2015;24(10):1635-1643. [54] ELHASSAN BT, WAGNER ER, WERTHEL JD. Outcome of lower trapezius transfer to reconstruct massive irreparable posterior- superior rotator cuff tear. J Shoulder Elbow Surg.2016;25(8): 1346-1353. [55] ROUKOZ S, NABHANE L, AIDIBI A, et al. Deltoid flap for management of massive irreparable rotator cuff tears: case series. J Med Liban.2016;64(1):8-12. [56] YAMAKADO K. Arthroscopic-Assisted Pectoralis Minor Transfer for Irreparable Anterosuperior Massive Rotator Cuff Tear. Arthrosc Tech.2018;7(3):e193-e198. [57] KOLK A, HENSELER JF, OVERES FJ, et al. Teres major tendon transfer in the treatment of irreparable posterosuperior rotator cuff tears: long-term improvement of shoulder function and pain reduction at eight to 12 years' follow-up. Bone Joint J.2018; 100-B(3):309-317. [58] SPAHN G, KIRSCHBAUM S, KLINGER HM. A study for evaluating the effect of the deltoid-flap repair in massive rotator cuff defects. Knee Surg Sports Traumatol Arthrosc.2006;14(4):365-372. [59] LU XW, VERBORGT O, GAZIELLY DF. Long-term outcomes after deltoid muscular flap transfer for irreparable rotator cuff tears. J Shoulder Elbow Surg.2008;17(5):732-737. [60] ERNSTBRUNNER L, ANDRONIC O, GRUBHOFER F, et al. Long-term results of reverse total shoulder arthroplasty for rotator cuff dysfunction: a systematic review of longitudinal outcomes. J Shoulder Elbow Surg.2019;28(4):774-781. [61] GERBER C, CANONICA S, CATANZARO S, et al. Longitudinal observational study of reverse total shoulder arthroplasty for irreparable rotator cuff dysfunction: results after 15 years. J Shoulder Elbow Surg.2018;27(5):831-838. [62] BOILEAU P, GONZALEZ JF, CHUINARD C, et al. Reverse total shoulder arthroplasty after failed rotator cuff surgery. J Shoulder Elbow Surg.2009;18(4):600-606. [63] ERNSTBRUNNER L, SUTER A, CATANZARO S, et al. Reverse Total Shoulder Arthroplasty for Massive, Irreparable Rotator Cuff Tears Before the Age of 60 Years: Long-Term Results. J Bone Joint Surg Am.2017;99(20):1721-1729. [64] EK ET, NEUKOM L, CATANZARO S, et al. Reverse total shoulder arthroplasty for massive irreparable rotator cuff tears in patients younger than 65 years old: results after five to fifteen years. J Shoulder Elbow Surg.2013;22(9):1199-1208. [65] FAVARD L, LEVIGNE C, NEROT C, et al. Reverse prostheses in arthropathies with cuff tear: are survivorship and function maintained over time?. Clin Orthop Relat Res.2011;469(9): 2469-2475. [66] HARTZLER RU, STEEN BM, HUSSEY MM, et al. Reverse shoulder arthroplasty for massive rotator cuff tear: risk factors for poor functional improvement. J Shoulder Elbow Surg.2015; 24(11): 1698-1706. [67] TOKISH JM, ALEXANDER TC, KISSENBERTH MJ, et al. Pseudoparalysis: a systematic review of term definitions, treatment approaches, and outcomes of management techniques. J Shoulder Elbow Surg.2017;26(6):e177-e187. [68] GERVASI E, MAMAN E, DEKEL A, et al. Fluoroscopy-guided biodegradable spacer implantation using local anesthesia: safety and efficacy study in patients with massive rotator cuff tears. Musculoskelet Surg.2016;100(Suppl 1):19-24. [69] SENEKOVIC V, POBERAJ B, KOVACIC L, et al. Prospective clinical study of a novel biodegradable sub-acromial spacer in treatment of massive irreparable rotator cuff tears. Eur J Orthop Surg Traumatol.2013;23(3):311-316. [70] SINGH S, REEVES J, LANGOHR G, et al. The subacromial balloon spacer versus superior capsular reconstruction in the treatment of irreparable rotator cuff tears: a biomechanical assessment. Arthroscopy.2019;35(2):382-389. [71] DERANLOT J, HERISSON O, NOURISSAT G, et al. Arthroscopic subacromial spacer implantation in patients with massive irreparable rotator cuff tears: clinical and radiographic results of 39 retrospectives cases. Arthroscopy. 2017;33(9):1639-1644. [72] SENEKOVIC V, POBERAJ B, KOVACIC L, et al. The biodegradable spacer as a novel treatment modality for massive rotator cuff tears: a prospective study with 5-year follow-up. Arch Orthop Trauma Surg.2017;137(1):95-103. [73] YALLAPRAGADA RK, APOSTOLOPOULOS A, KATSOUGRAKIS I, et al. The use of a subacromial spacer-inspace balloon in managing patients with irreparable rotator cuff tears. J Orthop. 2018;15(3):862-868. [74] RUIZ IM, LORENTE MR, RUIZ DR, et al. The absorbable subacromial spacer for irreparable posterosuperior cuff tears has inconsistent results. Knee Surg Sports Traumatol Arthrosc. 2018; 26(12):3848-3854. [75] AHMAD Z, HENSON F, WARDALE J, et al. Review article: Regenerative techniques for repair of rotator cuff tears. J Orthop Surg (Hong Kong). 2013;21(2):226-231. [76] LIU F, MENG Q, YIN H, et al. Stem Cells in Rotator Cuff Injuries and Reconstructions: A Systematic Review and Meta-Analysis. Curr Stem Cell Res Ther. 2019;14(8):683-697. [77] CENTENO C J, AL-SAYEGH H, BASHIR J, et al. A prospective multi-site registry study of a specific protocol of autologous bone marrow concentrate for the treatment of shoulder rotator cuff tears and osteoarthritis. J Pain Res. 2015;8:269-276. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [3] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [4] | Wang Debin, Bi Zhenggang. Related problems in anatomy mechanics, injury characteristics, fixed repair and three-dimensional technology application for olecranon fracture-dislocations [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1446-1451. |
| [5] | Ji Zhixiang, Lan Changgong. Polymorphism of urate transporter in gout and its correlation with gout treatment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1290-1298. |
| [6] | Yuan Mei, Zhang Xinxin, Guo Yisha, Bi Xia. Diagnostic potential of circulating microRNA in vascular cognitive impairment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1299-1304. |
| [7] | Wang Xianyao, Guan Yalin, Liu Zhongshan. Strategies for improving the therapeutic efficacy of mesenchymal stem cells in the treatment of nonhealing wounds [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1081-1087. |
| [8] | Wan Ran, Shi Xu, Liu Jingsong, Wang Yansong. Research progress in the treatment of spinal cord injury with mesenchymal stem cell secretome [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1088-1095. |
| [9] | Liao Chengcheng, An Jiaxing, Tan Zhangxue, Wang Qian, Liu Jianguo. Therapeutic target and application prospects of oral squamous cell carcinoma stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1096-1103. |
| [10] | Zhao Min, Feng Liuxiang, Chen Yao, Gu Xia, Wang Pingyi, Li Yimei, Li Wenhua. Exosomes as a disease marker under hypoxic conditions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1104-1108. |
| [11] | Xie Wenjia, Xia Tianjiao, Zhou Qingyun, Liu Yujia, Gu Xiaoping. Role of microglia-mediated neuronal injury in neurodegenerative diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1109-1115. |
| [12] | Li Shanshan, Guo Xiaoxiao, You Ran, Yang Xiufen, Zhao Lu, Chen Xi, Wang Yanling. Photoreceptor cell replacement therapy for retinal degeneration diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1116-1121. |
| [13] | Jiao Hui, Zhang Yining, Song Yuqing, Lin Yu, Wang Xiuli. Advances in research and application of breast cancer organoids [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1122-1128. |
| [14] | Wang Shiqi, Zhang Jinsheng. Effects of Chinese medicine on proliferation, differentiation and aging of bone marrow mesenchymal stem cells regulating ischemia-hypoxia microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1129-1134. |
| [15] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||