Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (36): 5879-5884.doi: 10.3969/j.issn.2095-4344.2014.36.024
Previous Articles Next Articles
Experimental animal models of osteonecrosis of the femoral head: classification and experimental applications
Wang Yan-mao, Zhang Chang-qing
- Department of Orthopedics, Sixth People’s Hospital, Shanghai Jiao Tong University, Shanghai 200233, China
-
Revised:2014-07-06Online:2014-08-30Published:2014-08-30 -
Contact:Zhang Chang-qing, M.D., Doctoral supervisor, Chief physician, Department of Orthopedics, Sixth People’s Hospital, Shanghai Jiao Tong University, Shanghai 200233, China -
About author:Wang Yan-mao, Studying for master’s degree, Department of Orthopedics, Sixth People’s Hospital, Shanghai Jiao Tong University, Shanghai 200233, China
CLC Number:
Cite this article
Wang Yan-mao, Zhang Chang-qing. Experimental animal models of osteonecrosis of the femoral head: classification and experimental applications[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(36): 5879-5884.
share this article
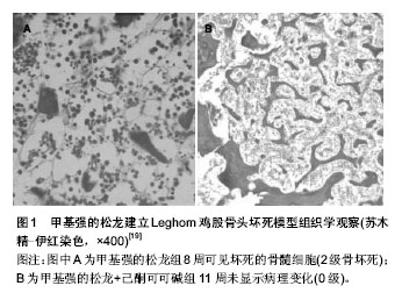
2.1 创伤性股骨头坏死模型 临床上,股骨颈骨折所造成的股骨头缺血是股骨头坏死发病的重要原因之一,对实验动物进行手术,例如结扎股骨颈、切除股骨头圆韧带等,从而阻断股骨头血供模拟临床上的发病过程是创伤性股骨头坏死模型的主要方法。 小猪模型是一个经常被用作骨坏死研究的动物模型。Zhang等[4]发现在未成熟小猪的解剖结构中,股骨干和近端骨骺间没有血管交通支,为结扎股骨颈造成股骨头缺血坏死提供了理论基础。Aruwajoye等[5]通过在股骨颈部紧密结扎并切断圆韧带的方法在8只五六周大的Yorkshire小猪单侧未成熟的股骨头上建模,而另一侧作为对照组。术后2周,对其中3只的坏死股骨头进行苏木精-伊红染色和TUNEL标记法,另外5只进行结合定量散射电子显像、纳米压痕技术、微裂纹评估进行检测;组织学结果显示在骨小梁及骨髓区分布有大量的坏死细胞,纳米压痕技术软骨下区微裂纹的密度显著增加。此模型是研究LCPD的经典模型,可用于发病机制及防治措施的探索。Shapiro等[6]用同样的方法成功地构造了小猪股骨头坏死模型,并且证实了坏死的股骨头会继发性地引起相邻髋臼的畸形,同时为髋臼发育畸形这类至今了解甚少的疾病提供了研究模型。而Kim等[7]在上述方法造模的同时,对小猪的一侧后肢进行截肢以避免负重,结果发现局部的避免负重可以减少坏死股骨头的畸形,并促进血管的再生及骨骺中血栓的吸收,对临床的治疗有一定的参考意义。 有学者用3个月大的新西兰兔造模[8],手术切除髋关节囊,完全分离环状韧带及软组织,切断股骨颈基底部,用不可吸收线将分离的股骨头固定在髋臼上以模拟股骨头坏死早期临床阶段,通过CT、MRI及组织学方法发现骺板两侧有坏死斑的分布,而软骨保存,这与人类早期股骨头坏死相似。Hofstaetter等[9]使用成年的新西兰兔建造股骨头坏死,实验者同时破坏了股骨头的髓内供血及髓外供血:髓内向股骨颈钻孔到达髓腔,髓外环形损伤股骨颈的骨膜的同时结扎圆韧带。术后使用影像学及组织学的方法进行评价,6个月未发现股骨头塌陷,12个月只有13.3%的动物出现了股骨头塌陷,并且只有软骨下骨的骨折,股骨头大体形态并没有显著改变,12个月的造模周期也比较难以接受。 范猛等[10]用手术方式将SD大鼠的髋关节脱位,切断圆韧带,并破坏股骨颈近端骨膜上的血供,通过影像学及多个组织学方法证实了股骨头出现塌陷,骨小梁结构改变,破骨细胞明显活跃,成功建造了大鼠创伤性股骨头坏死模型。Gao等[11]通过低速钻头对狗的股骨颈造成Garden IV型骨折,从术后2个月的X射片上观察到未经治疗的股骨颈骨折造成了典型的股骨头坏死。Hang等[12]使用手术方式对狗造成股骨颈骨折及髋关节脱位,并通过3枚克氏针进行内固定的方式建立了股骨头坏死的动物模型。术后4周X射线显示骨折愈合,骨密度均匀,未出现硬化带及新月征或者塌陷;但苏木精-伊红染色显示有坏死骨小梁并伴微结构的改变。这种方法模拟了临床上常见的股骨颈骨折手术后出现股骨头坏死的过程,曾有学者做过类似研究,但结果不一,重复性较差。 创伤性股骨头坏死动物模型在LCPD的造模上具有重要作用,但对于成人的股骨头坏死,其造模操作复杂、周期长、重复性差、成功率低等缺点较为明显,并不是理想的股骨头坏死模型。 2.2 激素性股骨头坏死的模型 当今,许多疾病,例如系统性红斑狼疮、肾病综合征、支气管哮喘等都需要长期大量的服用激素进行治疗,但其带来的并发症如股骨头坏死等同样是显而易见的。Tong等[13]通过基因芯片技术发现激素性股骨头坏死小鼠有多种基因的表达发生了显著变化,这些改变的基因包括:血管形成基因、凋亡基因、信号转导基因、氧化应激相关基因等类型,因此可以得出结论是有多种基因参与到了激素性股骨头坏死形成的过程中。 2.2.1 单纯激素性股骨头坏死模型 大剂量及长时间使用糖皮质激素是引起股骨头坏死的一个高危因素,因此国内外有学者给予兔注射甲基强的松龙建模。Yamaguchi等[14]对30只日本白兔单次肌肉注射20 mg/kg的甲强龙,注射后3周发现股骨及肱骨干骺端有73.3%的兔发生了骨坏死,动物死亡率为0%;Iwakiri等[15]运用相同的方法通过影像学及组织学方法发现有83%的股骨头坏死率。而Kuribayashi等[16]则表示4周股骨头坏死率为70%,但动物死亡率为20%。在兔的激素性骨坏死模型中,骨坏死的病灶还会出现在肱骨近端等其余长骨处,不仅仅局限于股骨头,而其股骨头坏死多为早期表现,这些兔的模型均不是理想的股骨头坏死实验动物模型,但可以为股骨头坏死的发病机制研究作为参考。 Nozaki等[17]对自发性高血压脑卒中大鼠运用甲基强的松龙皮下注射(1 000 mg/60 kg类似于人类激素冲击疗法的剂量),组织学检测股骨头坏死的发生率要显著大于对照组(P < 0.001)。Tian等[18]对SD大鼠连续8周注射甲基强的松龙(20 mg/kg, 1次/周),也成功构建了大鼠的股骨头坏死模型,并证实了激素引导的股骨头坏死模型中,Toll样受体4信号通路(TLR4 signaling pathway)干扰了正常的免疫反应,从而进一步说明了免疫反应的破坏在股骨头坏死中扮演了重要的角色。大鼠有90%的基因与人类一致,喂养时占地面积小,较为经济,而且从解剖学上看来,大鼠的股骨头也同样具有颈干角和前倾角,在生物力学方面与人类相似。但大鼠的股骨头坏死激素模型也有着其局限性:造模周期较长,股骨头形态较难形成塌陷等等。 Erken等[19]通过对25只Leghorn鸡每周肌肉注射 3 mg/kg甲基强的松龙建立了的股骨头坏死模型,造模的14周过程中有48%的动物死亡,组织学发现了软骨下骨小梁的破坏,但未出现股骨头的塌陷(图1)。鸡与人类同为双足行走动物,股骨头的生物力学相近,这是相较于其他四足行走动物的优势,其股骨头坏死的病理病生过程与人类也相似。但动物死亡率极高,坏死大体表现不典型,基因与人类相差甚远,这些因素造成了鸡作为股骨头坏死模型运用较少的原因。"
| [1] Babis GC, Sakellariou V, Parvizi J. Osteonecrosis of the femoral head. Orthopedics.2011;34(1):39. [2] 郑志辉,王少伟,李伟居,等.保髋治疗股骨头坏死的特异性量表[J].中国组织工程研究,2012,16(35):6570-6577. [3] Gao YS, Zhang CQ. Cytotherapy of osteonecrosis of the femoral head: a mini review. Int Orthop.2010;34(6):779-782. [4] Zhang P, Liang Y, Kim H, et al. Evaluation of a pig femoral head osteonecrosis model. J Orthop Surg Res.2010;5:15-21. [5] Aruwajoye OO, Patel MK, Allen MR,et al. Microcrack density and nanomechanical properties in the subchondral region of the immature piglet femoral head following ischemic osteonecrosis. Bone.2013;52(2):632-639. [6] Shapiro F, Connolly S, Zurakowski D, et al. Acetabular changes associated with avascular necrosis of the femoral head in a piglet model. Bone and Joint Res.2014;3(4):130-138. [7] Kim HK, Aruwajoye O, Stetler J,et al. Effects of Non-Weight-Bearing on the Immature Femoral Head Following Ischemic Osteonecrosis An Experimental Investigation in Immature Pigs. J Bone Joint Surg Am.2012;94A(24):2228-2237. [8] Wen Q, Jin D, Zhou CY, et al. HGF-transgenic MSCs can improve the effects of tissue self-repair in a rabbit model of traumatic osteonecrosis of the femoral head. PloS one.2012;7(5):e37503. [9] Hofstaetter JG, Wang J, Yan J, et al.The effects of alendronate in the treatment of experimental osteonecrosis of the hip in adult rabbits. Osteoarthritis Cartilage. 2009;17(3):362-370. [10] 范猛,姜文学,汪爱媛,等. NEL样1型基因联合唑来膦酸预防股骨头坏死塌陷作用的初步观察[J].中国医学科学院学报,2013, 35(5): 553-560. [11] Gao YS, Zhu ZH, Chen SB,et al.Injury-to-surgery interval does not affect the occurrence of osteonecrosis of the femoral head: A prospective study in a canine model of femoral neck fractures. Medical Science Monitor.2012;18(7):BR259-BR64. [12] Hang D, Wang Q, Guo C, et al. Treatment of osteonecrosis of the femoral head with VEGF165 transgenic bone marrow mesenchymal stem cells in mongrel dogs. Cells Tissues Organs.2011;195(6):495-506. [13] Tong P, Wu C, Jin H, et al. Gene Expression Profile of Steroid-induced Necrosis of Femoral Head of Rats. Calcif Tissue Int. 2011;89(4):271-284. [14] Yamaguchi R, Yamamoto T, Motomura G, et al. Effects of an anti-platelet drug on the prevention of steroid-induced osteonecrosis in rabbits. Rheumatology. 2012;51(5):789-793. [15] Iwakiri K, Oda Y, Kaneshiro Y, et al.Effect of simvastatin on steroid-induced osteonecrosis evidenced by the serum lipid level and hepatic cytochrome P4503A in a rabbit model. J Orthop Sci. 2008;13(5):463-468. [16] Kuribayashi M, Fujioka M, Takahashi KA, et al. Vitamin E prevents steroid-induced osteonecrosis in rabbits. Acta orthopaedica.2010;81(1):154-160. [17] Nozaki Y, Kumagai K, Miyata N, et al. Pravastatin reduces steroid-induced osteonecrosis of the femoral head in SHRSP rats. Acta orthopaedica.2012;83(1):87-92. [18] Tian L, Wen Q, Dang X, et al. Immune response associated with Toll-like receptor 4 signaling pathway leads to steroid-induced femoral head osteonecrosis. BMC Musculoskelet Disord. 2014;15:18. [19] Erken HY, Ofluoglu O, Aktas M, et al. Effect of pentoxifylline on histopathological changes in steroid-induced osteonecrosis of femoral head: experimental study in chicken. Int Orthop.2012;36(7):1523-1528. [20] Qin L, Zhang G, Sheng H, et al. Multiple bioimaging modalities in evaluation of an experimental osteonecrosis induced by a combination of lipopolysaccharide and methylprednisolone. Bone.2006;39(4):863-871. [21] Wu X, Yang S, Duan D, et al. Experimental osteonecrosis induced by a combination of low-dose lipopolysaccharide and high-dose methylprednisolone in rabbits. Joint Bone Spine. 2008;75(5):573-578. [22] Wu X, Yang S, Wang H, et al. G-CSF/SCF exert beneficial effects via anti-apoptosis in rabbits with steroid-associated osteonecrosis.Exp Mol Pathol. 2013;94(1):247-254. [23] Zhang YG, Wang X, Yang Z, et al. The therapeutic effect of negative pressure in treating femoral head necrosis in rabbits. PloS one.2013;8(1):e55745. [24] Guan XY, Han D. Role of hypercoagulability in steroid-induced femoral head necrosis in rabbits. J Orthop Sci.2010;15(3):365-370. [25] Ryoo S, Lee S, Jo S,et al.Effect of lipopolysaccharide (LPS) on mouse model of steroid-induced avascular necrosis in the femoral head (ANFH). J Microbiol Biotechnol.2014;24(3):394-400. [26] Zheng LZ, Liu Z, Lei M, et al. Steroid-associated hip joint collapse in bipedal emus. PLoS One.2013;8(10):e76797. [27] Wang W, Liu L, Dang X, et al. The effect of core decompression on local expression of BMP-2, PPAR-γ and bone regeneration in the steroid-induced femoral head osteonecrosis. BMC Musculoskelet Disord. 2012;13:142. [28] Wang L, Luo DK, Pan ZY. Expression of 11 beta-HSD in steroid-induced avascular necrosis of the femoral head. Mol Med Rep.2013;7(5):1482-1486. [29] Zhao G, Yamamoto T, Motomura G, et al. Cholesterol-and lanolin-rich diets may protect against steroid-induced osteonecrosis in rabbits. Acta orthopaedica.2013;84(6):593-597. [30] 李瑞琦,张国平,李宜炯,等.提高激素性股骨头坏死模型成活率的方法[J].中国组织工程研究,2013,50):8729-8734. [31] Okazaki S, Nagoya S, Tateda K. Experimental rat model for alcohol‐induced osteonecrosis of the femoral head. Int J Exp Pathol. 2013;94(5):312-319. [32] Mont MA, Zywiel MG, Marker DR, et al. The Natural History of Untreated Asymptomatic Osteonecrosis of the Femoral HeadA Systematic Literature Review. J Bone Joint Surg Am. 2010;92(12):2165-2170. [33] Ikemura S, Yamamoto T, Motomura G, et al. Lipid metabolism abnormalities in alcohol‐treated rabbits: a morphometric and haematologic study comparing high and low alcohol doses. Int J Exp Pathol. 2011;92(4):290-295. [34] Zhu ZH, Gao YS, Luo SH, et al. An animal model of femoral head osteonecrosis induced by a single injection of absolute alcohol: an experimental study. Med Sci Monit.2011;17(4):R97-R102. [35] Feitosa ML, Fadel L, Beltrão-Braga PC,et al. Successful transplant of mesenchymal stem cells in induced osteonecrosis of the ovine femoral head. Preliminary results. Acta Cir Bras. 2010;25(5):416-422. [36] 陈东,华文彬,叶树楠,等.骨内注射无水乙醇建立兔股骨头坏死模型[J].中国组织工程研究,2013,16(2):205-209. [37] Wang C, Wang J, Zhang Y, et al. A Canine Model of Femoral Head Osteonecrosis Induced by an Ethanol Injection Navigated by a Novel Template. nt J Med Sci.2013;27;10(11):1451-1418. [38] 马坤,顾建平.股骨头坏死动物模型制作方法的研究进展[J].中国介入影像与治疗学,2009,6(3):286-289. [39] Vélez R, Hernández-Fernández A, Caminal M, et al. Treatment of femoral head osteonecrosis with advanced cell therapy in sheep. Arch Orthop Trauma Surg.2012;132(11):1611-1618. [40] Jin H, Xia B, Yu N, et al. The effects of autologous bone marrow mesenchymal stem cell arterial perfusion on vascular repair and angiogenesis in osteonecrosis of the femoral head in dogs. Int Orthop.2012;36(12):2589-2596. [41] 周正丽,张潜,彭笳宸,等.液氮冷冻兔股骨头坏死模型制备新方法及可靠性评价[J].解剖学报,2012,43(2):284-288. [42] Fan M, Peng J, Wang A, et al. Emu model of full-range femoral head osteonecrosis induced focally by an alternating freezing and heating insult. J Int Med Res.2011;39(1):187-198. [43] Goetz JE, Robinson DA, Pedersen DR,et al.Cryoinsult parameter effects on the histologically apparent volume of experimentally induced osteonecrotic lesions. J Orthop Res. 2011;29(6):931-937. [44] Suzuki M, Kumagai K, Osaki M, et al.Osteonecrosis of femoral head in the stroke-prone spontaneously hypertensive rats, especially old rats. Clin Exp Hypertens.2008;30(7):689-697. [45] Gao YS, Wang HF, Ding H, et al. A novel rat model of osteonecrosis of the femoral head induced by periarticular injection of vascular endothelial growth factor receptor 2 antibody. J Surg Res. 2013;183(1):e1-5. [46] Long T, Xu J, McClure SR, et al. Potential Femoral Head Osteonecrosis Model Induced by High-Intensity Focused Ultrasound. Ultrasound Med Biol. 2013;39(6):1056-1065. [47] Sobakin AS, Wilson MA, Lehner CE, et al. Oxygen pre-breathing decreases dysbaric diseases in UW sheep undergoing hyperbaric exposure. Undersea Hyperb Med.2008;35(1):61-67. [48] Li Y, Han R, Geng C,et al. A new osteonecrosis animal model of the femoral head induced by microwave heating and repaired with tissue engineered bone. Int Orthop.2009; 33(2): 573-580. |
| [1] | Han Jie1, Chen Yueping1, Mo Jian1, Wang Dawei1, Su Bo1, Li Shuzhen1, Xia Tian2, Wang Shixin2. Ultrastructural evaluation of a rabbit model of steroid-induced osteonecrosis of the femoral head after treatment with panax notoginseng saponins [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(7): 1035-1039. |
| [2] | Zhai Pei, Li Pengfei, Liang Zhenghui, Zeng Jianchun, Cai Guoxiong, Zeng Yirong, Fan Yueguang. Differential expression of miR-672-5p in rat osteoblasts after intervention by long-acting, intermediate-acting and short-acting hormones [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(5): 809-814. |
| [3] | Hu Liang1, Wang Junhai1, Wang Zhilie1, Xie Jinyuan1, Chen Deng1, Ding Fan2. Vascular endothelial growth factor combined with mutant hypoxia-inducible factor 1alpha promotes angiogenesis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(3): 378-383. |
| [4] | Su Lianbin, Feng Eryou, Zhang Yiyuan, Zhuo Youguang, Xiao Lili, Wang Wulian, Lin Feitai. Whether direct anterior approach for total hip arthroplasty is a risk factor of eccentric reaming to the anterior column of the acetabulum? [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(20): 3117-3123. |
| [5] | Sun Liang1, Liu Wanlin1, Na Risong2, Zhao Zhenqun1. 3-Methyladenine regulating autophagy gene Beclin1 can alleviate the occurrence and development of steroid-induced avascular necrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(15): 2391-2396. |
| [6] | Peng Chenjian, Du Bin, Sun Guangquan, Liu Xin, Xue Peng, Cao Liangquan. Three-dimensional printing beta-tricalcium phosphate scaffold loaded with icariin particles for repairing osteonecrosis of the femoral head in rabbits [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2162-2168. |
| [7] | Zhao Jun, Zhang Xiaofeng, Xu Xilin, Wang Zhengchun, Fang Xiangchun, He Xuefeng, Xie Xinsheng, Zhang Cheng. Treating femoral head necrosis by directed differentiation of bone marrow mesenchymal stem cells: application and evaluation [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(13): 2127-2132. |
| [8] | Li Yunlong, Zhao Zhenqun, Liu Wanlin. Regulation of PI3K/Akt/mTOR signaling pathway on autophagy in steroid-induced avascular necrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(12): 1921-1929. |
| [9] | Feng Li, Wang Jun-yuan, Liu Feng, Cheng Bo. Dynamic simulation of the edge load caused by the separation of the ceramic cup and femoral head [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(7): 985-990. |
| [10] | Zhang Tian-yi, Dong Wei, Mi Pan-pan, Kong Fan-lin, Zhu Jun, Wu Jian-wei, Qiao Jin-huan, Fan Guo-feng, Tian Feng-de. Three-dimensional finite element analysis on stress distribution after greater trochanter bone flap for treating osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(7): 1090-1095. |
| [11] | Yang Li-feng, Xiao Dong-min, Peng Chun-lei, Li Kang-hua, Yang Bin-hui, Liu Feng-hu, Wei Yong-kun, Zhang Bo, Li Wu-jian, Zheng Jin-zhe, Wang Wei-gang. Finite element analysis for self-made femoral head brace device in the treatment of early femoral head necrosis [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(7): 1096-1101. |
| [12] | Zeng Ping1, Lai Chongrong2, Li Jinyi1, Du Mindong1, He Kaiyi1, Sun Bin1, Huang Xiaohua1, Qin Gang1 . Core decompression, autologous iliac bone graft, allogeneic fibular fixation combined with traditional Chinese medicine for treatment of peri-collapse stage osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(36): 5746-5752. |
| [13] | Zhou Xin, Yang Yanfei, Niu Wenjie, Wei Xiaochun, Duan Wangping. Relationship between internal fixation removal and femoral head necrosis after femoral neck fracture in young and middle-aged patients: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(35): 5724-5729. |
| [14] | Fan Siqi, Zeng Ping, Lai Chongrong, Liu Xiong. Association of methylenetetrahydrofolate reductase C677T polymorphism with femoral head necrosis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(35): 5730-5734. |
| [15] | Tong Peng1, Wang Yang2, Liang Ying3. Establishment and comprehensive evaluation of animal models of steroid-induced avascular necrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(32): 5169-5174. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||