Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (34): 5421-5429.doi: 10.12307/2023.804
Previous Articles Next Articles
Repair of rabbit cartilage defects with double-layer bionic scaffold loaded with nerve growth factor cartilage and subchondral bone
Zhou Jie1, Ye Peng1, Zhang Tianxi1, Li Xingyu1, Li Shasha1, Yu Anyong1, Deng Jiang2
- 1Emergency Department of Affiliated Hospital of Zunyi Medical University, Zunyi 563003, Guizhou Province, China; 2Department of Orthopedics, Zunyi First People’s Hospital, Zunyi 563003, Guizhou Province, China
-
Received:2022-09-17Accepted:2022-10-29Online:2023-12-08Published:2023-04-20 -
Contact:Ye Peng, MD, Associate chief physician, Emergency Department of Affiliated Hospital of Zunyi Medical University, Zunyi 563003, Guizhou Province, China -
About author:Zhou Jie, Master, Emergency Department of Affiliated Hospital of Zunyi Medical University, Zunyi 563003, Guizhou Province, China -
Supported by:National Natural Science Foundation of China (H0606) Regional Science Fund (to DJ); Guizhou Provincial Science and Technology Plan Project, No. [2021]074 (to YP); Zunyi Science and Technology Joint Fund, No. HZ(2020)247 (to YP); Doctoral Initiation Fund of Zunyi Medical University, No. (2018)02 (to YP)
CLC Number:
Cite this article
Zhou Jie, Ye Peng, Zhang Tianxi, Li Xingyu, Li Shasha, Yu Anyong, Deng Jiang. Repair of rabbit cartilage defects with double-layer bionic scaffold loaded with nerve growth factor cartilage and subchondral bone[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(34): 5421-5429.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
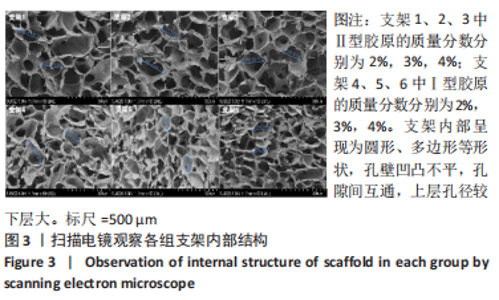
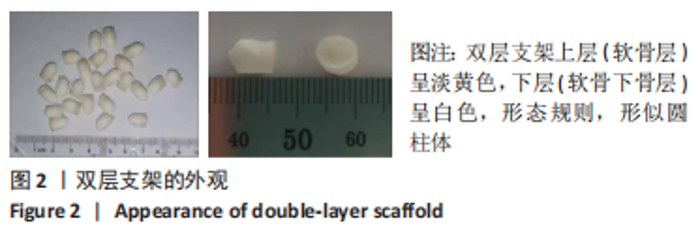
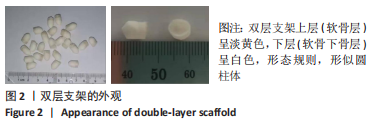
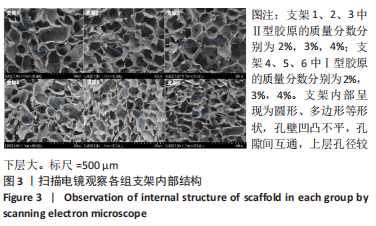
2.1.3 双层支架形态及孔径大小 如图3所示,扫描电镜显示支架内部呈现为圆形、多边形等形状,孔壁凹凸不平,孔隙间互通,上层支架1、2、3的平均孔径分别为(271.31±23.29),(268.31±22.36),(269.14±10.24) μm,各组间对比差异无显著性意义(F=0.063,P=0.939,n=10);下层支架4、5、6的平均孔径分别为(190.24±13.73),(188.45±12.73),(192.57±8.35) μm,各组间对比差异无显著性意义(F=0.274,P=0.761,n=10)。上层支架整体平均孔径为(269.08±20.49) μm,下层支架整体平均孔径为(190.42±11.96) μm,上层孔径较下层更大(P < 0.05)。"
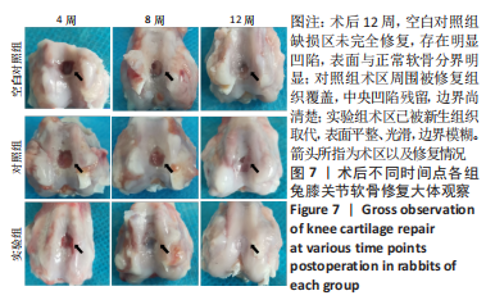
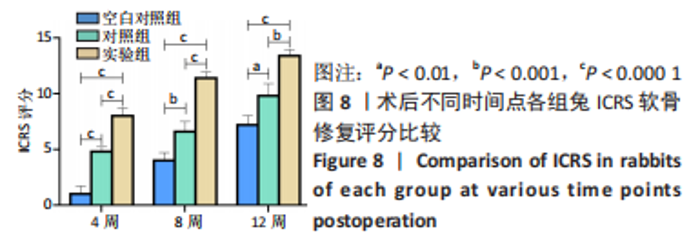
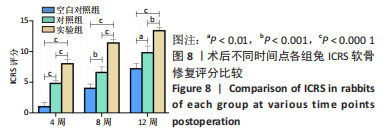
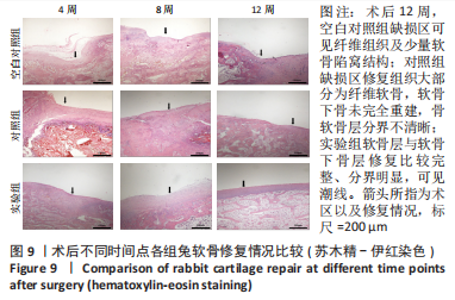
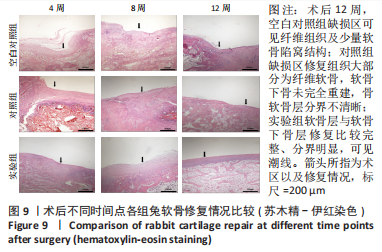
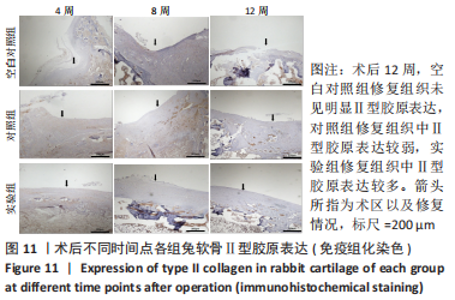
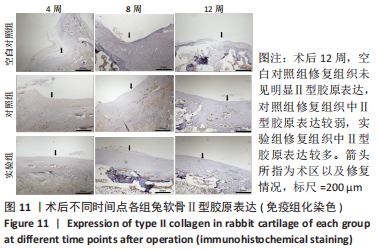
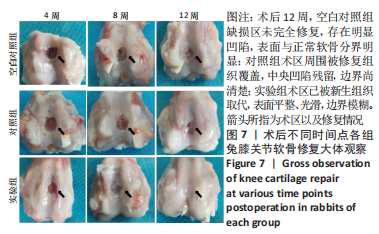
2.3 双层支架兔软骨缺损修复效果 2.3.1 实验动物数量分析 30只新西兰大白兔均存活,术后第1-3天术区及关节肿胀,活动以及饮食欠佳;术后1周术区及关节处肿胀明显消退,活动较前明显好转。30只兔全部进入结果分析。 2.3.2 软骨大体学观察及ICRS软骨修复评分 关节软骨大体学观察(图7):术后标本提取时发现,空白对照组关节少许粘连,滑囊呈现轻度充血水肿,其余两组动物关节及滑囊正常,没有明显滑膜炎症、骨赘形成。空白对照组术后4,8,12周缺损区未完全修复,存在明显凹陷,表面与正常软骨分界明显。对照组术后4周见术区凹陷明显;术后8周时术区被部分的组织覆盖,凹陷区域变平;术后12周时术区周围被修复组织覆盖,中央凹陷残留,边界尚清楚。实验组术后4周尚可见缺损区凹陷轮廓;术后8周时术区被修复组织填充,凹陷区域明显变平;术后12周时术区已被新生组织取代,表面平整、光滑,边界模糊。"
| [1] BEATA Ż, ALEKSANDRA SR, URSZULA L, et al. Structure and Pathologies of Articular Cartilage. In Vivo. 2021;35:1355-1363. [2] ABHIJIT MB, JAMES BR. Articular cartilage: structure, injuries and review of management. Br Med Bull. 2008;87:77-95. [3] JOSÉ B, JOSÉ AA, ENRIQUE G, et al. Articular cartilage: structure and regeneration. Tissue Eng Part B Rev. 2010;16:617-627. [4] MATTHEW JK, JOHN WB, JUSTIN MP, et al. Microfracture Versus Autologous Chondrocyte Implantation for Articular Cartilage Lesions in the Knee: A Systematic Review of 5-Year Outcomes. Am J Sports Med. 2018;46:995-999. [5] REISSIS D, TANG QO, COOPER NC, et al. Current clinical evidence for the use of mesenchymal stem cells in articular cartilage repair. Expert Opin Biol Ther. 2016; 16(4):535-557. [6] XIN L, ZHANG C, XU WX, et al. Current advances on surgical treatment for knee articular cartilage injuries. Zhongguo Gu Shang. 2018;31:281-285. [7] HÖNLE W, JEZUSSEK D, FABIJANI R, et al. Surgical treatment of knee osteoarthritis. MMW Fortschr Med. 2007;149:33-34,36. [8] CHASE SD, JORGE C, CRUZ RS, et al. Fresh Osteochondral Allograft Transplantation for Treatment of Articular Cartilage Defects of the Knee. Arthrosc Tech. 2016;5: e157-161. [9] EREN Y, ALI E, EMRE Y, et al. The Effect of Intraarticular Insulin on Chondral Defect Repair. Cartilage. 2021;13:684S-691S. [10] RIMTAUTAS G, AGNE G, ARNOLDAS P, et al. Ten-year follow-up of a prospective, randomized clinical study of mosaic osteochondral autologous transplantation versus microfracture for the treatment of osteochondral defects in the knee joint of athletes. Am J Sports Med. 2012;40:2499-2508. [11] SAHAR J, SADRABADI AMIN E, FATEMEH Z, et al. New Insights into Cartilage Tissue Engineering: Improvement of Tissue-Scaffold Integration to Enhance Cartilage Regeneration. Biomed Res Int. 2022;2022:7638245. [12] 杨东翔,元香南,孔战,等.组织工程软骨的研究现状与进展[J].山东医药, 2011,51(40):113-114. [13] HOLZAPFEL BM, RUDERT M, HUTMACHER DW. Scaffold-based Bone Tissue Engineering. Orthopade. 2017;46:701-710. [14] ABIY W, ELENI KT, CAGRI A, et al. Current state of fabrication technologies and materials for bone tissue engineering. Acta Biomater. 2018;80:1-30. [15] 张佼佼,王冬青,王志强,等.组织工程软骨支架材料的应用选择[J].中国组织工程研究与临床康复,2011,15(29):5467-5470. [16] XIAO HL, HUANG WL, XIONG K, et al. Osteochondral repair using scaffolds with gradient pore sizes constructed with silk fibroin, chitosan, and nano-hydroxyapatite. Int J Nanomedicine. 2019;14:2011-2027. [17] LU ZH, LEI DQ, JIANG TM, et al. Nerve growth factor from Chinese cobra venom stimulates chondrogenic differentiation of mesenchymal stem cells. Cell Death Dis. 2017;8:e2801. [18] ZHAN XT, CAI PA, LEI DQ, et al. Comparative profiling of chondrogenic differentiation of mesenchymal stem cells (MSCs) driven by two different growth factors. Cell Biochem Funct. 2019;37:359-367. [19] JI L, SONG ZW, ZENG FH, et al. Research progress on controlled release of various growth factors in bone regeneration. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2019;33:750-755. [20] CHEN ZJ, CHENG Q, YU XF, et al. Research progress of growth factor sustained -release microspheres in fat transplantation. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2017;31:1402-1406. [21] 王富友.组织工程骨软骨仿生设计与初步构建[D].重庆:第三军医大学,2008. [22] LEVINGSTONE TJ, THOMPSON E, MATSIKO A, et al. Multi-layered collagenbased scaffolds for osteochondral defect repair in rabbits. Acta Biomater. 2016;32:149-160. [23] LEVINGSTONE TJ, MATSIKO A, DICKSON GR, et al. A biomimetic multilayered collagen-based scaffold for osteochondral repair. Acta Biomater. 2014;10:1996-2004. [24] FU LW, YANG Z, GAO CJ, et al. Advances and prospects in biomimetic multilayered scaffolds for articular cartilage regeneration. Regen Biomater. 2020;7:527-542. [25] 康嘉宇,吕建伟,赵志虎,等.骨软骨组织工程分层支架的研究进展[J].中华骨科杂志,2019,39(22):1413-1420. [26] PEREIRA DR, RUI L REIS RL, OLIVEIRA JM. Layered Scaffolds for Osteochondral Tissue Engineering. Adv Exp Med Biol. 2018;1058:193-218. [27] IVANA G, GORDAN VN.Challenges in engineering osteochondral tissue grafts with hierarchical structures. Expert Opin Biol Ther. 2015;15:1583-1599. [28] 朱浩方,毛宏理,顾忠伟.医用组织粘合剂的研究进展[J].中国材料进展,2020, 39(Z1):535-550+557-558. [29] KAZUNORI S, YU M, CHRISTOPHER DM, et al. Osteochondral tissue engineering with biphasic scaffold: current strategies and techniques. Tissue Eng Part B Rev. 2014; 20:468-476. [30] PROMITA B, BANANI K, DEBOKI N, et al. Silk scaffolds in bone tissue engineering: An overview. Acta Biomater. 2017;63:1-17. [31] WALTER B, WEERASAK S, ARAMWIT P, et al. Natural Origin Materials for Osteochondral Tissue Engineering. Adv Exp Med Biol. 2018;1058:3-30. [32] MIRIAM F, GORDIAN B, MANSOOR C, et al. Natural Polymeric Scaffolds in Bone Regeneration. Front Bioeng Biotechnol. 2020;8:474. [33] JOANNE R, JOHN R, KEVIN MS, et al. Biomaterials and scaffold design: key to tissue-engineering cartilage. Biotechnol Appl Biochem. 2007;46:73-84. [34] DEL BAKHSHAYESH AR, ASADI N, ALIHEMMATI A, et al. An overview of advanced biocompatible and biomimetic materials for creation of replacement structures in the musculoskeletal systems: focusing on cartilage tissue engineering. J Biol Eng. 2019;13:85. [35] NAZANIN A, MARZIYEH F, NOROOZI PN, et al. Bioactive polymeric scaffolds for osteogenic repair and bone regenerative medicine. Med Res Rev. 2020;40:1833-1870. [36] MANO JF, REIS RL. Osteochondral defects: present situation and tissue engineering approaches. J Tissue Eng Regen Med. 2007;1:261-273. [37] HUTMACHER DW. Scaffolds in tissue engineering bone and cartilage. Biomaterials. 2000;21:2529-2543. [38] SMITH GD, KNUTSEN G, RICHARDSON JB. A clinical review of cartilage repair techniques. J Bone Joint Surg Br. 2005;87:445-449. [39] TANYA JL, AMOS M, GLENN RD, et al. A biomimetic multi-layered collagen-based scaffold for osteochondral repair. Acta Biomater. 2014;10:1996-2004. [40] MASTROGIACOMO M, MURAGLIA A, KOMLEV V, et al. Tissue engineering of bone: search for a better scaffold. Orthod Craniofac Res. 2005;8:277-284. [41] 高泽,石志良,李锋,等.材料和孔隙率对可降解支架内骨形成的影响[J].医用生物力学,2021,36(4):582-588. [42] LAMINE C, JÉRÔME C, MARION D, et al. Autologous osteochondral mosaicplasty in osteochondritis dissecans of the patella in adolescents. Int Orthop. 2017;41:197-202. [43] AARON JK, HEATHER WH, SCOTT AR, et al. Activity levels are higher after osteochondral autograft transfer mosaicplasty than after microfracture for articular cartilage defects of the knee: a retrospective comparative study. J Bone Joint Surg Am. 2012;94:971-978. [44] MARCUS M, ANDREA B, SYLVIE M, et al. Nasal chondrocyte-based engineered autologous cartilage tissue for repair of articular cartilage defects: an observational first-in-human trial. Lancet. 2016;388:1985-1994. [45] MAURILIO M, ELIZAVETA K, MARCO D, et al. Arthroscopic autologous osteochondral grafting for cartilage defects of the knee: prospective study results at a minimum 7-year follow-up. Am J Sports Med. 2007;35:2014-2021. [46] WIDYASRI P, YOSHIHITO N, SILVIA G, et al. Bone ingrowth of various porous titanium scaffolds produced by a moldless and space holder technique: an in vivo study in rabbits. Biomed Mater. 2016;11:015012. [47] ORTH M, FRITZ T, STUTZ J, et al. Local Application of Mineral-Coated Microparticles Loaded With VEGF and BMP-2 Induces the Healing of Murine Atrophic Non-Unions. Front Bioeng Biotechnol. 2021;9:809397. [48] MIKAËL MM, PRISCILLA SB, KENTA M, et al. Extracellular matrix-inspired growth factor delivery systems for bone regeneration. Adv Drug Deliv Rev. 2015;94:41-52. [49] VALENTINA D, ELISA L, GABRIELA C, et al. Growth factors in bone repair. Chir Organi Mov. 2008;92:161-168. [50] 刘华蔚.壳聚糖导管复合NGF缓释微球修复兔面神经缺损的实验研究[D].北京:中国人民解放军军医进修学院,2011. [51] ZHANG JX, ZHU KJ, CHEN D. Preparation of bovine serum albumin loaded poly (D, L-lactic -co-glycolic acid) microspheres by a modified phase separation technique. J Microencapsul. 2005;22:117-126. [52] KEN Y, KATHY T, SHALLEY AR, et al. Osteochondral repair using an acellular dermal matrix-pilot in vivo study in a rabbit osteochondral defect model. J Orthop Res. 2018;36:1919-1928. [53] TROY DB, ADETOLA BA, NADR MJ, et al. Articular Cartilage Repair with Mesenchymal Stem Cells After Chondrogenic Priming: A Pilot Study. Tissue Eng Part A. 2018;24: 761-774. [54] HUANG Y, FAN HQ, GONG XY, et al. Scaffold With Natural Calcified Cartilage Zone for Osteochondral Defect Repair in Minipigs .Am J Sports Med. 2021;49:1883-1891. [55] IRINA AD M, RAFAEL AVB, HAROLD B, et al. Fixation of Hydrogel Constructs for Cartilage Repair in the Equine Model: A Challenging Issue. Tissue Eng Part C Methods. 2017;23:804-814. [56] FREED LE, GRANDE DA, LINGBIN Z, et al. Joint resurfacing using allograft chondrocytes and synthetic biodegradable polymer scaffolds. J Biomed Mater Res. 1994;28:891-899. [57] ISABEL RD, CARLOS AV, PEDRO PC. Large Animal Models for Osteochondral Regeneration. Adv Exp Med Biol. 2018;1059:441-501. |
| [1] | Sun Kexin, Zeng Jinshi, Li Jia, Jiang Haiyue, Liu Xia. Mechanical stimulation enhances matrix formation of three-dimensional bioprinted cartilage constructs [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(在线): 1-7. |
| [2] | Xu Xingxing, Wen Chaoju, Meng Maohua, Wang Qinying, Chen Jingqiao, Dong Qiang. Carbon nanomaterials in oral implant [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1062-1070. |
| [3] | Yang Yitian, Wang Lu, Yao Wei, Zhao Bin. Application of the interaction between biological scaffolds and macrophages in bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1071-1079. |
| [4] | Li Cheng, Zheng Guoshuang, Kuai Xiandong, Yu Weiting. Alginate scaffold in articular cartilage repair [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1080-1088. |
| [5] | Shi Yehong, Wang Cheng, Chen Shijiu. Early thrombosis and prevention of small-diameter blood vessel prosthesis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1110-1116. |
| [6] | Tang Haotian, Liao Rongdong, Tian Jing. Application and design of piezoelectric materials for bone defect repair [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1117-1125. |
| [7] | Xu Yan, Li Ping, Lai Chunhua, Zhu Peijun, Yang Shuo, Xu Shulan. Piezoelectric materials for vascularized bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1126-1132. |
| [8] | Li Xinyue, Li Xiheng, Mao Tianjiao, Tang Liang, Li Jiang. Three-dimensional culture affects morphology, activity and osteogenic differentiation of human periodontal ligament stem cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 846-852. |
| [9] | Li Xiaoyin, Yang Xiaoqing, Chen Shulian, Li Zhengchao, Wang Ziqi, Song Zhen, Zhu Daren, Chen Xuyi. Collagen/silk fibroin scaffold combined with neural stem cells in the treatment of traumatic spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 890-896. |
| [10] | Yuan Bo, Xie Lide, Fu Xiumei. Schwann cell-derived exosomes promote the repair and regeneration of injured peripheral nerves [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 935-940. |
| [11] | Qin Yuxing, Ren Qiangui, Li Zilong, Quan Jiaxing, Shen Peifeng, Sun Tao, Wang Haoyu. Action mechanism and prospect of bone microvascular endothelial cells for treating femoral head necrosis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 955-961. |
| [12] | Xiong Bohan, Yu Yang, Lu Xiaojun, Wang Xu, Yang Tengyun, Zhang Yaozhang, Liao Xinyu, Zhou Xiaoxiang, He Lu, Li Yanlin. Research progress in promoting tendon to bone healing during anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 779-786. |
| [13] | Zhang Min, Zhang Xiaoming, Liu Tongbin. Application potential of naringin in bone tissue regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 787-792. |
| [14] | Liu Zixuan, Li Yan, Ji Lin, Xia Delin. Biological properties of nano-hydroxyapatite-zinc oxide composite scaffolds and their effects on the behavior of MC3T3-E1 osteoblasts [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(34): 5441-5447. |
| [15] | Teng Jianxiang, Zhu Jisheng, Yuan Daizhu, Wang Zhen, Zhou Yuhu, Tian Xiaobin. Preparation of cartilage decellularized extracellular matrix-loaded composite nanofiber scaffolds based on two-nozzle electrospinning [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(34): 5448-5454. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||