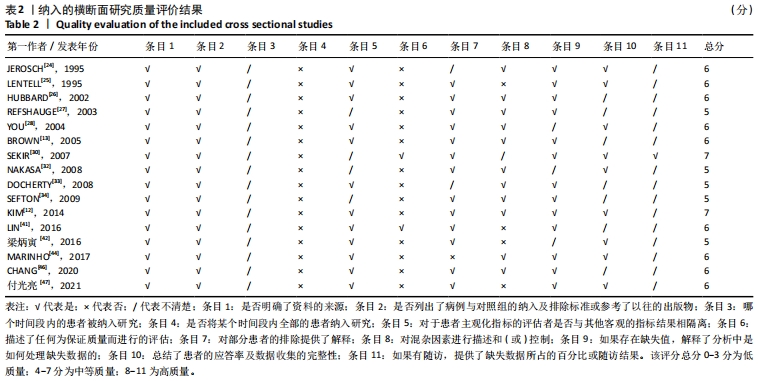
Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (18): 2943-2952.doi: 10.12307/2023.341
Proprioception characteristics of functional ankle instability: a meta-analysis
Wu Yihan1, Wei Qiaoye2, Pang Yu1, Liu Zhongqiang1
- 1School of Physical Education, Southwest Medical University, Luzhou 646000, Sichuan Province, China; 2Department of Rehabilitation Medicine, People’s Hospital of Wulong District of Chongqing, Chongqing 408500, China
-
Received:2022-04-21Accepted:2022-06-13Online:2023-06-28Published:2022-09-19 -
Contact:Liu Zhongqiang, MD, Associate professor, Master’s supervisor, School of Physical Education, Southwest Medical University, Luzhou 646000, Sichuan Province, China -
About author:Wu Yihan, Master candidate, School of Physical Education, Southwest Medical University, Luzhou 646000, Sichuan Province, China -
Supported by:The Joint Funds Project of Luzhou-Southwest Medical University, No. 2015LZCYD-R11(1/7) (to PY); Scientific Research Project of Sichuan Provincial Department of Education in 2018, No. 18SB0811 (to LZQ)
CLC Number:
Cite this article
Wu Yihan, Wei Qiaoye, Pang Yu, Liu Zhongqiang. Proprioception characteristics of functional ankle instability: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(18): 2943-2952.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
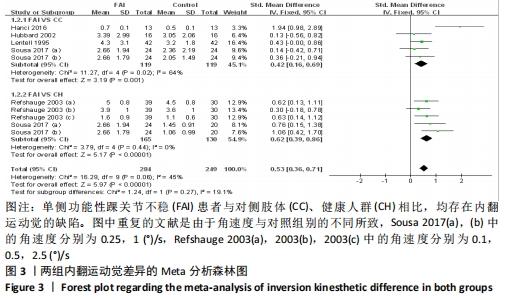
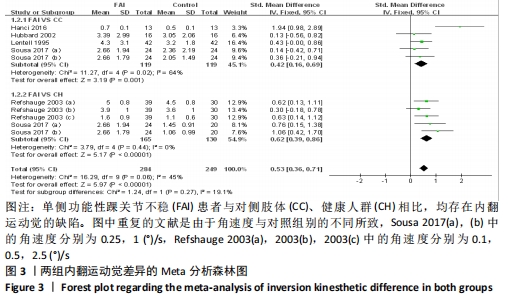
2.4 Meta分析的结果 2.4.1 两组内翻运动觉差异 共纳入5篇文献[24,26-27,39,43]。异质性分析结果显示:I2=45%,P=0.06,纳入研究的异质性较低。采用固定效应模型进行Meta分析结果显示:单侧功能性踝关节不稳患者相较于对照组(对侧肢体、健康人群)存在内翻运动觉缺陷(SMD=0.53,95%CI:0.36-0.71,P < 0.000 01)。按对照来源进行亚组分析显示,单侧功能性踝关节不稳患者与对侧肢体相比存在内翻运动觉缺陷(SMD=0.42,95%CI:0.16-0.69,P=0.001),与健康人群相比存在内翻运动觉缺陷(SMD=0.62,95%CI:0.39-0.86,P < 0.000 01),见图3。"
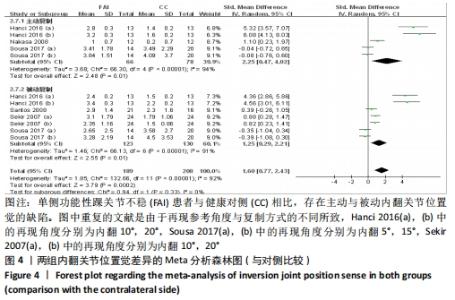
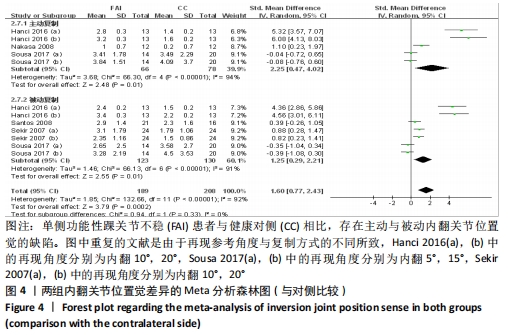
2.4.2 两组关节位置觉差异 功能性踝关节不稳与对侧肢体比较:共5篇观察踝关节内翻的文献[30-32,39,43],异质性分析结果显示:I2=92%,P < 0.000 01,纳入研究的异质性较大,进行敏感性分析调查异质性来源,当剔除HANCI等[39]后汇总的异质性显示,I2=64%,P < 0.000 7,这提示HANCI等[39]可能是较大异质性的来源。采用随机效应模型进行Meta分析结果显示:单侧功能性踝关节不稳患者相比于对侧肢体存在内翻关节位置觉(主动与被动复制)的缺陷(SMD=1.60,95%CI:0.77-2.43,P=0.000 2)。按主被动复制进行亚组分析显示,主动复制条件下,单侧功能性踝关节不稳患者相比于对侧肢体存在内翻关节位置觉的缺陷(SMD=2.25,95%CI:0.47-4.02,P=0.01),被动复制条件下,单侧功能性踝关节不稳患者相比于对侧肢体存在内翻关节位置觉的缺陷(SMD=1.25,95%CI:0.29-2.21,P=0.01),见图4。"
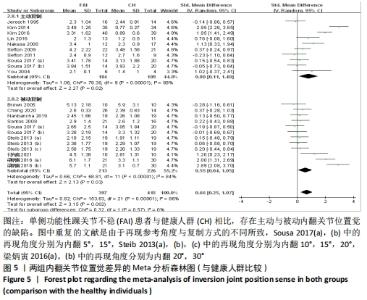
共纳入16篇观察踝关节内翻的文献[12-13,24,28,31-32,34-35,37,40-43,45-47]。异质性分析结果显示:I2=86%,P < 0.000 01,纳入研究的异质性较大,进行敏感性分析调查异质性来源,当剔除梁炳寅等[42]文献后被动内翻复制的异质性显示,I2=0%,P=0.17,这提示梁炳寅等[42]文献可能是被动内翻位置觉较大异质性的来源。采用随机效应模型进行Meta分析结果显示:单侧功能性踝关节不稳患者相比于健康人群存在内翻关节位置觉的缺陷(SMD=0.66,95%CI:0.25-1.07,P=0.002)。按主被动进行亚组分析显示,主动复制条件下,单侧功能性踝关节不稳患者相比于健康人群存在内翻关节位置觉的缺陷(SMD=0.80,95%CI:0.11-1.48,P=0.02),被动复制条件下,单侧功能性踝关节不稳患者相比于健康人群存在内翻关节位置觉的缺陷(SMD=0.55,95%CI:0.04-1.05,P=0.03),见图5。 "
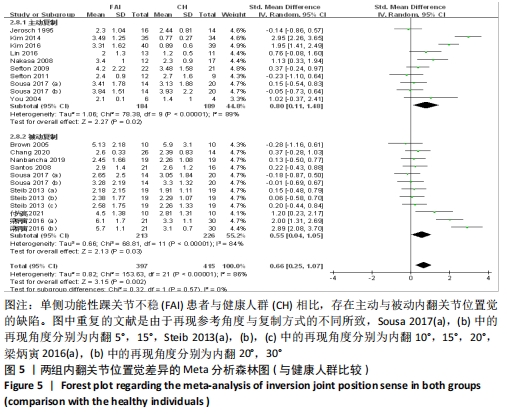
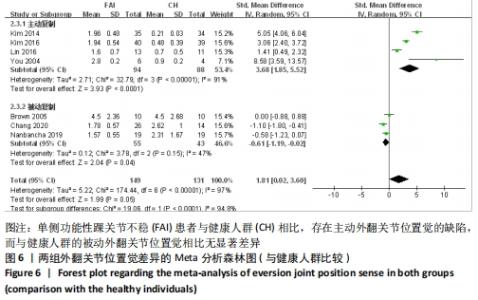
共纳入有7篇文献观察了踝关节外翻[12-13,28,40-41,45-46]。异质性分析结果显示:I2=97%,P < 0.000 01,纳入研究的异质性较大,进行主被动亚组分析显示主动外翻位置觉可能是较大异质性的来源(I2=91%,P < 0.000 01)。采用随机效应模型进行Meta分析结果显示:单侧功能性踝关节不稳患者与健康人群相比不存在外翻关节位置觉的差异(SMD=1.81,95%CI:0.02-3.60,P=0.05)。按主被动进行亚组分析显示,主动复制条件下,单侧功能性踝关节不稳患者与健康人群相比存在外翻关节位置觉缺陷(SMD=3.68,95%CI:1.85-5.52,P < 0.000 1),被动复制条件下,健康人群相比于单侧功能性踝关节不稳患者存在外翻关节位置觉缺陷(SMD=-0.61,95%CI:-1.19至-0.02,P=0.04),见图6。 "
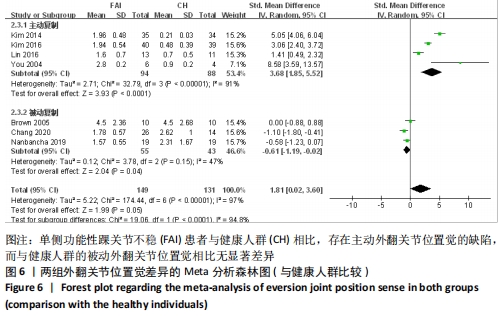
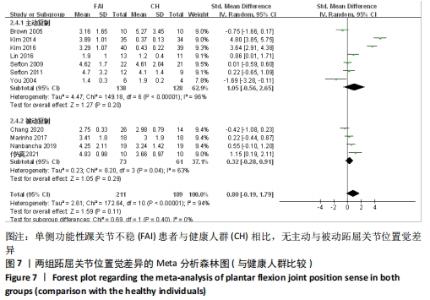
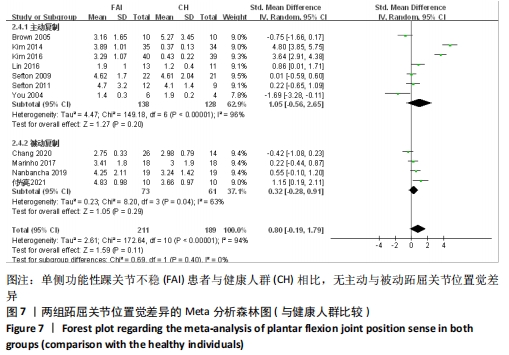
共纳入11篇文献观察了踝关节跖屈[12-13,28,34-35,40-41,44-47]。异质性分析结果显示:I2=94%,P < 0.000 01,纳入研究的异质性较大,进行敏感性分析调查异质性来源,当剔除后CHANG等[46]被动跖屈复制的异质性显示,I2=19%,P=0.29,这提示CHANG等[46]可能是被动跖屈位置觉较大异质性的来源。采用随机效应模型进行Meta分析结果显示:单侧功能性踝关节不稳患者与健康人群相比不存在跖屈关节位置觉的差异(SMD=0.80,95%CI:-0.19-1.79,P=0.11)。按主被动进行亚组分析显示,主动复制条件下,单侧功能性踝关节不稳患者与健康人群相比不存在跖屈关节位置觉的差异(SMD=1.05,95%CI:-0.56-2.65,P=0.20),被动复制条件下,单侧功能性踝关节不稳患者与健康人群相比不存在跖屈关节位置觉的差异(SMD=0.32,95%CI:-0.28-0.91,P=0.29),见图7。 "
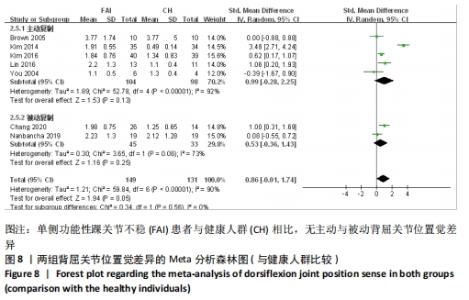
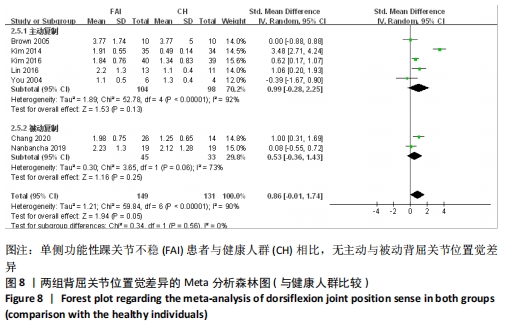
共纳入7篇文献观察了踝关节背屈[12-13,28,40-41,45-46]。异质性分析结果显示,I2=90%,P < 0.000 01,纳入研究的异质性较大,进行敏感性分析调查异质性来源,当剔除后KIM等[12]主动背屈复制的异质性显示,I2=40%,P=0.17,这提示KIM等[12]可能是主动复制较大异质性的来源。采用随机效应模型进行Meta分析结果显示:单侧功能性踝关节不稳患者与健康人群相比不存在背屈关节位置觉差异(SMD=0.86,95%CI:-0.01-1.74,P=0.05)。按主被动进行亚组分析显示,主动复制条件下,单侧功能性踝关节不稳患者与健康人群相比不存在背屈关节位置觉差异(SMD=0.99,95%CI:-0.28-2.25,P=0.13),被动复制条件下,单侧功能性踝关节不稳患者与健康人群相比不存在背屈关节位置觉差异(SMD=0.53,95%CI:-0.36-1.443,P=0.25),见图8。 "
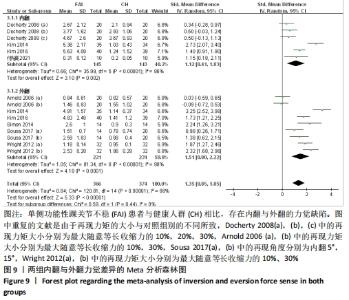
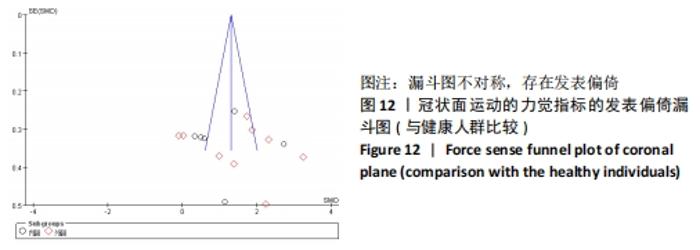
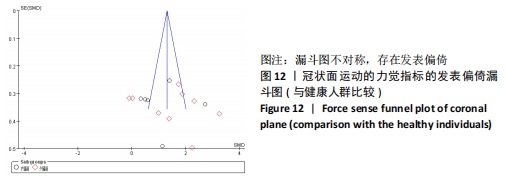
2.4.3 两组力觉差异 共纳入8篇文献观察了力觉[12,29,33,36,38,40,43,47]。异质性分析结果显示:I2=88%,P < 0.000 01,纳入研究的异质性较大,进行敏感性分析调查异质性来源,当剔除KIM等[12]后外翻力觉的异质性显示,I2=46%,P=0.10,这提示KIM等[12]可能是外翻力觉较大异质性的来源。采用随机效应模型Meta分析结果显示:单侧功能性踝关节不稳患者相比于健康人群存在冠状面运动的力觉缺陷(SMD=1.35,95%CI:0.85-1.85,P < 0.000 01)。按内外翻进行亚组分析显示,在内翻方向,单侧功能性踝关节不稳患者相比于健康人群存在力觉缺陷(SMD=1.12,95%CI:0.41-1.83,P=0.002),在外翻方向,单侧功能性踝关节不稳患者相比于健康人群存在力觉缺陷(SMD=1.51,95%CI:0.80-2.22,P < 0.000 1),见图9。"

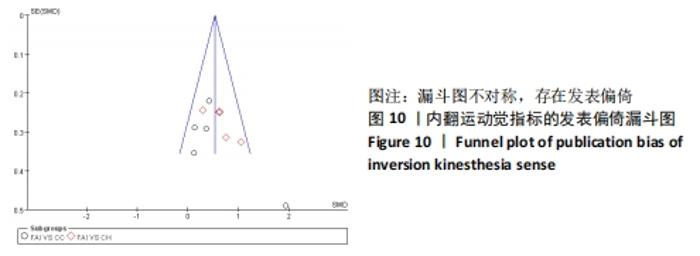
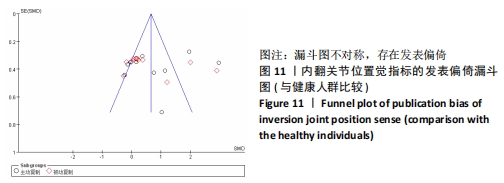
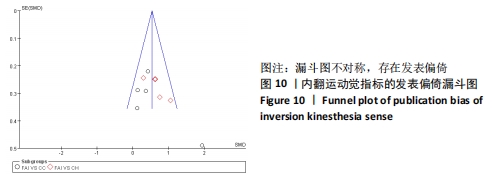
2.5 敏感性分析结果 对每篇纳入的文献进行逐一剔除,再将剩余文献的效应量进行合并。敏感性分析结果显示,在内翻关节位置觉的Meta分析中,当剔除KIM等[12]后效应量由(SMD=0.86,95%CI:-0.01-1.74,P=0.05)变为(SMD=0.48,95%CI:0.09-0.88,P=0.02),当剔除YOU等[28]后效应量由(SMD=0.86,95%CI:-0.01-1.74,P=0.05)变为(SMD=1.04,95%CI:0.10-1.97,P=0.03),其余文献剔除后均未见明显改变。 2.6 发表偏倚分析 根据《Cochrane 干预措施系统评价手册》的建议,当纳入的研究过少时,漏斗图无法真实反映可能存在的发表偏倚,因此文章仅将内翻运动觉、内翻关节位置觉(与健康人群比较)、冠状面运动的力觉进行偏倚漏斗图分析。结果显示,在内翻运动觉方面,通过观察发现有1篇文献存在较大的偏倚风险[39],剔除后所有研究均分布于漏斗图内,分析发现相比于其他研究,文献HANCI等[39]中的角速度较慢,仅为0.1 (°)/s,因此测试出最小运动检测阈值也较小,可能因角速度的不同而产生发表偏倚,见图10。"
| [1] MIKLOVIC TM, DONOVAN L, PROTZUK OA, et al. Acute lateral ankle sprain to chronic ankle instability: a pathway of dysfunction. Phys Sports Med. 2018;46(1):116-122. [2] FREEMAN MA. Instability of the foot after injuries to the lateral ligament of the ankle. J Bone Joint Surg Br. 1965;47(4): 669-677. [3] FREEMAN MA, DEAN MR, HANHAM IW. The etiology and prevention of functional instability of the foot. J Bone Joint Surg Br. 1965;47(4):678-685. [4] DOHERTY C, BLEAKLEY C, HERTEL J, et al. Recovery from a first-time lateral ankle sprain and the predictors of chronic ankle instability: a prospective cohort analysis. Am J Sports Med. 2016;44(4):995-1003. [5] DOHERTY C, DELAHUNT E, CAULFIELD B, et al. The incidence and prevalence of ankle sprain injury: a systematic review and meta-analysis of prospective epidemiological studies. Sports Med. 2014; 44(1):123-140. [6] HERZOG MM, KERR ZY, MARSHALL SW, et al. Epidemiology of ankle sprains and chronic ankle instability. J Athl Train. 2019; 54(6):603-610. [7] 张秋霞,张林,王国祥,等.功能性不稳踝关节位置觉和肌肉力觉特征[J].中国运动医学杂志,2012,31(1):9-13 [8] ROSS SE, LINENS SW, WRIGHT CJ, et al. Noise-enhanced eversion force sense in ankles with or without functional instability. J Athl Train. 2015;50(8):819-824. [9] LIM EC, TAN MH. Side-to-side difference in joint position sense and kinesthesia in unilateral functional ankle instability. Foot Ankle Int. 2009;30(10):1011-1017. [10] GOBLE DJ. Proprioceptive acuity assessment via joint position matching: from basic science to general practice. Phys Ther. 2010; 90(8):1176-1184. [11) HAGEN M, LEMKE M, LAHNER M. Deficits in subtalar pronation and supination proprioception in subjects with chronic ankle instability. Hum Mov Sci. 2018;57: 324-331. [12] KIM CY, CHOI JD, KIM HD. No correlation between joint position sense and force sense for measuring ankle proprioception in subjects with healthy and functional ankle instability. Clin Biomech (Bristol, Avon). 2014;29(9):977-983. [13] BROWN C, ROSS S, MYNARK R, et al. Assessing functional ankle instability with joint position sense, time to stabilization, and electromyography. J Sport Rehabil. 2004;13(2):122-134. [14] CHO BK, PARK JK. Correlation between joint-position sense, peroneal strength, postural control, and functional performance ability in patients with chronic lateral ankle instability. Foot Ankle Int. 2019;40(8):961-968. [15] ALGHADIR AH, IQBAL ZA, IQBAL A, et al. Effect of chronic ankle sprain on pain, range of motion, proprioception, and balance among athletes. Int J Environ Res Public Health. 2020;17(15):5318. [16] OTZEL DM, HASS CJ, WIKSTROM EA, et al. Motoneuron function does not change following whole-body vibration in individuals with chronic ankle instability. J Sport Rehabil. 2019;28(6):614-622. [17] WITCHALLS J, WADDINGTON G, BLANCH P, et al. Ankle instability effects on joint position sense when stepping across the active movement extent discrimination apparatus. J Athl Train. 2012;47(6):627-634. [18] HILLER CE, NIGHTINGALE EJ, LIN CW, et al. Characteristics of people with recurrent ankle sprains: a systematic review with meta-analysis. Br J Sports Med. 2011;45(8): 660-672. [19] XUE X, CHEN Z, XUAN W, et al. Force sense deficits in chronic ankle instability: a systematic review and meta-analysis. PM R. 2022. doi: 10.1002/pmrj.12833. [20] GRIBBLE PA, DELAHUNT E, BLEAKLEY CM, et al. Selection criteria for patients with chronic ankle instability in controlled research: a position statement of the International Ankle Consortium. J Athl Train. 2014;49(1):121-127. [21] Wells G. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Non-Randomised Studies in Meta-Analyses// Symposium on Systematic Reviews: Beyond the Basics. 2014. [22] ROSTOM A, DUBÉ C, CRANNEY A, et al. Celiac disease. Evid Rep Technol Assess (Summ). 2004;(104):1-6. [23] HIGGINS JP, THOMPSON SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21(11):1539-1558. [24] JEROSCH J, HOFFSTETTER I, BORK H, et al. The influence of orthoses on the proprioception of the ankle joint. Knee Surg Sports Traumatol Arthrosc. 1995; 3(1):39-46. [25] LENTELL G, BAAS B, LOPEZ D, et al. The contributions of proprioceptive deficits, muscle function, and anatomic laxity to functional instability of the ankle. J Orthop Sports Phys Ther. 1995;21(4):206-215. [26] HUBBARD TJ, KAMINSKI TW. Kinesthesia is not affected by functional ankle instability status. J Athl Train. 2002;37(4):481-486. [27] REFSHAUGE KM, KILBREATH SL, RAYMOND J. Deficits in detection of inversion and eversion movements among subjects with recurrent ankle sprains. J Orthop Sports Phys Ther. 2003;33(4):166-176. [28] YOU SH, GRANATA KP, BUNKER LK. Effects of circumferential ankle pressure on ankle proprioception, stiffness, and postural stability: a preliminary investigation. J Orthop Sports Phys Ther. 2004;34(8):449-460. [29] ARNOLD BL, DOCHERTY CL. Low-load eversion force sense, self-reported ankle instability, and frequency of giving way. J Athl Train. 2006;41(3):233-238. [30] SEKIR U, YILDIZ Y, HAZNECI B, et al. Effect of isokinetic training on strength, functionality and proprioception in athletes with functional ankle instability. Knee Surg Sports Traumatol Arthrosc. 2007;15(5):654-664. [31] SANTOS MJ, LIU W. Possible factors related to functional ankle instability. J Orthop Sports Phys Ther. 2008;38(3):150-157. [32] NAKASA T, FUKUHARA K, ADACHI N, et al. The deficit of joint position sense in the chronic unstable ankle as measured by inversion angle replication error. Arch Orthop Trauma Surg. 2008;128(5):445-449. [33] DOCHERTY CL, ARNOLD BL. Force sense deficits in functionally unstable ankles. J Orthop Res. 2008;26(11):1489-1493. [34] SEFTON JM, HICKS-LITTLE CA, HUBBARD TJ, et al. Sensorimotor function as a predictor of chronic ankle instability. Clin Biomech (Bristol, Avon). 2009;24(5):451-458. [35] SEFTON JM, YARAR C, HICKS-LITTLE CA, et al. Six weeks of balance training improves sensorimotor function in individuals with chronic ankle instability. J Orthop Sports Phys Ther. 2011;41(2):81-89. [36] WRIGHT CJ, ARNOLD BL. Fatigue’s effect on eversion force sense in individuals with and without functional ankle instability. J Sport Rehabil. 2012;21(2):127-136. [37] STEIB S, HENTSCHKE C, WELSCH G, et al. Effects of fatiguing treadmill running on sensorimotor control in athletes with and without functional ankle instability. Clin Biomech (Bristol, Avon). 2013;28(7):790-795. [38] SIMON J, GARCIA W, DOCHERTY CL. The effect of kinesio tape on force sense in people with functional ankle instability. Clin J Sport Med. 2014;24(4):289-294. [39] HANCI E, SEKIR U, GUR H, et al. Eccentric training improves ankle evertor and dorsiflexor strength and proprioception in functionally unstable ankles. Am J Phys Med Rehabil. 2016;95(6):448-458. [40] KIM CY, CHOI JD. Comparison between ankle proprioception measurements and postural sway test for evaluating ankle instability in subjects with functional ankle instability. J Back Musculoskelet Rehabil. 2016;29(1): 97-107. [41] LIN CH, CHIANG SL, LU LH, et al. Validity of an ankle joint motion and position sense measurement system and its application in healthy subjects and patients with ankle sprain. Comput Methods Programs Biomed. 2016;131:89-96. [42] 梁炳寅,李坤,王予彬,等.本体感觉功能与慢性踝关节不稳相关性的初步研究[J].中华物理医学与康复杂志,2016, 38(11):850-852. [43] SOUSA ASP, LEITE J, COSTA B, et al. Bilateral proprioceptive evaluation in individuals with unilateral chronic ankle instability. J Athl Train. 2017;52(4):360-367. [44] MARINHO HVR, AMARAL GM, DE SOUZA MOREIRA B, et al. Influence of passive joint stiffness on proprioceptive acuity in individuals with functional instability of the ankle. J Orthop Sports Phys Ther. 2017; 47(12):899-905. [45] NANBANCHA A, TRETRILUXANA J, LIMROONGREUNGRAT W, et al. Decreased supraspinal control and neuromuscular function controlling the ankle joint in athletes with chronic ankle instability. Eur J Appl Physiol. 2019;119(9):2041-2052. [46] CHANG YS, AREFIN MS, YOU YL, et al. Effect of novel remodeled bicycle pedal training on balance performance in athletes with functional ankle instability. Front Bioeng Biotechnol. 2020;8:600187. [47] 付光亮,孟庆华,鲍春雨.功能性踝关节不稳者本体感觉力学差异及平衡训练干预效果[J].应用力学学报,2021,38(6): 2426-2431. [48] GRIBBLE PA, BLEAKLEY CM, CAULFIELD BM, et al. Evidence review for the 2016 International Ankle Consortium consensus statement on the prevalence, impact and long-term consequences of lateral ankle sprains. Br J Sports Med. 2016;50(24):1496-1505. [49] DELAHUNT E, REMUS A. Risk factors for lateral ankle sprains and chronic ankle instability. J Athl Train. 2019;54(6):611-616. [50] ALGHADIR AH, IQBAL ZA, IQBAL A, et al. Effect of chronic ankle sprain on pain, range of motion, proprioception, and balance among athletes. Int J Environ Res Public Health. 2020;17(15):5318. [51] EVANS T, HERTEL J, SEBASTIANELLI W. Bilateral deficits in postural control following lateral ankle sprain. Foot Ankle Int. 2004;25(11):833-839. [52] HERTEL J, BUCKLEY WE, DENEGAR CR. Serial testing of postural control after acute lateral ankle sprain. J Athl Train. 2001;36(4):363-368. [53] PROSKE U, CHEN B. Two senses of human limb position: methods of measurement and roles in proprioception. Exp Brain Res. 2021;239(11):3157-3174. [54] PROSKE U, GANDEVIA SC. The proprioceptive senses: their roles in signaling body shape, body position and movement, and muscle force. Physiol Rev. 2012;92(4):1651-1697. [55] NIESPODZIŃSKI B, KOCHANOWICZ A, MIESZKOWSKI J, et al. Relationship between joint position sense, force sense, and muscle strength and the impact of gymnastic training on proprioception. Biomed Res Int. 2018;2018:5353242. [56] LAKIE M, CAMPBELL KS. Muscle thixotropy-where are we now? J Appl Physiol (1985). 2019;126(6):1790-1799. [57] ABDULKARIM Z, EHRSSON HH. Recalibration of hand position sense during unconscious active and passive movement. Exp Brain Res. 2018;236(2):551-561. [58] KRÖGER S. Proprioception 2.0: novel functions for muscle spindles. Curr Opin Neurol. 2018;31(5):592-598. [59] ASHTON-MILLER JA, WOJTYS EM, HUSTON LJ, et al. Can proprioception really be improved by exercises? Knee Surg Sports Traumatol Arthrosc. 2001;9(3):128-136. [60] PROSKE U, GANDEVIA SC. Kinesthetic Senses. Compr Physiol. 2018;8(3):1157-1183. [61] 张帆,蒋琴华,林榕,等.视觉认知任务介入时踝关节稳定程度对纵跳落地模式影响的研究[J].成都体育学院学报,2020, 46(1):78-85. [62] HAN J, WADDINGTON G, ADAMS R, et al. Assessing proprioception: a critical review of methods. J Sport Health Sci. 2016;5(1): 80-90. |
| [1] | Wang Yanjin, Zhou Yingjie, Chai Xubin, Zhuo Hanjie. Meta-analysis of the efficacy and safety of 3D printed porous titanium alloy fusion cage in anterior cervical discectomy and fusion [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1434-1440. |
| [2] | Jiang Xiaocheng, Shi Lu, Wang Yinbin, Li Qiujiang, Xi Chuangzhen, Ma Zefeng, Cai Lijun. Systematical evaluation of bone fusion rate after interbody fusion in patients with osteoporosis and lumbar degenerative disease treated with teriparatide [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1427-1433. |
| [3] | Du Xueting, Zhang Xiaodong, Chen Yanjun, Wang Mei, Chen Wubiao, Huang Wenhua. Application of compressed sensing technology in two-dimensional magnetic resonance imaging of the ankle joint [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1396-1402. |
| [4] | Guo Tingting, Xie Hong, Xu Guanghua. Finite element analysis of elastic ankle brace performance [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1031-1037. |
| [5] | Li Wenjie, You Aijia, Zhou Junli, Fang Sujuan, Li Chun. Effects of different dressings in the treatment of burn wounds: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1141-1148. |
| [6] | Chen Guanting, Zhang Linqi, Li Qingru. Meta-analysis of the value of exosomal miRNA for the diagnosis of chronic kidney disease [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 970-976. |
| [7] | Yan Le, Zhang Huiping, Dai Lintong. Mesenchymal stem cells for allergic rhinitis: a meta-analysis based on animal experiments [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 977-984. |
| [8] | Feng Liang, Gong Shuhui, Huo Hongfeng. Effect of short-foot training on foot and ankle function in patients with flat feet: Meta-analysis and systematic review [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 799-804. |
| [9] | Pan Weimin, Wang Bing, Han Yabing, Li Ting, Song Jiaqi, Qin Huasheng, Liu Yang. Effects of blood flow restriction training on muscle strength, muscle mass and physical performance in older adults: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 805-812. |
| [10] | Yu He, Zheng Jiafa, Song Xiufeng, Guan Shengyi. Tibiotalocalcaneal arthrodesis with blood supplied fibular flap combined with hollow screw in the treatment of end-stage ankle osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 588-593. |
| [11] | Yu Jiaan, Liu Xinwei, Lian Hongyu, Liu Kexin, Li Zitao. Medial open-wedge tibial osteotomy versus lateral closed-wedge tibial osteotomy for unicompartmental knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 632-639. |
| [12] | Xu Yangyang, He Peiliang, Meng Qingqi, Li Siming. A meta-analysis of the effects of continuous adductor canal block and continuous femoral nerve block on early activity after knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 640-645. |
| [13] | Chai Hao, Yang Deyong, Zhang Lei, Shu Li. 3D printing personalized osteotomy guide technology versus conventional total knee arthroplasty on the accuracy of lower limb force alignment: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 646-654. |
| [14] | You Aijia, Li Wenjie, Zhou Junli, Li Chun. Systematic evaluation of six dressings on wound safety following total hip and knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 486-492. |
| [15] | Zeng Guanglong, Xie Qingxiang, Li Yongcong, Su Boyuan. All-arthroscopic repair of anterior talofibular ligament with suture anchors versus InternalBrace for chronic lateral ankle instability [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(13): 2064-2070. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||