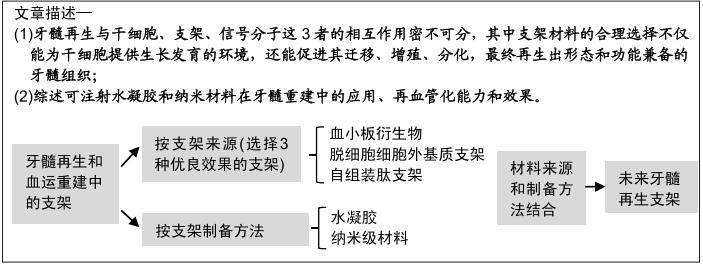
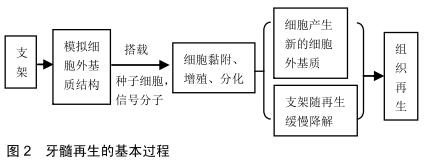
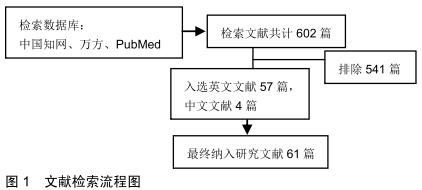
|
[1] WIGLER R, KAUFMAN AY, LIN S, et al. Revascularization: a treatment for permanent teeth with necrotic pulp and incomplete root development.J Endod.2013;39(3):319-326.
[2] YANG J, YUAN G, CHEN Z. Pulp Regeneration: Current Approaches and Future Challenges. Front Physiol. 2016;7: 58.
[3] SOARES DG, ANOVAZZI G, BORDINI E, et al. Biological Analysis of Simvastatin-releasing Chitosan Scaffold as a Cell-free System for Pulp-dentin Regeneration. J Endod. 2018;44(6):971-976.
[4] TETI G, SALVATORE V, FOCAROLI S, et al. In vitro osteogenic and odontogenic differentiation of human dental pulp stem cells seeded on carboxymethyl cellulose-hydroxyapatite hybrid hydrogel. Front Physiol. 2015;6:297.
[5] CHREPA V, AUSTAH O, DIOGENES A. Evaluation of a Commercially Available Hyaluronic Acid Hydrogel (Restylane) as Injectable Scaffold for Dental Pulp Regeneration: An In Vitro Evaluation. J Endod. 2017;43(2):257-262.
[6] ZHANG L, YU Y, FENG K, et al. Templated dentin formation by dental pulp stem cells on banded collagen bundles nucleated on electrospun poly (4-vinyl pyridine) fibers in vitro. Acta Biomater. 2018;76:80-88.
[7] CHEN G, CHEN J, YANG B, et al. Combination of aligned PLGA/Gelatin electrospun sheets, native dental pulp extracellular matrix and treated dentin matrix as substrates for tooth root regeneration. Biomaterials. 2015;52:56-70.
[8] RUANGSAWASDI N, ZEHNDER M, WEBER FE. Fibrin gel improves tissue ingrowth and cell differentiation in human immature premolars implanted in rats. J Endod. 2014;40(2): 246-250.
[9] YANG JW, ZHANG YF, SUN ZY, et al. Dental pulp tissue engineering with bFGF-incorporated silk fibroin scaffolds. J Biomater Appl. 2015;30(2):221-229.
[10] 李龙飚,汪成林,叶玲.天然支架材料在牙髓组织工程再生中的研究进展[J].国际口腔医学杂志,2018,45(6):666-672.
[11] LI Y, HE L, PAN S, et al. Three-dimensional simulated microgravity culture improves the proliferation and odontogenic differentiation of dental pulp stem cell in PLGA scaffolds implanted in mice. Mol Med Rep. 2017;15(2): 873-878.
[12] MOUSSA DG, APARICIO C. Present and future of tissue engineering scaffolds for dentin-pulp complex regeneration. J Tissue Eng Regen Med. 2019;13(1):58-75.
[13] HARKE H, TANGER D, FURST-DENZER S, et al. Effect of a preoperative separation of platelets on the postoperative blood loss subsequent to extracorporeal circulation in open heart surgery (author's transl). Anaesthesist.1977;26(2): 64-71.
[14] WEN J, LI HT, LI SH, et al. Investigation of modified platelet-rich plasma (mPRP) in promoting the proliferation and differentiation of dental pulp stem cells from deciduous teeth. Braz J Med Biol Res. 2016;49(10):e5373.
[15] STAMBOLSKY C, RODRÍGUEZ-BENÍTEZ S, GUTIÉRREZ-PÉREZ JL, et al. Histologic characterization of regenerated tissues after pulp revascularization of immature dog teeth with apical periodontitis using tri-antibiotic paste and platelet-rich plasma. Arch Oral Biol. 2016;71:122-128.
[16] ZHU X, WANG Y, LIU Y, et al. Immunohistochemical and Histochemical Analysis of Newly Formed Tissues in Root Canal Space Transplanted with Dental Pulp Stem Cells Plus Platelet-rich Plasma. J Endod. 2014;40(10):1573-1578.
[17] DOHAN DM, CHOUKROUN J, DISS A, et al. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part I: technological concepts and evolution. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3):e37-e44.
[18] CASTRO AB, MESCHI N, TEMMERMAN A, et al. Regenerative potential of leucocyte- and platelet-rich fibrin. Part A: intra-bony defects, furcation defects and periodontal plastic surgery. A systematic review and meta-analysis. J Clin Periodontol. 2017;44(1):67-82.
[19] HUANG F, YANG S, ZHAO J, et al. Platelet-rich Fibrin Increases Proliferation and Differentiation of Human Dental Pulp Cells. J Endod. 2010;36(10):1628-1632.
[20] WOO S, KIM W, LIM H, et al. Combination of Mineral Trioxide Aggregate and Platelet-rich Fibrin Promotes the Odontoblastic Differentiation and Mineralization of Human Dental Pulp Cells via BMP/Smad Signaling Pathway. J Endod. 2016;42(1):82-88.
[21] KIM JDP, WOO SP, CHOI NDP, et al. Effect of Platelet-rich Fibrin on Odontoblastic Differentiation in Human Dental Pulp Cells Exposed to Lipopolysaccharide. J Endod. 2016;43(3): 433-438.
[22] KESWANI D, PANDEY RK. Revascularization of an immature tooth with a necrotic pulp using platelet-rich fibrin: a case report. Int Endod J. 2013;46(11):1096-1104.
[23] CHEN Y, ZHAO Y, ZHAO Y, et al. Potential dental pulp revascularization and odonto-/osteogenic capacity of a novel transplant combined with dental pulp stem cells and platelet-rich fibrin. Cell Tissue Res. 2015;361(2):439-455.
[24] BAKHTIAR H, ESMAEILI S, FAKHR TABATABAYI S, et al. Second-generation Platelet Concentrate (Platelet-rich Fibrin) as a Scaffold in Regenerative Endodontics: A Case Series. J Endod. 2017;43(3):401-408.
[25] 周延民,付丽.富血小板纤维蛋白在口腔软硬组织再生中的作用—回顾与展望[J].口腔医学, 2018,38(11):961-965.
[26] MURRAY PE. Platelet-Rich Plasma and Platelet-Rich Fibrin Can Induce Apical Closure More Frequently Than Blood-Clot Revascularization for the Regeneration of Immature Permanent Teeth: A Meta-Analysis of Clinical Efficacy. Front Bioeng Biotechnol. 2018;6:139.
[27] SHIVASHANKAR VY, JOHNS DA, MAROLI RK, et al. Comparison of the Effect of PRP, PRF and Induced Bleeding in the Revascularization of Teeth with Necrotic Pulp and Open Apex: A Triple Blind Randomized Clinical Trial. J Clin Diagn Res. 2017;11(6):C34-C39.
[28] RAVINDRAN S, HUANG C, GEORGE A. Extracellular matrix of dental pulp stem cells: applications in pulp tissue engineering using somatic MSCs. Front Physiol. 2014;4:395.
[29] HU L, GAO Z, XU J, et al. Decellularized Swine Dental Pulp as a Bioscaffold for Pulp Regeneration. Biomed Res Int. 2017; 2017:1-9.
[30] ALQAHTANI Q, ZAKY SH, PATIL A, et al. Decellularized Swine Dental Pulp Tissue for Regenerative Root Canal Therapy. J Dent Res. 2018;97(13):1460-1467.
[31] HUANG C, NARAYANAN R, WARSHAWSKY N, et al. Dual ECM Biomimetic Scaffolds for Dental Pulp Regenerative Applications. Front Physiol. 2018;9:495.
[32] MATOUG-ELWERFELLI M, DUGGAL MS, NAZZAL H, et al. A biocompatible decellularized pulp scaffold for regenerative endodontics. Int Endod J. 2018;51(6):663-673.
[33] SONG JS, TAKIMOTO K, JEON M, et al. Decellularized Human Dental Pulp as a Scaffold for Regenerative Endodontics. J Dent Res.2017;96(6):640-646.
[34] ZHANG S, HOLMES TC, DIPERSIO CM, et al. Self-complementary oligopeptide matrices support mammalian cell attachment. Biomaterials. 1995;16(18): 1385-1393.
[35] CAVALCANTI BN, ZEITLIN BD, NOR JE. A hydrogel scaffold that maintains viability and supports differentiation of dental pulp stem cells. Dent Mater. 2013;29(1):97-102.
[36] CHAN B, WONG RWK, RABIE B. In vivo production of mineralised tissue pieces for clinical use: a qualitative pilot study using human dental pulp cell. Int J Oral Maxillofac Surg. 2011;40(6):612-620.
[37] DISSANAYAKA WL, HARGREAVES KM, JIN L, et al. The Interplay of Dental Pulp Stem Cells and Endothelial Cells in an Injectable Peptide Hydrogel on Angiogenesis and Pulp RegenerationIn Vivo. Tissue Eng Part A. 2015;21(3-4): 550-563.
[38] ROSA V, ZHANG Z, GRANDE RHM, et al. Dental Pulp Tissue Engineering in Full-length Human Root Canals. J Dent Res. 2013;92(11):970-975.
[39] GALLER KM, HARTGERINK JD, CAVENDER AC, et al. A customized self-assembling peptide hydrogel for dental pulp tissue engineering. Tissue Eng Part A. 2012;18(1-2):176-184.
[40] HORII A. Screening of functionalized self-assembling peptide nanofiber scaffolds with angiogenic activity for endothelial cell growth. Progress in Natural Science: Materials International. 2011;21(2):111-116.
[41] NGUYEN PK, GAO W, PATEL SD, et al. Self-Assembly of a Dentinogenic Peptide Hydrogel. ACS Omega. 2018;3(6): 5980-5987.
[42] ENGLER AJ, SEN S, SWEENEY HL, et al. Matrix elasticity directs stem cell lineage specification. Cell. 2006;126(4): 677-689.
[43] 夏鹍,张旗.水凝胶支架材料在牙髓再生中的研究进展[J].口腔医学,2019,39(7):651-654.
[44] ZHU J, MARCHANT RE. Design properties of hydrogel tissue-engineering scaffolds. Expert Rev Med Devices. 2014; 8(5):607-626.
[45] SILVA CR, BABO PS, GULINO M, et al. Injectable and tunable hyaluronic acid hydrogels releasing chemotactic and angiogenic growth factors for endodontic regeneration. Acta Biomater.2018;77:155-171.
[46] ZHANG YS, KHADEMHOSSEINI A. Advances in engineering hydrogels. Science. 2017;356(6337):f3627.
[47] LU Q, PANDYA M, RUFAIHAH AJ, et al. Modulation of Dental Pulp Stem Cell Odontogenesis in a Tunable PEG-Fibrinogen Hydrogel System. Stem Cells Int. 2015;2015:1-9.
[48] MÜLLER AS, ARTNER M, JANJIĆ K, et al. Synthetic Clay–based Hypoxia Mimetic Hydrogel for Pulp Regeneration: The Impact on Cell Activity and Release Kinetics Based on Dental Pulp–derived Cells In Vitro. J Endod. 2018;44(8): 1263-1269.
[49] PASQUI D, TORRICELLI P, CAGNA M, et al.Carboxymethyl cellulose—hydroxyapatite hybrid hydrogel as a composite material for bone tissue engineering applications. J Biomed Mater Res A. 2014;102(5):1568-1579.
[50] JONES TD, KEFI A, SUN S, et al. An Optimized Injectable Hydrogel Scaffold Supports Human Dental Pulp Stem Cell Viability and Spreading. Adv Med. 2016;2016:1-8.
[51] 张倩莉,袁重阳,王晓燕.静电纺纳米纤维支架在牙髓再生中的应用[J].口腔疾病防治,2018,26(11):738-742.
[52] CHIERUZZI M, PAGANO S, MORETTI S, et al.Nanomaterials for Tissue Engineering In Dentistry. Nanomaterials. 2016;6(7): 134.
[53] PRAVEENA C, MANNE P, KALLURI L, et al.Nanobiomaterials and Their Application in Prosthodontics//CHAUGHULE R S. Dental Applications of Nanotechnology.Cham: Springer International Publishing,2018:177-201.
[54] MOHAMMADIAN F, EATEMADI A. Drug loading and delivery using nanofibers scaffolds. Artif Cells Nanomed Biotechnol. 2017;45(5):881-888.
[55] KELLER L, OFFNER D, SCHWINTÉ P, et al. Active Nanomaterials to Meet the Challenge of Dental Pulp Regeneration. Materials. 2015;8(11):7461-7471.
[56] SAGHIRI MA, ASATOURIAN A,GARCIA-GODOY F, et al. Effect of biomaterials on angiogenesis during vital pulp therapy. Dent Mater J. 2016;35(5):701-709.
[57] BOTTINO MC, PANKAJAKSHAN D, NOR JE. Advanced Scaffolds for Dental Pulp and Periodontal Regeneration. Dent Clin North Am. 2017;61(4):689-711.
[58] PANKAJAKSHAN D, ALBUQUERQUE MTP, EVANS JD, et al. Triple Antibiotic Polymer Nanofibers for Intracanal Drug Delivery: Effects on Dual Species Biofilm and Cell Function.J Endod. 2016;42(10):1490-1495.
[59] SOARES DG, ZHANG Z, MOHAMED F, et al. Simvastatin and nanofibrous poly( l -lactic acid) scaffolds to promote the odontogenic potential of dental pulp cells in an inflammatory environment.Acta Biomater.2018;68:190-203.
[60] HASSAN S, PRAKASH G, BAL OZTURK A, et al. Evolution and clinical translation of drug delivery nanomaterials.Nano Today. 2017;15:91-106.
[61] KUANG R, ZHANG Z, JIN X, et al. Nanofibrous spongy microspheres for the delivery of hypoxia-primed human dental pulp stem cells to regenerate vascularized dental pulp. Acta Biomater. 2016;33:225-234.
|