 Quantitative analysis of experimental animals
Quantitative analysis of experimental animals
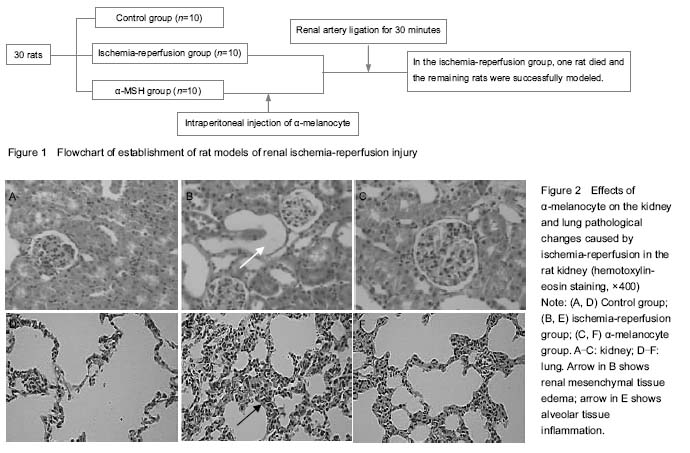
During the injection of drugs, body mass, food intake and color of all rats had no obvious change and awake in 45 minutes, allowed free access to water in 1 hour. A total of 30 rats entered the experiment at beginning. It was divided into control group (
n=10), ischemia-reperfusion group group (
n=10), α-MSH group (
n=10). During experimental process, one rat in ischemia-reperfusion group was dead because of misoperation and all the rats of control group and α-MSH group survived. 29 rats were sacrificed at 24 hours after reperfusion. Flowchart of model establishment is listed in
Figure 1.
Effect of α-MSH on urine, kidney function and water content of rat kidney and lung after ischemia-reperfusion injury
The urine volume in ischemia-reperfusion group rats was higher than that in the control group and α-MSH group
(
P < 0.05). The urine osmotic pressure in the ischemia-reperfusion group was lower than that in the control group and α-MSH group (
P < 0.05). The urea nitrogen and creatinine levels in the ischemia-reperfusion group were higher than in the control group and α-MSH group (
P < 0.05). There was not obvious change in the urea nitrogen and creatinine in the control group and α-MSH group. Kidney and lung water content of the ischemia- reperfusion group was significantly increased compared with control group and α-MSH group (
P < 0.05;
Table 1).

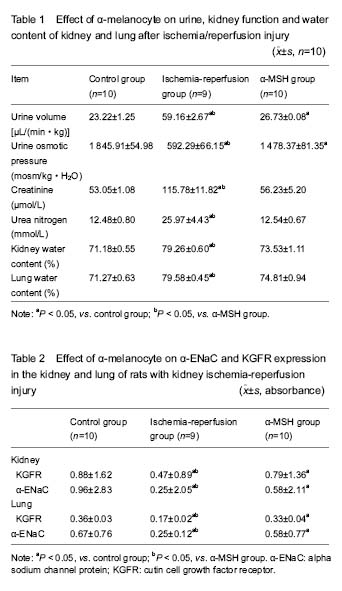
Effects of α-MSH on pathological changes caused by ischemia-reperfusion injury in the rat kidney
Control structure complete renal tubule neat to rows was observed by hematoxylin-eosin staining. Kidney in the ischemia-reperfusion group had obvious pathological changes, malpighian tube lumen exfoliated cells and tube type of necrosis, interstitial hyperemia edema, and glomerular change was not significant. In the α-MSH group, tube type was found. In the ischemia-reperfusion group, dead cells reduced, interstitial hyperemia edema was seen (
Figure 2A-C).
Effects of α-MSH on the lung pathological changes caused by ischemia-reperfusion injury in the rat kidney
A control lung volume was moderate, the color pink, and no congestion. In the ischemia-reperfusion group, lung volume increased, subcapsular flake bleeding. Compared with the ischemia-reperfusion group, the renal pathological changes of α-MSH group significantly reduced. Structure of normal lung tissue was observed under light: control group, no inflammatory cell infiltration, capillaries expansion and congestion, alveolar wall thickening. After ischemia- reperfusion, the experimental alveolar structure disordered, alveolar epithelium swelled, capillary expansion congestion, alveolar interstitial and alveolar seepage, inflammatory cells and proteins in the pathological change of acute lung injury. In the α-MSH group, alveolar exudates were obviously reduced; interstitial edema and alveolar structure tended to be normal (
Figure 2D-F).
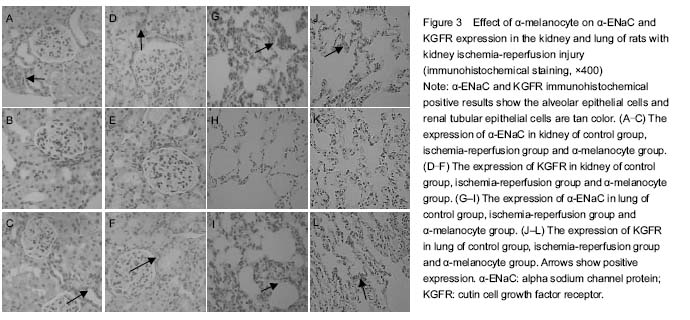
Effects of α-MSH on the KGFR and α-ENaC protein expression change in the kidney and lung of each group after ischemia-reperfusion injury in the rat kidney
In the control group, the expressions of KGFR and α-ENaC protein in the alveolar epithelial cells and renal tubular epithelial cells were strongly positive. Compared with the ischemia-reperfusion group, the KGFR and α-ENaC protein expression was significantly increased in the control group and α-MSH group (
P < 0.05;
Figure 3, Table 2).
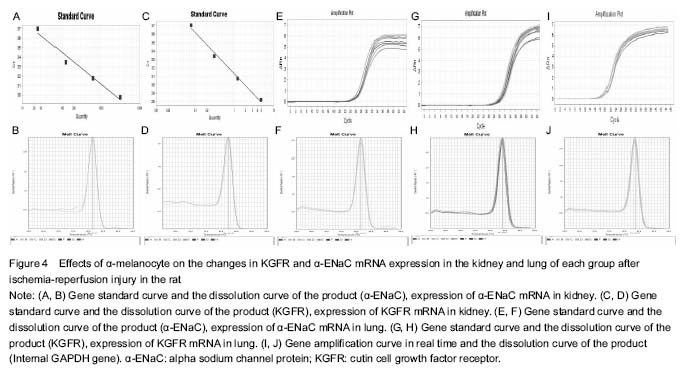
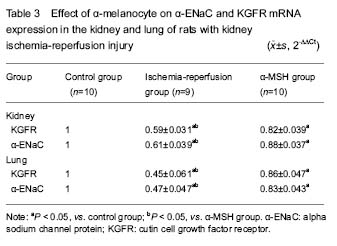
Changes in KGFR and α-ENaC mRNA levels in the kidney and lung of each group
The results of RT-PCR showed that KGFR and α-ENaC mRNA levels were significantly increased in the α-MSH group than in the ischemia-reperfusion group (P < 0.05), and it was lower in the α-MSH group and ischemia- reperfusion group than in the control group (
P < 0.05;
Figure 4, Table 3).