中国组织工程研究 ›› 2016, Vol. 20 ›› Issue (20): 2940-2948.doi: 10.3969/j.issn.2095-4344.2016.20.008
• 骨组织构建 bone tissue construction • 上一篇 下一篇
阿伐他汀激活wnt/β-catenin信号通路促进骨质疏松模型大鼠移植物的骨整合
梁耀中1,陈 舒2,杨裕豪1,蓝春海1,张国威1,纪志盛1,林宏生1
- 暨南大学附属第一医院,1骨科,2妇产科,广东省广州市 510630
-
收稿日期:2016-04-06出版日期:2016-05-13发布日期:2016-05-13 -
通讯作者:林宏生,博士,教授,主任医师。暨南大学附属第一医院骨科,广东省广州市 510630 -
作者简介:梁耀中,男,1980年生,广西壮族自治区人,汉族,2010年暨南大学毕业,硕士,主治医师,主要从事脊柱外科及关节外科与骨组织工程研究。 -
基金资助:广东省自然科学基金(2014A030313357)
Atorvastatin promotes implant osseointegration via the activation of Wnt/β-catenin signal pathway in osteoporotic rats
Liang Yao-zhong1, Chen Shu2, Yang Yu-hao1, Lan Chun-hai1, Zhang Guo-wei1, Ji Zhi-sheng1, Lin Hong-sheng1
- 1 Department of Orthopedics, the First Affiliated Hospital of Jinan University, Guangzhou 510630, Guangdong Province, China
2 Department of Gynaecology and Obstetrics, the First Affiliated Hospital of Jinan University, Guangzhou 510630, Guangdong Province, China
-
Received:2016-04-06Online:2016-05-13Published:2016-05-13 -
Contact:Lin Hong-sheng, M.D., Chief physician, Department of Orthopedics, the First Affiliated Hospital of Jinan University, Guangzhou 510630, Guangdong Province, China -
About author:Liang Yao-zhong, Master, Attending physician, Department of Orthopedics, the First Affiliated Hospital of Jinan University, Guangzhou 510630, Guangdong Province, China -
Supported by:the Natural Science Foundation of Guangdong Province, China, No. 2014A030313357
摘要:
文章快速阅读:
.jpg)
文题释义: 骨质疏松症:是多种原因引起的一组骨病,骨组织有正常的钙化,钙盐与基质呈正常比例,以单位体积内骨组织量减少为特点的代谢性骨病变。在多数骨质疏松中,骨组织的减少主要由于骨质吸收增多所致,以骨骼疼痛、易于骨折为特征。 骨结合:为正常的改建骨和种植体直接接触,无光学显微镜下可见到的软组织长入,并能使种植体的负荷持续传导并分散在骨组织中。
中图分类号:
引用本文
梁耀中1,陈 舒2,杨裕豪1,蓝春海1,张国威1,纪志盛1,林宏生1. 阿伐他汀激活wnt/β-catenin信号通路促进骨质疏松模型大鼠移植物的骨整合[J]. 中国组织工程研究, 2016, 20(20): 2940-2948.
Liang Yao-zhong1, Chen Shu2, Yang Yu-hao1, Lan Chun-hai1, Zhang Guo-wei1, Ji Zhi-sheng1, . Atorvastatin promotes implant osseointegration via the activation of Wnt/β-catenin signal pathway in osteoporotic rats[J]. Chinese Journal of Tissue Engineering Research, 2016, 20(20): 2940-2948.
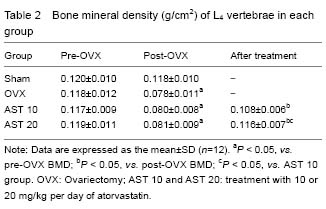
BMD of L4 vertebrae in the Sham, ovariectomy, AST 10 and AST 20 groups at different time points are showed in Table 2. BMD of rats receiving ovariectomy was decreased. BMD of rats in AST 20 group was significantly increased compared with AST 10 group (P < 0.05). There was no significant difference in BMD between AST 20 and Sham groups (P > 0.05).
| [1] Kanis JA. Assessment of fracture risk and its application to screening for postmenopausal osteoporosis: synopsis of a WHO report. WHO Study Group. Osteoporos Int. 1994;4(6):368-381.[2] Ray NF, Chan JK, Thamer M, et al. Medical expenditures for the treatment of osteoporotic fractures in the United States in 1995: report from the National Osteoporosis Foundation. J Bone Miner Res. 1997;12(1):24-35.[3] Kwak B, Mulhaupt F, Myit S, et al. Statins as a newly recognized type of immunomodulator. Nat Med. 2000; 6(12):1399-1402.[4] Kobashigawa JA. Statins as immunosuppressive agents. Liver Transpl. 2001;7(6):559-561.[5] Gomberg-Maitland M, Fuster V, Fayad ZA, et al. Statins and plaque stability. J Cardiovasc Risk. 2003;10(3):161-167.[6] Skaletz-Rorowski A, Walsh K. Statin therapy and angiogenesis. Curr Opin Lipidol. 2003;14(6):599-603.[7] Dimmeler S, Aicher A, Vasa M, et al. HMG-CoA reductase inhibitors (statins) increase endothelial progenitor cells via the PI 3-kinase/Akt pathway. J Clin Invest. 2001;108(3):391-397.[8] Lu D, Goussev A, Chen J, et al. Atorvastatin reduces neurological deficit and increases synaptogenesis, angiogenesis, and neuronal survival in rats subjected to traumatic brain injury. J Neurotrauma. 2004;21(1):21-32.[9] Edwards CJ, Hart DJ, Spector TD. Oral statins and increased bone-mineral density in postmenopausal women. Lancet. 2000;355(9222):2218-2219.[10] Chan KA, Andrade SE, Boles M, et al. Inhibitors of hydroxymethylglutaryl-coenzyme A reductase and risk of fracture among older women. Lancet. 2000;355 (9222): 2185-2188.[11] Meier CR, Schlienger RG, Kraenzlin ME, et al. HMG-CoA reductase inhibitors and the risk of fractures. JAMA. 2000;283(24):3205-3210.[12] Wang PS, Solomon DH, Mogun H, et al. HMG-CoA reductase inhibitors and the risk of hip fractures in elderly patients. JAMA. 2000;283(24):3211-3216.[13] Schoofs MW, Sturkenboom MC, van der Klift M, et al. HMG-CoA reductase inhibitors and the risk of vertebral fracture. J Bone Miner Res. 2004;19(9):1525-1530.[14] Bauer DC, Mundy GR, Jamal SA, et al. Use of statins and fracture. Results of 4 prospective studies and cumulative meta-analysis of observational studies and controlled trials. Arch Int Med. 2004;164(2):146-152.[15] Ruiz-Gaspa S, Nogues X, Enjuanes A, et al. Simvastatin and atorvastatin enhance gene expression of collagen type 1 and osteocalcin in primary human osteoblasts and MG-63 cultures. J Cell Biochem. 2007;101(6):1430-1438.[16] Kim JY, Lee EY, Lee EB, et al. Atorvastatin inhibits osteoclastogenesis by decreasing the expression of RANKL in the synoviocytes of rheumatoid arthritis. Arthritis Res Ther. 2012;14(4):R187.[17] Viereck V, Grundker C, Blaschke S, et al. Atorvastatin stimulates the production of osteoprotegerin by human osteoblasts. J Cell Biochem. 2005;96(6):1244-1253.[18] Gradosova I, Zivna H, Palicka V, et al. Protective effect of atorvastatin on bone tissue in orchidectomised male albino Wistar rats. Eur J Pharmacol. 2012;679(1-3):144-150.[19] Lima CEVD, Calixto JC, Anbinder AL. Influence of the association between simvastatin and demineralized bovine bone matrix on bone repair in rats. Braz Oral Res. 2011;25(1):42-48.[20] Alvarez K, Fukuda M, Yamamoto O. Titanium Implants after alkali heating treatment with a [Zn(OH)4]2 complex: analysis of interfacial bond strength using push-out tests. Clin Implant Dent Relat Res. 2010;12 Suppl 1:e114-e125.[21] NIH Consensus Development Panel on Osteoporosis Prevention, Diagnosis, and Therapy. Osteoporosis prevention, diagnosis, and therapy. JAMA. 2001;285(6): 785-795.[22] Osteoporosis prevention, diagnosis, and therapy. NIH Consens Statement. 2000;17(1):1-45.[23] Sato M, Bryant HU, Iversen P, et al. Advantages of raloxifene over alendronate or estrogen on nonreproductive and reproductive tissues in the long-term dosing of ovariectomized rats. J Pharmacol Exp Ther. 1996;279(1):298-305.[24] Zheng X, Wu G, Nie Y, et al. Electroacupuncture at the governor vessel and bladder meridian acupoints improves postmenopausal osteoporosis through osteoprotegerin/ RANKL/RANK and Wnt/beta-catenin signaling pathways. Exp Ther Med. 2015;10(2):541-548.[25] Ray S, Thormann U, Sommer U, et al. Effects of macroporous, strontium loaded xerogel-scaffolds on new bone formation in critical-size metaphyseal fracture defects in ovariectomized rats. Injury. 2016;47 Suppl 1:S52-S61.[26] Mundy G, Garrett R, Harris S, et al. Stimulation of bone formation in vitro and in rodents by statins. Science. 1999;286(5446):1946-1949.[27] Chen PY, Sun JS, Tsuang YH, et al. Simvastatin promotes osteoblast viability and differentiation via Ras/Smad/Erk/BMP-2 signaling pathway. Nutr Res. 2010; 30(3):191-199.[28] Chen S, Yang JY, Zhang SY, et al. Effects of simvastatin gel on bone regeneration in alveolar defects in miniature pigs. Chin Med J (Engl). 2011;124(23):3953-3958.[29] Kajinami K, Takekoshi N, Matsui S, et al. Effect of pretreatment vitamin D levels on in vivo effects of atorvastatin on bone metabolism in patients with heterozygous familial hypercholesterolemia. Am J Cardiol. 2003;92(9):1113-1116.[30] Liu C, Wu Z, Sun HC. The effect of simvastatin on mRNA expression of transforming growth factor-beta1, bone morphogenetic protein-2 and vascular endothelial growth factor in tooth extraction socket. Int J Oral Sci. 2009;1(2):90-98.[31] Zhang M, Zhou SH, Li XP, et al. Atorvastatin downregulates BMP-2 expression induced by oxidized low-density lipoprotein in human umbilical vein endothelial cells. Circ J. 2008;72(5):807-812.[32] Savopoulos C, Dokos C, Kaiafa G, et al. Adipogenesis and osteoblastogenesis: trans-differentiation in the pathophysiology of bone disorders. Hippokratia. 2011;15(1):18-21.[33] Song C, Guo Z, Ma Q, et al. Simvastatin induces osteoblastic differentiation and inhibits adipocytic differentiation in mouse bone marrow stromal cells. Biochem Biophys Res Commun. 2003;308(3):458-462.[34] Cruz AC, Gruber BL. Statins and osteoporosis: can these lipid-lowering drugs also bolster bones? Cleve Clin J Med. 2002;69(4):277-278.[35] Lacey DL, Timms E, Tan HL, et al. Osteoprotegerin ligand is a cytokine that regulates osteoclast differentiation and activation. Cell. 1998;93(2):165-176.[36] Maritz FJ, Conradie MM, Hulley PA, et al. Effect of statins on bone mineral density and bone histomorphometry in rodents. Arterioscler Thromb Vasc Biol. 2001;21(10):1636-1641.[37] Golabek K, Ostrowska Z, Ziora K, et al. Association between omentin-1, bone metabolism markers, and cytokines of the RANKL/RANK/OPG system in girls with anorexia nervosa. Endokrynologia Polska. 2015;66(6): 514-520.[38] Goes P, Lima AP, Melo IM, et al. Effect of Atorvastatin in radiographic density on alveolar bone loss in wistar rats. Braz Dent J. 2010;21(3):193-198.[39] Marie PJ,Kassem M. Osteoblasts in osteoporosis: past, emerging, and future anabolic targets. Eur J Endocrinol. 2011;165(1):1-10.[40] Rabbani SA, Arakelian A, Farookhi R. LRP5 knockdown: effect on prostate cancer invasion growth and skeletal metastasis in vitro and in vivo. Cancer Med. 2013;2(5): 625-635.[41] Chu TQ, Teng JJ, Jiang LY, et al. Lung cancer-derived Dickkopf1 is associated with bone metastasis and the mechanism involves the inhibition of osteoblast differentiation. Biochem Biophys Res Commun. 2014; 443(3):962-968.[42] Morvan F, Boulukos K, Clement-Lacroix P, et al. Deletion of a single allele of the Dkk1 gene leads to an increase in bone formation and bone mass. J Bone Miner Res. 2006;21(6):934-945.[43] Li J, Sarosi I, Cattley RC, et al. Dkk1-mediated inhibition of Wnt signaling in bone results in osteopenia. Bone. 2006;39(4):754-766.[44] Lozano D, Sanchez-Salcedo S, Portal-Nunez S, et al. Parathyroid hormone-related protein (107-111) improves the bone regeneration potential of gelatin-glutaraldehyde biopolymer-coated hydroxyapatite. Acta Biomater. 2014;10(7):3307-3316.[45] Li XD, Ominsky MS, Niu QT, et al. Targeted deletion of the sclerostin gene in mice results in increased bone formation and bone strength. J Bone Miner Res. 2008; 23(6):860-869.[46] Winkler DG, Sutherland MK, Geoghegan JC, et al. Osteocyte control of bone formation via sclerostin, a novel BMP antagonist. EMBO J. 2003;22(23):6267-6276.[47] Rajamannan NM, Subramaniam M, Caira F, et al. Atorvastatin inhibits hypercholesterolemia-induced calcification in the aortic valves via the Lrp5 receptor pathway. Circulation. 2005;112(9 Suppl):1229-1234. |
| [1] | 肖方骏, 陈树东, 栾继耀, 侯 宇, 何 坤, 林定坤. 丹参干预骨质疏松症:网络药理学解释的作用机制[J]. 中国组织工程研究, 2021, 25(5): 772-778. |
| [2] | 吴子健, 胡昭端, 谢有琼, 王 峰, 李 佳, 李柏村, 蔡国伟, 彭 锐. 3D打印技术与骨组织工程研究文献计量及研究热点可视化分析[J]. 中国组织工程研究, 2021, 25(4): 564-569. |
| [3] | 李晓壮, 段 浩, 王伟舟, 唐志宏, 王旸昊, 何 飞. 骨组织工程材料治疗骨缺损疾病在体内实验中的应用[J]. 中国组织工程研究, 2021, 25(4): 626-631. |
| [4] | 张立书, 刘安琪, 何小宁, 金 岩, 李 蓓, 金 钫. Alpl基因影响骨髓间充质干细胞治疗溃疡性结肠炎[J]. 中国组织工程研究, 2021, 25(25): 3970-3975. |
| [5] | 陈 崧, 何远丽, 谢雯佳, 钟林娜, 王 剑. 磷酸钙纳米颗粒药物递送系统在骨组织工程研究与应用中的优势[J]. 中国组织工程研究, 2021, 25(22): 3565-3570. |
| [6] | 张振华, 刘姿辰, 禹宝庆. 聚己内酯及其复合材料在组织工程骨构建中的地位与问题[J]. 中国组织工程研究, 2021, 25(22): 3571-3577. |
| [7] | 蒋昇源, 李 丹, 姜建浩, 杨上游, 杨淑野. 假体无菌性松动过程中Co2+对成骨前体细胞的生物学反应[J]. 中国组织工程研究, 2021, 25(21): 3292-3299. |
| [8] | 许 辉, 康冰心, 钟 声, 高晨鑫, 赵 翅, 邱国伟, 孙松涛, 解 骏, 肖涟波, 施 杞. 点按局部腧穴与坐位调膝法联用治疗膝关节骨关节炎:随机对照研究[J]. 中国组织工程研究, 2021, 25(2): 216-221. |
| [9] | 李 平, 林 煜, 陈 翔, 刘振涛, 肖莉莉, 林学义, 华 鹏. 二至丸提取物干预去势骨质疏松雌性模型大鼠的骨重建特点[J]. 中国组织工程研究, 2021, 25(2): 191-195. |
| [10] | 魏 琴, 张 雪, 马 磊, 李志强, 寿 玺, 段明军, 吴 硕, 贾麒钰, 马 创. 血小板衍生生长因子BB诱导大鼠骨髓间充质干细胞向成骨细胞分化[J]. 中国组织工程研究, 2021, 25(19): 2953-2957. |
| [11] | 汪 鎏, 宋东哲, 黄定明. 骨形态发生蛋白9调控干细胞分化与骨再生[J]. 中国组织工程研究, 2021, 25(19): 3064-3070. |
| [12] | 艾力麦尔旦•艾尼瓦尔, 王 玲, 古 丽, 迪丽达尔•塔西甫拉提, 王 珊, 尹宏斌. 转化生长因子β3对成骨细胞增殖和成骨能力的影响[J]. 中国组织工程研究, 2021, 25(17): 2664-2669. |
| [13] | 付力伟, 杨 振, 李 浩, 高仓健, 眭 翔, 刘舒云, 郭全义 . 亲和肽在软骨组织工程中应用的新策略和问题[J]. 中国组织工程研究, 2021, 25(16): 2569-2574. |
| [14] | 李晏乐, 岳肖华, 聂 真, 张峻玮, 李朝辉, 聂伟志, 姜红江. 生物可吸收材料特点及在骨科中的应用[J]. 中国组织工程研究, 2021, 25(16): 2612-2617. |
| [15] | 罗诒财, 李 昊. 增强芳香烃受体表达对糖尿病模型大鼠牙槽骨缺损区愈合及炎症反应的影响[J]. 中国组织工程研究, 2021, 25(14): 2166-2171. |
中国组织工程研究杂志出版内容重点:组织构建;骨细胞;软骨细胞;细胞培养;成纤维细胞;血管内皮细胞;骨质疏松;组织工程
|
Table 1 Primer sequences for RT-qPCR
|
|
|
Note: DKK1: Dickkopf Wnt signaling pathway inhibitor 1; Sost: sclerostin; LRP5: low-density lipoprotein associated protein 5; GAPDH: glyceraldehyde-3-phosphate dehydrogenase;
|
Data were analyzed using SPSS 13.0 statistical software (SPSS, Chicago, IL, USA). The measurement data were experssed as the mean± SD. Intergroup comparisons were analyzed using one-way analysis of variance. A value of P < 0.05 was considered statistically significant.
中国组织工程研究杂志出版内容重点:组织构建;骨细胞;软骨细胞;细胞培养;成纤维细胞;血管内皮细胞;骨质疏松;组织工程
.jpg)
骨质疏松症是多种原因引起的一组骨病,骨组织有正常的钙化,钙盐与基质呈正常比例,以单位体积内骨组织量减少为特点的代谢性骨病变。在多数骨质疏松中,骨组织的减少主要由于骨质吸收增多所致,以骨骼疼痛、易于骨折为特征。 中国组织工程研究杂志出版内容重点:组织构建;骨细胞;软骨细胞;细胞培养;成纤维细胞;血管内皮细胞;骨质疏松;组织工程
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||