Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (47): 7591-7596.doi: 10.3969/j.issn.2095-4344.2014.47.009
Previous Articles Next Articles
Effect of phosphorus ions on human bone marrow mesenchymal stem cells under three-dimensional culture
Lei Qun, Chen Jiang, Huang Wen-xiu, Wu Dong, Lin Dong
- Department of Dental Implant, Stomatological Hospital of Fujian Medical University, Fuzhou 350000, Fujian Province, China
-
Revised:2014-10-18Online:2014-11-19Published:2014-11-19 -
Contact:Chen Jiang, M.D., Professor, Chief physician, Doctoral supervisor, Department of Dental Implant, Stomatological Hospital of Fujian Medical University, Fuzhou 350000, Fujian Province, China -
About author:Lei Qun, M.D., Physician, Department of Dental Implant, Stomatological Hospital of Fujian Medical University, Fuzhou 350000, Fujian Province, China -
Supported by:the Key Clinical Specialty Discipline Construction Program of Fujian Province, No. (2012)1589; Key Project of Fujian Provincial Department of Science and Technology, No. 2013Y0039
CLC Number:
Cite this article
Lei Qun, Chen Jiang, Huang Wen-xiu, Wu Dong, Lin Dong. Effect of phosphorus ions on human bone marrow mesenchymal stem cells under three-dimensional culture [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(47): 7591-7596.
share this article
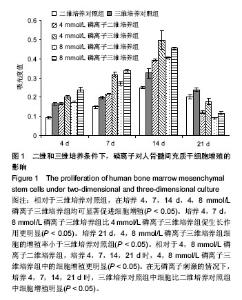
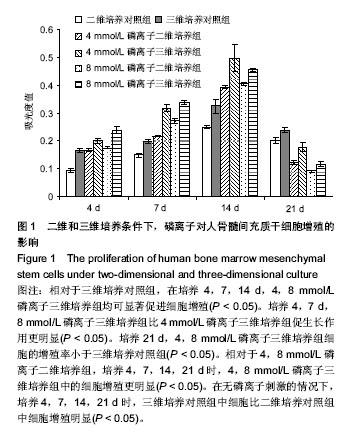
2.1 磷离子对人骨髓间充质干细胞增殖的影响 在聚苯乙烯三维支架上培养人骨髓间充质干细胞,相对于三维培养对照组,在培养4,7,14 d,4,8 mmol/L磷离子三维培养组均可显著促进细胞增殖(P < 0.05)。培养4,7 d,8 mmol/L磷离子三维培养组比4 mmol/L磷离子三维培养组促生长作用更明显(P < 0.05)。 培养21 d,4,8 mmol/L磷离子三维培养组细胞的增殖率小于三维培养对照组(P < 0.05)。相对于4,8 mmol/L磷离子二维培养组,培养4,7,14,21 d时,4,8 mmol/L磷离子三维培养组中的细胞增殖更明显(P < 0.05)。在无磷离子刺激的情况下,培养4,7,14,21 d时,三维培养对照组中细胞比二维培养对照组中细胞增殖明显(P < 0.05)。见图1。"
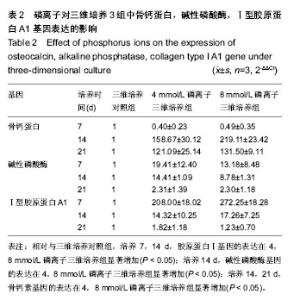
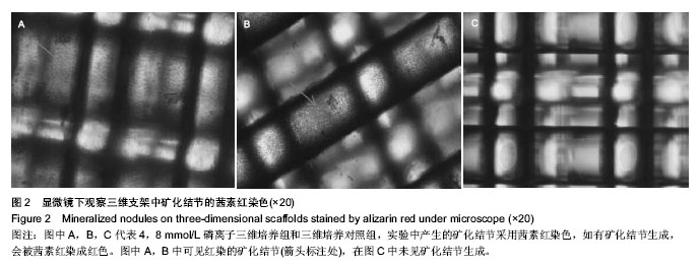
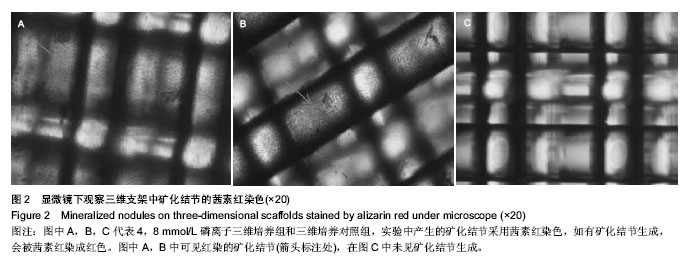
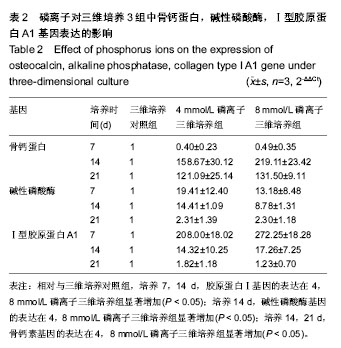
2.2 磷离子对三维培养3组中骨钙蛋白,碱性磷酸酶,Ⅰ型胶原蛋白A1基因表达的影响 RT-PCR结果显示,在三维培养支架上,培养14 d,4,8 mmol/L磷离子三维培养组中骨钙蛋白基因的表达明显上调(P < 0.05)。培养21 d,4,8 mmol/L磷离子三维培养组中骨钙蛋白基因的表达也明显上调(P < 0.05)。培养14 d,8 mmol/L磷离子三维培养组中骨钙蛋白基因的表达高于4 mmol/L磷离子三维培养组(P < 0.05)。见表2。 人骨髓间充质干细胞在4 mmol/L磷离子三维培养组中培养7,14 d时,碱性磷酸酶基因的表达明显高于三维培养对照组(P < 0.05)。在8 mmol/L磷离子三维培养组培养14 d时,碱性磷酸酶基因的表达明显高于三维培养对照组(P < 0.05)。见表2。 人骨髓间充质干细胞在三维培养各组培养7 d,4,8 mmol/L磷离子三维培养组Ⅰ型胶原蛋白A1基因的表达高于三维培养对照组(P < 0.05),8 mmol/L磷离子三维培养组中Ⅰ型胶原蛋白A1基因的表达水平同时明显高于4 mmol/L磷离子三维培养组(P < 0.05)。在三维培养对照组,4和8 mmol/L磷离子三维培养组培养14 d,4,8 mmol/L磷离子三维培养组Ⅰ型胶原蛋白A1基因的表达水平高于三维培养对照组(P < 0.05)。见表2。"
| [1] Bokhari M, Carnachan RJ, Cameron NR, et al. Novel cell culture device enabling three-dimensional cell growth and improved cell function. Biochem Biophys Res Commun. 2007;354(4):1095-1100. [2] Inanc B, Elcin AE, Elcin YM. Osteogenic induction of human periodontal ligament fibroblasts under two-and three- dimensional culture conditions. Tissue Eng. 2006;12(2):257-266. [3] Parekkadan B, Milwid JM. Mesenchymal stem cells as therapeutics. Annu Rev Biomed Eng. 2010;15(12):87-117. [4] Asari S, Itakura S, Ferreri K, et al. Mesenchymal stem cells suppress B-cell terminal differentiation. Exp Hematol. 2009; 37(5):604-615. [5] Ramasamy R, Tong CK, Seow HF, et al. The immunosuppressive effects of human bone marrow derived mesenchymal stem cells target T cell prolifferation but not its effector function. Cell Immunol. 2008;251(2):131-136. [6] Honda Y, Anada T, Kamakura S, et al. Elevated extracellular calcium stimulates secretion of bone morphogenetic protein 2 by a macrophage cell line. Biochem Biophys Res Commun. 2006;345(3):1155-1160. [7] Livak KJ, Schmittgen TD. Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods. 2001;25(4):402-408. [8] Joe AW, Gregory-Evans K. Mesenchymal stem cells and potential applications in treating ocular disease. Curr Eye Res. 2010;35(11):941-952. [9] Giordano R, Canesi M, Isalberti M, et al. Autologous mesenchymal stem cell therapy for progressive supranuclear palsy: translation into a phase I controlled, randomized clinical study. J Transl Med. 2014;12:14. [10] Gopal K, Amirhamed HA, Kamarul T. Advances of human bone marrow-derived mesenchymal stem cells in the treatment of cartilage defects: a systematic review. Exp Biol Med (Maywood). 2014;239(6):663-669. [11] Moghadasali R, Azarnia M, Hajinasrollah M, et al. Intra-renal arterial injection of autologous bone marrow mesenchymal stromal cells ameliorates cisplatin-induced acute kidney injury in a rhesus Macaque mulatta monkey model. Cytotherapy. 2014;16(6):734-749. [12] Pan XH, Yang XY, Yao X, et al. Bone-marrow mesenchymal stem cell transplantation to treat diabetic nephropathy in tree shrews. Cell Biochem Funct. 2014;32(5):453-463. [13] Huang NF, Li S. Mesenchymal stem cells for vascular regeneration. Regen Med. 2008;3(6):877-892. [14] Bruder SP, Fink DJ, Caplan AL. Mesenchymal stem cells in bonedevelopment, bone repair and skeletal regeneration therapy. J Cell Biochem. 1994;56(3):283-294. [15] Badet L, Benhamou PY, Wojtusciszyn A, et al. Expectations and strategies regardingislet transplantation: metabolic data from the GRAGIL 2 trial. Transplantation. 2007;84(1):89-96. [16] Janssens S, Dubois C, Bogaert J, et al. Autologous bone marrow-derived stem-cell transfer in patients with ST-segment elevation myocardial infarction: doubleblind, randomized controlled trials. Lancet. 2006;367(9505):113-121. [17] Wang C, Wang S, Li K, et al. Preparation of Laponite Bioceramics for Potential Bone Tissue Engineering Applications. PLoS One. 2014;9(6):e99585. [18] Nazemi K, Moztarzadeh F, Jalali N, et al. Synthesis and Characterization of Poly(lactic-co-glycolic) Acid Nanoparticles-Loaded Chitosan/Bioactive Glass Scaffolds as a Localized Delivery System in the Bone Defects. Biomed Res Int. 2014;2014:898930. [19] Salehi S, Grünert AK, Bahners T, et al. New nanofibrous scaffold for corneal tissue engineering. Klin Monbl Augenheilkd. 2014;231(6):626-630. [20] Stevanato L, Sinden JD. The effects of microRNAs on human neural stem cell differentiation in two- and three-dimensional cultures. Stem Cell Res Ther. 2014;5(2):49. [21] Ülker HE, Ülker M, Gümü? et al. Cytotoxicity testing of temporary luting cements with two- and three-dimensional cultures of bovine dental pulp-derived cells. Biomed Res Int. 2013;2013:910459. [22] Saltzman WM. Weaving cartilage at zero g: the reality of tissue engineering in space. Proc Natl Acad Sci U S A. 1997;94(25):13380-13382. [23] Komlev VS, Barinov SM, Bozo II, et al. Bioceramics composed of octacalcium phosphate demonstrate enhanced biological behavior. ACS Appl Mater Interfaces. 2014;6(19): 16610-16620 . [24] Zorin VL, Komlev VS, Zorina AI, et al. Octacalcium phosphate ceramics combined with gingiva-derived stromal cells for engineered functional bone grafts. Biomed Mater. 2014;9(5): 055005. [25] Ling LE, Feng L, Liu HC, et al. The effect of calcium phosphate composite scaffolds on the osteogenic differentiation of rabbit dental pulp stem cells. J Biomed Mater Res A. 2014 [Epub ahead of print]. [26] Bléry P, Corre P, Malard O, et al. Evaluation of new bone formation in irradiated areas using association of mesenchymal stem cells and total fresh bone marrow mixed with calcium phosphate scaffold. J Mater Sci Mater Med. 2014 [Epub ahead of print]. [27] Baykan E, Koc A, Eser Elcin A, et al. Evaluation of a biomimetic poly(ε-caprolactone)/β-tricalcium phosphate multispiral scaffold for bone tissue engineering: in vitro and in vivo studies. Biointerphases. 2014;9(2):029011. [28] Qiao PY, Li FF, Dong LM, et al. Delivering MC3T3-E1 cells into injectable calcium phosphate cement through alginate-chitosan microcapsules for bone tissue engineering. J Zhejiang Univ Sci B. 2014;15(4):382-392. [29] Rendenbach C, Yorgan TA, Heckt T, et al. Effects of extracellular phosphate on gene expression in murine osteoblasts. Calcif Tissue Int. 2014;94(5):474-483. [30] LeGeros RZ. Properties of Osteoconductive Biomaterials: Calcium Phosphates. Clin Orthop Related Res. 2002;395: 81-89. [31] Song IH, Dennis JE. Simple evaluation method for osteoinductive capacity of cells or scaffolds using ceramic cubes. Tissue Cell. 2014;46(5):372-378. [32] Perez RA, Riccardi K, Altankov G, et al. Dynamic cell culture on calcium phosphate microcarriers for bone tissue engineering applications. J Tissue Eng. 2014;5: 2041731414543965. [33] Brennan MA, Renaud A, Amiaud J, et al. Pre-clinical studies of bone regeneration with human bone marrow stromal cells and biphasic calcium phosphate. Stem Cell Res Ther. 2014; 5(5):114. [34] Zhou R, Xu W, Chen F, et al. Amorphous calcium phosphate nanospheres/polylactide composite coated tantalum scaffold: Facile preparation, fast biomineralization and subchondral bone defect repair application. Colloids Surf B Biointerfaces. 2014[Epub ahead of print]. [35] Rajzer I, Menaszek E, Kwiatkowski R, et al. Electrospun gelatin/poly(ε-caprolactone) fibrous scaffold modified with calcium phosphate for bone tissue engineering. Mater Sci Eng C Mater Biol Appl. 2014;44:183-190. [36] Sanda M, Shiota M, Fujii M, et al. Capability of new bone formation with a mixture of hydroxyapatite and beta-tricalcium phosphate granules. Clin Oral Implants Res. 2014[Epub ahead of print]. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Lin Qingfan, Xie Yixin, Chen Wanqing, Ye Zhenzhong, Chen Youfang. Human placenta-derived mesenchymal stem cell conditioned medium can upregulate BeWo cell viability and zonula occludens expression under hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 4970-4975. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Zhang Xiumei, Zhai Yunkai, Zhao Jie, Zhao Meng. Research hotspots of organoid models in recent 10 years: a search in domestic and foreign databases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1249-1255. |
| [5] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [6] | Shi Yangyang, Qin Yingfei, Wu Fuling, He Xiao, Zhang Xuejing. Pretreatment of placental mesenchymal stem cells to prevent bronchiolitis in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 991-995. |
| [7] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [8] | Fan Quanbao, Luo Huina, Wang Bingyun, Chen Shengfeng, Cui Lianxu, Jiang Wenkang, Zhao Mingming, Wang Jingjing, Luo Dongzhang, Chen Zhisheng, Bai Yinshan, Liu Canying, Zhang Hui. Biological characteristics of canine adipose-derived mesenchymal stem cells cultured in hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1002-1007. |
| [9] | Geng Yao, Yin Zhiliang, Li Xingping, Xiao Dongqin, Hou Weiguang. Role of hsa-miRNA-223-3p in regulating osteogenic differentiation of human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1008-1013. |
| [10] | Lun Zhigang, Jin Jing, Wang Tianyan, Li Aimin. Effect of peroxiredoxin 6 on proliferation and differentiation of bone marrow mesenchymal stem cells into neural lineage in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1014-1018. |
| [11] | Zhu Xuefen, Huang Cheng, Ding Jian, Dai Yongping, Liu Yuanbing, Le Lixiang, Wang Liangliang, Yang Jiandong. Mechanism of bone marrow mesenchymal stem cells differentiation into functional neurons induced by glial cell line derived neurotrophic factor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1019-1025. |
| [12] | Duan Liyun, Cao Xiaocang. Human placenta mesenchymal stem cells-derived extracellular vesicles regulate collagen deposition in intestinal mucosa of mice with colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1026-1031. |
| [13] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [14] | Guan Qian, Luan Zuo, Ye Dou, Yang Yinxiang, Wang Zhaoyan, Wang Qian, Yao Ruiqin. Morphological changes in human oligodendrocyte progenitor cells during passage [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1045-1049. |
| [15] | Wang Zhengdong, Huang Na, Chen Jingxian, Zheng Zuobing, Hu Xinyu, Li Mei, Su Xiao, Su Xuesen, Yan Nan. Inhibitory effects of sodium butyrate on microglial activation and expression of inflammatory factors induced by fluorosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1075-1080. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||