Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (26): 4178-4183.doi: 10.12307/2024.434
Previous Articles Next Articles
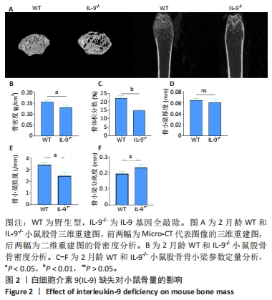
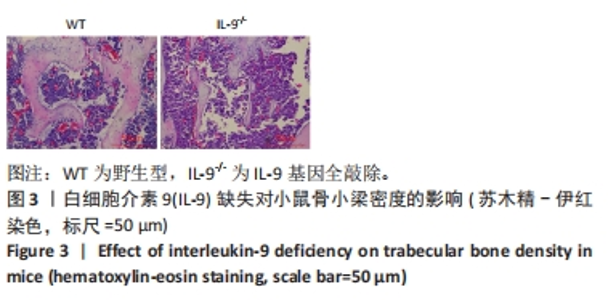
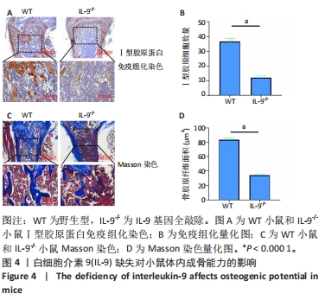
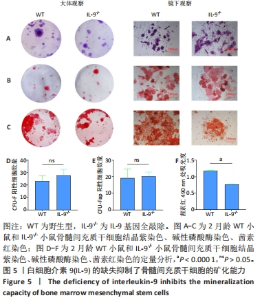
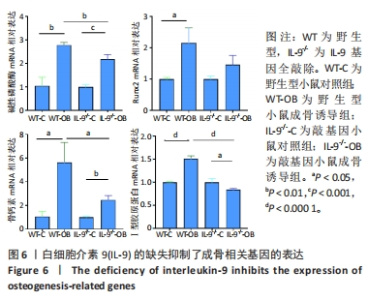
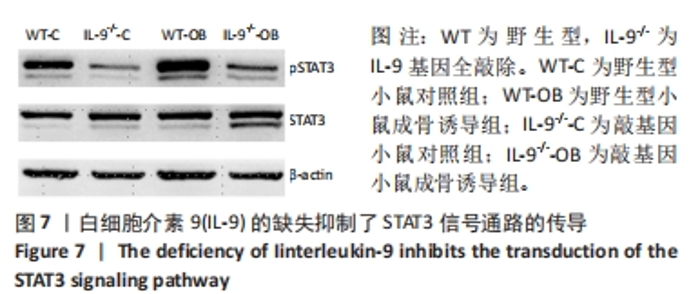
Deficiency of interleukin-9 inhibits osteogenic potential in mice
Wang Yi, Chen Chichi, Zhou Xichao, Shi Qin
- Department of Orthopedics, the First Affiliated Hospital of Soochow University, Institute of Orthopedics of Soochow University, Suzhou 215006, Jiangsu Province, China
-
Received:2023-06-10Accepted:2023-08-01Online:2024-09-18Published:2023-09-28 -
Contact:Shi Qin, MD, Professor, Department of Orthopedics, the First Affiliated Hospital of Soochow University, Institute of Orthopedics of Soochow University, Suzhou 215006, Jiangsu Province, China -
About author:Wang Yi, Department of Orthopedics, the First Affiliated Hospital of Soochow University, Institute of Orthopedics of Soochow University, Suzhou 215006, Jiangsu Province, China -
Supported by:the National Natural Science Foundation of China (General Program), No. 81972059 (to SQ)
CLC Number:
Cite this article
Wang Yi, Chen Chichi, Zhou Xichao, Shi Qin. Deficiency of interleukin-9 inhibits osteogenic potential in mice[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(26): 4178-4183.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
| [1] COMPSTON JE, MCCLUNG MR, LESLIE WD. Osteoporosis. Lancet. 2019;393(10169):364-376. [2] EASTELL R, O’NEILL TW, HOFBAUER LC, et al. Postmenopausal osteoporosis. Nat Rev Dis Primers. 2016;2:16069. [3] Management of Osteoporosis in Postmenopausal Women: The 2021 Position Statement of The North American Menopause Society’’ Editorial Panel. Management of osteoporosis in postmenopausal women: the 2021 position statement of The North American Menopause Society. Menopause. 2021;28(9):973-997. [4] YU F, XIA W. The epidemiology of osteoporosis, associated fragility fractures, and management gap in China. Arch Osteoporos. 2019;14(1):32. [5] ZHU X, BAI W, ZHENG H. Twelve years of GWAS discoveries for osteoporosis and related traits: advances, challenges and applications. Bone Res. 2021;9(1):23. [6] ZEBAZE R, LIBANATI C, MCCLUNG MR, et al. Denosumab Reduces Cortical Porosity of the Proximal Femoral Shaft in Postmenopausal Women With Osteoporosis. J Bone Miner Res. 2016;31(10):1827-1834. [7] CHAVASSIEUX P, CHAPURLAT R, PORTERO-MUZY N, et al. Bone-Forming and Antiresorptive Effects of Romosozumab in Postmenopausal Women With Osteoporosis: Bone Histomorphometry and Microcomputed Tomography Analysis After 2 and 12 Months of Treatment. J Bone Miner Res. 2019;34(9):1597-1608. [8] LOTINUN S, KIVIRANTA R, MATSUBARA T, et al. Osteoclast-specific cathepsin K deletion stimulates S1P-dependent bone formation. J Clin Invest. 2013;123(2):666-681. [9] KRAENZLIN ME, MEIER C. Parathyroid hormone analogues in the treatment of osteoporosis. Nat Rev Endocrinol. 2011;7(11):647-656. [10] REID IR. Short-term and long-term effects of osteoporosis therapies. Nat Rev Endocrinol. 2015; 11(7):418-428. [11] WHITAKER M, GUO J, KEHOE T, et al. Bisphosphonates for osteoporosis--where do we go from here? N Engl J Med. 2012;366(22):2048-2051. [12] FENG X, MCDONALD JM. Disorders of bone remodeling. Annu Rev Pathol. 2011;6:121-145. [13] CHAKRABORTY S, KUBATZKY KF, MITRA DK. An Update on Interleukin-9: From Its Cellular Source and Signal Transduction to Its Role in Immunopathogenesis. Int J Mol Sci. 2019;20(9):2113. [14] GOSWAMI R, KAPLAN MH. A brief history of IL-9. J Immunol. 2011;186(6):3283-3288. [15] NOELLE RJ, NOWAK EC. Cellular sources and immune functions of interleukin-9. Nat Rev Immunol. 2010;10(10):683-687. [16] GENG W, ZHANG W, MA J. IL-9 exhibits elevated expression in osteonecrosis of femoral head patients and promotes cartilage degradation through activation of JAK-STAT signaling in vitro. Int Immunopharmacol. 2018;60:228-234. [17] ZHENG Y, HE Y, XIAO M, et al. Interleukin 9 prevents immune thrombocytopenia in mice via JAK/STAT5 signaling. Exp Cell Res. 2020; 88(1):111801. [18] 邹旺辉,钱楠楠,张萌,等.间充质干细胞临床前研究启示:间充质干细胞的细胞功能与JAK/STAT信号通路的关系[J]. 中国组织工程研究,2022,26(19):3048-3055. [19] SANPAOLO ER, ROTONDO C, CICI D, et al. JAK/STAT pathway and molecular mechanism in bone remodeling. Mol Biol Rep. 2020;47(11):9087-9096. [20] ZHOU S, DAI Q, HUANG X, et al. STAT3 is critical for skeletal development and bone homeostasis by regulating osteogenesis. Nat Commun. 2021;12(1):6891. [21] LEE J, SEONG S, KIM JH, et al. STAT5 is a key transcription factor for IL-3-mediated inhibition of RANKL-induced osteoclastogenesis. Sci Rep. 2016;6:30977. [22] ZHAO Y, XIE L. Unique bone marrow blood vessels couple angiogenesis and osteogenesis in bone homeostasis and diseases. Ann N Y Acad Sci. 2020;1474(1):5-14. [23] DATTA HK, NG WF, WALKER JA, et al. The cell biology of bone metabolism. J Clin Pathol. 2008; 61(5):577-587. [24] KATSIMBRI P. The biology of normal bone remodelling. Eur J Cancer Care (Engl). 2017;26(6). doi: 10.1111/ecc.12740. [25] RAGGATT LJ, PARTRIDGE NC. Cellular and molecular mechanisms of bone remodeling. J Biol Chem. 2010;285(33):25103-25108. [26] SIDDIQUI JA, PARTRIDGE NC. Physiological Bone Remodeling: Systemic Regulation and Growth Factor Involvement. Physiology (Bethesda). 2016;31(3):233-245. [27] BATOON L, MILLARD SM, RAGGATT LJ, et al. Osteal macrophages support osteoclast-mediated resorption and contribute to bone pathology in a postmenopausal osteoporosis mouse model. J Bone Miner Res. 2021; 36(11):2214-2228. [28] MCNAMARA LM. Osteocytes and Estrogen Deficiency. Curr Osteoporos Rep. 2021;19(6):592-603. [29] FöGER-SAMWALD U, KERSCHAN-SCHINDL K, BUTYLINA M, et al. Age Related Osteoporosis: Targeting Cellular Senescence. Int J Mol Sci. 2022;23(5):2701. [30] SCHETT G. Effects of inflammatory and anti-inflammatory cytokines on the bone. Eur J Clin Invest. 2011;41(12):1361-1366. [31] ZUPAN J, JERAS M, MARC J. Osteoimmunology and the influence of pro-inflammatory cytokines on osteoclasts. Biochem Med (Zagreb). 2013;23(1):43-63. [32] RAUBER S, LUBER M, WEBER S, et al. Resolution of inflammation by interleukin-9-producing type 2 innate lymphoid cells. Nat Med. 2017;23(8):938-944. [33] KAR S, GUPTA R, MALHOTRA R, et al. Interleukin-9 Facilitates Osteoclastogenesis in Rheumatoid Arthritis. Int J Mol Sci. 2021;22(19):10397. [34] CHAKRABORTY S, SCHNEIDER J, MITRA DK, et al. Mechanistic insight of interleukin-9 induced osteoclastogenesis. Immunology. 2023;169(3):309-322. |
| [1] | Chen Kaijia, Liu Jingyun, Cao Ning, Sun Jianbo, Zhou Yan, Mei Jianguo, Ren Qiang. Application and prospect of tissue engineering in treatment of osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1450-1456. |
| [2] | Guo Sutong, Feng Dehong, Guo Yu, Wang Ling, Ding Yujian, Liu Yi, Qian Zhengying, Li Mingyang. Construction and finite element analysis of normal and osteoporotic hip models [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1342-1346. |
| [3] | Zhang Xiaoyun, Liu Hua, Chai Yuan, Chen Feng, Zeng Hao, Gao Zhengang, Huang Yourong. Effect of Yishen Gushu Formula on bone metabolic markers and clinical efficacyn in patients with osteoporosis of kidney deficiency and blood stasis type [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1155-1160. |
| [4] | Dai Yuexing, Zheng Liqin, Wu Minhui, Li Zhihong, Li Shaobin, Zheng Desheng, Lin Ziling. Effect of vessel number on computational fluid dynamics in vascular networks [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1206-1210. |
| [5] | Pan Xiaolong, Fan Feiyan, Ying Chunmiao, Liu Feixiang, Zhang Yunke. Effect and mechanism of traditional Chinese medicine on inhibiting the aging of mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1091-1098. |
| [6] | Ma Shuwei, He Sheng, Han Bing, Zhang Liaoyun. Exosomes derived from mesenchymal stem cells in treatment of animals with acute liver failure: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1137-1142. |
| [7] | Feng Ruiqin, Han Na, Zhang Meng, Gu Xinyi, Zhang Fengshi. Combination of 1% platelet-rich plasma and bone marrow mesenchymal stem cells improves the recovery of peripheral nerve injury [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 985-992. |
| [8] | Qiu Xiaoyan, Li Bixin, Li Jingdi, Fan Chuiqin, Ma Lian, Wang Hongwu. Differentiation of insulin-producing cells from human umbilical cord mesenchymal stem cells infected by MAFA-PDX1 overexpressed lentivirus [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1000-1006. |
| [9] | Liu Qiwei, Zhang Junhui, Yang Yuan, Wang Jinjuan. Role and mechanism of umbilical cord mesenchymal stem cells on polycystic ovary syndrome [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1015-1020. |
| [10] | Zhang Min, Peng Jing, Zhang Qiang, Chen Dewang. Mechanical properties of L3/4 laminar decompression and intervertebral fusion in elderly osteoporosis patients analyzed by finite element method [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 847-851. |
| [11] | Xue Xiaofeng, Wei Yongkang, Qiao Xiaohong, Du Yuyong, Niu Jianjun, Ren Lixin, Yang Huifeng, Zhang Zhimin, Guo Yuan, Chen Weiyi. Finite element analysis of osteoporosis in proximal femur after cannulated screw fixation for femoral neck fracture [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 862-867. |
| [12] | Kaiyisaier•Abudukelimu, Maimaitimin•Abulimiti, Li Lei, Yang Xiaokai, Zhang Yukun, Liu Shuai. Effect of lumbar CT values in the diagnosis of osteoporosis in women patients with lumbar degenerative diseases [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 945-949. |
| [13] | Wang Liping, Lian Tianxing, Hu Yongrong, Yang Hongsheng, Zeng Zhimou, Liu Hao, Qu Bo. HU value of chest CT vertebral body in the opportunistic screening of type 2 diabetes mellitus osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 950-954. |
| [14] | Zhang Kefan, Shi Hui. Research status and application prospect of cytokine therapy for osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 961-967. |
| [15] | Yu Zhaoyu, Tan Lixin, Sun Kai, Lu Yao, Li Yong. Meta-analysis of cement-augmented pedicle screw for thoracolumbar degenerative diseases with osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 813-820. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||