Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (12): 1938-1943.doi: 10.12307/2023.037
Previous Articles Next Articles
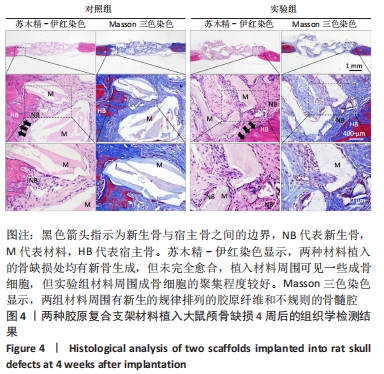
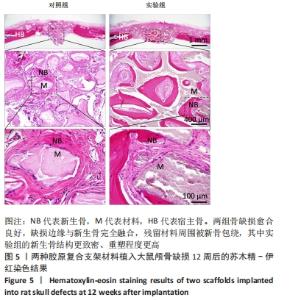
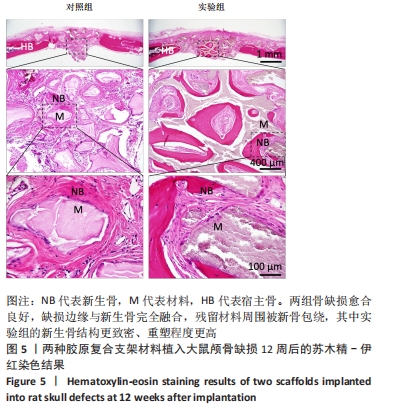
Calcined antler cancellous bone/collagen composite scaffolds promote bone defect repair
Zhou Yingying1, Zhang Xuehui1, 2
- 1Institute of Medical Technology, Peking University Health Science Center, Beijing 100191, China; 2Department of Dental Materials, Peking University Hospital of Stomatology, Beijing 100081, China
-
Received:2021-11-01Accepted:2022-02-08Online:2023-04-28Published:2022-07-30 -
Contact:Zhang Xuehui, Associate professor, Institute of Medical Technology, Peking University Health Science Center, Beijing 100191, China; Department of Dental Materials, Peking University Hospital of Stomatology, Beijing 100081, China -
About author:Zhou Yingying, Master candidate, Institute of Medical Technology, Peking University Health Science Center, Beijing 100191, China -
Supported by:Sub-Project of National Key Research and Development Program of China, No. 2018YFC1105303 (to ZXH)
CLC Number:
Cite this article
Zhou Yingying, Zhang Xuehui. Calcined antler cancellous bone/collagen composite scaffolds promote bone defect repair[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(12): 1938-1943.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
| [1] WANG W, YEUNG KWK. Bone grafts and biomaterials substitutes for bone defect repair: A review. Bioact Mater. 2017;2(4):224-247. [2] JUSTYNA W. Biomaterials for craniofacial bone regeneration. Dent Clin North Am. 2017;61(4):835-856. [3] TURNBULL G, CLARKE J, PICARD F, et al. 3D bioactive composite scaffolds for bone tissue engineering. Bioact Mater. 2018;3(3):278-314. [4] DEWEY MJ, HARLEY BAC. Biomaterial design strategies to address obstacles in craniomaxillofacial bone repair. RSC Adv. 2021;11(29): 17809-17827. [5] WANG D, LIU Y, LIU Y, et al. A dual functional bone-defect-filling material with sequential antibacterial and osteoinductive properties for infected bone defect repair. J Biomed Mater Res. 2019;107A:2360-2370. [6] ZHANG H, HE X, ZHANG Y, et al. Shapable bulk agarose-gelatine-hydroxyapatite-minocycline nanocomposite fabricated using a mineralizing system aided with electrophoresis for bone tissue regeneration. Biomed Mater. 2021;16(3):035024. [7] WONG RWK, RABIE ABM. Effect of Bio-Oss® Collagen and Collagen Matrix on Bone Formation. Open Biomed Eng J. 2010;4:71-76. [8] ARAUJO MG, LINDHE J. Ridge preservation with the use of Bio-Oss® collagen : A 6-month study in the dog. Clin Oral Impl Res. 2009;20:433-440. [9] FAN Q, ZENG H, FAN W, et al. Ridge preservation of a novel extraction socket applying Bio-Oss collagen : An experimental study in dogs. J Dent Sci. 2021;16(3):831-839. [10] MENG S, ZHANG X, XU M, et al. Effects of deer age on the physicochemical properties of deproteinized antler cancellous bone: An approach to optimize osteoconductivity of bone graft. Biomed Mater. 2015;10(3):35006. [11] ZHANG X, CAI Q, LIU H, et al. Osteoconductive effectiveness of bone graft derived from antler cancellous bone: An experimental study in the rabbit mandible defect model. Int J Oral Maxillofac Surg. 2012;41(11): 1330-1337. [12] 彭晖,张学慧.煅烧鹿角松质骨在骨缺损修复过程中的早期血管化[J].中国组织工程研究,2018,22(18):2807-2812. [13] ZHANG X, XU M, SONG L, et al. Effects of compatibility of deproteinized antler cancellous bone with various bioactive factors on their osteogenic potential. Biomaterials. 2013;34(36):9103-9114. [14] PATNTIRAPONG S, JANVIKUL W, THEERATHANAGORN T, et al. Osteoinduction of stem cells by collagen peptide-immobilized hydrolyzed poly(butylene succinate)/β-tricalcium phosphate scaffold for bone tissue engineering. J Biomater Appl. 2017;31(6):859-870. [15] YU L, WEI M. Biomineralization of collagen-based materials for hard tissue repair. Int J Mol Sci. 2021;22(2):944. [16] CARVALHO RG, ALVAREZ MMP, DE SÁ OLIVEIRA T, et al. The interaction of sodium trimetaphosphate with collagen I induces conformational change and mineralization that prevents collagenase proteolytic attack. Dent Mater. 2020;36(6):e184-e193. [17] MALCOR JD, BAX D, HAMAIA SW, et al. The synthesis and coupling of photoreactive collagen-based peptides to restore integrin reactivity to an inert substrate, chemically-crosslinked collagen. Biomaterials. 2016;85:65-77. [18] KACZMAREK B, SIONKOWSKA A, KOZLOWSKA J, et al. New composite materials prepared by calcium phosphate precipitation in chitosan/collagen/hyaluronic acid sponge cross-linked by EDC/NHS. Int J Biol Macromol. 2018;107:247-253. [19] ZHANG D, WU X, CHEN J, et al. The development of collagen based composite scaffolds for bone regeneration. Bioact Mater. 2018;3(1): 129-138. [20] KASHTE S, JAISWAL AK, KADAM S. Artificial Bone via Bone Tissue Engineering: Current Scenario and Challenges. Tissue Eng Regen Med. 2017;14(1):1-14. [21] PILLIAR RM, KANDEL RA, GRYNPAS MD, et al. Calcium polyphosphate particulates for bone void filler applications. J Biomed Mater Res Part B. 2017;105B:874-884. [22] BÉDUER A, BONINI F, VERHEYEN CA, et al. An Injectable Meta-Biomaterial: From Design and Simulation to In Vivo Shaping and Tissue induction. Adv Mater. 2021;33:2102350. [23] HERFORD AS, NGUYEN K. Complex Bone Augmentation in Alveolar Ridge Defects. Oral Maxillofac Surg Clin North Am. 2015;27(2):227-244. [24] SAITO M, MARUMO K. Collagen cross-links as a determinant of bone quality: a possible explanation for bone fragility in aging, osteoporosis, and diabetes mellitus. Osteoporos Int. 2010;21(2):195-214. [25] SAITO M, MARUMO K. Effects of Collagen Crosslinking on Bone Material Properties in Health and Disease. Calcif Tissue Int. 2015;97(3):242-261. [26] 王迎军,杨春蓉,汪凌云.EDC/NHS交联对胶原物理化学性能的影响[J].华南理工大学学报,2007,35(12):66-70. [27] GRABSKA-ZIELIŃSKA S, SIONKOWSKA A, CARVALHO Â, et al. Biomaterials with potential use in bone tissue regeneration-collagen/chitosan/silk fibroin scaffolds cross-linked by EDC/NHS. Materials. 2021; 14(5):1-21. [28] NONG LM, ZHOU D, ZHENG D, et al. The effect of different cross-linking conditions of EDC/NHS on type II collagen scaffolds: an in vitro evaluation. Cell Tissue Bank. 2019;20(4):557-568. [29] ZHANG W, LIU Y, ZHANG H. Extracellular matrix: an important regulator of cell functions and skeletal muscle development. Cell Biosci. 2021; 11(1):65. [30] FATTAHI R, MOHEBICHAMKHORAMI F, TAGHIPOUR N, et al. The effect of extracellular matrix remodeling on material-based strategies for bone regeneration: Review article. Tissue Cell. 2022;76:101748. [31] LIN X, PATIL S, GAO YG, et al. The Bone Extracellular Matrix in Bone Formation and Regeneration. Front Pharmacol. 2020;11:757. [32] ZHU G, ZHANG T, CHEN M, et al. Bone physiological microenvironment and healing mechanism: Basis for future bone-tissue engineering scaffolds. Bioact Mater. 2021;6(11):4110-4140. [33] JIANG S, WANG M, HE J. A review of biomimetic scaffolds for bone regeneration: Toward a cell-free strategy. Bioeng Transl Med. 2020;6(2): e10206. [34] YU L, CAI Y, WANG H, et al. Biomimetic bone regeneration using angle-ply collagen membrane-supported cell sheets subjected to mechanical conditioning. Acta Biomater. 2020;112:75-86. [35] WANG T, LI Q, ZHANG G, et al. Comparative evaluation of a biomimic collagen/hydroxyapatite/β-tricaleium phosphate scaffold in alveolar ridge preservation with Bio-Oss Collagen. Front Mater Sci. 2016;10(2): 122-133. [36] BEKETOV EE, ISAEVA EV, YAKOVLEVA ND, et al. Bioprinting of Cartilage with Bioink Based on High-Concentration Collagen and Chondrocytes. Int J Mol Sci. 2021;22(21):11351. [37] SARIAN MN, IQBAL N, SOTOUDEHBAGHA P, et al. Potential bioactive coating system for high-performance absorbable magnesium bone implants. Bioact Mater. 2021;12:42-63. [38] ZHA K, TIAN Y, PANAYI AC, et al. Recent Advances in Enhancement Strategies for Osteogenic Differentiation of Mesenchymal Stem Cells in Bone Tissue Engineering. Front Cell Dev Biol. 2022;10:824812. [39] SBRICOLI L, GUAZZO R, ANNUNZIATA M, et al. Selection of Collagen Membranes for Bone Regeneration: A Literature Review. Materials (Basel). 2020;13(3):786. [40] 孟松,张学慧,邓旭亮.煅烧鹿角松质骨浸提液对BMSCs成骨分化的影响[J].现代口腔医学杂志,2015,29(3):129-132. [41] PARK JW, HANAWA T, CHUNG JH. The relative effects of Ca and Mg ions on MSC osteogenesis in the surface modification of microrough Ti implants. Int J Nanomedicine. 2019;14:5697-5711. [42] QI T, WENG J, YU F, et al. Insights into the Role of Magnesium Ions in Affecting Osteogenic Differentiation of Mesenchymal Stem Cells. Biol Trace Elem Res. 2021;199(2):559-567. [43] MEHTA KJ. Role of iron and iron-related proteins in mesenchymal stem cells: Cellular and clinical aspects. J Cell Physiol. 2021;236(10):7266-7289. |
| [1] | Yang Yitian, Wang Lu, Yao Wei, Zhao Bin. Application of the interaction between biological scaffolds and macrophages in bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1071-1079. |
| [2] | Li Cheng, Zheng Guoshuang, Kuai Xiandong, Yu Weiting. Alginate scaffold in articular cartilage repair [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1080-1088. |
| [3] | Tang Haotian, Liao Rongdong, Tian Jing. Application and design of piezoelectric materials for bone defect repair [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1117-1125. |
| [4] | Xu Yan, Li Ping, Lai Chunhua, Zhu Peijun, Yang Shuo, Xu Shulan. Piezoelectric materials for vascularized bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1126-1132. |
| [5] | Li Xiaoyin, Yang Xiaoqing, Chen Shulian, Li Zhengchao, Wang Ziqi, Song Zhen, Zhu Daren, Chen Xuyi. Collagen/silk fibroin scaffold combined with neural stem cells in the treatment of traumatic spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 890-896. |
| [6] | Zhang Min, Zhang Xiaoming, Liu Tongbin. Application potential of naringin in bone tissue regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 787-792. |
| [7] | Zhang Hui, Wang Jiayang, Wang Qian, Gan Hongquan, Wang Zhiqiang. Effects of hyaluronic acid combined with domestic porous tantalum on chondrocyte function under the dynamic environment [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 339-345. |
| [8] | Liu Huan, Li Han, Ma Yunhao, Zhong Weijian, Ma Guowu. Osteogenic capacity of partially demineralized dentin particles in the maxillary sinus lift [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 354-359. |
| [9] | Zong Mingrui, Liu Haiyan, Li Bing, Wu Xiuping. Application of carboxymethyl chitosan in tissue engineering of stomatology [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 447-452. |
| [10] | Niu Zihan, Yu Yang, Ai Jiang, Bu Panpan, Li Wenbo, Suriye·Reheman, Ma Shaolin. Total flavonoids of Hippophae rhamnoides L. interfere with the regression of hypertrophic scar tissue blocks in a rabbit ear model [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 258-263. |
| [11] | Zhang Jie, Tian Ai. Advances in the signaling pathway of M2 macrophages involved in bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 314-321. |
| [12] | Wang Xu, Yang Tengyun, Xiong Bohan, Zhang Yaozhang, Lu Xiaojun, Long Dan, Zhao Daohong. Regeneration mechanism and problems of tissue engineering in rotator cuff tendon-bone healing [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(18): 2928-2934. |
| [13] | Liang Weiye, Duan Qinghong. Correlation between femur bone morphogenetic protein 2 expression and bone fluoride content in fluorosis rabbits [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(17): 2675-2680. |
| [14] | Zhang Chuhan, Zhang Dongmin, Xu Wenan. Cell co-culture system of dental pulp regenerative tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(15): 2379-2384. |
| [15] | Liao Jianzhao, Yang Nan, Zhou Yi, Xu Hang, Xia Tian, Song Shilei, Zeng Qi, Chen Yueping. Protective effect of astragaloside IV against inflammatory injury in chondrocytes [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(14): 2158-2163. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||