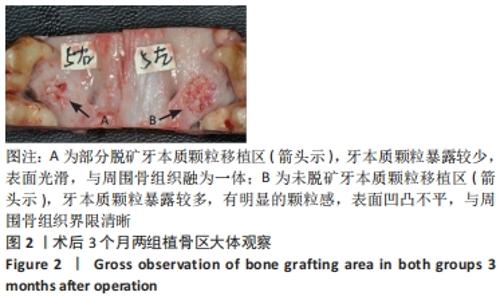
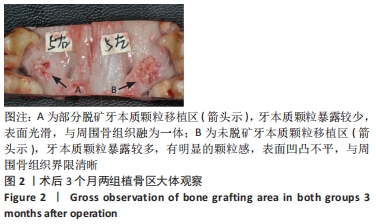
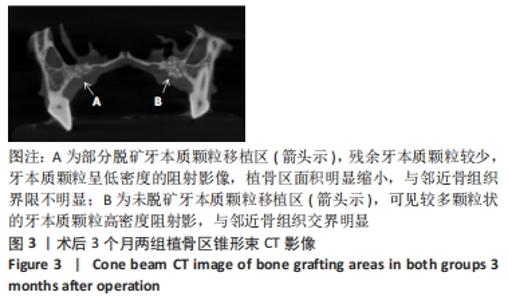
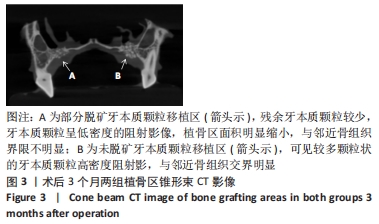
Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (3): 354-359.doi: 10.12307/2023.050
Previous Articles Next Articles
Osteogenic capacity of partially demineralized dentin particles in the maxillary sinus lift
Liu Huan, Li Han, Ma Yunhao, Zhong Weijian, Ma Guowu
- Stomatological Hospital of Stomatology College of Dalian Medical University, Dalian 116023, Liaoning Province, China
-
Received:2021-09-26Accepted:2021-11-15Online:2023-01-28Published:2022-05-20 -
Contact:Zhong Weijian, Associate professor, Master’s supervisor, Stomatological Hospital of Stomatology College of Dalian Medical University,Dalian 116023,Liaoning Province, China -
About author:Liu Huan, Master candidate, Stomatological Hospital of Stomatology College of Dalian Medical University, Dalian 116023, Liaoning Province, China -
Supported by:the Natural Science Foundation of Liaoning Province, No. 2015020313 (to ZWJ)
CLC Number:
Cite this article
Liu Huan, Li Han, Ma Yunhao, Zhong Weijian, Ma Guowu. Osteogenic capacity of partially demineralized dentin particles in the maxillary sinus lift[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 354-359.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
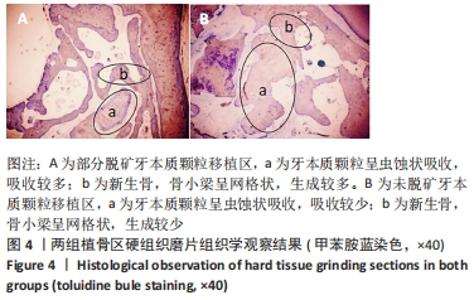
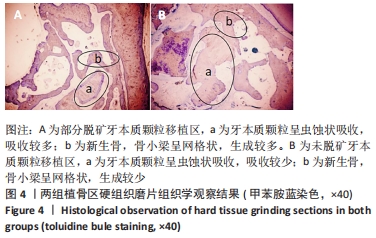
实验组、对照组植骨区平均密度分别为(1 043.95±123.09),(1 387.77±194.96) HU,组间比较差异有显著性意义(P < 0.05);实验组、对照组植骨区平均面积分别为(16.38±2.91),(26.48±3.44) mm2,组间比较差异有显著性意义(P < 0.05),说明实验组牙本质颗粒较对照组吸收快。 2.4 两组植骨区组织形态学观察结果 由于切片甲苯胺蓝染色后放置时间过长,有些褪色,但并不影响结果观察。对硬组织磨片的观察可见,两组植骨区的牙本质颗粒均呈虫蚀样吸收,实验组吸收程度较对照组明显,两组牙本质颗粒周围均可见新生的编织骨,呈网格状,新生骨组织包绕牙本质颗粒并与基骨紧密连接,实验组新生骨多于对照组,对照组牙本质颗粒周围有较多的纤维组织,两组植骨区均未见炎症细胞浸润,见图4。 "

2.5 两组植骨区组织学测量和统计学分析 术后3个月,实验组和对照组的新骨生成率分别为(41.91±4.66)%和(30.80±5.31)%,组间比较差异有显著性意义(P < 0.05),说明在相同时间内,部分脱矿牙本质颗粒的新骨生成量多于未脱矿牙本质颗粒。术后3个月,实验组和对照组的牙本质颗粒所占面积比率分别为(12.41±6.76)%和(20.66±2.34)%,组间比较差异有显著性意义(P < 0.05),说明未脱矿牙本质颗粒吸收较慢,有利于维持空间。 2.6 牙本质颗粒的组织相容性 由动物实验的大体观察与组织学观察结果可知,部分脱矿牙本质颗粒与未脱矿牙本质颗粒均具有良好的组织相容性。"

| [1] BEAMAN FD, BANCROFT LW, PETERSON JJ, et al. Bone graft materials and synthetic substitutes. Radiol Clin North Am. 2006;44(3):451-461. [2] GARCIA-JÚNIOR IR, SOUZA FÁ, FIGUEIREDO AAS, et al. Maxillary Alveolar Ridge Atrophy Reconstructed With Autogenous Bone Graft Harvested From the Proximal Ulna. J Craniofac Surg. 2018;29(8):2304-2306. [3] SAKKAS A, WILDE F, HEUFELDER M, et al. Autogenous bone grafts in oral implantology-is it still a “gold standard”? A consecutive review of 279 patients with 456 clinical procedures. Int J Implant Dent. 2017; 3(1):23. [4] 王宁,崔婷婷,李永奇,等.自体块状皮质骨修复种植区颌骨缺损[J].中国组织工程研究,2020,24(17):2675-2679. [5] ROGERS GF, GREENE AK. Autogenous bone graft: basic science and clinical implications. J Craniofac Surg. 2012;23(1):323-327. [6] YOSHIDA T, VIVATBUTSIRI P, MORRISS-KAY G, et al. Cell lineage in mammalian craniofacial mesenchyme. Mech Dev. 2008;125(9-10): 797-808. [7] KABIR MA, MURATA M, AKAZAWA T, et al. Evaluation of perforated demineralized dentin scaffold on bone regeneration in critical-size sheep iliac defects. Clin Oral Implants Res. 2017;28(11):e227-e235. [8] LEI G, WANG Y, YU Y, et al. Dentin-Derived Inorganic Minerals Promote the Osteogenesis of Bone Marrow-Derived Mesenchymal Stem Cells: Potential Applications for Bone Regeneration. Stem Cells Int. 2020;(2):1-16. [9] YEOMANS JD, URIST MR. Bone induction by decalcified dentine implanted into oral, osseous and muscle tissues. Arch Oral Biol. 1967; 12(8):999-1008. [10] UM IW, KU JK, LEE BK, et al. Postulated release profile of recombinant human bone morphogenetic protein-2 (rhBMP-2) from demineralized dentin matrix. J Korean Assoc Oral Maxillofac Surg. 2019;45(3):123-128. [11] ZHANG S, LI X, QI Y, et al. Comparison of Autogenous Tooth Materials and Other Bone Grafts. Tissue Eng Regen Med. 2021;18(3):327-341. [12] ATIYA BK, SHANMUHASUNTHARAM P, HUAT S, et al. Liquid nitrogen-treated autogenous dentin as bone substitute: an experimental study in a rabbit model. Int J Oral Maxillofac Implants. 2014;29(2):e165-170. [13] REIS-FILHO CR, SILVA ER, MARTINS AB, et al. Demineralised human dentine matrix stimulates the expression of VEGF and accelerates the bone repair in tooth sockets of rats. Arch Oral Biol. 2012;57(5):469-476. [14] 肖闻澜,胡琛,荣圣安,等.自体牙本质作为骨移植材料的临床应用进展[J].口腔疾病防治,2020(6):394-398. [15] KOGA T, MINAMIZATO T, KAWAI Y, et al. Bone Regeneration Using Dentin Matrix Depends on the Degree of Demineralization and Particle Size. PLoS One. 2016;11(1):e0147235. [16] BALDWIN P, LI DJ, AUSTON DA, et al. Autograft, allograft, and bone graft substitutes: clinical evidence and indications for use in the setting of orthopaedic trauma surgery. J Orthop Trauma. 2019;33(4):203-213. [17] KIM Y, NOWZARI H, RICH SK. Risk of prion disease transmission through bovine-derived bone substitutes: a systematic review. Clin Implant Dent Relat Res. 2013;15(5):645-653. [18] TAYLOR JC, CUFF SE, LEGER JP, et al. In vitro osteoclast resorption of bone substitute biomaterials used for implant site augmentation: a pilot study. Int J Oral Maxillofac Implants. 2002;17(3):321-330. [19] GIANNOUDIS P, DINOPOULOS H, TSIRIDIS E. Bone Substitutes: An Update. Injury. 2005;36 Suppl 3(3):S20-27. [20] KIM YK, KIM SG, YUN PY, et al. Autogenous teeth used for bone grafting: A comparison with traditional grafting materials. Oral Surg Oral Med Oral Pathol Oral Radiol. 2014;117:39-45. [21] KOZUMA W, KON K, KAWAKAMI S, et al. Osteoconductive potential of a hydroxyapatite fiber material with magnesium: In vitro and in vivo studies. Dent Mater J. 2019;38:771-778. [22] MURATA M, AKAZAWA T, MITSUGI M, et al. Autograft of Dentin Materials for Bone Regeneration. Advances in Biomaterials Science and Biomedical Applications. 2013:391-403. [23] Um IW. Demineralized Dentin Matrix (DDM) As a Carrier for Recombinant Human Bone Morphogenetic Proteins (rhBMP-2). Adv Exp Med Biol. 2018;1077:487-499. [24] Um IW, Ku JK, Kim YK, et al. Histological Review of Demineralized Dentin Matrix as a Carrier of rhBMP-2. Tissue Eng Part B Rev. 2020; 26(3):284-293. [25] BESSHO K, TAGAWA T, MURATA M. Purification of bone morphogenetic protein derived from bovine bone matrix. Biochem Biophys Res Commun. 1989;165(2):595-601. [26] ZHANG S, LI X, QI Y, et al. Comparison of Autogenous Tooth Materials and Other Bone Grafts. Tissue Eng Regen Med. 2021;18(3):327-341. [27] SUN Y, LU Y, CHEN L, et al. DMP1 processing is essential to dentin and jaw formation. J Dent Res. 2011;90(5):619-624. [28] SINGH A, GILL G, KAUR H, et al. Role of osteopontin in bone remodeling and orthodontic tooth movement: a review. Prog Orthod. 2018;19(1):18. [29] KIM YK, KIM SG, BYEON JH, et al. Development of a novel bone grafting material using autogenous teeth. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010;109(4):496-503. [30] 靳夏莹,仲维剑,马国武.自体牙制成骨移植材料在上前牙即刻种植中的应用1例[J].口腔医学研究,2017(11):1228-1229. [31] 崔婷婷,寇霓,仲维剑,等.自体牙本质颗粒联合富血小板纤维蛋白在上颌窦提升同期种植中的应用[J]. 口腔医学研究,2018,34(5): 532-534. [32] 崔婷婷,邱泽文,邵阳,等.异种牙本质颗粒复合骨髓浓缩物在上颌窦提升中的成骨效应[J].中国组织工程研究,2018,22(30):4806-4811. [33] 赵彬彬,仲维剑,马国武.牙本质作为骨移植材料的研究进展[J].国际口腔医学杂志,2021,48(1):82-89. [34] 赵彬彬,邱泽文,马程辉,等.不同处理方法对未脱钙异种牙本质颗粒成骨性能的影响[J].中国组织工程研究,2019,23(26):4154-4159. [35] LI R, GUO W, YANG B, et al. Human treated dentin matrix as a natural scaffold for complete human dentin tissue regeneration.Biomater. 2011;32(20):4523-4538. [36] KIM YK, KIM SG, OH JS, et al. Analysis of the inorganic component of autogenous tooth bone graft material. J Nanosci Nanotechnol. 2011;11(8):7442-7445. [37] GALLER KM, BUCHALLA W, HILLER KA, et al. Influence of root canal disinfectants on growth factor release from dentin. J Endod. 2015; 41(3):363-368. [38] MATHEWS S, BHONDE R, GUPTA PK, et al. Novel biomimetic tripolymer scaffolds consisting of chitosan, collagen type 1, and hyaluronic acid for bone marrow-derived human mesenchymal stem cells-based bone tissue engineering. J Biomed Mater Res B Appl Biomater. 2014;102(8):1825-1834. [39] CHU C, DENG J, SUN X, et al. Collagen Membrane and Immune Response in Guided Bone Regeneration: Recent Progress and Perspectives. Tissue Eng Part B Rev. 2017;23(5):421-435. [40] REDDI AH. Bone matrix in the solid state:geometric infl uence on differentiation of fibroblasts. Adv Biol Med Phys. 1974;15:1-18. [41] GUO W, HE Y, ZHANG X, et al. The use of dentin matrix scaffold and dental follicle cells for dentin regeneration. Biomaterials. 2009;30(35): 6708-6723. [42] LI R, GUO W, YANG B, et al. Human treated dentin matrix as a natural scaffold for complete human dentin tissue regeneration. Biomaterials. 2011;32(20):4525-4538. [43] MINAMIZATO T, KOGA T, I T, et al. Clinical application of autogenous partially demineralized dentin matrix prepared immediately after extraction for alveolar bone regeneration in implant dentistry: a pilot study. Int J Oral Maxillofac Surg. 2018;47(1):125-132. |
| [1] | Yang Yufang, Yang Zhishan, Duan Mianmian, Liu Yiheng, Tang Zhenglong, Wang Yu. Application and prospects of erythropoietin in bone tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1443-1449. |
| [2] | Chen Kaijia, Liu Jingyun, Cao Ning, Sun Jianbo, Zhou Yan, Mei Jianguo, Ren Qiang. Application and prospect of tissue engineering in treatment of osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1450-1456. |
| [3] | Bai Chen, Yang Wenqian, Meng Zhichao, Wang Yuze. Strategies for repairing injured anterior cruciate ligament and promoting graft healing [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1457-1463. |
| [4] | Wang Menghan, Qi Han, Zhang Yuan, Chen Yanzhi. Three kinds of 3D printed models assisted in treatment of Robinson type II B2 clavicle fracture [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1403-1408. |
| [5] | Yang Cekai, Cai Zhuoyan, Chen Ming, Liu Hao, Weng Rui, Cui Jianchao, Zhang Shuncong, Yao Zhensong. Relationship between degeneration of paraspinal muscle and refractures in postmenopausal women treated by percutaneous vertebroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1414-1419. |
| [6] | Zhuang Xinyi, Peng Yuanhao, Yu Ting, Lyu Dongmei, Wen Xiujie, Cheng Qian. Cone-beam CT evaluation of bone mass in the external oblique line of the mandible in adolescents with different cervical vertebral bone ages [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1253-1258. |
| [7] | Xiaheida·Yilaerjiang, Nijiati·Tuerxun, Reyila·Kuerban, Baibujiafu·Yelisi, Chen Xin. Three-dimensional finite element analysis of the distribution pattern of stress in bone tissues with different characteristics [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1277-1282. |
| [8] | Lin Zeyu, Xu Lin. Research progress in gout-induced bone destruction mechanism [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1295-1300. |
| [9] | Zhang Xiaoyun, Liu Hua, Chai Yuan, Chen Feng, Zeng Hao, Gao Zhengang, Huang Yourong. Effect of Yishen Gushu Formula on bone metabolic markers and clinical efficacyn in patients with osteoporosis of kidney deficiency and blood stasis type [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1155-1160. |
| [10] | Cheng Jie, Wang Jihong, Zhang Pei. Functional exercise for tendon adhesion in a model of deep flexor tendon II injury of the third toe [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1161-1167. |
| [11] | Huang Xiarong, Hu Lizhi, Sun Guanghua, Peng Xinke, Liao Ying, Liao Yuan, Liu Jing, Yin Linwei, Zhong Peirui, Peng Ting, Zhou Jun, Qu Mengjian. Effect of electroacupuncture on the expression of P53 and P21 in articular cartilage and subchondral bone of aged rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1174-1179. |
| [12] | Dai Yuexing, Zheng Liqin, Wu Minhui, Li Zhihong, Li Shaobin, Zheng Desheng, Lin Ziling. Effect of vessel number on computational fluid dynamics in vascular networks [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1206-1210. |
| [13] | Wang Shanshan, Shu Qing, Tian Jun. Physical factors promote osteogenic differentiation of stem cells [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1083-1090. |
| [14] | Huang Peizhen, Dong Hang, Cai Qunbin, Lin Ziling, Huang Feng. Finite element analysis of anterograde and retrograde intramedullary nail for different areas of femoral shaft fractures [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 868-872. |
| [15] | Wang Tihui, Wang Xu, Wu Jinqing, Chen Jiliang, Wang Xiaolu, Miao Juan. Application of three-dimensional simulated osteotomy of the distal femur in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 905-910. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||