Chinese Journal of Tissue Engineering Research ›› 2017, Vol. 21 ›› Issue (26): 4210-4216.doi: 10.3969/j.issn.2095-4344.2017.26.019
Previous Articles Next Articles
The local application of recombinant human parathyroid hormone (1-34) promotes osseointegration of an immediate implant
- Department of Prosthodontics, the Third Hospital of Hebei Medical University, Shijiazhuang 050000, Hebei Province, China
-
Received:2017-04-19Online:2017-09-18Published:2017-09-28 -
Contact:Hou Xiao-wei, Professor, Department of Prosthodontics, the Third Hospital of Hebei Medical University, Shijiazhuang 050000, Hebei Province, China -
About author:Sun Zhi-hui, Studying for master’s degree, Department of Prosthodontics, the Third Hospital of Hebei Medical University, Shijiazhuang 050000, Hebei Province, China
CLC Number:
Cite this article
Sun Zhi-hui, Zheng Yu, Wang Li-jie, Fan Shi-feng, Hou Xiao-wei.
share this article
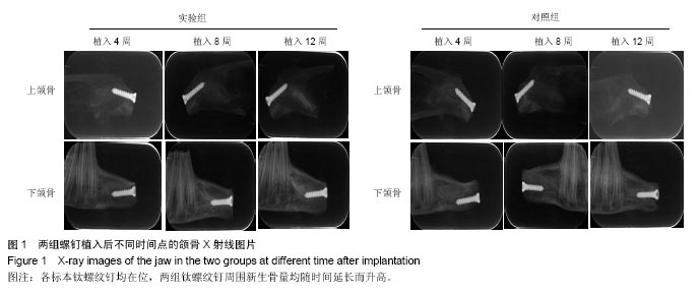
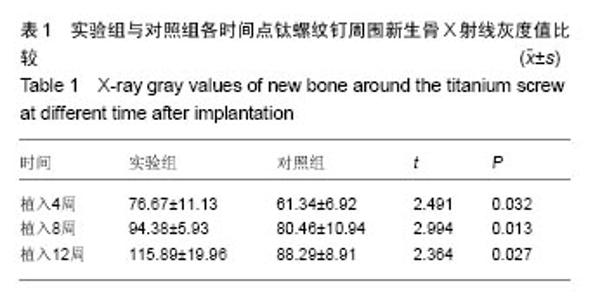
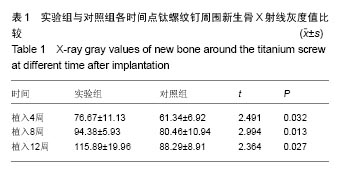
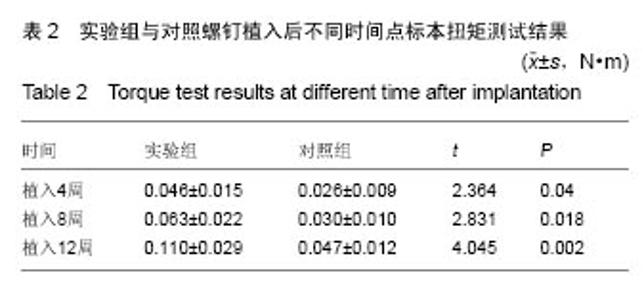
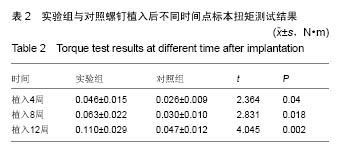
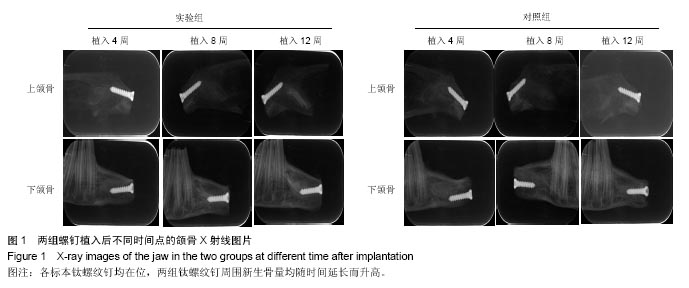
2.1 实验动物数量分析 9只兔均进入结果分析。 2.2 大体观察结果 所有术后实验动物均健康无死亡,术后1周创口愈合良好。定期检查见各时段植区周围牙龈无红肿、无破溃、无溢脓炎症表现。 9只实验动物共得36个标本,所有标本钛螺纹钉均无脱落。实验组钛螺纹钉未见松动现象,钛螺纹钉周围骨组织紧密包绕,未见纤维组织长入。对照组植入4周,部分钛螺纹钉松动,钛螺纹钉龈方周围存在角形骨缺损;植入8周,钛螺纹钉松动度有好转,骨缺损面积减小,植入12周,钛螺纹钉顶端周围有骨组织包绕。 2.3 X射线观察及骨密度分析结果 X射线观察结果:X射线片可见各标本钛螺纹钉均在位,两组钛螺纹钉周围新生骨量均随时间延长而升高。植入后4周时,两组拔牙窝内异种冻干骨与周围骨组织均无明显边界,实验组可见钛螺纹钉周围新生骨影像呈云雾状,包绕钛螺纹钉整体,外周皮质骨密度无降低;对照组钛螺纹钉周围较大透射区,新生骨云雾状不明显且钛螺纹钉顶端见骨缺损区。植入后8周时,两组钛螺纹钉-骨界面密度较4周均有明显升高,实验组新生骨量增多,密度与正常骨密度接近,新生骨界限不明显;对照组钛螺纹钉顶端仍可见透射影像,新生骨密度较低且界限清晰。植入后12周,实验组可见新生骨组织紧密包绕在螺纹钉周围,密度较正常骨密度稍高;对照组龈方透射影像基本消失,新生骨密度较植入8周时增加但仍低于正常骨组织,新生骨界限仍可分辨,见图1。 骨密度结果分析:实验组各时间点钛螺纹钉周围骨组织的灰度值均高于对照组(P < 0.05),见表1。"
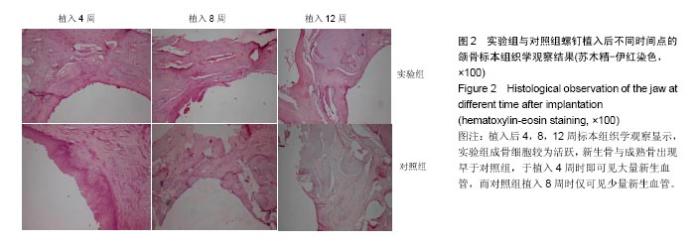
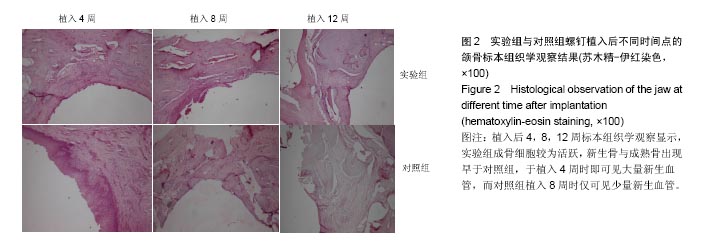
2.5 组织学观察结果 植入后4,8,12周标本组织学观察显示,实验组成骨细胞较为活跃,新生骨与成熟骨出现较早。 实验组:植入后4周,可见成骨细胞活跃,在新生骨小梁周围紧密排列,钛螺纹钉周围区域可见骨吸收陷窝及类骨质分泌,新生骨小梁呈片状分布,可见编织骨形成,视野内见丰富的新生血管。植入后8周,成骨细胞数量减少,骨细胞增多,破骨细胞几乎不可见,大量类骨质矿化为骨基质,骨小梁较4周排列密集、粗大,可见编织骨转变成板状新骨。植入后12周,可见骨细胞较多,排列紧密,骨小梁排列粗大致密,大量板状新骨形成,见图2。 对照组:植入后4周,见大量结缔组织细胞成分,成骨细胞量少,破骨细胞较多,但形成的骨吸收陷窝较少,类骨质分泌少,骨小梁几乎不可见,新生血管极其稀疏。植入后8周,可见成骨细胞较4周增多,破骨细胞减少,类骨质沉积较实验组低,新生骨小梁纤细、稀疏,新生血管较4周增多。植入后12周,骨细胞排列混杂,骨小梁较实验组纤细,骨成熟度较低,仅有少量板状新骨形成,见图2。"
| [1]Brennan-Calanan RM,Genco RJ,Wilding GE,et al. Osteoporosis and oral infection: Independent risk factors for oral bone loss.J Dent Res.2008;87(4):323-327.[2]Prank K,Nowlan SJ,Harms HM,et al.Time series prediction of plasma hormone concentration. Evidence for differences in predictability of parathyroid hormone secretion between osteoporoctic patients and normal controls.J Clin Invest.1995; 95(6):2910-2919.[3]Blind E,Raue F,Knappe V,et al.Cyclic AMP formation in rat bone and kidney cells is stimulated equally by parathyroid hormone-related protein (PTHrP) 1-34 and PTH 1-34. Exp Clin Endocrinol.1993;101(3):150-155.[4]四川美康医药软件研究开发有限公司.药物临床信息参考[M].成都:四川科学技术出版社,2007:1507-1508.[5]Yu XH,Wang LP,Jiang X,et al.Biomimetic CaP coating incorporated with parathyroid hormone improves the osseointegration of titanium implant.J Mater Sci Mater Med. 2012;23(9):2177-2186.[6]Brnemark PI,Hansson BO,Adell R,et al. Osseointegrated implants in the treatment of the edentulous jaw.Experience from a 10-year period.Scand J Plast Reconstr Surg Suppl. 1977;16:1-132.[7]Marquezan M,Osorio A,Sant’ Anna E,et al. Does bone mineral density influence the primary stability of dental implants? A systematic review.Clin Oral Implants Res.2012;23(7):767~774.[8]中华医学会骨质疏松和骨矿盐疾病分会.原发性骨质疏松症诊治指南(2011年)[J].中华骨质疏松和骨矿盐疾病杂志, 2011, 4(1):2-17.[9]Binte AR,Tanaka M,Kohno S,et al.Relationship between porotic changes in alveolar bone and spinal osteoporosis.J Dent Res.2007;86(1):52-57.[10]Khosla S,Westendorf JJ,Oursler MJ. Building bone to reverse osteoporosis and repair fractures.J Clin Invest. 2008;118(2): 421-428.[11]梁红.内源性及外源性甲状旁腺激素对小鼠拔牙创骨愈合的影响[D].南京医科大学,2010.[12]Tang ZL,Zhang WJ,Wang DX,et al.An experimental study addressing the promotion of mandibular defect repair through the intermittent subcutaneous injection of parathyroid hormone.J Oral Maxillofac Surg.2014;72(2):419-430.[13]Deshpande SS,Gallagher KK,Donneys A,et al.Parathyroid hormone therapy mollifies radiation-induced biomechanical degradation in murine distraction osteogenesis. Plast Reconstr Surg.2013;132(1):91-100.[14]Reynolds DG,Takahata M,Lerner AL,et al.Teriparatide therapy enhances devitalized femoral allograft osseointegration and biomechanics in a murine model. Bone.2011;48(3):562-570.[15]Hodsman AB,Bauer DC,Dempster DW,et al.Parathyroid hormone and teriparatide for the treatment of osteoporosis: a review of the evidence and suggested guidelines for its use. Endocr Rev.2005;26(5):688-703.[16]Jilka RL,Weinstein RS,Bellido T,et al.Increased bone formation by prevention of osteoblast apoptosis with parathyroid hormone.J Clin Invest.1999;104(4):439-446. [17]Chen HL,Demiralp B,Schneider A,et al.Parathyroid hormone and parathyroid hormone-related protein exert both pro- and anti-apoptotic effects in mesenchymal cells.J Biol Chem.2002; 277(22):19374-19381.[18]Dobnig H,Turner RT.Evidence that intermittent treatment with parathyroid hormone increase bone formation in adult rats by activation of bone lining cells. Endocrinology.1995;136(8): 3632-3638.[19]Gasser JA,Kneissel M,Thomsen JS,et al. PTH and interactions with bisphoshonates.J Musculoskelet Neuronal Interact.2000;1(1):53-56.[20]Hodsman AB,Steer BM.Early histomorphometric changes in response to parathyroid hormone therapy in osteoporosis: Evidence for de novo bone formation on quiescent cancellous surfaces.Bone.1993;14(3):523-527.[21]Jilka RL,O'Brien CA,Ali AA,et al.Intermittent PTH stimulates periosteal bone formation by actions on post-mitotic preosteoblasts.Bone.2009;44(2):275-286.[22]Rickard DJ,Wang FL,Rodriguez-Rojas AM,et al.Intermittent treatment with parathyroid hormone(PTH)as well as a non-peptide small molecule agonist of the PTH1 receptor inhibits adipocyte differentiation in human bone marrow stromal cells. Bone.2006;39(6):1361-1372. [23]唐雯菁,杜艳萍,洪维,等.甲状旁腺素对骨髓间充质干细胞增殖、分化和旁分泌功能的影响[J].中华骨质疏松和骨矿盐疾病杂志, 2014,7(1):42-47.[24]Frisch SM.cAMP takes controls.Nat Cell Biol. 2000;2(9): E167-168.[25]Drake MT,Srinivasan B,Mdder UI,et al.Effects of intermittent parathyroid hormone treatment on osteoprogenitor cells in postmenopausal women.Bone.2011;49(3):349-355.[26]Neer M,Slovik DM,Daly M,et al.Treatment of postmenopausal osteoporosis with daily parathyroid hormone plus calcitriol. Osteoporos Int.1993;3(1):204-205.[27]Burr DB,Hirano T,Turner CH,et al.Intermittently administered human parathyroid hormone (1-34) treatment increases intracortical bone turnover and porosity without reducing bone strength in the humerus of ovariectomized cynomolgous monkeys.J Bone Miner Res.2001;16(1):157-165.[28]Sato M.Westmore M,Ma YL,et al.Teriparatide [PTH(1-34)] strengthens the proximal femur of onariectomized nonhuman primates despite increasing porosity.J Bone Miner Res. 2004; 19(4):623-629.[29]Datta NS,Abou-Samra AB.PTH and PTHrP signaling in osteoblasts.Cell Signal.2009; 21(8):1245-1254.[30]卫红艳,朱梅.甲状旁腺素治疗骨质疏松研究进展[J].药品评价, 2013,10(5):40-44.[31]王晶晶,孟维艳,张喆,等.负载 PTH(1-34) 聚乳酸微球体外促成骨分化作用的研究[J].实用口腔医学杂志,2015,31(3):360-364.[32]于美娜.负载PTH(1-34)的温水凝胶的制备及细胞学研究[D].吉林大学,2013.[33]Valderrama P,Jung RE,Thoma DS,et al.Evaluation of parathyroid hormone bound to a synthetic matrix for guided bone regeneration around dental implants: A histomorphometric study in dogs.J Periodontol. 2010;81(5): 737-747.[34]Yu X,Wei M.Preparation and evaluation of parathyroid hormone incorporated CaP coating via a biomimetic method.J Biomed Mater Res B Appl Biomater.2011;97(2):345-354.[35]李德超,刘惠萍,李慕勤,等.具有微弧氧化-硅烷-褪黑素复合膜层钛合金种植体的体内骨结合[J].中国组织工程研究, 2016, 20(43):6438-6444.[36]Weng J,Wang M,Chen J.Plasma-sprayed calcium phosphate particles with high bioactivity and their use in bioactive scaffolds.Biomaterials.2002;23(13):2623-2629.[37]Milella E,Cosentino F,Licciulli A,et al.Preparation and characterisation of titania/hydroxyapatite composite coatings obtained by sol-gel process. Biomaterials. 2001;22(11): 1425-1431. [38]邓炜,王贻宁.仿生溶液生长法磷酸钙涂层种植体的研究进展[J].国外医学口腔医学分册,2001,28(2):76-78.[39]Junker R,Dimakis A,Thoneick M,et al.Effects of implant surface coatings and composition on bone integration: a systematic review.Clin Oral Implants Res. 2009;20(4): 185-206.[40]Luong LN,McFalls KM,Kohn DH.Gene delivery via DNA incorporation within a biomimetic apatite coating. Biomaterials. 2009;30(36):6996-7004.[41]Stigter M,Bezemer J,de Groot K,et al.Incorporation of different antibiotics into carbonated hydroxyapatite coatings on titanium implants, release and antibiotic efficacy.J Control Release.2004;99(1):127-137. [42]Liu Y,Li JP,Hunziker EB,et al.Incorporation of growth factors into medical devices via biomimetic coatings.Philos Trans A Math Phys Eng Sci.2006;364(1838):233-248.[43]Wang CX,Liu JJ,Xiao Y,et al.Study on preparation and activity of a novel recombinant human parathyroid hormone(1-34) analog with N-terminal Pro-Pro extension. Regul Pept.2007; 141(1-3):35-43. |
| [1] | Yao Xiaoling, Peng Jiancheng, Xu Yuerong, Yang Zhidong, Zhang Shuncong. Variable-angle zero-notch anterior interbody fusion system in the treatment of cervical spondylotic myelopathy: 30-month follow-up [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1377-1382. |
| [2] | Zhang Jinglin, Leng Min, Zhu Boheng, Wang Hong. Mechanism and application of stem cell-derived exosomes in promoting diabetic wound healing [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1113-1118. |
| [3] | An Weizheng, He Xiao, Ren Shuai, Liu Jianyu. Potential of muscle-derived stem cells in peripheral nerve regeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1130-1136. |
| [4] | Gao Wenbo, Ma Zongmin, Li Shuxian, Nie Xiuji. Finite element analysis on the effect of implant length and diameter on initial stability under different bone conditions [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 875-880. |
| [5] | He Yunying, Li Lingjie, Zhang Shuqi, Li Yuzhou, Yang Sheng, Ji Ping. Method of constructing cell spheroids based on agarose and polyacrylic molds [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 553-559. |
| [6] | He Guanyu, Xu Baoshan, Du Lilong, Zhang Tongxing, Huo Zhenxin, Shen Li. Biomimetic orientated microchannel annulus fibrosus scaffold constructed by silk fibroin [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 560-566. |
| [7] | Zhang Jianguo, Chen Chen, Hu Fengling, Huang Daoyu, Song Liang. Design and biomechanical properties of dental implant pore structure based on three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 585-590. |
| [8] | Chen Xiaoxu, Luo Yaxin, Bi Haoran, Yang Kun. Preparation and application of acellular scaffold in tissue engineering and regenerative medicine [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 591-596. |
| [9] | Kang Kunlong, Wang Xintao. Research hotspot of biological scaffold materials promoting osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 597-603. |
| [10] | Shen Jiahua, Fu Yong. Application of graphene-based nanomaterials in stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 604-609. |
| [11] | Zhang Tong, Cai Jinchi, Yuan Zhifa, Zhao Haiyan, Han Xingwen, Wang Wenji. Hyaluronic acid-based composite hydrogel in cartilage injury caused by osteoarthritis: application and mechanism [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 617-625. |
| [12] | Li Hui, Chen Lianglong. Application and characteristics of bone graft materials in the treatment of spinal tuberculosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 626-630. |
| [13] | Gao Cangjian, Yang Zhen, Liu Shuyun, Li Hao, Fu Liwei, Zhao Tianyuan, Chen Wei, Liao Zhiyao, Li Pinxue, Sui Xiang, Guo Quanyi. Electrospinning for rotator cuff repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 637-642. |
| [14] | Guan Jian, Jia Yanfei, Zhang Baoxin , Zhao Guozhong. Application of 4D bioprinting in tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 446-455. |
| [15] | Liu Jiali, Suo Hairui, Yang Han, Wang Ling, Xu Mingen. Influence of lay-down angles on mechanical properties of three-dimensional printed polycaprolactone scaffolds [J]. Chinese Journal of Tissue Engineering Research, 2022, 10(16): 2612-2617. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||