Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (29): 7680-7687.doi: 10.12307/2026.290
Previous Articles Next Articles
Meta-analysis of blood flow restriction training to improve knee function and muscle strength in patients after anterior cruciate ligament reconstruction
Chen Ziang, Li Qinlong, Wu Xue, Zhou Yue
- Beijing Sport University, Beijing 100084, China
-
Received:2025-10-15Revised:2025-12-08Online:2026-10-18Published:2026-03-06 -
Contact:Zhou Yue, PhD, Professor, Doctoral supervisor, Beijing Sport University, Beijing 100084, China -
About author:Chen Ziang, MS candidate, Beijing Sport University, Beijing 100084, China Li Qinlong, PhD candidate, Beijing Sport University, Beijing 100084, China Chen Ziang and Li Qinlong contributed equally to the work. -
Supported by:National Key Research and Development Program of China, No. 2018YFF0300801 (to ZY)
CLC Number:
Cite this article
Chen Ziang, Li Qinlong, Wu Xue, Zhou Yue. Meta-analysis of blood flow restriction training to improve knee function and muscle strength in patients after anterior cruciate ligament reconstruction[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(29): 7680-7687.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
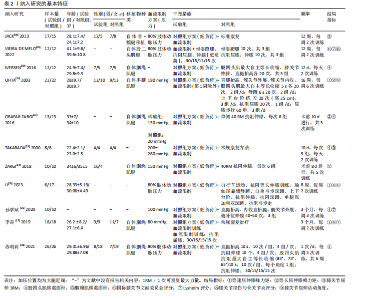
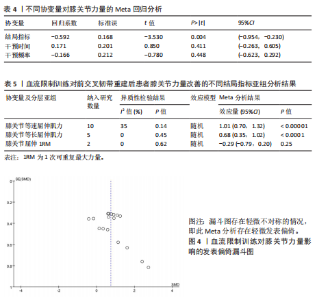
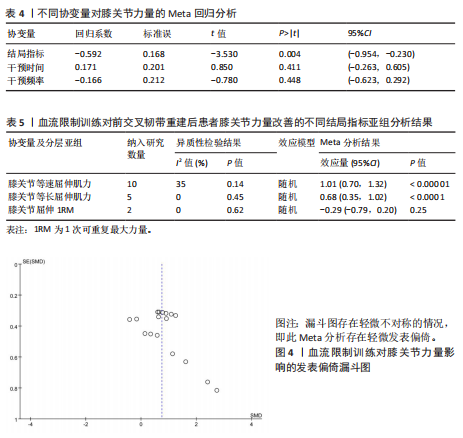
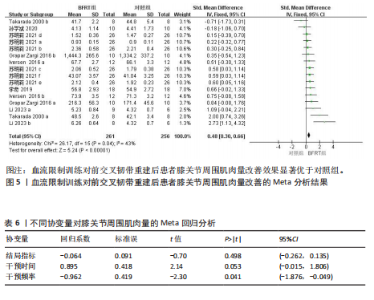
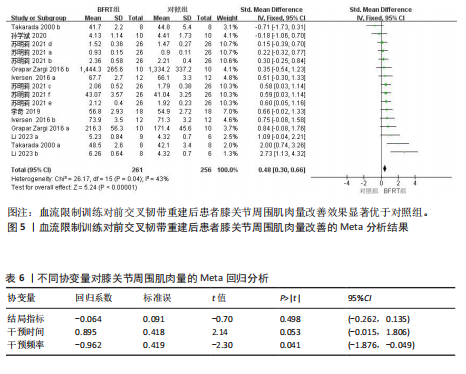
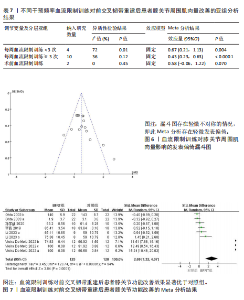
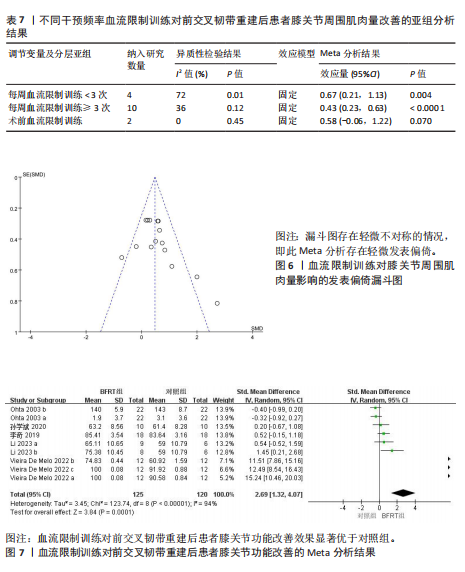
量改善优于对照组[SMD=0.75,95%CI(0.46,1.04),P < 0.000 01],如图3所示。 为查找此Meta分析异质性的来源,根据纳入研究的特征和设置的3个协变量进行Meta回归分析,结果见表4。在结局指标(P=0.004)干预时间(P=0.411)和干预频率(P=0.448)3个协变量中,协变量结局指标的P < 0.05。因此,干预时间和干预频率不是导致异质性的主要来源,而结局指标则可能是产生异质性的主要来源。 以结局指标为分组依据对纳入研究进行亚组分析,结果见表5,血流限制训练组对膝关节等速屈伸肌力的影响优于对照组[SMD=1.01,95%CI(0.70,1.32),P < 0.000 01];血流限制训练组对膝关节等长屈伸肌力的影响优于对照组[SMD=0.68,95%CI(0.35,1.02),P < 0.000 1];血流限制训练组对膝关节屈伸1RM的影响小于对照组[SMD=-0.29,95%CI(-0.79,0.20),P=0.25],但该亚组仅纳入2项研究,样本量仅为64例,Meta分析结果有待进一步研究。 由于此Meta分析存在异质性,故对相关文献进行逐一剔除以确定是否存在单篇文献与总效应量存在较大差异进而影响Meta分析结果。通过逐个剔除发现,当剔除某一项研究后对Meta分析的整体结果影响不大,即此Meta分析的结果较为稳定。 针对该Meta分析进行发表偏倚检验,Egger’s检验结果P > 0.05(P=0.09),但结合漏斗图发现漏斗图存在轻微不对称的情况,即此Meta分析存在轻微发表偏倚,漏斗图如图4所示。采用非参数剪补法对此Meta分析结果进行矫正,矫正结果显示血流限制训练组肌肉力量改善优于对照组[SMD=0.65,95%CI(0.33,0.96),P < 0.000 01]。 2.4.2 血流限制训练对膝关节周围肌肉量的影响 共纳入7篇文献的16项研究[20,22-23,25-28],试验组和对照组共517例患者。固定效应模型Meta分析结果显示,血流限制训练组肌肉量改善优于对照组[SMD=0.48,95%CI(0.30,0.66),P < 0.000 01],如图5所示。 为查找此Meta分析异质性的来源,根据纳入研究的特征和设置的3个协变量进行Meta回归分析,结果见表6。在结局指标(P=0.498)干预时间(P=0.053)和干预频率(P=0.041)3个协变量中,协变量干预频率的P < 0.05。因此,结局指标和干预时间不是导致异质性的主要来源,而干预频率则可能是产生异质性的主要来源。 以干预频率为分组依据对纳入研究进行亚组分析,结果见表7,每周血流限制训练 < 3次时,血流限制训练组对膝关节周围肌肉量的影响优于对照组[SMD=0.67,95%CI(0.21,1.13),P=0.004];每周血流限制训练≥3次时,血流限制训练组对膝关节周围肌肉量的影响优于对照组[SMD=0.43,95%CI(0.23,0.63),P < 0.000 1];仅术前进行血流限制训练时,血流限制训练组对膝关节周围肌肉量的影响优于对照组[SMD=0.58,95%CI(-0.06,1.22),P=0.070],但影响效果不显著,且该亚组仅纳入2项研究,样本量仅为40例,Meta分析结果有待进一步研究。 由于此Meta分析存在异质性,故对相关文献进行逐一剔除以确定是否存在单篇文献与总效应量存在较大差异进而影响Meta分析结果。通过逐个剔除发现,当剔除某一项研究后对Meta分析的整体结果影响不大,即此Meta分析的结果较为稳定。 针对该Meta分析进行发表偏倚检验,Egger’s检验结果P > 0.05(P=0.09),但结合漏斗图发现漏斗图存在轻微不对称的情况,即此Meta分析存在轻微发表偏倚,漏斗图如图6所示。采用非参数剪补法对此Meta分析结果进行矫正,矫正结果显示血流限制训练组肌肉量改善优于对照组[SMD=0.4,95%CI(0.23,0.57),P < 0.000 01]。 2.4.3 血流限制训练对膝关节功能的影响 共纳入5篇文献的9项研究[19,21,25-27],试验组和对照组共245例患者。随机效应模型Meta分析结果显示,血流限制训练组膝关节功能改善优于对照组[SMD=2.69,95%CI(1.32,4.07),P=0.000 1],如图7所示。 由于此Meta分析纳入的研究过少,故不进行Meta回归分析。产生高异质性的原因可能是由于此次所纳入的研究采用不同的膝关节"
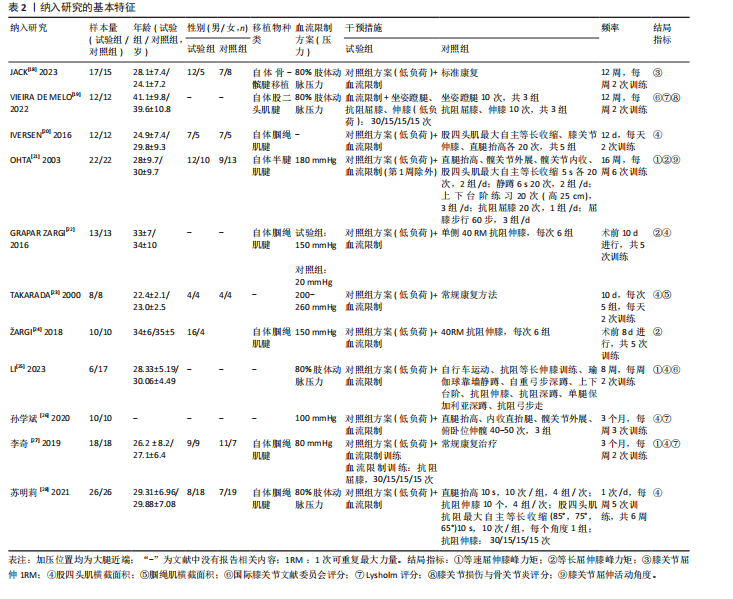
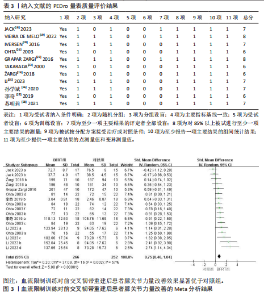
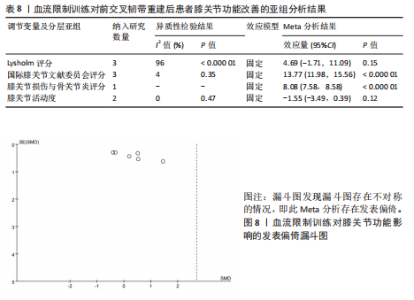
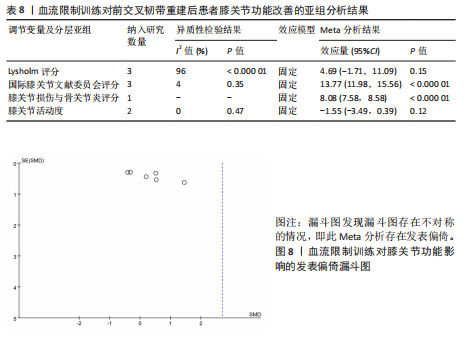
功能评定结局指标所导致,所以以结局指标为分组依据对纳入研究进行亚组分析(表8),亚组分析发现,采用不同量表评价血流限制训练对前交叉韧带重建后患者膝关节功能改善效果的结果不一,其中采用国际膝关节文献委员会评分[MD=13.77,95%CI(11.98,15.56),P < 0.000 01]和膝关节损伤与骨关节炎评分 [MD=8.08,95%CI(7.58,8.58),P < 0.000 01]评价膝关节功能发现血流限制训练组对膝关节功能的影响优于对照组,但采用Lysholm评分[MD=4.69,95%CI(-1.71,11.09),P=0.15]评价膝关节功能发现血流限制训练组对膝关节功能的影响不显著。同时血流限制训练组对膝关节活动度[MD=-1.55,95%CI(-3.49,0.39),P=0.12]的影响不显著。"
| [1] 陈连旭, 付立功. 前交叉韧带断裂和重建的临床流行病学分析[J]. 中国组织工程研究,2016, 20(24):3602-3608. [2] GRAPAR ŽARGI T, DROBNIČ M, VAUHNIK R, et al. Factors predicting quadriceps femoris muscle atrophy during the first 12 weeks following anterior cruciate ligament reconstruction. Knee. 2017;24(2):319-328. [3] KILINÇ BE, KARA A, CAMUR S, et al. Isokinetic dynamometer evaluation of the effects of early thigh diameter difference on thigh muscle strength in patients undergoing anterior cruciate ligament reconstruction with hamstring tendon graft. J Exerc Rehabil. 2015;11(2):95-100. [4] HIEMSTRA LA, WEBBER S, MACDONALD PB, et al. Contralateral limb strength deficits after anterior cruciate ligament reconstruction using a hamstring tendon graft. Clin Biomech (Bristol, Avon). 2007; 22(5):543-550. [5] SCHMITT LC, PATERNO MV, HEWETT TE. The impact of quadriceps femoris strength asymmetry on functional performance at return to sport following anterior cruciate ligament reconstruction. J Orthop Sports Phys Ther. 2012; 42(9):750-759. [6] FILBAY SR. Longer-term quality of life following ACL injury and reconstruction. Br J Sports Med. 2018;52(3):208-209. [7] THOMAS AC, WOJTYS EM, BRANDON C, et al. Muscle atrophy contributes to quadriceps weakness after anterior cruciate ligament reconstruction. J Sci Med Sport. 2016;19(1):7-11. [8] HUGHES L, ROSENBLATT B, PATON B, et al. Blood Flow Restriction Training in Rehabilitation Following Anterior Cruciate Ligament Reconstructive Surgery: A Review. Tech Orthop. 2018;33(2):106-113. [9] PATTERSON SD, HUGHES L, WARMINGTON S, et al. Blood Flow Restriction Exercise: Considerations of Methodology, Application, and Safety. Front Physiol. 2019;10:533. [10] 吴旸, 李倩, 包大鹏. 加压力量训练对下肢骨骼肌影响的Meta分析[J]. 中国体育科技,2019, 55(3):20-26. [11] RATAMESS NA, ALVAR BA, EVETOCH TK, et al. American College of Sports Medicine position stand. Progression models in resistance training for healthy adults. Med Sci Sports Exerc. 2009; 41(3):687-708. [12] WERNBOM M, AUGUSTSSON J, RAASTAD T. Ischemic strength training: a low-load alternative to heavy resistance exercise? Scand J Med Sci Sports. 2008;18(4):401-416. [13] DE QUEIROS VS, ROLNICK N, DE ALCÂNTARA VARELA PW, et al. Physiological adaptations and myocellular stress in short-term, high-frequency blood flow restriction training: A scoping review. PLoS One. 2022;17(12):e0279811. [14] VOPAT BG, VOPAT LM, BECHTOLD MM, et al. Blood Flow Restriction Therapy: Where We Are and Where We Are Going. J Am Acad Orthop Surg. 2020;28(12):e493-e500. [15] CUMPSTON M, LI T FAU -PAGE MJ, PAGE MJ FAU -CHANDLER J, et al. Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Syst Rev. 2019;10(10):ED000142. [16] MAHER CG, SHERRINGTON C, HERBERT RD, et al. Reliability of the PEDro scale for rating quality of randomized controlled trials. Phys Ther. 2003; 83(8):713-721. [17] 张天嵩, 钟文昭. 非参数剪补法在Stata中的实现[J]. 循证医学,2009,9(4):240-242. [18] JACK RA 2ND, LAMBERT BS, HEDT CA, et al. Blood Flow Restriction Therapy Preserves Lower Extremity Bone and Muscle Mass After ACL Reconstruction. Sports Health. 2023;15(3):361-371. [19] VIEIRA DE MELO RF, KOMATSU WR, FREITAS MS, et al. Comparison of Quadriceps and Hamstring Muscle Strength after Exercises with and without Blood Flow Restriction following Anterior Cruciate Ligament Surgery: A Randomized Controlled Trial. J Rehabil Med. 2022;54:jrm00337. [20] IVERSEN E, RØSTAD V, LARMO A. Intermittent blood flow restriction does not reduce atrophy following anterior cruciate ligament reconstruction. J Sport Health Sci. 2016;5(1): 115-118. [21] OHTA H, KUROSAWA H, IKEDA H, et al. Low-load resistance muscular training with moderate restriction of blood flow after anterior cruciate ligament reconstruction. Acta Orthop Scand. 2003; 74(1):62-68. [22] GRAPAR ZARGI T, DROBNIC M, JKODER J, et al. The effects of preconditioning with ischemic exercise on quadriceps femoris muscle atrophy following anterior cruciate ligament reconstruction: a quasi-randomized controlled trial. Eur J Phys Rehabil Med. 2016;52(3):310-320. [23] TAKARADA Y, TAKAZAWA H, ISHII N. Applications of vascular occlusion diminish disuse atrophy of knee extensor muscles. Med Sci Sports Exerc. 2000;32(12):2035-2039. [24] ŽARGI T, DROBNIČ M, STRAŽAR K, et al. Short-Term Preconditioning With Blood Flow Restricted Exercise Preserves Quadriceps Muscle Endurance in Patients After Anterior Cruciate Ligament Reconstruction. Front Physiol. 2018;9:1150. [25] LI X, LI J, QING L, et al. Effect of quadriceps training at different levels of blood flow restriction on quadriceps strength and thickness in the mid-term postoperative period after anterior cruciate ligament reconstruction: a randomized controlled external pilot study. BMC Musculoskelet Disord; 2023;24(1):360. [26] 孙学斌, 岐飞, 曹力. 不同康复治疗方法对关节镜下前交叉韧带重建术后患者的短期疗效观察[J]. 新疆医学,2020,50(5):441-445. [27] 李奇, 李蕊, 罗昌禄, 等. 血流限制性运动对前交叉韧带重建术后膝关节功能的影响[J]. 广东医学,2019,40(10):1405-1408. [28] 苏明莉. 血流限制训练对前交叉韧带重建术后患者早期股四头肌萎缩的影响研究[D].西安:西安体育学院,2021. [29] 苏利强, 黄红拾, 常翠青. 离心收缩训练对前交叉韧带断裂患者股四头肌萎缩影响的研究进展[J]. 中国康复医学杂志,2013,28(11):1067-1071. [30] 袁丽, 胥方元, 钟大勇, 等. 可穿戴振动反馈训练对前交叉韧带重建术后患者平衡及行走功能的影响[J]. 中国康复医学杂志,2023,38(3):325-330. [31] ABERNETHY PJ, JÜRIMÄE J, LOGAN PA, et al. Acute and chronic response of skeletal muscle to resistance exercise. Sports Med. 1994;17(1):22-38. [32] GABRIEL DA, KAMEN G, FROST G. Neural adaptations to resistive exercise: mechanisms and recommendations for training practices. Sports Med. 2006;36(2):133-149. [33] LORENZ DS, BAILEY L, WILK KE, et al. Blood Flow Restriction Training. J Athl Train. 2021;56(9):937-944. [34] 刘晨晨,刘锐泽,鲍蒙蒙,等. 血流限制训练干预老年肌少性肥胖[J]. 中国组织工程研究,2025,29(32):6963-6970. [35] MELISSA L, MACDOUGALL JD, TARNOPOLSKY MA, et al. Skeletal muscle adaptations to training under normobaric hypoxic versus normoxic conditions. Med Sci Sports Exerc. 1997;29(2):238-243. [36] FUJITA S, ABE T, DRUMMOND MJ, et al. Blood flow restriction during low-intensity resistance exercise increases S6K1 phosphorylation and muscle protein synthesis. J Appl Physiol (1985). 2007; 103(3):903-910. [37] 魏佳, 李博, 杨威, 等. 血流限制训练的应用效果与作用机制[J]. 体育科学,2019,39(4):71-80. [38] MADARAME H, SASAKI K, ISHII N. Endocrine responses to upper- and lower-limb resistance exercises with blood flow restriction. Acta Physiol Hung. 2010;97(2):192-200. [39] ABE T, LOENNEKE JP, FAHS CA, et al. Exercise intensity and muscle hypertrophy in blood flow-restricted limbs and non-restricted muscles: a brief review. Clin Physiol Funct Imaging. 2012; 32(4):247-252. [40] COGNETTI DJ, SHEEAN AJ, OWENS JG. Blood Flow Restriction Therapy and Its Use for Rehabilitation and Return to Sport: Physiology, Application, and Guidelines for Implementation. Arthrosc Sports Med Rehabil. 2022;4(1):e71-e76. [41] HOOGEBOOM TJ, OOSTING E, VRIEZEKOLK JE, et al. Therapeutic validity and effectiveness of preoperative exercise on functional recovery after joint replacement: a systematic review and meta-analysis. PLoS One. 2012;7(5):e38031. [42] WANG L, LEE M, ZHANG Z, et al. Does preoperative rehabilitation for patients planning to undergo joint replacement surgery improve outcomes? A systematic review and meta-analysis of randomised controlled trials. BMJ Open. 2016; 6(2):e009857. [43] 王周, 吴迎. 缺血预处理提升运动表现:方法、应用及机制[J]. 中国组织工程研究,2023, 27(30):4869-4875. [44] 范紫菡, 吴迎. 缺血处理在运动训练中的应用:效果、机制及问题[J]. 中国运动医学杂志, 2024,43(9):753-766. [45] FRANZ A, QUEITSCH F P, BEHRINGER M, et al. Blood flow restriction training as a prehabilitation concept in total knee arthroplasty: A narrative review about current preoperative interventions and the potential impact of BFR. Med Hypotheses. 2018;110:53-59. [46] FRANZ A, JI S, BITTERSOHL B, et al. Impact of a Six-Week Prehabilitation With Blood-Flow Restriction Training on Pre- and Postoperative Skeletal Muscle Mass and Strength in Patients Receiving Primary Total Knee Arthroplasty. Front Physiol. 2022;13: 881484. [47] KACIN A, DROBNIČ M, MARŠ T, et al. Functional and molecular adaptations of quadriceps and hamstring muscles to blood flow restricted training in patients with ACL rupture. Scand J Med Sci Sports. 2021;31(8):1636-1646. |
| [1] | Fang Chao, Deng Miao, Wang Yang, Gao Fei, Li Jiahang, Yu Fangfang. Relationship between gait parameter characteristics and joint function recovery after arthroscopic minimally invasive surgery in patients with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(21): 5468-5476. |
| [2] | Li Chengke, Gao Miaomiao, Lei Lei, Ma Rongxing, Zhang Jingyu, Hu Yongcheng. Dynamic evolution of evaluation standards for effectiveness and safety after anterior cruciate ligament reconstruction in the knee [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(21): 5605-5613. |
| [3] | Liu Yanzhe, Liu Hua, Yang Tubao, Liu Yupeng. Effects of human umbilical cord blood mesenchymal stem cells on pain and function in patients with knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(19): 5066-5071. |
| [4] | Cheng Xiaofei, Yang Yuanyuan, Li Sihui, Wang Dehua, Liang Chunting, Li Jiawei, Yao Mingyang, Yao Xiaoduo, Tang Jiqin. Effects of different non-invasive brain stimulation protocols on gait and balance function in patients with Parkinson’s disease: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(18): 4749-4762. |
| [5] | Wang Juan, Wang Guanglan, Zuo Huiwu. Efficacy of exercise therapy in the treatment of anterior cruciate ligament reconstruction patients: #br# a network meta-analysis #br# [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(8): 1714-1726. |
| [6] | Wang Feng, Cao Chunfeng, He Chao, Zhang Tao, Zhou Zixian, Zhu Fengchen. All-inside versus traditional techniques of anterior cruciate ligament reconstruction: meta-analysis of therapeutic efficacy and radiological outcomes [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(35): 7629-7638. |
| [7] | Liu Mengling, Li Yongjie, Liu Hongju. Effect of increased stride length on knee kinematics and dynamics of asymmetric gait after anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(33): 7109-7115. |
| [8] | Shi Lei, Shi Song, Lu Yue, Tao Ran, Ma Hongdong. Comparison of unicondylar knee arthroplasty and high tibial osteotomy in treatment of medial knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(3): 503-509. |
| [9] | Wang Xia, Xue Boshi, Yang Chen, Zhou Zhipeng, Zheng Liangliang. Influence of neuromuscular function on the risk of biomechanical injury in landing manoeuvres in patients undergoing anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(26): 5556-5562. |
| [10] | Zhang Sizhuo, Liu Xiaoqian, Wang Guanglan. Effects of visual interference on biomechanical characteristics of lower limbs in athletes after anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(20): 4223-4229. |
| [11] | Wei Mengli, Zhong Yaping, Yu Tingting, Tan Xilin, Cao Sijia. Correlation between muscle synergy characteristics of the affected leg and gait stability during walking in patients undergoing anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(14): 2899-2906. |
| [12] | Chen Wenhan, Men Jie, Yang Wei, Zhao Xiaoyu. Effect of vibration therapy combined with suspension training on movement and knee joint function after anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(11): 2225-2230. |
| [13] | Bai Chen, Yang Wenqian, Meng Zhichao, Wang Yuze. Strategies for repairing injured anterior cruciate ligament and promoting graft healing [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1457-1463. |
| [14] | Wang Juan, Wang Ling, Zuo Huiwu, Zheng Cheng, Wang Guanglan, Chen Peng. Rehabilitative efficacy of kinesio taping following anterior cruciate ligament reconstruction: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 651-656. |
| [15] | Li Qi, Gao Mingwei, Li Shihao, Chu Xiaolei, Li Yajie, Ding Ning, Liu Minqi. Rate of force development and its relationship with functional performance in patients after anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(34): 5536-5543. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||