Chinese Journal of Tissue Engineering Research ›› 2017, Vol. 21 ›› Issue (21): 3420-3425.doi: 10.3969/j.issn.2095-4344.2017.21.023
Previous Articles Next Articles
Anterior cruciate ligament injury and stem cell therapy
Zhao Liang1, Han Chang-xu2, Ren Yi-zhong2
- 1Inner Mongolia Medical University, Hohhot 010030, Inner Mongolia Autonomous Region, China; 2the Second Affiliated Hospital of Inner Mongolia Medical University, Hohhot 010030, Inner Mongolia Autonomous Region, China
-
Revised:2017-02-19Online:2017-07-28Published:2017-08-02 -
Contact:Ren Yi-zhong, M.D., Master’s supervisor, the Second Affiliated Hospital of Inner Mongolia Medical University, Hohhot 010030, Inner Mongolia Autonomous Region, China -
About author:Zhao Liang, Studying for master’s degree, Inner Mongolia Medical University, Hohhot 010030, Inner Mongolia Autonomous Region, China
CLC Number:
Cite this article
Zhao Liang, Han Chang-xu, Ren Yi-zhong. Anterior cruciate ligament injury and stem cell therapy[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(21): 3420-3425.
share this article
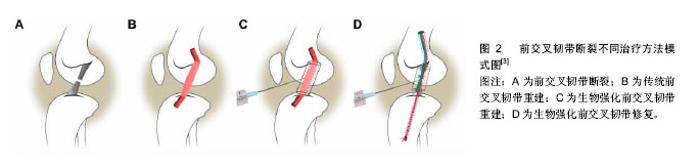
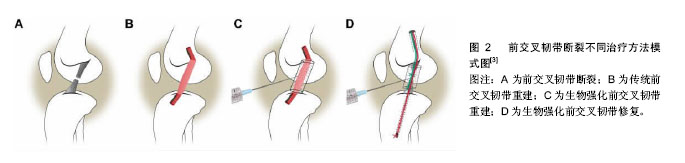
2.1 受损前交叉韧带的愈合及治疗 2.1.1 影响前交叉韧带愈合过程的因素 肌腱和韧带的愈合过程发生缓慢,可分为3个阶段:①组织炎症期;②血管长入与细胞增生期;③韧带重建期。各阶段间无明显组织学与时间界限,约在第8周起,纤维瘢痕开始形成[4]。前交叉韧带再生的一个困难是其损伤或断裂后无法引起血小板聚集,从而不能激活凝血系统,因此难以自愈,这一点对第一阶段至关重要[5]。在受损前交叉韧带的愈合过程中,关节内环境发挥着至关重要的作用。 因此,在韧带受损后,研究滑膜液的组成对分析影响韧带愈合的因素至关重要。在前交叉韧带断裂患者的滑膜液中,可以观察到基质金属蛋白酶3、白细胞介素6、组织金属蛋白酶抑制剂1的增多[6-7]。基质金属蛋白酶和组织金属蛋白酶抑制剂是组织重塑过程中重要的酶。基质金属蛋白酶/组织金属蛋白酶抑制剂比值较高的膝关节更易发生软骨破坏[6]。这种不平衡也可能会对前交叉韧带的愈合产生影响。Tang等[8]认为基质金属蛋白酶在关节内的积累是前交叉韧带修复减弱的原因。Higuchi等[6]的研究表明在前交叉韧带伤后的一段时间内,基质金属蛋白酶3浓度依然很高,然而组织金属蛋白酶抑制剂1浓度却下降。因此认为,前交叉韧带受伤后,治疗时机的选择可能对愈合产生一定影响。 2.1.2 前交叉韧带损伤的治疗 目前前交叉韧带重建术的金标准是使用自体腘绳肌(半腱肌和股薄肌)或髌腱代替前交叉韧带。手术治疗特别适用于日常生活中膝盖承受高负荷运动的患者,尤其是经常做急停急起、快速变向的运动员患者。保守治疗包括矫形术、本体感觉训练,以及一些加强肌肉从而增加膝关节稳定性的训练。Lohmander等[9]在一项12年的随访中发现,在一组受伤的女性足球运动员中,其中82%患者的膝关节有骨性关节炎的影像学表现。成功地对受伤的运动员行前交叉韧带重建术,可以将创伤性骨关节炎进行有效的控制[10]。使用自体移植物重建前交叉韧带,存在来源限制、供区并发症等问题[11]。目前还没有由于移植物的差异而导致临床预后及稳定性差异的文献报道[12]。Frobell等[13]最近公布的一项前瞻性随机对照试验认为,经过5年随访研究,对于前交叉韧带断裂的患者,康复为主要治疗方式的非手术治疗与手术治疗相比,两者在膝关节损伤和骨关节炎的评分中治疗效果相当。此外,Costa-Paz等[14]发现前交叉韧带也有自愈的可能。他们回顾性分析了14例患者,均被建议手术,但因为种种原因未完成手术。这些患者均复查了MRI,显示断端有愈合以及轴移试验为阴性,这表明前交叉韧带存在自发愈合的可能性。2006年Steadman等[15]发表了促进骨骼未成熟运动员前交叉韧带损伤愈合的新方法。所谓的“愈合反应技术”(HRT)是前交叉韧带微裂隙旁的股骨,可在血液凝块的帮助下在促进前交叉韧带断端附着。他们还报导了此技术在一组超过40岁的全前交叉韧带断裂患者中是有效的[16]。前交叉韧带断裂不同治疗方法模式图见图2。"
| [1] Clayton R, Court-Brown CM.The epidemiology of musculoskeletal tendinous and ligamentous injuries. Inj Int J Care Inj.2008;39:1338-1344.[2] Haaori K, Sano H, Komatsuda T, et al. Efect of estrogen on tissue elasticity of the ligament proper in rabbit anterior cruciate ligament:measurements using scanning acoustic microscopy. J Orthop Sci.2010;15(4):584-588.[3] MM Murray, BC Fleming.Use of a bioactive scaffold to stimulate anterior cruciate ligament healing also minimizes posttraumatic osteoarthritis after surgery. Am J Sports Med. 2013;41(8):1762-1770.[4] Sharma P, Maffulli N. Basic biology of tendon injury and healing. Surgeon. 2005;3(5):309 -316.[5] Murray MM, Spindler KP, Ballard P, et al. Enhanced histologic repair in a central wound in the anterior cruciate ligament with a collagen-platelet-rich plasma scaffold. J Orthop Res.2007; 25(8):1007-1017.[6] Higuchi H, Shirakura K, Kimura M,et al. Changes in biochemical parameters after anterior cruciate ligament injury. Int Orthop.2006;1:43-47.[7] Lohmander LS, Hoerrner LA, Lark MW. Metalloproteinases, tissue inhibitor, and proteoglycan fragments in knee synovial fluid in human osteoarthritis. Arthritis Rheum.1993;36: 181-189.[8] Tang Z, Yang L, Wang Y,et al. Contributions of different intraarticular tissues to the acute phase elevation of synovial fluid MMP-2 following rat ACL rupture. J Orthop Res.2009;2: 243-248.[9] Lohmander LS, Ostenberg A, Englund M, et al.High prevalence of knee osteoarthritis, pain, and functional limitations in female soccer players twelve years after anterior cruciate ligament injury. Arthritis Rheum.2004;50:3145- 3152.[10] Hoffelner T, Resch H, Forstner Michael M,et al. Arthroscopic all-inside meniscal repair—does the Meniscus heal? A clinical and radiological follow-up examination to verify meniscal healing using a 3-T MRI. Skeletal Radiol.2011; 40(2):181-187.[11] Mascarenhas R, MacDonald PB. Anterior cruciate ligament reconstruction: a look at prosthetics--past, present and possible future.Mcgill J Med. 2008;11(1):29-37.[12] Lide´n M, Ejerhed L, Sernert N,et al. Patellar tendon or semitendinosus tendon autografts for anterior cruciate ligament reconstruction: a prospective, randomized study with a 7-year follow-up. Am J Sports Med.2007;35:740-748.[13] Frobell RB, Roos HP, Roos EM,et al. Treatment for acute anterior cruciate ligament tear: five year outcome of randomised trial. BMJ.2013;346:232-244[14] Costa-Paz M, Ayerza MA, Tanoira I,et al.Spontaneous healing in complete ACL ruptures: a clinical and MRI study. Clin Orthop Relat Res.2012;470(4):979-985.[15] Steadman JR, Cameron-Donaldson ML, Briggs KK,et al.A minimally invasive technique (‘‘healing response’’) to treat proximal ACL injuries in skeletally immature athletes. J Knee Surg.2006;19(1):8-13.[16] Steadman JR, Matheny LM, Briggs KK,et al. Outcomes following healing response in older, active patients: a primary anterior cruciate ligament repair technique. J Knee Surg. 2012;25(3):255-260.[17] Burdon T, Smith A, Savatier P.Signalling, cell cycle and pluripotency in embryonic stem cells. Trends Cell Biol.2002; 12:432-438.[18] Thomson JA, Itskovitz-Eldor J, Shapiro SS,et al. Embryonic stem cell lines derived from human blastocysts. Science. 1998;5391:1145-1147.[19] Watts AE, Yeager AE, Kopyov OV, Fetal derived embryonic-like stem cells improve healing in a large animal flexor tendonitis model. Stem Cell Res Ther.2011; 2(1):4.[20] Lodi D, Iannitti T, Palmieri B. Stem cells in clinical practice: applications and warnings.J Exp Clin Cancer Res.2011; 17(30):9.[21] Satija NK, Singh VK, Verma YK, et al. Mesenchymal stem cell-based therapy: a new paradigm in regenerative medicine.J Cell Mol Med.2009;13(11 -12):4385-402.[22] Dominici M,Le Blanc K,Mueller I,et al.Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy.2006;4:315-317.[23] Salingcarnboriboon R, Yoshitake H, Tsuji K,et al. Establishment of tendonderived cell lines exhibiting pluripotent mesenchymal stem celllike property. Exp Cell Res.2003;287:289-300.[24] Bi Y, Ehirchiou D, Kilts TM,et al. Identification of tendon stem/progenitor cells and the role of the extracellular matrix in their niche. Nat Med.2007; 10:1219-1227.[25] Cheng MT, Liu CL, Chen TH,et al. Comparison of potentials between stem cells isolated from human anterior cruciate ligament and bone marrow for ligament tissue engineering. Tissue Eng Part A.2010;16(7):2237-2253.[26] Matsumoto T, Ingham SM, Mifune Y,et al.Isolation and characterization of human anterior cruciate ligament-derived vascular stem cells. Stem Cells Develop 2012;6:859-872.[27] Tempfer H, Wagner A, Gehwolf R,et al. Perivascular cells of the supraspinatus tendon express both tendon- and stem cell related markers. Histochem Cell Biol.2009; 131:733-741.[28] Steinert AF, Kunz M, Prager P,et al. Mesenchymal stem cell characteristics of human anterior cruciate ligament outgrowth cells. Tissue Eng Part A 2011;17:1375-1388.[29] Lui PP, Wong OT, Lee YW.Application of tendon-derived stem cell sheet for the promotion of graft healing in anterior Cruciate ligament reconstruction. Am J Sports Med. 2014 Mar;42(3):681-689. [30] van Steensel CJ, Schreuder O, van den Bosch BF, et al. Failure of anterior cruciate-ligament reconstruction using tendon xenograft.J Bone Joint Surg Am. 1987;69(6): 860-864.[31] Rumian AP, Wallace AL, Birch HL.Tendons and ligaments are anatomically distinct but overlap in molecular and morphological features-a comparative study in an ovine mode journal of orthopaedic research. J Orthop Res.2007;25(4): 458-464.[32] Hadjicostas PT, Soucacos PN, Koleganova N,et al. Comparative and morphological analysis of commonly used autografts for anterior cruciate ligament reconstruction with the native ACL: an electron, microscopic and morphologic study. Knee Surg Sports Traumatol Arthrosc.2008;16:1099-1107.[33] Becerra P, Valde´s Va´zquez MA, Dudhia J,et al. Distribution of injected technetium(99m)-labeled mesenchymal stem cells in horses with naturally occurring tendinopathy. J Orthop Res. 2013;31(7):1096-1102.[34] Agung M, Ochi M, Yanada S,et al. Mobilization of bone marrow-derived mesenchymal stem cells into the injured tissues after intraarticular injection and their contribution to tissue regeneration. Knee Surg Sports Traumatol Arthrosc. 2006;14:1307-1314.[35] Murphy JM, Fink DJ, Hunziker EB, et al.Stem cell therapy in a caprine model of osteoarthritis. Arthritis Rheum.2003;48: 3464-3474.[36] Kanaya A, Deie M, Adachi N,et al.Intra-articular injection of mesenchymal stromal cells in partially torn anterior cruciate ligaments in a rat model. Arthroscopy.2007;23:610-617.[37] Kasper G, Glaeser JD, Geissler S,et al. Matrix metalloprotease activity is an essential link between mechanical stimulus and mesenchymal stem cell behavior. Stem Cells.2007;25(8):1985-1994.[38] Xie J, Wang C, Huang DY,et al. TGF-beta1 induces the different expressions of lysyl oxidases and matrix metalloproteinases in anterior cruciate ligament and medial collateral ligament fibroblasts after mechanical injury. J Biomech.2013; 46:890-898. [39] Smith-Mungo LI, Kagan HM. Lysyl oxidase: properties, regulation and multiple functions in biology. Matrix Biol.1998; 16(7):387-398.[40] Figueroa D, Espinosa M, Calvo R,et al.(2013) Anterior cruciate ligament regeneration using mesenchymal stem cells and collagen type I scaffold in a rabbit model. Knee Surg Sports Traumatol Arthrosc. 2014;22(5):1196-202.[41] Silva A, Sampaio R, Fernandes R,et al. Is there a role for adult non-cultivated bone marrow stem cells in ACL reconstruction? Knee Surg Sports Traumatol Arthrosc. 2014; 22(1):66-71.[42] Orozco L,Munar A,Soler R, et al. Treatment of knee osteoarthritis with autologous mesenchymal stem cells: a pilot study. Transplantation.2013;12:1535–1541.[43] Davatchi F, Abdollahi BS, Mohyeddin M,et al. Mesenchymal stem cell therapy for knee osteoarthritis.Preliminary report of four patients. Int J Rheum Dis.2011; 14:211-215.[44] 张平平,向川. 骨髓间充质干细胞治疗骨关节炎:可能与未来[J].中国组织工程研究,2014,18(6):968-973.[45] Centeno CJ, Schultz JR, Cheever M,et al. Safety and complications reporting update on the re-implantation of cultured-expanded mesenchymal stem cells using autologous platelet lysate technique. Curr Stem Cell Res Ther.2011;6: 368-378. |
| [1] | Tan Xinfang, Guo Yanxing, Qin Xiaofei, Zhang Binqing, Zhao Dongliang, Pan Kunkun, Li Yuzhuo, Chen Haoyu. Effect of uniaxial fatigue exercise on patellofemoral cartilage injury in a rabbit [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(在线): 1-6. |
| [2] | Yao Xiaoling, Peng Jiancheng, Xu Yuerong, Yang Zhidong, Zhang Shuncong. Variable-angle zero-notch anterior interbody fusion system in the treatment of cervical spondylotic myelopathy: 30-month follow-up [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1377-1382. |
| [3] | Wu Cong, Jia Quanzhong, Liu Lun. Relationship between transforming growth factor beta1 expression and chondrocyte migration in adult articular cartilage after fragmentation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1167-1172. |
| [4] | Wang Jing, Xiong Shan, Cao Jin, Feng Linwei, Wang Xin. Role and mechanism of interleukin-3 in bone metabolism [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1260-1265. |
| [5] | Xiao Hao, Liu Jing, Zhou Jun. Research progress of pulsed electromagnetic field in the treatment of postmenopausal osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1266-1271. |
| [6] | An Weizheng, He Xiao, Ren Shuai, Liu Jianyu. Potential of muscle-derived stem cells in peripheral nerve regeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1130-1136. |
| [7] | Fan Yiming, Liu Fangyu, Zhang Hongyu, Li Shuai, Wang Yansong. Serial questions about endogenous neural stem cell response in the ependymal zone after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1137-1142. |
| [8] | Hui Xiaoshan, Bai Jing, Zhou Siyuan, Wang Jie, Zhang Jinsheng, He Qingyong, Meng Peipei. Theoretical mechanism of traditional Chinese medicine theory on stem cell induced differentiation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1125-1129. |
| [9] | Tian Chuan, Zhu Xiangqing, Yang Zailing, Yan Donghai, Li Ye, Wang Yanying, Yang Yukun, He Jie, Lü Guanke, Cai Xuemin, Shu Liping, He Zhixu, Pan Xinghua. Bone marrow mesenchymal stem cells regulate ovarian aging in macaques [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 985-991. |
| [10] | Hou Jingying, Guo Tianzhu, Yu Menglei, Long Huibao, Wu Hao. Hypoxia preconditioning targets and downregulates miR-195 and promotes bone marrow mesenchymal stem cell survival and pro-angiogenic potential by activating MALAT1 [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1005-1011. |
| [11] | Zhou Ying, Zhang Huan, Liao Song, Hu Fanqi, Yi Jing, Liu Yubin, Jin Jide. Immunomodulatory effects of deferoxamine and interferon gamma on human dental pulp stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1012-1019. |
| [12] | Liang Xuezhen, Yang Xi, Li Jiacheng, Luo Di, Xu Bo, Li Gang. Bushen Huoxue capsule regulates osteogenic and adipogenic differentiation of rat bone marrow mesenchymal stem cells via Hedgehog signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1020-1026. |
| [13] | Wang Jifang, Bao Zhen, Qiao Yahong. miR-206 regulates EVI1 gene expression and cell biological behavior in stem cells of small cell lung cancer [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1027-1031. |
| [14] | Liu Feng, Peng Yuhuan, Luo Liangping, Wu Benqing. Plant-derived basic fibroblast growth factor maintains the growth and differentiation of human embryonic stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1032-1037. |
| [15] | Wen Dandan, Li Qiang, Shen Caiqi, Ji Zhe, Jin Peisheng. Nocardia rubra cell wall skeleton for extemal use improves the viability of adipogenic mesenchymal stem cells and promotes diabetes wound repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1038-1044. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||