Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (53): 8565-8569.doi: 10.3969/j.issn.2095-4344.2014.53.007
Previous Articles Next Articles
Comparison of different anesthesia drugs in hip joint replacement
vZhu Wei-bing
- Chongming Branch, Xinhua Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai 202150, China
-
Revised:2014-11-20Online:2014-12-24Published:2014-12-24 -
Contact:Zhu Wei-bing, Attending physician, Chongming Branch, Xinhua Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai 202150, China -
About author:Zhu Wei-bing, Attending physician, Chongming Branch, Xinhua Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai 202150, China
CLC Number:
Cite this article
Zhu Wei-bing. Comparison of different anesthesia drugs in hip joint replacement[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(53): 8565-8569.
share this article
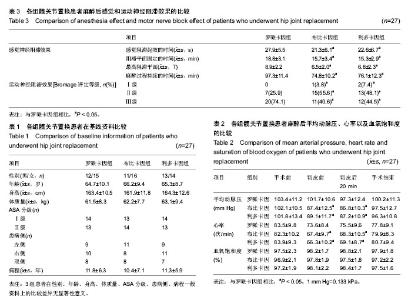
2.1 参与者数量分析 所选81例患者研究期间均无退出,均进入结果分析。 2.2 各组患者基线资料分析 由表1可得,3组患者在性别、年龄、身高、体质量、美国麻醉师协会评估标准(ASA分级)、患病侧、病程的比较差异无显著性意义(P > 0.05),则说明3组患者在一般资料上有可比性。 2.3 各组患者麻醉后不同时间点平均动脉压、心率以及血氧饱和度的比较 通过监测与记录手术前、切皮前、切皮后20 min以及手术结束时3组患者平均动脉压、心率以及血氧饱和度情况。 总体结果显示,3组患者在平均动脉压、心率以及血氧饱和度上表现都比较好。相对布比卡因组与利多卡因组,罗哌卡因组患者的平均动脉压与心率具有更加显著的稳定性。特别是在切皮前、切皮后20 min,相对罗哌卡因组,布比卡因组与利多卡因组患者的平均动脉压与心率下降较为显著(P < 0.05);而布比卡因组与利多卡因组患者平均动脉压与心率差异无显著性意义(P > 0.05)。 3组患者的血氧饱和度差异无显著性意义(P > 0.05)。见表2。 2.4 各组患者麻醉后感觉神经阻滞效果的比较 相对布比卡因组与利多卡因组,罗哌卡因组患者在感觉阻滞起效的时间上较长(P < 0.05)。相对布比卡因组与利多卡因组,罗哌卡因组患者阻滞平面固定的时间长、最高阻滞平面大、麻醉过程持续的时间长(P < 0.05)。布比卡因组与利多卡因组患者用药麻醉后在感觉阻滞起效的时间、阻滞平面固定的时间、最高阻滞平面以及麻醉过程持续的时间上相比差异无显著性意义(P > 0.05)。见表3。 通过对3组患者运动神经阻滞效果进行Bromage评级比较可知,3组患者运动神经阻滞效果总体都比较好。相对布比卡因组与利多卡因组,罗哌卡因组患者评级效果更好,具有显著的优势(P < 0.05)。布比卡因组与利多卡因组患者评级效果差异无显著性意义(P > 0.05)。 2.5 各组患者麻醉中不良反应情况的比较 通过对3组患者麻醉后的不良反应情况进行统计分析可得,布比卡因组有1例(3.8%)出现了低血压现象,利多卡因组有1例(3.8%)出现了心律失常现象,但是情况都不严重,都得到了及时、有效的控制,3组患者在术中不良反应方面总体表现都比较好。3组患者在恶心、呕吐、头痛、呼吸抑制、低血压、心律失常等不良反应方面差异无显著性意义(P > 0.05)。"
| [1] 韩金宝, 毕郑钢.老年股骨头缺血坏死的临床诊断及治疗现状[J].中国老年学杂志, 2012,32(5):1089-1091. [2] 孙晓娟, 张红星, 董补怀, 等.连续髂筋膜阻滞和硬膜外阻滞下行全髋置换后镇痛的比较[J].中国组织工程研究, 2014,18(31): 4934-4938. [3] 李民, 胡秋芳, 杨高.不同麻醉管理方法对双侧全膝关节置换术后栓塞的预防[J].河北医药, 2014,36(3):359-360. [4] 李帅, 李万里.局部麻醉药物的不良反应及预防[J].海军医学杂志, 2010,31(4):383. [5] 杨程, 闫诺, 杨宜平.左旋布比卡因、盐酸罗哌卡因、氯普鲁卡因术后持续硬膜外自控镇痛效应研究[J].海南医学院学报, 2012, 18(4):548-550. [6] 丁生权, 张文艺, 王建功, 等.氯普鲁卡因、布比卡因和罗哌卡因在下肢手术腰-硬联合麻醉中的比较[J].临床麻醉学杂志, 2011, 27(8):772-774. [7] 黄邵强, 王婷婷, 李宁, 等.三种不同局麻药腰麻最大运动阻滞效应的比较[J].临床麻醉学杂志, 2010,26(8):670-673. [8] 张涛, 陈建伟, 徐康清, 等.蛛网膜下腔注射罗哌卡因与布比卡因运动神经阻滞效力的比较[J].中华麻醉学杂志, 2011, 31(2): 214-216. [9] 杨进国, 任凌云, 曾文强.不同麻醉药物在髋关节置换术临床应用中的对比研究[J].医学综述, 2013,19(15):2862-2863. [10] 范捷.0.2%罗哌卡因在高龄病人髋部手术的应用[J].中医正骨, 2009,21(12):46-47. [11] 张铨, 卓飞豹, 阮丁异, 等.轻比重0.5%罗哌卡因腰麻在高龄髋关节及下肢手术的应用[J].临床麻醉学杂志,2010,26(12):1095. [12] Lirk P, Hollmann MW, Fleischer M, et al. Lidocaine and ropivacaine, but not bupivacaine, demethylate deoxyribonucleic acid in breast cancer cells in vitro. Br J Anaesth. 2014;113 Suppl 1:i32-i38. [13] Taha AM, Abd-Elmaksoud AM. Ropivacaine in ultrasound- guided femoral nerve block: what is the minimal effective anaesthetic concentration (EC90)? Anaesthesia. 2014;69(7): 678-682. [14] Baptista-Hon DT, Robertson FM, Robertson GB, et al.Potent inhibition by ropivacaine of metastatic colon cancer SW620 cell invasion and NaV1.5 channel function. Br J Anaesth. 2014;113 Suppl 1:i39-i48. [15] Widfeldt N, Kolmodin L. CNS symptoms of ropivacaine in bloodless field disappeared with Intralipid. Lakartidningen. 2014;111(16-17):742-743. [16] Yakoshi C, Hashimoto H, Niwa H, et al. Analgesic efficacy and clinical safety of intraperitoneal instillation combined with rectus sheath block using ropivacaine for pain relief after laparoscopic gynecological surgery. Masui. 2014;63(3): 296-302. [17] Gao W, Xi JH, Ju NY, et al. Ropivacaine via trans-cricothyroid membrane injection inhibits the extubation response in patients undergoing surgery for maxillary and mandibular fractures. Genet Mol Res. 2014;13(1):1635-1642. [18] Gill AM, Scott NB, Abbas M, et al. Ropivacaine plasma levels following local infiltration analgesia for primary total hip arthroplasty. Anaesthesia. 2014;69(4):368-373. [19] Baptista JF, Gomez RS, Paulo DN, et al. Epidural anesthesia with ropivacaine with or without clonidine and postoperative pain in hemorrhoidectomies. Acta Cir Bras. 2014;29(3): 201-208. [20] Piegeler T, Votta-Velis EG, Bakhshi FR, et al. Endothelial barrier protection by local anesthetics: ropivacaine and lidocaine block tumor necrosis factor-α-induced endothelial cell Src activation. Anesthesiology. 2014;120(6):1414-1428. [21] Hotta A, Yagi Y, Hakata S, et al. Case of Leriche's syndrome treated with safe and effective analgesia after laparotomy by transversus abdominis plane block, rectus sheath block, and continuous wound infusion with ropivacaine. Masui. 2013; 62(12):1461-1465. [22] Kim EM, Lee JR, Koo BN, et al. Analgesic efficacy of caudal dexamethasone combined with ropivacaine in children undergoing orchiopexy. Br J Anaesth. 2014;112(5):885-891. [23] Yoshida T, Fujiwara T, Furutani K, et al. Effects of ropivacaine concentration on the spread of sensory block produced by continuous thoracic paravertebral block: a prospective, randomised, controlled, double-blind study. Anaesthesia. 2014;69(3):231-239. [24] McDermott AM, Chang KH, Mieske K, et al. Total systemic ropivacaine concentrations following aerosolized intraperitoneal delivery using the AeroSurge. J Clin Anesth. 2014;26(1):18-24. [25] Niknam F, Saxena A, Niles N, et al. Does irrigation of the subdiaphragmatic region with ropivacaine reduce the incidence of right shoulder tip pain after laparoscopic cholecystectomy? A prospective randomized, double-blind, controlled study. Am Surg. 2014;80(1):E17-E18. [26] Theodosiadis P, Sachinis N, Goroszeniuk T, et al. Ropivacaine versus bupivacaine for 3-in-1 block during total knee arthroplasty. J Orthop Surg (Hong Kong). 2013;21(3):300-304. [27] Thomassen BJ, Touw D, van der Woude P, et al. Safety of blood reinfusion after local infiltration analgesia with ropivacaine in total knee arthroplasty. Int J Clin Pharmacol Ther. 2014;52(2):135-142. [28] Ok SH, Han JY, Sung HJ, et al. Ropivacaine-induced contraction is attenuated by both endothelial nitric oxide and voltage-dependent potassium channels in isolated rat aortae. Biomed Res Int. 2013;2013:565271. [29] Liu HL, Ma CH, Zhang XQ, et al. Combined efficacy of parecoxib and incisional ropivacaine infiltration on pain management after diagnostic hysteroscopy and laparoscopy. Beijing Da Xue Xue Bao. 2013;45(6):901-905. [30] Wilson SH, Auroux AS, Eloy JD, et al. Ropivacaine 0.1% versus 0.2% for continuous lumbar plexus nerve block infusions following total hip arthroplasty: a randomized, double blinded study.Pain Med. 2014;15(3):465-472. [31] Fritsch G, Danninger T, Allerberger K, et al. Dexmedetomidine added to ropivacaine extends the duration of interscalene brachial plexus blocks for elective shoulder surgery when compared with ropivacaine alone: a single-center, prospective, triple-blind, randomized controlled trial. Reg Anesth Pain Med. 2014;39(1):37-47. [32] Bleckner L, Solla C, Fileta BB, et al. Serum free ropivacaine concentrations among patients receiving continuous peripheral nerve block catheters: is it safe for long-term infusions? Anesth Analg. 2014;118(1):225-229. [33] Yue HL, Shao LJ, Li J, et al. Effect of epidural analgesia with 0.075% ropivacaine versus 0.1% ropivacaine on the maternal temperature during labor: a randomized controlled study. Chin Med J (Engl). 2013;126(22):4301-4305. [34] Kato A, Koitabashi T, Masuda S, et al. Comparison of the efficacy of ropivacaine and that of levobupivacaine for postoperative epidural analgesia in patients undergoing gynecological open abdominal surgery. Masui. 2013; 62(10): 1160-1165. [35] Abbas M, Ahmad L, Shah Y, et al. Development of a method to measure free and bound ropivacaine in human plasma using equilibrium dialysis and hydrophilic interaction chromatography coupled to high resolution mass spectrometry. Talanta. 2013;117:60-63. [36] Parikh GP, Shah VR, Vora KS, et al. Ultrasound guided peritubal infiltration of 0.25% ropivacaine for postoperative pain relief in percutaneous nephrolithotomy. Middle East J Anaesthesiol. 2013;22(2):149-154. [37] Gencer ZK, Ozkiri? M, Gencer M, et al. Comparison of ropivacaine, bupivacaine, prilocaine, and lidocaine in the management of pain and hemorrhage during nasal pack removal. Am J Rhinol Allergy. 2013;27(5):423-425. [38] Nader A, Kendall MC, De Oliveira GS Jr, et al. A dose-ranging study of 0.5% bupivacaine or ropivacaine on the success and duration of the ultrasound-guided, nerve-stimulator-assisted sciatic nerve block: a double-blind, randomized clinical trial. Reg Anesth Pain Med. 2013;38(6):492-502. [39] Kulkarni K, Namazi IJ, Deshpande S, et al. Cervical epidural anaesthesia with ropivacaine for modified radical mastectomy. Kathmandu Univ Med J (KUMJ). 2013;11(42):126-131. [40] Ju NY, Cui GX, Gao W. Ropivacaine plus dexamethasone infiltration reduces postoperative pain after tonsillectomy and adenoidectomy. Int J Pediatr Otorhinolaryngol. 2013;77(11): 1881-1885. [41] Lin YN, Li Q, Yang RM, et al. Addition of dexmedetomidine to ropivacaine improves cervical plexus block. Acta Anaesthesiol Taiwan. 2013;51(2):63-66. [42] 李建, 金国光, 叶卫东.左旋布比卡因与布比卡因蛛网膜下腔麻醉在老年前列腺手术中麻醉效果的比较[J].中华全科医师杂志, 2011,10(7):501-503. [43] Hampl K, Steinfeldt T, Wulf H. Spinal anesthesia revisited: toxicity of new and old drugs and compounds. Curr Opin Anaesthesiol. 2014;27(5):549-555. [44] Covino BG. Toxicity of local anesthetic agents. Acta Anaesthesiol Belg. 1988;39(3 Suppl 2):159-164. [45] Myers RR, Kalichman MW, Reisner LS, et al. Neurotoxicity of local anesthetics: altered perineurial permeability, edema, and nerve fiber injury. Anesthesiology. 1986;64(1):29-35. [46] Ready LB, Plumer MH, Haschke RH, et al. Neurotoxicity of intrathecal local anesthetics in rabbits. Anesthesiology. 1985; 63(4):364-370. [47] Corke BC, Spielman FJ. Problems associated with epidural anesthesia in obstetrics. Obstet Gynecol. 1985;65(6): 837-839. [48] Li DF, Bahar M, Cole G, et al. Neurological toxicity of the subarachnoid infusion of bupivacaine, lignocaine or 2-chloroprocaine in the rat. Br J Anaesth. 1985;57(4): 424-429. [49] Rosen MA, Baysinger CL, Shnider SM, et al. Evaluation of neurotoxicity after subarachnoid injection of large volumes of local anesthetic solutions. Anesth Analg. 1983;62(9):802-808. [50] Barsa J, Batra M, Fink BR, et al. A comparative in vivo study of local neurotoxicity of lidocaine, bupivacaine, 2-chloroprocaine, and a mixture of 2-chloroprocaine and bupivacaine. Anesth Analg. 1982;61(12):961-967. [51] Ravindran RS, Turner MS, Muller J. Neurologic effects of subarachnoid administration of 2-chloroprocaine-CE, bupivacaine, and low pH normal saline in dogs. Anesth Analg. 1982;61(3):279-283. [52] Moore DC, Spierdijk J, vanKleef JD, et al. Chloroprocaine neurotoxicity: four additional cases. Anesth Analg. 1982;61(2): 155-159. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [3] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [4] | Zhang Nianjun, Chen Ru. Analgesic effect of cocktail therapy combined with femoral nerve block on total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 866-872. |
| [5] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [6] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [7] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [8] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [9] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [10] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [11] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [12] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [13] | Cheng Chongjie, Yan Yan, Zhang Qidong, Guo Wanshou. Diagnostic value and accuracy of D-dimer in periprosthetic joint infection: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3921-3928. |
| [14] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [15] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||