Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (24): 3921-3928.doi: 10.12307/2021.103
Previous Articles Next Articles
Diagnostic value and accuracy of D-dimer in periprosthetic joint infection: a systematic review and meta-analysis
Cheng Chongjie1, 2, 3, Yan Yan3, 4, Zhang Qidong1, 3, Guo Wanshou1, 2, 3
- 1Graduate School of Peking Union Medical College, Beijing 100730, China; 2China-Japan Friendship Institute of Clinical Medicine, Beijing 100029, China; 3Department of Orthopedic Surgery, China-Japan Friendship Hospital, Beijing 100029, China; 4China-Japan Friendship Institute of Clinical Medicine, Peking University, Beijing 100029, China
-
Received:2020-10-09Revised:2020-10-12Accepted:2020-11-09Online:2021-08-28Published:2021-03-18 -
Contact:Guo Wanshou, MD, Professor, Doctoral supervisor, Graduate School of Peking Union Medical College, Beijing 100730, China; China-Japan Friendship Institute of Clinical Medicine, Beijing 100029, China; Department of Orthopedic Surgery, China-Japan Friendship Hospital, Beijing 100029, China -
About author:Cheng Chongjie, Master candidate, physician, Graduate School of Peking Union Medical College, Beijing 100730, China; China-Japan Friendship Institute of Clinical Medicine, Beijing 100029, China; Department of Orthopedic Surgery, China-Japan Friendship Hospital, Beijing 100029, China -
Supported by:the National Natural Science Foundation of China, No. 81972130 (to GWS)
CLC Number:
Cite this article
Cheng Chongjie, Yan Yan, Zhang Qidong, Guo Wanshou. Diagnostic value and accuracy of D-dimer in periprosthetic joint infection: a systematic review and meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3921-3928.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
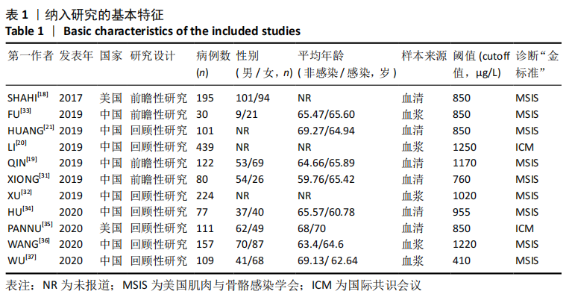
纳入的11篇文献共包含1 645例患者,其中515例患者被确诊假体周围感染,1 130例患者被排除假体周围感染。各研究的基本特征和所有病例的人口统计学数据见表1。所有纳入的患者均为全髋关节置换后或全膝关节置换后,所有纳入的研究均来自于中国或美国。其中4项研究是前瞻性研究[18-19,31,33],另外7项研究为回顾性研究[20-21,32,34-37]。其中5项研究使用血浆样本量化患者的血D-二聚体数值[20,32-33,36-37],另外6项研究使用血清样本量化患者的血D-二聚体数值[18-19,21,31,34-35]。其中9项研究采用2011 MSIS标准作为诊断假体周围感染的“金标准”[18-19,21,31-34,36-37],另有2项研究采用2013 ICM标准作为诊断假体周围感染的“金标准”[20,35]。"
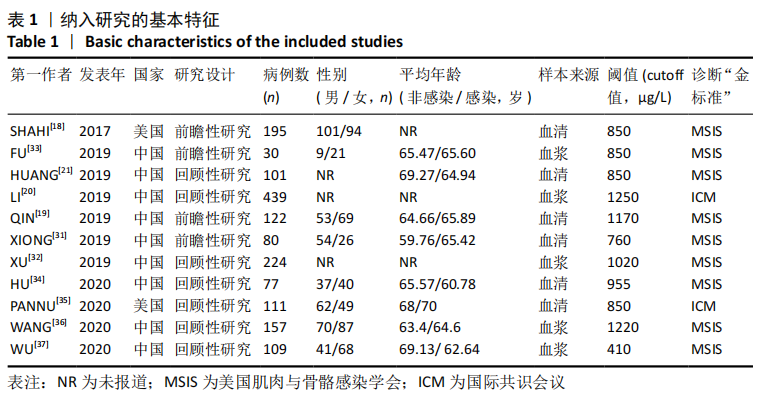
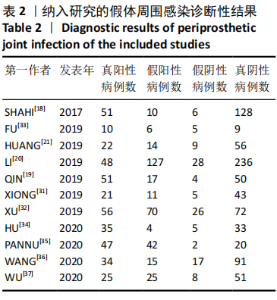
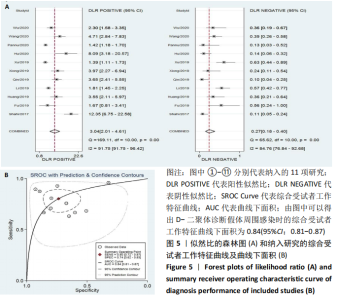
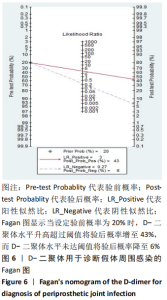
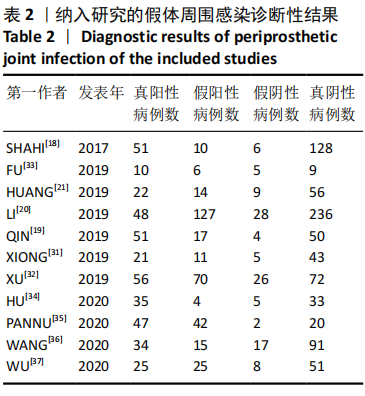
2.3 D-二聚体在诊断假体周围感染中的阈值和准确性结果 有4项研究使用850 μg/L作为D-二聚体升高诊断假体周围感染的阈值[18,21,33,35],850 μg/L同时也是2018 ICM所推荐使用D-二聚体辅助诊断假体周围感染的阈值[17,38]。另有5项研究使用的D-二聚体阈值高于850 μg/L[19-20,32,34,36],有2项研究使用的D-二聚体阈值低于850 μg/L[31,37]。 各研究中使用D-二聚体诊断假体周围感染时的真阳性、假阳性、假阴性及真阴性具体病例数见表2。D-二聚体在诊断假体周围感染时的敏感性为0.80(95%CI,0.72-0.87),特异性为0.74(95%CI:0.62-0.83),但各研究间的异质性较明显,合并敏感性的I2值为79.42%(95%CI:67.82%-91.01%),合并特异性的I2值为93.30%(95%CI:90.56%-96.05%),见图4A。合并的诊断分数及诊断优势比分别为2.43(95%CI:1.70-3.16)和11.40(95%CI:5.50-23.63),见图4B。合并的阳性似然比(PLR)和阴性似然比(NLR)分别为3.04(95%CI:2.01-4.61)和0.27(95%CI:0.18-0.40),见图5A。综合受试者工作特征曲线(SROC)下面积(AUC)为0.84(95%CI:0.81-0.87),见图5B。 有文献报道,假体周围感染约占所有关节置换后翻修原因的20%[39],所以文章将诊断假体周围感染时的验前概率设定为20%(代表未进行血清或血浆D-二聚体水平检测时,待进一步确诊的患者有20%的概率罹患假体周围感染),以此得出Fagan图,见图6。如Fagan图所示,当患者血清或血浆D-二聚体水平升高超过阈值时,其罹患假体周围感染的验后概率增加至43%,而如果患者血清或血浆D-二聚体水平未达阈值,其罹患假体周围感染的概率降至6%。"
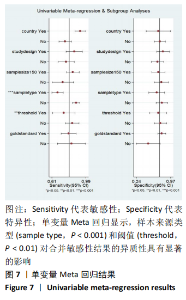
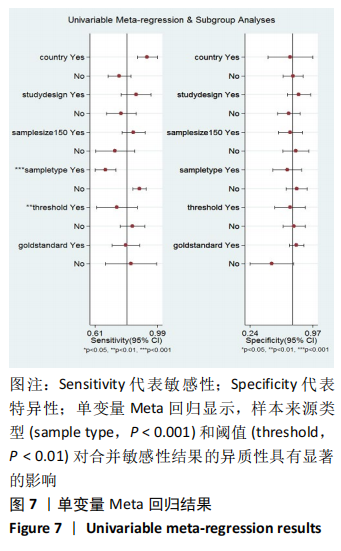
2.4 基于Meta回归和亚组分析的异质性分析结果 所纳入的文献之间具有较高的异质性,见图4,在其存在异质性的以下几个方面:研究设计类型,标本来源类型,阈值,研究对象所处的国家或地区,样本量和确诊的“金标准”,使用单变量Meta回归方式来寻找潜在的异质性来源,见图7,样本来源类型(sample type,P < 0.001)和阈值(threshold,P < 0.01)对合并敏感性结果的异质性具有显著的影响。于是文章基于以上两方面进行了亚组分析,以进一步探索异质性来源,见表3。在血清D-二聚体的亚组结果中,合并的敏感性和特异性分别为0.88(95%CI:0.81-0.93)和0.78(95%CI:0.61-0.90);在血浆D-二聚体的亚组结果中,合并的敏感性和特异性均为0.67,95%CI分别为0.61-0.73和0.55-0.78。血清D-二聚体亚组和血浆D-二聚体亚组的AUC值分别为0.91(95%CI:0.89-0.94)和0.68(95%CI:0.64-0.72)。在设定阈值> 1 000 μg/L的亚组中,合并的敏感性、特异性和AUC值分别为0.74(95%CI:0.59-0.86),0.70(95%CI:0.56-0.82),0.79(95%CI:0.75-0.82);在设定阈值≤ 1 000 μg/L的亚组中,合并的敏感性、特异性、AUC分别为0.84(95%CI:0.75-0.90),0.76(95%CI:0.59-0.87)和0.87 (95%CI:0.84-0.90)。文章计算了各研究间敏感性与1-特异性对数的Spearman相关系数为-0.137,P=0.689,表明异质性来源并非阈值效应。"
| [1] KURTZ S, ONG K, LAU E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am. 2007;89(4):780-785. [2] JAFARI SM, COYLE C, MORTAZAVI SMJ, et al. Revision hip arthroplasty: infection is the most common cause of failure. Clin Orthop Relat Res. 2010;468(8):2046-2051. [3] URISH K L, QIN Y, SALKA B, et al. Comparison of readmission and early revision rates as a quality metric in total knee arthroplasty using the Nationwide Readmission Database. Ann Transl Med. 2020;8(11):687. [4] PARVIZI J, PAWASARAT IM, AZZAM KA, et al. Periprosthetic joint infection. J Arthroplasty. 2010; 25(6):103-107. [5] BOZIC KJ, KURTZ SM, LAU E, et al. The epidemiology of revision total knee arthroplasty in the United States. Clin Orthop Relat Res. 2010,468(1):45-51. [6] KAPADIA BH, BERG RA, DALEY JA, et al. Periprosthetic joint infection. Lancet. 2016;387(10016):386-394. [7] FINK B, ANAGNOSTAKOS K, WINKLER H. Periprosthetic Joint Infection. BioMed Res Int. 2019;2019:1-2. [8] FEHRING TK, ODUM SM, BEREND KR, et al. Failure of irrigation and débridement for early postoperative periprosthetic infection. Clin Orthop Relat Res. 2013;471(1):250-257. [9] BABIS GC. Another candidate marker for preoperative diagnosis of periprosthetic joint infection. J Bone Joint Surg. 2019;101(7):e30. [10] PARVIZI J, ZMISTOWSKI B, BERBARI E F, et al. New definition for periprosthetic joint infection: from the Workgroup of the Musculoskeletal Infection Society. Clin Orthop Relat Res. 2011;469(11):2992-2994. [11] ZMISTOWSKI B, DELLA VC, BAUER TW, et al. Diagnosis of periprosthetic joint infection. J Arthroplasty. 2014;29(2 Suppl):77-83. [12] LI C, OJEDA-THIES C, TRAMPUZ A. Culture of periprosthetic tissue in blood culture bottles for diagnosing periprosthetic joint infection. BMC Musculoskelet Disord. 2019;20(1):299. [13] MEERMANS G, HADDAD F S. Is there a role for tissue biopsy in the diagnosis of periprosthetic infection? Clin Orthop Relat Res. 2010;468(5):1410-1417. [14] SALEH A, GEORGE J, FAOUR M, et al. Serum biomarkers in periprosthetic joint infections. Bone Joint Res. 2018;7(1):85-93. [15] DEIRMENGIAN C, KARDOS K, KILMARTIN P, et al. Diagnosing periprosthetic joint infection: has the era of the biomarker arrived? Clin Orthop Relat Res. 2014;472(11):3254-3262. [16] PIPER KE, FERNANDEZ-SAMPEDRO M, STECKELBERG KE, et al. C-reactive protein, erythrocyte sedimentation rate and orthopedic implant infection. PLoS One. 2010;5(2):e9358. [17] PARVIZI J, TAN TL, GOSWAMI K, et al. The 2018 Definition of Periprosthetic Hip and Knee Infection: An Evidence-Based and Validated Criteria. J Arthroplasty. 2018;33(5):1309-1314. [18] SHAHI A, KHEIR MM, TARABICHI M, et al. Serum d-dimer test is promising for the diagnosis of periprosthetic joint infection and timing of reimplantation. J Bone Joint Surg. 2017;99(17):1419-1427. [19] QIN L, LI F, GONG X, et al. Combined measurement of d-dimer and c-reactive protein levels: highly accurate for diagnosing chronic periprosthetic joint infection. J Arthroplasty. 2020;35(1):229-234. [20] LI R, SHAO H, HAO L, et al. Plasma fibrinogen exhibits better performance than plasma d-dimer in the diagnosis of periprosthetic joint infection. J Bone Joint Surg. 2019;101(7):613-619. [21] HUANG J, ZHANG Y, WANG Z, et al. The serum level of D-Dimer is not suitable for distinguishing between prosthetic joint infection and aseptic loosening. J Orthop Surg Res. 2019;14(1):407. [22] MOHER D, LIBERATI A, TETZLAFF J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535. [23] WHITING PF, RUTJES AWS, WESTWOOD ME, et al. QUADAS-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann Int Med. 2011;155(8):529. [24] VAN HOUWELINGEN HC, ZWINDERMAN KH, STIJNEN T. A bivariate approach to meta-analysis. Stat Med. 1993;12(24):2273-2284. [25] REITSMA JB, GLAS AS, RUTJES AWS, et al. Bivariate analysis of sensitivity and specificity produces informative summary measures in diagnostic reviews. J Clin Epidemiol. 2005;58(10):982-990. [26] CHU H, COLE SR. Bivariate meta-analysis of sensitivity and specificity with sparse data: a generalized linear mixed model approach. J Clin Epidemiol. 2006;59(12):1331-1332. [27] RILEY RD, ABRAMS KR, SUTTON AJ, et al. Bivariate random-effects meta-analysis and the estimation of between-study correlation. BMC Med Res Methodol. 2007;7(1):3. [28] WACKER C, PRKNO A, BRUNKHORST F M, et al. Procalcitonin as a diagnostic marker for sepsis: a systematic review and meta-analysis. Lancet Infect Dis. 2013;13(5):426-435. [29] HIGGINS JPT, THOMPSON SG, DEEKS JJ, et al. Measuring inconsistency in meta-analyses. BMJ. 2003;327(7414):557-560. [30] DEEKS JJ, MACASKILL P, IRWIG L. The performance of tests of publication bias and other sample size effects in systematic reviews of diagnostic test accuracy was assessed. J Clin Epidemiol. 2005;58(9):882-893. [31] XIONG L, LI S, DAI M. Comparison of D-dimer with CRP and ESR for diagnosis of periprosthetic joint infection. J Orthop Surg Res. 2019;14(1):240. [32] XU H, XIE J, HUANG Q, et al. Plasma fibrin degradation product and d-dimer are of limited value for diagnosing periprosthetic joint infection. J Arthroplasty. 2019;34(10):2454-2460. [33] FU J, NI M, CHAI W, et al. Synovial fluid viscosity test is promising for the diagnosis of periprosthetic joint infection. J Arthroplasty. 2019;34(6):1197-1200. [34] HU Q, FU Y, TANG L. Serum D-dimer as a diagnostic index of PJI and retrospective analysis of etiology in patients with PJI. Clinica Chimica Acta. 2020;506:67-71. [35] PANNU TS, VILLA JM, PATEL PD, et al. The utility of serum d-dimer for the diagnosis of periprosthetic joint infection in revision total hip and knee arthroplasty. J Arthroplasty. 2020;35(6):1692-1695. [36] WANG Y, LI Y, QIAO L, et al. Comparison of a comprehensive set of fibrinolytic markers with c-reactive protein and erythrocyte sedimentation rate for the diagnosis of periprosthetic joint infection. J Arthroplasty. 2020;35(9):2613-2618. [37] WU H, MENG Z, PAN L, et al. Plasma fibrinogen performs better than plasma d-dimer and fibrin degradation product in the diagnosis of periprosthetic joint infection and determination of reimplantation timing. J Arthroplasty. 2020;35(8):2230-2236. [38] ABDELAZIZ H, RADEMACHER K, SUERO E M, et al. The 2018 international consensus meeting minor criteria for chronic hip and knee periprosthetic joint infection: validation from a single center. J Arthroplasty. 2020;35(8):2200-2203. [39] XIE K, DAI K, QU X, et al. Serum and synovial fluid interleukin-6 for the diagnosis of periprosthetic joint infection. Sci Rep. 2017;7(1):1496. [40] PUPAIBOOL J, FULNECKY EJ, SWORDS RJ, et al. Alpha-defensin-novel synovial fluid biomarker for the diagnosis of periprosthetic joint infection. Int Orthop. 2016;40(12):2447-2452. [41] CHISARI E, PARVIZI J. Accuracy of blood-tests and synovial fluid-tests in the diagnosis of periprosthetic joint infections. Expert Rev Anti Infect Ther. 2020. doi: 10.1080/14787210.2020.1792771. [42] GLEHR M, FRIESENBICHLER J, HOFMANN G, et al. Novel biomarkers to detect infection in revision hip and knee arthroplasties. Clin Orthop Relat Res. 2013;471(8):2621-2628. [43] GALLIERA E, DRAGO L, MARAZZI M G, et al. Soluble urokinase-type plasminogen activator receptor (suPAR) as new biomarker of the prosthetic joint infection: correlation with inflammatory cytokines. Clin Chim Acta. 2015;441:23-28. [44] HUGLE T, SCHUETZ P, MUELLER B, et al. Serum procalcitonin for discrimination between septic and non-septic arthritis. Clin Exp Rheumatol. 2008;26(3):453-456. [45] MUMINGJIANG Y, ZHOU X, HE R. Value of knee skin temperature measured by infrared thermography and soluble intercellular adhesion molecule-1 in the diagnosis of peri-prosthetic knee infection in Chinese individuals following total knee arthroplasty. Chin Med J (Engl). 2014;127(17):3105-3109. [46] DAPUNT U, GIESE T, MAURER S, et al. Neutrophil-derived MRP-14 is up-regulated in infectious osteomyelitis and stimulates osteoclast generation. J Leukoc Biol. 2015;98(4):575-582. [47] ETTINGER M, CALLIESS T, KIELSTEIN JT, et al. Circulating biomarkers for discrimination between aseptic joint failure, low-grade infection, and high-grade septic failure. Clin Infect Dis. 2015;61(3):332-341. [48] FRANGIAMORE SJ, GAJEWSKI ND, SALEH A, et al. Alpha-defensin accuracy to diagnose periprosthetic joint infection-best available test? J Arthroplasty. 2016;31(2):456-460. [49] HANSRANI V, KHANBHAI M, MCCOLLUM C. The diagnosis and management of early deep vein thrombosis. Adv Exp Med Biol. 2017;906:23-31. [50] SCHWAMEIS M, STEINER MM, SCHOERGENHOFER C, et al. D-dimer and histamine in early stage bacteremia: a prospective controlled cohort study. Eur J Intern Med. 2015;26(10):782-786. [51] LEE JW, HER SM, KIM JH, et al. D-dimer as a marker of acute pyelonephritis in infants younger than 24 months with urinary tract infection. Pediatr Nephrol. 2018;33(4):631-637. [52] TURAK O, CANPOLAT U, OZCAN F, et al. D-dimer level predicts in-hospital mortality in patients with infective endocarditis: a prospective single-centre study. Thromb Res. 2014;134(3):587-592. [53] MELE N, TURC G. Stroke associated with recent mycoplasma pneumoniae infection: a systematic review of clinical features and presumed pathophysiological mechanisms. Front Neurol. 2018;9:1109. [54] RIBERA T, MONREAL L, ARMENGOU L, et al. Synovial fluid D-dimer concentration in foals with septic joint disease. J Vet Intern Med. 2011;25(5):1113-1117. [55] ISKANDER KN, OSUCHOWSKI MF, STEARNS-KUROSAWA DJ, et al. Sepsis: multiple abnormalities, heterogeneous responses, and evolving understanding. Physiol Rev. 2013;93(3):1247-1288. [56] LIBBY P, SIMON DI. Inflammation and thrombosis: the clot thickens. Circulation. 2001;103(13):1718-1720. [57] BAUER TW, BEDAIR H, CREECH JD, et al. Hip and knee section, diagnosis, laboratory tests: proceedings of international consensus on orthopedic infections. J Arthroplasty. 2019;34(2S):S351-S359. [58] ZHANG H, SUN X, XIN P, et al. Diagnostic accuracy of D-dimer in periprosthetic joint infection: a diagnostic meta-analysis. J Orthop Surg Res. 2020;15(1):334. [59] LU G, LI T, YE H, et al. D-dimer in the diagnosis of periprosthetic joint infection: a systematic review and meta-analysis. J Orthop Surg Res. 2020;15(1):265. [60] LI C, MARGARYAN D, OJEDA-THIES C, et al. Meta-analysis of serum and/or plasma D-dimer in the diagnosis of periprosthetic joint infection. J Orthop Surg Res. 2020;15(1):298. [61] CARLI AV, ABDELBARY H, AHMADZAI N, et al. Diagnostic accuracy of serum, synovial, and tissue testing for chronic periprosthetic joint infection after hip and knee replacements: a systematic review. J Bone Joint Surg Am. 2019;101(7):635-649. [62] BOISCLAIR MD, LANE DA, WILDE JT, et al. A comparative evaluation of assays for markers of activated coagulation and/or fibrinolysis: thrombin-antithrombin complex, D-dimer and fibrinogen/fibrin fragment E antigen. Br J Haematol. 1990;74(4):471-479. [63] KORTE W, RIESEN W. Latex-enhanced immunoturbidimetry allows D-dimer determination in plasma and serum samples. Clin Chem. 2000; 46(6 Pt 1):871-872. [64] BOISCLAIR MD, LANE DA, WILDE JT, et al. A comparative evaluation of assays for markers of activated coagulation and/or fibrinolysis: thrombin–antithrombin complex, D-dimer and fibrinogen/fibrin fragment E antigen. Br J Haematol. 1990;74(4):471-479. [65] LEE YS, LEE YK, HAN SB, et al. Natural progress of D-dimer following total joint arthroplasty: a baseline for the diagnosis of the early postoperative infection. J Orthop Surg Res. 2018; 13(1):36. [66] CHEN CJ, WANG CJ, HUANG CC. The value of D-dimer in the detection of early deep-vein thrombosis after total knee arthroplasty in Asian patients: a cohort study. Thromb J. 2008;6:5. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [5] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [6] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [7] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [8] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [9] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [10] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [11] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [12] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [13] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [14] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| [15] | Liang Yan, Zhao Yongfei, Xu Shuai, Zhu Zhenqi, Wang Kaifeng, Liu Haiying, Mao Keya. Imaging evaluation of short-segment fixation and fusion for degenerative lumbar scoliosis assisted by highly selective nerve root block [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1423-1427. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||