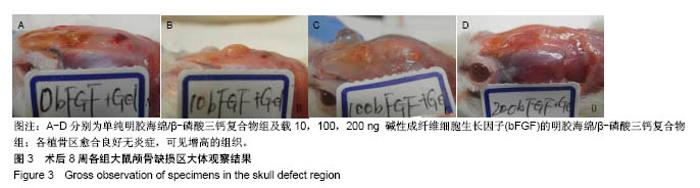
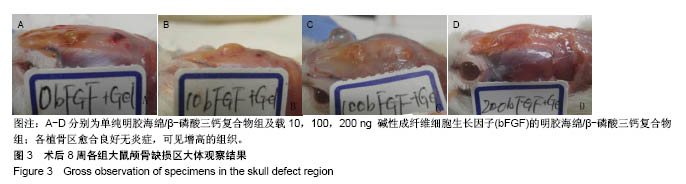
Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (2): 190-195.doi: 10.3969/j.issn.2095-4344.1506
Previous Articles Next Articles
Effect of gelatin sponge/beta-tricalcium phosphate composite with different doses of basic fibroblast growth factor on bone regeneration
Cui Tingting1, Qiu Zewen2, Gui Lin1, Zhong Weijian1, Ma Guowu1
- 1Hospital of Stomatology, Stomatology College of Dalian Medical University, Dalian 116023, Liaoning Province, China; 2Animal Laboratory Center, Dalian Medical University, Dalian 116044, Liaoning Province, China
-
Received:2018-08-17Online:2019-01-18Published:2019-01-18 -
Contact:Zhong Weijian, Associate professor, Master’s supervisor, Hospital of Stomatology, Stomatology College of Dalian Medical University, Dalian 116023, Liaoning Province, China -
About author:Cui Tingting, Master candidate, Hospital of Stomatology, Stomatology College of Dalian Medical University, Dalian 116023, Liaoning Province, China -
Supported by:the Natural Science Foundation of Liaoning Province, No. 2015010313-301 (to ZWJ)
CLC Number:
Cite this article
Cui Tingting, Qiu Zewen, Gui Lin, Zhong Weijian, Ma Guowu. Effect of gelatin sponge/beta-tricalcium phosphate composite with different doses of basic fibroblast growth factor on bone regeneration[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(2): 190-195.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
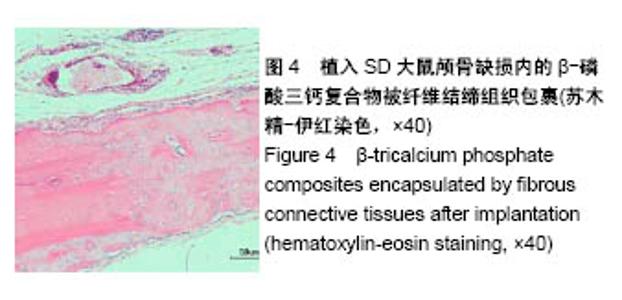
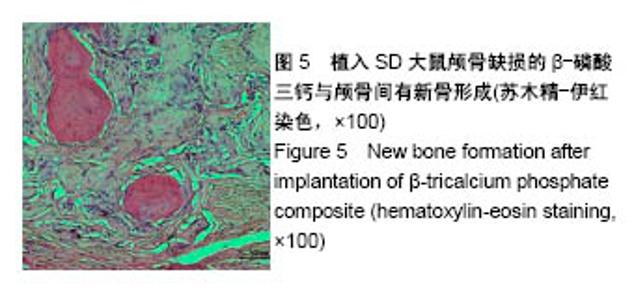
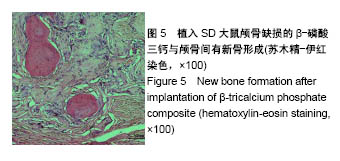
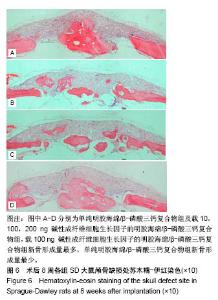
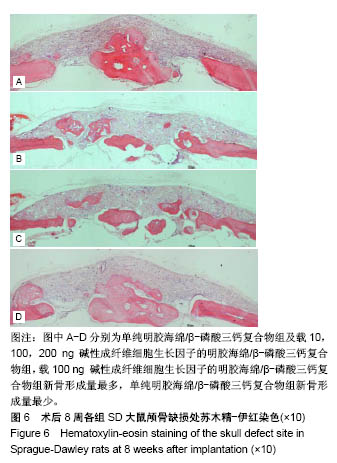
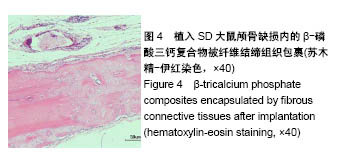
2.2 组织学观察结果 术后8周取材(只选取存活大鼠),经固定、包埋和光镜下苏木精-伊红染色可见,明胶海绵/β-磷酸三钙复合物被大量的纤维结缔组织包裹,见图4,纤维结缔组织中可见大量的新生血管及淋巴细胞,在β-磷酸三钙颗粒周围可见巨噬细胞,β-磷酸三钙颗粒未见明显吸收,β-磷酸三钙与颅骨间有新骨形成,见图5,载100 ng bFGF的明胶海绵/β-磷酸三钙复合物组新骨形成的量最多,其次是载10,200 ng bFGF的明胶海绵/β-磷酸三钙复合物组,最后是单纯明胶海绵/β-磷酸三钙复合物组,见图6。新骨的骨小梁之间有较多活跃的骨细胞,编织骨结构紊乱,编织骨的下方为成熟的板层骨,是未经破坏的原有颅骨。 2.3 统计学分析结果 单纯明胶海绵/β-磷酸三钙复合物组及载10,100,200 ng碱性成纤维细胞生长因子的明胶海绵/β-磷酸三钙复合物组的新骨生成率分别为(13.37± 1.32)%,(25.68±2.01)%,(31.39±2.31)%,(22.54±0.98)%,除载10 ng碱性成纤维细胞生长因子的明胶海绵/β-磷酸三钙复合物组与载200 ng碱性成纤维细胞生长因子的明胶海绵/β-磷酸三钙复合物组新骨生成率比较差异无显著性意义外,其余组间两两比较差异均有显著性意义(P < 0.05)。"
| [1] Masaoka T, Yamada T, Yuasa M, et al. Biomechanical evaluation of the rabbit tibia after implantation of porous hydroxyapatite/collagen in a rabbit model. J Orthop Sci. 2016; 21(2):230-236. [2] Omata K, Matsuno T, Kazunari A, et al. Enhanced bone regeneration by gelatin-β-tricalcium phosphate composites enabling controlled release of bFGF. J Tissue Eng Regen Med. 2014;8(3):604-611. [3] Andreas S, Frank W, Marcus H, et al. Autonomic bone grafts in oralimplantology—is it still a"gold standard? "A consecutive review of 279 patients with 456 clinical procedures. Int J Implant Dent. 2017; 46(1):3-23. [4] Azi ML, Aprato A, Santi I, et al. Autologous bone graft in the treatment of post-traumatic bone defects: a systematic review and meta-analysis. BMC Musculoskelet Disord. 2016; 17(1):465. [5] Rezende ML, Consolaro A, Sant'Ana AC, et al. Demineralization of the contacting surfaces in autologous onlay bone grafts improves bone formation and bone consolidation. J Periodontol. 2014;85(5):121-129. [6] Horowitz RA, Leventis MD. Bone grafting: history, rationale, and selection of materials and techniques. Compend Contin Educ Dent. 2014;35(4):1-6. [7] Liu J, Schmidlin P, Philipp A, et al. Novel bone substitute material in alveolar bone healing following tooth extraction: an experimental study in sheep. Clin Oral Implants Res. 2016;27(7):762-770. [8] Arima Y, Uemura N, Hashimoto Y, et al. Evaluation of bone regeneration by porous alpha-tricalcium phosphate/atelo-collagen sponge composite in rat calvarial defects. Orthod Waves. 2013;72(3): 23-29. [9] Li P, Hashimoto Y. The effect of interferon-γ and zoledronate treatment on alpha-tricalcium phosphate/collagen sponge-mediated bone-tissue engineering. Int J Mol Sci. 2015;16(3):25678-25690. [10] Ito T, Hashimoto Y, Baba S, et al. Bone regeneration with a collagen model polypeptides/ -tricalcium phosphate sponge in a canine tibia defect model. Implant. Dent. 2015;12(24):197-203. [11] Li P, Hashimoto Y, Honda Y, et al. The effect of interferon- and zoledronate treatment on alpha-tricalcium phosphate/collagen sponge-mediated bone-tissue engineering. Int J Mol Sci. 2015;23(16): 25678-25690. [12] Sun D, Wang W, Wang X, et al. bFGF plays a neuroprotective role by suppressing excessive autophagy and apoptosis after transient global cerebral ischemia in rats. Cell Death Dis. 2018;9(2):172. [13] Kakinoki S, Sakai Y, Fujisato T, et al. Accelerated tissue integration into porous materials by immobilizing basic fibroblast growth factor using a biologically safe three-step reaction. J Biomed Mater Res. 2015;103(6): 3790-3797. [14] O'Keefe RJ, Mao J. Bone tissue engineering and regeneration: from discovery to the clinic--an overview. Tissue Eng Part B Rev. 2011;17(6): 389-392. [15] Shrivats AR, McDermott MC, Hollinger J. Bone tissue engineering: state of the union. Drug Discov Today. 2014;19(6):781-786. [16] Venkatesan J, Nithya R, Sudha PN, et al. Role of alginate in bone tissue engineering. Adv Food Nutr Res. 2014;45(73):45-57. [17] Taktak R, Elghazel A, Bouaziz J, et al. Tricalcium phosphate- Fluorapatite as bone tissue engineering: Evaluation of bioactivity and biocompatibility. Mater Sci Eng C Mater Biol Appl. 2018;1(86):121-128. [18] Sionek A, Czwojdziński A, Kowalczewski J, et al. Hip osteonecroses treated with calcium sulfate-calcium phosphate bone graft substitute have different results according to the cause of osteonecrosis: alcohol abuse or corticosteroid-induced. Int Orthop. 2018;42(7):1491-1498. [19] Laverty DP, Kelly R, Addison O. Survival of dental implants placed in autogenousbonegrafts and bone flaps in head and neck oncology patients: a systematic review. Int J Implant Dent 2018;4(1):19. [20] Dos Santos Pereira R, Boos FB, Gorla LF, et al. Maxillary Sinus Elevation Surgery with ChronOS and Autogenous Bone Graft: Immunohistochemical Assessment of RUNX2, VEGF, TRAP, and Osteocalcin. Int J Periodontics Restorative Dent. 2017;37(6): e321-e327. [21] Noguchi T, Sarukawa S, Tsuchiya Y, et al. Evaluation of postoperative changes in vascularized iliac bone grafts used for mandibular reconstruction. Int J Oral Maxillofac Surg. 2018;47(8):990-997. [22] Sarikaya B, Aydin HM. Collagen/Beta-Tricalcium Phosphate Based Synthetic Bone Grafts via Dehydrothermal Processing. Biomed Mater. 2015;10(6):532-552. [23] Fonseca H, Moreira-Gonçalves D, Coriolano HJ, et al. Bone quality: the determinants of bone strength and fragility. Sports Med. 2014;44(1): 37-53. [24] Hamdy RC. Bone Mineral Density and Fractures. J Clin Densitom. 2016;19(2):125-126. [25] Zain NM, Seriramulu VP, Chelliah KK. Bone Mineral Density and Breast Cancer Risk Factors among Premenopausal and Postmenopausal Women A Systematic Review. Asian Pac J Cancer Prev. 2016;17(7):3229-3234. [26] Arahira T, Todo M. Variation of mechanical behavior of β-TCP/collagen two phase composite scaffold with mesenchymal stem cell in vitro. J Mech Behav Biomed Mater. 2016;16(61):464-474. [27] Xu L, Zhang W. Peri-Implant Bone Regeneration Using rhPDGF-BB, BMSCs, and β-TCP in a Canine Model. Clin Implant Dent Relat Res. 2016;8(2):241-252. [28] ?ivadinovi? M, Andri? M, Miloševi? V, et al. Histomorphometric evaluation of bone regeneration usingautogenous bone and beta-tricalcium phosphate in diabetic rabbits. Vojnosanit Pregl. 2016;73(12):1132-1138. [29] Ramesh N, Moratti SC, Dias GJ. Hydroxyapatite-polymer biocomposites for bone regeneration: A review of current trends. Journal of biomedical materials research. J Biomed Mater Res B Appl Biomater. 2018;106(5):2046-2057. [30] Huang YC, Chen CY, et al. Comparing morbidities of bone graft harvesting from theanterior iliac crest and proximal tibia: a retrospective study. J Orthop Surg Res. 2018;13(1):115. [31] Gross JB, Diligent J, Bensoussan D, et al. Percutaneous autologous bone marrow injection for treatment of delayed and non-union of long bone: a retrospective study of 45 cases. Biomed Mater Eng. 2015; 25(1):187-197. [32] Lee DH, Ryu KJ, Kim JW, et al. Bone marrow aspirate concentrate and platelet-rich plasma enhanced bone healing in distraction osteogenesis of the tibia. Clin Orthop Relat Res. 2014;472(12): 3789-3797. [33] Wu J, Cai XH, Qin XX, et al. The effects of sclerostin antibody plus parathyroid hormone (1-34) on bone formation in ovariectomized rats. Z Gerontol Geriatr. 2018;51(5):550-556. [34] Han Z, Bhavsar M, Leppik L, et al. Histological Scoring Method to Assess Bone Healing in Critical Size Bone Defect Models. Tissue Eng Part C Methods. 2018;24(5):272-279. [35] Akkaya S, Nazal? M, K?l?ç A, et al. Cefazolin-sodium has no adverse effect on fracture healing in an experimental rabbit model. Eklem Hastalik Cerrahisi. 2012;23(1):44-48. [36] Angle SR, Sena K, Sumner DR, et al. Healing of rat femoral segmental defect with bonemorphogenetic protein-2: a dose response study. J Musculoskelet Neuronal Interact. 2012;12(1):28-37. [37] Il'in DA, Arkhipov SA, Shkurupy VA. Analysis of IL-1α, bFGF, TGF-β1, IFNγ, MMP-1, and CatD Expression in Multinuclea Macrophages In Vitro. Bull Exp Biol Med. 2018;164(4):456-458. [38] Qu Y, Cao C, Wu Q, et al. The dual delivery of KGF and bFGF by collagen membrane to promote skin wound healing. J Tissue Eng Regen Med. 2018;12(6):1508-1518. [39] Xiao WL, Zhang DZ, Chen XJ, et al. Osteogenesis effect of guided bone regeneration combined with alveolar cleft grafting: assessment by cone beam computed tomography. Int J Oral Maxillofac Surg. 2016;45(6):683-687. [40] He B, Zhao J, Ou Y, et al. Biofunctionalized peptide nanofiber-based composite scaffolds for bone regeneration. Materials science & engineering. Mater Biol Appl. 2018;9(2):728-738. [41] Hiwatashi N, Hirano S, Mizuta M, et al. The efficacy of a novel collagen-gelatin scaffold with basic fibroblast growth factor for the treatment of vocal fold scar. J Tissue Eng Regen Med. 2017;11(5): 1598-1609. [42] Lu J, Descamps M, Dejou J, et al. The biodegradation mechanism of calcium phosphate biomaterials in bone. J BiomedMater Res. 2002; 34(63):408-412. [43] Bettach R, Guillaume B, Taschieri S, et al. Clinical performance of a highly porous beta-TCP as the grafting material for maxillary sinus augmentation. Implant Dent. 2014;23(3):357-364. [44] Castilho M, Rodrigues J, Pires I, et al. Fabrication of individual alginate-TCP scaffolds for bone tissue engineering by means of powder printing. Biofabrication. 2015;7(1):4-15. [45] Zhang C, Li Q, Deng S, et al. bFGF- and CaPP-Loaded Fibrin Clots Enhance the Bioactivity of the Tendon-Bone Interface to Augment Healing. Am J Sports Med. 2016;44(8):1972-1982. [46] Wang JS, Aspenberg P. Basic fibroblast growth factor enhances bone-graft incorporation: dose and time dependence in rats. J Orthop Res. 1996;14(2):316-23. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wang Yujiao, Liu Dan, Sun Song, Sun Yong. Biphasic calcium phosphate loaded with advanced platelet rich fibrin can promote the activity of rabbit bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 504-509. |
| [5] | Liu Jiangfeng. Nano-hydroxyapatite/polyamide 66 composite filling combined with locking plate in the treatment of fibrous dysplasia of femoral bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 542-547. |
| [6] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [7] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [8] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [9] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [10] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [11] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [12] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [13] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [14] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [15] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||