Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (4): 591-596.doi: 10.3969/j.issn.2095-4344.0584
Previous Articles Next Articles
Clinical application of bone morphogenetic proteins in bone and cartilage tissue engineering
Tang Xianneng1, Chen Yueping2, Zhang Xiaoyun2
- 1Guangxi University of Chinese Medicine, Nanning 530000, Guangxi Zhuang Autonomous Region, China; 2Department of Orthopedic Trauma and Hand Surgery, Ruikang Hospital Affiliated to Guangxi University of Chinese Medicine, Nanning 530012, Guangxi Zhuang Autonomous Region, China
-
Online:2019-02-08Published:2019-02-08 -
Contact:Chen Yueping, MD, Chief physician, Master’s supervisor, Department of Orthopedic Tramua and Hand Surgery, Ruikang Hospital Affiliated to Guangxi University of Chinese Medicine, Nanning 530012, Guangxi Zhuang Autonomous Region, China Zhang Xiaoyun, Master, Attending physician, Department of Orthopedic Trauma and Hand Surgery, Ruikang Hospital Affiliated to Guangxi University of Chinese Medicine, Nanning 530012, Guangxi Zhuang Autonomous Region, China -
About author:Tang Xianneng, Master candidate, Guangxi University of Chinese Medicine, Nanning 530000, Guangxi Zhuang Autonomous Region, China -
Supported by:the National Natural Science Foundation of China, No. 81760796; the Natural Science Foundation of Guangxi Zhuang Autonomous Region, No. 2015GXNSFAA139136; the Project of Improving the Basic Ability of Young Teachers in Guangxi Universities, No. KY2016YB204; the Research Project of Guangxi University of Chinese Medicine, No. B170045; the Central Support for the Development of Special Funds for Local Colleges and Universities (2017 Bone Surgery), No. 04B2017082 (to CYP); the Guangxi Graduate Education Innovation Program, No. YCSY2018038
CLC Number:
Cite this article
Tang Xianneng, Chen Yueping, Zhang Xiaoyun. Clinical application of bone morphogenetic proteins in bone and cartilage tissue engineering[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 591-596.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
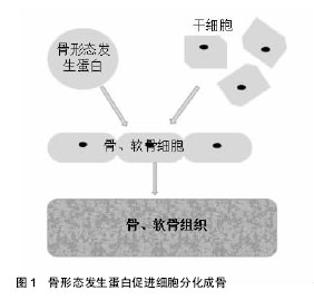
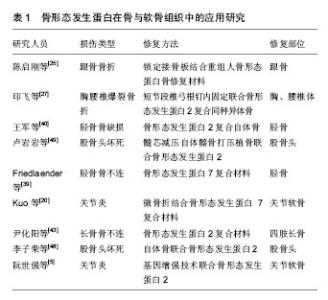
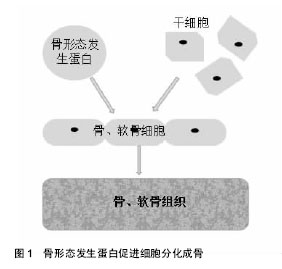
2.1 纳入文献基本情况 研究内容由第一作者依据纳入、排除标准独立提取,主要侧重骨形态发生蛋白在骨与软骨组织工程临床应用的相关研究报道,共纳入62篇文献,从①关节炎治疗;②骨折治疗;③骨不连、骨缺损治疗;④股骨头坏死治疗;⑤基因治疗等5个方面进行归纳、总结。 2.2 骨形态发生蛋白在骨与软骨组织工程中的临床应用研究 2.2.1 关节炎的治疗 关节软骨组织退化是骨关节炎和类风湿性关节炎等关节炎最常见的原因[10]。其中,骨关节炎主要表现为关节软骨退变、软骨下骨硬化和骨赘的形成[11-12]。之前的研究发现,临床存在多种骨关节炎表型,比如创伤后骨关节炎、骨质疏松性骨关节炎和类风湿性关节炎等某些自发性骨关节炎[13]。尽管骨关节炎有不同表型,但是临床表现出的症状和体征大致相同,病理改变诱发骨性关节炎、关节疼痛或关节畸形甚至残疾,给患者的身心健康和日常生活带来极大的不便。 国内外学者为解决此难题,进行了大量的相关研究。阮世强等[5]通过利用基因增强成骨诱导因子骨形态发生蛋白2刺激脂肪干细胞,同时结合Mosaicplasty技术可显著促进软骨缺损修复,即转染骨形态发生蛋白2对骨软骨的缺损有更佳的临床修复效果。有研究表明骨形态发生蛋白2高水平在正常对照组中检测到[14],骨形态发生蛋白2是唯一的关节内生长因子,表明它在外科手术中可能起着重要作用,可诱导软骨修复与再生。lópiz-morales等[15]证实重组人骨形态发生蛋白2和重组人骨形态发生蛋白4观察兔骨软骨缺损模型中透明软骨的修复达到较好的软骨下骨修复效果。Ozeki等[16]在大鼠跟腱内注射骨形态发生蛋白7,并报道了骨形态发生蛋白7通过改变肌腱组织胶原基因图谱,诱导大鼠异位软骨形成,防止软骨退变。在最近的一项研究中,一种特定的细胞因子和三维培养系统将含有人骨形态发生蛋白7和绿色荧光蛋白(Ad.hBMP7-GFP)转染软骨细胞的腺病毒与基质胶结合,发现该腺病毒可修复兔膝关节软骨缺损[17]。Honsawek等[18]专家发现骨形态发生蛋白7的表达量与骨关节炎的病变程度有着密切联系,骨关节炎病变越重,其表达量越高,这反映了内源性软骨修复的启动,而骨形态发生蛋白7可能是骨关节炎中具有软骨保护的一个潜在因子。李灿锋等[19]研究发现BMP/ALK1/Smad1/5/8信号通路与骨关节炎发生发展有着密切关系。Kuo等[20]采用微骨折结合骨形态发生蛋白7治疗青春期兔全层关节软骨损伤,发现该方法具有协同作用,改善软骨修复。再生组织与天然透明关节软骨非常相似,从而提高了再生软骨的质量和数量,骨形态发生蛋白与微骨折技术相结合,增加了骨髓干细胞向软骨损伤区的迁移,也将促进软骨的修复。同时,研究发现骨形态发生蛋白9可能是最具成骨性的骨形态发生蛋白,近年来受到了广泛的关注,这在体内研究中得到了很好的证明[21]。 2.2.2 骨折的治疗 骨折,指的是在外界暴力作用下,骨的连续性和完整性遭到破坏。由于一些严重的开放性骨折具有较高的不愈合率或延迟愈合率,导致肢体功能的丧失,此时骨折的修复就显得格外重要,这也是骨科领域的公认的难题之一。骨折修复是由大量细胞因子调控的复杂的骨再生过程[22],而骨形态发生蛋白在骨折修复过程中发挥重要作用。骨形态发生蛋白2是目前业界内公认的成骨细胞转化因子,通过对该特定的骨膜祖细胞的诱导,不可逆地进行分化软骨及骨细胞,可加快骨折断端的修复[23],见图1。"

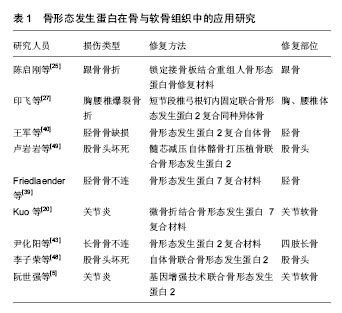
Kuzyk等[24]学者认为骨愈合修复分为早、中、晚期3个阶段。由于涉及人体对非自身物质的初始反应,例如凝血、炎症及蛋白的吸附,并且形成较稳定的蛋白,产生大量的骨生长因子,所以早中期阶段显得尤为重要,骨愈合的后期是骨塑形过程,类似骨折端的骨愈合塑形过程。陈启刚等[25]对15例跟骨骨折患者经锁定板结合重组人骨形态发生蛋白2治疗后,骨折均完全愈合,无畸形愈合,一定程度上说明了在锁定板坚强固定基础上重组人骨形态发生蛋白2骨修复材料能够促进骨愈合,减少骨不连发生率,并获得较满意的足功能恢复。王军等[26]研究发现,采用载有万古霉素的硫酸钙复合骨形态发生蛋白2一期用于治疗小范围骨缺损的创伤性骨髓炎患者,安全性高,并发症低,临床治疗效果良好。印飞等[27]对于胸腰椎爆裂性骨折采用短节段椎弓根钉固定辅以重组人骨形态发生蛋白2结合同种异体骨在爆裂骨折的椎体内打压植骨的临床效果较单纯植骨疗效更好,能够有效维持椎体的高度,防止后凸畸形,最大限度降低伤椎骨缺损的程度。 美国食品和药物管理局(Food and Drug Administration,FDA)以开放性胫骨骨折为例,批准了将其作为对骨形态发生蛋白临床疗效的评价实验模型。其中一组评价骨形态发生蛋白2在胫骨骨折手术治疗效果的小组进行了一个在全球大规模、多中心、前瞻性、随机性、单盲及对照的临床试验,涉及有11个国家和地区[28],最终研究发现使用1.5 g/L重组人骨形态发生蛋白治疗长骨骨折是安全的,效果较单纯内固定更优。 骨形态发生蛋白是一种低分子糖蛋白,是促使间充质细胞向成骨细胞转化的始发信号,能够诱导未完全分化的间充质细胞及成骨细胞的前体细胞往成骨细胞发展[29-30],在骨形态发生蛋白家族中以骨形态发生蛋白2的成骨诱导作用最强[31-32]。这个研究结果使得美国FDA于2004年认可骨形态发生蛋白2与可吸收胶原海绵复合物(骨形态发生蛋白2/胶原蛋白海绵,商品名:INFUSE),临床治疗胫骨开放性骨折。 2.2.3 骨不连及骨缺损的治疗 美国FDA将“骨折后至少9个月没有愈合,且没有进一步愈合倾向有3个月”定义成骨不连,它是由于诸多因素而引起的骨愈合功能停止,是严重骨折损伤术后的常见并发症,通过手术修复让骨折重新生长获得愈合[33]。尽管大多数骨折都能够治愈,但骨不连仍为目前骨折治疗的难题之一,其发病率为5%-10%[34]。对于骨不连的治疗,自体骨移植被认为是治疗的“金标准”[35]。但近几年的文献报道证实,在自体移植也存在较大的弊端,如供区的疼痛、植骨区的血肿、神经损伤及感觉异常,甚至感染等并发症,同时也存在手术时间较长,增加术中额外出血并且所能提供骨量有限的缺点[36-37]。郑金文等[38]研究说明在无特殊情况下一般不需要进行植骨,其适应证仅限于有骨缺损时,只是治疗骨不连的一个重要手段。随着骨组织工程学的兴起和发展,为种子细胞生长分化、新骨的形成和不同部位的骨不连、骨缺损修复提供了新的理论和技术。 美国FDA批准了将骨形态发生蛋白7在美国进行大规模、多中心的胫骨骨不连治疗的临床试验。Friedlaender等[39]学者进行了一个运用骨形态发生蛋白7治疗胫骨骨不连的大规模多中心的临床试验,研究发现骨形态发生蛋白复合型胶原治疗胫骨骨不连与自体取骨移植相比,具有无供区疼痛、出血少、手术时间缩短的优点,是一个安全有效的治疗方式。王军等[40]在下肢小段骨缺损一期控制感染的前提下,二期使用骨形态发生蛋白2与自体骨的混合骨治疗感染性骨不连取得了良好的临床疗效,不仅有充分的植骨量,同时还有较高的骨诱导性能,安全有效的弥补和修复骨缺损。若对于骨缺损> 6 cm的骨缺损,则需要采用带有血管的自体腓骨、髂骨进行植骨,或采用Ilizarov外固定技术[41-42]。尹化阳等[43]研究发现在四肢长骨骨不连的治疗中,重组人骨形态发生蛋白2可加速骨不连愈合,具有高效成骨活性,是一种优良的植骨材料,能有效治疗四肢长骨骨不连。 2.2.4 股骨头坏死治疗 股骨头坏死是一种破坏性、退行性疾患,随着病情的发展易形成软骨下骨及关节面软骨的塌陷变形[44],引发股骨头畸形、疼痛及行走活动功能障碍等一系列临床表现[45]。主要包括创伤性股骨头坏死和非创伤性股骨头坏死,前者是由股骨颈骨折引起的,后者属于慢性缺血坏死,是由酒精和激素所致;是骨科临床常见的难治性疾患之一[46]。因此,探索安全有效的股骨头坏死的治疗方案已经成为骨科医务工作人员研究的热点问题。近年来以骨髓间充质干细胞向成骨细胞、脂肪细胞转化失衡[47],使得脂肪细胞分化增多,骨髓腔内压力增高而引发股骨头缺血性坏死的理论观点受到业界众多学者的青睐。 李子荣等[48]发现对于股骨头坏死ARCOⅡ期或者CJFH的C型、L1型患者,加入骨形态发生蛋白2后,可以有效提高打压植骨术治疗股骨头坏死的手术疗效及股骨头骨修复程度。卢岩岩等[49]采用髓芯减压自体髂骨打压植骨联合骨形态发生蛋白2治疗38例(52髋)早中期股骨头坏死的患者,发现可以有效治疗早中期股骨头坏死,能延缓甚至避免髋关节手术置换,具有重大临床意义。诸多因素可破坏股骨头的营养供给,使其骨细胞死亡和骨髓结构改变,造成股骨头的坏死。骨形态发生蛋白不仅能够在股骨头坏死修复中刺激骨髓细胞分化为成骨细胞,同时还可以促进骨细胞生长,其中骨形态发生蛋白2就是这个过程中最关键的成骨调节因子[50-51]。秦朝等[52]研究分别经过1,2,3周的大鼠股骨头坏死观察,发现随着愈合过程的推进,骨形态发生蛋白2的含量也呈递增的趋势,成骨细胞也不断分化增殖,从而促进大鼠股骨头坏死的愈合。 2.2.5 基因治疗 骨的形成及再生修复需要在一定的时间内,在局部有足量的骨细胞诱导因子并且能使细胞对诱导因子有生物应答[53]。从20世纪60年代后期发现有效骨诱导的骨形态发生蛋白以来,临床上已广泛应用于骨的再生治疗[54-55],以骨形态发生蛋白2的应用最有效和最广泛[56]。同时受到骨形态发生蛋白其诱导因子的可控制性释放较难把握的限制,使得在临床更广泛的应用也受到了一定影响[57]。 基因治疗与重组骨蛋白细胞因子的不可控爆发性释放不同,它通过把骨基因导入细胞中,能够达到一个高活性成骨蛋白的持久稳定释放[58]。同时也有一些学者证实[59],利用这类稳定表达骨形态发生蛋白基因的干细胞有利于促进骨组织的修复,实现骨形态蛋白的持续性释放,提供能成骨分化的干细胞,介导骨组织的再生修复[60]。韩杰等[61]研究发现三七总皂苷对于提高激素性股骨头坏死模型兔的血清内皮生长因子mRNA和骨形态发生蛋白2 mRNA表达量具有正向影响,可促进局部微循环,进而改善股骨头坏死情况。研究证实了骨基因治疗不同于重组骨蛋白细胞因子,能使骨蛋白高活性持久稳定表达、释放,有利于实验室基础研究成果的临床应用转化,促进骨再生修复,在业界内有较好的临床应用前景,见表1。同时在临床转化治疗中,基因治疗也面临较大挑战,主要是安全问题,主要包括包括病毒基因载体的免疫反应、病毒感染、转染外源性基因细胞的排斥以及外源性基因的表达失控等[62],所以基因治疗还有待进一步深入研究。"

| [1] Urist MR.Bone formation by autoinduction. Science. 1965;150: 893-899.[2] Barcak EA, Beebe MJ.Bone morphogenetic protein:is there still a role in orthopedic trauma in 2017.Orthop Clin North Am.2017; 48(3): 301-309.[3] Venkatesan J, Bhatnagar I, Manivasagan P, et al.Alginate composites for bone tissue engineering:a review.Int J Biol Macromol.2015;72:269-281.[4] 杨林,徐军美,王亚平,等.骨形态发生蛋白2/4在神经系统中的作用及其研究进展[J].中南大学学报(医学版), 2018,43(02):222-228.[5] 阮世强,邓江,等.聚乳酸/聚羟基乙酸共聚物支架复合骨形态发生蛋白2基因增强的脂肪干细胞促进软骨缺损修复[J].中国组织工程研究,2018,22(6):840-845.[6] Pilipchuk SP, Plonka AB, Monje A, et al.Tissue engineering for bone regeneration and osseointegration in the oral cavity.Dent Mater.2015;31(4):317-338. [7] Claros S, Rico-Llanos GA, Becerra J, et al.A novel human TGF-beta1 fusion protein in combination with rhBMP-2 increases chondro-osteogenic differentiation of bone marrow mesenchymal stem cells.Int J Mol Sci. 2014;15(7):11255-11274.[8] 盛俊东,顾九君,刘兴炎,等.骨形态发生蛋白-7复合纤维蛋白对大鼠骨质疏松性椎体骨折愈合的影响[J].中国脊柱脊髓杂志,2010,20(4): 291-294.[9] Labibzadeh N, Emadedin M, Fazeli R, et al.Msenchymal strumal cells implantation in combination with platelet lysate product is safe for reconstruction of human long bone nonunion.Cell J.2016; 18(3):302-309.[10] Deng ZH, Li YS, Gao X, et al. Bone morphogenetic proteins for articular cartilage regeneration. Osteoarthritis Cartilage. 2018 Mar 24.[11] Varady NH, Grodzinsky AJ.steoarthritis year in review2015:mechanics.Osteoarthritis Cartilage. 2016;24(1):27.[12] Lane NE, Shidara K, Wise BL.Osteoarthritis year in review 2016:clinical.Osteoarthritis Cartilage. 2017;25(2):209-215.[13] Barton KI, Shekarforoush M, Heard BJ, et al.Use of preclinical surgically induced models to understand biomechanical and biological consequences of PTOA development.J Orthop Res. 2017;35(3):454.[14] Schmal H, Niemeyer P, Zwingmann J, et al. Association between expression of the bone morphogenetic proteins 2 and7 in the repair of circumscribed cartilage lesions with clinical outcome. BMC Musculoskelet Disord 2010;11:170.[15] Lópiz-Morales Y, Abarrategi A, Ramos V, et al. In vivo comparison of the effects of rhBMP-2 and rhBMP-4 in osteochondral tissue 5 regeneration. Eur Cell Mater 2010;20:367-378.[16] Ozeki N, Muneta T, Koga H, et al.Transplantation of Achilles tendon treated with bone morphogenetic protein 7 promotes meniscus regeneration in a rat model of massive meniscal defect. Arthritis Rheum 2013;65:2876-2886.[17] Xia X, Li J, Xia B, et al. Matrigel scaffold combined with Ad-hBMP7-transfected chondrocytes improves the repair of rabbit cartilage defect. Exp Ther Med 2017;13:542-550.[18] Honsawek S,Chayanupatkul M,Tanavalee A,et al. Relationship of plasma and synovial fluid BMP-7 with disease severity in knee osteoarthritis patients:a pilot study.Int Orthop.2009;33(4): 1171-1175.[19] 李灿锋,陈卓,曾羿,等.骨形态发生蛋白信号通路在骨关节炎发病机制中的作用研究[J].中华关节外科杂志(电子版), 2017,11(5):500-505.[20] Kuo AC, Rodrigo JJ, Reddi AH,et al. Microfracture and bone 30 morphogenetic protein 7(BMP-7) synergistically stimulate articular cartilage repair.Osteoarthritis 31 Cartilage.2006;14:1126-1135.[21] Majumdar MK, Wang E, Morris EA.BMP-2 and BMP-9 promotes chondrogenic differentiation of human multipotential mesenchymal cells and overcomes the inhibitory effect of IL-1. J Cell Physiol 2001;189:275-284.[22] Einhorn TA, Gerstenfeld LC.Fracture healing:mechanisms and interventions.Nat Rev Rheumatol.2015;11(1):45-54.[23] Wu M, Chen G, Li YP.TGF-b and BMP signialing in osteoblast, skeletal development,and bone fromation,bomeostasis and disease.Bone Res.2016;4:16009.[24] Kuzyk PR, Schemitsch EH.The basic science of peri-im-plant bone healing. Indian J Orthop. 2011;45(2):108-115.[25] 陈启刚,胡永军,胡海,等.锁定接骨板结合重组人骨形态发生蛋白骨修复材料治疗跟骨骨折的临床分析[J].安徽医药, 2018,22(4):703-706.[26] 王军,时宁文,邱阳,等.载万古霉素硫酸钙复合BMP-2治疗创伤性骨髓炎[J].中国骨科临床与基础研究杂志,2017,9(3):133-139.[27] 印飞,孙振中,殷渠东,等.短节段椎弓根钉固定联合重组人BMP-2和同种异体骨植骨治疗胸腰椎爆裂骨折[J].中国修复重建外科杂志, 2017,31(9):1080-1085.[28] Govender S, Csimma C, Genant HK, et al.Recombinant human bone orphogenetic protein-2 for treatment of open tibial fractures:a prospective,controlled,randomized study of four hundred and fifty patients.J Bone Joint Surg Am. 2002;84-A (12):2123-2134.[29] Kokubo S, Fujimoto R, Yokota S, et al. Bone regeneration by recombineant human bone morphogenetic protein-2 and a novel biodegradable carrier in arabbit ulnar defect model. Biomaterials. 2003;24(9):1643-1651.[30] Sándor GK, Tuovinen VJ, Wolff J, et al.Adipose stem cell tissue-engineered construct used to treat large anterior mandibular defect:a case report and review of the clinical application of good manufacturing practice-level adipose stem cells for bone regeneration.J Oral Maxillofac Surg.2013;71(5): 938-950.[31] Stancoven BW,Lee J,Dixon DR,et al.Effect of bone morphogeneticprotein-2,demineralized bone matrix and systemic parathyroid hormone(1-34)on local bone formation in a rat calvaria critical size defect model.J Periodontal Res.2013;48(2): 243-251.[32] Wu G, Liu Y, Iizuka T, et al.The effect of a slow mode of BMP-2 delivery on the inflammatory response provoked by bone-defect-filling polymeric scaffolds.Biomaterials. 2010;31(29): 7485-7493.[33] 郑昊,吕游,徐丽,等.下肢长管骨骨折合并骨不连的原因分析及治疗[J].中国临床医师杂志,2015,9(17):3286-3290.[34] Kadhim M, Holmes L Jr, Gesheff MG, et al.Treatment options for nonunion with segmental bone defects:systematic review and quantitative evidence synthesis.J Orthop Trauma.2017;31(2): 111-119.[35] Maceroli MA, Gage MJ, Wise BT, et al.Risk factors for failure of bone grafting of tibia nonunions and segmental bone defects:anew preoperative risk assessment score.J Orthop Trauma.2017;31(Suppl 5):S55-S59.[36] Slette EL, Mikula JD, Turnbull TL, et al.Treatment of midshaft clavicle fractures:application of local autograft with concurrent plate fixation.Arthosc Tech.2016;5(3):e557-e562.[37] Radcliff K, Hwang R, Hilibrand A, et al.The effect of iliac crest autograft on the outcome of fusion in the setting of degenerative spondylolisthesis:a subgroup analysis of the spine patient outcomes research.J Bone Joint Surg Am.2012;94(18): 1685-1692.[38] 郑金文,刘显东,王小兵,等.下肢骨干骨折术后骨不连的原因分析及手术治疗[J].中国骨与关节损伤杂志, 2014,29(12):1236-1238.[39] Friedlaender GE, Perry CR, Cole JD, et al.Osteogenic protein-1(bone morphogenetic protein-7) in the treatment of tibial nonunions.J Bone Joint Surg Am 2001;83-A Suppl 1(Pt2): S151-158.[40] 王军,时宁文,钱红波,等.自体微小颗粒骨与骨形态发生蛋白2混合移植修复感染性骨不连[J].中国组织工程研究, 2014,18(43): 6896-6901.[41] 王建超,蔡锦方,曹学成,等.Ilizarov骨搬移技术修复胫骨创伤性骨髓炎大段骨缺损[J].实用骨科杂志,2016,22(4):324-327.[42] Megas P, Saridis A, Kouzelis A, et al.The treatment of infected nonunion of the tibia following intramedullary nailing by the Ilizarov method. Injury. 2010;41(3):294-299. [43] 尹化阳,王皓宇,黄明,等.重组人骨形态发生蛋白-2治疗四肢长骨骨不连临床研究[J].淮海医药,2017,35(6):668-671.[44] Zhang YL, Yin JH, Ding H, et al.Vitamin K2 Prevents Glucocorticoid-induced Osteonecrosis of the Femoral Head in Rats.Int J Biol Sci.2016;12(4):347-358.[45] 农峰,唐毓金,赵凯丽.激素性股骨头坏死与相关单核苷酸基因多态性关系的研究进展[J].中华实用诊断与治疗杂志, 2017,31(7):722-725.[46] Zhao DW, Hu YC.Chinese experts' consensus on the diagnosis and treatment of osteonecrosis of the femoral head in adults. Orthop Surg.2012;4(3):125-130.[47] 谭钢,康鹏德,裴福兴,等.激素性股骨头坏死与髋关节骨关节炎患者离体标本相关因子表达水平的比较研究[J]. 中华关节外科杂志:电子版,2012,6(2):260-267.[48] 李子荣,孙伟,史振才,等.加入和未加骨形态发生蛋白2的打压植骨术治疗股骨头坏死[J].中国骨与关节外科,2012,5(5):377-381.[49] 卢岩岩,翟明玉,魏宗星,等.髓芯减压自体髂骨打压植骨联合骨形态发生蛋白2治疗早中期股骨头坏死疗效观察[J].风湿病与关节炎, 2015,4(09):42-44.[50] Ma XW, Cui DP, Zhao DW. et al.Vascular endothelial growth factor/bone morphogenetic protein-2 bone marrow combined modification of the mesenchymal stem cells to repair the avascular necrosis of the femoral head.Int J Clin Exp Med. 2015;8(9):15528-15534.[51] Kim HK, Aruwajoye O, Du J, et al.Local administration of bone morphogenetic protein-2 and bisphosphonate during non-weight-bearing treatment of ischemic osteonecrosis of the femoral head:an experimental investigation in immature pigs.J Bone Joint Surg Am.2014;96(18):1515-1524.[52] 秦朝,官立萍,司艳莉,等.骨形态发生蛋白-2对股骨头坏死大鼠模型的愈合作用[J].中国生物制品学杂志,2016,29(12):1288.[53] Bueno EM, Glowacki J. Cell-free and cell-based approaches for bone regeneration.Nature reviews.Rheumatology. 2009;5(12): 685-697.[54] Liu X, Yu B, Huang Q, et al.In vitro BMP-2 peptide release from thiolated chitosan based hydrogel.Int J Biol Macromol.2016;93(Pt A):314-321.[55] Williams JC, Maitra S, Anderson MJ, et al.BMP-7 and Bone Regeneration:Evaluation of Dose-Response in a Rodent Segmental Defect Model.J Orthop Trauma. 2015;29(9):e336-341.[56] Sierra-García GD, Castro-Ríos R, Gónzalez-Horta A, et al. Bone morphogenetic proteins(BMP):clinical application for reconstruction of bone defects.Gac Med Mex.2016;152(3):381-385.[57] Carragee EJ, Hurwitz EL, Weiner BK.A critical review of recombinant human bone morphogenetic protein-2 trials in spinal surgery:emerging safety concerns and lessons learned.Spine J. 2011;11(6):471-491. [58] Evans CH, Huard J.Gene therapy approaches to regenerating the musculoskeletal system.Nat Rev Rheumatol. 2015;11(4):234-242.[59] Yang Y, Jin G, Li L, et al.Enhanced osteogenic activity of mesenchymal stem cells and co-modified BMP-2 and b FGF genes.Ann Transplant.2014;19:629-638.[60] Deschaseaux F, Pontikoglou C, Sensébé L.Bone regeneration:the stem/progenitor cells point of view.J Cell Mol Med.2010;14(1-2): 103-115.[61] 韩杰,王世鑫,莫坚,等.三七总皂苷对激素性股骨头缺血性坏死模型兔骨组织血管内皮生长因子和骨形态形成蛋白-2 mRNA表达的影响[J].广西医学,2016,38(5):611-614.[62] Gottfried ON, Dailey AT. Mesenchymal stem cell and gene therapies for spinal fusion. Neurosurgery.2008;63(3):380-391; discussion 391-382. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Wu Xun, Meng Juanhong, Zhang Jianyun, Wang Liang. Concentrated growth factors in the repair of a full-thickness condylar cartilage defect in a rabbit [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1166-1171. |
| [3] | Li Jiacheng, Liang Xuezhen, Liu Jinbao, Xu Bo, Li Gang. Differential mRNA expression profile and competitive endogenous RNA regulatory network in osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1212-1217. |
| [4] | Geng Qiudong, Ge Haiya, Wang Heming, Li Nan. Role and mechanism of Guilu Erxianjiao in treatment of osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1229-1236. |
| [5] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [6] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [7] | Liu Xin, Yan Feihua, Hong Kunhao. Delaying cartilage degeneration by regulating the expression of aquaporins in rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 668-673. |
| [8] | Deng Zhenhan, Huang Yong, Xiao Lulu, Chen Yulin, Zhu Weimin, Lu Wei, Wang Daping. Role and application of bone morphogenetic proteins in articular cartilage regeneration [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 798-806. |
| [9] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [10] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [11] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [12] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [13] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [14] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [15] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||