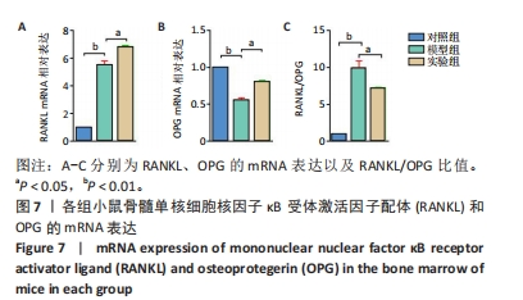
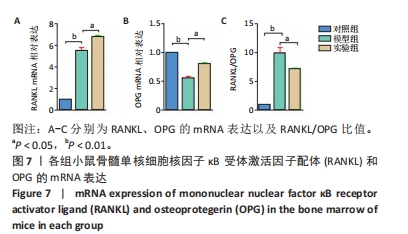
Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (35): 5649-5655.doi: 10.12307/2024.824
Previous Articles Next Articles
Protective effect of ulinastatin on acute bone loss in sepsis
Yang Peng1, Tang Yubin1, 2, Yang Jing1, Liu Jian3, Yao Runjie1, Chen Lin1, Su Nan1
- 1Center of Osteoporosis and Bone Development, Laboratory of Injury Repair and Rehabilitation Medicine, Laboratory for Prevention and Rehabilitation of Training Injuries, State Key Laboratory of Trauma and Chemical Poisoning, Daping Hospital, Army Medical University, Chongqing 400042, China; 2Emergency Department of the 940th Hospital of Joint Logistics Support Force of Chinese PLA, Lanzhou 730050, Gansu Province, China; 3Department of Orthopedics, Tongji Hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430030, Hubei Province, China
-
Received:2023-11-08Accepted:2024-01-12Online:2024-12-18Published:2024-03-15 -
Contact:Su Nan, Professor, Center of Osteoporosis and Bone Development, Laboratory of Injury Repair and Rehabilitation Medicine, Laboratory for Prevention and Rehabilitation of Training Injuries, State Key Laboratory of Trauma and Chemical Poisoning, Daping Hospital, Army Medical University, Chongqing 400042, China Chen Lin, Professor, Center of Osteoporosis and Bone Development, Laboratory of Injury Repair and Rehabilitation Medicine, Laboratory for Prevention and Rehabilitation of Training Injuries, State Key Laboratory of Trauma and Chemical Poisoning, Daping Hospital, Army Medical University, Chongqing 400042, China -
About author:Yang Peng, Master, Experimentalist, Center of Osteoporosis and Bone Development, Laboratory of Injury Repair and Rehabilitation Medicine, Laboratory for Prevention and Rehabilitation of Training Injuries, State Key Laboratory of Trauma and Chemical Poisoning, Daping Hospital, Army Medical University, Chongqing 400042, China Tang Yubin, Master, Associate chief physician, Center of Osteoporosis and Bone Development, Laboratory of Injury Repair and Rehabilitation Medicine, Laboratory for Prevention and Rehabilitation of Training Injuries, State Key Laboratory of Trauma and Chemical Poisoning, Daping Hospital, Army Medical University, Chongqing 400042, China; Emergency Department of the 940th Hospital of Joint Logistics Support Force of Chinese PLA, Lanzhou 730050, Gansu Province, China -
Supported by:the National Natural Science Foundation of China, No. 81870621 (to SN) and 81991513 (to SN [project participant]); National Key R&D Program of China, No. 2018YFA0800802 (to CL)
CLC Number:
Cite this article
Yang Peng, Tang Yubin, Yang Jing, Liu Jian, Yao Runjie, Chen Lin, Su Nan. Protective effect of ulinastatin on acute bone loss in sepsis[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(35): 5649-5655.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
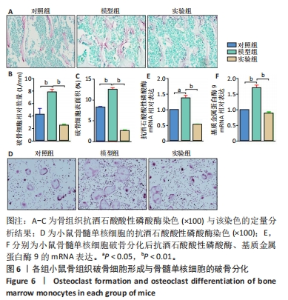
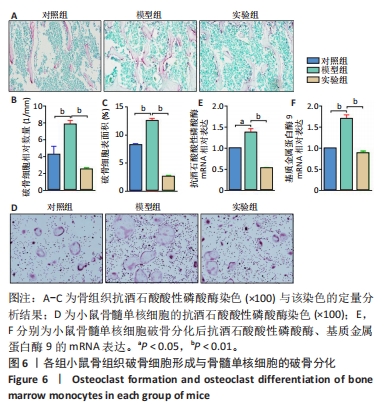
以上结果显示,乌司他丁的骨保护作用主要是通过促进成骨细胞增殖来保证成骨细胞数量稳定的。 2.3 乌司他丁可显著减少脂多糖造成的破骨细胞生成 骨吸收功能的发挥离不开破骨细胞,腹腔注射脂多糖可以引发小鼠全身炎症反应,进而激活破骨细胞功能,最终导致骨丢失。乌司他丁是重要的抗炎药物,因此研究了乌司他丁对破骨细胞的影响。 小鼠骨组织抗酒石酸酸性磷酸酶染色显示,与对照组相比,模型组破骨细胞的数量和表面积明显增加,实验组破骨细胞数量和表面积较模型组显著减少,见图6A-C,表明乌司他丁可通过抑制破骨细胞的形成来缓解脂多糖诱导的骨丢失。 为了研究乌司他丁是否直接对破骨细胞发挥调控作用,进行了破骨细胞体外诱导实验,结果显示脂多糖处理后破骨细胞的数量明显增加,实验组破骨细胞数量较模型组显著减少,见图6D,说明乌司他丁对脂多糖造成的破骨细胞形成有抑制作用。 Q-PCR检测结果显示,与对照组比较,模型组抗酒石酸酸性磷酸酶、基质金属蛋白酶9的mRNA表达升高(P < 0.05,P < 0.01);与模型组比较,实验组抗酒石酸酸性磷酸酶、基质金属蛋白酶9的mRNA表达降低(P < 0.01),见图6E,F。结果说明乌司他丁能够通过抑制破骨相关基因的表达抑制破骨细胞分化。"
| [1] CONFAVREUX CB. Bone: from a reservoir of minerals to a regulator of energy metabolism. Kidney Int. 2011;79121:S14-19. [2] FUKUMOTO S, MARTIN TJ. Bone as an endocrine organ. Trends Endocrinol Metab. 2009;20(5):230-236. [3] GUNTUR AR, ROSEN CJ. Bone as an endocrine organ. Endocr Pract. 2012;18(5):758-762. [4] SINGER M, DEUTSCHMAN CS, SEYMOUR CW, et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA. 2016;315(8):801-810. [5] CECCONI M, EVANS L, LEVY M, et al. Sepsis and septic shock. Lancet. 2018;392(10141):75-87. [6] LEE P, NAIR P, EISMAN JA, et al. Bone Failure in Critical Illness. Review Crit Care Med. 2016;44(12):2270-2274. [7] BLIUC D, TRAN T, VAN GEEL T, et al. Mortality risk reduction differs according to bisphosphonate class: a 15-year observational study. Osteoporos Int. 2019;30:817-828. [8] ORFORD NR, BAILEY M, BELLOMO R, et al. The association of time and medications with changes in bone mineral density in the 2 years after critical illness. Crit Care. 2017;21(1):69. [9] ATAL SS, ATAL S. Ulinastatin - a newer potential therapeutic option for multiple organ dysfunction syndrome. J Basic Clin Physiol Pharmacol. 2016;27(2):91-99. [10] ORFORD N, CATTIGAN C, BRENNAN SL, et al. The association between critical illness and changes in bone turnover in adults: a systematic review. Osteoporos Int. 2014;25(10):2335-2346. [11] ORFORD NR, SAUNDERS K, MERRIMAN E, et al. Skeletal morbidity among survivors of critical illness. Crit Care Med. 2011;39(6):1295-1300. [12] HUANG J, REN R, BAO Y, et al. Ulinastatin Inhibits Osteoclastogenesis and Suppresses Ovariectomy-Induced Bone Loss by Downregulating uPAR. Front Pharmacol. 2018;9:1016. [13] MENG J, ZHOU C, ZHANG W, et al. Stachydrine prevents LPS-induced bone loss by inhibiting osteoclastogenesis via NF-κB and Akt signalling. J Cell Mol Med. 2019;23(10):6730-6743. [14] LI S, DAI Q, ZHANG S, et al. Ulinastatin attenuates LPS-induced inflammation in mouse macrophage RAW264.7 cells by inhibiting the JNK/NF-kB signaling pathway and activating the PI3K/Akt/Nrf2 pathway. Acta Pharmacol. 2018;39(8):1294-1304. [15] CAO C, YIN C, CHAI Y, et al. Ulinastatin mediates suppression of regulatory T cells through TLR4/NF-kB signaling pathway in murine sepsis. Int Immunopharmacol. 2018;64:411-423. [16] TSOYI K, JANG HJ, NIZAMUTDINOVA IT, et al. Metformin inhibits HMGB1 release in LPS-treated RAW 264.7 cells and increases survival rate of endotoxaemic mice. Br J Pharmacol. 2011;162(7):1498-1508. [17] JI J, GU Z, LI H, et al. Cryptdin-2 predicts intestinal injury during heatstroke in mice. Int J Mol Med. 2017;41:137-146. [18] GUO C, YUAN L, WANG J, et al. Lipopolysaccharide (LPS) induces the apoptosis and inhibits osteoblast differentiation through JNK pathway in MC3T3-E1 cells. Inflammation. 2014;37(2):621-631. [19] ZHAO Y, GAO J, ZHANG Y, et al. Cyclosporine A Promotes Bone Remodeling in LPS-Related Inflammation via Inhibiting ROS/ERK Signaling: Studies. Oxid Med Cell Longev. 2021;2021:8836599-8836599. [20] 茹江英,丛宇,赵建宁,等.乌司他丁对骨水泥颗粒诱导MC3T3-E1鼠前成骨细胞凋亡的干预作用[J].中国组织工程研究,2014,18(43): 6945-6950. [21] SU N, SUN Q, LI C, et al. Gain-of-function mutation in FGFR3 in mice leads to decreased bone mass by affecting both osteoblastogenesis and osteoclastogenesis. Hum Mol Genet. 2010;19(7):1199-210. [22] IKEBUCHI Y, AOKI S, HONMA M, et al. Coupling of bone resorption and formation by RANKL reverse signalling. Nature. 2018;561(7722): 195-200. [23] TAKAMI M, KIM N, RHO J, et al. Stimulation by toll-like receptors inhibits osteoclast differentiation. J Immunol. 2002;169(3):1516-1523. [24] 夏维波,章振林,林华,等.原发性骨质疏松症诊疗指南(2017)[J].中国骨质疏松杂志,2019,25(3):281-309. [25] WALSH MC, TAKEGAHARA N, KIM H, et al. Updating osteoimmunology: regulation of bone cells by innate and adaptive immunity. Nat Rev Rheumatol. 2018;14(3):146-156. [26] PARK-MIN KH, LORENZO J. Osteoclasts: Other functions. Bone. 2022; 165:116576. [27] KODE A, MANAVALAN JS, MOSIALOU I, et al. Leukaemogenesis induced by an activating β-catenin mutation in osteoblasts. Nature. 2014;506(7487):240-244.. [28] MAO H, LI L, FAN Q, et al. Endothelium-specific depletion of LRP1 improves glucose homeostasis through inducing osteocalcin. Nat Commun. 2021;12(1):5296-5296. [29] KHRIMIAN L, OBRI A, RAMOS-BROSSIER M, et al. Gpr158 mediates osteocalcin’s regulation of cognition. J Exp Med. 2017;214(10): 2859-2873. [30] GU P, TAO D, XU Y, et al. Osteocalcin inhibits myocyte aging through promotion of starvation-induced autophagy via IL-6/STAT3 signaling. Exp Gerontol. 2023;173:112082-112082. [31] ZHOU R, LIU D, LI R, et al. Low Bone Mass is Associated with Stroke in Chinese Postmenopausal Women: The Chongqing Osteoporosis Study. Cell Biochem Biophys. 2015;71(3):1695-1701. [32] HU MC, SHIIZAKI K, KURO-O M, et al. Fibroblast Growth Factor 23 and Klotho: Physiology and Pathophysiology of an Endocrine Network of Mineral Metabolism. Annu Rev Physiol. 2013;75(1):503-533. [33] ZOCH ML, ABOU DS, CLEMENS TL, et al. In vivo radiometric analysis of glucose uptake and distribUTIon in mouse bone. Bone Res. 2016;4(Pt 1): 16004. [34] WEI J, SHIMAZU J, MAKINISTOGLU MP, et al. Glucose Uptake and Runx2 Synergize to Orchestrate Osteoblast Differentiation and Bone Formation. Cell. 2015;161(7):1576-1591. [35] RU JY, XU HD, SHI D, et al. Blockade of NF-κB and MAPK pathways by ulinastatin attenuates wear particle-stimulated osteoclast differentiation in vitro and in vivo. Biosci Rep. 2016;36(5):e00399. [36] LI L, SAPKOTA M, KIM S, et al. Herbacetin inhibits RANKL-mediated osteoclastogenesis in vitro and prevents inflammatory bone loss in vivo. Eur J Pharmacol. 2016;777:17-25. [37] LIU H, DONG Y, GAO Y, et al. Hesperetin suppresses RANKL-induced osteoclastogenesis and ameliorates lipopolysaccharide-induced bone loss. J Cell Physiol. 2019;234(7):11009-11022. [38] SHUTO T, JIMI E, KUKITA T, et al. Granulocyte-macrophage colony stimulating factor suppresses lipopolysaccharide-induced osteoclast-like cell formation in mouse bone marrow cultures. Endocrinology. 1994;134(2):831-837. [39] ISLAM S, HASSAN F, TUMURKHUU G, et al. Bacterial lipopolysaccharide induces osteoclast formation in RAW 264.7 macrophage cells. Biochem Biophys Res Commun. 2007;360(2):346-351. [40] MÖRMANN M, THEDERAN M, NACKCHBANDI I, et al. Lipopolysaccharides (LPS) induce the differentiation of human monocytes to osteoclasts in a tumour necrosis factor (TNF) α-dependent manner: A link between infection and pathological bone resorption. Mol Immunol. 2008;45(12):3330-3337. [41] ITOH K, UDAGAWA N, KOBAYASHI K, et al. Lipopolysaccharide promotes the survival of osteoclasts via Toll-like receptor 4, but cytokine production of osteoclasts in response to lipopolysaccharide is different from that of macrophages. J Immunol. 2003;170(7):3688-3695. [42] CHEN YH, HSUEH KK, CHU PW, et al. AMP-activated protein kinase mediates lipopolysaccharide-induced proinflammatory responses and elevated bone resorption in differentiated osteoclasts. J Cell Biochem. 2022;123(2):275-288. [43] 《乌司他丁用于临床常见急危重症的专家共识》专家组.乌司他丁用于临床常见急危重症的专家共识[J].中国全科医学,2023,26(26): 3207-3219. [44] BOYCE BF, XING L. The RANKL/RANK/OPG pathway. Curr Osteoporos Rep. 2007;5(3):98-104. |
| [1] | Wang Wentao, Hou Zhenyang, Wang Yijun, Xu Yaozeng. Apelin-13 alleviates systemic inflammatory bone loss by inhibiting macrophage M1 polarization [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(8): 1548-1555. |
| [2] | Zhu Hanmin, Wang Song, Xiao Wenlin, Zhang Wenjing, Zhou Xi, He Ye, Li Wei, . Mitophagy regulates bone metabolism [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(8): 1676-1683. |
| [3] | Chi Wenxin, Zhang Cunxin, Gao Kai, Lyu Chaoliang, Zhang Kefeng. Mechanism by which nobiletin inhibits inflammatory response of BV2 microglia [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(7): 1321-1327. |
| [4] | Aikepaer · Aierken, Chen Xiaotao, Wufanbieke · Baheti. Osteogenesis-induced exosomes derived from human periodontal ligament stem cells promote osteogenic differentiation of human periodontal ligament stem cells in an inflammatory microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(7): 1388-1394. |
| [5] | Li Yueyao, Zhang Min, Yang Jiaju. Cistanoside A mediates p38/MAPK pathway to inhibit osteoclast activity [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(6): 1144-1151. |
| [6] | Ji Huihui, Jiang Xu, Zhang Zhimin, Xing Yunhong, Wang Liangliang, Li Na, Song Yuting, Luo Xuguang, Cui Huilin, Cao Ximei. SR9009 combined with indolepropionic acid alleviates inflammation in C2C12 myoblasts through the nuclear factor-kappa B signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(6): 1220-1229. |
| [7] | Lang Mecuo, Zhang Yilin, Wang Li. MiR-338-3p affects proliferation and apoptosis of alveolar bone osteoblasts by targeting receptor activator of nuclear factor-kappaB ligand [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(5): 899-907. |
| [8] | Bai Jing, Zhang Xue, Ren Yan, Li Yuehui, Tian Xiaoyu. Effect of lncRNA-TNFRSF13C on hypoxia-inducible factor 1alpha in periodontal cells by modulation of #br# miR-1246 #br# [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(5): 928-935. |
| [9] | Xiao Fang, Huang Lei, Wang Lin. Magnetic nanomaterials and magnetic field effects accelerate bone injury repair [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(4): 827-838. |
| [10] | Yang Cheng, Li Weimin, Ran Dongcheng, Xu Jiamu, Wu Wangxiang, Xu Jiafu, Chen Jingjing, Jiang Guangfu, Wang Chunqing. Ferroptosis and osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(3): 554-562. |
| [11] | Du Zhongqiu, Qi Xiaoyang, Yang Ping, Yu Jianglin, Chen Yixin, Zhang Linjian, Qiu Xusheng. Effects of the prolyl hydroxylase 2 inhibitor cpd17 on mouse osteogenic precursor cells [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(2): 238-244. |
| [12] | Li Haishan, Wu Yuheng, Liang Zixuan, Zhang Shiyin, Zhang Zhen, Mai Bin, Deng Wei, Li Yongxian, Tang Yongchao, , Zhang Shuncong, , Yuan Kai, . Carnosic acid inhibits osteoclast differentiation by inhibiting mitochondrial activity [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(2): 245-253. |
| [13] | Hou Chengzhi, Han Jiatong, Wei Guangcheng, Zhuo Zechuan, Li Qiuyue, Zhao Yong, Yu Zhangjingze . Gushukang interferes with osteoclasts: activation of nuclear factor erythroid 2-related factor 2 regulates the c-Fos/NFATc1 pathway in the treatment of osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(2): 279-285. |
| [14] | Yu Peng, Meng Dongfang, Li Huiying, Liu Hongfei, He Zike. Pinoresinol diglucoside activates the Wnt/beta-catenin signaling pathway to protect osteoblasts [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(2): 339-346. |
| [15] | Zhang Jun, Guo Jian, Jia Qiyu, Tang Lili, Wang Xi, Abudusalamu · Alimujiang, Wu Tong, Maihemuti · Yakufu, Ma Chuang. Effect and mechanism of BYL-719 on Mycobacterium tuberculosis-induced differentiation of abnormal osteoclasts [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(2): 355-360. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||