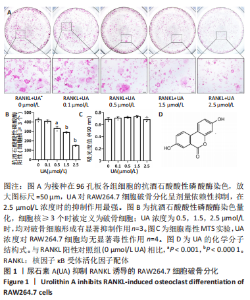
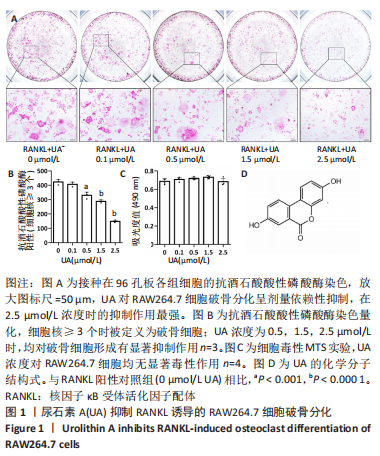
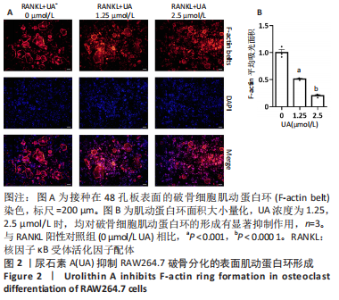
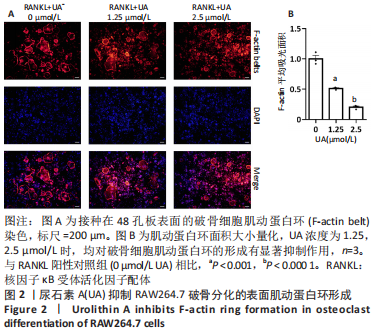
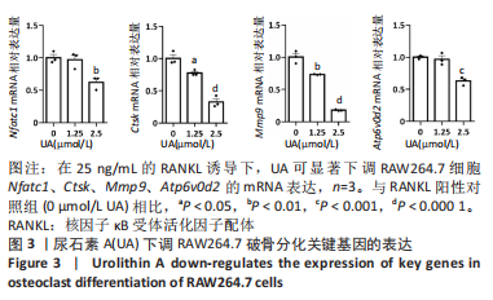
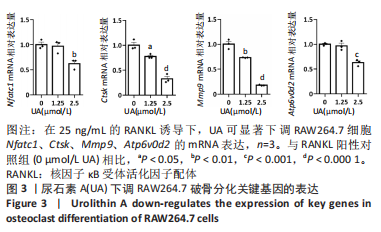
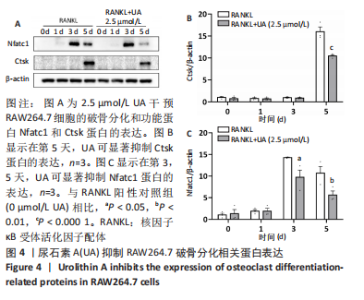
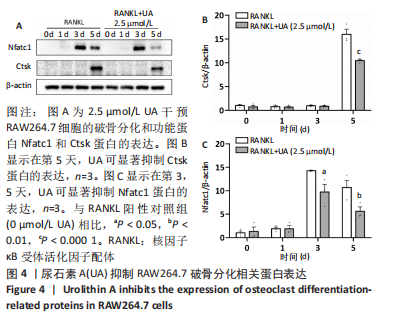
Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (8): 1149-1154.doi: 10.12307/2023.893
Urolithin A mediates p38/MAPK pathway to inhibit osteoclast activity
Huang Haoran1, Fan Yinuo2, Wei-Yang Wenxiang1, Jiang Mengyu1, Fang Hanjun1, Wang Haibin1, Chen Zhenqiu1, Liu Yuhao1, Zhou Chi1
- 1First Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China; 2Third Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510378, Guangdong Province, China
-
Received:2022-10-13Accepted:2022-11-25Online:2024-03-18Published:2023-07-18 -
Contact:Zhou Chi, MD, Associate chief physician, First Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China Liu Yuhao, MD, Physician, First Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China -
About author:Huang Haoran, Master candidate, Physician, First Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China -
Supported by:Guangdong Provincial Education Department Project, No. 2021KTSCX021 (to ZC); Guangdong Provincial Natural Science Foundation, No. 2021A1515011484 (to LYH); grants from Guangdong Provincial Administration of Traditional Chinese Medicine, Nos. 20221136 (to LYH), 20231162 (to CZQ), and 20231122 (to FHJ); Guangzhou University of Chinese Medicine "Double First-Class" and High-level University Discipline Collaborative Innovation Team Project, No. 2021xk46 (to CZQ)
CLC Number:
Cite this article
Huang Haoran, Fan Yinuo, Wei-Yang Wenxiang, Jiang Mengyu, Fang Hanjun, Wang Haibin, Chen Zhenqiu, Liu Yuhao, Zhou Chi. Urolithin A mediates p38/MAPK pathway to inhibit osteoclast activity[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1149-1154.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
| [1] SEEBACH E, KUBATZKY KF. Chronic Implant-Related Bone Infections-Can Immune Modulation be a Therapeutic Strategy? Front Immunol. 2019; 10:1724. [2] WALSH MC, KIM N, KADONO Y, et al. Osteoimmunology: interplay between the immune system and bone metabolism. Annu Rev Immunol. 2006;24:33-63. [3] ZHAO H, LU A, HE X. Roles of MicroRNAs in Bone Destruction of Rheumatoid Arthritis. Front Cell Dev Biol. 2020;8:600867. [4] RAUT N, WICKS SM, LAWAL TO, et al. Epigenetic regulation of bone remodeling by natural compounds. Pharmacol Res. 2019;147:104350. [5] DEL PUENTE A, ESPOSITO A, DEL PUENTE A, et al. Physiopathology of osteoporosis: from risk factors analysis to treatment. J Biol Regul Homeost Agents. 2015;29(3):527-531. [6] PARK DR, KIM J, KIM GM, et al. Osteoclast-associated receptor blockade prevents articular cartilage destruction via chondrocyte apoptosis regulation. Nat Commun. 2020;11(1):4343. [7] KIM JH, KIM N. Signaling Pathways in Osteoclast Differentiation. Chonnam Med J. 2016;52(1):12-17. [8] KIM JH, KIM N. Regulation of NFATc1 in Osteoclast Differentiation. J Bone Metab. 2014;21(4):233-241. [9] MARTIN TJ. Historically significant events in the discovery of RANK/RANKL/OPG. World J Orthop. 2013;4(4):186-197. [10] LIU J, ZHANG HX, LU XX, et al. Bisphosphonates and risk of subtrochanteric, femoral shaft, and atypical femur fracture: sensitivity and trim and fill studies. Genet Test Mol Biomarkers. 2014;18(2):117-122. [11] D’AMICO D, ANDREUX PA, VALDÉS P, et al. Impact of the Natural Compound Urolithin A on Health, Disease, and Aging. Trends Mol Med. 2021;27(7):687-699. [12] SAHA P, YEOH BS, SINGH R, et al. Gut Microbiota Conversion of Dietary Ellagic Acid into Bioactive Phytoceutical Urolithin A Inhibits Heme Peroxidases. PLoS One. 2016;11(6):e0156811. [13] NORDEN E, HEISS EH. Urolithin A gains in antiproliferative capacity by reducing the glycolytic potential via the p53/TIGAR axis in colon cancer cells. Carcinogenesis. 2019;40(1):93-101. [14] LIN X, YUAN G, LI Z, et al. Ellagic acid protects ovariectomy-induced bone loss in mice by inhibiting osteoclast differentiation and bone resorption. J Cell Physiol. 2020;35(9):5951-5961. [15] RANTLHA M, SAGAR T, KRUGER MC, et al. Ellagic acid inhibits RANKL-induced osteoclast differentiation by suppressing the p38 MAP kinase pathway. Arch Pharm Res. 2017;40(1):79-87. [16] XU H, CHEN F, LIU T, et al. Ellagic acid blocks RANKL-RANK interaction and suppresses RANKL-induced osteoclastogenesis by inhibiting RANK signaling pathways. Chem Biol Interact. 2020;331:109235. [17] LEE HJ, JUNG YH, CHOI GE, et al. Urolithin A suppresses high glucose-induced neuronal amyloidogenesis by modulating TGM2-dependent ER-mitochondria contacts and calcium homeostasis. Cell Death Differ. 2021;28(1):184-202. [18] KIM KB, LEE S, KIM JH. Neuroprotective effects of urolithin A on H(2)O(2)-induced oxidative stress-mediated apoptosis in SK-N-MC cells. Nutr Res Pract. 2020;14(1):3-11. [19] DASILVA NA, NAHAR PP, MA H, et al. Pomegranate ellagitannin-gut microbial-derived metabolites, urolithins, inhibit neuroinflammation in vitro. Nutr Neurosci. 2019;22(3):185-195. [20] RIGGS BL, WAHNER HW, DUNN WL, et al. Differential changes in bone mineral density of the appendicular and axial skeleton with aging: relationship to spinal osteoporosis. J Clin Invest. 1981;67(2):328-335. [21] RIGGS BL, WAHNER HW, SEEMAN E, et al. Changes in bone mineral density of the proximal femur and spine with aging. Differences between the postmenopausal and senile osteoporosis syndromes. J Clin Invest. 1982;70(4):716-723. [22] O’BRIEN MS, MCDOUGALL JJ. Age and frailty as risk factors for the development of osteoarthritis. Mech Ageing Dev. 2019;180:21-28. [23] PEREIRA D, SEVERO M, RAMOS E, et al. Potential role of age, sex, body mass index and pain to identify patients with knee osteoarthritis. Int J Rheum Dis. 2017;20(2):190-198. [24] MURATOVIC D, FINDLAY DM, CICUTTINI FM, et al. Bone matrix microdamage and vascular changes characterize bone marrow lesions in the subchondral bone of knee osteoarthritis. Bone. 2018;108:193-201. [25] XU Q, CAO Z, XU J, et al. Effects and mechanisms of natural plant active compounds for the treatment of osteoclast-mediated bone destructive diseases. J Drug Target. 2022;30(4):394-412. [26] HUANG WC, LIOU CJ, SHEN SC, et al. Urolithin A Inactivation of TLR3/TRIF Signaling to Block the NF-κB/STAT1 Axis Reduces Inflammation and Enhances Antioxidant Defense in Poly(I:C)-Induced RAW264.7 Cells. Int J Mol Sci. 2022;23(9):4697. [27] KOMATSU W, KISHI H, YAGASAKI K, et al. Urolithin A attenuates pro-inflammatory mediator production by suppressing PI3-K/Akt/NF-κB and JNK/AP-1 signaling pathways in lipopolysaccharide-stimulated RAW264 macrophages: Possible involvement of NADPH oxidase-derived reactive oxygen species. Eur J Pharmacol. 2018;833:411-424. [28] ZHANG W, CHEN JH, AGUILERA-BARRANTES I, et al. Urolithin A suppresses the proliferation of endometrial cancer cells by mediating estrogen receptor-α-dependent gene expression. Mol Nutr Food Res. 2016;60(11):2387-2395. [29] ALAUDDIN M, OKUMURA T, RAJAXAVIER J, et al. Gut Bacterial Metabolite Urolithin A Decreases Actin Polymerization and Migration in Cancer Cells. Mol Nutr Food Res. 2020;64(7):e1900390. [30] HSU H, LACEY DL, DUNSTAN CR, et al. Tumor necrosis factor receptor family member RANK mediates osteoclast differentiation and activation induced by osteoprotegerin ligand. Proc Natl Acad Sci U S A. 1999; 96(7):3540-3545. [31] HAYMAN AR. Tartrate-resistant acid phosphatase (TRAP) and the osteoclast/immune cell dichotomy. Autoimmunity. 2008;41(3):218-223. [32] VääNäNEN HK, ZHAO H, MULARI M, et al. The cell biology of osteoclast function. J Cell Sci. 2000;113(Pt 3):377-381. [33] LIU Y, WANG Z, MA C, et al. Dracorhodin perchlorate inhibits osteoclastogenesis through repressing RANKL-stimulated NFATc1 activity. J Cell Mol Med. 2020;24(6):3303-3313. [34] TAKAYANAGI H, KIM S, KOGA T, et al. Induction and activation of the transcription factor NFATc1 (NFAT2) integrate RANKL signaling in terminal differentiation of osteoclasts. Dev Cell. 2002;3(6):889-901. [35] LIU Y, WANG C, WANG G, et al. Loureirin B suppresses RANKL-induced osteoclastogenesis and ovariectomized osteoporosis via attenuating NFATc1 and ROS activities. Theranostics. 2019;9(16):4648-4662. [36] LOTINUN S, KIVIRANTA R, MATSUBARA T, et al. Osteoclast-specific cathepsin K deletion stimulates S1P-dependent bone formation. J Clin Invest. 2013;123(2):666-681. [37] WU H, XU G, LI YP. Atp6v0d2 is an essential component of the osteoclast-specific proton pump that mediates extracellular acidification in bone resorption. J Bone Miner Res. 2009;24(5):871-885. [38] KIM Y, KIM J, LEE H, et al. Tetracycline Analogs Inhibit Osteoclast Differentiation by Suppressing MMP-9-Mediated Histone H3 Cleavage. Int J Mol Sci. 2019;20(16):4038. [39] LEE K, SEO I, CHOI MH, et al. Roles of Mitogen-Activated Protein Kinases in Osteoclast Biology. Int J Mol Sci. 2018;19(10):3004. [40] WEI W, PENG C, GU R, et al. Urolithin A attenuates RANKL-induced osteoclastogenesis by co-regulating the p38 MAPK and Nrf2 signaling pathway. Eur J Pharmacol. 2022;921:174865. |
| [1] | Liu Jianhong, Liao Shijie, Li Boxiang, Tang Shengping, Wei Zhendi, Ding Xiaofei. Extracellular vesicles carrying non-coding RNA regulate the activation of osteoclasts [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1076-1082. |
| [2] | Wei Yuanxun, Chen Feng, Lin Zonghan, Zhang Chi, Pan Chengzhen, Wei Zongbo. The mechanism of Notch signaling pathway in osteoporosis and its prevention and treatment with traditional Chinese medicine [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 587-593. |
| [3] | Zuo Jun, Ma Shaolin. Mechanism of beta-sitosterol on hypertrophic scar fibroblasts: an analysis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 216-223. |
| [4] | Dang Yi, Du Chengyan, Yao Honglin, Yuan Nenghua, Cao Jin, Xiong Shan, Zhang Dingmei, Wang Xin. Hormonal osteonecrosis and oxidative stress [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1469-1476. |
| [5] | Long Guiyue, Li Dongdong, Liao Hongbing. Calcium phosphate cement/poly(lactic-co-glycolic acid) degradation products promote osteoclast differentiation of mouse monocytes [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1193-1198. |
| [6] | Huang Linke, Wei Linhua, Jiang Jie, Liu Qian, Chen Weiwei. Effects of estrogen combined with treadmill exercise on bone mass and articular cartilage in ovariectomized mice [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1166-1171. |
| [7] | Yang Zhishan, Tang Zhenglong. YAP/TAZ, a core factor of the Hippo signaling pathway, is involved in bone formation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1264-1271. |
| [8] | Zhang Min, Zhang Xiaoming, Liu Tongbin. Application potential of naringin in bone tissue regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 787-792. |
| [9] | Guo Yongjuan, Zhang Li, Lu Huamei. Effects of sevoflurane combined with propofol on pain mediators and neuronal activity in rats with spinal cord fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(36): 5850-5855. |
| [10] | Tang Xuyun, Chen Panbi, Du Dijia, Qin Zhongyin, Long Runjin. Acupoint catgut embedding regulates the role of type II alveolar epithelial cells in airway inflammation in asthmatic rats [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(35): 5688-5694. |
| [11] | Liu Chunli, Yan Yujuan, Mo Liwen, Wu Zhijie, Zhang Li. Effects of puerarin on osteoclast differentiation of RAW264.7 cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(32): 5114-5119. |
| [12] | Huang Haozhe, Zheng Min, Li Na, Sun Libo, Lan Yuyan, Liu Min. Effects of naringin on healing of tooth extraction wound in osteoporotic rats [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(32): 5144-5149. |
| [13] | Mo Yaomin, Liu Pan, Ma Ruixin, Zeng Gaofeng, Zong Shaohui. Mechanism of paroxetine on osteoclast differentiation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(32): 5184-5190. |
| [14] | Wang Huida, Sun Xiaotong, Bi Lan, Wang Zixuan, Zhang Ronghe. Effect of astragalus polysaccharides on orthodontic bone remodeling [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(32): 5214-5218. |
| [15] | Han Jie, Lin Zhiyu, Xu Zhiwei, Zhang Xiaoyun, Shang Yuzhi, Liu Hao. Interventional effect of microRNA on osteonecrosis of the femoral head through bone metabolism mechanism [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(32): 5238-5248. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||