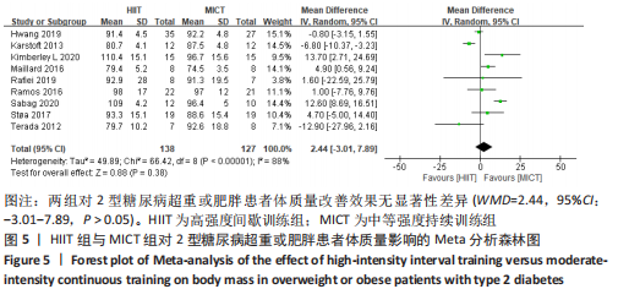
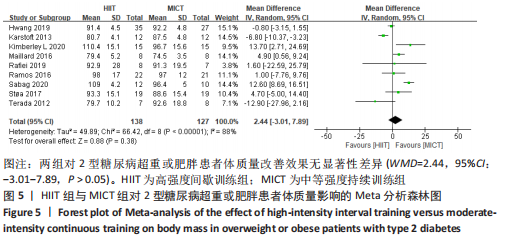
Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (14): 2274-2281.doi: 10.12307/2024.290
Previous Articles Next Articles
Effects of high-intensity interval training and moderate-intensity continuous training on body composition and glucose metabolism in overweight or obese patients with type 2 diabetes: a Meta-analysis
Liu Renfan1, 2, Lyu Liting2, Wu Yi2, Wang Lu2
- 1The Engineering & Technical College of Chengdu University of Technology, Leshan 614000, Sichuan Province, China; 2Teaching and Research Section of Sport Anatomy, Chengdu Sport University, Chengdu 610000, Sichuan Province, China
-
Received:2023-02-22Accepted:2023-04-10Online:2024-05-18Published:2023-07-28 -
Contact:Wang Lu, PhD, Associate professor, Master’s supervisor, Teaching and Research Section of Sport Anatomy, Chengdu Sport University, Chengdu 610000, Sichuan Province, China -
About author:Liu Renfan, Master, The Engineering & Technical College of Chengdu University of Technology, Leshan 614000, Sichuan Province, China; Teaching and Research Section of Sport Anatomy, Chengdu Sport University, Chengdu 610000, Sichuan Province, China -
Supported by:National Natural Science Foundation of China (Youth Program), No. 31900848 (to WL); 2021-2022 Innovation Project of Medicine and Health/Zheng Huaixian Institute of Orthopedic Injuries of Chengdu Sport University, No. CX21B05 (to WL); Youth Project of Sichuan Science and Technology Department, No. 2022NSFSC1724 (to WL)
CLC Number:
Cite this article
Liu Renfan, Lyu Liting, Wu Yi, Wang Lu. Effects of high-intensity interval training and moderate-intensity continuous training on body composition and glucose metabolism in overweight or obese patients with type 2 diabetes: a Meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(14): 2274-2281.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
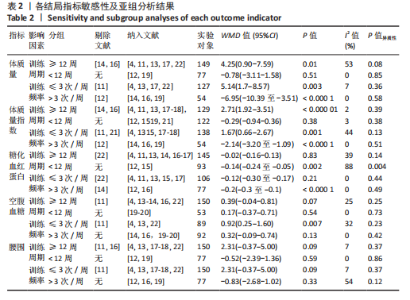
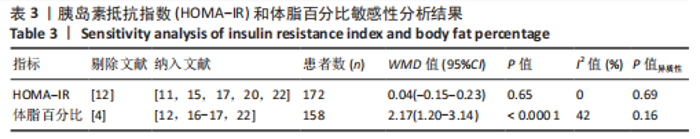
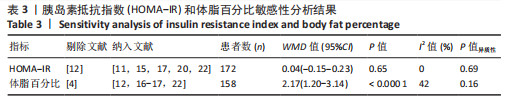
文章进一步探究异质性较高的原因,对体质量结局指标进行敏感性及亚组分析,结果见表2。由于2型糖尿病超重或肥胖患者结局指标可能受到干预周期及干预频率的影响,对上述影响因素进行亚组分析。对纳入9项随机对照试验根据训练周期、训练频率分组,训练周期分为≥12周与< 12周,训练频率分为≤3次/周与> 3次/周。训练周期≥12周纳入文献包括7篇[4,11,13-14,16-17,22],剔除2篇异质性较高的研究[14,16],异质性下降,I2=53%,P < 0.1,采用随机效应模型分析。Meta分析结果显示,总体合并效应量:WMD=4.25,95%CI:0.90-7.59,P=0.01。训练周期< 12周纳入文献2篇[12,19],I2=0%,P=0.85,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=-0.78,95%CI:-3.11-1.58,P=0.51。结果表明,当训练周期≥12周,MICT能显著减轻2型糖尿病超重或肥胖患者体质量,P < 0.05;当训练周期< 12周时,HIIT与MICT对2型糖尿病超重或肥胖患者体质量的改善效果无显著性差异,P > 0.05。"
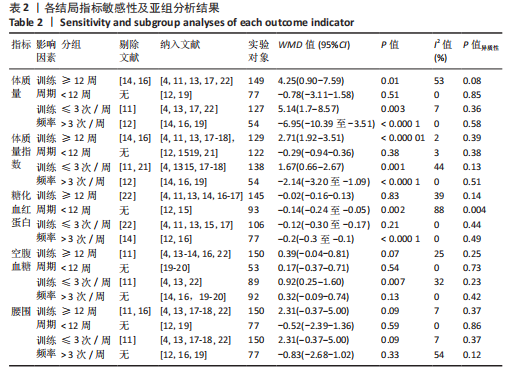
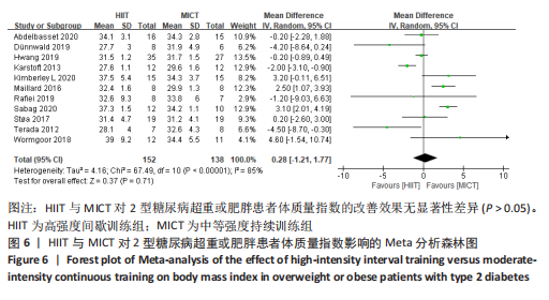
训练频率≤3次/周纳入文献5篇[4,11,13,17,22],剔除1篇研究[11],异质性显著下降,I2=7%,P=0.36,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=5.14,95%CI:1.7-8.57,P=0.003。训练频率>3次/周纳入文献4篇[12,14,16,19],剔除1篇文献[12],异质性显著下降,I2=0%,P=0.58,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=-6.95,95%CI:-10.39至-3.51,P < 0.000 1。因此,当训练频率≤3次/周时,MICT能显著减轻2型糖尿病超重或肥胖患者体质量;当训练频率> 3次/周时,HIIT能显著减轻2型糖尿病超重或肥胖患者体质量。 2.4.2 HIIT与MICT对2型糖尿病超重或肥胖患者体质量指数的影响 HIIT与MICT对2型糖尿病超重或肥胖患者体质量指数的影响共纳入11项随机对照试验[4,11-19,21],包括290例患者。纳入11项随机对照试验具有高度异质性,I2=85%,P < 0.1,采用随机效应模型分析。Meta分析结果显示,总体合并效应量:WMD=0.28,95%CI:-1.21-1.77,P > 0.05,见图6。"
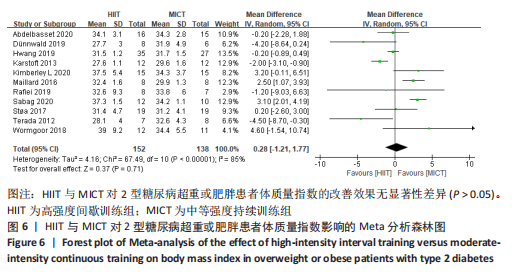

文章进一步探究异质性较大的原因,对体质量指数结局指标进行敏感性及亚组分析,见表2。训练周期≥12周纳入文献7篇[4,11,13-14,16-18],剔除2篇异质性较高的文献[14,16],异质性显著降低,I2=2%,P=0.39,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=2.71,95%CI:1.92-3.51,P < 0.000 01。训练周期< 12周纳入异质性极低的4篇文献[12,15,19,21],I2=3%,P=0.38,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=-0.29,95%CI:-0.94-0.36,P=0.38。因此,当训练周期≥12周时,MICT能显著降低2型糖尿病超重或肥胖患者体质量指数;当训练周期< 12周时,HIIT与MICT对2型糖尿病超重或肥胖患者体质量指数的改善效果无显著性差异。 训练频率≤3次/周纳入7篇文献[4,11,13,15,17-18,21],剔除2篇异质性较高的文献[11,21],异质性显著降低,I2=44%,P=0.13,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=1.67,95%CI:0.66-2.67,P=0.001。训练频率> 3次/周纳入4篇文献[12, 14, 16, 19],剔除1篇文献[12],异质性显著降低,I2=0%,P=0.51。Meta分析结果显示, 合并效应量:WMD=-2.14,95%CI:-3.20至-1.09,P < 0.000 1。表明:训练频率≤3次/周时,MICT能显著降低2型糖尿病超重或肥胖患者体质量指数,P < 0.05;训练频率> 3次/周时,HIIT能显著降低2型糖尿病超重或肥胖患者体质量指数,P < 0.05。 2.4.3 HIIT与MICT对2型糖尿病超重或肥胖患者腰围的影响 HIIT与MICT对2型糖尿病超重或肥胖患者腰围的影响共纳入文献9篇[4,11-13,16-19],包括264例患者。高度异质性,I2=82%,P < 0.1,采用随机效应模型。Meta分析结果显示,两组合并效应量显示差异无显著性意义(WMD=2.16,95%CI:-2.04-6.35,P > 0.05),见图7。"
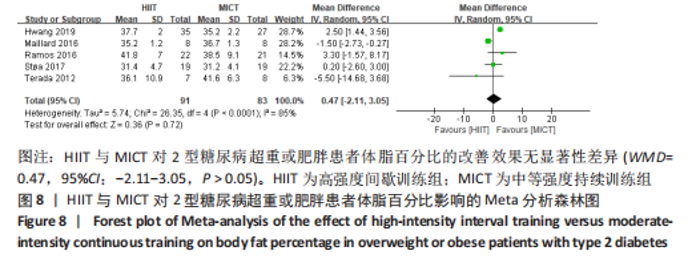
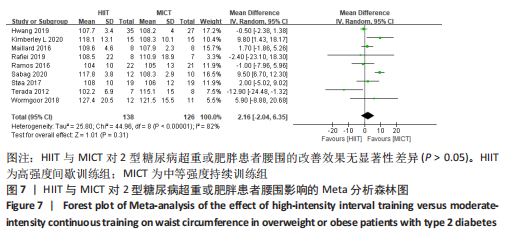

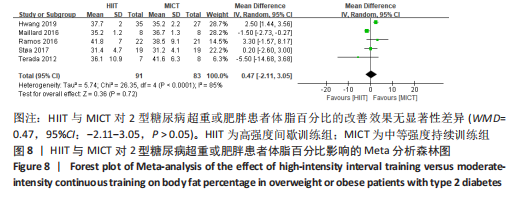
文章进一步探究异质性较大的原因,对腰围结局指标进行敏感性及亚组分析,结果见表2,训练周期≥12周纳入文献7篇[4,11,13,16-18,22],剔除文献2篇[11,16],异质性显著下降,I2=7%,P=0.37,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=2.31,95%CI:-0.37-5.00,P=0.09。训练周期< 12周纳入2篇文献[12,19],异质性极低,I2=0%、P=0.86,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=-0.52,95%CI:-2.39-1.36,P=0.59。表明HIIT与MICT训练周期的长短对改善2型糖尿病超重或肥胖患者腰围的效果影响不大,二者对腰围的改善效果无显著差异,P > 0.05。 训练频率≤3次/周纳入6篇文献[4,11,13,17,18,22],剔除1篇文献[11],异质性显著降低,I2=7%,P=0.37,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=2.31,95%CI:-0.37-5.00,P=0.09。训练频率> 3次/周纳入文献3篇[12,16,19],异质性降低,I2=54%,P=0.12,采用随机效应模型。Meta分析结果显示,总体合并效应量:WMD=-0.83,95%CI:-2.68-1.02,P=0.38。结果显示,HIIT与MICT训练频率多少对改善2型糖尿病超重或肥胖患者腰围的效果影响不大,二者对腰围的改善效果无显著差异(P > 0.05)。 2.4.4 HIIT与MICT对2型糖尿病超重或肥胖患者体脂百分比的影响 HIIT与MICT对2型糖尿病超重或肥胖患者体脂百分比的影响共纳入5项研究[4,12,16,17,22],包括174例患者,见图8,结果异质性较高,I2=85%,P < 0.1,采用随机效应模型,Meta分析结果显示,WMD=0.47,95%CI:-2.11-3.05,P > 0.05。"
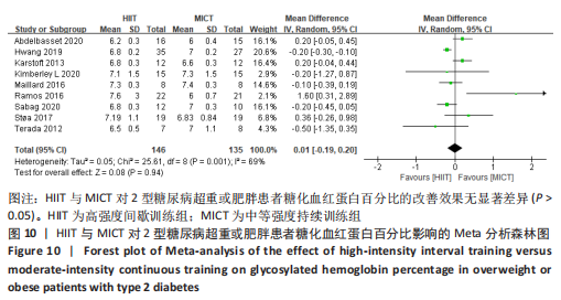
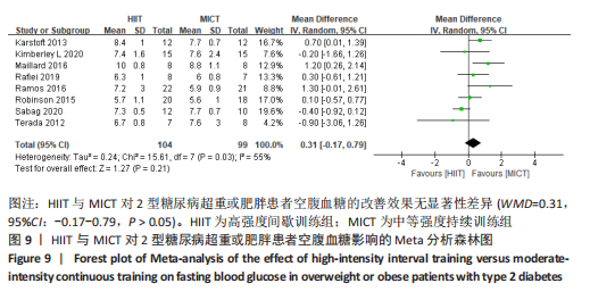
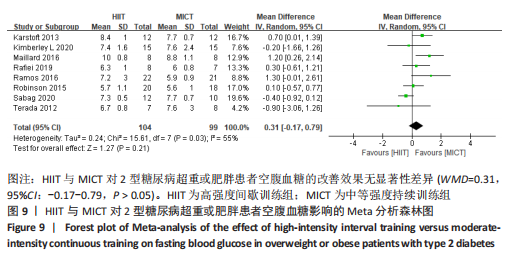
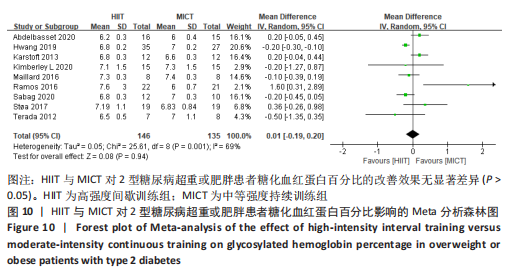
文章进一步探究异质性较大的原因,对空腹血糖结局指标进行敏感性及亚组分析,结果见表2。训练周期≥12周纳入文献6篇[4,11,13-14,16,22],剔除1篇文献[11],研究结果呈轻度异质性,I2=25%,P=0.25,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=0.39,95%CI:-0.04-0.81,P=0.07。训练周期< 12周纳入文献2篇[19-20],I2=0%,P=0.73,采用固定效应模型。Meta结果显示,总体合并效应量:WMD=0.17,95%CI:-0.37-0.71,P=0.54。因此,当训练周期对HIIT与MICT对2型糖尿病超重或肥胖患者空腹血糖的改善效果影响不大,二者无显著性差异,P > 0.05。 训练频率≤3次/周纳入文献4篇[4,11,13,22],剔除文献1篇[11],轻度异质性,I2=32%,P=0.23,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=0.92,95%CI:0.25-1.60,P=0.007。训练频率> 3次/周纳入4篇文献[14,16,19,20],异质性极低,I2=0%、P=0.42,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=0.32,95%CI:-0.09-0.74,P=0.13,表明当训练频率≤3次/周,MICT能显著降低2型糖尿病肥胖或超重患者空腹血糖,P < 0.05;当训练频率> 3次/周,二者对2型糖尿病超重肥胖或患者空腹血糖改善效果无显著差异性,P > 0.05。 2.4.6 HIIT与MICT对2型糖尿病超重或肥胖患者糖化血红蛋白的影响 HIIT与MICT对2型糖尿病超重或肥胖患者糖化血红蛋白的影响共纳入9篇研究[4,11-17,22],包括281例患者。 纳入9项随机对照试验显示中度异质性,I2=69%,P < 0.1,采用随机效应模型。Meta分析结果显示,总体合并效应量:WMD=0.01,95%CI:-0.19-0.20,P > 0.05,见图10。"
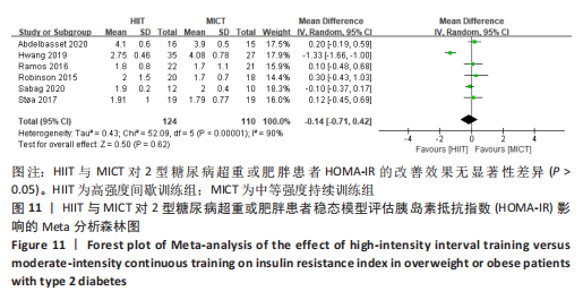
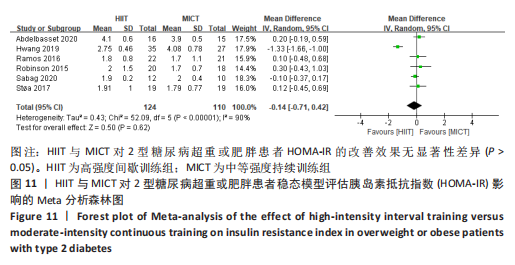
文章进一步探究异质性较大的原因,对糖化血红蛋白百分比结局指标进行敏感性及亚组分析,结果见表2。训练周期≥12周纳入文献7篇[4,11,13-14,16-17,22],剔除1篇[22],研究结果显示异质性下降,I2=39%,P=0.14,采用固定效应模型。Meta分析结果,合并效应量:WMD=-0.02,95%CI:-0.16-0.13,P=0.83;训练周期< 12周纳入文献2篇[12,15],研究结果显示异质性较高,I2=88%,P=0.004,不做Meta亚组分析。当训练周期≥12周,HIIT与MICT对2型糖尿病超重或肥胖患者糖化血红蛋白百分比的改善效果无显著差异,P > 0.05。 训练频率≤3次/周纳入文献6篇[4,11,13,15,17,22],剔除文献1篇[22],异质性显著降低,I2=0%、P=0.44,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=-0.12,95%CI:-0.3-0.06,P=0.21;训练频率> 3次/周纳入文献3篇[12,14,16],剔除1篇文献[14],异质性显著降低,I2=0%,P=0.49,采用固定效应模型。Meta分析结果显示,总体合并效应量:WMD=-0.2,95%CI:-0.3至-0.1,P < 0.000 1。表明:当训练频率≤3次/周时,HIIT与MICT对2型糖尿病超重或肥胖患者糖化血红蛋白百分比的改善效果无显著差异,P > 0.05;当训练频率> 3次/周,HIIT能显著降低2型糖尿病超重或肥胖患者糖化血红蛋白百分比,P < 0.05。 2.4.7 HIIT与MICT对2型糖尿病超重或肥胖患者HOMA-IR的影响 HIIT与MICT对2型糖尿病超重或肥胖患者HOMA-IR的影响共纳入文献6篇[11-12,15,17. 20,22],包括234例患者,结果见图11,异质性较高I2=90%,P < 0.1,采用随机效应模型。Meta分析结果显示,总体合并效应量:WMD=-0.14,95%CI:-0.71-0.42,P > 0.05。"
| [1] AMANAT S, GHAHRI S, DIANATINASAB A, et al. Exercise and type 2 diabetes. Adv Exp Med Biol. 2020;1228:91-105. [2] CARBONE S, DEL BUONO MG, OZEMEK C, et al. Obesity, risk of diabetes and role of physical activity, exercise training and cardiorespiratory fitness. Prog Cardiovasc Dis. 2019;62(4):327-333. [3] COLE JB, FLOREZ JC. Genetics of diabetes mellitus and diabetes complications. Nat Rev Nephrol. 2020;16(7):377-390. [4] MAILLARD F, ROUSSET S, PEREIRA B, et al. High-intensity interval training reduces abdominal fat mass in postmenopausal women with type 2 diabetes. Diabetes Metab. 2016;42(6):433-441. [5] ABEL ED, PERONI O, KIM JK, et al. Adipose-selective targeting of the GLUT4 gene impairs insulin action in muscle and liver. Nature. 2001;409(6821):729-733. [6] SAMUEL VT, SHULMAN GI. The pathogenesis of insulin resistance: integrating signaling pathways and substrate flux. J Clin Invest. 2016;126(1):12-22. [7] STANFORD KI, GOODYEAR LJ. Exercise and type 2 diabetes:molecular mechanisms regulating glucose uptake in skeletal muscle. Adv Physiol Educ. 2014;38(4):308-314. [8] UMPIERRE D, RIBEIRO PA, KRAMER CK, et al. Physical activity advice only or structured exercise training and association with HbA1c levels in type 2 diabetes: a systematic review and meta-analysis. JAMA. 2011;305(17):1790-1799. [9] SNOWLING NJ, HOPKINS WG. Effects of different modes of exercise training on glucose control and risk factors for complications in type 2 diabetic patients: a meta-analysis. Diabetes Care. 2006;29(11):2518-2527. [10] JORGE ML, DE OLIVEIRA VN, RESENDE NM, et al. The effects of aerobic, resistance, and combined exercise on metabolic control, inflammatory markers, adipocytokines, and muscle insulin signaling in patients with type 2 diabetes mellitus. Metabolism. 2011;60(9):1244-1252. [11] SABAG A, WAY KL, SULTANA RN, et al. The effect of a novel low-volume aerobic exercise intervention on liver fat in type 2 diabetes: a randomized controlled trial. Diabetes Care. 2020;43(10):2371-2378. [12] HWANG CL, LIM J, YOO JK, et al. Effect of all-extremity high-intensity interval training vs. moderate-intensity continuous training on aerobic fitness in middle-aged and older adults with type 2 diabetes: a randomized controlled trial. Exp Gerontol. 2019;116:46-53. [13] WAY KL, SABAG A, SULTANA RN, et al. The effect of low-volume high-intensity interval training on cardiovascular health outcomes in type 2 diabetes: a randomised controlled trial. Int J Cardiol. 2020;320:148-154. [14] KARSTOFT K, WINDING K, KNUDSEN SH, et al. The effects of free-living interval-walking training on glycemic control, body composition, and physical fitness in type 2 diabetic patients: a randomized, controlled trial. Diabetes Care. 2013;36(2):228-236. [15] ABDELBASSET WK, TANTAWY SA, KAMEL DM, et al. Effects of high-intensity interval and moderate-intensity continuous aerobic exercise on diabetic obese patients with nonalcoholic fatty liver disease: a comparative randomized controlled trial. Medicine (Baltimore). 2020; 99(10):e19471. [16] TERADA T, FRIESEN A, CHAHAL BS, et al. Feasibility and preliminary efficacy of high intensity interval training in type 2 diabetes. Diabetes Res Clin Pract. 2013;99(2): 120-129. [17] STOA EM, MELING S, NYHUS LK, et al. High-intensity aerobic interval training improves aerobic fitness and HbA1c among persons diagnosed with type 2 diabetes. Eur J Appl Physiol. 2017;117(3):455-467. [18] WORMGOOR SG, DALLECK LC, ZINN C, et al. High-intensity interval training is equivalent to moderate-intensity continuous training for short- and medium-term outcomes of glucose control, cardiometabolic risk, and microvascular complication markers in men with type 2 diabetes. Front Endocrinol (Lausanne). 2018;9:475. [19] RAFIEI H, ROBINSON E, BARRY J, et al. Short-term exercise training reduces glycaemic variability and lowers circulating endothelial microparticles in overweight and obese women at elevated risk of type 2 diabetes. Eur J Sport Sci. 2019;19(8):1140-1149. [20] ROBINSON E, DURRER C, SIMTCHOUK S, et al. Short-term high-intensity interval and moderate-intensity continuous training reduce leukocyte TLR4 in inactive adults at elevated risk of type 2 diabetes. J Appl Physiol (1985). 2015;119(5):508-516. [21] DüNNWALD T, MELMER A, GATTERER H, et al. Supervised short-term high-intensity training on plasma irisin concentrations in type 2 diabetic patients. Int J Sports Med. 2019;40(3):158-164. [22] RAMOS JS, DALLECK LC, BORRANI F, et al. The effect of different volumes of high-intensity interval training on proinsulin in participants with the metabolic syndrome:a randomised trial. Diabetologia. 2016;59(11):2308-2320. [23] AMERICAN DIABETES ASSOCIATION. 2. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes-2018. Diabetes Care. 2018;41(Suppl 1):S13-S27. [24] DAVEGåRDH C, GARCíA-CALZóN S, BACOS K, et al. DNA methylation in the pathogenesis of type 2 diabetes in humans. Mol Metab. 2018;14:12-25. [25] STEFANI L, GALANTI G. Physical exercise prescription in metabolic chronic disease. Adv Exp Med Biol. 2017;1005:123-141. [26] MENDES R, SOUSA N, THEMUDO-BARATA JL, et al. High-intensity interval training versus moderate-intensity continuous training in middle-aged and older patients with type 2 diabetes: a randomized controlled crossover trial of the acute effects of treadmill walking on glycemic control. Int J Environ Res Public Health. 2019;16(21):4163. [27] ESPINOZA SILVA JM, LATORRE ROMÁN PÁ, CABRERA LINARES JC, et al. Effects of a high intensity interval training (HIIT) program on anthropomorphic and cardiometabolic variables in school children with overweight and obesity. Children (Basel). 2023;10(2):317. [28] DUPUIT M, RANCE M, MOREL C, et al. MICT or HIIT ± RT programs for altering body composition in postmenopausal women. Med Sci Sports Exerc. 2019;52(3):1. [29] 赵广高,洪熊,苏利强,等.高强度间歇训练与中强度持续训练对超重/肥胖成人体成分干预作用的比较:Meta分析[J].成都体育学院学报,2017,43(4):93-99. [30] 曹文玲.高强度间歇运动对肥胖青年女性血压、心率恢复和血清肌钙蛋白水平的影响及其训练适应[D].石家庄:河北师范大学, 2018. |
| [1] | Su Xiaoyang, Chen Wenting, Fu Yidan, Zhao Yan, Lan Danfeng, Yang Qiuping. Correlation between Mer receptor tyrosine kinase and diabetic peripheral neuropathy in Sprague-Dawley rats [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(8): 1593-1599. |
| [2] | Wang Yida, Liu Jun, Wang Xiaoling, Wang Liyan, Yang Chengru, Zhang Xuexiao. Effects of wearable electronic device-based interventions on physical activity and sedentary behavior in healthy adolescents: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(8): 1693-1704. |
| [3] | Zhang Zixian, Xu Youliang, Wu Shaokui, Wang Xiangying. Effects of blood flow restriction training combined with resistance training on muscle indicators in college athletes: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(8): 1705-1713. |
| [4] | Wang Juan, Wang Guanglan, Zuo Huiwu. Efficacy of exercise therapy in the treatment of anterior cruciate ligament reconstruction patients: #br# a network meta-analysis #br# [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(8): 1714-1726. |
| [5] | Zheng Huakun, Yin Mingyue, Liu Qian. Effects of interval and continuous training on the quality of life in physically inactive adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(8): 1727-1740. |
| [6] | Wang Jianlei, He Peiliang, Sun Yongjian. A meta-analysis of clinical efficacy and safety of intravenous glucocorticoids before lower limb joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(3): 599-607. |
| [7] | Li Jia, Liu Qianru, Xing Mengnan, Chen Bo, Jiao Wei, Meng Zhaoxiang. A network meta-analysis on therapeutic effect of different types of exercise on knee osteoarthritis patients [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(3): 609-616. |
| [8] | Zhou Yanjie, Cao Chunfeng, Zhang Zhongzu, Niu Xiong, Wang Xin, Yang Zaihai, Zhou Liang, Li Bo. Meta-analysis of anterior cervical decompression and fusion ROI-CTM self-locking system in treatment of degenerative cervical spondylosis [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(3): 617-627. |
| [9] | Hu Shujuan, Cheng Ping, Zhang Xiao, Ding Yiting, Liu Xuan, Pu Rui, Wang Xianwang. Effects of different exercise interventions on carboxylesterase 1 and inflammatory factors in skeletal muscle of type 2 diabetic rats [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(2): 269-278. |
| [10] | Yu Hanglin, Tian Haodong, Wen Shiyuan, Huang Li, Liu Haowei, Li Hansen, Wang Peisong, Peng Li. Changes in glucose metabolism and intestinal flora in patients with type 2 diabetes mellitus after high-intensity intermittent exercise [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(2): 286-293. |
| [11] |
Yang Fengying, Zhao Yuqing, You Huijuan, Zhang Pengyi, Chen Yan, Wang Qinglu, Liu Yingying .
Macrophage efferocytosis: a new target for the treatment of obesity-related metabolic diseases #br#
#br#
[J]. Chinese Journal of Tissue Engineering Research, 2025, 29(2): 430-440.
|
| [12] | Zhong Jun, Wang Wen. Network meta-analysis of different anatomical repair strategies to improve chronic lateral ankle instability [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1470-1476. |
| [13] | Wang Ji, Zhang Min, Li Wenbo, Yang Zhongya, Zhang Long. Effect of aerobic exercise on glycolipid metabolism, skeletal muscle inflammation and autophagy in type 2 diabetic rats [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1200-1205. |
| [14] | Wei Juan, Li Ting, Huan Mengting, Xie Ying, Xie Zhouyu, Wei Qingbo, Wu Yunchuan. Mechanism by which static exercise improves insulin resistance in skeletal muscle of type 2 diabetes [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1271-1276. |
| [15] | Wang Weiqing, Zhou Yue. Chronic inflammation regulates adipose tissue fibrosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1307-1312. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||