Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (28): 4494-4501.doi: 10.12307/2023.518
Previous Articles Next Articles
Zoledronic acid promotes alveolar bone formation in ovariectomized rats
Song Na, Liu Guanjuan, Cheng Yuting, Xiong Yue, Luo Shanshan, Hong Wei, Liao Jian
- School of Stomatology/Affiliated Stomatological Hospital of Guizhou Medical University, Key Laboratory of Molecular Biology, Guiyang 550004, Guizhou Province, China
-
Received:2022-07-08Accepted:2022-08-24Online:2023-10-08Published:2023-01-29 -
Contact:Liao Jian, MD, Professor, Chief physician, Master’s supervisor, Doctoral supervisor, School of Stomatology/Affiliated Stomatological Hospital of Guizhou Medical University, Key Laboratory of Molecular Biology, Guiyang 550004, Guizhou Province, China -
About author:Song Na, Master candidate, School of Stomatology/Affiliated Stomatological Hospital of Guizhou Medical University, Key Laboratory of Molecular Biology, Guiyang 550004, Guizhou Province, China -
Supported by:the National Natural Science Foundation of China, Nos. 82060207 and 81660179 (both to LJ); Guizhou Provincial Health Commission Science and Technology Foundation, No. gzwkj2022-165 (to LJ)
CLC Number:
Cite this article
Song Na, Liu Guanjuan, Cheng Yuting, Xiong Yue, Luo Shanshan, Hong Wei, Liao Jian. Zoledronic acid promotes alveolar bone formation in ovariectomized rats[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(28): 4494-4501.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
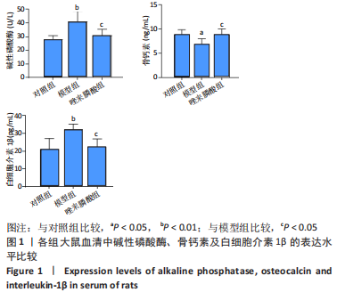
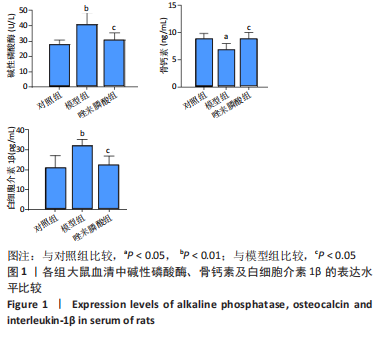
2.1 实验动物数量分析 纳入实验动物数量36只,随机分为3组,每组12只,实验过程中无脱失。 2.2 唑来膦酸对骨质疏松大鼠血清中成骨细胞分化因子及炎性因子的影响 与对照组比较,模型组大鼠血清中成骨分化相关因子碱性磷酸酶活性显著升高(P < 0.01)、骨钙素质量浓度显著降低(P < 0.05),炎性因子IL-1β水平显著升高(P < 0.01);与模型组比较,唑来磷酸组大鼠血清中碱性磷酸酶活性显著降低(P < 0.05)、骨钙素质量浓度显著升高(P < 0.05),炎性因子IL-1β水平显著降低(P < 0.05);与对照组比较,唑来膦酸组大鼠血清中碱性磷酸酶、骨钙素、IL-1β表达无明显差异,见图1。"
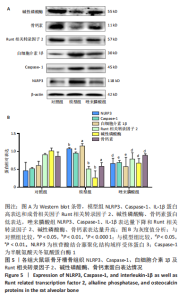
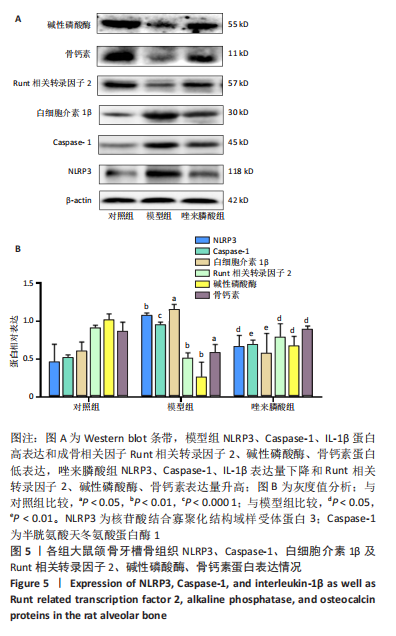
2.6 唑来膦酸对骨质疏松大鼠牙槽骨骨组织蛋白中成骨细胞分化相关因子及NLRP3、Caspase-1、IL-1β蛋白表达的影响 与对照组相比,模型组牙槽骨骨组织Runt 相关转录因子 2、碱性磷酸酶、骨钙素蛋白相对表达量显著降低(P < 0.05),NLRP3、Caspase-1、IL-1β蛋白相对表达量显著升高(P < 0.05);与模型组相比,唑来膦酸组牙槽骨骨组织Runt 相关转录因子 2、碱性磷酸酶、骨钙素蛋白相对表达量显著升高(P < 0.05),NLRP3、Caspase-1、IL-1β蛋白相对表达量显著降低(P < 0.05),而对照组与唑来膦酸组相比差异无显著性意义,见图5。"
| [1] CHEN X, MORIYAMA Y, TAKEMURA Y, et al. Influence of osteoporosis and mechanical loading on bone around osseointegrated dental implants: A rodent study. J Mech Behav Biomed Mater. 2021;123: 104771. [2] ALIPPE Y, MBALAVIELE G. Omnipresence of inflammasome activities in inflammatory bone diseases. Semin Immunopathol. 2019;41(5):607-618. [3] HENDRICKS R, VICATOS G. Creation of bone and soft tissue in postmaxillectomy patients using curvilinear transport distraction osteogenesis. Ann Maxillofac Surg. 2019;9(2):319-325. [4] FISCHER V, HAFFNER-LUNTZER M. Interaction between bone and immune cells: Implications for postmenopausal osteoporosis. Semin Cell Dev Biol. 2022;123:14-21. [5] NOH JY, YANG Y, JUNG H. Molecular mechanisms and emerging therapeutics for osteoporosis. Int J Mol Sci. 2020;21(20):7623. [6] PARIHAR AS, MADHURI S, DEVANNA R, et al. Assessment of failure rate of dental implants in medically compromised patients. J Family Med Prim Care. 2020;9(2):883-885. [7] DIACHKOVA E, ABRAMOVA EV, BLAGUSHINA NA, et al. Surgical treatment with dental implants in a patient with secondary loss of teeth and osteoporosis caused by an imbalance of vitamin D. BMJ Case Rep. 2020;13(11):e235585. [8] GIRO G, CHAMBRONE L, GOLDSTEIN A, et al.Impact of osteoporosis in dental implants: A systematic review. word J Orthop,2015,6(2): 31-35. [9] SCALA R, MAQOUD F, ANTONACCI M, et al. Bisphosphonates targeting ion channels and musculoskeletal effects. Front Pharmacol. 2022;13: 837534. [10] DERENNE S, AMIOT M, BARILLÉ S, et al. Zoledronate is a potent inhibitor of myeloma cell growth and secretion of IL-6 and MMP-1 by the tumoral environment. J Bone Miner Res. 1999;14(12):2048-2056. [11] PLOTKIN LI, MANOLAGAS SC, BELLIDO T. Dissociation of the pro-apoptotic effects of bisphosphonates on osteoclasts from their anti-apoptotic effects on osteoblasts/osteocytes with novel analogs. Bone. 2006;39(3):443-452. [12] FREDIANI B, SPREAFICO A, CAPPERUCCI C, et al. Long-term effects of neridronate on human osteoblastic cell cultures. Bone. 2004;35(4): 859-869. [13] RUGGIERO SL, DODSON TB, FANTASIA J, et al. American Association of Oral and Maxillofacial Surgeons position paper on medication-related osteonecrosis of the jaw--2014 update. J Oral Maxillofac Surg. 2014;72(10):1938-1956. [14] SRIVICHIT B, THONUSIN C, CHATTIPAKORN N, et al. Impacts of bisphosphonates on the bone and its surrounding tissues: mechanistic insights into medication-related osteonecrosis of the jaw. Arch Toxicol. 2022;96(5):1227-1255. [15] VERGARA-HERNANDEZ FB, NIELSEN BD, COLBATH AC. Is the Use of bisphosphonates putting horses at risk? An Osteoclast Perspective. Animals (Basel). 2022;12(13):1722. [16] HUANG X, HUANG S, GUO F, et al. Dose-dependent inhibitory effects of zoledronic acid on osteoblast viability and function in vitro. Mol Med Rep. 2016;13(1):613-622. [17] 李颉颃, 苏志飞, 白璇, 等. 唑来膦酸对大鼠骨髓间充质干细胞增殖及成骨分化的作用研究[J]. 华西口腔医学杂志,2019,37(3):242-247. [18] LI JH, SU ZF, BAI X, et al. Effect of zoladronate on the proliferation and osteogenic differentiation of rat bone mesenchymal stem cells. Hua Xi Kou Qiang Yi Xue Za Zhi. 2019;37(3):242-247. [19] BASSO FG, PANSANI TN, CARDOSO LM, et al. Influence of bisphosphonates on the behavior of osteoblasts seeded onto titanium discs. Braz Dent J. 2020;31(3):304-309. [20] 霍花, 刘官娟, 宋娜, 等. 唑来膦酸干预去势大鼠牙槽骨骨代谢及核苷酸结合寡聚化结构域样受体蛋白3炎症小体表达的变化 [J]. 中国组织工程研究,2022,26(17):2660-2666. [21] 程余婷, 伍超, 黄晓林, 等. 低剂量唑来膦酸对去势拔牙大鼠破骨及成骨细胞的影响[J]. 中国组织工程研究,2020,24(17):2686-2693. [22] CHENG YT, LIAO J, ZHOU Q, et al. Zoledronic acid modulates osteoclast apoptosis through activation of the NF-κB signaling pathway in ovariectomized rats. Exp Biol Med (Maywood). 2021;246(15):1727-1739. [23] HUANG XL, HUANG LY, CHENG YT, et al. Zoledronic acid inhibits osteoclast differentiation and function through the regulation of NF-κB and JNK signalling pathways. Int J Mol Med. 2019;44(2):582-592. [24] HUANG XL, LIU C, SHI XM, et al. Zoledronic acid inhibits osteoclastogenesis and bone resorptive function by suppressing RANKL‑mediated NF‑κB and JNK and their downstream signalling pathways. Mol Med Rep. 2022;25(2):59. [25] BASSO FG, SILVEIRA TURRIONI AP, HEBLING J, et al. Zoledronic acid inhibits human osteoblast activities. Gerontology. 2013;59(6):534-541. [26] JIANG N, AN J, YANG K, et al. NLRP3 Inflammasome: A new target for prevention and control of osteoporosis? Front Endocrinol (Lausanne). 2021;12:752546. [27] CLINE-SMITH A, AXELBAUM A, SHASHKOVA E, et al. Ovariectomy activates chronic low-grade inflammation mediated by memory T cells, which promotes osteoporosis in mice. J Bone Miner Res. 2020;35(6): 1174-1187. [28] XIN W, WANG X, ZHANG W, et al. Tumor necrosis factor-α inhibits bone marrow stem cell differentiation into osteoblasts by downregulating microRNA-34a expression. Ann Clin Lab Sci. 2019;49(3):324-329. [29] LATZ E, DUEWELL P. NLRP3 inflammasome activation in inflammaging. Semin Immunol. 2018;40:61-73. [30] YOUSEFZADEH N, KASHFI K, JEDDI S, et al. Ovariectomized rat model of osteoporosis: a practical guide. Excli J. 2020;19:89-107. [31] JAYUSMAN PA, MOHAMED IN, ALIAS E, et al. The Effects of quassinoid-rich eurycoma longifolia extract on bone turnover and histomorphometry indices in the androgen-deficient osteoporosis rat model. Nutrients. 2018;10(7):799. [32] ARIOKA M, ZHANG X, LI Z, et al. Osteoporotic changes in the periodontium impair alveolar bone healing. J Dent Res. 2019;98(4): 450-458. [33] LIU Y, LI Z, ARIOKA M, et al. WNT3A accelerates delayed alveolar bone repair in ovariectomized mice. Osteoporos Int. 2019;30(9):1873-1885. [34] CHEN CH, WANG L, SERDAR TULU U, et al. An osteopenic/osteoporotic phenotype delays alveolar bone repair. Bone. 2018;112:212-219. [35] Só BB, SILVEIRA FM, LLANTADA GS, et al. Effects of osteoporosis on alveolar bone repair after tooth extraction: A systematic review of preclinical studies. Arch Oral Biol. 2021;125:105054. [36] LOTZ EM, COHEN DJ, SCHWARTZ Z, et al. Titanium implant surface properties enhance osseointegration in ovariectomy induced osteoporotic rats without pharmacologic intervention. Clin Oral Implants Res. 2020;31(4):374-387. [37] LIU W, ZHOU L, ZHOU C, et al. GDF11 decreases bone mass by stimulating osteoclastogenesis and inhibiting osteoblast differentiation. Nat Commun. 2016;7:12794. [38] SHAPIRO JR, BOSKEY AL, DOTY SB, et al. Zoledronic acid improves bone histomorphometry in a murine model of Rett syndrome. Bone. 2017; 99:1-7. [39] OCHIAI H, OKADA S, SAITO A, et al. Inhibition of insulin-like growth factor-1 (IGF-1) expression by prolonged transforming growth factor-β1 (TGF-β1) administration suppresses osteoblast differentiation. J Biol Chem. 2012;287(27):22654-22661. [40] ALSALIH A, DAM A, LINDBERG P, et al. Medication-related osteonecrosis of the jaws initiated by zoledronic acid and potential pathophysiology. Dent J (Basel). 2021; 9(8):85. [41] MCGOWAN K, MCGOWAN T, IVANOVSKI S. Risk factors for medication-related osteonecrosis of the jaws: A systematic review. Oral Dis. 2018; 24(4):527-536. [42] YING G, BO L, YANJUN J, et al. Effect of a local, one time, low-dose injection of zoledronic acid on titanium implant osseointegration in ovariectomized rats. Arch Med Sci. 2016;12(5):941-949. [43] GREY A, BOLLAND MJ, HORNE A, et al. Bone mineral density and bone turnover 10 years after a single 5 mg dose or two 5-yearly lower doses of zoledronate in osteopenic older women: an open-label extension of a randomized controlled trial. J Bone Miner Res. 2022;37(1):3-11. [44] OMIDVAR MH, SOLTANI-ZANGBAR MS, ZAMANI M, et al. The effect of osteoporotic and non-osteoporotic individuals’ T cell-derived exosomes on osteoblast cells’ bone remodeling related genes expression and alkaline phosphatase activity. BMC Res Notes. 2022;15(1):272. [45] SHAIKHOMAR OA, ABDELGHNAY AH, QUTOB HMH. Diagnosis of low bone mass density: serological versus radiological methods. Int J Gen Med. 2022;15:5937-5945. [46] 张萌萌, 张秀珍, 邓伟民, 等. 骨代谢生化指标临床应用专家共识(2020) [J]. 中国骨质疏松杂志,2020,26(6):781-796. [47] QI S. Synergistic effects of genistein and zinc on bone metabolism and the femoral metaphyseal histomorphology in the ovariectomized rats. Biol Trace Elem Res. 2018;183(2):288-295. [48] MIZOKAMI A, KAWAKUBO-YASUKOCHI T, HIRATA M. Osteocalcin and its endocrine functions. Biochem Pharmacol. 2017;132:1-8. [49] YU C, LI L, XIE F, et al. LncRNA TUG1 sponges miR-204-5p to promote osteoblast differentiation through upregulating Runx2 in aortic valve calcification. Cardiovasc Res. 2018;114(1): 68-179. [50] YANG JX, XIE P, LI YS, et al. Osteoclast-derived miR-23a-5p-containing exosomes inhibit osteogenic differentiation by regulating Runx2. Cell Signal. 2020;70:109504. [51] XU X, CHEN Y, TAN B, et al. Circular RNA circ_0011269 sponges miR-122 to regulate RUNX2 expression and promotes osteoporosis progression. J Cell Biochem. 2020; doi: 10.1002/jcb.29709. [52] NAITO J, KAJI H, SOWA H, et al. Menin suppresses osteoblast differentiation by antagonizing the AP-1 factor, JunD. J Biol Chem. 2005; 280(6):4785-4791. [53] XU L, SHEN L, YU X, et al. Effects of irisin on osteoblast apoptosis and osteoporosis in postmenopausal osteoporosis rats through upregulating Nrf2 and inhibiting NLRP3 inflammasome. Exp Ther Med. 2020;19(2):1084-1090. [54] SCHRODER K, TSCHOPP J. The inflammasomes. Cell. 2010;140(6):821-832. [55] MURAKAMI T, NAKAMINAMI Y, TAKAHATA Y, et al. Activation and function of NLRP3 inflammasome in bone and joint-related diseases. Int J Mol Sci. 2022;23(10):5365. [56] CHENG C, CHEN L, CHEN K. Osteoporosis due to hormone imbalance: an overview of the effects of estrogen deficiency and glucocorticoid overuse on bone turnover. Int J Mol Sci. 2022;23(3):1376. [57] PINGALI U, NUTALAPATI C. Shilajit extract reduces oxidative stress, inflammation, and bone loss to dose-dependently preserve bone mineral density in postmenopausal women with osteopenia: A randomized, double-blind, placebo-controlled trial. Phytomedicine. 2022;105:154334. [58] XU L, ZHANG L, WANG Z, et al. Melatonin suppresses estrogen deficiency-induced osteoporosis and promotes osteoblastogenesis by inactivating the NLRP3 inflammasome. Calcif Tissue Int. 2018;103(4): 400-410. [59] TAO H, LI W, ZHANG W, et al. Urolithin a suppresses RANKL-induced osteoclastogenesis and postmenopausal osteoporosis by, suppresses inflammation and downstream NF-κB activated pyroptosis pathways. Pharmacol Res. 2021;174:105967. [60] AN Y, ZHANG H, WANG C, et al. Activation of ROS/MAPKs/NF-κB/NLRP3 and inhibition of efferocytosis in osteoclast-mediated diabetic osteoporosis. Faseb J. 2019;33(11):12515-12527. [61] CHEN L, CHENG S, SUN K, et al. Changes in macrophage and inflammatory cytokine expressions during fracture healing in an ovariectomized mice model. BMC Musculoskelet Disord. 2021;22(1):494. |
| [1] | Dang Yi, Du Chengyan, Yao Honglin, Yuan Nenghua, Cao Jin, Xiong Shan, Zhang Dingmei, Wang Xin. Hormonal osteonecrosis and oxidative stress [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1469-1476. |
| [2] | Liu Xiaolin, Mu Xinyue, Ma Ziyu, Liu Shutai, Wang Wenlong, Han Xiaoqian, Dong Zhiheng. Effect of hydrogel-loaded simvastatin microspheres on osteoblast proliferation and differentiation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 998-1003. |
| [3] | Liu Wentao, Feng Xingchao, Yang Yi, Bai Shengbin. Effect of M2 macrophage-derived exosomes on osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 840-845. |
| [4] | Qiao Luhui, Ma Ziyu, Guo Haoyu, Hou Yudong. Comparison of puerarin and icariin on the biological properties of mouse preosteoblasts [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 872-877. |
| [5] | Liu Guanjuan, Song Na, Huo Hua, Luo Shanshan, Cheng Yuting, Xiong Yue, Hong Wei, Liao Jian. Zoledronic acid inhibits lipopolysaccharide-induced osteoclast differentiation by regulating NLRP3 signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(29): 4677-4683. |
| [6] | Shen Mengran, Ren Yansong, Zhou Yu, Yue Debo, Ma Jinhui, Wang Bailiang. Interleukin-33-mediated bone immunity [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(29): 4723-4728. |
| [7] | Wei Zongbo, Su Yunyu, Zhang Xiaoyun, Huang Wei, Xu Hang, Liu Rongfa. Role and mechanism by which long non-coding RNAs regulate subchondral bone homeostasis in knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(29): 4736-4744. |
| [8] | Jiang Dajun, Jiang Wanwei, Zhou Ying, Tian Yong, Yang Guohui. The role of NLRC4 inflammasome-mediated autophagy in a mouse model of sepsis-induced myocardial dysfunction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(23): 3667-3673. |
| [9] | Cao Jin, Wang Ansu, Huang Nijiao, Wu Fujun, Chen Ping, Li Chengmei, Wang Xin. Role and mechanism of polyphosphate in bone tissue regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(21): 3375-3381. |
| [10] | Wang Yanyang, Xu Pu. hFOB1.19 application in bone tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(20): 3266-3272. |
| [11] | Mei Jie, He Qiang, Sun Xin, Yin Hong, Qian Weiqing. Icariin promotes osteoblast proliferation and differentiation through a non-nuclear signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(20): 3129-3135. |
| [12] | Duan Jiahao, Tan Xuyi, Lu Min, Kuang Gaoyan, Fang Chuanlong, Xiao Man. Effects of Sanhua Jiegu San on Wnt/beta-catenin signaling pathway in osteoblasts [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(20): 3230-3235. |
| [13] | Wu Yongli, Li Long, Liu Junwei, Liu Di, Wang Duo. Warm-needling moxibusion inhibits NLRP3 inflammasome activation and improves cartilage injury in a rabbit model of knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(20): 3202-3208. |
| [14] | Yuan Shuyue, Liu Chunyan, Liu Bing, Zhao Fei. Macrophage polarization and periodontitis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(17): 2699-2707. |
| [15] | Huang Haoran, Wei Yangwenxiang, Zhang Jiahao, Mo Liang, Liu Yuhao, Chen Zhenqiu, Wang Haibin, Zhou Chi. Piezo1-mediated mechanical stress stimulation in anti-osteoporosis treatment [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(17): 2716-2722. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||