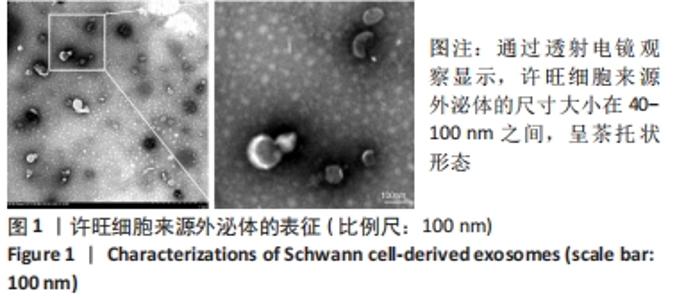
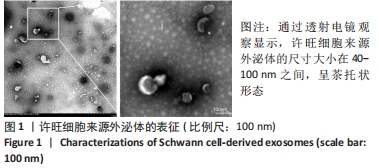
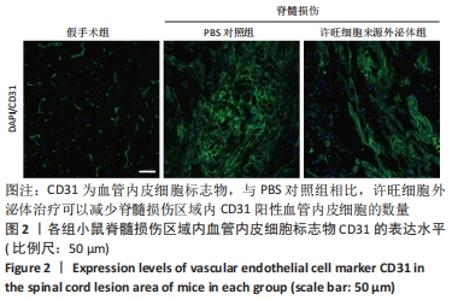
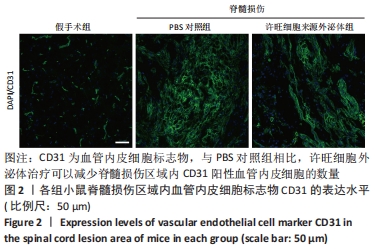
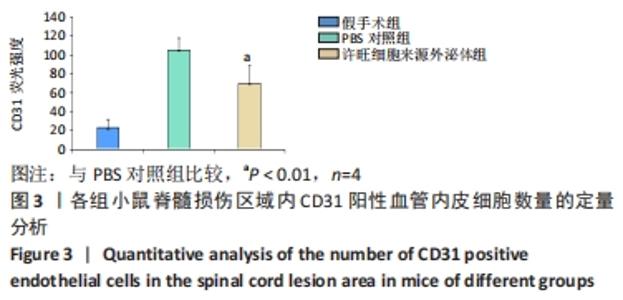
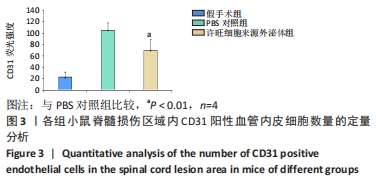
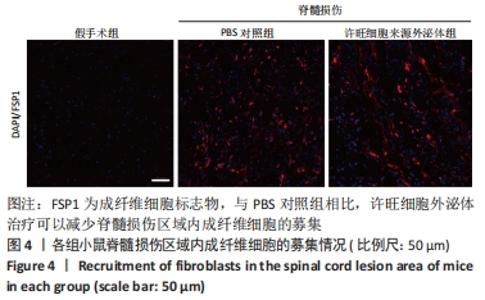
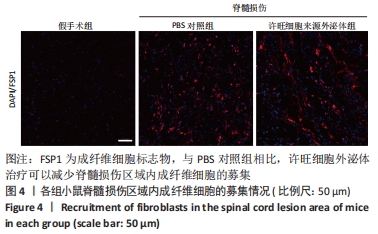
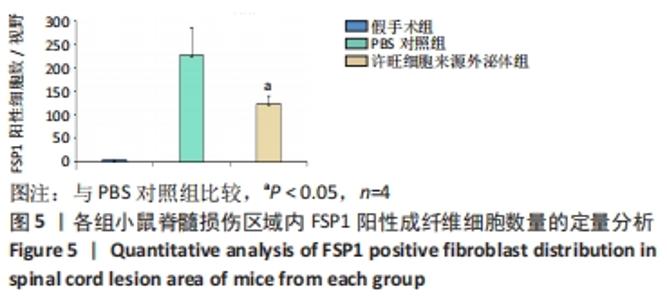
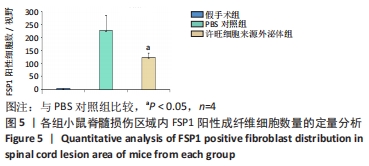
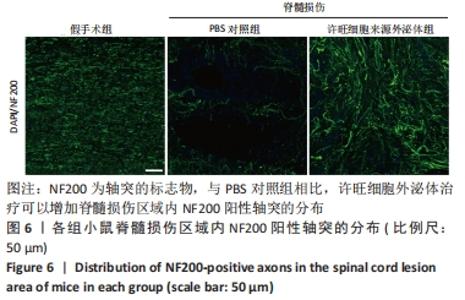
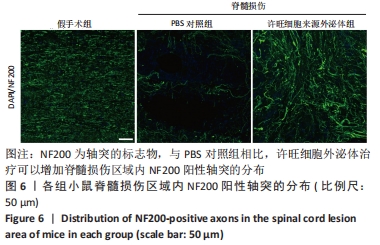
Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (10): 1567-1571.doi: 10.12307/2023.363
Previous Articles Next Articles
Schwann cell-derived exosomes attenuate angiogenesis and fibrotic scar formation and promote nerve repair
Li Xialin1, Hu Guangxun1, Pan Dayu2
- 1Department of Spinal Surgery, Union Shenzhen Hospital, Huazhong University of Science and Technology, Shenzhen 518052, Guangdong Province, China; 2Department of Orthopedics, General Hospital, Tianjin Medical University, Tianjin 300052, China
-
Received:2022-01-22Accepted:2022-06-23Online:2023-04-08Published:2022-09-08 -
Contact:Pan Dayu, Doctoral candidate, Department of Orthopedics, General Hospital, Tianjin Medical University, Tianjin 300052, China -
About author:Li Xialin, MD, Associate chief physician, Department of Spinal Surgery, Union Shenzhen Hospital, Huazhong University of Science and Technology, Shenzhen 518052, Guangdong Province, China
CLC Number:
Cite this article
Li Xialin, Hu Guangxun, Pan Dayu. Schwann cell-derived exosomes attenuate angiogenesis and fibrotic scar formation and promote nerve repair[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(10): 1567-1571.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
| [1] HOLMES D. Spinal-cord injury: spurring regrowth. Nature. 2017;552 (7684):S49. [2] AHUJA CS, WILSON JR, NORI S, et al. Traumatic spinal cord injury. Nat Rev Dis Primers. 2017;3:17018. [3] LOANE DJ, FADEN AI. Neuroprotection for traumatic brain injury: translational challenges and emerging therapeutic strategies. Trends Pharmacol Sci. 2010;31(12):596-604. [4] DORRIER CE, JONES HE, PINTARIĆ L, et al. Emerging roles for CNS fibroblasts in health, injury and disease. Nat Rev Neurosci. 2022;23(1): 23-34. [5] BRESLIN K, AGRAWAL D. The use of methylprednisolone in acute spinal cord injury: a review of the evidence, controversies, and recommendations. Pediatr Emerg Care. 2012;28(11):1238-1245; quiz 1246-1248. [6] HURLBERT RJ. Methylprednisolone for the treatment of acute spinal cord injury: point. Neurosurgery. 2014;61 Suppl 1:32-35. [7] GONCALVES MB, MALMQVIST T, CLARKE E, et al. Neuronal RARβ Signaling Modulates PTEN Activity Directly in Neurons and via Exosome Transfer in Astrocytes to Prevent Glial Scar Formation and Induce Spinal Cord Regeneration. J Neurosci. 2015;35(47):15731-15745. [8] GONCALVES MB, WU Y, CLARKE E, et al. Regulation of Myelination by Exosome Associated Retinoic Acid Release from NG2-Positive Cells. J Neurosci. 2019;39(16):3013-3027. [9] GONCALVES MB, WU Y, TRIGO D, et al. Retinoic acid synthesis by NG2 expressing cells promotes a permissive environment for axonal outgrowth. Neurobiol Dis. 2018;111:70-79. [10] PAN D, LI Y, YANG F, et al. Increasing toll-like receptor 2 on astrocytes induced by Schwann cell-derived exosomes promotes recovery by inhibiting CSPGs deposition after spinal cord injury. J Neuroinflammation. 2021;18(1):172. [11] PAN D, ZHU S, ZHANG W, et al. Autophagy induced by Schwann cell-derived exosomes promotes recovery after spinal cord injury in rats. Biotechnol Lett. 2022;44(1):129-142. [12] WEBBER C, ZOCHODNE D. The nerve regenerative microenvironment: early behavior and partnership of axons and Schwann cells. Exp Neurol. 2010;223(1):51-59. [13] AHUJA CS, SCHROEDER GD, VACCARO AR, et al. Spinal Cord Injury-What Are the Controversies? J Orthop Trauma. 2017;31 Suppl 4:S7-S13. [14] DE RIVERO VACCARI JP, DIETRICH WD, KEANE RW. Therapeutics targeting the inflammasome after central nervous system injury. Transl Res. 2016;167(1):35-45. [15] GAO ZS, ZHANG CJ, XIA N, et al. Berberine-loaded M2 macrophage-derived exosomes for spinal cord injury therapy. Acta Biomater. 2021; 126:211-223. [16] KIM GU, SUNG SE, KANG KK, et al. Therapeutic Potential of Mesenchymal Stem Cells (MSCs) and MSC-Derived Extracellular Vesicles for the Treatment of Spinal Cord Injury. Int J Mol Sci. 2021;22(24):13672. [17] CARUSO BAVISOTTO C, SCALIA F, MARINO GAMMAZZA A, et al. Extracellular Vesicle-Mediated Cell⁻Cell Communication in the Nervous System: Focus on Neurological Diseases. Int J Mol Sci. 2019;20(2):434. [18] CIREGIA F, URBANI A, PALMISANO G. Extracellular Vesicles in Brain Tumors and Neurodegenerative Diseases. Front Mol Neurosci. 2017;10:276. [19] HOLM MM, KAISER J, SCHWAB ME. Extracellular Vesicles: Multimodal Envoys in Neural Maintenance and Repair. Trends Neurosci. 2018;41(6): 360-372. [20] SAEEDI S, ISRAEL S, NAGY C, et al. The emerging role of exosomes in mental disorders. Transl Psychiatry. 2019;9(1):122. [21] YATES AG, ANTHONY DC, RUITENBERG MJ, et al. Systemic Immune Response to Traumatic CNS Injuries-Are Extracellular Vesicles the Missing Link? Front Immunol. 2019;10:2723. [22] DUTTA D, KHAN N, WU J, et al. Extracellular Vesicles as an Emerging Frontier in Spinal Cord Injury Pathobiology and Therapy. Trends Neurosci. 2021;44(6):492-506. [23] ZHANG B, YEO RW, TAN KH, et al. Focus on Extracellular Vesicles: Therapeutic Potential of Stem Cell-Derived Extracellular Vesicles. Int J Mol Sci. 2016;17(2):174. [24] ZHOU Y, WEN LL, LI YF, et al. Exosomes derived from bone marrow mesenchymal stem cells protect the injured spinal cord by inhibiting pericyte pyroptosis. Neural Regen Res. 2022;17(1):194-202. [25] LOPEZ-VERRILLI MA, COURT FA. Transfer of vesicles from schwann cells to axons: a novel mechanism of communication in the peripheral nervous system. Front Physiol. 2012;3:205. [26] SERINI G, BUSSOLINO F. Common cues in vascular and axon guidance. Physiology (Bethesda). 2004;19:348-354. [27] ADAMS RH, EICHMANN A. Axon guidance molecules in vascular patterning. Cold Spring Harb Perspect Biol. 2010;2(5):a001875. [28] HIMMELS P, PAREDES I, ADLER H, et al. Motor neurons control blood vessel patterning in the developing spinal cord. Nat Commun. 2017;8: 14583. [29] SILVA NA, SOUSA N, REIS RL, et al. From basics to clinical: a comprehensive review on spinal cord injury. Prog Neurobiol. 2014;114:25-57. [30] TRAN AP, WARREN PM, SILVER J. The Biology of Regeneration Failure and Success After Spinal Cord Injury. Physiol Rev. 2018;98(2):881-917. [31] CARMELIET P. Mechanisms of angiogenesis and arteriogenesis. Nat Med. 2000;6(4):389-395. [32] CASELLA GT, MARCILLO A, BUNGE MB, et al. New vascular tissue rapidly replaces neural parenchyma and vessels destroyed by a contusion injury to the rat spinal cord. Exp Neurol. 2002;173(1):63-76. [33] FASSBENDER JM, WHITTEMORE SR, HAGG T. Targeting microvasculature for neuroprotection after SCI. Neurotherapeutics. 2011;8(2):240-251. [34] LOSEY P, YOUNG C, KRIMHOLTZ E, et al. The role of hemorrhage following spinal-cord injury. Brain Res. 2014;1569:9-18. [35] LOY DN, CRAWFORD CH, DARNALL JB, et al. Temporal progression of angiogenesis and basal lamina deposition after contusive spinal cord injury in the adult rat. J Comp Neurol. 2002;445(4):308-324. [36] NG MT, STAMMERS AT, KWON BK. Vascular disruption and the role of angiogenic proteins after spinal cord injury. Transl Stroke Res. 2011; 2(4):474-491. |
| [1] | Nong Fuxiang, Jiang Zhixiong, Li Yinghao, Xu Wencong, Shi Zhilan, Luo Hui, Zhang Qinglang, Zhong Shuang, Tang Meiwen. Bone cement augmented proximal femoral nail antirotation for type A3.3 intertrochanteric femoral fracturalysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(在线): 1-10. |
| [2] | Pan Zhongjie, Qin Zhihong, Zheng Tiejun, Ding Xiaofei, Liao Shijie. Targeting of non-coding RNAs in the pathogenesis of the osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1441-1447. |
| [3] | Yang Jiujie, Li Zhi, Wang Shujie, Tian Ye, Zhao Wei. Intraoperative neurophysiological monitoring of functional changes following durotomy with decompression for acute spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1232-1236. |
| [4] | Xu Yan, Li Ping, Lai Chunhua, Zhu Peijun, Yang Shuo, Xu Shulan. Piezoelectric materials for vascularized bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1126-1132. |
| [5] | Liu Wentao, Feng Xingchao, Yang Yi, Bai Shengbin. Effect of M2 macrophage-derived exosomes on osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 840-845. |
| [6] | Li Qicheng, Deng Jin, Fu Xiaoyang, Han Na. Effects of bone marrow mesenchymal stem cells-derived exosomes on hypoxia-treated myoblasts [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 853-859. |
| [7] | Wang Min, Yin Xiushan, Wang Yingxi, Zhang Yan, Zhao Long, Xia Shuyue. Inhalation of bone marrow mesenchymal stem cells-derived exosomes alleviates inflammatory injury in chronic obstructive pulmonary disease [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 827-834. |
| [8] | Zhang Houjun, Deng Bowen, Jiang Shengyuan, Zhao Yi, Ren Jingpei, Xu Lin, Mu Xiaohong. Proteomic analysis of cerebrospinal fluid exosomes derived from cerebral palsy children [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 903-908. |
| [9] | Gao Ting, Ma Xiaohong, Li Xiaorong. Extraction and identification of exosomes from three different sources of ovarian granulosa cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 860-865. |
| [10] | Hao Liufang, Duan Hongmei, Wang Zijue, Hao Fei, Hao Peng, Zhao Wen, Gao Yudan, Yang Zhaoyang, Li Xiaoguang. Spatiotemporal dynamic changes of ependymal cells after spinal cord injury in transgenic mice [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 883-889. |
| [11] | Li Xiaoyin, Yang Xiaoqing, Chen Shulian, Li Zhengchao, Wang Ziqi, Song Zhen, Zhu Daren, Chen Xuyi. Collagen/silk fibroin scaffold combined with neural stem cells in the treatment of traumatic spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 890-896. |
| [12] | Zhang Qijian, Xu Ximing. Acquisition and application of ectodermal mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 928-934. |
| [13] | Yuan Bo, Xie Lide, Fu Xiumei. Schwann cell-derived exosomes promote the repair and regeneration of injured peripheral nerves [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 935-940. |
| [14] | Xu Qijing, Yang Yichun, Lei Wei, Yang Ying, Yu Jiang, Xia Tingting, Zhang Meng, Zhang Tao, Zhang Qian. Advances and problems in cell-free treatment of diabetic skin chronic wounds [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 962-969. |
| [15] | Chen Guanting, Zhang Linqi, Li Qingru. Meta-analysis of the value of exosomal miRNA for the diagnosis of chronic kidney disease [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 970-976. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||