Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (13): 1993-1999.doi: 10.12307/2022.323
Previous Articles Next Articles
Mechanism of separation of graft-versus-host disease and graft versus leukemia in unrelated cord blood transplantation for hematological malignancies
Xu Anhui, Lin Xiuxiu, Zhang Xuhan, Song Kaidi, Sun Guangyu, Tang Baolin, Sun Zimin, Zheng Changcheng
- Department of Hematology, First Affiliated Hospital of University of Science and Technology of China, Hefei 230001, Anhui Province, China
-
Received:2021-01-13Revised:2021-01-16Accepted:2021-03-06Online:2022-05-08Published:2021-12-18 -
Contact:Zheng Changcheng, MD, Professor, Chief physician, Doctoral supervisor, Department of Hematology, First Affiliated Hospital of University of Science and Technology of China, Hefei 230001, Anhui Province, China Sun Zimin, Professor, Chief physician, Doctoral supervisor, Department of Hematology, First Affiliated Hospital of University of Science and Technology of China, Hefei 230001, Anhui Province, China -
About author:Xu Anhui, Master candidate, Department of Hematology, First Affiliated Hospital of University of Science and Technology of China, Hefei 230001, Anhui Province, China -
Supported by:the Fundamental Research Funds for the Central Universities of China, No. WK9110000003 (to ZCC)
CLC Number:
Cite this article
Xu Anhui, Lin Xiuxiu, Zhang Xuhan, Song Kaidi, Sun Guangyu, Tang Baolin, Sun Zimin, Zheng Changcheng. Mechanism of separation of graft-versus-host disease and graft versus leukemia in unrelated cord blood transplantation for hematological malignancies[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(13): 1993-1999.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
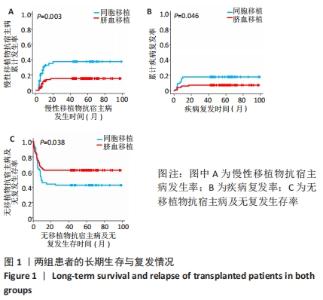
2.1 非血缘脐血移植具有明显的慢性移植物抗宿主病与移植物抗白血病效应分离现象 自2012-07-01/2017-06-31,共有154例成人血液肿瘤患者(年龄≥18岁)接受了造血干细胞移植治疗,其中非血缘脐血移植93例,同胞外周血干细胞移植61例。经过中位61个月(42-99个月)的长期随访,非血缘脐血移植组5年慢性移植物抗宿主病发生率为15.6%(95%CI:7.0-23.4),明显低于同胞外周血干细胞移植组37.6%(95%CI:22.4-49.9)(P=0.003),见图1A;非血缘脐血移植组5年广泛型慢性移植物抗宿主病发生率为7.6%(95%CI:1.5-13.3),明显低于同胞外周血干细胞移植组33.9%(95%CI:19.2-46.0)(P < 0.001)。非血缘脐血移植组5年移植后疾病复发率为7.5%(95%CI:3.3-14.1),明显低于同胞外周血干细胞移植组18.0%(95%CI:9.6-38.7)(P=0.046),见图1B。非血缘脐血移植组5年总生存率为71%(95%CI:60.6-79.1),同胞外周血干细胞移植组为63.9%(95%CI:50.6-74.6)(P=0.37);非血缘脐血移植组5年无病生存率为69.9%(95%CI:59.5-78.1),同胞外周血干细胞移植组为60.7%(95%CI:47.3-71.6)(P=0.28)。整合Ⅲ-Ⅳ度移植物抗宿主病、广泛性慢性移植物抗宿主病以及疾病复发、5年无复发生存(无移植物抗宿主病无疾病复发生存),非血缘脐血移植组为62.4% (95%CI:51.7-71.3),明显高于同胞外周血干细胞移植组42.6%(95%CI:30.1-54.5)(P=0.038),见图1C。 "
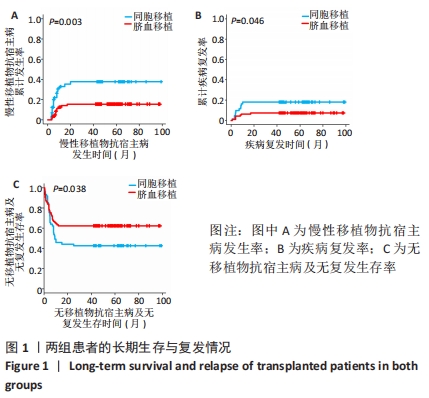
2.2 非血缘脐血移植患者T细胞及其亚群的分化 临床资料提示脐血移植具有较强的移植物抗白血病效应,为了进一步探讨脐血移植后T细胞及其亚群在移植物抗白血病效应中的作用,该研究收集脐血移植后1年内患者的骨髓血标本(n=14),采用流式细胞术进一步分析脐血移植后免疫细胞分化情况,见图2A。分析比较非血缘脐血移植患者和健康供者的CD3+/CD4+/CD8+T细胞占CD45+细胞的比例,发现非血缘脐血移植患者的CD45+CD3+T细胞比例与正常对照组相似(65.92% vs. 67.79%,P=0.86),见图2B,CD45+CD4+T细胞比例与正常对照组无明显差异(25.87% vs. 33.62%,P=0.28),见图2C,而CD45+CD8+T细胞的比例高于正常对照组(43.97% vs. 29.77%,P=0.05),见图2D。非血缘脐血移植患者CD45+CD4+T细胞群的比例(25.87%)明显低于CD45+CD8+T细胞群(43.97%)(P=0.004),见图2E,而健康供者CD45+CD4+T细胞群比例(33.62%)与CD45+CD8+T细胞群(29.77%)相似(P=0.37),见图2F。"

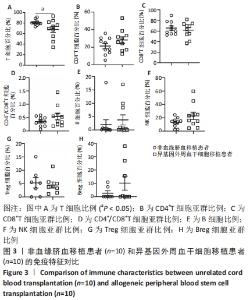
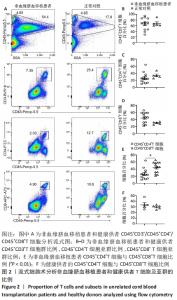
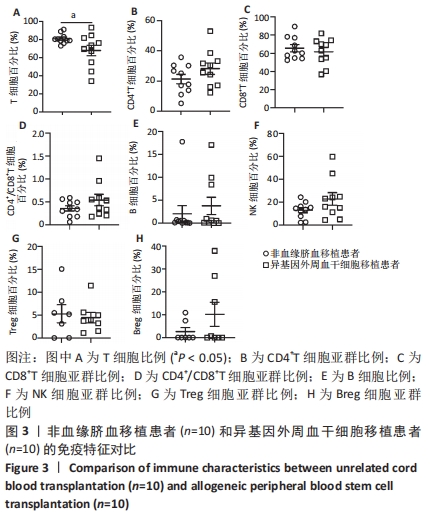
2.3 非血缘脐血移植和外周血干细胞移植后免疫细胞群的比较 检测了10例非血缘脐血移植和10例同胞异基因外周血干细胞移植患者的免疫细胞亚群分化情况,见图3。非血缘脐血移植组CD3+T细胞为81.03%,明显高于外周血干细胞移植组67.97%,差异有显著性意义(P=0.04),见图3A。移植后CD3+CD4+T细胞亚群比例:非血缘脐血移植组为21.33%,低于外周血干细胞移植组28.28%,见图3B;移植后CD3+CD8+细胞亚群比例:非血缘脐血移植组为65.60%,高于外周血干细胞移植组61.70%,见图3C;移植后CD4+/CD8+两个细胞亚群之比:非血缘脐血移植组为0.36,低于外周血干细胞移植组0.54,见图3D。尽管统计学差异不明显(可能与检测病例数较少有关),但是在非血缘脐血移植组以CD8+T细胞占主导趋势。 移植后CD19+B细胞比例,在非血缘脐血移植组为2.02%,外周血干细胞移植组为3.76%(P=0.51),见图3E。移植后CD56+NK细胞比例,在非血缘脐血移植组为12.86%,稍低于外周血干细胞移植组22.79%(P=0.11),见图3F;移植后Treg细胞亚群比例,在非血缘脐血移植组为5.29%,外周血干细胞移植组为4.45%(P=0.71),见图3G;移植后Breg细胞亚群比例,在非血缘脐血移植组为2.61%,稍低于外周血干细胞移植组10.16%(P=0.23),见图3H。 "
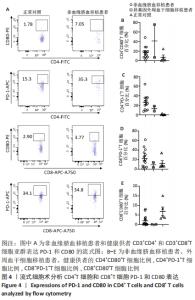
2.4 非血缘脐血移植和外周血干细胞移植后T细胞PD-1和CD80表达水平变化 CD80和PD-1是T细胞表面的两种重要的激活信号和抑制信号分子,继续进一步检测移植后CD4+T细胞和CD8+T细胞亚群的CD80和PD-1分子表达,见图4A。非血缘脐血移植组CD4+CD80+T细胞为17.08%,低于外周血干细胞移植组41.36%(P=0.089),见图4B,且非血缘脐血移植组CD4+PD-1+T细胞为25.76%,高于外周血干细胞移植组13.03%,见图4C,非血缘脐血移植组CD8+PD-1+T细胞为22.28%,高于外周血干细胞移植组9.01%(P=0.35),见图4D;非血缘脐血移植组CD8+CD80+T细胞为1.90%,高于外周血干细胞移植组0.05%,见图4E。与健康对照组相比,非血缘脐血移植后CD4+T细胞和CD8+T细胞表达PD-1和CD80的水平差异均显著性意义。"

| [1] ADACHI Y, UKAI S, SAGOU K, et al. Promising Outcome of Umbilical Cord Blood Transplantation in Patients with Multiple Comorbidities. Biol Blood Marrow Transplant. 2018;24(7):1455-1462. [2] THANGAVELU G, DU J, PAZ KG, et al. Inhibition of inositol kinase B controls acute and chronic graft-versus-host disease. Blood. 2020; 135(1):28-40. [3] ALYEA EP, DEANGELO DJ, MOLDREM J, et al. NCI First International Workshop on The Biology, Prevention and Treatment of Relapse after Allogeneic Hematopoietic Cell Transplantation: report from the committee on prevention of relapse following allogeneic cell transplantation for hematologic malignancies. Biol Blood Marrow Transplant. 2010;16(8):1037-1069. [4] CHOI J, COOPER ML, STASER K, et al. Baricitinib-induced blockade of interferon gamma receptor and interleukin-6 receptor for the prevention and treatment of graft-versus-host disease. Leukemia. 2018; 32(11):2483-2494. [5] LI D, LI X, LIAO L, et al. Unrelated cord blood transplantation versus haploidentical transplantation in adult and pediatric patients with hematological malignancies-A meta-analysis and systematic review. Am J Blood Res. 2020;10(1):1-10. [6] CASSADY K, MARTIN PJ, ZENG D. Regulation of GVHD and GVL Activity via PD-L1 Interaction With PD-1 and CD80. Front Immunol. 2018;9: 3061. [7] DEKKER L, DE KONING C, LINDEMANS C, et al. Reconstitution of T Cell Subsets Following Allogeneic Hematopoietic Cell Transplantation. Cancers (Basel). 2020;12(7):1974. [8] TAKAMI A. Hematopoietic stem cell transplantation for acute myeloid leukemia. Int J Hematol. 2018;107(5):513-518. [9] GRAGERT L, EAPEN M, WILLIAMS E, et al. HLA match likelihoods for hematopoietic stem-cell grafts in the U.S. registry. N Engl J Med. 2014; 371(4):339-348. [10] KANAKRY CG, FUCHS EJ, LUZNIK L. Modern approaches to HLA-haploidentical blood or marrow transplantation. Nat Rev Clin Oncol. 2016;13(2):132. [11] LIU JH, KANAKRY CG, LUZNIK L. Have haploidentical transplants replaced umbilical cord transplants for acute leukemias? Curr Opin Hematol. 2018;25(2):103-111. [12] BASHEY A, ZHANG X, JACKSON K, et al. Comparison of Outcomes of Hematopoietic Cell Transplants from T-Replete Haploidentical Donors Using Post-Transplantation Cyclophosphamide with 10 of 10 HLA-A, -B, -C, -DRB1, and -DQB1 Allele-Matched Unrelated Donors and HLA-Identical Sibling Donors: A Multivariable Analysis Including Disease Risk Index. Biol Blood Marrow Transplant. 2016;22(1):125-133. [13] LUZNIK L, FUCHS EJ. High-dose, post-transplantation cyclophosphamide to promote graft-host tolerance after allogeneic hematopoietic stem cell transplantation. Immunol Res. 2010;47(1-3):65-77. [14] WU R, MA L. Haploidentical Hematopoietic Stem Cell Transplantation Versus Umbilical Cord Blood Transplantation in Hematologic Malignancies: A Systematic Review and Meta-Analysis. Cell Transplant. 2020;29:963689720964771. [15] BASHEY A, ZHANG MJ, MCCURDY SR, et al. Mobilized Peripheral Blood Stem Cells Versus Unstimulated Bone Marrow As a Graft Source for T-Cell-Replete Haploidentical Donor Transplantation Using Post-Transplant Cyclophosphamide. J Clin Oncol. 2017;35(26):3002-3009. [16] RUGGERI A, LABOPIN M, BACIGALUPO A, et al. Bone marrow versus mobilized peripheral blood stem cells in haploidentical transplants using posttransplantation cyclophosphamide. Cancer. 2018;124(7): 1428-1437. [17] CIUREA SO, AL MALKI MM, KONGTIM P, et al. The European Society for Blood and Marrow Transplantation (EBMT) consensus recommendations for donor selection in haploidentical hematopoietic cell transplantation. Bone Marrow Transplant. 2020;55(1):12-24. [18] GUPTA AO, WAGNER JE. Umbilical Cord Blood Transplants: Current Status and Evolving Therapies. Front Pediatr. 2020;8:570282. [19] HWANG WY, SAMUEL M, TAN D, et al. A meta-analysis of unrelated donor umbilical cord blood transplantation versus unrelated donor bone marrow transplantation in adult and pediatric patients. Biol Blood Marrow Transplant. 2007;13(4):444-453. [20] LIU H, RICH ES, GODLEY L, et al. Reduced-intensity conditioning with combined haploidentical and cord blood transplantation results in rapid engraftment, low GVHD, and durable remissions. Blood. 2011;118(24): 6438-6445. [21] GLUCKMAN E, RUGGERI A, ROCHA V, et al. Family-directed umbilical cord blood banking. Haematologica. 2011;96(11):1700-1707. [22] PEFFAULT DE LATOUR R, BRUNSTEIN CG, PORCHER R, et al. Similar overall survival using sibling, unrelated donor, and cord blood grafts after reduced-intensity conditioning for older patients with acute myelogenous leukemia. Biol Blood Marrow Transplant. 2013;19(9): 1355-1360. [23] LIU HL, SUN ZM, GENG LQ, et al. Similar survival, but better quality of life after myeloablative transplantation using unrelated cord blood vs matched sibling donors in adults with hematologic malignancies. Bone Marrow Transplant. 2014;49(8):1063-1069. [24] TAKAHASHI S, OOI J, TOMONARI A, et al. Comparative single-institute analysis of cord blood transplantation from unrelated donors with bone marrow or peripheral blood stem-cell transplants from related donors in adult patients with hematologic malignancies after myeloablative conditioning regimen. Blood. 2007;109(3):1322-1330. [25] JACOBSON CA, TURKI AT, MCDONOUGH SM, et al. Immune reconstitution after double umbilical cord blood stem cell transplantation: comparison with unrelated peripheral blood stem cell transplantation. Biol Blood Marrow Transplant. 2012;18(4):565-574. [26] SCHOEMANS H, THEUNISSEN K, MAERTENS J, et al. Adult umbilical cord blood transplantation: a comprehensive review. Bone Marrow Transplant. 2006;38(2):83-93. [27] MILANO F, EMERSON RO, SALIT R, et al. Impact of T Cell Repertoire Diversity on Mortality Following Cord Blood Transplantation. Front Oncol. 2020;10:583349. [28] BHATT ST, BEDNARSKI JJ. Immune Reconstitution in Pediatric Patients Following Hematopoietic Cell Transplant for Non-malignant Disorders. Front Immunol. 2020;11:1988. [29] HIWARKAR P, QASIM W, RICCIARDELLI I, et al. Cord blood T cells mediate enhanced antitumor effects compared with adult peripheral blood T cells. Blood. 2015;126(26):2882-2891. [30] MILANO F, GOOLEY T, WOOD B, et al. Cord-Blood Transplantation in Patients with Minimal Residual Disease. N Engl J Med. 2016;375(10): 944-953. [31] TONG J, XUAN L, SUN Y, et al. Umbilical Cord Blood Transplantation without Antithymocyte Globulin Results in Similar Survival but Better Quality of Life Compared with Unrelated Peripheral Blood Stem Cell Transplantation for the Treatment of Acute Leukemia-A Retrospective Study in China. Biol Blood Marrow Transplant. 2017;23(9):1541-1548. [32] 郑昌成,朱小玉,汤宝林,等.非血缘脐血移植与HLA相合同胞外周血干细胞移植治疗成人恶性血液病的对比研究[J].中华血液学杂志,2017,38(8):673-679. [33] POLITIKOS I, BOUSSIOTIS VA. The role of the thymus in T-cell immune reconstitution after umbilical cord blood transplantation. Blood. 2014; 124(22):3201-3211. [34] ZHENG CC, ZHU XY, TANG BL, et al. Clinical separation of cGvHD and GvL and better GvHD-free/relapse-free survival (GRFS) after unrelated cord blood transplantation for AML. Bone Marrow Transplant. 2017; 52(1):88-94. [35] ZEISER R, BLAZAR BR. Acute Graft-versus-Host Disease - Biologic Process, Prevention, and Therapy. N Engl J Med. 2017;377(22):2167-2179. [36] HOLTAN SG, DEFOR TE, LAZARYAN A, et al. Composite end point of graft-versus-host disease-free, relapse-free survival after allogeneic hematopoietic cell transplantation. Blood. 2015;125(8):1333-1338. [37] LAUGHLIN MJ, EAPEN M, RUBINSTEIN P, et al. Outcomes after transplantation of cord blood or bone marrow from unrelated donors in adults with leukemia. N Engl J Med. 2004;351(22):2265-2275. [38] PARK BG, PARK CJ, JANG S, et al. Reconstitution of lymphocyte subpopulations after hematopoietic stem cell transplantation: comparison of hematologic malignancies and donor types in event-free patients. Leuk Res. 2015;39(12):1334-1341. [39] WALLER EK, LOGAN BR, FEI M, et al. Kinetics of immune cell reconstitution predict survival in allogeneic bone marrow and G-CSF-mobilized stem cell transplantation. Blood Adv. 2019;3(15):2250-2263. [40] TIAN DM, WANG Y, ZHANG XH, et al. Rapid Recovery of CD3+CD8+ T Cells on Day 90 Predicts Superior Survival after Unmanipulated Haploidentical Blood and Marrow Transplantation. PLoS One. 2016; 11(6):e0156777. [41] MINCULESCU L, MARQUART HV, RYDER LP, et al. Improved Overall Survival, Relapse-Free-Survival, and Less Graft-vs.-Host-Disease in Patients With High Immune Reconstitution of TCR Gamma Delta Cells 2 Months After Allogeneic Stem Cell Transplantation. Front Immunol. 2019;10:1997. [42] HIWARKAR P, ADAMS S, GILMOUR K, et al. Cord blood CD8+ T-cell expansion following granulocyte transfusions eradicates refractory leukemia. Blood Adv. 2020;4(17):4165-4174. [43] NI X, SONG Q, CASSADY K, et al. PD-L1 interacts with CD80 to regulate graft-versus-leukemia activity of donor CD8+ T cells. J Clin Invest. 2017; 127(5):1960-1977. |
| [1] | Xiang Xinjian, Liu Fang, Wu Liangliang, Jia Daping, Tao Yue, Zhao Zhengnan, Zhao Yu. High-dose vitamin C promotes the survival of autologous fat transplantation in rats [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1242-1246. |
| [2] | An Weizheng, He Xiao, Ren Shuai, Liu Jianyu. Potential of muscle-derived stem cells in peripheral nerve regeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1130-1136. |
| [3] | Xuan Juanjuan, Bai Hongtai, Zhang Jixiang, Wang Yaoquan, Chen Guoyong, Wei Sidong. Role of regulatory T cell subsets in liver transplantation and progress in clinical application [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1143-1148. |
| [4] | Zhou Ying, Zhang Huan, Liao Song, Hu Fanqi, Yi Jing, Liu Yubin, Jin Jide. Immunomodulatory effects of deferoxamine and interferon gamma on human dental pulp stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1012-1019. |
| [5] | Cui Xing, Sun Xiaoqi, Zheng Wei, Ma Dexin. Huangqin Decoction regulates autophagy to intervene with intestinal acute graft-versus-host disease in mice [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1057-1062. |
| [6] | Fang Xiaolei, Leng Jun, Zhang Chen, Liu Huimin, Guo Wen. Systematic evaluation of different therapeutic effects of mesenchymal stem cell transplantation in the treatment of ischemic stroke [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1085-1092. |
| [7] | Yang Zhiwei, Liu Junchang, Gao Xiaolin, Jiang Taimao. Relationship between tacrolimus metabolic rate and early BK virus infection after kidney transplantation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 712-716. |
| [8] | Chen Jinmin, Chen Suisheng, Ding Jing, Xia Baoquan, Luo Xiaojia, Lu Chenghai. Stability of balloon dilation with injectable calcium sulfate cement for tibial plateau fractures [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 414-418. |
| [9] | Min Keting, Zhang Yiguo, Yang Hao, Lü Xin. Effect of mesenchymal stem cells on negative regulation of immune response of myeloid-derived suppressor cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(19): 3084-3089. |
| [10] | Zhang Jixiang, Yan Hongxian, Xuan Juanjuan, Bai Hongtai, Wang Yaoquan, Wei Sidong, Chen Guoyong. Rapid establishment of rat liver transplantation model by portal vein preferential reverse anastomosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(17): 2696-2701. |
| [11] | Zhao Jiling, Peng Yi, Peng Zhiyong, Yu Guolong. Effects of human umbilical cord blood mesenchymal stem cells secreting tumor necrosis factor alpha stimulating gene-6 protein on conversion of mouse bone marrow-derived macrophage subtypes [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(13): 2012-2019. |
| [12] | Zheng Youfei, Shi Wentao, Liu Xiaogu, Zhuang Qin, Lü Demin, Zhang Jiayin, Yuan Yiwen, Zhang Zhijian, Xu Xiaofeng. Biocompatibility of plant-derived nerve conduits to nasal ectomesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(13): 2040-2044. |
| [13] | Sun Jianwei, Yang Xinming, An Xiaogang. Effects of various methods on improving bone marrow mesenchymal stem cell transplantation for spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(13): 2075-2080. |
| [14] | Yao Yanyi, Chen Xiaoling, Zhang Min, Wang Hong, Hao Liying, Shi Chao, Zhao Bingfeng, Jin Yaqiao, Dong Wei. miR-210/YWHAG axis with adipocyte proliferation and angiogenesis after autologous fat transplantation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(1): 59-63. |
| [15] | Li Shanshan, Guo Xiaoxiao, You Ran, Yang Xiufen, Zhao Lu, Chen Xi, Wang Yanling. Photoreceptor cell replacement therapy for retinal degeneration diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1116-1121. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

