中国组织工程研究 ›› 2026, Vol. 30 ›› Issue (28): 7494-7504.doi: 10.12307/2026.831
• 组织构建循证医学 evidence-based medicine in tissue construction • 上一篇
神经调控技术促进脑卒中后上肢运动功能的系统评价与网状Meta分析
范萌萌,丁嘉莉,万宇杰,黄海量
- 山东中医药大学康复医学院,山东省济南市 250355
-
收稿日期:2025-10-29修回日期:2025-12-29出版日期:2026-10-08发布日期:2026-02-27 -
通讯作者:黄海量,博士,教授,山东中医药大学康复医学院,山东省济南市 250355 -
作者简介:范萌萌,女,2000年生,山东省青岛市人,汉族,山东中医药大学在读硕士。 -
基金资助:山东省名老中医药专家刘昭纯传承工作室建设项目(鲁卫中发展字〔2018〕1号),项目负责人:黄海量
A systematic review and network meta-analysis of neuromodulation techniques for promoting upper limb motor function after stroke
Fan Mengmeng, Ding Jiali, Wan Yujie, Huang Hailiang
- Rehabilitation Medicine School of Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China
-
Received:2025-10-29Revised:2025-12-29Online:2026-10-08Published:2026-02-27 -
Contact:Huang Hailiang, MD, Professor, Rehabilitation Medicine School of Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China -
About author:Fan Mengmeng, MS candidate, Rehabilitation Medicine School of Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China -
Supported by:Construction Project of Liu Zhaochun Inheritance Studio for Famous Traditional Chinese Medicine in Shandong Province, No. [2018]1 (to HHL)
摘要:
文题释义:
神经调控技术:通过非侵入性或微创方式作用于中枢神经系统,调节皮质兴奋性及脑网络活动,从而促进神经可塑性与功能恢复的康复干预方法。
脑卒中:由脑部血液循环障碍引起的急性脑功能损伤,包括缺血性和出血性脑卒中,常导致不同程度的运动、感觉及认知功能障碍,是致残率和复发率极高的神经系统疾病。
目的:系统比较多种神经调控技术对脑卒中患者上肢运动功能恢复的疗效与安全性,并通过网状Meta分析对不同干预措施的相对优势进行排序,为临床康复干预提供循证依据。
方法:系统检索中国知网、万方数据库、维普数据库、中国生物医学文献数据库、PubMed、EMbase、Web of Science、Cochrane Library数据库,纳入关于不同神经调控技术治疗脑卒中后上肢运动障碍的随机对照试验,检索时限为各数据库建库至2025年8月公开发表的中英文文献。对照组采用假刺激以及传统康复手段,试验组为在对照组基础上加入不同的神经调控技术。采用Cochrane随机对照试验偏倚风险评价工具对纳入文献进行质量评价。采用Stata 16.0和RevMan 5.4软件进行网状Meta分析。
结果:纳入51项随机对照试验,涉及12种神经调控刺激方式。网状Meta分析结果显示:与常规治疗相比,高频重复经颅磁刺激(MD=11.50,95%CI:6.83-16.16,P < 0.05)在改善脑卒中患者上肢基础运动功能恢复方面的疗效最佳;在改善脑卒中患者上肢功能的实用性与精细性方面,连续性节律爆发刺激(MD=12.10,95%CI:44.99-19.21,P < 0.05;MD=9.60,95%CI:1.32-17.88,P < 0.05)的疗效最佳;在改善脑卒中患者日常生活活动能力受限或伴有明显痉挛方面,阴极经颅直流电刺激(MD=15.40,95%CI:0.03-30.77,P < 0.05;MD=-0.83,95%CI:-1.64至-0.03,P < 0.05)的疗效最佳。
结论:在以促进上肢基础运动功能恢复为目标时,高频重复经颅磁刺激疗效最好;在提升上肢功能的实用性与精细性方面,连续性节律爆发刺激疗效最好;对于提高日常生活能力伴有明显痉挛的患者,阴极经颅直流电刺激疗效最好。
https://orcid.org/0009-0004-0479-0182(范萌萌)
中国组织工程研究杂志出版内容重点:干细胞;骨髓干细胞;造血干细胞;脂肪干细胞;肿瘤干细胞;胚胎干细胞;脐带脐血干细胞;干细胞诱导;干细胞分化;组织工程
中图分类号:
引用本文
范萌萌, 丁嘉莉, 万宇杰, 黄海量. 神经调控技术促进脑卒中后上肢运动功能的系统评价与网状Meta分析[J]. 中国组织工程研究, 2026, 30(28): 7494-7504.
Fan Mengmeng, Ding Jiali, Wan Yujie, Huang Hailiang. A systematic review and network meta-analysis of neuromodulation techniques for promoting upper limb motor function after stroke[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(28): 7494-7504.
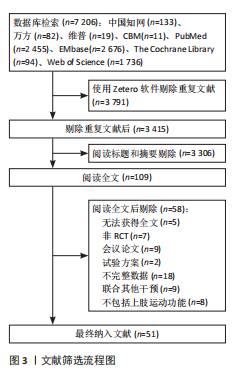
2.2 纳入文献的基本信息 共纳入51篇文献,涉及2 614例脑卒中患者,其中对照组1 180例,试验组1 434例。其中共纳入12种神经调控技术,包括脑机接口7篇[23-29],taVNS 3篇[30-32],低频重复经颅磁刺激(Low-Frequency Repetitive Transcranial Magnetic Stimulation,LF-rTMS) 16篇[33-48],高频+低频重复经颅磁刺激(High-Frequency + Low-Frequency Repetitive Transcranial Magnetic Stimulation, HF+LF-rTMS) 3篇[35,42,49],高频重复经颅磁刺激(High-Frequency Repetitive Transcranial Magnetic
Stimulation,HF-rTMS) 11篇[34-39,49-53],连续性节律爆发刺激(Continuous Theta-Burst Stimulation,cTBS) 3篇[47,54-55],间歇性节律爆发刺激(Intermittent Theta-Burst Stimulation,iTBS ) 4篇[33,55-57],双侧节律爆发刺激(Bilateral Theta-
Burst Stimulation,Bilateral-TBS) 1篇[58],阴极经颅直流电刺激(Cathodal Transcranial Direct Current Stimulation,Cathodal-tDCS)4篇[59-62],阳极经颅直流电刺激(Anodal Transcranial Direct Current Stimulation,Anodal-tDCS )6篇[59-60,63-66],
双侧经颅直流电刺激(Bilateral Transcranial Direct Current Stimulation,Bilateral-tDCS )6篇[67-72],高分辨率经颅直流电刺激(High-Definition Transcranial Direct Current Stimulation,HD-tDCS) 2篇[63,73]。文献基本信息见附表1。
2.3 文献质量评价 在纳入的51项研究中均报道采用随机分组[23-73],但其中有12项未说明具体的实施方法为不明确风险[28,31,34,38,42-43,46-47,53,57-58,67]。共有24项研究明确采取了不透明信封、加密邮件或储物柜等方式进行分配隐藏为低风险[23-27,33,35,37,44,50,52,54-55,58-62,65-66,69-71,73],其余研究未见相关描述。共有45项试验的研究人员或受试者在分组分配上实施盲法[24,26,30-49,51-73],在47项研究中,结果测量者实施盲法[23-27,29-35,37-44,46-48,50-73]。所纳入的研究数据均完整,没有选择性报告结果或其他偏倚风险。对纳入研究的偏倚风险评估见图4,5。
2.4 Meta分析结果
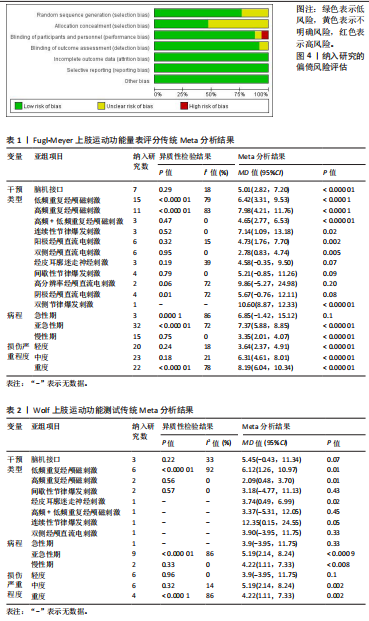
2.4.1 Fugl-Meyer上肢运动功能评定 纳入的50篇研究结局指标涉及2 502例脑卒中患者[23-39,41-73],其中试验组1 376例,对照组1 126例。异质性检验结果提示研究间差异较大(I2=73%,P < 0.000 01),还因纳入研究中神经调控技术类型差异显著,且患者病程跨度大,采用随机效应模型进行分析。合并效应量显示,神经调控干预在改善患者上肢运动功能方面较常规治疗具有显著优势(MD=6.22,95%CI:4.88-7.54,P < 0.000 01)。为探究异质性来源,依据干预类型、病程、损伤严重程度进行亚组分析,部分亚组的异质性显著降低,提示可能是异质性的重要影响因素。传统Meta分析结果显示干预措施方面脑机接口、低频重复经颅磁刺激、高频重复经颅磁刺激、高频+低频重复经颅磁刺激、连续性节律爆发刺激、阳极经颅直流电刺激、双侧经颅直流电刺激及双侧节律爆发刺激在提升评分改善患者上肢运动功能方面均显著优于常规康复治疗;病程方面,亚急性期与慢性期评分均优于对照组,亚急性期效果最佳;损伤严重程度方面,各程度评分高于对照组,重度损伤患者治疗效果最佳,见表1。
2.4.2 Wolf上肢运动功能测试 纳入的12篇研究结局指标涉及Wolf上肢运动功能测试[23,27-28,32-33,35-36,40,45,48,55,70]。其中试验组526例,对照组415例。异质性检验结果提示研究间差异较大(I2=83%,P < 0.000 01),采用随机效应模型进行分析。合并效应量显示,神经调控干预在改善患者上肢运动功能方面较常规治疗具有显著优势(MD=5.15,95%CI:2.52-7.78,P=0.000 1)。为探究异质性来源,依据干预类型、病程、损伤严重程度进行亚组分析,部分亚组的异质性显著降低,提示以上可能是异质性的重要影响因素。传统Meta分析结果显示低频重复经颅磁刺激与高频重复经颅磁刺激在提升Wolf上肢运动功能测试评分方面均显著优于常规康复治疗;病程方面,亚急性期与慢性期评分均优于对照组,亚急性期效果最佳;损伤严重程度方面,中度与重度损伤患者评分高于对照组,中度损伤患者治疗效果最佳,见表2。
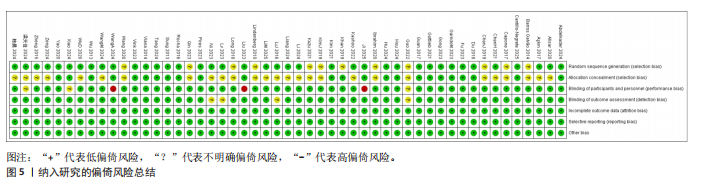
2.4.3 上肢动作研究量表 纳入的12篇研究结局指标涉及764例脑卒中患者[23-25,30。54,56-57,62-64,71-72],均采用上肢动作研究量表进行上肢运动功能评定。其中试验组394例,对照组370例。异质性检验结果提示研究间差异小(I2=0%,P=0.98),采用固定效应模型进行分析。合并效应量显示,神经调控干预在改善患者上肢运动功能方面较常规治疗具有显著优势(MD=5.98,95%CI:3.81-8.15,P < 0.000 01)。
尽管总体异质性较低,此次研究仍进行了亚组分析,以进一步探索不同干预方式、病程、损伤严重程度下的效果差异。传统Meta分析结果显示阳极经颅直流电刺激在提升上肢动作研究量表评分改善患者上肢运动功能方面均显著优于常规康复治疗;病程、损伤严重程度方面,亚急性期与重度损伤患者治疗效果最佳,见表3。
2.4.4 改良Barthel指数 纳入的18篇研究结局指标涉及改良Barthel指数[25,27,29-30,34,39-40,46,50-52,54-55,58,61-63,72]。其中试验组543例,对照组454例。异质性检验结果提示研究间差异较大(I2=76%,P < 0.000 01),采用随机效应模型进行分析。合并效应量显示,神经调控干预在改善患者上肢运动功能方面较常规治疗具有显著优势(MD=10.25,95%CI:7.26-13.25,P=0.000 1)。为探究异质性来源,依据干预类型进行亚组分析,显示异质性仍较高,因此仅对结果进行描述性分析。传统Meta分析结果显示脑机接口、低频重复经颅磁刺激、高频重复经颅磁刺激及阴极经颅直流电刺激在提升改良Barthel指数评分方面均显著优于常规康复治疗,病程、损伤严重程度方面,亚急性期与重度损伤患者治疗效果最佳,见表4。
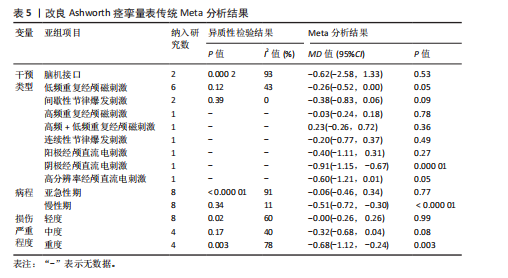
2.4.5 改良Ashworth痉挛量表 纳入的13篇研究结局指标涉及改良Ashworth痉挛量表[23,28,35,41,43-44,46-47,56-57,61,66,73]。其中试验组365例,对照组317例。异质性检验结果提示研究间差异较大(I2=83%,P < 0.000 01),采用随机效应模型进行分析。合并效应量显示,神经调控干预在改善患者上肢运动功能方面较常规治疗具有显著优势(MD=-0.31,95%CI:-0.57至-0.04,P=0.02)。为探究异质性来源,依据干预类型进行亚组分析,部分亚组的异质性显著降低,提示干预类型差异可能是异质性的重要影响因素,但传统Meta分析结果显示各单项技术未见显著优势,病程、损伤严重程度方面,亚急性期与重度损伤患者治疗效果最佳,见表5。
2.5 网状Meta分析结果
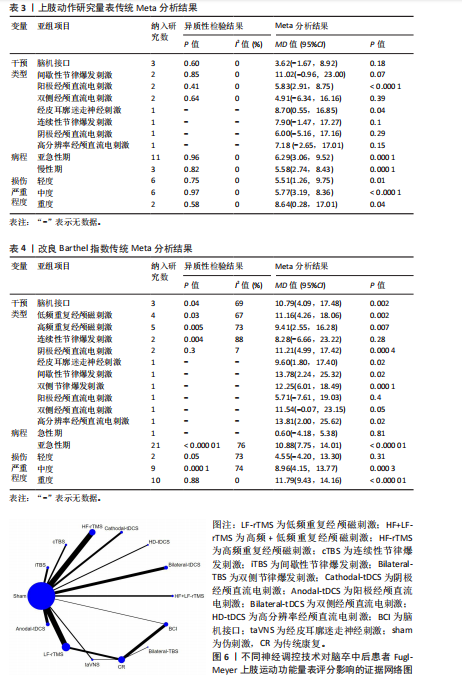
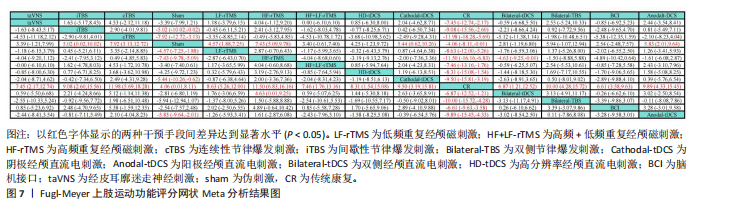
2.5.1 Fugl-Meyer上肢运动功能评定 该结局指标共纳入50项研究[23-39,41-73],涉及12种神经调控技术,包括脑机接口、低频重复经颅磁刺激、高频重复经颅磁刺激、高频+低频重复经颅磁刺激、连续性节律爆发刺激、间歇性节律爆发刺激、双侧节律爆发刺激、阳极经颅直流电刺激、阴极经颅直流电刺激、双侧经颅直流电刺激、高分辨率经颅直流电刺激、经皮耳廓迷走神经刺激。其上肢运动功能评定证据网络,见图6。在网络一致性检验中,节点分析结果显示P=0.904,提示模型整体一致性较为理想。局部一致性通过节点劈裂法进行检验,发现各比较P值均> 0.05,表明未见显著局部不一致性,直接与间接证据保持较高一致性,故采用一致性模型完成后续分析。网状Meta分析结果显示,脑机接口、低频重复经颅磁刺激、高频重复经颅磁刺激、高频+低频重复经颅磁刺激、连续性节律爆发刺激、间歇性节律爆发刺激、双侧节律爆发刺激、阳极经颅直流电刺激、阴极经颅直流电刺激、双侧经颅直流电刺激、高分辨率经颅直流电刺激、经皮耳廓迷走神经刺激对上肢运动功能的改善效果显著优于传统疗法。12种神经调控技术之间,高频重复经颅磁刺激对上肢运动功能的改善效果显著优于双侧经颅直流电刺激,而其他神经调控技术之间对上肢运动功能的改善效果两两比较差异均无显著性意义(P > 0.05),见图7。针对12种干预方式对上肢运动障碍的改善效果进行比较排序,其最优概率依次为:高频重复经颅磁刺激(85.1%) > 连续性节律爆发刺激(84.1%) > 阳极经颅直流电刺激(67.7%) > 双侧节律爆发刺激(66.0%) > 阴极经颅直流电刺激(63.7%) > 间歇性节律爆发刺激(58.6%) > 低频重复经颅磁刺激(54.5%) > 高分辨率经颅直流电刺激(51.3%) >
高频+低频重复经颅磁刺激(43.0%) > 经皮耳廓迷走神经刺激(42.5%) > 双侧经颅直流电刺激(36.8%) > 脑机接口(34.4%),见图8。
2.5.2 Wolf上肢运动功能测试 该结局指标共纳入12项研究[23,27-28,32-33,35-36,40,45,48,55,70],涉及8种神经调控技术,包括脑机接口、低频重复经颅磁刺激、高频重复经颅磁刺激、高频+低频重复经颅磁刺激、连续性节律爆发刺激、间歇性节律爆发刺激、双侧经颅直流电刺激、经皮耳廓迷走神经刺激。其评定证据网络,见图9。在网络一致性检验中,节点分析结果显示P=0.933,提示模型整体一致性较为理想。局部一致性通过节点劈裂法进行检验,发现各比较P值均> 0.05,表明未见显著局部不一致
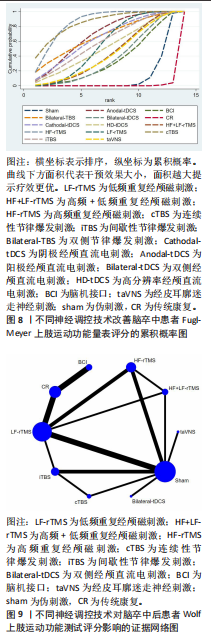
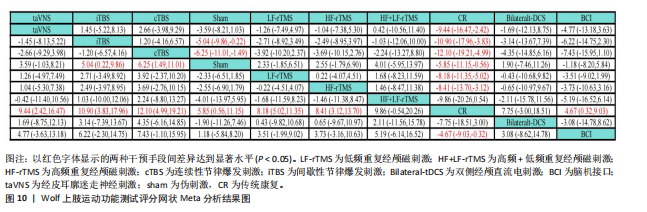
性,直接与间接证据保持较高一致性,故采用一致性模型完成后续分析。网状Meta分析结果显示,脑机接口、低频重复经颅磁刺激、高频重复经颅磁刺激、连续性节律爆发刺激、间歇性节律爆发刺激、经皮耳廓迷走神经刺激对上肢运动功能的改善效果显著优于传统疗法。8种神经调控技术之间对上肢运动功能的改善效果两两比较差异均无显著性意义(P > 0.05),见图10。针对8种干预方式对上肢运动障碍的改善效果进行比较排序,其最优概率依次为:连续性节律爆发刺激(84.6%) > 间歇性节律爆发刺激(75.4%) > 高频+低频重复经颅磁刺激(63.9%) > 经皮耳廓迷走神经刺激(63.8%) > 高频重复经颅磁刺激(54.2%) > 低频重复经颅磁刺激(52.8%) > 双侧经颅直流电刺激(49.2%) > 脑机接口(26.3%),见图11。
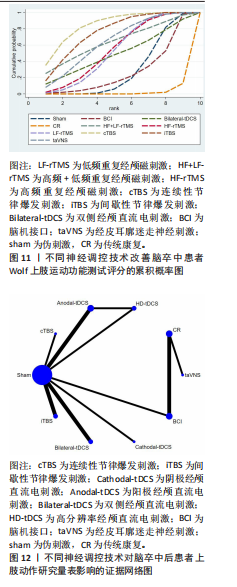
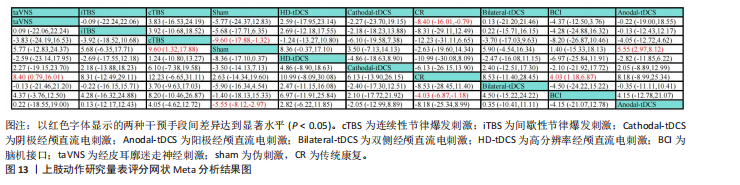
2.5.3 上肢动作研究量表 该结局指标共纳入12项研究[23-25,30,54,56-57,62-64,71-72],涉及8种神经调控技术,包括脑机接口、连续性节律爆发刺激、间歇性节律爆发刺激、阳极经颅直流电刺激、阴极经颅直流电刺激、双侧经颅直流电刺激、高分辨率经颅直流电刺激、经皮耳廓迷走神经刺激。其上肢运动功能恢复情况证据网络,见图12。在上肢动作研究量表的网络一致性检验中,节点分析结果显示P=0.552,提示模型整体一致性较为理想。局部一致性通过节点劈裂法进行检验,发现各比较P值均大于0.05,表明未见显著局部不一致性,直接与间接证据保持较高一致性,故采用一致性模型完成后续分析。网状Meta分析结果显示,脑机接口、经皮耳廓迷走神经刺激对上肢运动功能恢复效果显著优于传统疗法。阳极经颅直流电刺激、连续性节律爆发刺激对上肢运动功能的改善效果显著优于伪刺激组。8种神经调控技术之间对上肢运动功能的改善效果两两比较差异均无显著性意义(P > 0.05),见图13。针对8种干预方式对上肢运动障碍的改善效果进行比较排序,其最优概率依次为:连续性节律爆发刺激(77.5%) > 高分辨率经颅直流电刺激(71.0%) > 经皮耳廓迷走神经刺激(60.4%) > 双侧经颅直流电刺激(57.1%) > 阳极经颅直流电刺激(56.2%)=间歇性节律爆发刺激(56.2%) > 阴极经颅直流电刺激(43.9%) > 脑机接口(39.5%),见图14。
2.5.4 改良Barthel指数 该结局指标共纳入18项研究[25,27,29-30,34,39-40,46,50-52,54-55,58,61-63,72],
涉及11种神经调控技术,包括脑机接口、低
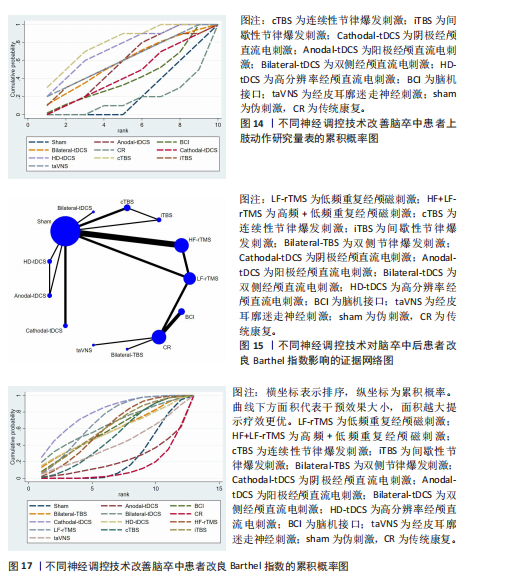
频重复经颅磁刺激、高频重复经颅磁刺激、连续性节律爆发刺激、间歇性节律爆发刺激、双侧节律爆发刺激、阳极经颅直流电刺激、阴极经颅直流电刺激、双侧经颅直流电刺激、高分辨率经颅直流电刺激、经皮耳廓迷走神经刺激。其日常生活活动证据网络,见图15。在改良Barthel指数的网络一致性检验中,节点分析结果显示P=0.491,提示模型整体一致性较为理想。局部一致性通过节点劈裂法进行检验,发现各比较P值均> 0.05,表明未见显著局部不一致性,直接与间接证据保持较高一致性,故采用一致性模型完成后续分析。网状Meta分析结果显示,脑机接口、低频重复经颅磁刺激、阴极经颅直流电刺激对日常生活活动改善效果显著优于传统疗法。11种神经调控技术之间对上肢运动功能的改善效果两两比较差异均无显著性意义(P > 0.05),见图16。针对12种干预方式对上肢运动障碍的改善效果进行比较排序,其最优概率依次为:阴极经颅直流电刺激(78.8%) > 低频重复经颅磁刺激(68.8%) > 双侧经颅直流电刺激(64.1%) > 间歇性节律爆发刺激(60.0%) > 高频重复经颅磁刺激(59.5%) > 脑机接口(58.7%) > 双侧节律爆发刺激(56.5%)=高分辨率经颅直流电刺激(56.5%) > 连续性节律爆发刺激(49.4%) > 经皮耳廓迷走神经刺激(41.1%) > 阳极经颅直流电刺激(21.0%),见图17。
2.5.5 改良Ashworth痉挛量表 该结局指标共纳入13项研究[23,28,35,41,43-44,46-47,56-57,61,66,73],涉及9种神经调控技术,包括脑机接口、低频重复经颅磁刺激、高频重复经颅磁刺激、高频+低频重复经颅磁刺激、连续性节律爆发刺激、间歇性节律爆发刺激、阳极经颅直流电刺激、阴极经颅直流电刺激、高分辨率经颅直流电刺激。其改良Ashworth痉挛量表证据网络,见图18。在网络一致性检验中,节点分析结果显示
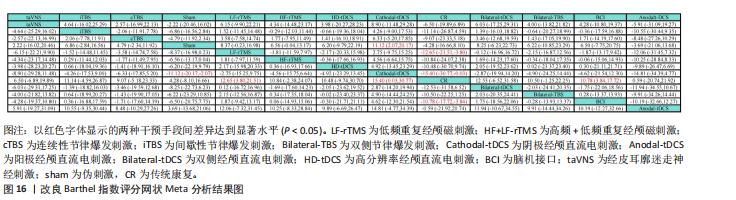
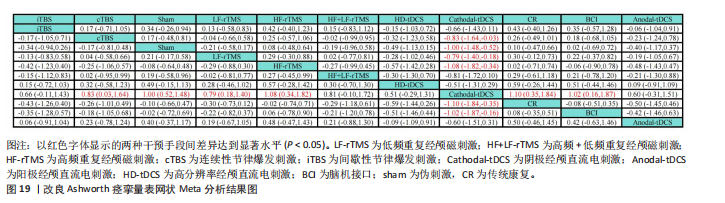
P=0.657,提示模型整体一致性较为理想。局部一致性通过节点劈裂法进行检验,发现各比较P值均 > 0.05,表明未见显著局部不一致性,直接与间接证据保持较高一致性,故采用一致性模型完成后续分析。网状Meta分析结果显示,阴极经颅直流电刺激对上肢运动功能的改善效果显著优于传统疗法与假刺激。9种神经调控技术之间,阴极经颅直流电刺激对上肢运动功能的改善效果显著优于连续性节律爆发刺激、低频重复经颅磁刺激、高频重复经颅磁刺激、脑机接口,而其他神经调控技术之间对上肢痉挛的改善效果两两比较差异均无显著性意义(P > 0.05),见图19。针对9种干预方式对上肢运动障碍的改善效果进行比较排序,其最优概率依次为:阴极经颅直流电刺激(96.7%) > 高分辨率经颅直流电刺激(772.1%) > 阳极经颅直流电刺激(63.6%) > 间歇性节律爆发刺激(61.3%) > 低频重复经颅磁刺激(53.7%) > 高频+低频重复经颅磁刺激(48.9%) > 连续性节律爆发刺激(47.0%) > 脑机接口(31.5%) > 高频重复经颅磁刺激(24.8%),见图20。
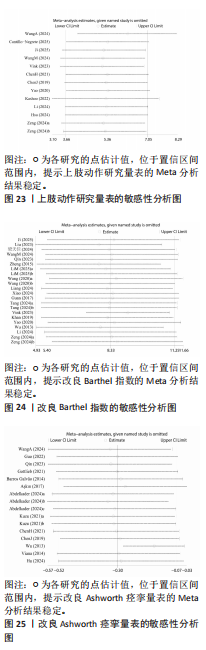
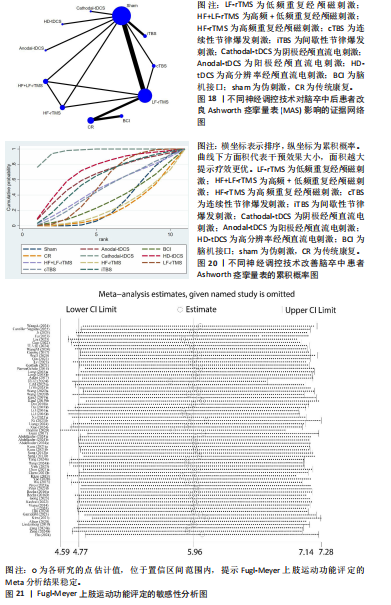
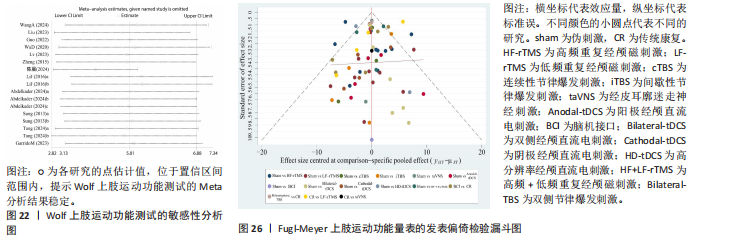
2.5.6 敏感性分析结果 对 Fugl-Meyer上肢运动功能评定、Wolf上肢运动功能测试、上肢动作研究量表、改良Barthel指数和改良Ashworth痉挛量表进行了敏感性分析。采用逐一排除单项研究的方法,评估剔除后的异质性变化。结果显示,剔除任一研究均未对5个结局指标的异质性产生显著影响,提示分析结果稳健,见图21-25。
2.6 发表偏倚结果 鉴于次要结局研究数量不足以支撑可靠的统计学检验,此次研究仅对主要结局指标 Fugl-Meyer上肢运动功能评定进行了发表偏倚分析。Begg’s检验(P=0.941)和 Egger’s检验(P=0.789)结果均未提示显著差异,漏斗图亦呈基本对称分布,表明该结局指标的发表偏倚风险较低,结果较为稳健,见图26。
2.7 不良反应 共有10篇文献报道了相关不良事件[23,32,36-37,44-55,62,64,70-71]。干预过程中患者主要表现为皮肤发红、患侧手部疼痛、麻木、短暂性头痛、疲劳、瘙痒及轻度刺痛等症状,但均在治疗结束后迅速缓解,提示整体安全性较高。

| [1] CAMPBELL BCV, KHATRI P. Stroke. The Lancet. 2020; 396(10244):129-142. [2] GBD 2016 Stroke Collaborators.Global, regional, and national burden of stroke, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2019;18(5):439-458. [3] O’FLAHERTY D, ALI K. Recommendations for Upper Limb Motor Recovery: An Overview of the UK and European Rehabilitation after Stroke Guidelines (2023). Healthcare (Basel). 2024;12(14):1433. [4] KHAN MA, FARES H, GHAYVAT H, et al. A systematic review on functional electrical stimulation based rehabilitation systems for upper limb post-stroke recovery. Front Neurol. 2023;14:1272992. [5] PSYCHOULI P, MAMAIS I, ANASTASIOU C. An Exploration of the Effectiveness of Different Intensity Protocols of Modified Constraint-Induced Therapy in Stroke: A Systematic Review. Rehabil Res Pract. 2023;2023:6636987. [6] 赵强, 周跃辉, 董泓, 等. 本体感觉神经肌肉促进技术的基础理论、方法及应用[J]. 中国组织工程研究,2026,30(17):4407-4416. [7] 魏达, 马超, 彭玉涛, 等. 神经调控技术在脑卒中康复中的应用进展[J]. 中国现代神经疾病杂志, 2025,25(1):84-91. [8] TAKEUCHI N, IZUMI SI.Noninvasive Brain Stimulation for Motor Recovery after Stroke: Mechanisms and Future Views. Stroke Res Treat. 2012:2012:584727. [9] DAN B. Neuroscience underlying rehabilitation: what is neuroplasticity?. Dev Med Child Neurol. 2019;61(11): 1240-1240. [10] HUANG XL, WU MY, WU CC, et al. Neuromodulation techniques in poststroke motor impairment recovery: Efficacy, challenges, and future directions. Tzu Chi Med J. 2024;36(2):136-141. [11] MA ZZ, WU J J, CAO Z, et al. Motor imagery-based brain–computer interface rehabilitation programs enhance upper extremity performance and cortical activation in stroke patients. J Neuroeng Rehabil. 2024;21(1): 91. [12] ZHANG J, XING Y, DU W, et al. Analysis of the effect of combined rehabilitation training and transcutaneous vagus nerve electrical stimulation on promoting central nervous system remodeling in stroke patients.Brain Res. 2025;1851:149460. [13] SENADHEERA I, HETTIARACHCHI P, HASLAM B, et al. AI Applications in Adult Stroke Recovery and Rehabilitation: A Scoping Review Using AI. Sensors (Basel). 2024;24(20):6585. [14] VINK JJT, VAN LIESHOUT E CC, OTTE WM, et al. Continuous Theta-Burst Stimulation of the Contralesional Primary Motor Cortex for Promotion of Upper Limb Recovery After Stroke: A Randomized Controlled Trial. Stroke. 2023;54(8):1962-1971. [15] AHMED I, MUSTAFAOGLU R, BENKHALIFA N, et al. Does noninvasive brain stimulation combined with other therapies improve upper extremity motor impairment, functional performance, and participation in activities of daily living after stroke? A systematic review and meta-analysis of randomized controlled trial. Top Stroke Rehabil. 2023;30(3):213-234. [16] CHEN S, ZHANG S, YANG W, et al.The effectiveness of intermittent theta burst stimulation for upper limb motor recovery after stroke: a systematic review and meta-analysis of randomized controlled trials. Front Neurosci. 2023;17:1272003. [17] 王海桥, 鲍春龄, 李鹤, 等. 针刺联合运动想象对脑卒中软瘫上肢精细动作的影响[J]. 中国针灸, 2015,35(6):534-538. [18] MASIERO S, CARRARO E. Upper limb movements and cerebral plasticity in post-stroke rehabilitation. Aging Clin Exp Res. 2008;20(2):103-108. [19] YU P, DONG R, WANG X, et al. NeuroImage. Clinical. 2024;43:103636. [20] STERNE JAC, SAVOVIĆ J, PAGE MJ, et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ (Clinical research ed.). 2019;366:l4898. [21] WOUDA N C, KNIJFF B, PUNT M, et al. Predicting Recovery of Independent Walking After Stroke: A Systematic Review. Am J Phys Med Rehabil. 2024; 103(5):458-464. [22] ROESNER K, BRODOWSKI H, STRUTZ N. Measuring severe stroke: a scoping review of RCTs. Front Neurol. 2025;16:1631275. [23] WANG A, TIAN X, JIANG D, et al. Rehabilitation with brain-computer interface and upper limb motor function in ischemic stroke: A randomized controlled trial. Med. 2024;5(6):559-569.e4. [24] CANTILLO-NEGRETE J, RODRÍGUEZ-GARCÍA ME, CARRILLO-MORA P, et al. The ReHand-BCI trial: a randomized controlled trial of a brain-computer interface for upper extremity stroke neurorehabilitation. Front Neurosci. 2025;19:1579988. [25] JI X, LU X, XU Y, et al. Effects and neural mechanisms of a brain-computer interface-controlled soft robotic glove on upper limb function in patients with subacute stroke: a randomized controlled fNIRS study.J Neuroeng Rehabil. 2025;22(1): 171. [26] FU J, CHEN S, SHU X, et al. Functional-oriented, portable brain–computer interface training for hand motor recovery after stroke: a randomized controlled study. Front Neurosci. 2023;17:1146146. [27] LIU X, ZHANG W, LI W, et al. Effects of motor imagery based brain-computer interface on upper limb function and attention in stroke patients with hemiplegia: a randomized controlled trial. BMC Neurol. 2023;23(1):136. [28] GUO N, WANG X, DUANMU D, et al. SSVEP-Based Brain Computer Interface Controlled Soft Robotic Glove for Post-Stroke Hand Function Rehabilitation. IEEE Trans Neural Syst Rehabil Eng. 2022;30:1737‐1744. [29] 梁天佳, 龙耀斌, 陆丽燕, 等. 绳带辅助本体感觉神经肌肉促进技术训练联合绳带辅助脑机接口训练对脑卒中偏瘫上肢康复效果的随机对照试验[J]. 中国康复理论与实践,2024,30(8):972-978. [30] WANG MH, WANG YX, XIE M, et al.Transcutaneous auricular vagus nerve stimulation with task-oriented training improves upper extremity function in patients with subacute stroke: a randomized clinical trial. Front Neurosci. 2024;18:1346634. [31] CAPONE F, MICCINILLI S, PELLEGRINO G, et al.Transcutaneous Vagus Nerve Stimulation Combined with Robotic Rehabilitation Improves Upper Limb Function after Stroke. Neural Plast. 2017;2017: 7876507. [32] WU D, MA J, ZHANG L, et al. Effect and Safety of Transcutaneous Auricular Vagus Nerve Stimulation on Recovery of Upper Limb Motor Function in Subacute Ischemic Stroke Patients: A Randomized Pilot Study. Neural Plast. 2020;2020:8841752. [33] SUNG WH, WANG CP, CHOU CL, et al. Efficacy of coupling inhibitory and facilitatory repetitive transcranial magnetic stimulation to enhance motor recovery in hemiplegic stroke patients. Stroke. 2013; 44(5):1375-1382. [34] WANG Q, ZHANG D, ZHAO YY, et al. Effects of high-frequency repetitive transcranial magnetic stimulation over the contralesional motor cortex on motor recovery in severe hemiplegic stroke: A randomized clinical trial. Brain Stimul. 2020;13(4):979-986. [35] ABDELKADER AA, AFIFI LM, MAHER EA, et al. Comparison of Bilateral Versus Unilateral 5 Hz or 1 Hz Repetitive Transcranial Magnetic Stimulation in Subacute Stroke: Assessment of Motor Function in a Randomized Controlled Study. J Clin Neurophysiol. 2024;41(5):478-483. [36] LI J, MENG XM, LI RY, et al. Effects of different frequencies of repetitive transcranial magnetic stimulation on the recovery of upper limb motor dysfunction in patients with subacute cerebral infarction. Neural Regen Res. 2016;11(10):1584-1590. [37] DU J, YANG F, HU J, et al. Effects of high- and low-frequency repetitive transcranial magnetic stimulation on motor recovery in early stroke patients: Evidence from a randomized controlled trial with clinical, neurophysiological and functional imaging assessments. Neuroimage Clin. 2018;21:101620. [38] KIM JS, KIM DH, KIM HJ, et al. Effect of Repetitive Transcranial Magnetic Stimulation in Post-stroke Patients with Severe Upper-Limb Motor Impairment.Brain Neurorehabil. 2019;13(1):e3. [39] LI M, JIA F, LIU P, et al. Effects of Repetitive Transcranial Magnetic Stimulation on Upper Limb Motor Function and Serum Lipid Metabolomics in Patients With Ischemic Stroke: A Randomized Controlled Study. Brain Behav. 2025;15(5):e70558. [40] ZHENG C, LIAO W, XIA W. Effect of combined low-frequency repetitive transcranial magnetic stimulation and virtual reality training on upper limb function in subacute stroke: a double-blind randomized controlled trail.J Huazhong Univ Sci Technolog Med Sci. 2015;35(2):248-254. [41] AŞKIN A, TOSUN A, DEMIRDAL ÜS. Effects of low-frequency repetitive transcranial magnetic stimulation on upper extremity motor recovery and functional outcomes in chronic stroke patients: A randomized controlled trial. Somatosens Mot Res. 2017;34(2): 102-107. [42] LONG H, WANG H, ZHAO C, et al. Effects of combining high- and low-frequency repetitive transcranial magnetic stimulation on upper limb hemiparesis in the early phase of stroke. Restor Neurol Neurosci. 2018;36(1):21-30. [43] BARROS GALVÃO SC, BORBA COSTA DOS SANTOS R, BORBA DOS SANTOS P, et al. Efficacy of coupling repetitive transcranial magnetic stimulation and physical therapy to reduce upper-limb spasticity in patients with stroke: A randomized controlled trial. Arch Phys Med Rehabil. 2014;95(2):222-229. [44] GOTTLIEB A, BOLTZMANN M, SCHMIDT SB, et al. Treatment of upper limb spasticity with inhibitory repetitive transcranial magnetic stimulation: A randomized placebo-controlled trial. NeuroRehabilitation. 2021;49(3):425-434. [45] LV Y, ZHANG JJ, WANG K, et al. Determining the Optimal Stimulation Sessions for TMS-Induced Recovery of Upper Extremity Motor Function Post Stroke: A Randomized Controlled Trial. Brain Sci. 2023; 13(12):1662. [46] QIN Y, LIU X, ZHANG Y, et al. Effects of transcranial combined with peripheral repetitive magnetic stimulation on limb spasticity and resting-state brain activity in stroke patients. Front Hum Neurosci. 2023; 17:992424. [47] KUZU Ö, ADIGUZEL E, KESIKBURUN S, et al. The Effect of Sham Controlled Continuous Theta Burst Stimulation and Low Frequency Repetitive Transcranial Magnetic Stimulation on Upper Extremity Spasticity and Functional Recovery in Chronic Ischemic Stroke Patients.J Stroke Cerebrovasc Dis.2021; 30(7): 105795. [48] 陈晨, 孟兆祥, 杨康, 等. 智能镜像手套任务导向性训练联合低频重复经颅磁刺激对脑卒中患者手功能效果的随机对照试验[J]. 中国康复理论与实践,2024,30(7):831-838. [49] NI J, JIANG W, GONG X, et al. Effect of rTMS intervention on upper limb motor function after stroke: A study based on fNIRS. Front Aging Neurosci. 2023;14:1077218. [50] XIAO J, SUN Y, LIU ZJ, et al. Ipsilesional 5 Hz Repetitive Transcranial Magnetic Stimulation for Motor Dysfunction in Subacute Intracerebral Hemorrhage: An Exploratory Trial. Arch Rehabil Res Clin Transl. 2024;7(1):100386. [51] LIANG S, WANG W, YU F, et al. Repetitive peripheral magnetic stimulation combined with transcranial magnetic stimulation in rehabilitation of upper extremity hemiparesis following stroke: A pilot study. J Rehabil Med. 2024;56:19449. [52] GUAN YZ, LI J, ZHANG XW, et al. Effectiveness of repetitive transcranial magnetic stimulation (rTMS) after acute stroke: A one‐year longitudinal randomized trial. CNS Neurosci Ther. 2017;23(12):940. [53] IBRAHIM EM, ZAKI MA, GABR MGM. Effect of high frequency repetitive transcranial mgnetic stimulation of the contralesional dorsal premotor cortex on recovery from post-stroke severe motor impairment. Eur J Neurology. 2020;27:397-398. [54] VINK JJT, VAN LIESHOUT ECC, OTTE WM, et al. Continuous Theta-Burst Stimulation of the Contralesional Primary Motor Cortex for Promotion of Upper Limb Recovery After Stroke: A Randomized Controlled Trial. Stroke. 2023;54(8):1962-1971. [55] TANG Z, HUANG J, ZHOU Y, et al. Efficacy and Safety of High-Dose TBS on Poststroke Upper Extremity Motor Impairment: A Randomized Controlled Trial. Stroke. 2024;55(9):2212-2220. [56] CHEN YH, CHEN CL, HUANG YZ, et al. Augmented efficacy of intermittent theta burst stimulation on the virtual reality-based cycling training for upper limb function in patients with stroke: a double-blinded, randomized controlled trial. J Neuroeng Rehabil. 2021;18(1):91. [57] CHEN YJ, HUANG YZ, CHEN CY, et al. Intermittent theta burst stimulation enhances upper limb motor function in patients with chronic stroke: a pilot randomized controlled trial.BMC Neurol. 2019;19(1):69. [58] KHAN F, RATHORE C, KATE M, et al. The comparative efficacy of theta burst stimulation or functional electrical stimulation when combined with physical therapy after stroke: a randomized controlled trial.Clin Rehabil. 2019;33(4):693-703. [59] ROCHA S, SILVA E, FOERSTER Á, et al. The impact of transcranial direct current stimulation (tDCS) combined with modified constraint-induced movement therapy (mCIMT) on upper limb function in chronic stroke: a double-blind randomized controlled trial. Disabil Rehabil. 2016;38(7):653-660. [60] PIRES R, BALTAR A, SANCHEZ MP, et al. Do Higher Transcranial Direct Current Stimulation Doses Lead to Greater Gains in Upper Limb Motor Function in Post-Stroke Patients?. Int J Environ Res Public Health. 2023;20(2):1279. [61] WU D, QIAN L, ZOROWITZ RD, et al. Effects on Decreasing Upper-Limb Poststroke Muscle Tone Using Transcranial Direct Current Stimulation: A Randomized Sham-Controlled Study. Arch Phys Med Rehabil. 2013; 94(1):1-8. [62] YAO X, CUI L, WANG J, et al. Effects of transcranial direct current stimulation with virtual reality on upper limb function in patients with ischemic stroke: a randomized controlled trial. J Neuroeng Rehabil. 2020;17:73. [63] ZENG Y, CHENG R, ZHANG L, et al.Clinical Comparison between HD-tDCS and tDCS for Improving Upper Limb Motor Function: A Randomized, Double-Blinded, Sham-Controlled Trial. Neural Plast. 2024;2024: 2512796. [64] KASHOO FZ, AL-BARADIE RS, ALZAHRANI M, et al. Effect of Transcranial Direct Current Stimulation Augmented with Motor Imagery and Upper-Limb Functional Training for Upper-Limb Stroke Rehabilitation: A Prospective Randomized Controlled Trial. Int J Environ Res Public Health. 2022;19(22): 15199. [65] GONG Q, YAN R, CHEN H, et al. Effects of cerebellar transcranial direct current stimulation on rehabilitation of upper limb motor function after stroke. Front Neurol. 2023;14:1044333. [66] VIANA RT, LAURENTINO GEC, SOUZA RJP, et al. Effects of the addition of transcranial direct current stimulation to virtual reality therapy after stroke: A pilot randomized controlled trial. NeuroRehabilitation. 2014;34(3):437-446. [67] LINDENBERG R, RENGA V, ZHU LL, et al. Bihemispheric brain stimulation facilitates motor recovery in chronic stroke patients. Neurology. 2010;75(24):2176-2184. [68] ALISAR DC, OZEN S, SOZAY S. Effects of Bihemispheric Transcranial Direct Current Stimulation on Upper Extremity Function in Stroke Patients: A randomized Double-Blind Sham-Controlled Study. J Stroke Cerebrovasc Dis. 2020;29(1):04454. [69] KIM SH. Effects of Dual Transcranial Direct Current Stimulation and Modified Constraint-Induced Movement Therapy to Improve Upper-Limb Function after Stroke: A Double-Blinded, Pilot Randomized Controlled Trial. J Stroke Cerebrovasc Dis. 2021;30(9): 105928. [70] GARRIDO MM, ÁLVAREZ EE, ACEVEDO PF, et al. Early transcranial direct current stimulation with modified constraint-induced movement therapy for motor and functional upper limb recovery in hospitalized patients with stroke: A randomized, multicentre, double-blind, clinical trial. Brain Stimul. 2023;16(1):40-47. [71] HSU SP, LU CF, LIN BF, et al. Effects of bihemispheric transcranial direct current stimulation on motor recovery in subacute stroke patients: a double-blind, randomized sham-controlled trial. J Neuroeng Rehabil. 2023;20(1):27. [72] LI C, CHEN Y, TU S, et al. Dual-tDCS combined with sensorimotor training promotes upper limb function in subacute stroke patients: A randomized, double-blinded, sham-controlled study. CNS Neurosci Ther. 2024;30(4):e14530. [73] HU C, TI CHE, YUAN K, et al. Effects of high-definition tDCS targeting individual motor hotspot with EMG-driven robotic hand training on upper extremity motor function: a pilot randomized controlled trial. J Neuroeng Rehabil. 2024;21(1):169. [74] WARD NS.Mechanisms underlying recovery of motor function after stroke. Postgrad Med J. 2005; 81(958):510-514. [75] TAUCHI Y, KYOUGOKU M, TAKAHASHI K, et al. Dimensionality and item-difficulty hierarchy of the Fugl-Meyer assessment of the upper extremity among Japanese patients who have experienced stroke.Top Stroke Rehabil. 2022;29(8):579-587. [76] TIAN D, IZUMI SI. Interhemispheric Facilitatory Effect of High-Frequency rTMS: Perspective from Intracortical Facilitation and Inhibition. Brain Sci. 2022;12(8):970. [77] RIZZO V, SIEBNER HR, MODUGNO N, et al. Shaping the excitability of human motor cortex with premotor rTMS. J Physiol. 2004;554(Pt 2):483-495. [78] CORTI M, PATTEN C, TRIGGS W. Repetitive Transcranial Magnetic Stimulation of Motor Cortex after Stroke: A Focused Review. Am J Phys Med Rehabil. 2012;91(3): 254-270. [79] NOWAK DA, GREFKES C, AMELI M, et al. Interhemispheric competition after stroke: brain stimulation to enhance recovery of function of the affected hand. Neurorehabil Neural Repair. 2009; 23(7):641-656. [80] 邵丹丽, 徐雪迪, 高晓平, 等. 基于上肢动作研究量表设计的改良块评价脑卒中患者上肢功能恢复潜能[J].中国组织工程研究,2020,24(35):5682-5687. [81] 吴娱倩, 张玉梅, 孟霞, 等. Wolf运动功能测试量表评定卒中患者偏瘫侧上肢功能的效度和信度研究[J]. 中国卒中杂志,2022,17(3):244-250. [82] 蔡伟强, 李浩正, 朱玉连, 等. 持续短阵脉冲刺激对脑卒中偏瘫患者静息态脑功能连接模式的影响[J]. 中国康复医学杂志,2023,38(7):898-903, 923. [83] DIONÍSIO A, GOUVEIA R, CASTELHANO J, et al. The Role of Continuous Theta Burst TMS in the Neurorehabilitation of Subacute Stroke Patients: A Placebo-Controlled Study. Front Neurol. 2021;12: 749798. [84] CHEN B, YANG T, LIAO Z, et al.Pathophysiology and Management Strategies for Post-Stroke Spasticity: An Update Review. Int J Mol Sci. 2025;26(1):406. [85] KATO N, HASHIDA G,KOBAYASHI M, et al.Characteristics and factors associated with independence in the activities of daily living of patients with amyotrophic lateral sclerosis at diagnosis. J Phys Ther Sci. 2024; 36(11):692-698. [86] HORDACRE B, GOLDSWORTHY MR, VALLENCE AM, et al. Variability in neural excitability and plasticity induction in the human cortex: A brain stimulation study. Brain Stimul. 2017;10(3):588-595. [87] BODDINGTON LJ, REYNOLDS JNJ. Targeting interhemispheric inhibition with neuromodulation to enhance stroke rehabilitation. Brain Stimul. 2017; 10(2):214-222. [88] FARAHANI F, KRONBERG G, FALLAHRAD M, et al. Effects of direct current stimulation on synaptic plasticity in a single neuron. Brain Stimul. 2021;14(3): 588-597. [89] QI F, NITSCHE MA, REN X, et al.Top-down and bottom-up stimulation techniques combined with action observation treatment in stroke rehabilitation: a perspective. Front Neurol. 2023;14:1156987. [90] QI S, CAO L, WANG Q, et al.The Physiological Mechanisms of Transcranial Direct Current Stimulation to Enhance Motor Performance: A Narrative Review. Biology. 2024;13(10):790. [91] DEL FELICE A, DALOLI V, MASIERO S, et al. Contralesional Cathodal versus Dual Transcranial Direct Current Stimulation for Decreasing Upper Limb Spasticity in Chronic Stroke Individuals: A Clinical and Neurophysiological Study. J Stroke Cerebrovasc Dis. 2016;25(12):2932-2941. |
| [1] | 王 峥, 程 吉, 于金龙, 刘文红, 王召红, 周鲁星. 水凝胶材料在脑卒中治疗中的应用进展与未来展望[J]. 中国组织工程研究, 2026, 30(8): 2081-2090. |
| [2] | 高 峰, 张 俊, 余文君, 单于玉婧, 赵 乐, 胡雨婷, 王俊华, 刘永富. 佩戴腕手矫形器对脑卒中患者手功能障碍作用的Meta分析[J]. 中国组织工程研究, 2026, 30(8): 2124-2131. |
| [3] | 陶代菊, 苏海玉, 王宇琪, 沈志强, 何 波. 高/低表达miR-122-5p稳转PC12细胞株的构建和鉴定[J]. 中国组织工程研究, 2026, 30(7): 1790-1799. |
| [4] | 曹新燕, 于子夫, 冷晓轩, 高世爱, 陈金慧, 刘西花. 重复经颅磁刺激和经颅直流电刺激对脑瘫患儿运动功能及步态影响的网状Meta分析[J]. 中国组织工程研究, 2026, 30(6): 1539-1548. |
| [5] | 郑 银, 吴振桦, 张 成, 阮可馨, 刚骁琳, 汲 泓. 免疫吸附治疗类风湿关节炎的安全性和有效性:网状Meta分析和系统评价[J]. 中国组织工程研究, 2026, 30(5): 1260-1268. |
| [6] | 冷晓轩, 赵玉欣, 刘西花. 不同神经调控刺激方式改善帕金森病患者非运动症状的网状Meta分析[J]. 中国组织工程研究, 2026, 30(5): 1282-1293. |
| [7] | 杨泽雨, 支 亮, 王 佳, 张婧欹, 张清芳, 王玉龙, 龙建军. 高频重复经颅磁刺激研究热点宏观角度的可视化分析[J]. 中国组织工程研究, 2026, 30(5): 1320-1330. |
| [8] | 杨媛媛, 周珊珊, 成小菲, 冯露叶, 汤继芹. 非侵入性脑刺激治疗脑卒中后下肢运动功能障碍的网状Meta分析[J]. 中国组织工程研究, 2026, 30(4): 1008-1018. |
| [9] | 王雪婷, 杨 巍, 王鹏琴. 脑卒中康复机器人:国内外研究现状及热点[J]. 中国组织工程研究, 2026, 30(28): 7404-7409. |
| [10] | 李思慧, 王 芹, 崔慎红, 成小菲, 冯梓芸, 王德花, 梁春婷, 冷 军. 非侵入性神经调控技术对脑卒中后失语患者言语功能影响的网状Meta分析[J]. 中国组织工程研究, 2026, 30(28): 7485-7493. |
| [11] | 房恩慧, 管 惠, 马丽虹. 非侵入性脑刺激改善孤独症谱系障碍儿童核心症状的网状Meta分析[J]. 中国组织工程研究, 2026, 30(24): 6373-6381. |
| [12] | 曹新燕, 冷晓轩, 高世爱, 陈金慧, 刘西花. 脑卒中偏瘫患者痉挛程度的影响因素及风险预测模型分析[J]. 中国组织工程研究, 2026, 30(23): 6092-6098. |
| [13] | 王乐军, 池雯欣, 宋筱倩, 李 倩, 乔敏洁, 陶海峰. 经颅直流电刺激干预后非稳定杠铃卧推运动表现及肌电活动变化[J]. 中国组织工程研究, 2026, 30(23): 6099-6109. |
| [14] | 高洪梅, 张 坤, 肖东杰, 刘 华. 人脂肪多系分化应激耐受细胞治疗大鼠缺血性脑卒中[J]. 中国组织工程研究, 2026, 30(19): 4853-4859. |
| [15] | 路安然, 王晨宇, 张 艳, 黄华生. 高强度间歇训练改善自发性高血压模型大鼠内皮祖细胞外泌体功能[J]. 中国组织工程研究, 2026, 30(18): 4627-4637. |
神经调控技术作为一类基于神经可塑性理论的中枢导向干预手段,通过非侵入性或微创方式作用于中枢神经系统,调节皮质兴奋性、跨半球功能平衡及脑网络连接性,为脑卒中上肢功能康复提供了新方向[7-9]。此次研究结合临床应用频率、现有随机对照试验数量及结局指标相关性,最终纳入12种主流神经调控技术开展分析[10],包括重复经颅磁刺激(repetitive transcranial magnetic stimulation,rTMS,含低频、高频及节律爆发刺激模式)、经颅直流电刺激(transcranial direct current stimulation,tDCS,含阳极、阴极、双侧及高分辨率亚型)、脑机接口(brain-computer interface,BCI)及经皮耳廓迷走神经刺激(transcutaneous auricular vagus nerve stimulation,taVNS)等,均已有独立研究显示这类技术联合传统康复可通过强化运动皮质兴奋性、优化神经网络协同效率,促进上肢运动功能恢复,但现有证据存在明显局限[11-14]。AHMED等[15]的系统综述与Meta分析虽提示重复经颅磁刺激与经颅直流电刺激整体有益,但未细分频率、极性等关键参数。多数研究仅聚焦单一技术[16],缺乏多技术的横向比较框架,无法形成疗效排序-临床选择的循证链条。而上肢在大脑皮质的功能分布高度精细[17],其功能重建需精准匹配干预方案,而当前研究难以满足临床分目标、个体化的康复需求[18-19]。
此次研究通过网状Meta分析,在统一方法学框架下综合多种神经调控证据,系统比较不同策略对脑卒中后上肢功能恢复的相对效果,为临床精准康复提供可解释、可排序的循证依据。
中国组织工程研究杂志出版内容重点:干细胞;骨髓干细胞;造血干细胞;脂肪干细胞;肿瘤干细胞;胚胎干细胞;脐带脐血干细胞;干细胞诱导;干细胞分化;组织工程
1.1 设计 研究设计流程见图1。
1.2 数据来源 研究已在PROSPERO 平台完成注册(注册号:CRD420251011226,https://www.
crd.york.ac.uk/PROSPERO/)。
1.2.1 检索者 由第一作者与第二作者按照既定检索策略开展文献检索。
1.2.2 数据库 PubMed、EMbase、Web of Science、
The Cochrane Library、中国知网、维普、万方和中国生物医学文献数据库。
1.2.3 检索词 中文检索词:“经皮迷走神经刺激术”“重复经颅磁刺激”“经颅直流电刺激”“脑机接口”“ 脑卒中”“ 脑出血”“ 脑缺血”“ 随机对照试验”;英文检索词:“vagus nerve stimulation”“vagus nerve stimulation” “VNS”“Transcranial Magnetic Stimulation” “TMS”“Transcranial Direct Current Stimulation”“tDCS”“stroke”“cerebrovascular accident”“randomized controlled trial”等。
1.2.4 检索时间跨度 各数据库自建库至2025年8月公开发表的中英文文献。
1.2.5 检索策略 以PubMed数据库为例,其完整检索流程见图2。
1.3 纳入标准
1.3.1 研究对象 受试者均为经颅脑CT或MRI影像学确诊的脑卒中人群,且伴随上肢运动功能障碍,年龄≥18岁,对国籍、种族、性别及病程均不作限制。
1.3.2 干预措施 试验组受试者在对照组干预的基础上,采用任一神经调控技术作为主要干预,包括但不限于:重复经颅磁刺激[包括低频、高频及θ短阵快速脉冲刺激(theta burst stimulation,TBS)模式]、经颅直流电刺激(包括高分辨率、阳极、阴极及双侧刺激)、经皮耳迷走神经刺激、脑机接口等。
1.3.3 对照措施 假刺激以及传统康复手段(物理治疗、作业治疗、运动训练及药物治疗等)。
1.3.4 结局指标 研究需至少报告以下任一结局。①主要结局指标:Fugl-Meyer上肢运动功能评定(Fugl-Meyer Assessment for Upper Extremity,FMA-UE)。②次要结局指标:Wolf
上肢运动功能测试(Wolf Motor Function Test,WMFT)、上肢动作研究量表(Action Research Arm Test,ARAT)、改良Barthel指数(Modified Barthel Index,MBI)及改良Ashworth痉挛量表(Modified Ashworth Scale,MAS)。
1.3.5 研究类型 随机对照试验。
1.4 排除标准 ①无法获取全文;②非中、英文文献;③干预措施为多种神经调控方式联合应用;④数据不完整;⑤会议摘要、综述性文章、学位论文、试验方案、重复发表。
1.5 文献筛选与数据提取 所有检索所得文献导入Zotero去除重复记录。由2名研究人员依照预先制定的检索策略独立筛选,阅读标题与摘要排除不符合纳入标准的文献,对初筛文献进一步阅读全文,以最终确定是否纳入。若2位研究人员在筛选结果上存在分歧,则由第三位研究人员裁决,直至达成一致。在数据提取前,研究团队依据研究目的与结局指标,提前制定并预设了标准化数据提取表,纳入文献的基本信息为第一作者、发表年份、研究国家、样本量、患者性别比例、患者年龄、病程、干预措施与方案、结局指标等,完成的数据提取结果经第三位研究人员比对与整合,以确保准确性与一致性。该数据提取表模板已作为补充材料提供,以便其他研究者参考和复现。
1.6 文献质量评价 偏倚风险的评估遵循Cochrane协作网指南[20],评价内容涵盖随机序列的生成方法、分配隐藏的实施情况、研究对象及研究人员盲法执行、结局指标评估过程盲法、结局数据的完整性、是否存在选择性报告以及其他潜在偏倚来源。风险等级共分为3类,即低风险(绿色)、高风险(红色)和不明确风险(黄色)。2名研究人员分别对纳入文献进行独立评估,并完成初步分级;随后由第三名研究人员对评估结果进行复核,以确保判定的客观性与一致性,团队在全面考察全文信息与质量评价的基础上,对其他潜在偏倚进行综合判断,结果以图表形式呈现。
1.7 统计分析 采用 RevMan 5.4 软件进行传统Meta分析。通过χ2检验 (α=0.1) 与 I²评估研究间异质性:当 P≥0.1 且 I² < 50% 时,提示异质性较小,采用固定效应模型;若 P < 0.1 或 I²≥50%,则认为异质性较大,采用随机效应模型。除统计异质性外,此次研究在模型选择时亦综合考虑研究设计、人群特征与干预差异等临床及方法学因素。例如,不同研究间的样本来源(单中心或多中心)、患者病程及卒中类型、刺激参数及疗程差异等均被纳入评估。当存在显著临床异质性时,即便I²较低,亦优先采用随机效应模型以提高结果稳健性。同时,针对异质性较大的结果,进一步开展干预措施、病程[21]、损伤严重程度的亚组分析与敏感性分析以探讨潜在来源[22],并验证结果的稳定性。效应量采用均数差(MD),并计算 95% 置信区间(CI)。
网状Meta分析使用Stata 16.0软件,构建干预措施间的网络关系图,其中节点代表干预方式,连线粗细表示比较次数。若网络中存在闭合环路,则采用节点劈裂法检验一致性,若直接与间接比较结果无显著差异(P > 0.05),采用一致性模型,否则结合原因分析选择不一致模型。干预措施的排序通过累积排名曲线下面积(The surface under the cumulative ranking,SUCRA)计算,结合均数差与95%置信区间进行综合判断用于辅助判断相对优势,但并不代表真实效应量的大小或临床意义,SUCRA值越高表明疗效越佳,并以联赛表的形式展示任意两种干预之间的相对效应和显著性差异,发表偏倚在研究数量不少于10篇时使用漏斗图进行评估,检验水准为α=0.05。文章的统计学方法已经山东中医药大学生物统计学专家审核。
网状Meta结果显示,在改善上肢基础运动功能(Fugl-Meyer上肢运动功能评定)方面,高频重复经颅磁刺激疗效最佳;在提升任务执行效率与精细活动(Wolf上肢运动功能测试、上肢动作研究量表)方面,连续性节律爆发刺激疗效最佳;在提高日常生活能力(改良
Barthel指数)与减轻痉挛(改良Ashworth痉挛量表)方面,阴极直流电刺激疗效最佳。
在上肢运动功能基础恢复方面,高频重复经颅磁刺激疗效最佳。Fugl-Meyer上肢运动功能评定用于评估上肢运动功能的完整性,涵盖关节主动活动度、协同与分离运动等基础指标[75]。高频重复经颅磁刺激可诱发长时程增强样神经可塑性,这是一种类似神经连接强化的生理过程,能提高患侧运动皮质的兴奋性,大脑向肢体传递运动信号的能力增强;通过作用于健侧运动皮质,减弱其对患侧的过度抑制,恢复两侧大脑半球的功能平衡,改善患侧运动功能[76-77];同时强化运动皮质与前运动区、体感皮质、小脑等脑区的协同连接,提升运动命令的编码与传递效率,还能通过调节神经修复的关键物质脑源性神经营养因子及谷氨酸、γ-氨基丁酸核心神经递质的比例,为神经修复创造有利环境[78-79]。WANG等[34]研究表明,高频重复经颅磁刺激通过调节运动皮质兴奋性,可显著促进脑卒中早期患者的上肢基础运动能力恢复,进一步验证了其在运动基础重建阶段的核心价值。
上肢实用功能与精细动作通过Wolf 上肢运动功能测试和上肢动作研究量表评估,聚焦任务执行效率与精细操作能力[80-81]。连续性节律爆发刺激在该维度表现最优,其优势并非简单提升皮质兴奋性,而是通过精准调控可塑性方向优化运动功能质量,以抑制健侧运动皮质为切入点,先削弱健侧对患侧的过度抑制,释放患侧皮质的可塑性潜力。同时,其特定的脉冲序列能在患者执行任务时,同步调节运动皮质的节律活动,减少无效代偿动作,优化运动计划的协调性[82]。DIONÍSIO等[83]的研究也观察到类似现象:单次连续性节律爆发刺激干预后,患者在拇指对指等精细任务中,患侧感觉运动区的β频段去同步化增强,这一神经电活动变化提示,大脑在任务准备与执行阶段的专注度提升,运动相关脑区的协同更高效,最终体现为精细动作的精准度与任务完成效率改善。
脑卒中患者的日常生活能力与上肢痉挛密切相关,痉挛会导致关节活动受限如手指僵硬、无法伸直,直接影响穿衣、进食等日常动作[84-85]。
此次研究发现,阴极经颅直流电刺激在改善该维度中表现最佳,其作用机制主要通过抑制过度兴奋、重建神经调控平衡实现[86-88]。通过阴极电流置于健侧使运动皮质神经元轻度超极化,减少过度兴奋的神经信号,纠正皮质内兴奋-抑制失衡[89-90]。通过皮质-脊髓通路向下调节脊髓前角运动神经元的兴奋性,降低H反射振幅、延长反射潜伏期,减少Ia纤维对运动神经元的过度激活,从而缓解肌肉痉挛[91]。诱发以长时程抑制为主的突触可塑性,持续巩固皮质功能平衡与脊髓反射控制,不仅可实现痉挛控制的改善,还可通过优化神经控制促进日常生活动作的恢复,最终实现痉挛减轻与生活能力提升的协同效益。
3.2 局限性 此次研究虽然系统整合了多种神经调控技术在脑卒中上肢功能康复中的疗效证据,但仍存在一定局限。首先,纳入的51项研究中,12种神经调控技术的分布不均,双侧节律爆发刺激仅1项研究支持,高分辨率经颅直流电刺激仅2项,这类小样本单研究技术的疗效排序难以避免统计效能不足的影响;第二,纳入文献在患者特征、干预参数(如刺激频率、强度、疗程)以及康复联合方式上差异较大,以高频重复经颅磁刺激为例,纳入研究的刺激频率涵盖 5,10,20 Hz,干预周期从1周到4周不等,增加了结果的异质性;第三,主要结局的发表偏倚检验显示结果稳健,但次要结局的研究数量相对有限,部分研究的随机化、分配隐藏及盲法等方法学质量欠佳,且多为单中心小样本试验,无法完全排除潜在发表偏倚的影响;第四,大多数研究随访时间较短,缺乏对远期疗效和安全性的系统观察,使得干预效果的持续性仍不明确。
3.3 适用性及对未来研究的启示 基于此次研究结果,未来研究可从以下3方面进一步突破现有局限。首先,应聚焦证据相对薄弱的技术领域,开展参数优化与疗效验证研究。如针对此次研究中样本量有限、证据不足的双侧节律爆发刺激与高分辨率经颅直流电刺激,通过小样本预实验明确关键参数(如刺激强度、频率、靶区)对疗效的影响机制,再开展多中心、随机对照试验以验证其临床有效性与可重复性。其次,可探索多技术联合干预的新策略。此次研究结果显示,单一神经调控技术难以同时兼顾基础运动恢复、精细功能提升及痉挛管理,未来可在急性期伴轻度痉挛的患者中设计高频重复经颅磁刺激联合阴极经颅直流电刺激的复合方案,以比较其与单一技术的相对疗效与安全性。第三,应强化机制与功能的关联研究,结合功能性磁共振成像、脑电及脑网络分析等技术,系统评估不同刺激模式对皮质兴奋性及运动网络连接性的调控效应,从而填补神经调控疗效与神经机制之间的证据空白。
3.4 结论 研究结果显示,不同神经调控技术在脑卒中后上肢运动功能恢复的不同阶段具有差异化优势,体现出“分阶段、分目标”的康复策略。急性期以恢复基础运动功能为主,高频重复经颅磁刺激可通过增强皮质兴奋性促进神经可塑性,疗效最为确切;亚急性期以提升上肢功能实用性和精细协调性为目标,连续性节律爆发刺激表现出更优效果;慢性期或伴有痉挛者以改善日常生活能力和肌张力调控为重点,阴极经颅直流电刺激疗效更佳。所有阶段均需以传统康复训练为基础,神经调控技术作为增效手段。该策略通过“阶段匹配目标、目标适配技术、技术结合训练”的逻辑,实现从“基础恢复”到 “功能独立”的递进,为临床精准康复提供可操作的路径。
中国组织工程研究杂志出版内容重点:干细胞;骨髓干细胞;造血干细胞;脂肪干细胞;肿瘤干细胞;胚胎干细胞;脐带脐血干细胞;干细胞诱导;干细胞分化;组织工程
脑卒中后上肢运动障碍常被形象地比喻为脑指挥手失灵。神经调控技术正是在这一核心环节发力,通过唤醒受损皮质的可塑性,促进大脑与肢体之间的信息重新连线。此次研究涵盖12种主流干预方式,系统比较其改善上肢功能的相对优势。与传统康复训练(如作业疗法、运动再学习)单独使用相比,当神经调控与传统康复联合应用时,可在练与调之间形成良性协同,使大脑在主动运动中得到更精准的刺激反馈。这些看不见的刺激,到底怎样帮大脑恢复对上肢的控制;高频重复经颅磁刺激是信号放大器,通过特定频率脉冲增强患侧运动皮质的神经信号,让大脑更有力地指挥手臂活动;阴极经颅直流电刺激是平衡调节器,抑制健侧过度活跃的神经,避免它抢占患侧的神经资源;而连续性节律爆发刺激更像精细教练,能优化大脑的运动计划,帮患者完成抓筷子、扣纽扣等精细动作。如果想帮家人或患者选择合适的康复方案,不妨记住这个:急性期用高频重复经颅磁刺激练基础动作,亚急性期靠连续性节律爆发刺激练精细技能,慢性期或伴痉挛选阴极经颅直流电刺激。
中国组织工程研究杂志出版内容重点:干细胞;骨髓干细胞;造血干细胞;脂肪干细胞;肿瘤干细胞;胚胎干细胞;脐带脐血干细胞;干细胞诱导;干细胞分化;组织工程#br#
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||