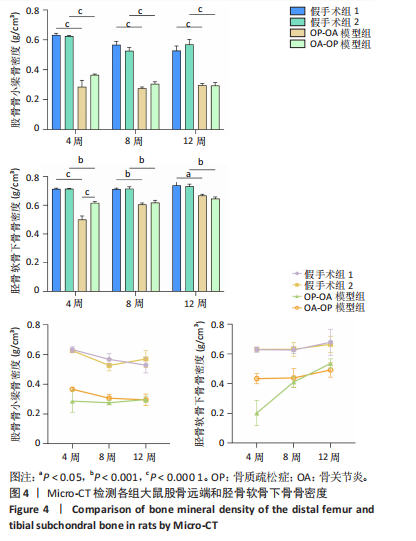
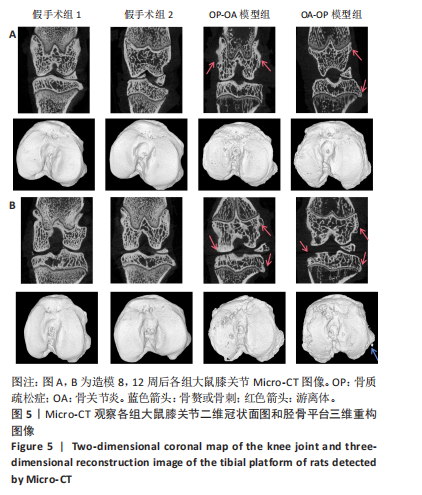
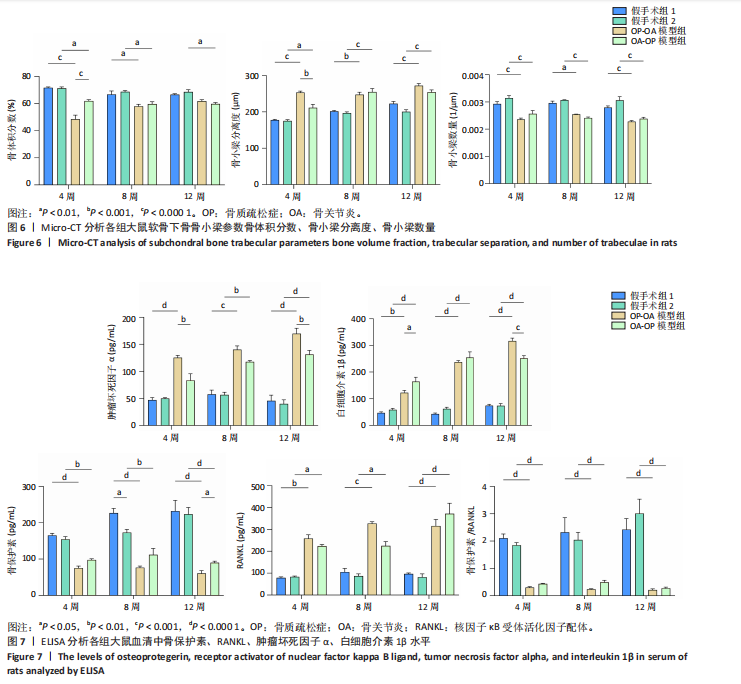
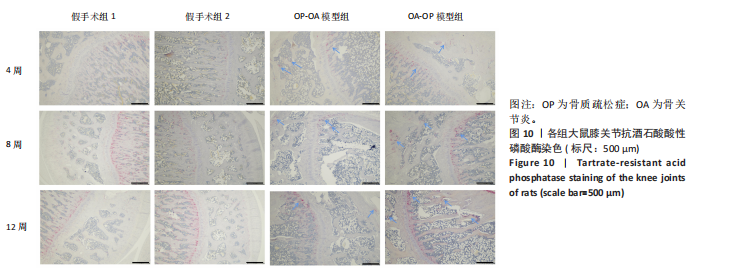
[1] WHITTY CJM, MACEWEN C, GODDARD A, et al. Rising to the challenge of multimorbidity. BMJ. 2020;368:l6964.
[2] THE LANCET. Making more of multimorbidity: an emerging priority. Lancet. 2018;391(10131):1637.
[3] GEUSENS PP, VAN DEN BERGH JP. Osteoporosis and osteoarthritis: shared mechanisms and epidemiology. Curr Opin Rheumatol. 2016; 28(2):97-103.
[4] CHEN X, TANG H, LIN J, et al. Temporal trends in the disease burden of osteoarthritis from 1990 to 2019, and projections until 2030. PLoS One. 2023;18(7):e0288561.
[5] MUÑOZ M, ROBINSON K, SHIBLI-RAHHAL A. Bone Health and Osteoporosis Prevention and Treatment. Clin Obstet Gynecol. 2020; 63(4):770-787.
[6] YUE L, BERMAN J. What Is Osteoarthritis? JAMA. 2022;327(13):1300.
[7] DAINESE P, WYNGAERT KV, DE MITS S, et al. Association between knee inflammation and knee pain in patients with knee osteoarthritis: a systematic review. Osteoarthritis Cartilage. 2022; 30(4):516-534.
[8] 北京医学会骨科学分会关节外科学组.老年骨关节炎及骨质疏松症诊断与治疗社区管理专家共识(2023版)[J].协和医学杂志, 2023,14(3):484-493.
[9] CLAYTON ES, HOCHBERG MC. Osteoporosis and osteoarthritis, rheumatoid arthritis and spondylarthropathies. Curr Osteoporos Rep. 2013;11(4):257-262.
[10] 魏戌,刘宁,章轶立,等.骨质疏松症的共病研究与早期筛查[J].中国全科医学,2022,25(35):4369-4374.
[11] KIM D, PIRSHAHID AA, LI Y, et al. Prevalence of osteoporosis in osteoarthritis: a systematic review and meta-analysis. Osteoporos Int. 2022;33(8):1687-1693.
[12] BULTINK IE, LEMS WF. Osteoarthritis and osteoporosis: what is the overlap? Curr Rheumatol Rep. 2013;15(5):328.
[13] 章轶立,黄馨懿,齐保玉,等.老年人共病研究的现实意义、内容方法与前景展望[J].中国循证医学杂志,2023,23(7):862-868.
[14] 章轶立,黄馨懿,齐保玉,等.老年人群共病问题现状挑战与应对策略[J].中国全科医学,2022,25(35):4363-4368.
[15] WANG D, QI Y, WANG Z, et al. Recent Advances in Animal Models, Diagnosis, and Treatment of Temporomandibular Joint Osteoarthritis. Tissue Eng Part B Rev. 2023;29(1):62-77.
[16] KIM JL, MOON CW, SON YS, et al. Combined Effect of Bilateral Ovariectomy and Anterior Cruciate Ligament Transection With Medial Meniscectomy on the Development of Osteoarthritis Model. Ann Rehabil Med. 2016;40(4):583-591.
[17] BEI MJ, TIAN FM, XIAO YP, et al. Raloxifene retards cartilage degradation and improves subchondral bone micro-architecture in ovariectomized rats with patella baja-induced - patellofemoral joint osteoarthritis. Osteoarthritis Cartilage. 2020;28(3):344-355.
[18] LUGO L, VILLALVILLA A, GÓMEZ R, et al. Effects of PTH [1-34] on synoviopathy in an experimental model of osteoarthritis preceded by osteoporosis. Osteoarthritis Cartilage. 2012;20(12):1619-1630.
[19] 方锐,艾力江·阿斯拉,卢勇,等.兔骨性关节炎模型构建及早中晚期的特点[J].中国组织工程研究与临床康复,2010,14(7):1218-1222.
[20] 麦聪英,谭峰,李星,等.左归丸对绝经后骨质疏松症合并骨关节炎模型大鼠下丘脑神经肽P物质及其受体的影响[J].中医杂志, 2021,62(14):1259-1265.
[21] 刘玲玲,许凌云,王斌.骨质疏松及骨关节炎与雌激素和细胞因子关系的研究进展[J].现代临床医学,2023,49(2):137-139.
[22] BUCAY N, SAROSI I, DUNSTAN CR, et al. Osteoprotegerin-deficient mice develop early onset osteoporosis and arterial calcification. Genes Dev. 1998;12(9):1260-1268.
[23] 周逸敏,邱友利,张俐.膝骨关节炎合并骨质疏松症大鼠模型的建立与评估[J].中国中医骨伤科杂志,2017,25(9):1-4.
[24] 李楠,王猛,刘永明,等.卵巢切除术构建大鼠骨关节炎合并骨质疏松模型的可行性[J].现代生物医学进展,2015,15(13):2413-2416.
[25] TORRENT A, MONTELL E, VERGÉS J, et al. Effect of chondroitin sulphate and glucosamine in combination in an animal model of osteoarthritis and Osteoporosis. Osteoarthritis Cartilage. 2014;22:S351.
[26] MA Z, WEI Y, ZHANG L, et al. GCTOF-MS Combined LC-QTRAP-MS/MS Reveals Metabolic Difference Between Osteoarthritis and Osteoporotic Osteoarthritis and the Intervention Effect of Erxian Decoction. Front Endocrinol (Lausanne). 2022;13:905507.
[27] PARK S, LEE LR, SEO JH, et al. Curcumin and tetrahydrocurcumin both prevent osteoarthritis symptoms and decrease the expressions of pro-inflammatory cytokines in estrogen-deficient rats. Genes Nutr. 2016;11:2.
[28] HU YC, HUANG TC, HUANG LW, et al. S-Equol Ameliorates Menopausal Osteoarthritis in Rats through Reducing Oxidative Stress and Cartilage Degradation. Nutrients. 2024;16(14):2364.
[29] ABRAMOFF B, CALDERA FE. Osteoarthritis: Pathology, Diagnosis, and Treatment Options. Med Clin North Am. 2020;104(2):293-311.
[30] 邢润麟,王培民,张农山,等.中医“肝肾同源”理论异病同治膝骨关节炎和绝经后骨质疏松症的实验理论基础研究[J].中医正骨,2017,29(1):1-10.
[31] HU W, CHEN Y, DOU C, et al. Microenvironment in subchondral bone: predominant regulator for the treatment of osteoarthritis. Ann Rheum Dis. 2021;80(4):413-422.
[32] 章家皓,田佳庆,王帅,等.补肾强筋胶囊对膝骨关节炎大鼠膝关节软骨下骨质的影响及其作用机制的实验研究[J].中医正骨, 2024,36(8):19-26.
[33] HULLEY PA, PAPADIMITRIOU-OLIVGERI I, KNOWLES HJ. Osteoblast-Osteoclast Coculture Amplifies Inhibitory Effects of FG-4592 on Human Osteoclastogenesis and Reduces Bone Resorption. JBMR Plus. 2020;4(7):e10370.
[34] LI Y, LIEM Y, DALL’ARA E, et al. Subchondral bone microarchitecture and mineral density in human osteoarthritis and osteoporosis: A regional and compartmental analysis. J Orthop Res. 2021;39(12):2568-2580.
[35] KENKRE JS, BASSETT J. The bone remodelling cycle. Ann Clin Biochem. 2018;55(3):308-327.
[36] 司元龙,陈志伟,申建军.基于OPG/RANKL/RANK信号通路探讨中医“血瘀”与膝骨关节炎[J/OL].中医学报,1-9[2025-03-20].http://kns.cnki.net/kcms/detail/41.1411.R.20241127.1424.036.html.
[37] BELLIDO M, LUGO L, ROMAN-BLAS JA, et al. Subchondral bone microstructural damage by increased remodelling aggravates experimental osteoarthritis preceded by osteoporosis. Arthritis Res Ther. 2010;12(4):R152.
[38] CHU L, LIU X, HE Z, et al. Articular Cartilage Degradation and Aberrant Subchondral Bone Remodeling in Patients with Osteoarthritis and Osteoporosis. J Bone Miner Res. 2020;35(3):505-515.
[39] CHE AHMAD TANTOWI NA, LAU SF, MOHAMED S. Ficus deltoidea Prevented Bone Loss in Preclinical Osteoporosis/Osteoarthritis Model by Suppressing Inflammation. Calcif Tissue Int. 2018;103(4):388-399.
[40] BULTINK IE, VIS M, VAN DER HORST-BRUINSMA IE, et al. Inflammatory rheumatic disorders and bone. Curr Rheumatol Rep. 2012;14(3):224-230.
|