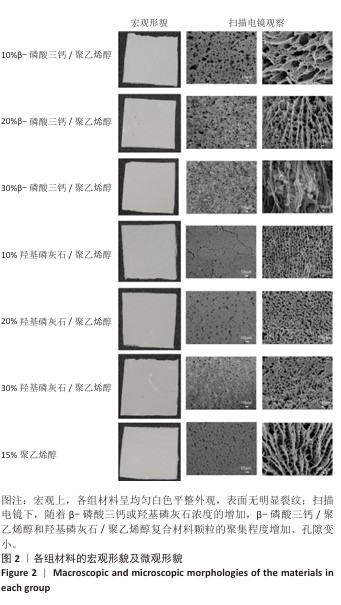
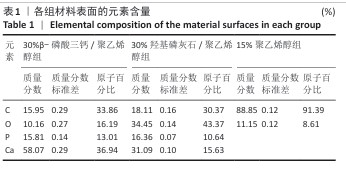
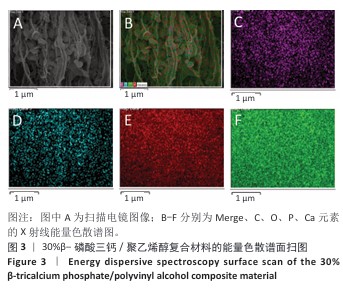
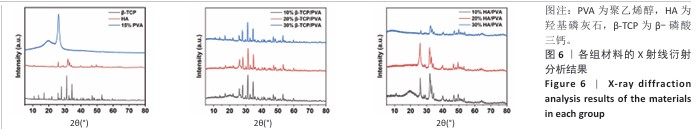
[1] MARIAN D, TORO G, D’AMICO G, et al. Challenges and Innovations in Alveolar Bone Regeneration: A Narrative Review on Materials, Techniques, Clinical Outcomes, and Future Directions. Medicina (Kaunas). 2024;61(1):20.
[2] XU Z, WANG J, GAO L, et al. Hydrogels in Alveolar Bone Regeneration. ACS Biomater Sci Eng. 2024;10(12):7337-7351.
[3] SHEKARIAN M, AGHAJANI F, HEJAZI ZSM, et al. Tooth Graft and Platelet-Rich Fibrin Mixture for Oral Bone Reconstruction and Preservation: A Scoping Review. Clin Exp Dent Res. 2025;11(4):e70160.
[4] LI L, XU J, YE C, et al. Biomaterials-based strategy for dental-oral tissue regeneration: current clinical application, laboratory development, and future direction. Biomaterials. 2025;326:123714.
[5] CHEN Y, ZHANG X, TANG Y, et al. The effects of FOXC2-gene-manipulated human periodontal ligament stem cells on bone regeneration of craniofacial bone defect. Dent Mater. 2025;41(6):708-720.
[6] HUANG K, LI Q, LIU Y, et al. 3D-printed functionalized strontium-silk fibroin-hydroxyapatite scaffolds facilitate bone regeneration via immunomodulatory and sequential angiogenic-osteogenic coupling. Bioact Mater. 2026;55:271-289.
[7] WANG FZ, LIU S, GAO M, et al. 3D-Printed Polycaprolactone/Hydroxyapatite Bionic Scaffold for Bone Regeneration. Polymers(Basel). 2025;17(7):858.
[8] MANDATORI D, D’AMICO E, ROMASCO T, et al. A 3D in vitro model of biphasic calcium phosphate (BCP) scaffold combined with human osteoblasts, osteoclasts, and endothelial cells as a platform to mimic the oral microenvironment for tissue regeneration. J Dent. 2024;151:105411.
[9] DU Y, LIU T, DING T, et al. Adhesive lipophilic gels delivering rapamycin prevent oral leukoplakia from malignant transformation. Mater Today Bio. 2024;29: 101305.
[10] HUANG Q, HAN L, WANG R, et al. Electrospun Nanofibers Loaded with Concentrated Growth Factors and Nanohydroxyapatite for the Healing of Alveolar Bone in Tooth Extraction Wounds. ACS Biomater Sci Eng. 2025;11(10):5975-5990.
[11] AMER AA, KARKAR Y, BINGLE L, et al. Fast-Disintegrating Oral Films Containing Nisin-Loaded Niosomes. Molecules. 2025;30(18):3715.
[12] MASLII Y, HERBINA N, DENE L, et al. Mucoadhesive polymeric film with plant-based compounds for dental applications: formulation, characterization and evaluation. Pharm Dev Technol. 2025;30(4):505-520.
[13] DOŁOWACKA-JÓŹWIAK A, NAWROT-HADZIK I, MATKOWSKI A, et al. Mucoadhesive PVA Film for Sustained Resveratrol Delivery: Formulation, Characterization, and Release Profile. Molecules. 2025;30(12):2642.
[14] ECKERMANN C, KLEIN CJ, SCHÄFER F, et al. Probiotics-embedded polymer films for oral health: Development, characterization, and therapeutic potential. Colloids Surf B Biointerfaces. 2025;255:114886.
[15] DONGWEN L, DAPENG M, JIAZHI Y, et al. Hydrogels in Oral Disease Management: A Review of Innovations in Drug Delivery and Tissue Regeneration. Med Sci Monit. 2025;31:e946122.
[16] CETIN GENC C, YILMAZ-DAGDEVIREN HD, DENIZ Y, et al. Unveiling Bone and Dental Regeneration Potential of Quince Seed Mucilage-Nanohydroxyapatite Scaffolds in Rabbit Mandibles. J Biomed Mater Res B Appl Biomater. 2025; 113(4):e35570.
[17] KHOSRONEJAD A, ARABION H, IRAJI A, et al. Mandibular bone defect healing using polylactic acid-nano-hydroxyapatite-gelatin scaffold loaded with hesperidin and dental pulp stem cells in rat. Tissue Cell. 2025;93:102700.
[18] FISCHER NG, DE SOUZA ARAÚJO IJ, DAGHRERY A, et al. Guidance on biomaterials for periodontal tissue regeneration: Fabrication methods, materials and biological considerations. Dent Mater. 2025;41(3):283-305.
[19] ZHANG X, CONTESSI NEGRINI N, CORREIA R, et al. Generating Tooth Organoids Using Defined Bioorthogonally Cross-Linked Hydrogels. ACS Macro Lett. 2024; 13(12):1620-1626.
[20] ZHANG Q, HE J, ZHU D, et al. Genetically modified organoids for tissue engineering and regenerative medicine. Adv Colloid Interfac. 2025;335:103337.
[21] ABEDI N, SADEGHIAN A, KOUHI M, et al. Immunomodulation in Bone Tissue Engineering: Recent Advancements in Scaffold Design and Biological Modifications for Enhanced Regeneration. Adv Colloid Interfac. 2025;11(3): 1269-1290.
[22] ZHAO X, YAO M, WANG Y, et al. Neuroregulation during Bone Formation and Regeneration: Mechanisms and Strategies. ACS Appl Mater Interfaces. 2025; 17(5):7223-7250.
[23] WANG J, CHEN X, LI R, et al. Standardization and consensus in the development and application of bone organoids. Theranostics. 2025;15(2):682-706.
[24] 丁刘闯,赵小琦,韩祥祯,等. 3D打印PVA/nHA支架与SF/PVA/nHA支架的性能比较[J].口腔医学,2018,38(7):598-602.
[25] 周琦琪,韩祥祯,宋艳艳,等. 3D打印羊椎骨粉/聚乙烯醇支架、纳米级羟基磷灰石/聚乙烯醇支架、羊椎骨粉/聚乙烯醇无孔骨板的性能比较[J]. 中国组织工程研究,2016,20(52):7851-7857.
[26] ZHU L, DU X, FU G, et al. Efficacy of different forms of concentrated growth factors combined with deproteinized bovine bone minerals in guided bone regeneration: a randomized clinical trial. BMC Oral Health. 2025;25(1):320.
[27] SHEN Z, ZHU YW, WEI YW, et al. Enhanced Osteogenic Activity of a Titanium Mesh Modified with Magnesium-Doped Nanowires for Peri-Implant Guided Bone Regeneration: In Vitro and In Vivo. ACS Biomater Sci Eng. 2025;11(5):2664-2676.
[28] YIN Z, CHEN Y, YANG G, et al. 3D Printed HA/β-TCP Scaffold: A Macroscopic Microscopic Analysis and Biological Validation Study of the Effect of the Component Ratio on Performance. ACS Appl Bio Mater. 2025;8(11):9807-9823.
[29] AYDIN A, ULAG S, NOURI S, et al. Production of Polyvinyl Alcohol/Amoxicillin - Chitosan/Collagen Hybrid Bilayer Membranes for Regeneration of Gingival Tissues. Macromol Biosci. 2025;25(1):e2400331.
[30] BARIK B, SATAPATHY BS, ACHARYA B, et al. Therapeutic Potential of AgNP-Infused Patches in Periodontal Disease: An Observational Study in Albino Rats. Int J Nanomed. 2025;20: 5337-5352.
[31] JIANG K, LUO C, LI YM, et al. An immunomodulatory and osteogenic bacterial cellulose scaffold for bone regeneration via regulating the immune microenvironment. Int J Biol Macromol. 2024;281(Pt 3):136375.
[32] KHADDOUR AS, DRĂGHICI EC, IONESCU M, et al. Bone Regeneration in Defects Created on Rat Calvaria Grafted with Porcine Xenograft and Synthetic Hydroxyapatite Reinforced with Titanium Particles-A Microscopic and Histological Study. J Funct Biomater. 2025;16(4):146.
[33] DE MORAES MARCONDES G, PARETSIS NF, DA SILVA DCB, et al. Bone Tissue Engineering With Chitosan, Carbon Nanotubes, and Hydroxyapatite Biomaterials Enriched With Mesenchymal Stem Cells: A Radiographic and Histological Evaluation in a Sheep Model Undergoing Ostectomy (Bone Tissue Engineering in a Sheep Model). J Appl Biomater Biom. 2025;113(1):e35523.
[34] WANG Z, SHANG J, ZHANG Z. Composite or Modified Hydroxyapatite Microspheres as Drug Delivery Carrier for Bone and Tooth Tissue Engineering. Curr Med Chem. 2025;32(5):974-981.
[35] YANG W, ZOU Q, WANG C, et al. Enhancing Bone Regeneration and Osteogenic Quality by n-HA Internalized Osteoblasts Synergized with ON Protein: Mechanistic Insights. ACS Appl Mater Interfaces. 2024;16(50):68967-68982.
[36] XIANG M, ZHANG G, LIU Y, et al. Polydopamine-functionalized nanohydroxyapatite coated exosomes with enhanced cytocompatibility and osteogenesis for bone regeneration. Biomed Mater Eng. 2025;36(2):98-109.
[37] QIU W, ZHANG K, WU M, et al. Tri-Layer Citrate-Based Hydroxyapatite Composite Scaffold Promoting Osteogenesis and Gingival Tissue Regeneration for Periodontal Bone Defect Repair. Adv Healthc Mater. 2025;14(13):e2501002.
[38] PITOL-PALIN L, MOURA J, FRIGÉRIO PB, et al. A preliminary study of cell-based bone tissue engineering into 3D-printed β-tricalcium phosphate scaffolds and polydioxanone membranes. Sci Rep. 2024;14(1):31184.
[39] VALDEC S, BOSSHARD FA, PATRIZI A, et al. Beta-Tricalcium Phosphate (β-TCP) for Customized Bone Regeneration (CBR) in the Aesthetic Area of the Maxillary Anterior Alveolar Ridge. Int J Oral Maxillofac Implants. 2025:1-18. doi: 10.11607/jomi.11352.
[40] ARORA V, JOSHI A, ANTHWAL N, et al. Bone regeneration using PRF, PRP and β-TCP in bone defects. Bioinformation. 2025;21(4):793-796.
[41] YU F, ZHAO X, ZHANG S, et al. Regulation of T Cell Glycosylation by MXene/β-TCP Nanocomposite for Enhanced Mandibular Bone Regeneration. Adv Healthc Mater. 2025;14(6):e2404015.
[42] PONGSETTAKUL A, LEEPONG N, SUTTAPREYASRI S. Repairing Dehiscence Defects at Implant Sites Using β-Tricalcium Phosphate/Calcium Sulfate Versus Xenograft Combined With Membrane: A Randomized Clinical Trial. J Oral Implantol. 2025; 51(1):6-13.
[43] CHAD MAB, CENCI EDS, ORLANDINI RK, et al. Socket preservation following tooth extraction: an experimental study comparing β-Tricalcium phosphate and F18 bioglass in rats. J Oral Maxil Surg. 2024;29(1):16.
[44] WEI L, SUN Y, YU D, et al. The Clinical Efficacy and Safety of ErhBMP-2/BioCaP/β-TCP as a Novel Bone Substitute Using the Tooth-Extraction-Socket-Healing Model: A Proof-of-Concept Randomized Controlled Trial. J Clin Periodontol. 2025;52(2):299-309.
[45] SHI A, SHI Y, LI J, et al. Advancements in 3D gel culture systems for enhanced angiogenesis in bone tissue engineering. J mater Chem B. 2025;13(11): 3516-3527.
[46] WU B, LI X, WANG R, et al. Biomimetic Mineralized Collagen Scaffolds for Bone Tissue Engineering: Strategies on Elaborate Fabrication for Bioactivity Improvement. Small. 2025;21(3):e2406441.
[47] VILLANI C, MURUGAN P, GEORGE A. Exosome-Laden Hydrogels as Promising Carriers for Oral and Bone Tissue Engineering: Insight into Cell-Free Drug Delivery. Int J Mol Sci. 2024;25(20):11092.
[48] PEI Z, XU H, GUO M, et al. A soft-hard hybrid scaffold for osteochondral regeneration through integration of composite hydrogel and biodegradable magnesium. Biomaterials. 2026;324:123493.
|