Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (30): 4774-4781.doi: 10.3969/j.issn.2095-4344.0978
Previous Articles Next Articles
Osteoporotic vertebral compression fractures treated by vertebroplasty with bone cements of different viscosity
Liu Yang
- Department of Orthopedics, First Affiliated Hospital of Guiyang College of Traditional Chinese Medicine, Guiyang 550001, Guizhou Province, China
-
Received:2018-06-01Online:2018-10-28Published:2018-10-28 -
About author:Liu Yang, Master, Attending physician, Department of Orthopedics, First Affiliated Hospital of Guiyang College of Traditional Chinese Medicine, Guiyang 550001, Guizhou Province, China
CLC Number:
Cite this article
Liu Yang. Osteoporotic vertebral compression fractures treated by vertebroplasty with bone cements of different viscosity[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(30): 4774-4781.
share this article
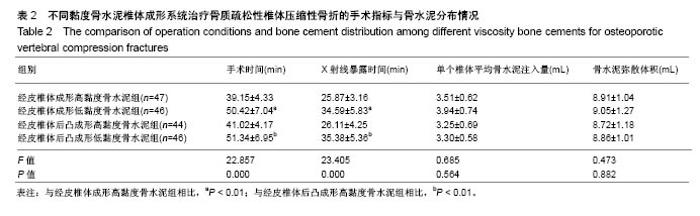
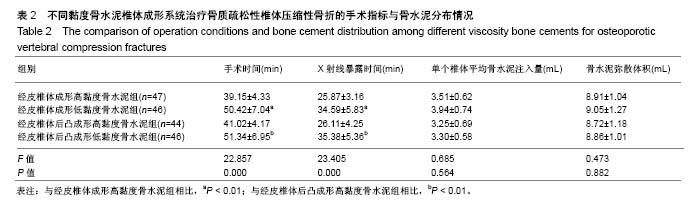
2.2 手术情况与骨水泥分布情况 结果显示,经皮椎体成形高黏度骨水泥组的手术时间和X射线暴露时间与经皮椎体成形低黏度骨水泥组相比差异有显著性意义(P < 0.01);经皮椎体后凸成形高黏度骨水泥组的手术时间和X射线暴露时间与经皮椎体后凸成形低黏度骨水泥组相比差异有显著性意义(P < 0.01);经皮椎体成形高黏度骨水泥组的手术时间和X射线暴露时间与经皮椎体后凸成形高黏度骨水泥组相比差异无显著性意义(P > 0.05);经皮椎体成形低黏度骨水泥组的手术时间和X射线暴露时间与经皮椎体后凸成形低黏度骨水泥组相比差异无显著性意义(P > 0.05)。4组单个椎体平均骨水泥注入量和骨水泥弥散体积接近(P > 0.05),见表2。"
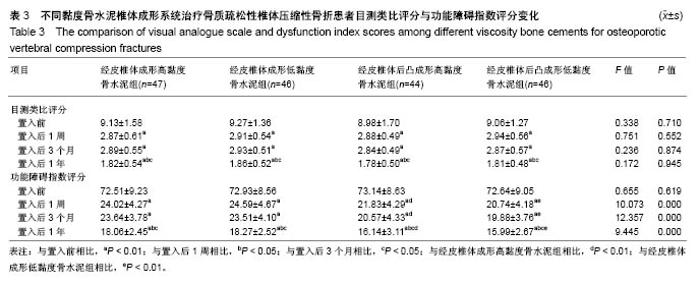
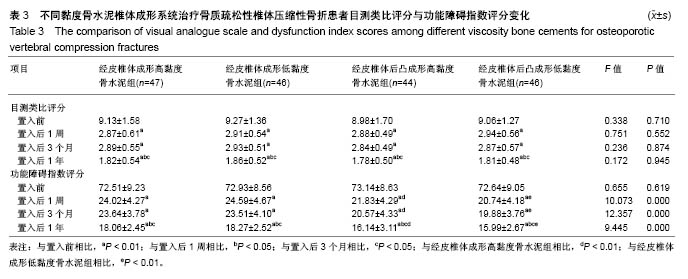
2.3 目测类比评分与功能障碍指数 结果显示,各组置入后1周、3个月、1年目测类比评分和功能障碍指数评分与置入前相比差异有显著性意义(P < 0.01);置入前、置入后1周、3个月、1年各组间目测类比评分差异无显著性意义 (P > 0.05);置入后1周和3个月各组目测类比评分和功能障碍指数评分与置入后1年比较相比有显著性意义(P < 0.05);置入后1周、3个月、1年经皮椎体成形高黏度骨水泥组功能障碍指数评分与经皮椎体后凸成形高黏度骨水泥组相比差异有显著性意义(P < 0.01);置入后1周、3个月、1年经皮椎体成形低黏度骨水泥组功能障碍指数评分与经皮椎体后凸成形低黏度骨水泥组相比差异有显著性意义 (P < 0.01);置入后1周、3个月、1年经皮椎体成形高黏度骨水泥组功能障碍指数评分与经皮椎体成形低黏度骨水泥组相比差异无显著性意义(P > 0.05);置入后1周、3个月、1年经皮椎体后凸成形高黏度骨水泥组功能障碍指数评分与经皮椎体后凸成形低黏度骨水泥组相比差异无显著性意义(P > 0.05),见表3。"
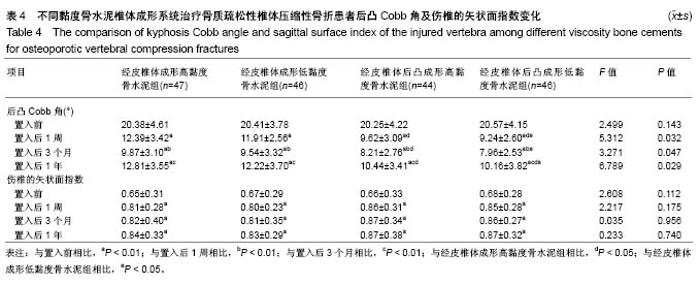
2.4 后凸Cobb角及伤椎的矢状面指数 结果显示,各组置入后1周、3个月、1年后凸Cobb角及伤椎的矢状面指数与置入前相比差异有显著性意义(P < 0.01);置入后1周各组后凸Cobb角与置入后3个月相比差异有显著性意义(P < 0.01);置入后3个月各组后凸Cobb角与置入后1年相比差异有显著性意义(P < 0.01);置入后1周、3个月、1年经皮椎体成形高黏度骨水泥组后凸Cobb角与经皮椎体后凸成形高黏度骨水泥组相比差异有显著性意义(P < 0.05);置入后1周和1年经皮椎体成形高黏度骨水泥组后凸Cobb角与经皮椎体后凸成形低黏度骨水泥组相比差异有显著性意义(P < 0.05);置入后1周、3个月、1年B组后凸Cobb角与经皮椎体后凸成形低黏度骨水泥组相比差异有显著性意义 (P < 0.05);置入后1周、3个月、1年经皮椎体成形高黏度骨水泥组后凸Cobb角及伤椎的矢状面指数与经皮椎体成形低黏度骨水泥组相比差异无显著性意义(P > 0.05);置入后1周、3个月、1年C组后凸Cobb角及伤椎的矢状面指数与经皮椎体后凸成形低黏度骨水泥组相比差异无显著性意义(P > 0.05);置入前、置入后1周、3个月、1年各组伤椎的矢状面指数相比差异无显著性意义(P > 0.05),见表4。 2.5 并发症发生情况与骨水泥渗漏发生率 结果显示,经皮椎体成形高黏度骨水泥组47例患者64个椎体中有1个椎体发生椎体皮质渗漏、1个椎体发生终板渗漏、2个椎体发生椎旁血管渗漏,渗漏发生率为6%;经皮椎体成形低黏度骨水泥组46例患者68个椎体中有4个椎体发生椎体皮质渗漏、2个椎体发生终板渗漏、4个椎体发生椎旁血管渗漏、1个椎体发生椎管内渗漏,渗漏发生率为16%;经皮椎体后凸成形高黏度骨水泥组44例患者66个椎体中有1个椎体发生椎体皮质渗漏、1个椎体发生终板渗漏、1个椎体发生椎旁血管渗漏,渗漏发生率为5%;经皮椎体后凸成形低黏度骨水泥组46例患者67个椎体中有5个椎体发生椎体皮质渗漏、1个椎体发生终板渗漏、3个椎体发生椎旁血管渗漏、1个椎体发生椎管内渗漏,渗漏发生率为15%。各组患者均未出现神经损伤症状、再次骨折或相邻椎体继发骨折、骨水泥肺栓塞和椎管狭窄。经皮椎体成形高黏度骨水泥组骨水泥渗漏发生率与经皮椎体后凸成形高黏度骨水泥组相比有显著性意义(P < 0.05);经皮椎体成形低黏度骨水泥组骨水泥渗漏发生率与经皮椎体后凸成形低黏度骨水泥组相比有显著性意义(P < 0.05);经皮椎体成形高黏度骨水泥组骨水泥渗漏发生率与经皮椎体成形低黏度骨水泥组相比无显著性意义(P > 0.05);经皮椎体后凸成形高黏度骨水泥组骨水泥渗漏发生率与经皮椎体后凸成形低黏度骨水泥组相比无显著性意义(P > 0.05)。"

| [1] 麦合木提江•穆海麦提,祝少博,李景峰,等.两种方法治疗骨质疏松致椎体压缩性骨折:安全与有效性的Meta分析[J].中国组织工程研究,2014,18(22):3551-3559.[2] 陈志强,石磊.椎体后凸成形术治疗老年骨质疏松脊柱压缩骨折[J].吉林医学,2018,39(3):500-502.[3] 冯新民,王静成,张亮,等.高黏度骨水泥在修复骨质疏松性胸腰椎骨折中的应用[J].中国组织工程研究,2014,18(30):4757-4763.[4] 张亮,王静成,冯新民,等.高粘度骨水泥椎体成形术与普通粘度椎体后凸成形术治疗骨质疏松性椎体压缩性骨折的效果比较[J].中国老年学杂志,2017,37(18):4601-4603.[5] 印平,马远征,马迅,等.骨质疏松性椎体压缩性骨折的治疗指南[J].中国骨质疏松杂志,2015,21(6):643-648.[6] 孙阳.经皮穿刺椎体成形术与保守法治疗骨质疏松性椎体压缩性骨折短期疗效对比[J].中国老年学杂志,2014,34(17): 5005-5006.[7] 周英杰,赵鹏飞,郑怀亮,等.两种骨水泥应用于老年胸腰椎骨折椎体成形术的疗效观察[J].中国矫形外科杂志,2015,23(4): 364-367.[8] 孟胜伟,蒋盛旦,蒋雷生.胸腰椎骨质疏松性椎体压缩性骨折椎体强化术后腰背痛原因的研究进展[J].脊柱外科杂志, 2017,15(2): 117-122.[9] 汪群,隋福革,汪丽静,等.经皮椎弓根钉棒置入结合椎体成形治疗胸腰椎压缩性骨折[J].中国组织工程研究,2014,18(17): 2716-2721.[10] 刘华,刘璠,魏爱淳,等.微创治疗老年骨质疏松性椎体压缩性骨折[J].中国现代医学杂志,2013,23(6):76-80.[11] 吕良庆,韦向东,蒙世远,等.老年骨质疏松性椎体压缩性骨折的治疗进展[J].中国临床新医学,2013,6(11):1123-1128.[12] 李志君,慈元,郑玉鹏,等.经皮椎体后凸成形注入骨水泥治疗骨质疏松性胸腰椎压缩骨折[J].中国组织工程研究, 2012,16(43): 8000-8004.[13] Zhai W, Jia Y, Wang J, et al. The clinical effect of percutaneous kyphoplasty for the treatment of multiple osteoporotic vertebral compression fractures and the prevention of new vertebral fractures. Int J Clin Exp Med. 2015;8(8):13473-13481. [14] Zhang L, Liu Z, Wang J, et al. Unipedicular versus bipedicular percutaneous vertebroplasty for osteoporotic vertebral compression fractures: a prospective randomized study. BMC Musculoskelet Disord. 2015;16:145. [15] Ee GW, Lei J, Guo CM, et al. Comparison of Clinical Outcomes and Radiographic Measurements in 4 Different Treatment Modalities for Osteoporotic Compression Fractures: Retrospective Analysis. J Spinal Disord Tech. 2015;28(6): E328-335.[16] 穆小平,易伟林,韦建勋,等.高黏度与普通黏度骨水泥椎体成形系统修复骨质疏松性椎体压缩性骨折的荟萃分析[J].中国组织工程研究,2017,21(2):322-328.[17] 彭昊,谭俊峰,刘洋,等.高黏度骨水泥与传统骨水泥治疗骨质疏松性椎体压缩性骨折的疗效比较[J].生物医学工程与临床, 2014, 18(4):344-348.[18] 杨刘柱,陈仲,严鑫平,等.椎体骨水泥注入联合抗骨质疏松药物治疗急性骨质疏松性椎体压缩性骨折[J].中国组织工程研究, 2014, 18(39):6265-6270.[19] 赵江,赵宇,李德成,等.经皮骨水泥注入对老年骨质疏松性椎体压缩性骨折患者的治疗效果[J].现代生物医学进展, 2016,16(30): 5864-5867.[20] 陈学忠,董玮,奚江明,等.高黏度与低黏度骨水泥在椎体成形术中应用的临床对比研究[J].成都医学院学报,2015,10(2):186-189.[21] 李停,宋建东,李志钢,等.经皮球囊扩张椎体后凸成形术治疗骨质疏松性椎体压缩性骨折骨水泥渗漏的预防[J].武汉大学学报(医学版),2014,35(2):314-317.[22] 铁镔,何仕诚,滕皋军,等.经皮椎体成形术后骨水泥渗漏的CT评价[J].中华医学杂志,2012,92(5):299-302.[23] 周湘桂,李思云.骨质疏松性椎体压缩性骨折治疗研究进展[J].中国骨质疏松杂志,2012,18(11):1062-1065.[24] Park JH, Kang KC, Shin DE, et al. Preventive effects of conservative treatment with short-term teriparatide on the progression of vertebral body collapse after osteoporotic vertebral compression fracture. Osteoporos Int. 2014;25(2): 613-618. [25] 洪鑫,吴小涛,刘磊,等.经皮椎体成形术和经皮椎体后凸成形术治疗重度骨质疏松性椎体压缩性骨折疗效分析[J].中国骨质疏松杂志,2011,17(11):969-973.[26] Zhao DH, Chen K, Zhu J, et al. Postoperative Functional Evaluation of Percutaneous Vertebroplasty Compared With Percutaneous Kyphoplasty for Vertebral Compression Fractures. Am J Ther. 2016;23(6):e1381-e1390.[27] 许立超,肖湘生.经皮椎体后凸成形术目前存在的若干问题[J].介入放射学杂志,2008,17(2):145-147.[28] 黄晓楠.骨质疏松性椎体压缩骨折治疗:注入高黏度与低黏度骨水泥的对比[J].中国组织工程研究,2014,18(16):2461-2467.[29] Hulme PA, Krebs J, Ferguson SJ, et al. Vertebroplasty and kyphoplasty: a systematic review of 69 clinical studies. Spine (Phila Pa 1976). 2006;31(17):1983-2001.[30] Eck JC, Nachtigall D, Humphreys SC,et al. Comparison of vertebroplasty and balloon kyphoplasty for treatment of vertebral compression fractures: a meta-analysis of the literature. Spine J. 2008;8(3):488-497. [31] Wang CH, Ma JZ, Zhang CC, et al. Comparison of high-viscosity cement vertebroplasty and balloon kyphoplasty for the treatment of osteoporotic vertebral compression fractures. Pain Physician. 2015;18(2):E187-194.[32] Niu J, Zhou H, Meng Q, et al. Factors affecting recompression of augmented vertebrae after successful percutaneous balloon kyphoplasty: a retrospective analysis. Acta Radiol. 2015;56(11):1380-1387. [33] 李晶.椎体后凸成形术治疗骨质疏松性椎体压缩性骨折的临床疗效观察[J].四川解剖学杂志,2017,25(1):23-25.[34] Chen X, Ren J, Zhang J, et al. Impact of Cement Placement and Leakage in Osteoporotic Vertebral Compression Fractures Followed by Percutaneous Vertebroplasty. Clin Spine Surg. 2016;29(7):E365-370. [35] Wang YT, Wu XT, Chen H, et al. Adjacent-level symptomatic fracture after percutaneous vertebral augmentation of osteoporotic vertebral compression fracture: a retrospective analysis. J Orthop Sci. 2014;19(6):868-876. [36] 黄天霁,寇玉辉,殷晓峰,等.椎体强化术后再发椎体骨折的临床特点和危险因素[J].北京大学学报(医学版),2015,47(2):237-241.[37] Rebolledo BJ, Gladnick BP, Unnanuntana A, et al. Comparison of unipedicular and bipedicular balloon kyphoplasty for the treatment of osteoporotic vertebral compression fractures: a prospective randomised study. Bone Joint J. 2013;95-B(3):401-406. [38] 杜曼•吐鲁木汗,祖帕尔•苏来曼,塔扎别克.后凸成形与椎体成形治疗骨质疏松性椎体压缩骨折的Meta分析[J].中国组织工程研究, 2014,18(13):2089-2095.[39] 王峙锦,王宏,马凯,等.高粘度骨水泥PVP 或PKP 结合体位复位治疗胸腰椎骨质疏松性椎体压缩骨折的疗效观察[J].中国骨关节损伤杂志,2016,31(S1):1-2.[40] 笪晓伟,李启中,区杰雄,等.高黏度与低黏度骨水泥在经皮椎体后凸成形术中的应用比较[J].中国骨科临床与基础研究杂志, 2015, 7(2):79-83.[41] Rapan S, Jovanovi? S, Gulan G, et al. Vertebroplasty--high viscosity cement versus low viscosity cement. Coll Antropol. 2010;34(3):1063-1067.[42] Lador R, Liberman S, Ben-Galim P, et al. A cadaver study to compare vertebral augmentation with a high-viscosity cement to augmentation with conventional lower-viscosity cement. J Spinal Disord Tech. 2013;26(2):68-73. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| [12] | Feng Guancheng, Fang Jianming, Lü Haoran, Zhang Dongsheng, Wei Jiadong, Yu Bingbing. How does bone cement dispersion affect the early outcome of percutaneous vertebroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3450-3457. |
| [13] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [14] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [15] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||