Chinese Journal of Tissue Engineering Research ›› 2015, Vol. 19 ›› Issue (23): 3633-3638.doi: 10.3969/j.issn.2095-4344.2015.23.005
Previous Articles Next Articles
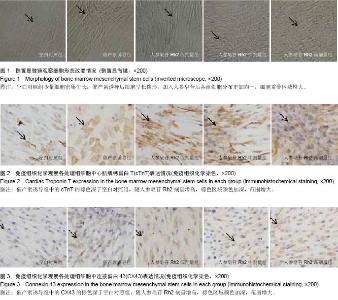
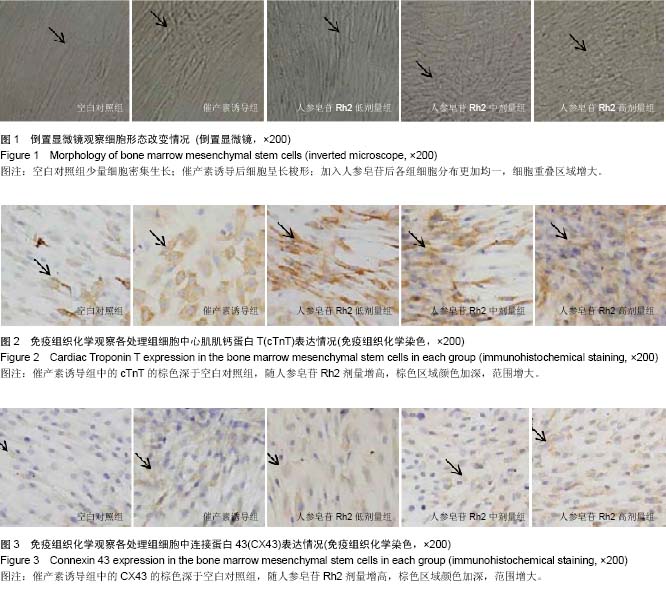
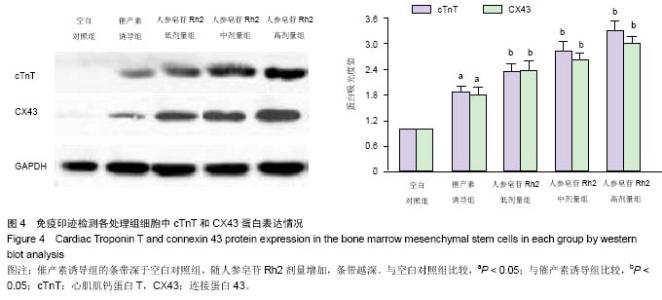
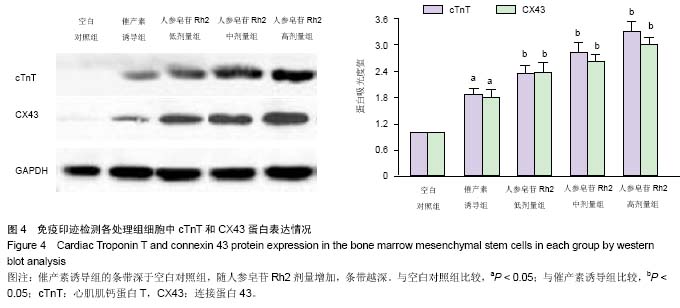
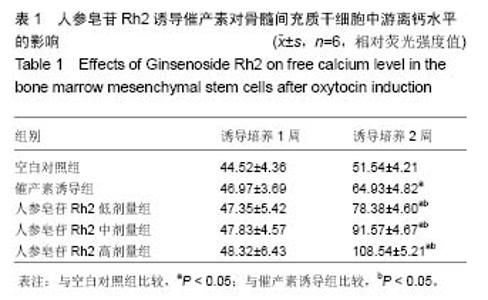
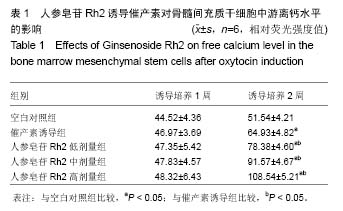
Effects of Ginsenoside Rh2 on oxytocin-induced transformation of bone marrow mesenchymal stem cells into myocardial cells
Wang Le, Tian Li, Zheng Ming-qi, Liu Gang, Ji Li-shuang, Ma Guo-ping
- Department of Cardiology, First Hospital of Hebei Medical University, Shijiazhuang 050031, Hebei Province, China
-
Online:2015-06-04Published:2015-06-04 -
Contact:Liu Gang, M.D., Chief physician, Department of Cardiology, First Hospital of Hebei Medical University, Shijiazhuang 050031, Hebei Province, China -
About author:Wang Le, Master, Attending physician, Department of Cardiology, First Hospital of Hebei Medical University, Shijiazhuang 050031, Hebei Province, China -
Supported by:a grant from Department of Science and Technology of Hebei Province of China, No. 12276102D
CLC Number:
Cite this article
Wang Le, Tian Li, Zheng Ming-qi, Liu Gang, Ji Li-shuang, Ma Guo-ping. Effects of Ginsenoside Rh2 on oxytocin-induced transformation of bone marrow mesenchymal stem cells into myocardial cells [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(23): 3633-3638.
share this article
| [1] Choi SH, Jung SY, Kwon SM, et al. Perspectives on stem cell therapy for cardiac regeneration. Advances and challenges. Circ J. 2012;76(6):1307-1312. [2] Leistner DM, Fischer-Rasokat U, Honold J, et al. Transplantation of progenitor cells and regeneration enhancement in acute myocardial infarction (TOPCARE-AMI): final 5-year results suggest long-term safety and efficacy. Clin Res Cardiol. 2011;100(10):925-934. [3] Clifford DM, Fisher SA, Brunskill SJ, et al. Stem cell treatment for acute myocardial infarction. Cochrane Database Syst Rev. 2012;2:CD006536. [4] Delewi R, Andriessen A, Tijssen JG, et al. Impact of intracoronary cell therapy on left ventricular function in the setting of acute myocardial infarction: a meta-analysis of randomised controlled clinical trials. Heart. 2013;99(4): 225-232. [5] Wu J, Li J, Zhang N, et al. Stem cell-based therapies in ischemic heart diseases: a focus on aspects of microcirculation and inflammation. Basic Res Cardiol. 2011; 106(3):317-324. [6] Zimmet H, Porapakkham P, Sata Y, et al. Short- and long-term outcomes of intracoronary and endogenously mobilized bone marrow stem cells in the treatment of ST-segment elevation myocardial infarction; a meta-analysis of randomized control trials. Eur J Heart Fail. 2012;14(1):91-105. [7] Zhang Z, Li S, Cui M, et al. Rosuvastatin enhances the therapeutic efficacy of adipose-derived mesenchymal stem cells for myocardial infarction via PI3K/Akt and MEK/ERK pathways. Basic Res Cardiol. 2013;108(2):333. [8] Dong Q, Yang Y, Song L, et al. Atorvastatin prevents mesenchymal stem cells from hypoxia and serum-free injury through activating AMP-activated protein kinase. Int J Cardiol. 2011;153(3):311-316. [9] Song L, Yang YJ, Dong QT, et al. Atorvastatin enhance efficacy of mesenchymal stem cells treatment for swine myocardial infarction via activation of nitric oxide synthase. PLoS One. 2013;8(5):e65702. [10] Qian HY, Yang YJ, Huang J, et al. Effects of Tongxinluo-facilitated cellular cardiomyoplasty with autologous bone marrow-mesenchymal stem cells on postinfarct swine hearts. Chin Med J (Engl). 2007;120(16): 1416-1425. [11] 陈声武,王岩,王毅,等.人参皂苷Rg1和Rh2抗肿瘤作用的研究[J].吉林大学学报:医学版,2003,29(1):25-28. [12] Liu J,He J,Huang L,et al.Neuroprotective effects of ginsenoside Rb1 on hippocampal neuronal injury and neurite outgrowth. Neural Regen Res. 2014;9(9):943-950. [13] Ke LN, Guo W, Xu JW,et al.Ginsenoside Rb1 attenuates activated microglia-induced neuronal damage. Neural Regen Res. 2014;9(3):252-259. [14] Moran AE, Foronzanfar MH, Roth G, et al. The Global Burden of Ischemic Heart Disease in 1990 and 2010: the Global Burden of Disease 2010 Study. Circulation. 2014;129(14): 1493-1501. [15] Hahn JY, Yu CW, Park HS, et al. Long-term effects of ischemic postconditioning on clinical outcomes: 1-year follow-up of the POST randomized trial. Am Heart J. 2015; 169(5):639-646. [16] Cherubini A, Palomba A, Morosin M, et al. Achieving optimal cholesterol levels in patients with chronic ischemic heart disease: from guidelines to the real world. G Ital Cardiol (Rome). 2015;16(4):240-249. [17] Trifunovi? Z, Obradovi? S, Balint B, et al. Functional recovery of patients with ischemic cardiomyopathy treated with coronary artery bypass surgery and concomitant intramyocardial bone marrow mononuclear cell implantation-a long-term follow-up study. Vojnosanit Pregl. 2015;72(3): 2252-2232. [18] Al-Amran FF, Shahkolahi M, Oxytocin ameliorates the immediate myocardial injury in heart transplant through down regulation of the neutrophil dependent myocardial apoptosis. Heart Views. 2014;15(2):37-45. [19] Gutkowska J, Jankowski M, Antunes-Rodrigues J, The role of oxytocin in cardiovascular regulation. Braz J Med Biol Res. 2014;47(3):206-214. [20] Gonzalez-Reyes A, Menaouar A, Yip D, et al. Molecular mechanisms underlying oxytocin-induced cardiomyocyte protection from simulated ischemia-reperfusion. Mol Cell Endocrinol. 2015. [21] Menaouar A, Florian M, Wang D, et al. Anti-hypertrophic effects of oxytocin in rat ventricular myocytes. Int J Cardiol. 2014;175(1):38-49. [22] Wei S1, Wo BL, Qi HP, et al. Early amniotomy and early oxytocin for prevention of, or therapy for, delay in first stage spontaneous labour compared with routine care. Cochrane Database Syst Rev. 2013;8:CD006794. [23] Nankali A, Keshavarzi F, Fakheri T, et al. Effect of intraumbilical vein oxytocin injection on third stage of labor. Taiwan J Obstet Gynecol. 2013;52(1):57-60. [24] Bouchard F, Paquin J, Skeletal and cardiac myogenesis accompany adipogenesis in P19 embryonal stem cells. Stem Cells Dev. 2009;18(7):1023-1032. [25] Noiseux N, Borie M, Desnoyers A, et al. Preconditioning of stem cells by oxytocin to improve their therapeutic potential. Endocrinology. 201;153(11):5361-5372. [26] Simsek Y, Celik O, Karaer A, et al. Elevated cardiac oxidative stress in newborn rats from mothers treated with atosiban. Arch Gynecol Obstet. 2012;285(3):655-661. [27] 王琪,张文祥,王思平,等.肌肉注射人脐带间充质干细胞健康大鼠心肌组织ki-67、phh3及cTnT的表达[J].中国组织工程研究,2014, 18(41):6671-6677. [28] Saad Y, Shugman IM, Kumar M, et al, Safety and efficacy of same-day discharge following elective percutaneous coronary intervention, including evaluation of next day troponin T levels. 2015;24(4):368-376. [29] 王伟光,张权宇,曹钰琨,等.к阿片受体可通过抑制β肾上腺素受体进而调节心肌细胞CX43发挥抗缺血/再灌注性心律失常[J].中国药理学通报,2010,26(4):471-476. [30] Ladenvall P, Andersson B, Dellborg M, et al. Genetic variation at the human connexin 43 locus but not at the connexin 40 locus is associated with left bundle branch block. Open Heart. 2015;2(1):e000187. [31] Kirca M, Kleinbongard P, Soetkamp D, et al. Interaction between Connexin 43 and nitric oxide synthase in mice heart mitochondria. J Cell Mol Med. 2015;19(4):815-825. [32] Gao J, Zhao Y, Wang Y, et al. Anti-arrhythmic effect of acupuncture pretreatment in the rats subjected to simulative global ischemia and reperfusion-involvement of intracellular Ca(2+) and connexin 43. BMC Complement Altern Med. 2015; 15:5. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Lin Qingfan, Xie Yixin, Chen Wanqing, Ye Zhenzhong, Chen Youfang. Human placenta-derived mesenchymal stem cell conditioned medium can upregulate BeWo cell viability and zonula occludens expression under hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 4970-4975. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Zhang Xiumei, Zhai Yunkai, Zhao Jie, Zhao Meng. Research hotspots of organoid models in recent 10 years: a search in domestic and foreign databases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1249-1255. |
| [5] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [6] | Shi Yangyang, Qin Yingfei, Wu Fuling, He Xiao, Zhang Xuejing. Pretreatment of placental mesenchymal stem cells to prevent bronchiolitis in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 991-995. |
| [7] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [8] | Fan Quanbao, Luo Huina, Wang Bingyun, Chen Shengfeng, Cui Lianxu, Jiang Wenkang, Zhao Mingming, Wang Jingjing, Luo Dongzhang, Chen Zhisheng, Bai Yinshan, Liu Canying, Zhang Hui. Biological characteristics of canine adipose-derived mesenchymal stem cells cultured in hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1002-1007. |
| [9] | Geng Yao, Yin Zhiliang, Li Xingping, Xiao Dongqin, Hou Weiguang. Role of hsa-miRNA-223-3p in regulating osteogenic differentiation of human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1008-1013. |
| [10] | Lun Zhigang, Jin Jing, Wang Tianyan, Li Aimin. Effect of peroxiredoxin 6 on proliferation and differentiation of bone marrow mesenchymal stem cells into neural lineage in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1014-1018. |
| [11] | Zhu Xuefen, Huang Cheng, Ding Jian, Dai Yongping, Liu Yuanbing, Le Lixiang, Wang Liangliang, Yang Jiandong. Mechanism of bone marrow mesenchymal stem cells differentiation into functional neurons induced by glial cell line derived neurotrophic factor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1019-1025. |
| [12] | Duan Liyun, Cao Xiaocang. Human placenta mesenchymal stem cells-derived extracellular vesicles regulate collagen deposition in intestinal mucosa of mice with colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1026-1031. |
| [13] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [14] | Guan Qian, Luan Zuo, Ye Dou, Yang Yinxiang, Wang Zhaoyan, Wang Qian, Yao Ruiqin. Morphological changes in human oligodendrocyte progenitor cells during passage [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1045-1049. |
| [15] | Wang Zhengdong, Huang Na, Chen Jingxian, Zheng Zuobing, Hu Xinyu, Li Mei, Su Xiao, Su Xuesen, Yan Nan. Inhibitory effects of sodium butyrate on microglial activation and expression of inflammatory factors induced by fluorosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1075-1080. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||