Chinese Journal of Tissue Engineering Research ›› 2015, Vol. 19 ›› Issue (18): 2814-2819.doi: 10.3969/j.issn.2095-4344.2015.18.005
Previous Articles Next Articles
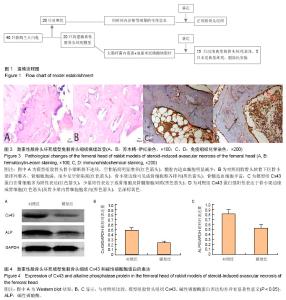
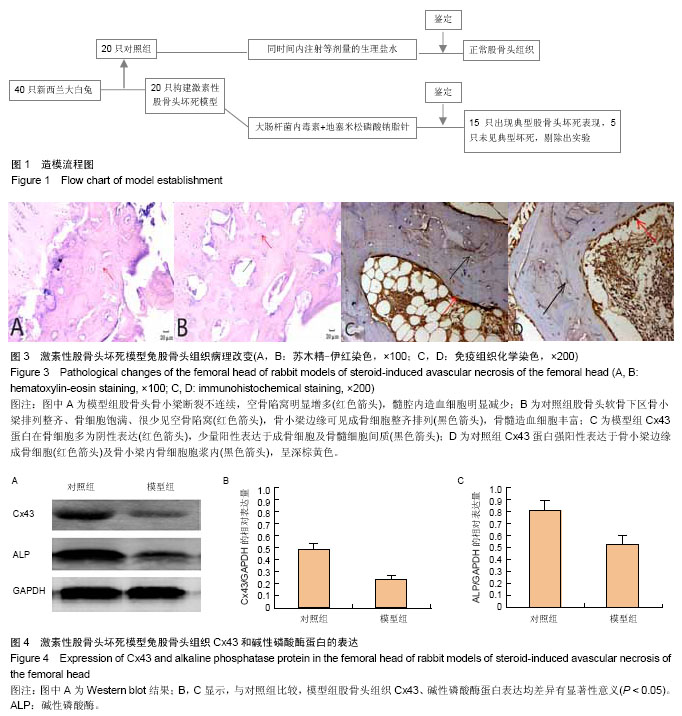
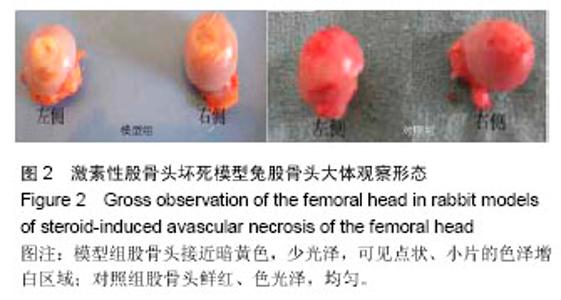
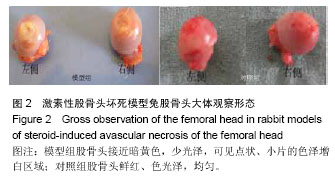
Cx43 expression in the femur of rabbit models of steroid-induced vascular necrosis of the femoral head
Wei Lu, Luo Gao-bin, Li Wei, Lin Yi-cai, Ruan Zhong-jian, Zhou Zhi-guang, Bo Zhan-dong
- Department of Bone and Joint Surgery, First Affiliated Hospital of Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China
-
Received:2015-02-13Online:2015-04-30Published:2015-04-30 -
Contact:Bo Zhan-dong, M.D., Chief physician, Department of Bone and Joint Surgery, First Affiliated Hospital of Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China -
About author:Wei Lu, Studying for master’s degree, Department of Bone and Joint Surgery, First Affiliated Hospital of Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China -
Supported by:the National Natural Science Foundation of China, No. 81460348; the General Project of Department of Education of Guangxi Zhuang Autonomous Region, No. 2013YB314
CLC Number:
Cite this article
Wei Lu, Luo Gao-bin, Li Wei, Lin Yi-cai, Ruan Zhong-jian, Zhou Zhi-guang, Bo Zhan-dong. Cx43 expression in the femur of rabbit models of steroid-induced vascular necrosis of the femoral head[J]. Chinese Journal of Tissue Engineering Research, 2015, 19(18): 2814-2819.
share this article
| [1] Wang C, Peng J, Lu S et al. Summary of the various treatments for osteonecrosis of the femoral head by mechanism: a review. Exp Ther Med, 2014;8(3):700-706. [2] TSakano-Murakam IR, Tokunaga K, Kondo N, et al. Glucocorticoid inhibits bone regeneration after osteonecrosis of the femoral head in aged female rats. Tohoku J Exp Med. 2009;217(1):51-58. [3] Kuribayashi M, Fujioka M, Takahashi KA, et al. Combination analysis of three polymorphisms for predicting the risk for steroid-induced osteonecrosis of the femoral head. J Orthop Sci. 2008;13(4):297-303. [4] Chernetsky SG, Mont MA, La Porte DM, et al. Pathologic features insteroid and nonsteroid associated osteonecrosis. Clin Orthop. 1999;368:149-161. [5] Jones LC, Hangerford DS. The pathogenesis of osteonecrosis. Instr Course Lect. 2007;56(1):179-196. [6] Guo KJ, Zhao FC, Guo Y et al. The influence of age, gender and treatment with steroids on the incidence of osteonecrosis of the femoral head during the management of severe acute respiratory syndrome: a retrospective study. Bone Joint J. 2014;96-B(2):259-262. [7] Varoga D, Drescher W, Pufe M, et al. Differential expression of vascular endothelial growth factor in glucocorticoid-related osteonecrosis of the femoral head. Clin Orthop Relat Res. 2009;467(12):3273-3282. [8] Nishida K, Yamamoto T, Motomura G, et al. Pitavastatin may reduce risk of steroid-induced osteonecrosis in rabbits: a preliminary histological study. Clin Orthop Relat Res. 2008; 466(5):1054-1058. [9] Zheng CY, Li XD, Du SX. The role of connexin43 in bone development and shaping. Int J Orthop. 2009;30(2):134-136. [10] 李瑞琦,张国平,李宜炯.激素性股骨头坏死模型:不同构建技术分析[J].中国组织工程研究,2013,17(37):6676-6681. [11] Shi B, Li G, Wang P. Effect of antler extract on corticosteroid-induced avascular necrosis of the femoral head in rats. J Ethnopharmacol. 2010;127(1):124-129. [12] 赵金东,吕松岑,薛震等.激素性股骨头坏死动物模型的建立与评价[J].中国骨肿瘤骨病,2007;6(4):220-224. [13] Orimo H. The mechanism of mineralization and the role of alkaline phosphatase in health and disease. J Nippon Med Sch. 2010;77(1):4-12. [14] 贾岩波,刘万林,任逸众.激素性股骨头坏死发病机制中细胞凋亡的研究进展[J].中国组织工程研究,2012,16(13):2444-2450. [15] O'Brien CA, Jia D, Plotkin LI, et al. Glucocorticoids act directly on osteoblasts and osteocytes to induce their apoptosis and reduce bone formation and strength. Endocrinology. 2004; 145(4):1835-1841. [16] Yun SI, Yoon HY, Jeong SY, et al. Glucocorticoid induces apoptosis of osteoblast cells through the activation of glycogen synthase kinase 3beta. J Bone Miner Metab. 2009; 27(2):140-148. [17] Hofbauer LC, Gorl F, Riggs BL, et al. Stimulation of osteop rotegerin ligand and inhibition of osteoprotegerin production byglucocorticoids in human osteoblastic lineage cells: potential paracrine mechanisms of glucocoticoid-induced osteoporosis. Endocrinology. 1999;140(10):4382-4389. [18] Moraes LA, Paul-Clark MJ, Rickman A, et al. Ligand-specific glucocorticoid receptor activation in human platelets. Blood. 2005;106(13):4167-4175. [19] 暴淑英,赵国庆,毕黎琦.激素性股骨头坏死早期细胞凋亡相关基因表达及阿轮磷酸钠的干预[J].中国组织工程研究与临床康复, 2008,12(46):9095-9099. [20] Kogianni G, Mann V, Ebetino F et al. Fas/CD95 is associated with glucocorticoid-induced osteocyte apoptosis. Life Sciences. 2004;75(24):2879-2895. [21] Plotkin LI. Connexin 43 hemichannels and intracellular signaling in bone cells. Front Physiol. 2014;5:131. [22] Buo AM, Stains JP. Gap junctional regulation of signal transduction in bone cells. FEBS Lett. 2014;588(8): 1315-1321. [23] Chung DJ, Castro CH, Watkins M, et al. Low peak bone mass and attenuated anabolic response to parathyroid hormone in mice with an osteoblast-specific deletion of connexin 43. J Cell Sci. 2006;119(20):4187-4198. [24] Bivi N, Condon KW, Allen MR, et al. Cell autonomous requirement of connexin 43 for osteocyte survival: consequences for endocortical resorption and periosteal bone formation. J Bone Miner Res. 2012;27(2):374-389. [25] Siller-Jackson AJ, Burra S, Gu S, et al. Adaptation of connexin 43-hemichannel prostaglandin release to mechanical loading. J Biol Chem. 2008;283(39):26374-26382. [26] Niger C, Buo AM, Hebert C, et al. ERK acts in parallel to PKC to mediate the connexin43-dependent potentiation of Runx2 activity by FGF2 in MC3T3 osteoblasts. Am J Physiol Cell Physiol. 2012;302(7):C1035-C1044. [27] Niger C, Luciotti MA, Buo AM. The regulation of Runx2 by FGF2 and connexin43 requires the inositol polyphosphate/protein kinase Cδ cascade. J Bone Miner Res. 2013;28(6):1468-1477. [28] Bivi N, Pacheco-Costa R, Brun LR, et al. Absence of Cx43 selectively from osteocytes enhances responsiveness to mechanical force in mice. J Orthop Res. 2013;31(7):1075-1081. [29] Mureli S, Gans CP, Bare DJ, et al. Mesenchymal stem cells improve cardiac conduction by upregulation of connexin 43 through paracrine signaling. Am J Physiol Heart Circ Physiol. 2013;304(4):600-609. [30] Kitase Y, Barragan L, Qing H, et al. Mechanical induction of PGE2 in osteocytes blocks glucocorticoid-induced apoptosis through both the beta-catenin and PKA pathways. J Bone Miner Res. 2010;25(12):2657-2668. [31] Schrobback K, Klein TJ, Woodfield TB. The importance of connexin hemichannels during chondroprogenitor cell differentiation in hydrogel versus microtissue culture models. Tissue Eng Part A. 2015. [32] Plotkin LI, Speacht TL, Donahue HJ. Cx43 and Mechanotransduction in Bone. Curr Osteoporos Rep. 2015. [33] Piryaei A, Soleimani M, Heidari MH, et al. Ultrastructural maturation of human bone marrow mesenchymal stem cells-derived cardiomyocytes under alternative induction of 5-azacytidine. Cell Biol Int. 2015. doi: 10.1002/cbin.10421. [34] Reikvam H, Ryningen A, Sæterdal LR, et al. Connexin expression in human acute myeloid leukemia cells: Identification of patient subsets based on protein and global gene expression profiles. Int J Mol Med. 2015;35(3):645-652. [35] Zhang J, Wang LL, Du W, et al. Hepatocyte growth factor modification enhances the anti-arrhythmic properties of human bone marrow-derived mesenchymal stem cells. PLoS One. 2014;9(10):e111246. [36] Xu H, Gu S, Riquelme MA, et al. Connexin 43 Channels are Essential for Normal Bone Structure and Osteocyte Viability. J Bone Miner Res. 2015;30(3):550-562. [37] Kuang W, Tang M, He X, et al. Differentiation of rat bone marrow-derived mesenchymal stem cells into cardiomyocyte-like cells induced by cyclic stretching strain. Sheng Wu Yi Xue Gong Cheng Xue Za Zhi. 2014;31(3): 596-600. [38] Rahimi M, Zarnani AH, Mohseni-Kouchesfehani H, et al. Comparative evaluation of cardiac markers in differentiated cells from menstrual blood and bone marrow-derived stem cells in vitro.Mol Biotechnol. 2014;56(12):1151-1162. [39] Geng X, Liu S, Chen Y. Involvement of ERK5 and JNK in the BMP9-induced differentiation of C3H10T1/2 cells into cardiomyocyte-like cells. Xi Bao Yu Fen Zi Mian Yi Xue Za Zhi. 2014;30(8):829-832, 840. [40] Gao Q, Guo M, Jiang X, et al. A cocktail method for promoting cardiomyocyte differentiation from bone marrow-derived mesenchymal stem cells. Stem Cells Int. 2014;2014:162024. [41] Pidoux G, Gerbaud P, Dompierre J, et al. A PKA-ezrin-Cx43 signaling complex controls gap junction communication and thereby trophoblast cell fusion. J Cell Sci. 2014;127(Pt 19): 4172-4185. [42] Nogueira-Pedro A, Dias CC, Regina H, et al. Nitric oxide-induced murine hematopoietic stem cell fate involves multiple signaling proteins, gene expression, and redox modulation. Stem Cells. 2014;32(11):2949-2960. [43] Sadr-Eshkevari P, Ashnagar S, Rashad A, et al. Bisphosphonates and connexin 43: a critical review of evidence. Cell Commun Adhes. 2014;21(5):241-247. [44] Hobolt-Pedersen AS, Delaissé JM, Søe K. Osteoclast fusion is based on heterogeneity between fusion partners. Calcif Tissue Int. 2014;95(1):73-82. [45] Damaraju S, Matyas JR, Rancourt DE, et al. The effect of mechanical stimulation on mineralization in differentiating osteoblasts in collagen-I scaffolds. Tissue Eng Part A. 2014; 20(23-24):3142-3153. [46] Zappitelli T, Aubin JE. The "connexin" between bone cells and skeletal functions. J Cell Biochem. 2014;115(10):1646-1658. [47] Plotkin LI. Connexin 43 hemichannels and intracellular signaling in bone cells. Front Physiol. 2014;5:131. [48] Lloyd SA, Loiselle AE, Zhang Y, et al. Evidence for the role of connexin 43-mediated intercellular communication in the process of intracortical bone resorption via osteocytic osteolysis. BMC Musculoskelet Disord. 2014;15:122. [49] Komori T. Mouse models for the evaluation of osteocyte functions. J Bone Metab. 2014;21(1):55-60. [50] Li N, Pasha Z, Ashraf M. Reversal of ischemic cardiomyopathy with Sca-1+ stem cells modified with multiple growth factors. PLoS One. 2014;9(4):e93645. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Zhang Lishu, Liu Anqi, He Xiaoning, Jin Yan, Li Bei, Jin Fang. Alpl gene affects the therapeutic effect of bone marrow mesenchymal stem cells on ulcerative colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3970-3975. |
| [12] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [13] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [14] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [15] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||