Chinese Journal of Tissue Engineering Research ›› 2015, Vol. 19 ›› Issue (14): 2243-2249.doi: 10.3969/j.issn.2095-4344.2015.14.019
Previous Articles Next Articles
Microfracture technique plus bone marrow mesenchymal stem cell transplantation for repair of articular cartilage injury of the knee
Hu Zuo-hong1, Wang Yu-long1, Cai Zheng-dong2, Chen Yu-quan1, Xia Yan1
- 1The 171st Hospital of PLA, Jiujiang 332000, Jiangxi Province, China; 2Shanghai Central Hospital, Shanghai 200080, China
-
Revised:2015-03-04Online:2015-04-02Published:2015-04-02 -
Contact:Wang Yu-long, Attending physician, the 171st Hospital of PLA, Jiujiang 332000, Jiangxi Province, China -
About author:Hu Zuo-hong, Associate chief physician, the 171st Hospital of PLA, Jiujiang 332000, Jiangxi Province, China -
Supported by:the Medical Research Foundation of Nanjing Military Region, No. 10MA061
CLC Number:
Cite this article
Hu Zuo-hong, Wang Yu-long, Cai Zheng-dong, Chen Yu-quan, Xia Yan. Microfracture technique plus bone marrow mesenchymal stem cell transplantation for repair of articular cartilage injury of the knee [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(14): 2243-2249.
share this article
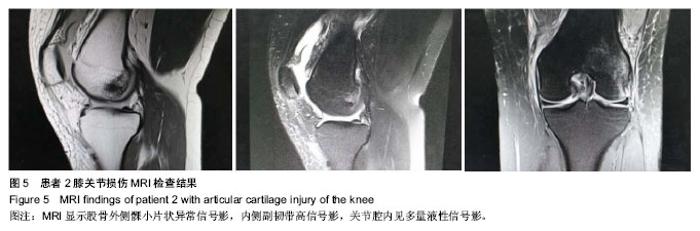
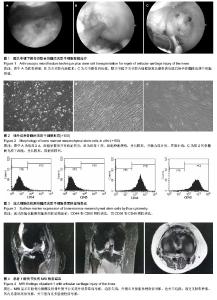
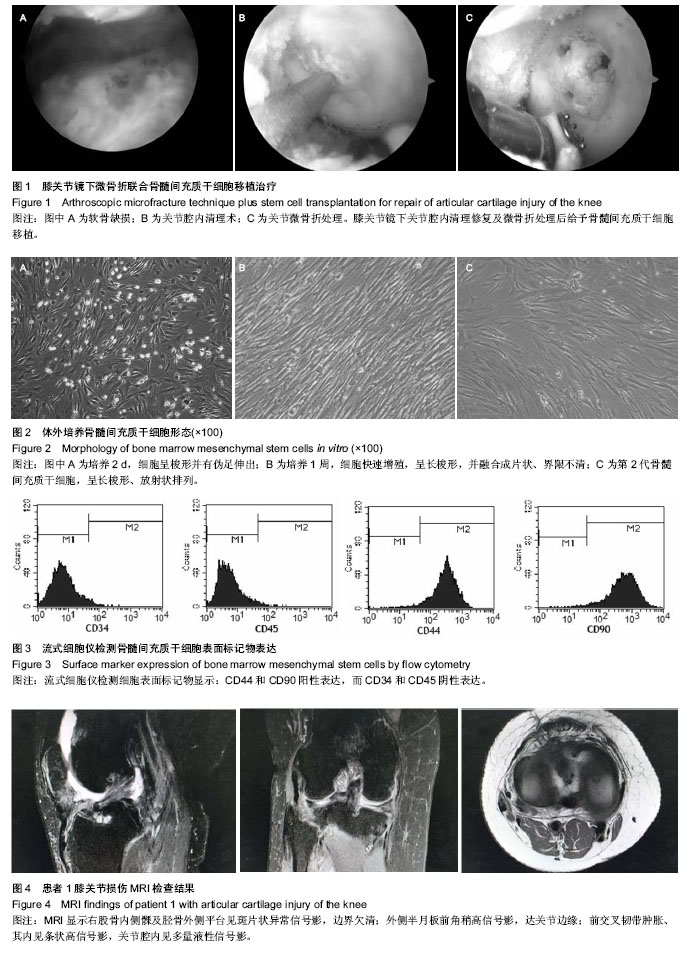
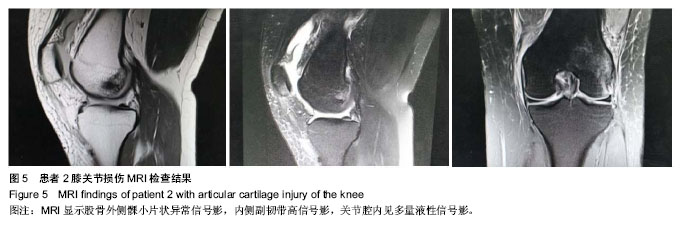
2.3 随访患者膝关节功能 随访4-18个月,显效13例,有效2例,无效1例。Lysholm膝关节评分治疗前平均42分(33-67分),治疗4周后平均89分(75-99分),平均提高47分。平均11.3个月随访均未出现症状反复和加重。 2.4 典型病例 病例1:患者女,42岁,外伤后致右膝关节肿痛1周入院治疗。患者于1周前下楼梯不慎摔伤致右膝关节肿胀、疼痛。膝关节间隙不同程度压痛,膝关节屈伸时症状明显加重。MRI显示:右股骨内侧髁、胫骨外侧平台见斑片状异常信号影,外侧半月板前角稍高信号影,前交叉韧带肿胀,其内见条状高信号影,关节腔内积液(图4)。Lysholm评分为40分。入院后完善相关检查给予关节镜下关节清理、关节镜下微骨折加自体骨髓间充质干细胞移植。治疗后4周Tegner运动评级为显效,主要症状基本消除,主要关节功能基本恢复或有明显进步。Lysholm膝关节功能评分为86分,随访未出现症状反复和加重。 病例2:患者女,32岁,外伤致左膝关节肿痛10 d入院治疗。患者于10 d前不慎扭伤致右膝关节肿胀、疼痛,活动轻度受限,休息时疼痛减轻。膝关节间隙有不同程度压痛,膝关节屈伸时症状明显加重。MRI显示:股骨外侧髁小片状异常信号影,内侧副韧带高信号影,关节腔内积液(图5)。Lysholm评分为41分。入院后完善相关检查给予关节镜下关节清理、关节镜下微骨折加自体骨髓间充质干细胞移植。治疗后4周Tegner运动评级为显效,主要症状基本消除,主要关节功能基本恢复或有明显进步。Lysholm膝关节功能评分为95分,随访未出现症状反复和加重。 2.5 不良反应 目前随访的患者中并没有发现与移植细胞相关的不良反应。"
| [1] Widuchowski W, Widuchowski J, Trzaska T. Articular cartilage defects: study of 25,124 knee arthroscopies. Knee. 2007; 14(3):177-182. [2] Dewan AK, Gibson MA, Elisseeff JH, et al. Evolution of autologous chondrocyte repair and comparison to other cartilage repair techniques. Biomed Res Int. 2014;2014: 272481.
[3] 李海鹏,刘玉杰.关节软骨损伤治疗的最新进展[J].中国矫形外科杂志,2006,14(14):1076-1078.
[4] Miller BS, Steadman JR, Briggs KK, et al. Patient satisfaction and outcome after microfracture of the degenerative knee. J Knee Surg. 2004;17(1):13-17.
[5] Steadman JR, Briggs KK, Rodrigo JJ, et al. Outcomes of microfracture for traumatic chondral defects of the knee: average 11-year follow-up.Arthroscopy. 2003;19(5):477-484.
[6] Steadman JR, Miller BS, Karas SG, et al. The microfracture technique in the treatment of full-thickness chondral lesions of the knee in National Football League players. J Knee Surg. 2003;16(2):83-86.
[7] Russlies M, Behrens P, Wünsch L,et al. A cell-seeded biocomposite for cartilage repair. Ann Anat. 2002;184(4): 317-323.
[8] Trattnig S, Ba-Ssalamah A, Pinker K, et al. Matrix-based autologous chondrocyte implantation for cartilage repair: noninvasive monitoring by high-resolution magnetic resonance imaging. Magn Reson Imaging. 2005;23(7): 779-787.
[9] 杜志坡,贝抗胜.干细胞在骨科疾病治疗中的应用[J].中国组织工程研究与临床康复,2010,14(36):6817-6820.
[10] Hernigou P, Beaujean F. Treatment of osteonecrosis with autologous bone marrow grafting. Clin Orthop Relat Res. 2002;(405):14-23.
[11] Kreuz PC, Erggelet C, Steinwachs MR, et al. Is microfracture of chondral defects in the knee associated with different results in patients aged 40 years or younger. Arthroscopy. 2006;22(11):1180-1186.
[12] Kreuz PC, Steinwachs MR, Erggelet C, et al. Results after microfracture of full-thickness chondral defects in different compartments in the knee. Osteoarthritis Cartilage. 2006; 14(11):1119-1125.
[13] Steadman JR, Briggs KK, Rodrigo JJ, et al. Outcomes of microfracture for traumatic chondral defects of the knee: average 11-year follow-up. Arthroscopy. 2003;19(5):477-484.
[14] Mithoefer K, Williams RJ 3rd, Warren RF, et al. The microfracture technique for the treatment of articular cartilage lesions in the knee. A prospective cohort study. J Bone Joint Surg Am. 2005;87(9):1911-1920.
[15] Brittberg M, Lindahl A, Nilsson A, et al. Treatment of deep cartilage defects in the knee with autologous chondrocyte transplantation. N Engl J Med. 1994;331(14):889-895.
[16] Marcacci M, Zaffagnini S, Kon E, et al. Arthroscopic autologous chondrocyte transplantation: technical note. Knee Surg Sports Traumatol Arthrosc. 2002;10(3):154-159.
[17] Xing L, Jiang Y, Gui J, et al. Microfracture combined with osteochondral paste implantation was more effective than microfracture alone for full-thickness cartilage repair. Knee Surg Sports Traumatol Arthrosc. 2013;21(8):1770-1776.
[18] Lane JG, Healey RM, Chen AC, et al. Can osteochondral grafting be augmented with microfracture in an extended-size lesion of articular cartilage. Am J Sports Med. 2010;38(7): 1316-1323.
[19] Tegner Y, Lysholm J. Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res. 1985;(198):43-49.
[20] Shapiro F, Koide S, Glimcher MJ. Cell origin and differentiation in the repair of full-thickness defects of articular cartilage. J Bone Joint Surg Am. 1993;75(4):532-553.
[21] Gomoll AH, Madry H, Knutsen G, et al. The subchondral bone in articular cartilage repair: current problems in the surgical management.Knee Surg Sports Traumatol Arthrosc. 2010; 18(4):434-447.
[22] Williams RJ 3rd, Harnly HW. Microfracture: indications, technique, and results. Instr Course Lect. 2007;56:419-428.
[23] Gill TJ, Asnis PD, Berkson EM. The treatment of articular cartilage defects using the microfracture technique. J Orthop Sports Phys Ther. 2006;36(10):728-738.
[24] Truong MD, Chung JY, Kim YJ, et al. Histomorphochemical comparison of microfracture as a first-line and a salvage procedure: is microfracture still a viable option for knee cartilage repair in a salvage situation. J Orthop Res. 2014; 32(6):802-810.
[25] Wang Q, Li ZL, Fu YM, et al. Effect of low-energy shock waves in microfracture holes in the repair of articular cartilage defects in a rabbit model. Chin Med J (Engl). 2011;124(9): 1386-1394.
[26] Kon E, Gobbi A, Filardo G, et al. Arthroscopic second-generation autologous chondrocyte implantation compared with microfracture for chondral lesions of the knee: prospective nonrandomized study at 5 years. Am J Sports Med. 2009;37(1):33-41.
[27] Peterson L, Brittberg M, Kiviranta I, et al. Autologous chondrocyte transplantation. Biomechanics and long-term durability. Am J Sports Med. 2002;30(1):2-12.
[28] Saris DB, Vanlauwe J, Victor J, et al. Characterized chondrocyte implantation results in better structural repair when treating symptomatic cartilage defects of the knee in a randomized controlled trial versus microfracture. Am J Sports Med. 2008;36(2):235-246.
[29] Knutsen G, Drogset JO, Engebretsen L, et al. A randomized trial comparing autologous chondrocyte implantation with microfracture. Findings at five years. J Bone Joint Surg Am. 2007;89(10):2105-2112.
[30] Knutsen G, Engebretsen L, Ludvigsen TC, et al. Autologous chondrocyte implantation compared with microfracture in the knee. A randomized trial. J Bone Joint Surg Am. 2004;86-A(3): 455-464.
[31] Yoo JU, Barthel TS, Nishimura K, et al. The chondrogenic potential of human bone-marrow-derived mesenchymal progenitor cells.J Bone Joint Surg Am. 1998;80(12): 1745-1757.
[32] Nejadnik H, Hui JH, Feng Choong EP, et al. Autologous bone marrow-derived mesenchymal stem cells versus autologous chondrocyte implantation: an observational cohort study. Am J Sports Med. 2010;38(6):1110-1116.
[33] 任杰,郑荣琴,黄冬梅,等.膝关节软骨退行性变的声像学表现[J].中国超声医学杂志,2006,22(2):151-153.
[34] 王万宗,陈宗雄,刘晓强.骨髓间充质干细胞与关节软骨细胞Transwell共培养诱导形成软骨[J].中国组织工程研究与临床康复,2010,14(38):7041-7044.
[35] Coleman RM, Case ND, Guldberg RE. Hydrogel effects on bone marrow stromal cell response to chondrogenic growth factors. Biomaterials. 2007;28(12):2077-2086.
[36] Gille J, Schuseil E, Wimmer J, et al. Mid-term results of Autologous Matrix-Induced Chondrogenesis for treatment of focal cartilage defects in the knee. Knee Surg Sports Traumatol Arthrosc. 2010;18(11):1456-1464.
[37] Siclari A, Mascaro G, Gentili C, et al. A cell-free scaffold-based cartilage repair provides improved function hyaline-like repair at one year. Clin Orthop Relat Res. 2012; 470(3):910-919.
[38] 赵卫民,聂振洪,张书玲. 关节镜下微骨折术治疗膝关节软骨损伤的临床观察[J].疑难病杂志,2010,9(6):456-457. |
| [1] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [2] | Wu Xun, Meng Juanhong, Zhang Jianyun, Wang Liang. Concentrated growth factors in the repair of a full-thickness condylar cartilage defect in a rabbit [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1166-1171. |
| [3] | Li Jiacheng, Liang Xuezhen, Liu Jinbao, Xu Bo, Li Gang. Differential mRNA expression profile and competitive endogenous RNA regulatory network in osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1212-1217. |
| [4] | Geng Qiudong, Ge Haiya, Wang Heming, Li Nan. Role and mechanism of Guilu Erxianjiao in treatment of osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1229-1236. |
| [5] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [6] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [7] | Geng Yao, Yin Zhiliang, Li Xingping, Xiao Dongqin, Hou Weiguang. Role of hsa-miRNA-223-3p in regulating osteogenic differentiation of human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1008-1013. |
| [8] | Lun Zhigang, Jin Jing, Wang Tianyan, Li Aimin. Effect of peroxiredoxin 6 on proliferation and differentiation of bone marrow mesenchymal stem cells into neural lineage in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1014-1018. |
| [9] | Zhu Xuefen, Huang Cheng, Ding Jian, Dai Yongping, Liu Yuanbing, Le Lixiang, Wang Liangliang, Yang Jiandong. Mechanism of bone marrow mesenchymal stem cells differentiation into functional neurons induced by glial cell line derived neurotrophic factor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1019-1025. |
| [10] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [11] | Wang Shiqi, Zhang Jinsheng. Effects of Chinese medicine on proliferation, differentiation and aging of bone marrow mesenchymal stem cells regulating ischemia-hypoxia microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1129-1134. |
| [12] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [13] | Liu Xin, Yan Feihua, Hong Kunhao. Delaying cartilage degeneration by regulating the expression of aquaporins in rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 668-673. |
| [14] | Xie Chongxin, Zhang Lei. Comparison of knee degeneration after anterior cruciate ligament reconstruction with or without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 735-740. |
| [15] | Deng Zhenhan, Huang Yong, Xiao Lulu, Chen Yulin, Zhu Weimin, Lu Wei, Wang Daping. Role and application of bone morphogenetic proteins in articular cartilage regeneration [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 798-806. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||