Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (24): 3900-3905.doi: 10.3969/j.issn.2095-4344.2014.24.021
Previous Articles Next Articles
New progress of periodontal tissue engineering: problems and applications
Lu Bo-wen, Xu Lu-lu, Zhang Yang, Han Guang
- Department of Orthodontics, General Hospital of Chinese PLA, Beijing 100853, China
-
Revised:2014-05-15Online:2014-06-11Published:2014-06-11 -
Contact:Xu Lu-lu, M.D., Associate chief physician, Associate professor, Master’s supervisor, Department of Orthodontics, General Hospital of Chinese PLA, Beijing 100853, China -
About author:Lu Bo-wen, Studying for master’s degree, Department of Orthodontics, General Hospital of Chinese PLA, Beijing 100853, China -
Supported by:the National Natural Science Foundation of China, No. 81100776; Military Medical Science Research during the Twelfth Five-Year Plan, No. CWS11J118; Clinical Scientific Research Program of General Hospital of Chinese PLA, No. 2013FC-TSYS-2007
CLC Number:
Cite this article
Lu Bo-wen, Xu Lu-lu, Zhang Yang, Han Guang. New progress of periodontal tissue engineering: problems and applications[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(24): 3900-3905.
share this article
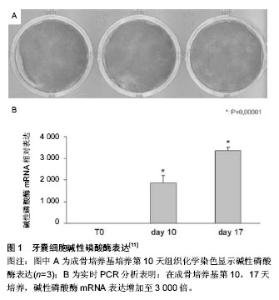
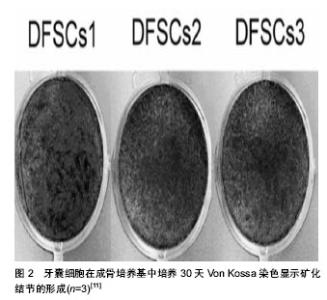
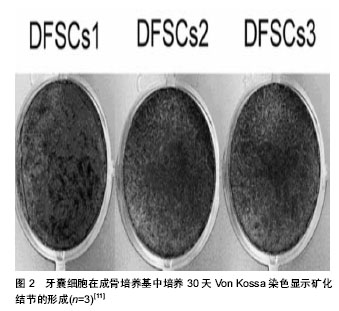
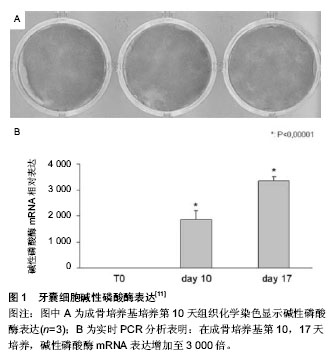
2.1 种子细胞 理想的种子细胞应该具备以下特点:便于取材,尽可能降低对机体的损伤;细胞增殖能力强;可塑性强;低免疫源性,无排斥反应;回植体内,对机体无毒性作用和致瘤性。 2.1.1 牙周膜干细胞 牙周膜干细胞是一组具有多向分化潜能的异质性多能干细胞,能向成纤维细胞、成骨细胞、成牙骨质细胞分化,进而形成牙周膜、牙槽骨和牙骨质,从而形成新的牙周附着结构。Gay等[1]将牙周膜干细胞和作为对照的骨髓基质干细胞在相同标准的条件下进行培养,通过向骨组织、软骨组织和脂肪组织分化的监测,结果表明,牙周膜干细胞和骨髓基质干细胞相比,具有明显分化为成骨细胞、软骨细胞和脂肪细胞的潜能。并且也证明了成熟的牙周膜干细胞群可以作为牙周组织再生的种子细胞。另外,也有大量的相关临床研究均证实牙周膜干细胞在牙周组织再生领域是非常具有应用前景的种子细胞之一[2-5]。 近期,Ji等[6]通过有限元稀释法将人的乳牙牙周膜干细胞分离、提纯,并在体内、外培养下和人的恒牙牙周膜干细胞进行比较后发现,体外培养下的人的乳牙牙周膜干细胞比人的恒牙牙周膜干细胞有更高的增殖率和更强的形成细胞群落的能力。而且,人的恒牙牙周膜干细胞和人的乳牙牙周膜干细胞相比,在碱性磷酸酶活性、矿化基质形成以及矿化相关基因表达包括RUNX2、碱性磷酸酶、Ⅰ型胶原、骨钙素等方面均有显著增强。由此表明乳牙牙周膜干细胞可以作为牙周组织工程的一种有希望的候选种子细胞。然而,牙周膜干细胞增殖分化再生的细胞数量少、自体获得困难等缺点尚不能满足临床的需要,还需深入的研究。 2.1.2 骨髓基质干细胞 骨髓基质干细胞来源丰富,取材简便,对机体的损伤小,具有较强的增殖能力和分化能力,这些多重优越性使其在临床上有较好的应用前景。最近,Li等[7]在5只比格犬口腔内手术形成骨缺损模型,然后分别将已转染人骨形态发生蛋白7基因的骨髓基质干细胞和未转染人骨形态发生蛋白7基因的骨髓基质干细胞在胶原蛋白膜培养后植入到骨缺损的模型中,术后12周观察结果显示,试验组在新骨形成上明显高于对照组,且已转染人骨形态发生蛋白7基因的骨髓基质干细胞比未转染人骨形态发生蛋白7基因的骨髓基质干细胞在新骨形成上也显著增强,表明骨髓基质干细胞可以用作修复牙周缺损的种子细胞。Zhou等[8]首先将骨保护素基因转染至骨髓基质干细胞,并用倒置相差显微镜和扫描电子显微镜观察在聚乳酸-羟基乙酸共聚物表面培养的经修饰的骨髓基质干细胞的细胞形态和增殖情况,结果显示,经骨保护素基因修饰过的骨髓基质干细胞能够在支架材料上大量增殖,且6周后新骨和牙骨质的形成量也明显的多于对照组,由此证明骨髓基质干细胞是修复牙周组织缺损的一种较为理想的种子细胞。 2.1.3 牙囊细胞 牙囊起源于神经嵴间叶细胞,是包绕于成釉器和牙乳头外周的疏松结缔组织。牙囊参与牙胚发育主要体现在其对于牙齿萌出、牙周组织形成及牙根形成具有重要作用。牙囊细胞是牙周组织的前体细胞,可以分化为成纤维细胞、成骨细胞和成牙骨质细胞,在牙发育后期可形成牙周膜、牙槽骨和牙本质,并已有学者成功分离和培养出具有多向分化潜能的牙囊细胞(dental follicle stem cells,DFSCs),同时证明可以形成牙周组织[9-11],牙囊细胞碱性磷酸酶表达及矿化结节形成见图1,2。 据Yang等[12]将携带SV40Tag基因的反转录病毒转染至SD大鼠的牙囊细胞中,通过对细胞形态、活性的观察以及对端粒酶活性、新骨生成及牙囊细胞扩增的分析,显示转染SV40Tag基因的牙囊细胞在体外可以稳定的培养60代左右且仍保持较好的生物学特性,说明牙囊细胞可以具备作为牙周组织工程种子细胞的条件。 Felthaus等[13]对信号分子和牙囊细胞迁徙之间的关系进行了研究,发现经骨形态发生蛋白2和转化生长因子β1处理过的牙囊细胞比经表皮生长因子处理过的细胞迁徙速度快,证明了骨形态发生蛋白2和转化生长因子β1是较好的细胞因子,进而对种子细胞成骨分化中最佳信号分子的选择具有提示作用。 最新研究显示,TRPM4在大鼠的牙囊细胞分化过程中对钙离子信号通道产生一定影响[14],表现在矿化作用和碱性磷酸酶活性均增强,由此说明了牙囊细胞在分化及成骨过程中信号传导的分子机制,特别是钙离子信号通道受到明显影响,从而对今后的种子细胞分化的分子机制研究具有一定指导意义。"
| [1] Gay IC,Chen S,MacDougall M, et al.Isolation and characterization of multipotent human periodontal ligament stem cells. Orthod Craniofac Res. 2007;10(3):149-160. [2] Wu C, Zhou Y, Lin C, et al.Strontium-containing mesoporous bioactive glass scaffolds with improved osteogenic/ cementogenic differentiation of periodontal ligament cells for periodontal tissue engineering. Acta Biomater. 2012;8(10): 3805-3815. [3] Liu Y, Zheng Y, Ding G, et al. Periodontal ligament stem cell-mediated treatment for periodontitis in miniature swine. Stem Cells. 2008;26(4):1065-1073. [4] Ding G, Liu Y, Wang W, et al. Allogeneic periodontal ligament stem cell therapy for periodontitis in swine. Stem Cells. 2010; 28(10):1829-1838. [5] Song DS, Park JC, Jung IH, et al. Enhanced adipogenic differentiation and reduced collagen synthesis induced by human periodontal ligament stem cells might underlie the negative effect of recombinant human bone morphogenetic protein-2 on periodontal regeneration. J Periodontal Res. 2011;46(2):193-203. [6] Ji K, Liu Y, Lu W, et al. Periodontal tissue engineering with stem cells from the periodontal ligament of human retained deciduous teeth. J Periodontal Res. 2013;48(1):105-116. [7] Li YF, Yan FH, Zhong Q, et al. Effect of hBMP-7 gene modified bone marrow stromal cells on periodontal tissue regeneration. Zhonghua Yi Xue Za Zhi. 2010;90(20): 1427-1430. [8] Zhou W, Zhao CH, Mei LX, et al. Effect of the compound of poly lactic-co-glycolic acid and bone marrow stromal cells modified by osteoprotegerin gene on the periodontal regeneration in Beagle dog periodontal defect. Hua Xi Kou Qiang Yi Xue Za Zhi. 2010;28(3):324-329. [9] Morsczeck CO, Dress J, Gosau M, et al. Lipopolysaccharide from Escherichia coli but not from Porphyromonas gingivalis induce pro-inflammatory cytokines and alkaline phosphatase in dental follicle cells. Arch Oral Biol. 2012;57(12):1595-1601. [10] Li C, Yang X, He Y, et al.Bone Morphogenetic Protein-9 Induces Osteogenic Differentiation of Rat Dental Follicle Stem Cells in P38 and ERK1/2 MAPK Dependent Manner. Int J Med Sci. 2012;9(10):862-871. [11] Mori G, Ballini A, Carbone C, et al. Osteogenic differentiation of dental follicle stem cells. Int J Med Sci. 2012;9(6):480-487. [12] Yang Z, Liu T, Zheng H, et al. The preliminary study on biological characteristics of the SD rat dental follicle cells infected with SV40Tag. Hua Xi Kou Qiang Yi Xue Za Zhi. 2013;31(1):4-7,12. [13] Felthaus O, Gosau M, Ettl T, et al. Migration of human dental follicle cells in vitro.J Periodontal Res. 2014;49(2):205-12. . [14] Nelson P, Ngoc-Tran T-D, et al. Transient receptor potential melastatin 4 channel controls calcium signals and dental follicle stem cell differentiation. Stem Cells. 2013;31(1): 167-177. [15] Tobita M, Mizuno H. Adipose-derived stem cells and platelet-rich plasma: the keys to functional periodontal tissue engineering. Curr Stem Cell Res Ther. 2013;8(5):400-406. [16] Inanç B, Elçin AE, Elçin YM, et al. In vitro differentiation and attachment of human embryonic stem cells on periodontal tooth root surfaces. Tissue Eng Part A. 2009;15(11): 3427-3435. [17] Chang PC, Dovban AS, Lim LP, et al. Dual delivery of PDGF and simvastatin to accelerate periodontal regeneration in vivo. Biomaterials. 2013;34(38):9990-9997. [18] Gruber R, Leimer M, Fischer MB, et al. Beta2-adrenergic receptor agonists reduce proliferation but not protein synthesis of periodontal fibroblasts stimulated with platelet-derived growth factor-BB. Arch Oral Biol. 2013;58(12): 1812-1817. [19] Soran Z. Chitosan scaffolds with BMP-6 loaded alginate microspheres for periodontal tissue engineering. J Microencapsul. 2012;29(8):770-780. [20] Hakki SS, Bozkurt B, Hakki EE, et al. Bone morphogenetic protein-2, -6, and -7 differently regulate osteogenic differentiation of human periodontal ligament stem cells. Acta Odontol Scand.2013;13(10):98-102. [21] Maeda H, Wada N, Tomokiyo A, et al. Prospective potency of TGF-β1 on maintenance and regeneration of periodontal tissue. Int Rev Cell Mol Biol. 2013;30(4):283-367. [22] Ochiai H, Okada S, Saito A,et al. Inhibition of insulin-like growth factor-1 (IGF-1) expression by prolonged transforming growth factor-β1 (TGF-β1) administration suppresses osteoblast differentiation. J Biol Chem. 2012;287(27): 22654-22661. [23] Shirakata Y, Takeuchi N. Effects of enamel matrix derivative and basic fibroblast growth factor with μ-tricalcium phosphate on periodontal regeneration in one-wall intrabony defects:an experimental study in dogs. Int J Periodontics Restorative Dent. 2013;33(5):641-649. [24] Santosh Kumar BB, Aruna DR, Gowda VS, et al. Clinical and radiographical evaluation of a bioresorbable collagen membrane of fish origin in the treatment of periodontal intrabony defects: A preliminary study. J Indian Soc Periodontol. 2013;17(5):624-630. [25] Shalumon KT, Sowmya S. Effect of incorporation of nanoscale bioactive glass and hydroxyapatite in PCL/chitosan nanofibers for bone and periodontal tissue engineering. J Biomed Nanotechnol. 2013;9(3):430-440. [26] Ge S, Zhao N, Wang L, et al. Bone repair by periodontal ligament stem cellseeded nanohydroxyapatite-chitosan scaffold. Int J Nanomedicine. 2012;7(5)405-414. [27] Mekala NK, Baadhe RR, Parcha SR, et al. Study on osteoblast like behavior of umbilical cord blood cells on various combinations of PLGA scaffolds prepared by salt fusion. Curr Stem Cell Res Ther. 2013;8(3):253-259. [28] Ge S, Zhao N, Wang L, et al. Effects of hydroxyapatite nanostructure on channel surface of porcine acellular dermal matrix scaffold on cell viability and osteogenic differentiation of human periodontal ligament stem cells. Int J Nanomedicine. 2013;8:1887-1895. [29] Stavropoulos A, Windisch P. Clinical and histologic evaluation of granular Beta-tricalcium phosphate for the treatment of human intrabony periodontal defects: a report on five cases. J Periodontol. 2010;81(2):325-334. [30] Saito A, Saito E, Kuboki Y, et al. Periodontal regeneration following application of basic fibroblast growth factor-2 in combination with beta tricalcium phosphate in class III furcation defects in dogs. Dent Mater J. 2013;32(2):256-262. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Lin Qingfan, Xie Yixin, Chen Wanqing, Ye Zhenzhong, Chen Youfang. Human placenta-derived mesenchymal stem cell conditioned medium can upregulate BeWo cell viability and zonula occludens expression under hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 4970-4975. |
| [3] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [4] | Shi Yangyang, Qin Yingfei, Wu Fuling, He Xiao, Zhang Xuejing. Pretreatment of placental mesenchymal stem cells to prevent bronchiolitis in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 991-995. |
| [5] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [6] | Fan Quanbao, Luo Huina, Wang Bingyun, Chen Shengfeng, Cui Lianxu, Jiang Wenkang, Zhao Mingming, Wang Jingjing, Luo Dongzhang, Chen Zhisheng, Bai Yinshan, Liu Canying, Zhang Hui. Biological characteristics of canine adipose-derived mesenchymal stem cells cultured in hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1002-1007. |
| [7] | Geng Yao, Yin Zhiliang, Li Xingping, Xiao Dongqin, Hou Weiguang. Role of hsa-miRNA-223-3p in regulating osteogenic differentiation of human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1008-1013. |
| [8] | Lun Zhigang, Jin Jing, Wang Tianyan, Li Aimin. Effect of peroxiredoxin 6 on proliferation and differentiation of bone marrow mesenchymal stem cells into neural lineage in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1014-1018. |
| [9] | Zhu Xuefen, Huang Cheng, Ding Jian, Dai Yongping, Liu Yuanbing, Le Lixiang, Wang Liangliang, Yang Jiandong. Mechanism of bone marrow mesenchymal stem cells differentiation into functional neurons induced by glial cell line derived neurotrophic factor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1019-1025. |
| [10] | Duan Liyun, Cao Xiaocang. Human placenta mesenchymal stem cells-derived extracellular vesicles regulate collagen deposition in intestinal mucosa of mice with colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1026-1031. |
| [11] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [12] | Wang Xianyao, Guan Yalin, Liu Zhongshan. Strategies for improving the therapeutic efficacy of mesenchymal stem cells in the treatment of nonhealing wounds [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1081-1087. |
| [13] | Wang Shiqi, Zhang Jinsheng. Effects of Chinese medicine on proliferation, differentiation and aging of bone marrow mesenchymal stem cells regulating ischemia-hypoxia microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1129-1134. |
| [14] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [15] | Zhang Mi, Wu Saixuan, Dong Ming, Lu Ying, Niu Weidong. Expression of interleukin-24 in a mouse model of periapical periodontitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 679-684. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||