Chinese Journal of Tissue Engineering Research
Previous Articles Next Articles
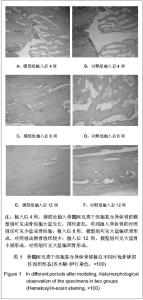
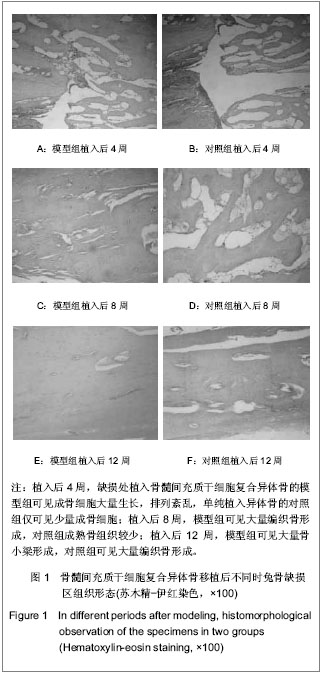
Bone marrow mesenchymal stem cells combined with allogeneic bone for cancellous bone defects
Wang Feng, Fu Zhi-hou
- Postgraduate Training Unit of Liaoning Medical University, General Hospital of Jinan Military Region, Jinan 250031, Shandong Province, China
-
Received:2013-03-15Revised:2013-04-18Online:2013-07-02Published:2013-07-02 -
Contact:Fu Zhi-hou, M.D., Chief physician, Professor, Master’s supervisor, Postgraduate Training Unit of Liaoning Medical University, General Hospital of Jinan Military Region, Jinan 250031, Shandong Province, China jzgbfzh@yahoo.com.cn -
About author:Wang Feng★ Studying for master’s degree, Postgraduate Training Unit of Liaoning Medical University, General Hospital of Jinan Military Region, Jinan 250031, Shandong Province, China medouni@163.com -
Supported by:the Postgraduate Foundation of Liaoning Medical University
CLC Number:
Cite this article
Wang Feng, Fu Zhi-hou. Bone marrow mesenchymal stem cells combined with allogeneic bone for cancellous bone defects[J]. Chinese Journal of Tissue Engineering Research, doi: 10.3969/j.issn.2095-4344.2013.27.004.
share this article
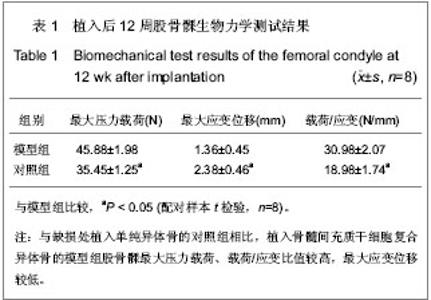
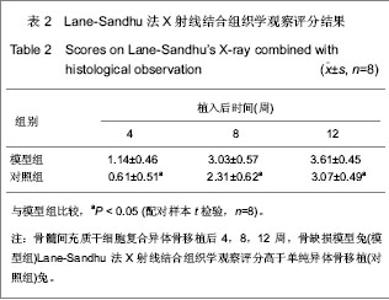
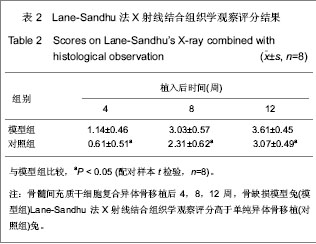
2.1 实验动物数量分析 纳入兔36只,其中2只兔因造模失败,后期1只兔子因感染死亡,1只取材失败,均直接剔除,未补充数量,最终32只兔计入结果分析。 2.2 骨髓间充质干细胞复合异体骨移植后松质骨缺损兔一般形态 植入后第1天,兔活动量与进食均较少。植入后第2天,兔均可恢复正常习性,饮食活动正常。兔切口初期略有红肿,稍有渗出,但后期切口均愈合良好。 股骨外髁表面观察:模型组与对照组股骨髁骨缺损处随时间变化,骨质形成均比较明显,逐步恢复平坦外观,植入后12周骨皮质均已修复。 股骨髁剖面观察:模型组:植入后4周,植入骨块之间明显粘连,但骨块之间较易分离,与周围骨质分界清晰;植入后8周,植入骨块间连接紧密,不易分离,与周围骨质界限变模糊;植入后12周,难以区分植入骨块与周围骨质,骨缺损基本修复。 对照组:植入后4周,植入骨块之间有少量粘连,植入骨块、骨床之间基本呈游离状态;植入后8 周,植入骨块明显粘连,但较容易剥离,与周围骨质分界清晰;植入后12周,植入骨块间级与周围骨质彼此粘连,分离困难,不易区分周围骨质与植入骨块。 2.3 骨髓间充质干细胞复合异体骨移植后松质骨缺损兔X射线检查结果 植入后4周,模型组骨缺损处密度高低不均,缺损区边缘模糊;对照组骨缺损处可见大量植入骨块高密度影,缺损区边缘清晰。植入后8周,模型组骨缺损处可见大量密度与周围骨质一致区域,缺损区域缩小,对照组骨缺损处植入骨块高密度影之外可见部分区域与周围骨质密度一致,缺损区域明显。植入后12周,模型组骨缺损处仍可见植入骨块高密度影,但大多区域基本与周围骨质一致,难以区分原缺损区域;对照组骨缺损处亦可见植入骨块高密度影,大量与周围骨质密度一致区域,但原缺损区域仍模糊可见。 2.4 骨髓间充质干细胞复合异体骨移植后松质骨缺损兔股骨髁生物力学指标变化 植入后12周,与对照组相比,模型组股骨髁最大压力载荷、载荷/应变比值较高确 (P < 0.05),最大应变位移较低(P < 0.05)。见表1。"
| [1] Niederauer GG, Lee DR, Sankaran S. Bone grafting in arthroscopy and sports medicine. sports Med Arthrosc. 2006; 14(3):163-168.[2] Garcia-Maya M, Anderson AA, Kendal CE, et al. Ligand concen-trafion is a driver of divergent signaling and pleiotropic cellular responses to FGF. J Cell Physiol. 2006;206(2):386-393.[3] 胡金龙,王静成,颜连启.组织工程学技术治疗骨缺损的最新研究进展[J].中国矫形外科杂志,2013,21(2):150-153.[4] Endres S, Kratz M. Gamma irradiation. An effective procedure for bone banks, but does it make sense from an osteobiological perspective. J Musculoskelet Neuronal Interact. 2009;9(1):25-31.[5] Dawn B, Bolli R. Adult bone marrow-derived cells: regenerative potential, plasticity, and tissuecommitment. Basic Res Cardiol. 2005;100(6):494-503.[6] Korda M, Blunn G, Phipps K, et al. Can mesenchymal stem cells survive under normal impaction force in revision total hip replacements? Tissue Eng. 2006;12(3):625-630.[7] The Ministry of Science and Technology of the People’s Republic of China. Guidance Suggestions for the Care and Use of Laboratory Animals. 2006-09-30.[8] Romanov YA, Darevskaya AN, Merzlikina NV, et al. Mesenchymalstem cells from human bone marrow and adipose tissue:isolation, characterization, and differentiation potentialities. Cell Technol Biol Med. 2005;140(1):138-143.[9] Yao J, Radin S, Reilly G, et al. Solution-mediated effect of bioactive glass in poly(lactic-coglyclic acid)-bioactive glass composites on osteogenesis of marrow stromal cells. J Biomed Mater Res A. 2005;75(4):794-801.[10] 付志厚,王爱民.假体与组织工程骨界面骨整合的生物学特征[J].中国组织工程研究与临床康复,2007,11(44):8852-8856.[11] 周健,戴尅戎,汤亭亭.BMSCs胶原刮膜对松质骨缺损的修复[J].上海第二医科大学学报,2004,24(8):627-631.[12] 窦强兵,孔荣,朱六龙,等.同种异体间充质干细胞复合纤维蛋白修复骨缺损[J].中国矫形外科杂志,2006,14(10):766-768.[13] Bostrom M, Lane JM, Tomin E, et al. Use of bone morphogenetic protein-2 in the rabbit ulnar nonunion model. Clin Orthop. 1996;327:272-282. [14] 刘阳,曹延林,朱立新,等.新型可注射性nHA/CS骨修复材料修复兔股骨髁骨缺损的X 线评估[J].中国矫形外科杂志,2011,19(17): 1472-1475.[15] 阳懿,赵承初,孙勇,等.两种骨修复材料修复兔颅骨骨缺损:X射线评估效果[J].中国组织工程研究与临床康复,2010,14(34): 6283-6286.[16] Khan SN, Cammisa FP, Sandhu HS, et al. The biology of bonegrafting. J Am Acad Orthop Surg. 2005;13(1):77-86.[17] 胡忠洲,孟凡丁,王韶进.颗粒骨打压植骨治疗全髋关节翻修中髋臼侧骨缺损[J].医学与哲学,2012,33(3):35-37.[18] Olivier V, Hivart P, Descamps M, et al. In vitro culture of large bone substitutes in a new bioreactor:importance of the flow direction. Biomed Mat. 2007;2(3):174-180.[19] 胥少汀,葛宝丰,许印坎.实用骨科学[M]. 3版.北京:人民军医出版社,2005.[20] Devine SM. Mesenehymal stem cells:will they have a role in the clinic. J Cell Biochem Suppl. 2002;38:73-79.[21] Niemeyer P, Kornacker M, Mehlhorn A, et al. Comparison of immunological properties of bone marrow stromal cells and adipose tissue-derived stem cells before and after osteogenic differentiation in vitro. Tissue Eng. 2007;13(1): 111-121.[22] Ohgushi H, Dohi Y, Tamai S, et al. Osteogenic differentiation of marrow stromal stem cells in porous hydroxyapatite ceramics. J Biomed Mater Res. 1993;27(11):1401-1407.[23] Matsushima A, Kotobuki N, Tadokoro M, et al. In vivo osteogenic capability of human mesenchymal cells cultured on hydroxyapatite and on beta-tricalcium phosphate. Artif Organs. 2009;33(6):474-481.[24] Park SH, Tofighi A, Wang X, et al. Calcium phosphate combination biomaterials as human mesenchymal stem cell delivery vehicles for bone repair. J Biomed Mater Res B Appl Biomater. 2011;97(2):235-244.[25] Mauney JR, Jaquiery C, Volloch V, et al. In vitro and in vivo evaluation of differentially demineralized cancellous bone scaffolds combined with human bone marrow stromal cells for tissue engineering. Biomaterials. 2005;26(16):3173- 3185.[26] Tsiridis E, Ali Z, Bhalla A, et al. In vitro proliferation and differentiation of human mesenchymal stem cells on hydroxyapatite versus human demineralised bone matrix with and without osteogenic protein-1. Expert Opin Biol Ther. 2009; 9(1):9-19.[27] Okamoto M, Dohi Y, Ohgushi H, et al. Influence of the porosity of hydroxyapatite ceramics on in vitro and in vivo bone formation by cultured rat bone marrow stromal cells. J Mater Sci Mater Med. 2006;17(4):327-336.[28] Hing KA, Revell PA, Smith N, et al. Effect of silicon level on rate, quality and progression of bone healing within silicate-substituted porous hydroxyapatite scaffolds. Biomaterials. 2006;27(29):5014-5026.[29] Hing KA, Wilson LF, Buckland T. Comparative performance of three ceramic bone graft substitutes. Spine J. 2007;7(4): 475-490.[30] Mankani MH, Kuznetsov SA, Wolfe RM, et al. In vivo bone formation by human bone marrow stromal cells: reconstruction of the mouse calvarium and mandible. Stem Cells. 2006;24(9):2140-2149.[31] Mankani MH, Kuznetsov SA, Shannon B, et al. Canine cranial reconstruction using autologous bone marrow stromal cells. Am J Pathol. 2006;168(2):542-550.[32] Quarto R, Mastrogiacomo M,Cancedda R, et al. Repair of large bone defects with the use of autologous bone marrow stromal cells. N Engl J Med. 2001;344(5):385-386.[33] Marcacci M, Kon E, Moukhachev V, et al. Stem cells associated with macroporous bioceramics for long bone repair: 6- to 7-year outcome of a pilot clinical study. Tissue Eng. 2007;13(5):947-955.[34] Bolland BJ, Partridge K, Tilley S, et al. Biological and mechanical enhancement of impacted allograft seeded with human bone marrow stromal cells: potential clinical role in impaction bone grafting. Regen Med. 2006;1(4):457-467.[35] Korda M, Blunn G, Goodship A, et al. Use of mesenchymal stem cells to enhance bone formation around revision hip replacements. J Orthop Res. 2008;26(6):880-885.[36] Casabona F, Martin I, Muraglia A, et al. Prefabricated engineered bone flaps: an experimental model of tissue reconstruction in plastic surgery. Plast Reconstr Surg. 1998; 101(3):577-581.[37] Mankani MH, Kuznetsov SA, Robey PG. Formation of hematopoietic territories and bone by transplanted human bone marrow stromal cells requires a critical cell density. Exp Hematol. 2007;35(6):995-1004.[38] 田志逢,秦书俭,张小玲,等.不同接种密度骨髓间充质干细胞/骨基质明胶复合体修复大鼠桡骨缺损[J].中国组织工程研究与临床康复,2010,14(49):9126-9130. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Zhang Xiumei, Zhai Yunkai, Zhao Jie, Zhao Meng. Research hotspots of organoid models in recent 10 years: a search in domestic and foreign databases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1249-1255. |
| [3] | Wang Zhengdong, Huang Na, Chen Jingxian, Zheng Zuobing, Hu Xinyu, Li Mei, Su Xiao, Su Xuesen, Yan Nan. Inhibitory effects of sodium butyrate on microglial activation and expression of inflammatory factors induced by fluorosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1075-1080. |
| [4] | Wang Xianyao, Guan Yalin, Liu Zhongshan. Strategies for improving the therapeutic efficacy of mesenchymal stem cells in the treatment of nonhealing wounds [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1081-1087. |
| [5] | Liao Chengcheng, An Jiaxing, Tan Zhangxue, Wang Qian, Liu Jianguo. Therapeutic target and application prospects of oral squamous cell carcinoma stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1096-1103. |
| [6] | Xie Wenjia, Xia Tianjiao, Zhou Qingyun, Liu Yujia, Gu Xiaoping. Role of microglia-mediated neuronal injury in neurodegenerative diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1109-1115. |
| [7] | Li Shanshan, Guo Xiaoxiao, You Ran, Yang Xiufen, Zhao Lu, Chen Xi, Wang Yanling. Photoreceptor cell replacement therapy for retinal degeneration diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1116-1121. |
| [8] | Jiao Hui, Zhang Yining, Song Yuqing, Lin Yu, Wang Xiuli. Advances in research and application of breast cancer organoids [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1122-1128. |
| [9] | Wang Shiqi, Zhang Jinsheng. Effects of Chinese medicine on proliferation, differentiation and aging of bone marrow mesenchymal stem cells regulating ischemia-hypoxia microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1129-1134. |
| [10] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [11] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [12] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [13] | Shi Yangyang, Qin Yingfei, Wu Fuling, He Xiao, Zhang Xuejing. Pretreatment of placental mesenchymal stem cells to prevent bronchiolitis in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 991-995. |
| [14] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [15] | Fan Quanbao, Luo Huina, Wang Bingyun, Chen Shengfeng, Cui Lianxu, Jiang Wenkang, Zhao Mingming, Wang Jingjing, Luo Dongzhang, Chen Zhisheng, Bai Yinshan, Liu Canying, Zhang Hui. Biological characteristics of canine adipose-derived mesenchymal stem cells cultured in hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1002-1007. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||