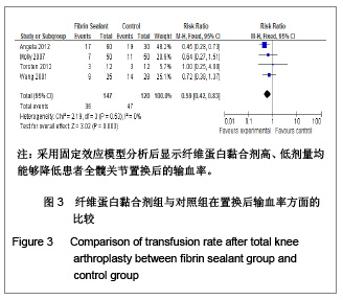
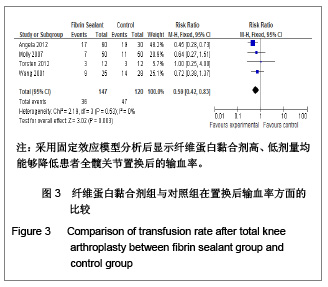
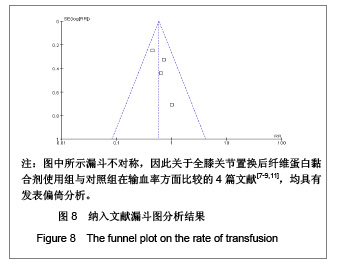
Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (13): 2399-2406.doi: 10.3969/j.issn.2095-4344.2013.13.017
Previous Articles Next Articles
Effectiveness of fibrin sealants in reducing blood drainage after total knee arthroplasty
Yang Li-yu, Wang Xing-li, Zhou Long, Xue Feng, Ba Gen, Fu Qin
- Department of Orthopedics, Shengjing Hospital of China Medical University, Shenyang 110004, Liaoning Province, China
-
Received:2012-11-27Revised:2012-12-12Online:2013-03-26Published:2013-03-26 -
Contact:Fu Qin, Professor, Doctoral supervisor, Chief physician, Department of Orthopedics, Shengjing Hospital of China Medical University, Shenyang 110004, Liaoning Province, China qinfucmu@hotmail.com -
About author:Yang Li-yu★, Studying for master’s degree, Department of Orthopedics, Shengjing Hospital of China Medical University, Shenyang 110004, Liaoning Province, China mark19871106@126.com
CLC Number:
Cite this article
Yang Li-yu, Wang Xing-li, Zhou Long, Xue Feng, Ba Gen, Fu Qin. Effectiveness of fibrin sealants in reducing blood drainage after total knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(13): 2399-2406.
share this article
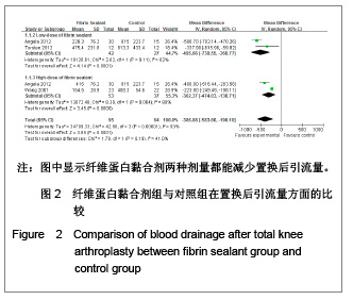
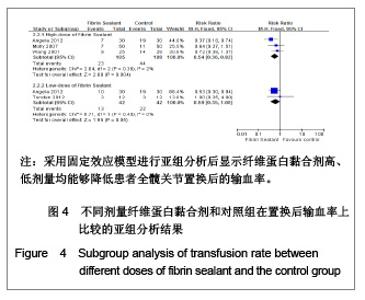
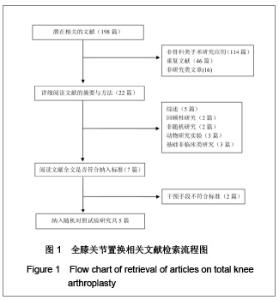
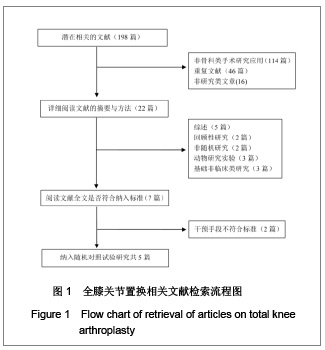
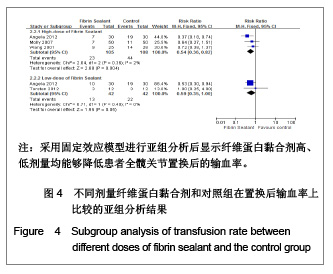
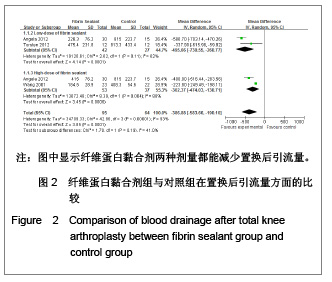
根据Cochrane 协作网提供的指导手册(5.1版),为了减少由于纤维蛋白黏合剂使用剂量的不同而造成的偏倚,实验进行了亚组分析,将10 mg及以上划为高剂量组,小于10 mg为低剂量组。其中1篇文献分别介绍了不同剂量纤维蛋白黏合剂止血效果的疗效[8],实验根据指导手册将这篇文献的对照组平均拆分为各15例,计数资料、计量资料分析均采用亚组分析的方式。由于相关并发症的内容没有具体叙述来自于何种剂量的患者,实验将采用了不同剂量的纤维蛋白黏合剂患者合并作为单一实验组进行分析。 2.3 Meta分析结果 置换后引流量:在5篇研究中,共有3个研究患者(159例)报告了置换后引流量[7-8, 11]。其他2个研究[9-10]置换后出血量是根据置换前置换后红细胞比容之差计算出来的,无直接观测值,未纳入分析之中。3篇文献分成高剂量与低剂量亚组分析,见图2。异质性分析可见高剂量组:χ2=35.58,P < 0.01,I2=97%;低剂量组:χ2=0.16,P=0.69,I2=0%,总异质性:χ2= 42.86,P < 0.01,I2=93%,异质性较大的采用随机效应模型。结果显示,高剂量组:SMD=-400.62,95%CI:-756.14- -45.10,Z=2.21,P=0.03;低剂量组WMD= -390.74,95%CI:-498.14- -283.33;低剂量组Z=7.13,P < 0.01。两组合并总效应量:WMD=-386.88,95%CI:-583.66- -190.10,Z=3.85,P < 0.01,说明两组都能减少置换后引流量。"
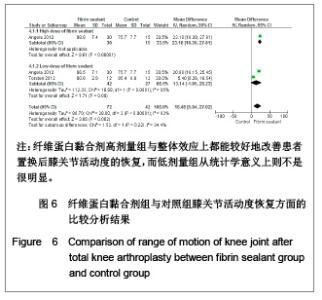
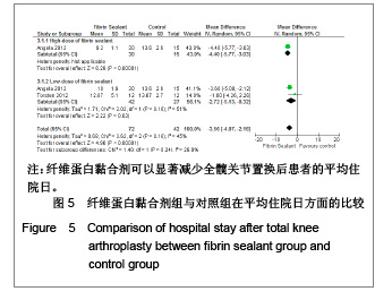
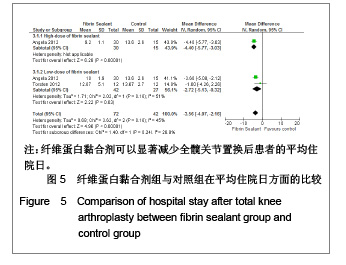
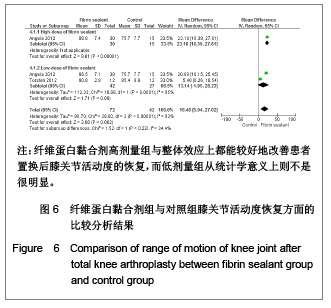
置换后膝关节活动度的恢复:有2篇文献(114例患者)报道了置换后膝关节活动恢复的相关数据[7-8]。低剂量组(χ2= 18.98,P < 0.01,I2=95%)与整体效应(χ2=28.60,P < 0.01,I2=93%)来看均存在较大异质性,见图6,故实验采用随机效应模型。从统计学上来看可见高剂量组与整体效应上都能较好地改善患者置换后膝关节活动度的恢复,而低剂量组的改善情况不明显(高剂量组:WMD=23.10,95%CI:18.39-27.81,Z=9.61,P < 0.01;低剂量组:WMD=13.14,95%CI:-1.95- 28.23,Z=1.71,P=0.09;整体效应:WMD=16.48,95%CI:5.94-27.02,Z=3.06,P < 0.01)。"
| [1] Lotke PA, Faralli VJ, Orenstein EM, et al. Blood loss after total knee replacement: effect of tourniquet release and continuous passive motion. J Bone Joint Surg Am. 1991;73(7):1037- 1040.[2] Jackson MR, MacPhee MJ, Drohan WN, et al. Fibrin sealant: current and potential clinical applications. Blood Coagul Fibrinolysis. 1996;7(8):737-746.[3] Radosevich M, Goubran HA, Burnouf T. Fibrin sealant: scientific rationale, production methods, properties, and current clinical use. Vox Sang. 1997;72(3):133-143.[4] Jadad AR, Moore RA, Carroll D, et al. Assessing the quality of reports of randomized clinical trials: is blinding necessary. Control Clin Trials. 1996;17(1):1-12.[5] Sabatini L, Trecci A, Imarisio D, et al. Fibrin tissue adhesive reduces postoperative blood loss in total knee arthroplasty. J Orthop Traumatol. 2012;13(3):145-151.[6] Levy O, Martinowitz U, Oran A, et al. The use of fibrin tissue adhesive to reduce blood loss and the need for blood transfusion after total knee arthroplasty. A prospective, randomized, multicenter study. J Bone Joint Surg Am.1999; 81(11):1580-1588.[7] Kluba T, Fiedler K, Kunze B, et al. Fibrin sealants in orthopaedic surgery: practical experiences derived from use of QUIXIL® in total knee arthroplasty. Arch Orthop Trauma Surg. 2012;132(8):1147-1152.[8] Notarnicola A, Moretti L, Martucci A, et al. Comparative efficacy of different doses of fibrin sealant to reduce bleeding after total knee arthroplasty. Blood Coagul Fibrinolysis. 2012; 23(4):278-284.[9] Molloy DO, Archbold HA, Ogonda L, et al. Comparison of topical fibrin spray and tranexamic acid on blood loss after total knee replacement: a prospective, randomised controlled trial. J Bone Joint Surg Br. 2007;89(3):306-309.[10] McConnell JS, Shewale S, Munro NA, et al. Reducing blood loss in primary knee arthroplasty: a prospective randomised controlled trial of tranexamic acid and fibrin spray. Knee. 2012;19(4):295-298.[11] Wang GJ, Hungerford DS, Savory CG, et al. Use of fibrin sealant to reduce bloody drainage and hemoglobin loss after total knee arthroplasty: a brief note on a randomized prospective trial. J Bone Joint Surg Am. 2001;83(10): 1503-1505.[12] Bierbaum BE, Callaghan JJ, Galante JO, et al. An analysis of blood management in patients having a total hip or knee arthroplasty. J Bone Joint Surg Am.1999;81(1):2-10.[13] Padala PR, Rouholamin E, Mehta RL. The role of drains andtourniquets in primary total knee replacement: a comparative study of TKR performed with drains and tourniquet versus no drains and adrenaline and saline infiltration. J Knee Surg. 2004;17(1):24-27.[14] Helm AT, Karski MT, Parsons SJ, et al. A strategy for reducing blood-transfusion requirements in elective orthopaedic surgery. Audit of an algorithm for arthroplasty of the lower limb. J Bone Joint Surg Br. 2003;85(4):484-489.[15] Lemaire R. Strategies for blood management in orthopaedic and trauma surgery. J Bone Joint Surg Br. 2008;90(9): 112-1136.[16] Goodnough LT, Shander A. Blood management. Arch Pathol Lab Med. 2007;131(5):695-701.[17] Rosencher N, Kerkkamp HE, Macheras G, et al. Orthopedic surgery transfusion hemoglobin european overview (OSTHEO) study: blood management in elective knee and hip arthroplasty in Europe. Transfusion. 2003;43(4):459-469.[18] Hill GE, Frawley WH, Griffith KE, et al. Allogeneic blood transfusion increases the risk of postoperative bacterial infection: a meta-analysis. J Trauma. 2003;54(5):908-914.[19] Everts PA, Devilee RJ, Oosterbos CJ, et al. Autologous platelet gel and fibrin sealant enhance the efficacy of total knee arthroplasty: improved range of motion, decreased length of stay and a reduced incidence of arthrofibrosis. Knee Surg Sports Traumatol Arthrosc. 2007;15(7):888-894.[20] Bernasek TL, Burris RB, Fujii H, et al. Effect on blood loss and cost-effectiveness of pain cocktails, platelet-rich plasma, or fibrin sealant after total knee arthroplasty. J Arthroplasty. 2012; 27(8):1448-1451.[21] Steuten L, Vallejo-Torres L, Bastide P, et al. Analysing uncertainty around costs of innovative medical technologies: the case of fibrin sealant (QUIXIL) for total knee replacement. Health Policy. 2009;89(1):46-57.[22] Thoms RJ, Marwin SE. The role of fibrin sealants in orthopaedic surgery. J Am Acad Orthop Surg. 2009;17(12): 727-736.[23] Alshryda S, Sarda P, Sukeik M, et al. Tranexamic acid in total knee replacement: a systematic review and meta-analysis. J Bone Joint Surg Br. 2011;93(12):1577-1585. |
| [1] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [2] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [3] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [4] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [5] | Wang Yongsheng, Wu Yang, Li Yanchun. Effect of acute high-intensity exercise on appetite hormones in adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1305-1312. |
| [6] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [7] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [8] | Li Yan, Wang Pei, Deng Donghuan, Yan Wei, Li Lei, Jiang Hongjiang. Electroacupuncture for pain control after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 957-963. |
| [9] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [10] | Hua Haotian, Zhao Wenyu, Zhang Lei, Bai Wenbo, Wang Xinwei. Meta-analysis of clinical efficacy and safety of antibiotic artificial bone in the treatment of chronic osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 970-976. |
| [11] | Zhan Fangbiao, Cheng Jun, Zou Xinsen, Long Jie, Xie Lizhong, Deng Qianrong. Intraoperative intravenous application of tranexamic acid reduces perioperative bleeding in multilevel posterior spinal surgery: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 977-984. |
| [12] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| [13] | Li Yang, Zhang Mingyong. Meta-analysis of the effect of double Endobutton and clavicular hook plate on the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 463-470. |
| [14] | Li Yanle, Yue Xiaohua, Wang Pei, Nie Weizhi, Zhang Junwei, Tan Yonghai, Jiang Hongjiang. Intramedullary nail fixation versus plate fixation in the treatment of displaced midshaft clavicular fractures in adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 471-476. |
| [15] | Liu Chang, Han Shufeng. Interlocking intramedullary nail for proximal femur versus proximal femoral anti-rotation intramedullary nail or proximal femoral anti-rotation intramedullary nail of Asian for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 477-485. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||