Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (3): 477-485.doi: 10.3969/j.issn.2095-4344.2989
Previous Articles Next Articles
Interlocking intramedullary nail for proximal femur versus proximal femoral anti-rotation intramedullary nail or proximal femoral anti-rotation intramedullary nail of Asian for intertrochanteric fractures in older adults: a meta-analysis
Liu Chang1, Han Shufeng2
- 1Shanxi Medical University, Taiyuan 030001, Shanxi Province, China; 2First Hospital of Shanxi Medical University, Taiyuan 030001, Shanxi Province, China
-
Received:2020-03-20Revised:2020-03-25Accepted:2020-04-27Online:2021-01-28Published:2020-11-19 -
Contact:Han Shufeng, Master, Professor, First Hospital of Shanxi Medical University, Taiyuan 030001, Shanxi Province, China -
About author:Liu Chang, Master, Shanxi Medical University, Taiyuan 030001, Shanxi Province, China
CLC Number:
Cite this article
Liu Chang, Han Shufeng. Interlocking intramedullary nail for proximal femur versus proximal femoral anti-rotation intramedullary nail or proximal femoral anti-rotation intramedullary nail of Asian for intertrochanteric fractures in older adults: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 477-485.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
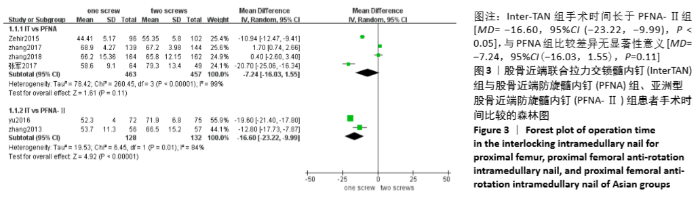
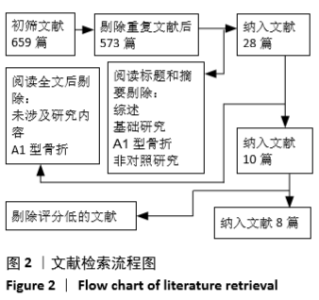
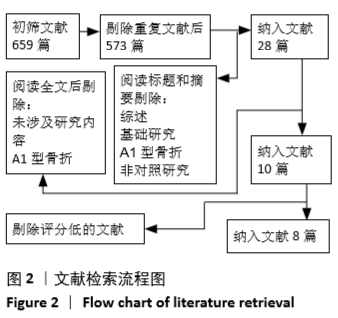
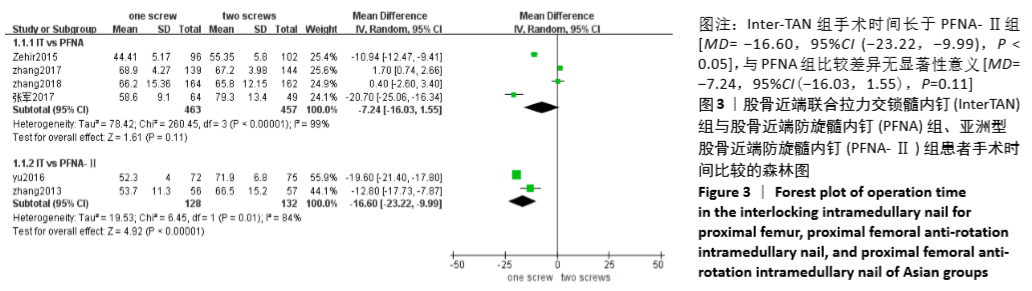
2.4 Meta分析结果 2.4.1 两组手术时间差异的Meta分析结果 6篇研究报道了手术时间的比较[6-11],其中Inter-TAN vs. PFNA内固定4篇[7,9-11],Inter-TAN组457例,PFNA组463例,文献间存在异质性(Chi2=260.45,df=3,P < 0.000 01,I2=99%),可以选择随机效应模型进行Meta分析;Inter-TAN vs. PFNA-Ⅱ内固定2篇[6,8],Inter-TAN组132例,PFNA-Ⅱ组128例,文献间存在异质性(Chi2=6.45,df=1,P=0.01,I2=84%),可以选择随机效应模型进行Meta分析。结果显示,Inter-TAN组手术时间长于PFNA-Ⅱ组[MD=-16.60,95%CI(-23.22,-9.99),P < 0.05],与PFNA组比较差异无显著性意义[MD=-7.24,95%CI (-16.03,1.55),P=0.11],见图3。"
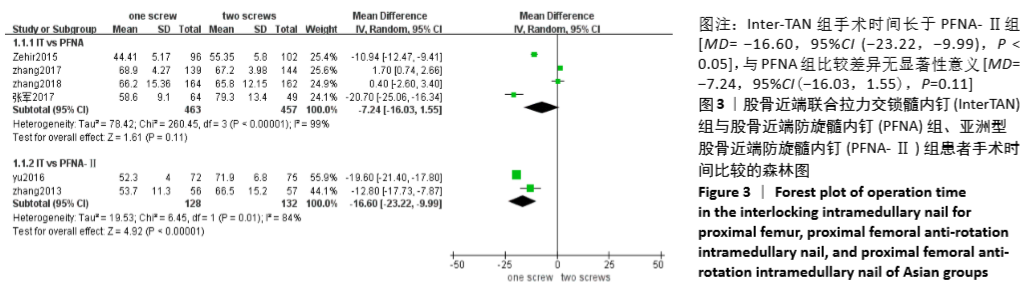
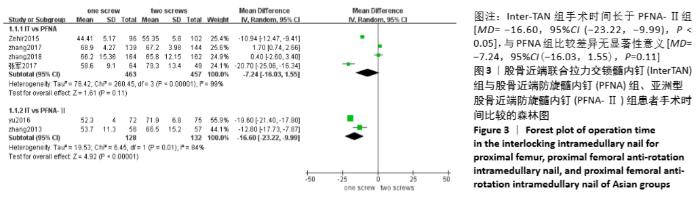
2.4 Meta分析结果 2.4.1 两组手术时间差异的Meta分析结果 6篇研究报道了手术时间的比较[6-11],其中Inter-TAN vs. PFNA内固定4篇[7,9-11],Inter-TAN组457例,PFNA组463例,文献间存在异质性(Chi2=260.45,df=3,P < 0.000 01,I2=99%),可以选择随机效应模型进行Meta分析;Inter-TAN vs. PFNA-Ⅱ内固定2篇[6,8],Inter-TAN组132例,PFNA-Ⅱ组128例,文献间存在异质性(Chi2=6.45,df=1,P=0.01,I2=84%),可以选择随机效应模型进行Meta分析。结果显示,Inter-TAN组手术时间长于PFNA-Ⅱ组[MD=-16.60,95%CI(-23.22,-9.99),P < 0.05],与PFNA组比较差异无显著性意义[MD=-7.24,95%CI (-16.03,1.55),P=0.11],见图3。"
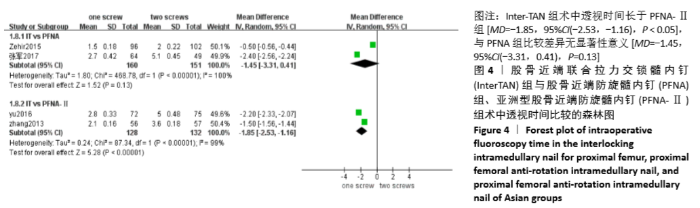
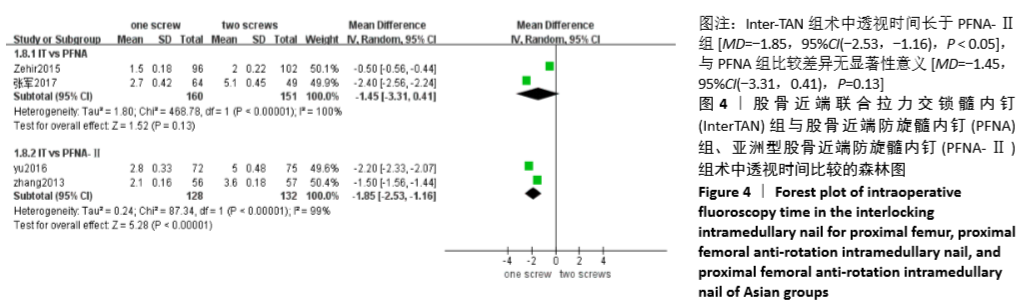
2.4.2 两组术中透视时间差异的Meta分析结果 4篇研究报道了术中透视时间的比较[6-8,11],其中Inter-TAN vs. PFNA内固定2篇[7,11],Inter-TAN组151例,PFNA组160例,文献间存在异质性(Chi2=468.78,df=1,P < 0.000 01,I2=100%),可以选择随机效应模型进行Meta分析;Inter-TAN vs. PFNA-Ⅱ内固定2篇[6,8],Inter-TAN组132例,PFNA-Ⅱ组128例,文献间存在异质性(Chi2=87.34,df=1,P < 0.000 01,I2=99%),可以选择随机效应模型进行Meta分析。结果显示,Inter-TAN组术中透视时间长于PFNA-Ⅱ组[MD= -1.85,95%CI(-2.53,-1.16),P < 0.05],与PFNA组比较差异无显著性意义[MD=-1.45,95%CI(-3.31,0.41),P=0.13],见图4。"
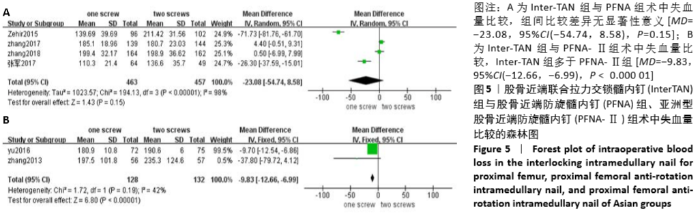
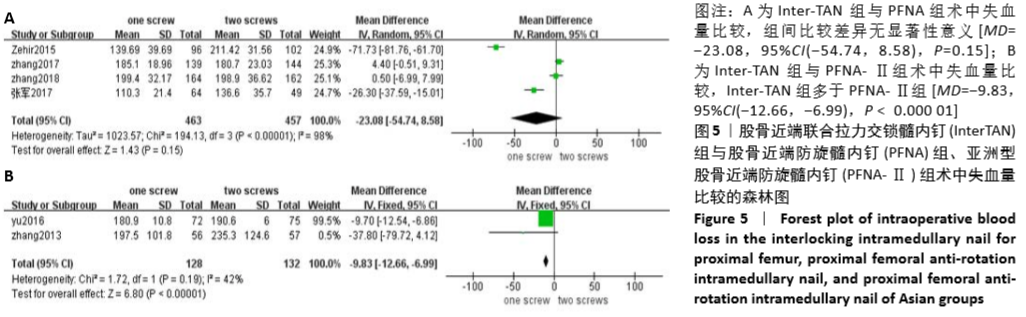
2.4.3 两组术中失血量差异的Meta 分析结果 6 篇研究报道了术中失血量的比较[6-11],其中Inter-TAN vs. PFNA 内固定4 篇[7,9-11],Inter-TAN组457 例,文献间存在异质性(Chi2=194.13,df=3,P < 0.000 01,I2=98%),可以选择随机效应模型进行Meta分析;Inter-TAN vs. PFNA-Ⅱ内固定2 篇[6,8],Inter-TAN组132例,文献间无明显异质性(Chi2=1.72,df=1,P=0.19,I2=42%),可以选择固定效应模型进行Meta 分析。结果显示,Inter-TAN 组术中失血量与PFNA组比较差异均无显著性意义[MD=-23.08,95%CI(-54.74,8.58),P=0.15],多于PFNA-Ⅱ组[MD= -9.83,95%CI(-12.66,-6.99),P < 0.000 01],见图5。"

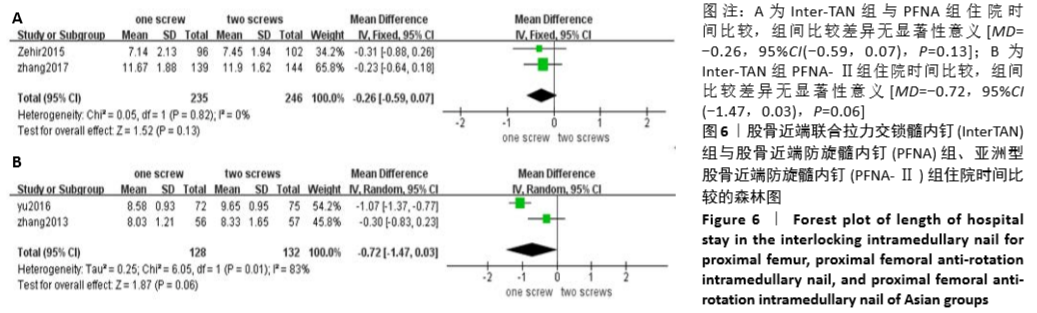
2.4.4 两组住院时间差异的Meta分析结果 4篇研究报道了住院时间的比较[6-9],其中Inter-TAN vs. PFNA内固定2 篇[7,9],Inter-TAN组246例,文献间无异质性(Chi2=0.05,df=1,P=0.82,I2=0%),可以选择固定效应模型进行Meta分析;Inter-TAN vs. PFNA-Ⅱ内固定2篇[6,8],Inter-TAN组132例,PFNA-Ⅱ组128例,文献间存在异质性(Chi2=6.05,df=1,P=0.01,I2=83%),可以选择随机效应模型进行Meta分析。结果显示,Inter-TAN住院时间与PFNA组、PFNA-Ⅱ组比较差异均无显著性意义[MD=-0.26,95%CI (-0.59,0.07),P=0.13;MD=-0.72,95%CI(-1.47,0.03),P=0.06],见图6。"
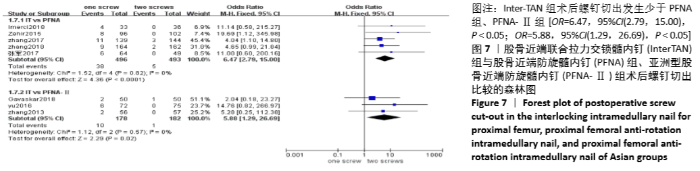
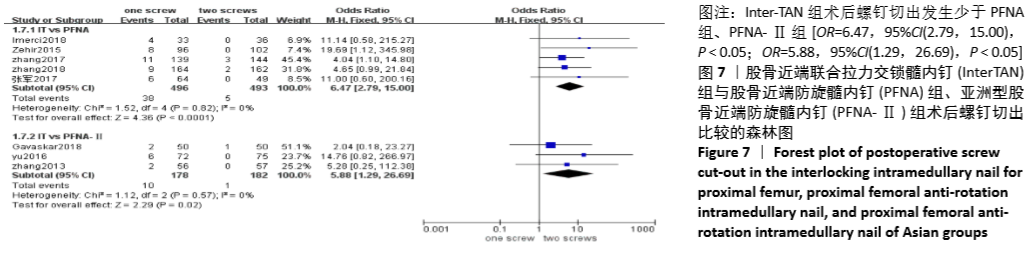
2.4.5 两组术后螺钉切出差异的Meta分析结果 8篇研究报道了术后螺钉切出的比较[4-11],其中Inter-TAN vs. PFNA内固定5篇[5,7,9-11],Inter-TAN组493例,PFNA组496例,文献间无异质性(Chi2=1.52,df=4,P=0.82,I2=0%),可以选择固定效应模型进行Meta分析;Inter-TAN vs. PFNA-Ⅱ内固定3篇[4,6,8],Inter-TAN组182例,PFNA-Ⅱ组178例,文献间无异质性(Chi2=1.12,df=2,P=0.57,I2=0%),可以选择固定效应模型进行Meta分析。结果显示,Inter-TAN组术后螺钉切出发生少于PFNA组、PFNA-Ⅱ组[OR=6.47,95%CI(2.79,15.00),P < 0.05;OR=5.88,95%CI(1.29,26.69),P < 0.05],见图7。"

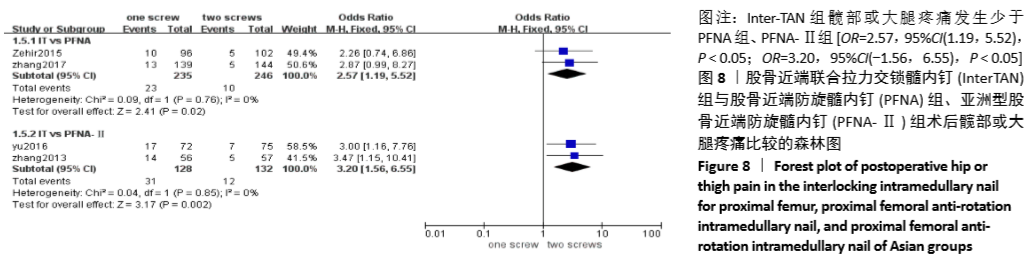
2.4.6 两组术后髋部或大腿疼痛差异的Meta分析结果 4篇研究比较了术后髋部或大腿疼痛[6-9],其中Inter-TAN vs. PFNA内固定2篇[7,9],Inter-TAN 组246例,PFNA组235例,文献间无异质性(Chi2=0.09,df=1,P=0.76,I2=0%),可以选择固定效应模型进行Meta分析;Inter-TAN vs. PFNA-Ⅱ内固定2篇[6,8],Inter-TAN组132例,PFNA-Ⅱ组128例,文献间无异质性(Chi2=0.04,df=1,P=0.85,I2=0%),可以选择固定效应模型进行Meta分析。结果显示,Inter-TAN组髋部或大腿疼痛发生少于PFNA组、PFNA-Ⅱ组[OR=2.57,95%CI(1.19,5.52),P < 0.05;OR=3.20,95%CI(-1.56,6.55),P < 0.05],见图8。"
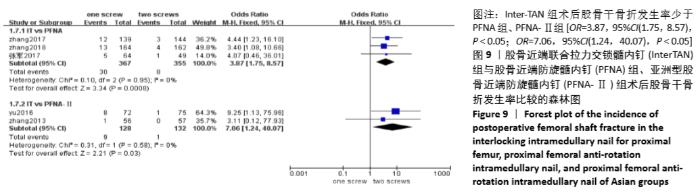
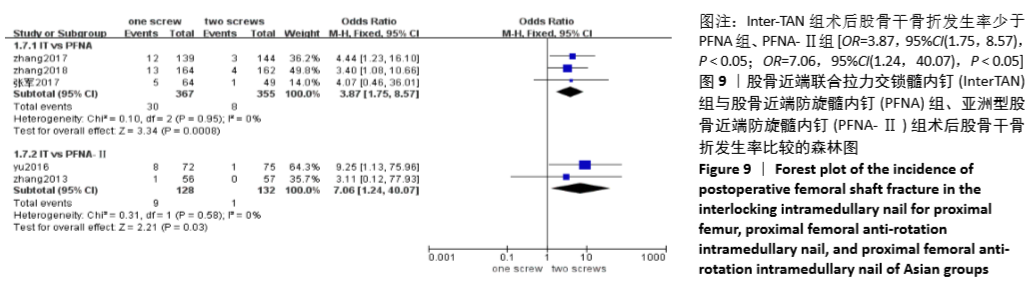
2.4.7 两组术后股骨干骨折发生率差异的Meta分析结果 5篇研究报道了术后股骨干骨折的比较[6,8-11],其中Inter-TAN vs. PFNA内固定3篇[9-11],Inter-TAN组355例,PFNA组367例,文献间无异质性(Chi2=0.10,df=2,P=0.95,I2=0%),可以选择固定效应模型进行Meta分析;Inter-TAN vs. PFNA-Ⅱ内固定2篇[6,8],Inter-TAN组132例,PFNA-Ⅱ组128例,文献间无异质性(Chi2=0.31,df=1,P=0.58,I2=0%),可以选择固定效应模型进行Meta分析。结果显示,Inter-TAN组术后股骨干骨折发生率少于PFNA组、PFNA-Ⅱ组[OR=3.87,95%CI(1.75,8.57),P < 0.05;OR=7.06,95%CI(1.24,40.07),P < 0.05],见图9。"
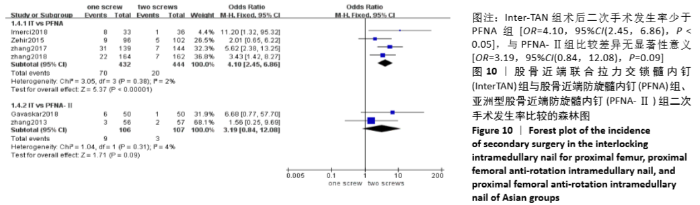
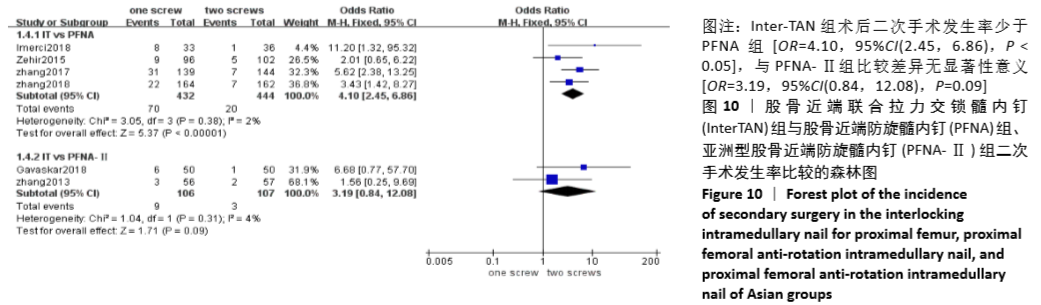
2.4.8 两组术后二次手术发生率差异的Meta分析结果 6篇研究报道了术后二次手术的比较[4-5,7-10],其中Inter-TAN vs. PFNA内固定4篇[5,7,9-10],Inter-TAN组444例,PFNA组432例,文献间无异质性(Chi2=3.05,df=3,P=0.38,I2=2%),可以选择固定效应模型进行Meta分析;Inter-TAN vs. PFNA-Ⅱ内固定2篇[4,8],Inter-TAN组107例,PFNA-Ⅱ组106例,文献间无异质性(Chi2=1.04,df=1,P=0.31,I2=4%),可以选择固定效应模型进行Meta分析。结果显示,Inter-TAN组术后二次手术发生率少于PFNA组[OR=4.10,95%CI(2.45,6.86),P < 0.05],与PFNA-Ⅱ组比较差异无显著性意义[OR=3.19,95%CI(0.84,12.08),P=0.09],见图10。"

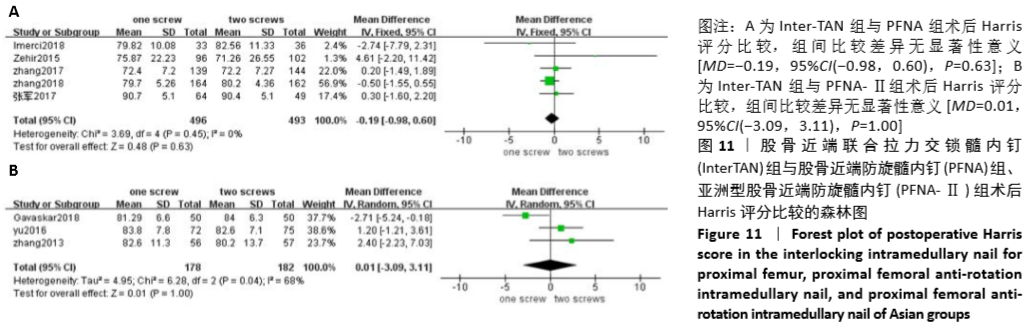
2.4.9 两组术后Harris 评分差异的Meta分析结果 8篇研究报道了术后Harris评分的比较[4-11],其中Inter-TAN vs. PFNA内固定5篇[5,7,9-11],Inter-TAN组493例,PFNA组496例,文献间无异质性(Chi2=3.69,df=4,P=0.45,I2=0%),可以选择固定效应模型进行Meta分析(结果无差异);Inter-TAN vs. PFNA-Ⅱ内固定3篇[4,6,8],Inter-TAN组182例,PFNA-Ⅱ组178例,文献间存在异质性(Chi2=6.28,df=2,P=0.04,I2=68%),可以选择随机效应模型进行Meta分析。结果显示,Inter-TAN组术后Harris评分与PFNA组、PFNA-Ⅱ组比较差异均无显著性意义[MD=-0.19,95%CI(-0.98,0.60),P=0.63;MD=0.01,95%CI(-3.09,3.11),P=1.00],见图11。"
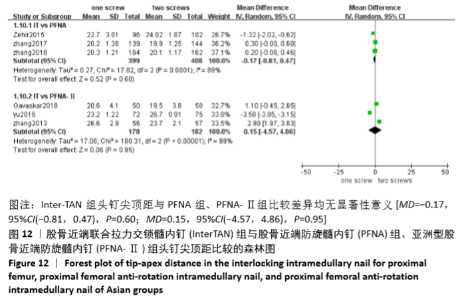
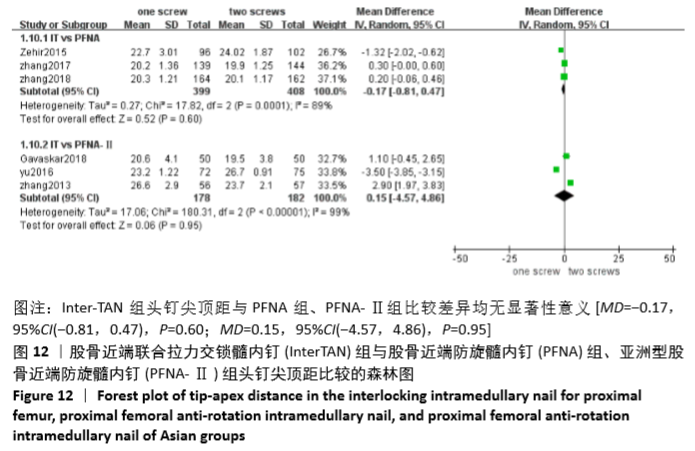
2.4.10 两组头钉尖顶距差异的Meta 分析结果 6 篇研究报道了头钉尖顶距的比较[4,6-10],其中Inter-TAN vs. PFNA内固定3 篇[7,9-10],Inter-TAN 组408 例,PFNA 组399 例,文献间存在异质性(Chi2=17.82,df=2,P < 0.05,I2=89%),可以选择随机效应模型进行Meta 分析;Inter-TANvs PFNA-Ⅱ内固定3 篇[4,6,8],Inter-TAN 组182 例,PFNA-Ⅱ组178 例,文献间存在异质性(Chi2=180.31,df=2,P < 0.05,I2=99%),可以选择随机效应模型进行Meta分析。结果显示,Inter-TAN 组头钉尖顶距与PFNA 组、PFNA-Ⅱ组比较差异均无显著性意义[MD=-0.17,95%CI(-0.81,0.47),P=0.60;MD=0.15,95%CI (-4.57,4.86),P=0.95],见图12。"
| [1] 高金华,王明洋,顾文浩,等.经皮撬拨复位PFNA内固定和股骨近端解剖锁定板内固定治疗老年不稳定股骨粗隆间骨折的疗效比较[J].中国骨与关节损伤杂志, 2017,32(6):619-620. [2] 唐佩福.股骨转子间骨折的治疗进展与策略[J].中华创伤骨科杂志,2017,19(2): 93-94. [3] 袁志,毕龙.老年股骨转子间骨折的治疗趋势[J].中华骨科杂志,2017,37(17): 1057-1060. [4] GAVASKAR AS, TUMMALA NC, SRINIVASAN P, et al.Helical blade or the integrated lag screws: a matched pair analysis of 100 patients with unstable trochanteric fractures.J Orthop Trauma.2018;32(6):274-277. [5] İMERCI A, AYDOGAN NH, TOSUN K. A comparison of the InterTan nail and proximal femoral fail antirotation in the treatment of reverse intertrochanteric femoral fractures. Acta Orthop Belg.2018; 84(2):123-131. [6] YU W, ZHANG X, ZHU X, et al. A retrospective analysis of the InterTan nail and proximal femoral nail anti-rotation-Asia in the treatment of unstable intertrochanteric femur fractures in the elderly.J Orthop Surg Res.2016;11:10. [7] ZEHIR S, ŞAHIN E, ZEHIR R. Comparison of clinical outcomes with three different intramedullary nailing devices in the treatment of unstable trochanteric fractures.Ulus Travma Acil Cerrahi Derg. 2015;21(6):469-476. [8] ZHANG S, ZHANG K, JIA Y, et al. InterTan nail versus Proximal Femoral Nail Antirotation-Asia in the treatment of unstable trochanteric fractures.Orthopedics. 2013; 36(3):e288-e294. [9] ZHANG H, ZHU X, PEI G, et al. A retrospective analysis of the InterTan nail and proximal femoral nail anti-rotation in the treatment of intertrochanteric fractures in elderly patients with osteoporosis:a minimum follow-up of 3 years.J Orthop Surg Res.2017;12(1):147. [10] ZHANG C, XU B, LIANG G, et al. Optimizing stability in AO/OTA 31-A2 intertrochanteric fracture fixation in older patients with osteoporosis.J Int Med Res.2018;46(5):1767-1778. [11] 张军,曹烈虎,陈晓,等.PFNA与InterTAN髓内钉治疗不稳定股骨粗隆间骨折疗效的比较[J].中国骨伤, 2017, 30(7):597-601. [12] 张保中,邱贵兴.高龄股骨转子间骨折的手术治疗[J].中华创伤杂志,2005, 21(8):582-584. [13] SCHIPPER IB, MARTI RK, VAN DER WERKEN C. Unstable trochanteric femoral fractures: extramedullary or intramedullary fixation.Review of literature.Injury.2004;35(2):142-151. [14] ROBERTS KC, BROX WT, JEVSEVAR DS, et al. Management of hip fractures in the elderly. J Am Acad Orthop Surg. 2015; 23(2):131-137. [15] PALM H, JACOBSEN S, SONNE-HOLM S, et al. Integrity of the lateral femoral wall in intertrochanteric hip fractures: an important predictor of a reoperation.J Bone Joint Surg Am.2007;89(3):470-475. [16] IRGIT K, RICHARD RD, BEEBE MJ, et al. Reverse Oblique and Transverse Intertrochanteric Femoral Fractures Treated With the Long Cephalomedullary Nail.J Orthop Trauma. 2015;29(9):e299-e304. [17] 俞光荣,王树青,饶志涛,等.防旋股骨近端髓内钉治疗不稳定性转子间骨折33例[J].中华创伤杂志,2007,23(2):83-86. [18] 郝有亮,张志山,周方,等.股骨近端防旋髓内钉固定治疗股骨反转子间骨折内固定失败的危险因素分析[J].中华创伤骨科杂志,2019,21(9):771-776. [19] 焦竞,熊元,王俊文,等.亚洲型股骨近端防旋髓内钉固定治疗股骨转子间骨折术后大腿痛的原因分析[J].中华创伤骨科杂志,2017,19(8):685-690. [20] HOFFMANN S, PAETZOLD R, STEPHAN D, et al. Biomechanical evaluation of interlocking lag screw design in intramedullary nailing of unstable pertrochanteric fractures.J Orthop Trauma.2013;27(9):483-490. [21] NÜCHTERN JV, RUECKER AH, SELLENSCHLOH K, et al. Malpositioning of the lag screws by 1- or 2-screw nailing systems for pertrochanteric femoral fractures:a biomechanical comparison of gamma 3 and intertan.J Orthop Trauma. 2014;28(5):276-282. [22] 高翔,李杰,姜勇,等.InterTAN 髓内钉治疗股骨转子间骨折术中主钉置入困难的原因分析[J].中华创伤骨科杂志, 2015,17(11):962-966. [23] 应霁翀,刘观燚,张勇,等.三种不同内固定方式治疗股骨转子间骨折术后隐性失血及血栓形成的比较[J].中华创伤骨科杂志,2016,18(5):442-446. [24] 杜力,沈玉春,肖海军.股骨转子间骨折股骨近端防旋髓内钉内固定术后螺旋刀片向内穿透股骨头一例[J].中国修复重建外科杂志,2019,33(10):1275-1276. [25] FREI HC, HOTZ T, CADOSCH D,et al.Central head perforation,or”cut through,” caused by the helical blade of the proximal femoral nail antirotation.J Orthop Trauma. 2012;26(8):e102-e107. [26] GOFFIN JM, PANKAJ P, SIMPSON AH,et al. Does bone compaction around the helical blade of a proximal femoral nail anti-rotation (PFNA) decrease the risk of cut-out?:A subject-specific computational study.Bone Joint Res.2013;2(5):79-83. [27] 余新平,刘康,何智勇,等.InterTan髓内钉治疗426例老年股骨转子间骨折的临床疗效及体会[J].创伤外科杂志,2017, 19(5):370-374. [28] SEYHAN M, TURKMEN I, UNAY K, et al. Do PFNA devices and Intertan nails both have the same effects in the treatment of trochanteric fractures? A prospective clinical study. J Orthop Sci.2015;20(6): 1053-1061. [29] 纪方,刘培钊,佟大可.股骨转子间骨折热点问题的探讨[J].中国骨伤,2017, 30(7):587-590. [30] 曹立,沈惠良,雍宜民.影响双拉力螺钉股骨近端髓内钉切出股骨头的因素[J].中国骨与关节损伤杂志,2008,23(3):177-179. [31] 肖湘,张铁良,马宝通.“尖顶距”值与拉力螺钉切出股骨头关系的临床回顾性研究[J].中华创伤骨科杂志,2006,8(8): 722-724. [32] KASHIGAR A, VINCENT A, GUNTON MJ, et al. Predictors of failure for cephalomedullary nailing of proximal femoral fractures.Bone Joint J.2014;96-B(8):1029-1034. [33] RUBIO-AVILA J, MADDEN K, SIMUNOVIC N, et al. Tip to apex distance in femoral intertrochanteric fractures:a systematic review.J Orthop Sci.2013;18(4):592-598. [34] 杨家赵,方诗元,夏睿,等.TAD值在INTERTAN髓内钉治疗骨质疏松性股骨粗隆间骨折中的应用价值[J].中国骨质疏松杂志,2012,18(12):1101-1104. [35] LENZ M, SCHWINN J, HOFMANN-FLIRI L, et al.Influence of reduced tip-apex distance on helical blade fixation-a biomechanical study.J Orthop Res.2019;37(3):649-654. [36] MCCONNELL T, TORNETTA P, BENSON E, et al. Gluteus medius tendon injury during reaming for gamma nail insertion.Clin Orthop Relat Res.2003;(407):199-202. [37] PU JS, LIU L, WANG GL, et al. Results of the proximal femoral nail anti-rotation (PFNA) in elderly Chinese patients.Int Orthop.2009;33(5):1441-1444. [38] LV C, FANG Y, LIU L, et al. The new proximal femoral nail antirotation-Asia:early results.Orthopedics.2011;34(5):351. [39] 郑颖捷,李开南.股骨转子间骨折外侧壁的研究进展[J].中华创伤骨科杂志,2017, 19(2):133-137. [40] NORRIS R, BHATTACHARJEE D, PARKER MJ. Occurrence of secondary fracture around intramedullary nails used for trochanteric hip fractures: a systematic review of 13,568 patients.Injury.2012;43(6):706-711. [41] HOU Z, BOWEN TR, IRGIT KS, et al. Treatment of pertrochanteric fractures (OTA 31-A1 and A2):long versus short cephalomedullary nailing.J Orthop Trauma. 2013;27(6):318-324. [42] 张世民,余斌.AO/OTA-2018版股骨转子间骨折分类的解读与讨论[J].中华创伤骨科杂志, 2018,20(7):583-587. |
| [1] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [2] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [3] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [4] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [5] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [6] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [7] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [8] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [9] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [10] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [11] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [12] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [13] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [14] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [15] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||