Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (30): 4888-4893.doi: 10.3969/j.issn.2095-4344.0990
Previous Articles Next Articles
Mechanisms of staurosporine intervention in tissue-engineered self-assembly construct contraction of the temporomandibular joint disc
Luo Yin-yue1, 2, Li Hong-yan1, Bao Guang-jie1, 2, 3, Kang Hong1
- 1Institute of Stomatology, Lanzhou University, Lanzhou 730000, Gansu Province, China; 2Key Lab of Stomatology of State Ethnic Affairs Commission, Northwest University for Nationalities, Lanzhou 730030, Gansu Province, China; 3Key Laboratory of Oral Diseases of Gansu Province, Northwest University for Nationalities, Lanzhou 730030, Gansu Province, China
-
Received:2018-05-26Online:2018-10-28Published:2018-10-28 -
Contact:Bao Guang-jie, Professor, Master’s supervisor, Institute of Stomatology, Lanzhou University, Lanzhou 730000, Gansu Province, China; Key Lab of Stomatology of State Ethnic Affairs Commission, Northwest University for Nationalities, Lanzhou 730030, Gansu Province, China; Key Laboratory of Oral Diseases of Gansu Province, Northwest University for Nationalities, Lanzhou 730030, Gansu Province, China -
About author:Luo Yin-yue, Master candidate, Institute of Stomatology, Lanzhou University, Lanzhou 730000, Gansu Province, China; Key Lab of Stomatology of State Ethnic Affairs Commission, Northwest University for Nationalities, Lanzhou 730030, Gansu Province, China -
Supported by:the National Natural Science Foundation of China, No. 81660189; the Fundamental Research Funds for the Central Universities, No. 2yp2015014
CLC Number:
Cite this article
Luo Yin-yue, Li Hong-yan, Bao Guang-jie, Kang Hong. Mechanisms of staurosporine intervention in tissue-engineered self-assembly construct contraction of the temporomandibular joint disc[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(30): 4888-4893.
share this article
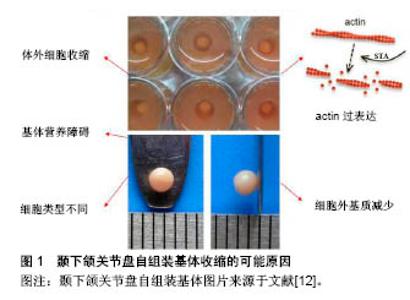
2.1 组织工程化颞下颌关节盘概述及自组装技术 2.1.1 颞下颌关节盘细胞 颞下颌关节盘并不是由单一种类的细胞构成,不同物种关节盘细胞类型相同,但各细胞数量比例却不尽相同。根据细胞形态学分类普遍认为颞下颌关节盘主要由纤维样细胞和软骨样细胞构成,以下简称“纤维软骨样细胞”,其中纤维样细胞占大多数[9]。 颞下颌关节盘不同区域的生化含量及细胞密度各不相同。关节盘主要由胶原、蛋白多糖、水等构成。其中胶原指大多数的Ⅰ型胶原和少量的Ⅱ型胶原。Ⅰ型胶原主要分布在纤维样细胞中,硫酸肤质蛋白多糖聚集周围;Ⅱ型胶原主要分布在软骨样细胞中,硫酸软骨素(氨基多糖的主要成分)包绕周围。 2.1.2 传统颞下颌关节盘组织工程 因为颞下颌关节盘中间带无血管分布,自愈能力差,故破损后无法修复,至今尚无理想的方法治疗颞下颌关节盘穿孔或退变。利用组织工程化关节盘替换破损的原生关节盘是一条有效途径,信号因子、细胞源和支架材料是颞下颌关节盘传统组织工程必不可少的要素。 但是传统的颞下颌关节盘组织工程因细胞源不足、机械性能不佳、细胞外基质少、降解产物的高细胞毒性、细胞表型发生改变等一系列问题困扰着科学家们[10-11]。 2.1.3 自组装技术在软骨、关节盘组织工程中的应用及存在问题 自组装技术在组织工程中的成功运用为研究者们提供了新的思路。但随着培养时间变长,颞下颌关节盘自组装基体体积逐渐收缩减小,这也是目前该项研究中遇到的瓶颈问题,发现主要与肌动蛋白骨架相关。 课题组利用琼脂糖井构造3D培养环境培养高密度的山羊颞下颌关节盘细胞,一段时间后发现自组装基体产生的细胞外基质与原生关节盘极其相似,说明3D无支架培养颞下颌关节盘的方法有其可行性[12],但在2周内颞下颌关节盘自组装基体直径只有同等条件下Hoben等培养软骨细胞自组装基体直径的1/4,这一现象说明了颞下颌关节盘自组装基体在体外培养时发生了收缩。此外,课题组Kang等[13]发现颞下颌关节盘自组装基体在培养第24小时后开始收缩,1周后收缩趋于稳定,基体直径最大约为2 mm,远小于原生关节盘,基体肌动蛋白表达大幅度增多,这提示基体的收缩与肌动蛋白过表达相关。国外学者Hinz等[14]也发现并支持“自组装基体体积收缩与肌动蛋白的过表达有关”这一观点。 除了肌动蛋白高表达之外,细胞是基体收缩的根源问题,因此依赖体外非收缩细胞或体内宿主细胞产生充足的细胞外基质减少收缩[15]。在自组装纤维细胞组织工程中,在最初的25 min,基体体积收缩至其原始体积的35%,几小时后降至9%[16],与软骨细胞相比,纤维细胞自组装基体发生更大幅度收缩。上文已叙述颞下颌关节盘由纤维样细胞和软骨样细胞组成,纤维样细胞含有大量肌动蛋白,而软骨样细胞肌动蛋白的表达却较少[17],相同时间内软骨细胞自组装基体直径是颞下颌关节盘的几倍,基体收缩与细胞类型相关。细胞外基质减少和颞下颌关节盘自组装基体内部营养缺乏,可能是基体收缩的又一原因[18](图1)。 "
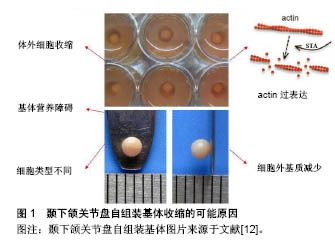
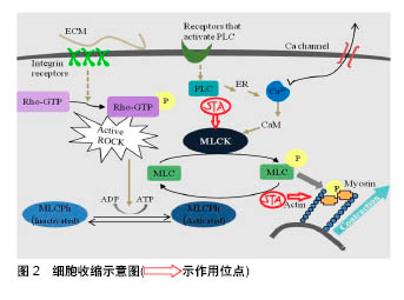
2.2 星孢菌素及其抑制细胞收缩的机制 星孢菌素可抑制肌动蛋白骨架收缩。星孢菌素(也称为抗生素AM-2282)最初是从链霉菌中分离的天然生物碱[19],作为广谱激酶抑制剂主要被用于抗肿瘤[20-25]、诱导凋亡研究中[26-28],如与表柔比星联合用于乳腺癌的化疗并取得了一定的疗效[29],通过Omi/HtrA2抑制PI3K/Akt信号传导途径诱导人肝癌细胞发生凋亡[30],通过Cyr1和PKA信号传导途径诱导白色念珠菌产生丝状体[20]。该药被注射入晶状体后,对视网膜疾病如青光眼具有良好的治疗效果[26,31]。此外,该药物还有有松弛平滑肌、细胞毒性和调节eNOS基因表达[32]、诱导细胞凋亡(如人神经母细胞瘤细胞系[33]、人角膜细胞和鸡胚胎神经元细胞[33-34])等作用。 星孢菌素抑制纤维细胞收缩的机制大致如下,即细胞收缩主要由肌动蛋白和肌球蛋白形成横桥后介导。肌球蛋白轻链激酶(MLCK)是平滑肌细胞收缩关键的调节蛋白[54]。肌球蛋白轻链的磷酸化会诱发肌动蛋白和肌球蛋白分子之间的相互作用。MLCK与肌球蛋白轻链磷酸酶(MLCPh)之间的平衡决定肌球蛋白轻链(MLC)的磷酸化。 细胞收缩根据Ca2+是否参与分为两种,一种是细胞通过黏附位点与微环境间的相互作用会活化Rho-GTP酶。活化的Rho-GTP激酶会抑制肌球蛋白磷酸酶的活性,MLCK与MLCPh的平衡被打破,促使MLC磷酸化,近而引起肌动蛋白和肌球蛋白横桥磷酸化,细胞收缩。另一种是细胞受外界刺激后,细胞膜上Ca2+通道打开,膜外Ca2+内流,膜内Ca2+浓度升高,Ca2+与螯合物M结合形成CaM,CaM作用于MLCK,那么MLCK与 MLCPh的平衡被打破,MLC磷酸化,激活肌动蛋白,横桥形成,肌丝滑动,细胞收缩。有学者验证了这一观点即Ca2+与钙调蛋白结合后激活MLCK,近而MLCK使肌球蛋白链(MLC20)上第19位的丝氨酸磷酸化,导致激活肌球蛋白头部的Mg2+-ATP酶(简称ATP酶),该酶水解ATP产生能量,使肌球蛋白与肌动蛋白相互作用,肌丝滑动,引发肌肉收缩[35](图2)。"
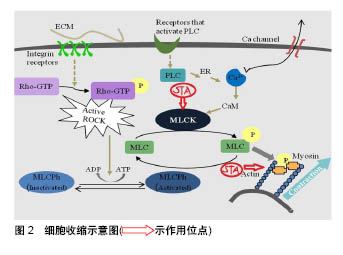

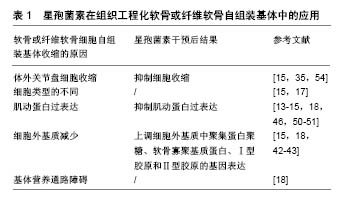
星孢菌素代替ATP与激酶的ATP结合域相互作用,缺少ATP的激酶无法发挥功能,如图1肌动蛋白、肌球蛋白不能被磷酸化,细胞收缩被抑制。这就解释了为什么星孢菌素及类似物(糖基与吲哚咔唑核心双连接)的抑制活性缺乏选择性(表1)。 2.3 关节盘细胞外基质的体外研究 颞下颌关节盘由关节盘细胞和细胞外基质组成。细胞外基质由细胞合成并分泌到胞外分布于细胞表面或细胞-细胞之间的大分子。细胞外基质不属于任何细胞,但它是组织的一部分,它决定结缔组织的特性,对细胞具有重要作用。 2.3.1 细胞外基质的组成及功能 绝大多数哺乳动物细胞-细胞间存在成分复杂的细胞外基质。细胞外基质由3类成分组成:①专一蛋白:如纤维蛋白等;②结构蛋白:如胶原蛋白(如Ⅰ型胶原、Ⅱ型胶原)、弹性蛋白等;③蛋白多糖(如氨基多糖)。已知细胞的运动、形态及分化均与细胞外基质有关。细胞外基质可以结合许多生长刺激因子和激素,给细胞提供信号,调节细胞功能。在急、慢性感染性炎症期,细胞外基质的生化成分发生改变。许多关节盘退变所导致的关节疾病均与细胞外基质的减少相关,并且自组装基体体积的减少也与之有密切联系。 2.3.2 Ⅰ型胶原和Ⅱ型胶原 颞下颌关节盘主要含Ⅰ型胶原和少量的Ⅱ、Ⅲ、 Ⅵ、Ⅸ、Ⅷ型胶原,胶原使关节盘富有弹性。Ⅰ型胶原前、后带含量比中间带 多[36-37]。Lin等[37-38]发现在狒和猴子的关节盘中Ⅱ型胶原镶嵌在Ⅰ型胶原纤维束间隙和细胞周围的细胞外基质中。胶原纤维在关节盘中有两种排列方式,围绕关节盘四周呈环形排列或通过其中间带呈竖形排列,不同的排列方式有助于维持颞下颌关节盘的结构与功能[39]。 2.3.3 氨基多糖和聚集蛋白聚糖 颞下颌关节盘细胞外基质主要由蛋白多糖及胶原组成。氨基多糖占蛋白多糖相对分子质量90%以上,是其决定性功能基团。氨基多糖的主要成分是硫酸角质素和硫酸软骨素,氨基多糖的分泌常作为测定蛋白多糖代谢的指标。聚集蛋白聚糖归属于蛋白多糖,是透明质酸中的一种[40],它使组织具有抵抗外界压力、吸收和分散负荷的能力。聚集蛋白聚糖丢失往往被认为是骨关节炎早期主要表现,在骨关节炎患者的软骨和关节液中,聚集蛋白聚糖核心蛋白特定位点断裂产生的碎片可被检测到。人椎间盘髓核中蛋白多糖特别是聚集蛋白聚糖的减少,被认为是椎间盘退变的重要标志[6]。 2.3.4 星孢菌素对关节盘细胞外基质的影响 星孢菌素可上调软骨或纤维软骨细胞细胞外基质的表达。细胞外基质对维持细胞表型具有重要作用。关节盘细胞在传代过程中(尤其是第4代以后)发生去分化现象,细胞骨架蛋白、细胞表型均发生变化。细胞表型的变化会导致细胞外基质产量的减少[41]。有研究表明,细胞骨架在细胞外基质组装方面起到重要作用。细胞外基质的减少也可能导致自组装基体收缩[42]。在体外传代培养软骨细胞时,发现软骨细胞P1和P4之间有140个基因存在差异,有12条是与细胞骨架蛋白和信号转导相关的基因,可见细胞骨架蛋白基因的表达在软骨细胞传代过程中发生了改变,说明其参与了细胞去分化过程[43]。细胞外基质、细胞骨架、细胞分化3者关系密切。 在组织工程化纤维软骨自组装基体中,星孢菌素可增加重要基质蛋白的基因表达,增加细胞外基质含量和减少基体收缩。星孢菌素明显破坏半月板纤维软骨细胞肌动蛋白纤维束,显著增加聚集蛋白聚糖、软骨寡聚基质蛋白基因表达,同时Ⅰ型胶原、Ⅱ型胶原基因表达也呈增加趋势[44]。 2.4 肌动蛋白细胞骨架 细胞骨架遍布真核细胞的细胞质,它包含3大类蛋白质:肌动蛋白丝、微管和中间丝。肌动蛋白丝是由球形的肌动蛋白单体聚合而成的长链状的纤维丝,又称微丝。在一定外界刺激作用下,肌动蛋白会发生解聚与重组,但重组现象只有在肌动蛋白增多时才可能发生。在具有轻微病变及正常人颞下颌关节盘中均可观察到部分散的平滑肌肌动蛋白阳性细胞,免疫组织化学发现穿孔或变性的颞下颌关节盘平滑肌肌动蛋白,在几乎所有的纤维样细胞和软骨样细胞中均强表达[45]。 星孢菌素可减少平滑肌肌动蛋白并抑制纤维软骨细胞基体的收缩。将星孢菌素(2.7 nmol/L)加进第3代软骨细胞,细胞骨架结构被破坏[46],在单层连续培养条件下细胞表型被恢复[47],软骨形成[48-49],微丝被快速解 聚[46]。将100 nmol/L星孢菌素加入半月板细胞中单层培养,发现细胞产生的收缩力量大幅度减小[50],将浓度降低至3 nmol/L时,发现平滑肌肌动蛋白合成降低,同时伴随同类型的肌动蛋白减少;同一实验将5 nmol/L星孢菌素加入Ⅰ型胶原-氨基多糖支架培养的细胞中,发现加药组比未加药组基体体积收缩减少35%[51]。纤维软骨细胞在体外连续培养时发生去分化现象,细胞表型改变,星孢菌素诱导细胞表型重新表达,这一过程与调整细胞骨架蛋白,激活PKC、PKA、P38/MAPK[17]、TGF-beta信号通路有关[52]。 2.5 肌动蛋白细胞骨架与细胞外基质的关系 细胞生物学、遗传学研究揭示了整合素连接激酶(ILK)及其相互作用蛋白在肌动蛋白细胞骨架和细胞外基质连接、通讯中的重要作用。在果蝇和秀丽隐杆线虫的遗传模型中,ILK的无效突变引起类似于ILK功能丧失的缺陷[53]。仔细研究果蝇中的ilk-null突变体,发现肌动蛋白丝在附着位点与膜分离[53]。几条证据表明CH-ILKBP–actopaxin– α-parvin作为关键桥分子之一,将ILK与肌动蛋白连接起来。首先,CH-ILKBP–actopaxin–α-parvin不仅可与ILK相互作用,还可与肌动蛋白相互作用。其次,CH-ILKBP– actopaxin–α-parvin与ILK结合的CH2片段过表达会抑制肌动蛋白应力纤维形成和细胞形状变化。paxillin及affixin–β-parvin是另两种连接肌动蛋白的ILK蛋白分子,affixin(包括CH2片段)过表达会抑制细胞的伸展。ILK和肌动蛋白细胞骨架之间的多重相互作用至少有两个重要的含义,一是它可允许细胞在细胞-细胞外基质连接位点调节组织物理强度,二是它可通过细胞-细胞外基质连接位点调节或促进信号转导。 综上所述,颞下颌关节盘自组装基体收缩的原因有细胞源不同、细胞收缩、营养障碍、肌动蛋白过表达和细胞外基质减少等。基体收缩的原因并不限于一种,它们之间也不是孤立存在的。星孢菌素减少软骨或纤维软骨细胞肌动蛋白,抑制细胞收缩并上调细胞外基质中胶原、聚集蛋白聚糖和软骨寡聚基质蛋白的基因表达,减小基体收缩幅度。"

| [1] Liu F,Steinkeler A.Epidemiology, diagnosis, and treatment of temporomandibular disorders.Dent Clin North Am. 2013;57(3): 465-479. [2] Tatli U,Benlidayi ME,Ekren O,et al.Comparison of the effectiveness of three different treatment methods for temporomandibular joint disc displacement without reduction.Int J Oral Maxillofac Surg.2017;46(5):603-609.[3] Kim JY,Jeon KJ,Kim MG,et al.A nomogram for classification of temporomandibular joint disc perforation based on magnetic resonance imaging.Oral Surg Oral Med Oral Pathol Oral Radiol. 2018;5(6):S2212-4403.[4] 齐梦怡.α-平滑肌肌动蛋白在山羊颞下颌关节盘和自组装基体中的表达[D]. 兰州: 兰州大学,2012. [5] Hoben GM,Hu JC,James RA,et al.Self-assembly of fibrochondrocytes and chondrocytes for tissue engineering of the knee meniscus.Tissue Eng.2007;13(5):939-946.[6] Hoben GM,Athanasiou KA.Use of staurosporine, an actin-modifying agent, to enhance fibrochondrocyte matrix gene expression and synthesis.Cell Tissue Res. 2008;334(3):469-476.[7] 何晓兰.传代和低氧培养对山羊颞下颌关节盘细胞表型及细胞骨架的影响[D]. 兰州: 兰州大学,2017.[8] Yao Y,Lacroix D,Mak AF.Effects of oxidative stress-induced changes in the actin cytoskeletal structure on myoblast damage under compressive stress: confocal-based cell-specific finite element analysis.Biomech Model Mechanobiol. 2016;15(6): 1495-1508. [9] Detamore MS,Hegde JN,Wagle RR,et al.Cell Type and Distribution in the Porcine Temporomandibular Joint Disc.J Oral Maxillofac Surg.2006;64(2):243-248.[10] Almarza AJ,Athanasiou KA.Evaluation of three growth factors in combinations of two for temporomandibular joint disc tissue engineering.Arch Oral Biol.2006;51(3):215-221. [11] Detamore MS,Athanasiou KA.Evaluation of Three Growth Factors for TMJ Disc Tissue Engineering. Ann Biomed Eng. 2005;33(3): 383-390. [12] 康宏,李振强,闭艳妲.自组装山羊颞下颌关节盘组织工程纤维软骨模型的构建[J].华西口腔医学杂志,2011,29(3):314-317. [13] Kang H,Qi M,Bao G.Expression of Alpha-smooth Muscle Action in Goat Temporoman-dibular Joint Disc and Its Effect on Self-Assembled Engineered Constructs// International Conference on Biomedical Engineering and Biotechnology.IEEE Computer Society,2012:1026-1029. [14] Hinz B,Celetta G,Tomasek JJ,et al.Alpha-Smooth Muscle Actin Expression Upregulates Fibroblast Contractile Activity.Mol Biol Cell.2001;12(9):2730-2741. [15] Picarddeland M,Ruel J,Galbraith T,et al.Tissue-Engineered Tubular Heart Valves Com-bining a Novel Precontraction Phase with the Self-Assembly Method.Ann Biomed Eng. 2016;45(2): 1-12.[16] Greene AF,Danielson M,Delawder AO,et al.Redox-responsive Artificial Molecular Muscles: Reversible Radical-based Self-assembly for Actuating Hydrogels.Chem Mater. 2017;29(21). DOI:10.1021/acs.chemmater.7b03635.[17] Rottmar M,Mhanna R,Guimond-Lischer S,et al.Interference with the contractile machinery of the fibroblastic chondrocyte cytoskeleton induces re-expression of the cartilage phenotype through involvement of PI3K, PKC and MAPKs. Exp Cell Res. 2014;320(2):175-187. [18] Kalpakci KN,Willard VP,Wong ME,et al.An interspecies comparison of the temporo-mandibular joint disc.J Dent Res. 2011;90(2):193-198. [19] Esvan YJ,Giraud F,Pereira E,et al.Synthesis and biological activity of pyrazole analogues of the staurosporine aglycon K252c.Bioorg Med Chem.2016;24(14):3116-3124. [20] Lee PY,Park BC,Chi SW,et al.Histone H4 is cleaved by granzyme A during staurosporine-induced cell death in B-lymphoid Raji cells. Bmb Rep.2016;49(10):560-565.[21] Cheng J,Park SB,Kim SH,et al.Suppressing activity of staurosporine from Streptomyces sp. MJM4426 against rice bacterial blight disease.J Appl Microbiol. 2016;120(4):975-985.[22] Zhang Y,Liu S,Yang X,et al.Staurosporine shows insecticidal activity against Mythimna separata Walker (Lepidoptera: Noctuidae) potentially via induction of apoptosis.Pestic Biochem Physiol.2016;128:37-44.[23] Tang WL,Chen WC,Roy A,et al.A Simple and Improved Active Loading Method to Effi-ciently Encapsulate Staurosporine into Lipid-Based Nanoparticles for Enhanced Therapy of Multidrug Resistant Cancer.Pharm Res.2016;33(5):1104-1114.[24] Del SV,Lizardo DY,Li N,et al.Differential Regulation of Specific Sphingolipids in Colon Cancer Cells during Staurosporine-Induced Apoptosis.Chem Biol. 2015;22(12):1662-1670.[25] Yadav SS,Prasad CB,Prasad SB,et al.Anti-tumor activity of staurosporine in the tumor microenvironment of cervical cancer: An in vitro study.Life Sci.2015;133:21-28.[26] Olguã¬N-Albuerne M,Ramos-Pittol JM,Coyoy A,et al.Peroxynitrite is Involved in the Apoptotic Death of Cultured Cerebellar Granule Neurons Induced by Staurosporine, but not by Potassium Deprivation.Neurochem Res. 2016;41(1-2):316-327.[27] Zhang Y,Liu S,Yang X,et al.Staurosporine shows insecticidal activity against Mythimna separata Walker (Lepidoptera: Noctuidae) potentially via induction of apoptosis.Pestic Biochem Physiol.2016;128:37-44.[28] Gonçalves AP,Cordeiro JM,Monteiro J,et al.Involvement of mitochondrial proteins in calcium signaling and cell death induced by staurosporine in Neurospora crassa.Bio-chimica Et Biophysica Acta.2015;1847(10):1064-1074.[29] Zhang J,Kinoh H,Hespel L,et al.Effective treatment of drug resistant recurrent breast tumors harboring cancer stem-like cells by staurosporine/epirubicin co-loaded polymeric mi-celles. J Control Release.2017;264:127-135.[30] Ding Y,Wang B,Chen X,et al.Staurosporine suppresses survival of HepG2 cancer cells through Omi/HtrA2-mediated inhibition of PI3K/Akt signaling pathway.Tumor Biol.2017; 39(3): 101042831769431.[31] Olguã¬N-Albuerne M,Ramos-Pittol JM,Coyoy A,et al.Peroxynitrite is Involved in the Apoptotic Death of Cultured Cerebellar Granule Neurons Induced by Staurosporine, but not by Potassium Deprivation.Neurochem Res. 2016;41(1-2):316-327.[32] Liu AH,Cao YN,Liu HT,et al.DIDS Attenuates Staurosporine- induced Cardiomyocyte Apoptosis by PI3K/Akt Signaling Pathway: Activation of eNOS/NO and Inhibition of Bax Translocation. Cell Physiol Biochem. 2008;22(1-4):177-186.[33] Jung JC,Huh MI,Paudelkattel S,et al.Modulation of Staurosporine Induced Neuronal Cell Differentiation and Neurite Outgrowth of Chick Retinal Neuroblasts by Inhibition of MMPs Activities.J Catal. 2011;165(2):129-139.[34] Mahajan S,Thieme D,Czugala M,et al.Lamin Cleavage: A Reliable Marker for Studying Staurosporine-Induced Apoptosis in Corneal Tissue.Invest Ophthalmol Vis Sci. 2017;58(13):5802-5809.[35] Detamore MS,Orfanos JG,Almarza AJ,et al.Quantitative analysis and comparative regional investigation of the extracellular matrix of the porcine temporomandibular joint disc.Matrix Biol. 2005;24: 45-57. [36] Wang KH,Chan WP,Chiu LH,et al. Histological and Immunohistochemical Analyses of Repair of the Disc in the Rabbit Temporomandibular Joint Using a Collagen Template. Materials. 2017; 2017(10):924. [37] Lin W,Zhang W,Zhang J,et al.Self-repair capability of surgically created incisions in TMJ disc: An experimental study on goats.J Craniomaxillofac Surg. 2014;42(7):1334-1340. [38] Scapino RP,Obrez A,Greising D.Organization and function of the collagen fiber system in the human temporomandibular joint disk and its attachments.Cells Tissues Organs.2006;182:201-225. [39] Naqvi SM,Gansau J,Buckley C.Priming and cryopreservation of microencapsulated marrow stromal cells as a strategy for intervertebral disc regeneration.Biomed Mater. 2018;13(3): 034106. [40] 高克海,李洪涛,黄彩虹.聚集蛋白聚糖酶-1在退变椎间盘中的表达及意义[J].中国矫形外科杂志, 2014,22(15):1412-1416.[41] 张艳,柴岗,刘伟,等.体外培养过程中去分化的人软骨细胞基因表达谱的变化[J].中华整形外科杂志, 2007,23(4):331-334. [42] Brennan JR,Hocking DC.Cooperative Effects of Fibronectin Matrix Assembly and Initial Cell-Substrate Adhesion Strength in Cellular Self-Assembly.Acta Biomaterialia. 2016;32:198-209.[43] Leonardi R,Villari LC,Bernasconi G,et al.Immunolocalization of vimentin and alpha-smooth muscle actin in dysfunctional human temporomandibular joint disc samples.J Oral Rehabil. 2002; 29(3):282-286. [44] Minjung K,Song K,Jin EJ,et al.Staurosporine and cytochalasin D induce chondrogenesis by regulation of actin dynamics in different way.Exp Mol Med.2012;44(9):521-528. [45] Lin L,Wang Q,Qian K,et al.bFGF Protects Against Oxygen Glucose Deprivation/Reoxygenation-Induced Endothelial Monolayer Permeability via S1PR1-Dependent Mechanisms.Mol Neurobiol.2018;55(4):3131-3142.[46] Lee CR,Grodzinsky AJ,Spector M.Modulation of the contractile and biosynthetic activity of chondrocytes seeded in collagen-glycosaminoglycan matrices.Tissue Eng. 2003;9(1): 27-36. [47] Battistelli M,Salucci S,Olivotto E,et al.Cell death in human articular chondrocyte: a morpho-functional study in micromass model.Apoptosis.2014;19(10):1471-1483. [48] Lee SW,Sun MC,Yun SC,et al.A purified extract from Clematis mandshurica, prevents staurosporin-induced downregulation of 14-3-3 and subsequent apoptosis on rat chondrocytes. J Ethnopharmacol.2007;111(2):213-218. [49] Zaleskas JM,Kinner B,Freyman TM,et al.Contractile forces generated by articular chondrocytes in collagen-glycosaminoglycan matrices.Biomaterials. 2004;25(7-8): 1299-1308. [50] Zervas CG,Gregory SL,Brown NH.DrosophilaIntegrin-Linked Kinase Is Required at Sites of Integrin Adhesion to Link the Cytoskeleton to the Plasma Membrane.J Cell Biol. 2001;152(5): 1007-1018. [51] Marotta A,Tan C,Gray V,et al.Dysregulation of integrin-linked kinase (ILK) signaling in colonic polyposis. Oncogene. 2001; 20(43):6250-6257. [52] Kim H,Kei K,Sonn JK.Staurosporine induces chondrogenesis of chick embryo wing bud mesenchyme in monolayer cultures through canonical and non-canonical TGF-β pathways.Vitro Cell Dev Biol Anim.2016;(1):120-129.[53] Kang L,Mokshagundam S,Reuter B,et al.Integrin-Linked Kinase in Muscle Is Necessary for the Development of Insulin Resistance in Diet-Induced Obese Mice.Diabetes. 2016;65(6):1590-1600. [54] Pika M,Konstantin E,Ayesha S,et al.Actin depolymerisation and crosslinking join forces with myosin II to contract actin coats on fused secretory vesicles.J Cell Sci. 2015;128(6):1193-1203. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [12] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [13] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [14] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [15] | Liu Liyong, Zhou Lei. Research and development status and development trend of hydrogel in tissue engineering based on patent information [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3527-3533. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||