Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (17): 2761-2768.doi: 10.3969/j.issn.2095-4344.0501
Previous Articles Next Articles
Effects of mechanical stresses on neural differentiation of mesenchymal stem cells
Jiang Jing-yi1, 2, Fan Yu-bo1, 2, Zheng Li-sha1, 2
- 1Key Laboratory for Biomechanics and Mechanobiology of Ministry of Education, School of Biological Science and Medical Engineering, Beihang University, Beijing 100083, China; 2Beijing Advanced Innovation Centre for Biomedical Engineering, Beihang University, Beijing 100083, China
-
Revised:2018-01-13Online:2018-06-18Published:2018-06-18 -
Contact:Zheng Li-sha, Ph.D., Associate professor, Master’s supervisor, Key Laboratory for Biomechanics and Mechanobiology of Ministry of Education, School of Biological Science and Medical Engineering, Beihang University, Beijing 100083, China; Beijing Advanced Innovation Centre for Biomedical Engineering, Beihang University, Beijing 100083, China -
About author:Jiang Jing-yi, Master candidate, Key Laboratory for Biomechanics and Mechanobiology of Ministry of Education, School of Biological Science and Medical Engineering, Beihang University, Beijing 100083, China; Beijing Advanced Innovation Centre for Biomedical Engineering, Beihang University, Beijing 100083, China -
Supported by:the National Natural Science Foundation of China, No. 11572030, 61227902, 11120101001, 11421202; the National Key R&D Program of China, No. 2017YFC0108505, 2017YFC0108500
CLC Number:
Cite this article
Jiang Jing-yi, Fan Yu-bo, Zheng Li-sha. Effects of mechanical stresses on neural differentiation of mesenchymal stem cells[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(17): 2761-2768.
share this article
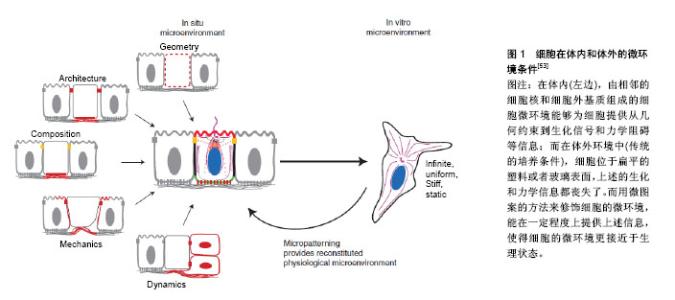
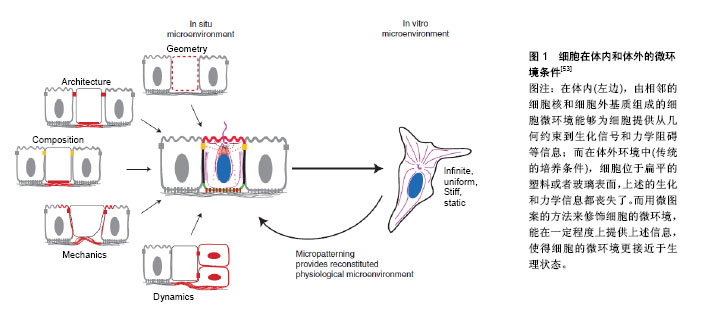
2.1 机械应力调控间充质干细胞神经向分化 2.1.1 流动剪切力 流动剪切力是组织再生和重建过程中最重要的机械刺激之一。研究表明流动剪切力对维持细胞、组织乃至整个机体正常的生理状态都有重要意义[19-21]。许多实验室根据流变学原理研制了相应的细胞力学实验装置,其中包括近些年研究较广泛的微流控等。目前,微流控细胞培养系统已经用于二维(2D)和三维(3D)细胞培养[22-24]。人类脂肪组织干细胞是一种组织特异性干细胞,可以分化成多种间充质细胞,如骨细胞、软骨细胞、脂肪细胞、肌肉细胞等[25-26]。Choi等[27]利用3D微流控通道芯片培养人脂肪干细胞,并加入神经分化诱导液。结果显示生长在芯片上的人脂肪干细胞形成的神经球比在普通培养皿中培养的细胞多,且诱导细胞产生更多的γ-氨基丁酸,几乎60%的细胞都表达γ-氨基丁酸。此外,芯片/PCR分析表明3D微流控细胞培养系统是通过诱导激活人脂肪干细胞中wnt5A/β-catenin信号通路,从而导致人脂肪干细胞的自我更新和神经向分化。Jeon等[28]连续2 d对接种在微图形化基底上的骨髓间充质干细胞加载3 h 0.1 Pa和0.25 Pa的流动剪切力,然后对细胞进行神经向诱导,结果显示流动剪切力促进了骨髓间充质干细胞中神经元标志物微管蛋白(β-tubulin Ⅲ)、微管相关蛋白2(MAP-2)等分子的表达。然而,另一研究给骨髓间充质干细胞施加1.5 Pa的流动剪切力,然后继续在神经向分化诱导培养基中培养细胞,结果显示流动剪切力并未影响骨髓间充质干细胞的神经向分化效率[29],可能原因是1 h的加载时间过短。 2.1.2 微重力 太空飞行会使宇航员处于微重力环境中,引起许多人体生理的变化[30]。大量研究证明了微重力对细胞内信号通路、细胞分泌物和基因表达的影响机制[31]。目前的研究发现模拟微重力作为一种机械因素可以影响间充质干细胞的分化和功能[32],并触发细胞在体外进行三维组装,从而模拟体内的状态[31,33-34],被认为是组织工程和再生医学领域的一种新策略。有学者研究了模拟微重力条件下骨髓间充质干细胞的多向分化能力。研究将骨髓间充质干细胞分为正常重力(NG)组和模拟微重力(SMG)组,模拟微重力组内细胞骨架从纺锤形变成圆形,细胞内干细胞多能性标记物OCT4表达量上调,特别是模拟微重力加载72 h时是最适合骨髓间充质干细胞多向分化的时间点。诱导两组细胞神经向分化,免疫染色和免疫印迹结果发现模拟微重力组内骨髓间充质干细胞分化形成的神经样细胞中MAP-2和神经丝蛋白(NF-H)的表达量均高于正常重力组。因此,该研究认为模拟微重力可能是通过调节细胞骨架和OCT4的表达来诱导骨髓间充质干细胞的分化[35]。Xue等[36]在不同的分化培养基中培养骨髓间充质干细胞72 h或10 d。结果发现短时间的微重力刺激(72 h)可以促进骨髓间充质干细胞向内皮细胞、神经元和脂肪细胞分化;而延长微重力(10 d)的刺激时间则会促进骨髓间充质干细胞分化为成骨细胞。他们还发现,短时间的微重力刺激显著降低了细胞内Ras家族成员RhoA激酶的活性,但长期的微重力刺激却使RhoA激酶的活性显著增加。而当RhoA激酶的活性受到抑制时,长期的微重力作用效果就会被恢复。这些结果表明,微重力刺激通过RhoA激酶相关的信号通路调节骨髓间充质干细胞的神经向分化能力。此外,Chen等[37]研究也表明模拟微重力显著增强了骨髓间充质干细胞成神经向分化的诱导效果。Zarrinpour等[38]使用快速旋转的回转器模拟微重力条件,研究微重力刺激对人脂肪干细胞神经向分化的影响。结果显示无论是神经诱导分化之前还是之后,模拟微重力都可以促进细胞内MAP-2、脑源性神经营养因子(BDNF)和神经营养因子(NT-3)表达量的上调。由以上所有研究结果可见,模拟微重力可以促进间充质干细胞的神经向分化。 2.1.3 牵张力 纵观机体所处的力学刺激环境,似乎可以发现一个有趣的现象,即大多数的力学刺激都是有“节奏”的,并常以牵张力的形式表达,譬如心脏规律泵血时外周血管壁的反复牵拉、运动状况下骨骼和肌肉的反复拉伸、口颌系统咀嚼运动时牙周膜组织承受的规律牵张等。近来已有不少相关研究证实了周期性牵张力的生物学重要性。研究发现骨髓间充质干细胞对机械牵张非常敏感,不同振幅、不同频率的牵张会有利于骨髓间充质干细胞向不同的方向分化[39-41]。而Leong等[42]发现只有低频率、低振幅的牵张(0.5 Hz,0.5%)能够在没有额外的诱导培养条件下促进骨髓间充质干细胞的神经向分化,同时,他们还发现该过程是通过活化Rac1而非Rho A来实现的。 2.1.4 次声振动 除了上述的机械力刺激对间充质干细胞的神经向分化有影响以外,研究发现次声振动也能影响骨髓间充质干细胞的分化方向。有研究给骨髓间充质干细胞施加了40 Hz的次声振动而不进行诱导培养,持续刺激5 d后发现细胞表现出神经细胞样形态,神经向标志物的表达量显著升高,而且此过程中还伴随着ERK激酶的激活[43]。同样的,在另一研究中,人脂肪组织干细胞无需神经向诱导培养,在30 Hz次声振动持续刺激4 d后,也表现出神经向分化的现象,同时伴随着ERK激酶的活化。上述研究表明次声振动能够通过激活ERK激酶信号通路调控间充质干细胞的神经向分化[44]。 2.2 细胞外基质调控间充质干细胞神经向分化 在生物体内,细胞并不是孤立存在的,而是存在于其周围一定的微环境中,这个微环境包括其周围的基质细胞、细胞间质、体液以及各种细胞因子和物理因素等[45-46]。细胞的微环境也被称为细胞生存的细胞外基质[47],越来越多的证据证明这些物理和化学因素共同影响细胞的命运[48-52]。因此,通过改变细胞外基质的物理环境来调控干细胞的生物学行为,已经成为组织工程和再生医学研究的热点领域。细胞在体内和体外的微环境条件,见图1[53]。"
| [1] Manchineella S, Thrivikraman G, Basu B, et al. Surface-Functionalized Silk Fibroin Films as a Platform To Guide Neuron-like Differentiation of Human Mesenchymal Stem Cells. ACS Appl Mater Interfaces. 2016;8(35):22849-22859.[2] Zhang J, Li D, Shen A, et al. Expression of RBMX after spinal cord injury in rats. J Mol Neurosci. 2013;49(2):417-429.[3] Burdick JA, Ward M, Liang E, et al. Stimulation of neurite outgrowth by neurotrophins delivered from degradable hydrogels. Biomaterials. 2006;27(3):452-459.[4] Shi W, Nie D, Jin G, et al. BDNF blended chitosan scaffolds for human umbilical cord MSC transplants in traumatic brain injury therapy. Biomaterials. 2012;33(11):3119-3126.[5] Wichterle H, Lieberam I, Porter JA, et al. Directed differentiation of embryonic stem cells into motor neurons. Cell. 2002;110(3): 385-397.[6] Nishikawa S, Jakt LM, Era T. Embryonic stem-cell culture as a tool for developmental cell biology. Nat Rev Mol Cell Biol. 2007;8(6):502-507.[7] Wang TT, Tio M, Lee W, et al. Neural differentiation of mesenchymal-like stem cells from cord blood is mediated by PKA. Biochem Biophys Res Commun. 2007;357(4):1021-1027.[8] Caiazzo M, Dell'Anno MT, Dvoretskova E, et al. Direct generation of functional dopaminergic neurons from mouse and human fibroblasts. Nature. 2011;476(7359):224-227.[9] Han DW, Tapia N, Hermann A, et al. Direct reprogramming of fibroblasts into neural stem cells by defined factors. Cell Stem Cell. 2012;10(4):465-472.[10] Zuba-Surma EK, Kucia M, Ratajczak J, et al. "Small stem cells" in adult tissues: very small embryonic-like stem cells stand up. Cytometry A. 2009;75(1):4-13.[11] Pereira Lda V. The importance of the use of stem cells for public health. Cien Saude Colet. 2008;13(1):7-14.[12] Lu P, Tuszynski MH. Can bone marrow-derived stem cells differentiate into functional neurons. Exp Neurol. 2005;193(2):273-278.[13] Woodbury D, Schwarz EJ, Prockop DJ, et al. Adult rat and human bone marrow stromal cells differentiate into neurons. J Neurosci Res. 2000;61(4):364-370.[14] Prockop DJ, Azizi SA, Colter D, et al. Potential use of stem cells from bone marrow to repair the extracellular matrix and the central nervous system. Biochem Soc Trans. 2000;28(4):341-345.[15] Zhong W, Tian K, Zheng X, et al. Mesenchymal stem cell and chondrocyte fates in a multishear microdevice are regulated by Yes-associated protein. Stem Cells Dev. 2013;22(14):2083-2093.[16] Ward DF Jr, Salasznyk RM, Klees RF, et al. Mechanical strain enhances extracellular matrix-induced gene focusing and promotes osteogenic differentiation of human mesenchymal stem cells through an extracellular-related kinase-dependent pathway. Stem Cells Dev. 2007;16(3):467-480.[17] Takahashi K, Yamanaka S. Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell. 2006;126(4):663-676.[18] Engler AJ, Sen S, Sweeney HL, et al. Matrix elasticity directs stem cell lineage specification. Cell. 2006;126(4):677-689.[19] Lee HJ, Ewere A, Diaz MF, et al. TAZ responds to fluid shear stress to regulate the cell cycle. Cell Cycle. 2017:1-21.[20] Sera T, Sumii T, Fujita R, et al. Effect of shear stress on the migration of hepatic stellate cells. In Vitro Cell Dev Biol Anim. 2018;54(1):11-22.[21] Nishii K, Brodin E, Renshaw T, et al. Shear stress upregulates regeneration-related immediate early genes in liver progenitors in 3D ECM-like microenvironments. J Cell Physiol. 2017 Oct 20. doi: 10.1002/jcp.26246. [Epub ahead of print][22] Kapur S, Baylink DJ, Lau KH. et al. Fluid flow shear stress stimulates human osteoblast proliferation and differentiation through multiple interacting and competing signal transduction pathways. Bone. 2003;32(3):241-251.[23] Jeong SI, Kwon JH, Lim JI, et al. Mechano-active tissue engineering of vascular smooth muscle using pulsatile perfusion bioreactors and elastic PLCL scaffolds. Biomaterials. 2005;26(12): 1405-1411.[24] Kim MS, Yeon JH, Park JK. A microfluidic platform for 3-dimensional cell culture and cell-based assays. Biomed Microdevices. 2007;9(1):25-34.[25] Gronthos S, Franklin DM, Leddy HA, et al. Surface protein characterization of human adipose tissue-derived stromal cells. J Cell Physiol. 2001;189(1):54-63.[26] Bunnell BA, Flaat M, Gagliardi C, et al. Adipose-derived stem cells: isolation, expansion and differentiation. Methods. 2008; 45(2):115-120.[27] Choi J, Kim S, Jung J, et al. Wnt5a-mediating neurogenesis of human adipose tissue-derived stem cells in a 3D microfluidic cell culture system. Biomaterials. 2011;32(29):7013-7022.[28] Jeon KJ, Park SH, Shin JW, et al. Combined effects of flow-induced shear stress and micropatterned surface morphology on neuronal differentiation of human mesenchymal stem cells. J Biosci Bioeng. 2014;117(2):242-247. [29] Mascotte-Cruz JU, Ríos A, Escalante B. Combined effects of flow-induced shear stress and electromagnetic field on neural differentiation of mesenchymal stem cells. Electromagn Biol Med. 2016;35(2):161-166.[30] Basso N, Bellows CG, Heersche JN. Effect of simulated weightlessness on osteoprogenitor cell number and proliferation in young and adult rats. Bone. 2005;36(1):173-183.[31] Grimm D, Bauer J, Kossmehl P, et al. Simulated microgravity alters differentiation and increases apoptosis in human follicular thyroid carcinoma cells. FASEB J. 2002;16(6):604-606.[32] Dai ZQ, Wang R, Ling SK, et al. Simulated microgravity inhibits the proliferation and osteogenesis of rat bone marrow mesenchymal stem cells. Cell Prolif. 2007;40(5):671-684.[33] Hochleitner B, Hengster P, Duo L, et al. A novel bioartificial liver with culture of porcine hepatocyte aggregates under simulated microgravity. Artif Organs. 2005;29(1):58-66.[34] Marquette ML, Byerly D, Sognier M. A novel in vitro three-dimensional skeletal muscle model. In Vitro Cell Dev Biol Anim. 2007;43(7):255-263.[35] Wang N, Wang H, Chen J, et al. The simulated microgravity enhances multipotential differentiation capacity of bone marrow mesenchymal stem cells. Cytotechnology. 2014;66(1):119-131.[36] Xue L, Li Y, Chen J. Duration of simulated microgravity affects the differentiation of mesenchymal stem cells. Mol Med Rep. 2017; 15(5):3011-3018.[37] Chen J, Liu R, Yang Y, et al. The simulated microgravity enhances the differentiation of mesenchymal stem cells into neurons. Neurosci Lett. 2011;505(2):171-175.[38] Zarrinpour V, Hajebrahimi Z, Jafarinia M. Expression pattern of neurotrophins and their receptors during neuronal differentiation of adipose-derived stem cells in simulated microgravity condition. Iran J Basic Med Sci. 2017;20(2):178-186.[39] Park JS, Chu JS, Cheng C, et al. Differential effects of equiaxial and uniaxial strain on mesenchymal stem cells. Biotechnol Bioeng. 2004;88(3):359-368.[40] Chen YJ, Huang CH, Lee IC, et al. Effects of cyclic mechanical stretching on the mRNA expression of tendon/ligament-related and osteoblast-specific genes in human mesenchymal stem cells. Connect Tissue Res. 2008;49(1):7-14.[41] Huang CH, Chen MH, Young TH, et al. Interactive effects of mechanical stretching and extracellular matrix proteins on initiating osteogenic differentiation of human mesenchymal stem cells. J Cell Biochem. 2009;108(6):1263-1273.[42] Leong WS, Wu SC, Pal M, et al. Cyclic tensile loading regulates human mesenchymal stem cell differentiation into neuron-like phenotype. J Tissue Eng Regen Med. 2012;6 Suppl 3:s68-79.[43] Cho H, Seo YK, Jeon S, et al. Neural differentiation of umbilical cord mesenchymal stem cells by sub-sonic vibration. Life Sci. 2012;90(15-16):591-599.[44] Choi YK, Cho H, Seo YK, et al. Stimulation of sub-sonic vibration promotes the differentiation of adipose tissue-derived mesenchymal stem cells into neural cells. Life Sci. 2012;91(9-10):329-337.[45] Discher DE, Janmey P, Wang YL. Tissue cells feel and respond to the stiffness of their substrate. Science. 2005;310(5751):1139-1143.[46] Yim EK, Pang SW, Leong KW. Synthetic nanostructures inducing differentiation of human mesenchymal stem cells into neuronal lineage. Exp Cell Res. 2007;313(9):1820-1829.[47] Hynes RO. The extracellular matrix: not just pretty fibrils. Science. 2009;326(5957):1216-1219.[48] Geiger B, Spatz JP, Bershadsky AD. Environmental sensing through focal adhesions. Nat Rev Mol Cell Biol. 2009;10(1):21-33.[49] Wang N, Tytell JD, Ingber DE. Mechanotransduction at a distance: mechanically coupling the extracellular matrix with the nucleus. Nat Rev Mol Cell Biol. 2009;10(1):75-82.[50] Vogel V, Sheetz M. Local force and geometry sensing regulate cell functions. Nat Rev Mol Cell Biol. 2006;7(4):265-275.[51] Dalby MJ, Gadegaard N, Tare R, et al. The control of human mesenchymal cell differentiation using nanoscale symmetry and disorder. Nat Mater. 2007;6(12):997-1003.[52] Janmey PA, Winer JP, Murray ME, et al. The hard life of soft cells. Cell Motil Cytoskeleton. 2009;66(8):597-605.[53] Théry M. Micropatterning as a tool to decipher cell morphogenesis and functions. J Cell Sci. 2010;123(Pt 24):4201-4213.[54] Higuchi A, Ling QD, Chang Y, et al. Physical cues of biomaterials guide stem cell differentiation fate. Chem Rev. 2013;113(5): 3297-3328.[55] Seiler C, Davuluri G, Abrams J, et al. Smooth muscle tension induces invasive remodeling of the zebrafish intestine. PLoS Biol. 2012;10(9):e1001386.[56] Butcher DT, Alliston T, Weaver VM. A tense situation: forcing tumour progression. Nat Rev Cancer. 2009;9(2):108-122.[57] Klein EA, Yin L, Kothapalli D, et al. Cell-cycle control by physiological matrix elasticity and in vivo tissue stiffening. Curr Biol. 2009;19(18):1511-1518.[58] Zaman MH, Trapani LM, Sieminski AL, et al. Migration of tumor cells in 3D matrices is governed by matrix stiffness along with cell-matrix adhesion and proteolysis. Proc Natl Acad Sci U S A. 2006;103(29):10889-10894.[59] Raab M, Swift J, Dingal PC, et al. Crawling from soft to stiff matrix polarizes the cytoskeleton and phosphoregulates myosin-II heavy chain. J Cell Biol. 2012;199(4):669-683.[60] Flanagan LA, Ju YE, Marg B, et al. Neurite branching on deformable substrates. Neuroreport. 2002;13(18):2411-2415.[61] Discher DE, Mooney DJ, Zandstra PW. Growth factors, matrices, and forces combine and control stem cells. Science. 2009;324 (5935):1673-1677.[62] Kong HJ, Polte TR, Alsberg E, et al. FRET measurements of cell-traction forces and nano-scale clustering of adhesion ligands varied by substrate stiffness. Proc Natl Acad Sci U S A. 2005; 102(12):4300-4305.[63] Rowlands AS, George PA, Cooper-White JJ. Directing osteogenic and myogenic differentiation of MSCs: interplay of stiffness and adhesive ligand presentation. Am J Physiol Cell Physiol. 2008; 295(4):C1037-1044.[64] Saha K, Keung AJ, Irwin EF, et al. Substrate modulus directs neural stem cell behavior. Biophys J. 2008;95(9):4426-4438.[65] Engler AJ, Griffin MA, Sen S, et al. Myotubes differentiate optimally on substrates with tissue-like stiffness: pathological implications for soft or stiff microenvironments. J Cell Biol. 2004; 166(6):877-887.[66] Wang LS, Chung JE, Chan PP, et al. Injectable biodegradable hydrogels with tunable mechanical properties for the stimulation of neurogenesic differentiation of human mesenchymal stem cells in 3D culture. Biomaterials. 2010;31(6):1148-1157. [67] Zhang QY, Zhang YY, Xie J, et al. Stiff substrates enhance cultured neuronal network activity. Sci Rep. 2014;4:6215.[68] Kostic A, Sap J, Sheetz MP. RPTPalpha is required for rigidity-dependent inhibition of extension and differentiation of hippocampal neurons. J Cell Sci. 2007;120(Pt 21):3895-3904.[69] Sun Y, Yong KM, Villa-Diaz LG, et al. Hippo/YAP-mediated rigidity-dependent motor neuron differentiation of human pluripotent stem cells. Nat Mater. 2014;13(6):599-604.[70] Leong WS, Tay CY, Yu H, et al. Thickness sensing of hMSCs on collagen gel directs stem cell fate. Biochem Biophys Res Commun. 2010;401(2):287-292.[71] Jiang L, Sun Z, Chen X, et al. Cells Sensing Mechanical Cues: Stiffness Influences the Lifetime of Cell-Extracellular Matrix Interactions by Affecting the Loading Rate. ACS Nano. 2016;10(1): 207-217.[72] Du J, Chen X, Liang X, et al. Integrin activation and internalization on soft ECM as a mechanism of induction of stem cell differentiation by ECM elasticity. Proc Natl Acad Sci U S A. 2011; 108(23):9466-9471.[73] Shih YR, Tseng KF, Lai HY, et al. Matrix stiffness regulation of integrin-mediated mechanotransduction during osteogenic differentiation of human mesenchymal stem cells. J Bone Miner Res. 2011;26(4):730-738.[74] Provenzano PP, Inman DR, Eliceiri KW, et al. Matrix density-induced mechanoregulation of breast cell phenotype, signaling and gene expression through a FAK-ERK linkage. Oncogene. 2009;28(49):4326-4343.[75] Alexanian AR, Liu QS, Zhang Z. Enhancing the efficiency of direct reprogramming of human mesenchymal stem cells into mature neuronal-like cells with the combination of small molecule modulators of chromatin modifying enzymes, SMAD signaling and cyclic adenosine monophosphate levels. Int J Biochem Cell Biol. 2013;45(8):1633-1638.[76] Zouani OF, Kalisky J, Ibarboure E, et al. Effect of BMP-2 from matrices of different stiffnesses for the modulation of stem cell fate. Biomaterials. 2013;34(9):2157-2166.[77] Lim SH, Liu XY, Song H, et al. The effect of nanofiber-guided cell alignment on the preferential differentiation of neural stem cells. Biomaterials. 2010;31(34):9031-9039.[78] Georgiou M, Golding JP, Loughlin AJ, et al. Engineered neural tissue with aligned, differentiated adipose-derived stem cells promotes peripheral nerve regeneration across a critical sized defect in rat sciatic nerve. Biomaterials. 2015;37:242-251.[79] Dalby MJ, McCloy D, Robertson M, et al. Osteoprogenitor response to semi-ordered and random nanotopographies. Biomaterials. 2006;27(15):2980-2987.[80] Silva GA, Czeisler C, Niece KL, et al. Selective differentiation of neural progenitor cells by high-epitope density nanofibers. Science. 2004;303(5662):1352-1355.[81] Curtis A, Wilkinson C. Nantotechniques and approaches in biotechnology. Trends Biotechnol. 2001;19(3):97-101.[82] McBeath R, Pirone DM, Nelson CM, et al. Cell shape, cytoskeletal tension, and RhoA regulate stem cell lineage commitment. Dev Cell. 2004;6(4):483-495.[83] Kilian KA, Bugarija B, Lahn BT, et al. Geometric cues for directing the differentiation of mesenchymal stem cells. Proc Natl Acad Sci U S A. 2010;107(11):4872-4877.[84] Watari S, Hayashi K, Wood JA, et al. Modulation of osteogenic differentiation in hMSCs cells by submicron topographically-patterned ridges and grooves. Biomaterials. 2012; 33(1):128-136.[85] Gobaa S, Hoehnel S, Roccio M, et al. Artificial niche microarrays for probing single stem cell fate in high throughput. Nat Methods. 2011;8(11):949-955.[86] Mirzaei E, Ai J, Ebrahimi-Barough S, et al. The Differentiation of Human Endometrial Stem Cells into Neuron-Like Cells on Electrospun PAN-Derived Carbon Nanofibers with Random and Aligned Topographies. Mol Neurobiol. 2016;53(7):4798-4808.[87] Javazon EH, Beggs KJ, Flake AW. Mesenchymal stem cells: paradoxes of passaging. Exp Hematol. 2004;32(5):414-425.[88] Alavi A, Stupack DG. Cell survival in a three-dimensional matrix. Methods Enzymol. 2007;426:85-101.[89] Nakajima M, Ishimuro T, Kato K, et al. Combinatorial protein display for the cell-based screening of biomaterials that direct neural stem cell differentiation. Biomaterials. 2007;28(6): 1048-1060.[90] Liu H, Lin J, Roy K. Effect of 3D scaffold and dynamic culture condition on the global gene expression profile of mouse embryonic stem cells. Biomaterials. 2006;27(36):5978-5989.[91] Zhao F, Grayson WL, Ma T, et al. Effects of hydroxyapatite in 3-D chitosan-gelatin polymer network on human mesenchymal stem cell construct development. Biomaterials. 2006;27(9):1859-1867.[92] Markusen JF, Mason C, Hull DA, et al. Behavior of adult human mesenchymal stem cells entrapped in alginate-GRGDY beads. Tissue Eng. 2006;12(4):821-830.[93] Lutolf MP. Biomaterials: Spotlight on hydrogels. Nat Mater. 2009; 8(6):451-453.[94] Lee JH, Yu HS, Lee GS, et al. Collagen gel three-dimensional matrices combined with adhesive proteins stimulate neuronal differentiation of mesenchymal stem cells. J R Soc Interface. 2011;8(60):998-1010.[95] Gu H, Yue Z, Leong WS, et al. Control of in vitro neural differentiation of mesenchymal stem cells in 3D macroporous, cellulosic hydrogels. Regen Med. 2010;5(2):245-253.[96] Lee JH, Lee JY, Yang SH, et al. Carbon nanotube-collagen three-dimensional culture of mesenchymal stem cells promotes expression of neural phenotypes and secretion of neurotrophic factors. Acta Biomater. 2014;10(10):4425-4436.[97] Khosravizadeh Z, Razavi S, Bahramian H, et al. The beneficial effect of encapsulated human adipose-derived stem cells in alginate hydrogel on neural differentiation. J Biomed Mater Res B Appl Biomater. 2014;102(4):749-755.[98] Rao SR, Subbarayan R, Dinesh MG, et al. Differentiation of human gingival mesenchymal stem cells into neuronal lineages in 3D bioconjugated injectable protein hydrogel construct for the management of neuronal disorder. Exp Mol Med. 2016;48:e209.[99] Roozafzoon R, Lashay A, Vasei M, et al. Dental pulp stem cells differentiation into retinal ganglion-like cells in a three dimensional network. Biochem Biophys Res Commun. 2015;457(2):154-160.[100] Gugliandolo A, Diomede F, Cardelli P, et al. Transcriptomic analysis of gingival mesenchymal stem cells cultured on 3D bioprinted scaffold: A promising strategy for neuroregeneration. J Biomed Mater Res A. 2018;106(1):126-137.[101] Feng X, Lu X, Huang D, et al. 3D porous chitosan scaffolds suit survival and neural differentiation of dental pulp stem cells. Cell Mol Neurobiol. 2014;34(6):859-870.[102] Zhang J, Lu X, Feng G, et al. Chitosan scaffolds induce human dental pulp stem cells to neural differentiation: potential roles for spinal cord injury therapy. Cell Tissue Res. 2016;366(1):129-142.[103] Ghasemi-Mobarakeh L, Prabhakaran MP, Morshed M, et al. Electrospun poly(epsilon-caprolactone)/gelatin nanofibrous scaffolds for nerve tissue engineering. Biomaterials. 2008;29(34): 4532-4539.[104] Jahani H, Jalilian FA, Wu CY, et al. Controlled surface morphology and hydrophilicity of polycaprolactone toward selective differentiation of mesenchymal stem cells to neural like cells. J Biomed Mater Res A. 2015;103(5):1875-1881. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Lin Qingfan, Xie Yixin, Chen Wanqing, Ye Zhenzhong, Chen Youfang. Human placenta-derived mesenchymal stem cell conditioned medium can upregulate BeWo cell viability and zonula occludens expression under hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 4970-4975. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [5] | Shi Yangyang, Qin Yingfei, Wu Fuling, He Xiao, Zhang Xuejing. Pretreatment of placental mesenchymal stem cells to prevent bronchiolitis in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 991-995. |
| [6] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [7] | Fan Quanbao, Luo Huina, Wang Bingyun, Chen Shengfeng, Cui Lianxu, Jiang Wenkang, Zhao Mingming, Wang Jingjing, Luo Dongzhang, Chen Zhisheng, Bai Yinshan, Liu Canying, Zhang Hui. Biological characteristics of canine adipose-derived mesenchymal stem cells cultured in hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1002-1007. |
| [8] | Geng Yao, Yin Zhiliang, Li Xingping, Xiao Dongqin, Hou Weiguang. Role of hsa-miRNA-223-3p in regulating osteogenic differentiation of human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1008-1013. |
| [9] | Lun Zhigang, Jin Jing, Wang Tianyan, Li Aimin. Effect of peroxiredoxin 6 on proliferation and differentiation of bone marrow mesenchymal stem cells into neural lineage in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1014-1018. |
| [10] | Zhu Xuefen, Huang Cheng, Ding Jian, Dai Yongping, Liu Yuanbing, Le Lixiang, Wang Liangliang, Yang Jiandong. Mechanism of bone marrow mesenchymal stem cells differentiation into functional neurons induced by glial cell line derived neurotrophic factor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1019-1025. |
| [11] | Duan Liyun, Cao Xiaocang. Human placenta mesenchymal stem cells-derived extracellular vesicles regulate collagen deposition in intestinal mucosa of mice with colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1026-1031. |
| [12] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [13] | Li Cai, Zhao Ting, Tan Ge, Zheng Yulin, Zhang Ruonan, Wu Yan, Tang Junming. Platelet-derived growth factor-BB promotes proliferation, differentiation and migration of skeletal muscle myoblast [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1050-1055. |
| [14] | Wang Feng, Zhou Liyu, Saijilafu, Qi Shibin, Ma Yanxia, Wei Shanwen. CaMKII-Smad1 promotes axonal regeneration of peripheral nerves [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1064-1068. |
| [15] | Wang Xianyao, Guan Yalin, Liu Zhongshan. Strategies for improving the therapeutic efficacy of mesenchymal stem cells in the treatment of nonhealing wounds [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1081-1087. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

