Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (32): 5085-5090.doi: 10.3969/j.issn.2095-4344.0395
Therapeutic targets of osteoporosis: correlation of age, body mass index, blood glucose and blood lipids with sclerostin and DKK-1
Zhang Shu-dong1, Zhao Si-cong2, Li Shi-fei1, Zhou Jian1, Yao Qi1, 3
- 1Department of Orthopedics, 2Department of Urology, Beijing Shijitan Hospital, Capital Medical University, Beijing 100038, China; 3Chinese PLA General Hospital, Beijing 100853, China
-
Received:2018-08-07Online:2018-11-18Published:2018-11-18 -
Contact:Yao Qi, MD, Chief physician, Master’s supervisor, Department of Orthopedics, Beijing Shijitan Hospital, Capital Medical University, Beijing 100038, China; Chinese PLA General Hospital, Beijing 100853, China -
About author:Zhang Shu-dong, Master candidate, Department of Orthopedics, Beijing Shijitan Hospital, Capital Medical University, Beijing 100038, China -
Supported by:a grant from the Beijing Municipal Science & Technology Commission, No. Z151100003915094
CLC Number:
Cite this article
Zhang Shu-dong1, Zhao Si-cong2, Li Shi-fei1, Zhou Jian1, Yao Qi1, 3. Therapeutic targets of osteoporosis: correlation of age, body mass index, blood glucose and blood lipids with sclerostin and DKK-1[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(32): 5085-5090.
share this article
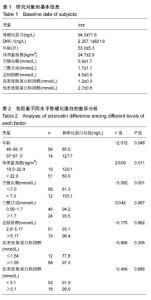
2.1 参与者数量分析 经严格筛选后试验共纳入70例男性受试者,全部进入结果分析。 2.2 受试者的基本特点 70例成年男性的相关资料包括血清骨硬化蛋白、DKK-1、年龄、体质量指数、空腹血糖、三酰甘油、总胆固醇、高密度脂蛋白胆固醇、低密度脂蛋白胆固醇,将其数值进行统计学描述(见表1)。 2.3 骨硬化蛋白、DKK-1与各因素不同水平的比较及其相关性分析 以《中国成人血脂异常防治指南》为依据[18],结合该次收集的数据选择合适的分组方法,对各因素进行统计学分析,以分析各因素不同水平之间骨硬化蛋白和DKK-1是否存在差异。 2.3.1 骨硬化蛋白在各因素不同水平中的比较 综合分析数据后将各因素分为不同水平,分析不同水平之间血清"
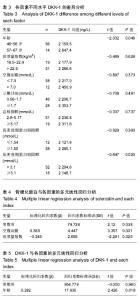
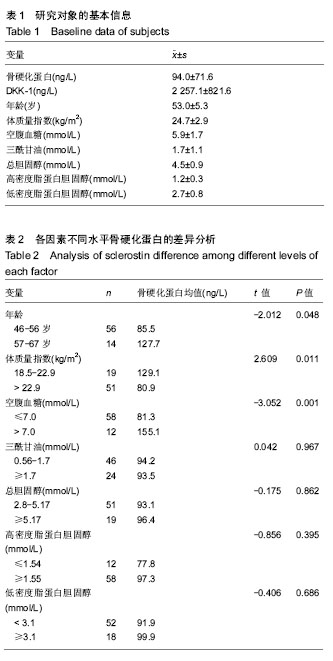

骨硬化蛋白水平,分组方法和统计学分析结果见表2,结果显示不同年龄、体质量指数、空腹血糖水平的骨硬化蛋白差异有显著性意义(P < 0.05),可以认为在相应因素的不同水平中骨硬化蛋白水平存在差异。 2.3.2 DKK-1在各因素不同水平中的比较 参考各因素不同水平中骨硬化蛋白分析方法,对DKK-1进行差异分析,分组信息和分析结果见表3,结果显示不同年龄组中骨硬化蛋白水平统计学分析P < 0.05,结果存在统计学意义,可以认为不同年龄阶段DKK-1的水平存在差异。 2.3.3 骨硬化蛋白与DKK-1的相关性分析 骨硬化蛋白和DKK-1都可以通过与LRP5/6的相互作用参与经典Wnt信号通路的调节过程,该次研究将测得的骨硬化蛋白与DKK-1水平进行相关性分析,检验两者之间是否存在相互作用机制,结果显示两者Pearson Correlation=0.138,P=0.254,两者之间不存在相关性。"
| [1] Balemans W, Ebeling M, Patel N, et al. Increased bone density in sclerosteosis is due to the deficiency of a novel secreted protein (SOST). Hum Mol Genet. 2001 1;10(5):537-543.. [2] Balemans W, Van Hul W. Human genetics of SOST. J Musculoskelet Neuronal Interact.2006;6(4):355-356. [3] Brunkow M. Bone dysplasia sclerosteosis results from loss of the SOST gene product, a novel cystine knot-containing protein. Am J Hum Genet. 2001;68(3):577-589. [4] Delgado-Calle J, Sato A Y, Bellido T. Role and mechanism of action of sclerostin in bone. Bone.2016;96:29. [5] Wu Y, Xu SY, Liu SY, et al. Upregulated serum sclerostin level in the T2DM patients with femur fracture inhibits the expression of bone formation/remodeling-associated biomarkers via antagonizing Wnt signaling. Eur Rev Med Pharmacol Sci. 2017;21(3):470-478. [6] Behets GJ, Viaene L, Meijers B, et al. Circulating levels of sclerostin but not DKK1 associate with laboratory parameters of CKD-MBD.Plos One.2017;12(5):e0176411. [7] Wei L, Guan L, Yan Z, et al. Sclerostin as a new key factor in vascular calcification in chronic kidney disease stages 3 and 4. Int Urol Nephrol. 2016;48(12):2043-2050. [8] Shen J, Meyers CA, Shrestha S, et al. Sclerostin Expression in Skeletal Sarcomas. Human Pathology.2016;58:24-34. [9] Hudson BD, Hum NR, Thomas CB, et al. SOST Inhibits Prostate Cancer Invasion. Plos One.2015;10(11):e0142058. [10] Zhu M, Liu C, Li S, et al. Sclerostin induced tumor growth, bone metastasis and osteolysis in breast cancer. Sci Rep. 2017;7(1):11399. [11] Ukita M, Yamaguchi T, Ohata N, et al. Sclerostin Enhances Adipocyte Differentiation in 3T3‐L1 Cells. J Cell Biochem. 2016;117(6): 1419-1428. [12] Koide M, Kobayashi Y, Yamashita T, et al. Bone formation is coupled to resorption via suppression of sclerostin expression by osteoclasts. J Bone Miner Res. 2017;32(10):2074-2086. [13] Menezes ME, Devine DJ, Shevde L A, et al. Dickkopf1: a tumor suppressor or metastasis promoter? Int J Cancer. 2012;130(7): 1477-1483. [14] Tian J, Xu XJ, Shen L, et al. Association of Serum Dkk-1 Levels with β-catenin in Patients with Postmenopausal Osteoporosis. J Huazhong Univ Sci Technolog Med Sci. 2015;35(2):212-218. [15] Xue J, Yang J, Yang L, et al. Dickkopf-1 Is a Biomarker for Systemic Lupus Erythematosus and Active Lupus Nephritis. J Immunol Res. 2017;2017:6861575. [16] Zarei A, Hulley PA, Sabokbar A, et al. Co-expression of DKK-1 and Sclerostin in Subchondral Bone of the Proximal Femoral Heads from Osteoarthritic Hips. Calcif Tissue Int.2017; 100(6):609-618. [17] Shen L, Wu X, Tan J, et al. Combined detection of dickkopf-1 subtype classification autoantibodies as biomarkers for the diagnosis and prognosis of non-small cell lung cancer. Onco Targets Ther. 2017;10: 3545-3556. [18] Cui R, Lin Z, Li Z, et al. Assessment risk of osteoporosis in Chinese people: relationship among body mass index, serum lipid profiles, blood glucose, and bone mineral density. Clin Interv Aging. 2016;11: 887-895. [19] Pietrzyk B, Smertka M, Chudek J. Sclerostin: Intracellular mechanisms of action and its role in the pathogenesis of skeletal and vascular disorders. Advances in clinical and experimental medicine. Adv Clin Exp Med. 2017;26(8):1283-1291. [20] Xie W, Zhou L, Li S, et al. Wnt/β-catenin signaling plays a key role in the development of spondyloarthritis. Ann N Y Acad Sci. 2016;1364: 25-31. [21] Zimmerman Z F, Moon RT, Chien AJ. Targeting Wnt pathways in disease. Cold Spring Harb Perspect Biol. 2012;4(11). pii: a008086. [22] Zhou Y, Wang T, Hamilton JL, et al. Wnt/β-catenin Signaling in Osteoarthritis and in Other Forms of Arthritis. Curr Rheumatol Rep. 2017 Sep;19(9):53. [23] Coulson J, Bagley L, Barnouin Y, et al. Circulating levels of dickkopf-1, osteoprotegerin and sclerostin are higher in old compared with young men and women and positively associated with whole-body bone mineral density in older adults. Osteoporos Int. 2017;28(9):2683-2689. [24] Bhattoa HP, Wamwaki J, Kalina E, et al. Serum sclerostin levels in healthy men over 50Â years of age. J Bone Miner Metab. 2013;31(5): 579-584. [25] Amrein K, Amrein S, Drexler C, et al. Sclerostin and its association with physical activity, age, gender, body composition, and bone mineral content in healthy adults. J Clin Endocrinol Metab. 2012; 97(1):148-154. [26] Gerber LM, Bener A, Alali HM, et al. Bone Mineral Density in Midlife Women: the Study of Women’s Health in Qatar. Climacteric. 2015; 18(2):316-322.[27] Lloyd JT, Alley DE, Hawkes WG, et al. Body mass index is positively associated with bone mineral density in US older adults. Arch Osteoporos. 2014;9:175. [28] Metzger TA, Schwaner SA, Laneve AJ, et al. Pressure and shear stress in trabecular bone marrow during whole bone loading. J Biomech. 2015;48(12):3035-3043. [29] Yu O H Y, Richards B, Berger C, et al. The association between sclerostin and incident type 2 diabetes risk: a cohort study. Clin Endocrinol (Oxf). 2017;86(4):520-525. [30] Tsentidis C, Gourgiotis D, Kossiva L, et al. Sclerostin distribution in children and adolescents with type 1 diabetes mellitus and correlation with bone metabolism and bone mineral density. Pediatric Diabetes. 2016;17(4):289-299. [31] Hygum K, Starup-Linde J, Harsløf T, et al. MECHANISMS IN ENDOCRINOLOGY: Diabetes mellitus, a state of low bone turnover - a systematic review and meta-analysis. Eur J Endocrinol. 2017;176(3): R137-R157. [32] Faienza M F, Ventura A, Delvecchio M, et al. High Sclerostin and Dickkopf-1 (DKK-1) Serum Levels in Children and Adolescents With Type 1 Diabetes Mellitus. J Clin Endocrinol Metab. 2017;102(4): 1174-1181. [33] Sundararaghavan V, Mazur MM, Evans B, et al. Diabetes and bone health: latest evidence and clinical implications. Ther Adv Musculoskelet Dis. 2017;9(3):67-74. [34] Wongdee K, Charoenphandhu N. Up date on type 2 diabetes-related osteoporosis. World J Diabetes. 2015;6(5):673-678. [35] Cui LH, Shin MH, Chung EK, et al. Association between bone mineral densities and serum lipid profiles of pre- and post-menopausal rural women in South Korea. Osteoporos Int. 2005;16(12):1975-1981. [36] Li S, Guo H, Liu Y, et al. Relationships of serum lipid profiles and bone mineral density in postmenopausal Chinese women. Clin Endocrinol (Oxf). 2015;82(1):53-58. [37] Cosman F, Crittenden D B, Adachi J D, et al. Romosozumab Treatment in Postmenopausal Women with Osteoporosis. N Engl J Med. 2016;375(16):1532-1543. [38] Recker R, Benson C, Matsumoto T, et al. A randomized, double-blind phase 2 clinical trial of blosozumab, a sclerostin antibody, in postmenopausal women with low bone mineral density. J Bone Miner Res. 2015;30(2):216-24. [39] Butler JS, Murray DW, Hurson CJ, et al. The role of Dkk1 in bone mass regulation: Correlating serum Dkk1 expression with bone mineral density. J Orthop Res. 2011;29(3):414-418. [40] Dovjak P, Dorfer S, Kudlacek S, et al. Serum levels of sclerostin and dickkopf-1: effects of age, gender and fracture status.Gerontology. 2014;60(6):493-501. [41] Hampson G, Edwards S, Conroy S, et al. The relationship between inhibitors of the Wnt signalling pathway (Dickkopf-1(DKK1) and sclerostin), bone mineral density, vascular calcification and arterial stiffness in post-menopausal women.Bone.2013;56(1):42-47. [42] Glantschnig H, Hampton R A, Lu P, et al. Generation and selection of novel fully human monoclonal antibodies that neutralize Dickkopf-1 (DKK1) inhibitory function in vitro and increase bone mass in vivo. J Biol Chem. 2010;285(51):40135-40147. [43] Goldstein S D, Matteo T, Bautista G W, et al. A monoclonal antibody against the Wnt signaling inhibitor dickkopf-1 inhibits osteosarcoma metastasis in a preclinical model. Oncotarget, 2016;7(16):21114-21123. [44] Kato T, Khanh VC, Sato K, et al. Elevated expression of Dkk-1 by glucocorticoid treatment impairs bone regenerative capacity of adipose tissue-derived mesenchymal stem cells. Stem Cells Dev. 2018;27(2):85-99. [45] Monica F, Kannan G, Marina S, et al. A bispecific antibody targeting sclerostin and DKK-1 promotes bone mass accrual and fracture repair. Nat Commun. 2016;7:11505. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Tang Hui, Yao Zhihao, Luo Daowen, Peng Shuanglin, Yang Shuanglin, Wang Lang, Xiao Jingang. High fat and high sugar diet combined with streptozotocin to establish a rat model of type 2 diabetic osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1207-1211. |
| [3] | Chen Jiming, Wu Xiaojing, Liu Tianfeng, Chen Haicong, Huang Chengshuo. Effects of silymarin on liver injury and bone metabolism induced by carbon tetrachloride in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1224-1228. |
| [4] | Geng Qiudong, Ge Haiya, Wang Heming, Li Nan. Role and mechanism of Guilu Erxianjiao in treatment of osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1229-1236. |
| [5] | Li Zhongfeng, Chen Minghai, Fan Yinuo, Wei Qiushi, He Wei, Chen Zhenqiu. Mechanism of Yougui Yin for steroid-induced femoral head necrosis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1256-1263. |
| [6] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [7] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [8] | Li Shibin, Lai Yu, Zhou Yi, Liao Jianzhao, Zhang Xiaoyun, Zhang Xuan. Pathogenesis of hormonal osteonecrosis of the femoral head and the target effect of related signaling pathways [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 935-941. |
| [9] | Zheng Xiaolong, He Xiaoming, Gong Shuidi, Pang Fengxiang, Yang Fan, He Wei, Liu Shaojun, Wei Qiushi. Bone turnover characteristics in patients with alcohol-induced osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 657-661. |
| [10] | Xiao Fangjun, Chen Shudong, Luan Jiyao, Hou Yu, He Kun, Lin Dingkun. An insight into the mechanism of Salvia miltiorrhiza intervention on osteoporosis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 772-778. |
| [11] | Liu Bo, Chen Xianghe, Yang Kang, Yu Huilin, Lu Pengcheng. Mechanism of DNA methylation in exercise intervention for osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 791-797. |
| [12] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [13] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [14] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [15] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||