Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (11): 1665-1670.doi: 10.3969/j.issn.2095-4344.0160
Previous Articles Next Articles
Influence of the artificial disc size on cervical artificial disc replacement
Song Qing-peng, Tian Wei, He Da, Han Xiao, Wang Jin-chao, Li Zu-chang, Feng Xiao
- Department of Spine Surgery, Beijing Jishuitan Hospital, Fourth Clinical Medical College of Peking University, Beijing 100035, China
-
Online:2018-04-18Published:2018-04-18 -
Contact:Tian Wei, Professor, Doctoral supervisor, Chief physician, Department of Spine Surgery, Beijing Jishuitan Hospital, Fourth Clinical Medical College of Peking University, Beijing 100035, China -
About author:Song Qing-peng, Doctoral candidate, Physician, Department of Spine Surgery, Beijing Jishuitan Hospital, Fourth Clinical Medical College of Peking University, Beijing 100035, China -
Supported by:the Scientific Research Program of Health Bureau of Beijing City, No. QML20160402; the Special Funding Project of the Beijing Municipal Science and Technology Committee, No. Z161100000516134
CLC Number:
Cite this article
Song Qing-peng, Tian Wei, He Da, Han Xiao, Wang Jin-chao, Li Zu-chang, Feng Xiao. Influence of the artificial disc size on cervical artificial disc replacement[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(11): 1665-1670.
share this article
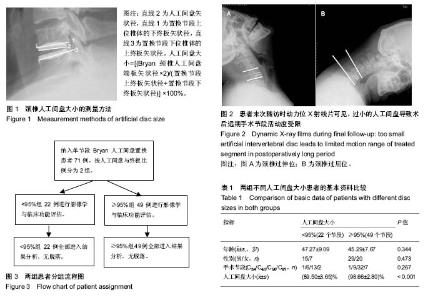
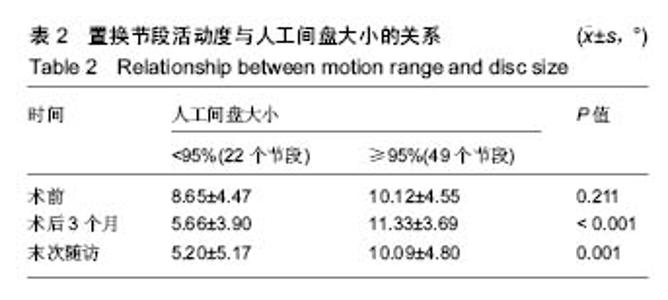
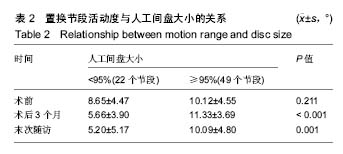
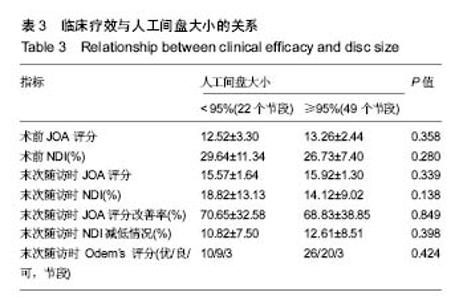
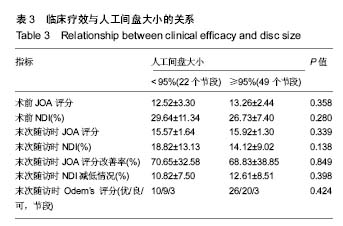
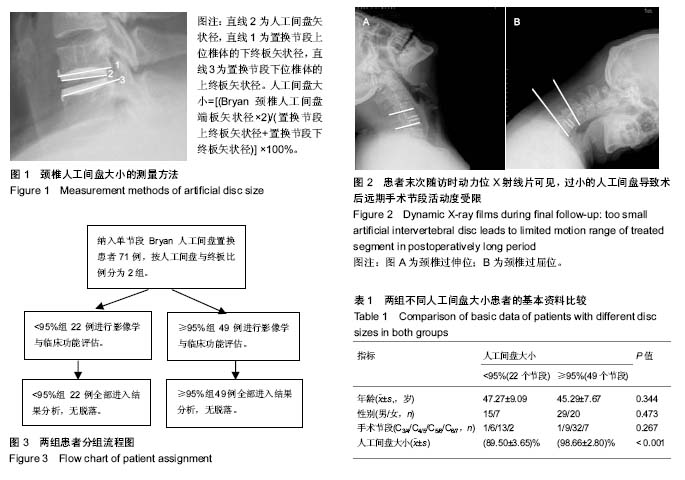
2.1 参与者数量分析 符合入组条件患者共89例,完成10年以上随访患者共71例,10年以上随访率为80%。其中人工间盘大小<95%组22例,≥95%组49例。试验流程图见图3。 2.2 基本资料 人工间盘大小<95%组患者共22例,年龄(47.27±9.09)岁(33-69岁);男15例,女7例;其中C3/4节段1例,C4/5节段6例,C5/6节段13例,C6/7节段2例;人工间盘的大小为(89.50±3.65)%;随访时间120-155个月。 人工间盘大小≥95%组患者共49例,年龄(45.29±7.67)岁(26-64岁);男29例,女性20例;其中C3/4节段1例,C4/5节段9例,C5/6节段32例,C6/7节段7例;人工间盘的大小为(98.66±2.80)%;随访时间121-154个月。 2组除人工间盘大小差异有显著性意义(P < 0.05),其余数据差异均无显著性意义,见表1。 2.3 影像学评估结果 术后3个月随访时,人工间盘大小<95%组置换节段活动度为(5.66±3.90)°,≥95%组为(11.33±3.69)°;末次随访时,人工间盘的大小<95%组置换节段活动度为(5.20±5.17)°,≥95%组为(10.09±4.80)°,差异有显著性意义(P < 0.05),见表2。 2.4 临床功能评估结果 2.4.1 JOA评分 人工间盘大小<95%组术前JOA评分为12.52±3.30(6.5-16.5),末次随访时JOA评分改善率为(70.65±32.58)%;人工间盘大小≥95%组术前JOA评分为13.26±2.44(4.0-16.5),末次随访时JOA评分改善率为(68.83±38.85)%,2组间各数据差异无显著性意义(P > 0.05),见表3。 2.4.2 NDI 人工间盘大小<95%组术前NDI为(29.64± 11.34)%(16%-52%),末次随访时NDI减低(10.82±7.50)%;人工间盘大小≥95%组术前NDI为(26.73±7.40)% (10%-50%),末次随访时NDI减低(12.61±8.51)%。2组间各数据差异无显著性意义(P > 0.05),见表3。 2.4.3 Odem’s评分 末次随访时,人工间盘大小<95%组Odem’s评分优10例(45%),良9例(41%),可3例(14%);人工间盘大小≥95%组Odem’s评分优26例(53%),良20例(41%),可3例(6%)。2组间差异无显著性意义(P > 0.05),见表3。"
| [1] Tian W, Han X, Liu B, et al. Clinical and radiographic results of cervical artificial disc arthroplasty: over three years follow-up cohort study. Chin Med J. 2010;123(21): 2969-2973.[2] Wu AM, Xu H, Mullinix KP, et al. Minimum 4-year outcomes of cervical total disc arthroplasty versus fusion: a meta-analysis based on prospective randomized controlled trials. Medicine. 2015;94(15):e665.[3] Shriver MF, Lubelski D, Sharma AM, et al. Adjacent segment degeneration and disease following cervical arthroplasty: a systematic review and meta-analysis. Spine J. 2016;16(2):168-181.[4] 韩骁,田伟,刘波,等. 不同影像学及症状学诊断颈椎退行性疾病患者行人工颈椎间盘置换术的中长期随访研究[J]. 中华骨与关节外科杂志, 2015, 8(1):15-20.[5] Quan GM, Vital JM, Hansen S, et al. Eight-year clinical and radiological follow-up of the Bryan cervical disc arthroplasty. Spine. 2011;36(8):639-646.[6] Thaler M, Hartmann S, Gstöttner M, et al. Footprint mismatch in total cervical disc arthroplasty. Eur Spine J. 2013;22(4):759-765.[7] Feng H, Fang XY, Huang DG, et al. A morphometric study of the middle and lower cervical vertebral endplates and their components. Medicine. 2017;96(10):e6296.[8] Ganbat D, Kim YH, Kim K, et al. Effect of mechanical loading on heterotopic ossification in cervical total disc replacement: a three-dimensional finite element analysis. Biomech Model Mechanobiol. 2015;15(5):1191-1199.[9] Lin CY, Kang HJ. Stress analysis of the interface between cervical vertebrae end plates and the Bryan, Prestige LP, and ProDisc-C cervical disc prostheses: an in vivo image-based finite element study. Spine. 2009;34(15):1554-1560.[10] 伍少玲,马超,伍时玲,等. 颈椎功能障碍指数量表的效度与信度研究[J]. 中国康复医学杂志, 2008, 23(7):625-628.[11] 田伟,吕艳伟,刘亚军,等. 北京市18岁以上居民颈椎病现况调查研究[J]. 中华骨科杂志,2012,32(8):707-713.[12] Burkhardt BW, Brielmaier M, Schwerdtfeger K, et al. Smith-Robinson procedure with an autologous iliac crest graft and caspar plating: report of 65 patients with an average follow-up of 22 years. World Neurosurg. 2016;90:244-250.[13] Burkhardt BW, Brielmaier M, Schwerdtfeger K, et al. Clinical outcome following anterior cervical discectomy and fusion with and without anterior cervical plating for the treatment of cervical disc herniation—a 25-year follow-up study. Neurosurg Rev. 2017. doi: 10.1007/s10143-017-0872-6. [Epub ahead of print][14] Kim SJ, Sang DK. Anterior cervical discectomy and fusion using a double cylindrical cage versus an anterior cervical plating system with iliac crest autografts for the treatment of cervical degenerative disc disease. J Korean Neurosurg Soc. 2014;55(1):12-17.[15] Shao MH, Fan Z, Yin J, et al. Titanium cages versus autogenous iliac crest bone grafts in anterior cervical discectomy and fusion treatment of patients with cervical degenerative diseases: a systematic review and meta-analysis. Curr Med Res Opin. 2017;33(5):803-811.[16] Sayyahmelli S, Alipanahi R. Anterior cervical discectomy and fusion with polyether ether ketone cage. Global Spine J. 2014;4(S1): 1023-1025.[17] Phillips FM, Geisler FH, Gilder KM, et al. Long-term outcomes of the US FDA IDE prospective, randomized controlled clinical trial comparing PCM cervical disc arthroplasty with anterior cervical discectomy and fusion. Spine. 2015;40(10):674-683.[18] van Eck CF, Regan C, Donaldson WF, et al. The revision rate and occurrence of adjacent segment disease after anterior cervical discectomy and fusion: a study of 672 consecutive patients. Spine. 2015;15(10):S165-S165.[19] Kong L, Cao J, Wang L, et al. Prevalence of adjacent segment disease following cervical spine surgery: A PRISMA-compliant systematic review and meta-analysis. Medicine. 2016;95(27):e4171.[20] Li J, Tong T, Niu R, et al. A study on the clinical outcomes of patients with revision surgery for adjacent segment disease after 10-year’s anterior cervical spine surgery. J Orthop Surg Res. 2016;11(1):5.[21] Zhang Y, Liang C, Tao Y, et al. Cervical total disc replacement is superior to anterior cervical decompression and fusion: a meta-analysis of prospective randomized controlled trials. Plos One. 2015;10(3):e0117826.[22] Demetriades AK, Ringel F, Meyer B. Cervical disc arthroplasty: a critical review and appraisal of the latest available evidence[M]// Advances and technical standards in neurosurgery. Springer International Publishing, 2014:107.[23] Qiang Y, Feng L, Yang X, et al. A meta-analysis comparing total disc arthroplasty with anterior cervical discectomy and fusion for the treatment of cervical degenerative diseases. Arch Orthop Trauma Surg. 2016;136(3):297-304.[24] Fay LY, Huang WC, Wu JC, et al. Arthroplasty for cervical spondylotic myelopathy: similar results to patients with only radiculopathy at 3 years' follow-up. J Neurosurg Spine. 2014;21(3):400-410.[25] Lee JH, Park WM, Kim YH, et al. A biomechanical analysis of an artificial disc with a shock-absorbing core property by using whole-cervical spine finite element analysis. Spine. 2016;41(15):E893.[26] Mcdonald CP, Chang V, Mcdonald M, et al. Three-dimensional motion analysis of the cervical spine for comparison of anterior cervical decompression and fusion versus artificial disc replacement in 17 patients: clinical article. J Neurosurg Spine. 2014; 20(3):245-255.[27] Mo Z, Zhao Y, Du C, et al. Does location of rotation center in artificial disc affect cervical biomechanics? Spine. 2015;40(8):E469.[28] Mummaneni PV, Burkus JK, Haid RW, et al. Clinical and radiographic analysis of cervical disc arthroplasty compared with allograft fusion: a randomized controlled clinical trial. J Neurosurg Spine. 2007;6(3):198.[29] Galbusera F, Bellini CM, Brayda-Bruno M, et al. Biomechanical studies on cervical total disc arthroplasty: A literature review. Clin Biomech. 2008;23(9):1095-1104.[30] Yanbin Z, Yu S. In vitro biomechanics of cervical arthroplasty with Bryan disc prosthesis or ProDisc-C prosthesis: a cadaveric study. Global Spine J. 2014.[31] Lazaro BC, Yucesoy K, Yuksel KZ, et al. Effect of arthroplasty design on cervical spine kinematics: analysis of the Bryan Disc, ProDisc-C, and Synergy disc. Neurosurg Focus. 2010;28(6):E6.[32] Ryu W H, Kowalczyk I, Duggal N. Long-term kinematic analysis of cervical spine after single-level implantation of Bryan cervical disc prosthesis. Spine J. 2013;13(6):628-634.[33] Zhao Y, Zhang Y, Sun Y, et al. Application of cervical arthroplasty with bryan cervical disc: 10-year follow-up results in China. Spine, 2016; 41(2):111.[34] Liberati C, Assietti R. Clinical and radiological results of Bryan cervical disc arthroplasty after follow-up of ten years. Spine J. 2015;15(10): S124-S124.[35] Dejaegher J, Walraevens J, Loon J V, et al. 10-year follow-up after implantation of the Bryan cervical disc prosthesis. Eur Spine J. 2017;26(4):1191-1198.[36] 戎鑫,刘浩,龚全,等. 颈椎下终板矢状面形态分型[J]. 中国矫形外科杂志, 2015,23(5):406-411.[37] Beer ND, Scheffer C. Reducing subsidence risk by using rapid manufactured patient-specific intervertebral disc implants. Spine J. 2012;12(11):1060-1066.[38] Tan SH,Teo EC,Chua HC,et al.Quantitative three-dimensional anatomy of cervical, thoracic and lumbar vertebrae of Chinese Singaporeans. Eur Spine J.2004;13(2):137-146.[39] Kim MK,Kwak DS,Park CK,et al.Quantitative anatomy of the endplate of the middle and lower cervical vertebrae in Koreans.Spine (Phila Pa 1976). 2007;32(14):E376-381. [40] Jin YJ, Park SB, Kim MJ, et al. An analysis of heterotopic ossification in cervical disc arthroplasty: a novel morphologic classification of an ossified mass. Spine J. 2013;13(4):408.[41] Lei T, Liu Y, Wang H, et al. Clinical and radiological analysis of Bryan cervical disc arthroplasty: eight-year follow-up results compared with anterior cervical discectomy and fusion. Int Orthop. 2016;40(6): 1197-1203.[42] Dejaegher J, Walraevens J, Van LJ, et al. 10-year follow-up after implantation of the Bryan Cervical Disc Prosthesis. Eur Spine J. 2017;26(4):1191-1198.[43] 张传健,丁坦,王哲,等. 人工颈椎间盘置换术临床应用探讨与存在问题[J].中国矫形外科杂志,2017,25(5):442-447.[44] Yi S, Kim KN, Yang MS, et al. Difference in occurrence of heterotopic ossification according to prosthesis type in the cervical artificial disc replacement. Spine. 2010;35(16):1556-1561. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [12] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [13] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [14] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [15] | Liu Liyong, Zhou Lei. Research and development status and development trend of hydrogel in tissue engineering based on patent information [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3527-3533. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||