Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (34): 9002-9007.doi: 10.12307/2026.871
Previous Articles Next Articles
Correlation between body mass index and early recovery outcomes after kidney transplantation
Zhong Xiaoping1, Chen Dan1, Xie Nianhua2
- 1Wuhan University of Science and Technology, Wuhan 430011, Hubei Province, China; 2Wuhan Center for Disease Control & Prevention, Wuhan 430024, Hubei Province, China
-
Received:2025-08-20Revised:2026-01-26Online:2026-12-08Published:2026-04-14 -
Contact:Xie Nianhua, MS, Associate chief physician, Wuhan Center for Disease Control & Prevention, Wuhan 430024, Hubei Province, China -
About author:Zhong Xiaoping, Wuhan University of Science and Technology, Wuhan 430011, Hubei Province, China -
Supported by:
CLC Number:
Cite this article
Zhong Xiaoping, Chen Dan, Xie Nianhua. Correlation between body mass index and early recovery outcomes after kidney transplantation[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(34): 9002-9007.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
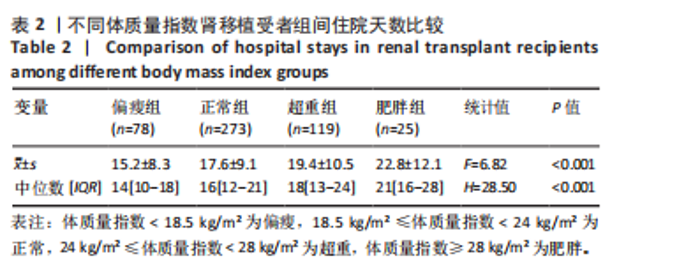
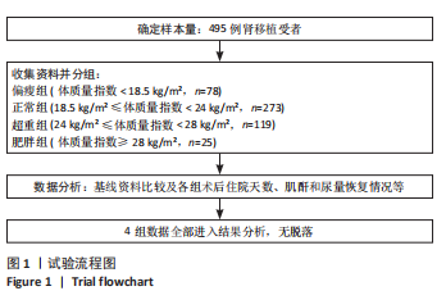
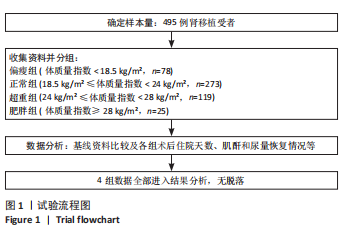
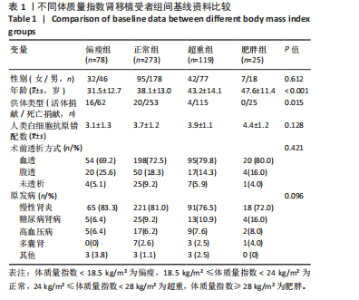
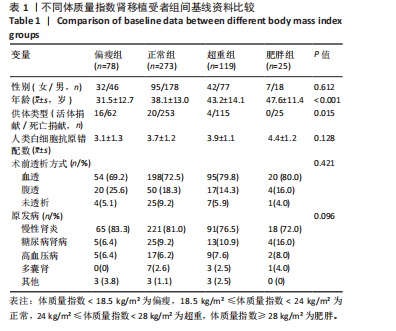
活体供体占比最高(20.5%),差异有显著性意义(P=0.015)。肥胖受者在大多数中心被要求减肥后进行活体肾移植,有利于术后恢复等,所以肥胖受者在活体肾移植中占比相对较少。 2.4 住院天数与体质量指数分层的关联 不同体质量指数分组的住院天数差异如表2所示。根据体质量指数分组,偏瘦组、正常组、超重组及肥胖组的住院天数呈现显著递增趋势。统计检验结果表明,各组间住院天数的差异有显著性意义。单因素方差分析(ANOVA)显示,F=6.82,P < 0.001;非参数Kruskal-Wallis检验结果为H=28.5,P < 0.001。以上结果提示,体质量指数较高的肾移植受者术后住院时间显著延长,且该趋势随体质量指数升高而愈发明显。这一发现支持了体质量指数与术后恢复速度的负相关性,可能为临床制定个体化康复策略提供依据。"
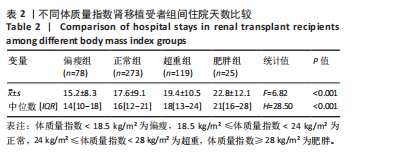
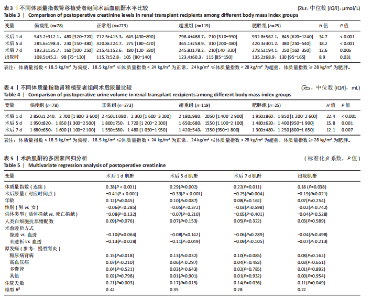
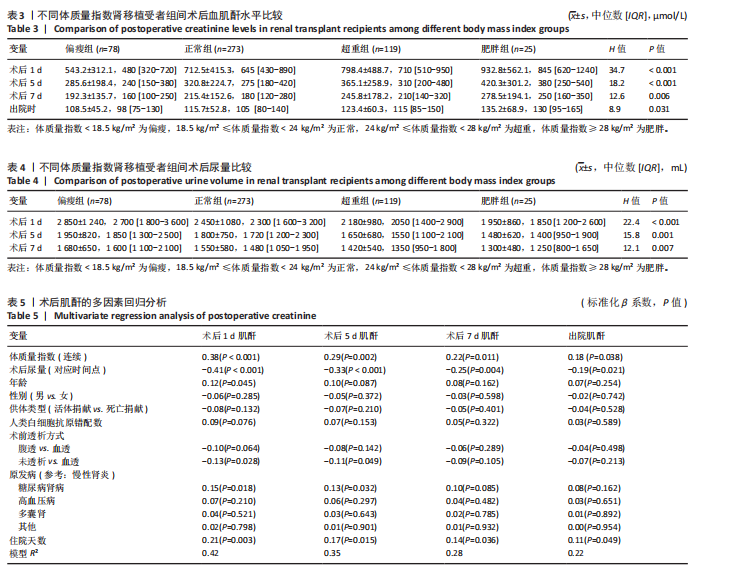
2.5 术后肾功能恢复的体质量指数依赖性 不同体质量指数受者的术后血肌酐水平差异如表3所示。根据体质量指数分组,偏瘦组、正常组、超重组及肥胖组的术后肌酐下降速度呈现显著递减趋势。 非参数Kruskal-Wallis检验结果显示,术后各时间点及出院时的组间差异均有显著性意义(术后1 d:H=34.7,P < 0.001;术后5 d:H=18.2,P < 0.001;术后7 d:H=12.6,P=0.006;出院时:H=8.9,P=0.031)。数据表明,体质量指数较高的肾移植受者术后肌酐水平显著高于低体质量指数组,且随着体质量指数升高,术后肌酐恢复速度减缓,出院时肥胖组的肌酐值仍处于较高水平。这一结果进一步支持了体质量指数与术后肾功能恢复的负相关性,提示肥胖可能影响肾移植后代谢清除效率,需在临床管理中加强监测与干预。 不同体质量指数受者的术后尿量差异如表4所示。偏瘦组、正常组、超重组及肥胖组的术后早期尿量呈现显著递减趋势。非参数Kruskal-Wallis检验结果显示,术后各时间点的组间差异均有显著性意义(术后1 d:H=22.4,P < 0.001;术后5 d:H=15.8,P=0.001;术后7 d:H=12.1,P=0.007)。数据表明,体质量指数较高的肾移植受者术后尿量显著低于低体质量指数组,且随着体质量指数升高,尿量减少的趋势持续至术后第7天。这一结果与前期发现的体质量指数与住院天数延长、肌酐水平升高的负相关性一致,提示肥胖可能影响术后肾功能恢复及体液代谢效率。 2.6 体质量指数对术后肌酐的独立影响 在肾移植术后肌酐恢复的多因素回归分析中,体质量指数和术后尿量被确定为影响术后肌酐水平的关键独立因素,见表5。结果显示,体质量指数作为连续变量与术后各时间点肌酐水平呈显著正相关(术后1 d:β=0.38,P < 0.001;术后5 d:β=0.29,P=0.002;术后7 d:β=0.22,P=0.011;出院时:β=0.18,P=0.038),表明体质量指数每增加1 kg/m2,术后肌酐水平相应升高。术后尿量则与肌酐水平呈显著负相关(术后1 d:β=-0.41,P < 0.001;术后5 d:β=-0.33,P < 0.001;术后7 d:β=-0.25,P=0.004;出院时:β=-0.19,P=0.021),提示尿量增加可能通过改善体液代谢降低肌酐水平。 其他显著影响因素有:①年龄在术后1 d对肌酐水平有正向影响(β=0.12,P=0.045),但随着时间推移影响减弱;②未透析患者(vs.血透)在术后早期(1 d和5 d)与较低肌酐水平相关(β=-0.13,P=0.028;β=-0.11,P=0.049);③糖尿病肾病(vs.慢性肾炎)显著增加术后1 d(β=0.15,P=0.018)和5 d(β=0.13,P=0.032)的肌酐水平;④住院天数在所有时间点均与肌酐水平正相关(术后1 d:β=0.21,P=0.003;出院时:β=0.11,P=0.049),提示住院时间延长可能反映肾功能恢复延迟。非显著变量如性别、供体类型(活体捐献 vs. 死亡捐献)、人类白细胞抗原错配数及多数原发病类型(如高血压病、多囊肾)对肌酐水平的影响未达到统计学意义。模型整体解释力随时间递减(术后1 d R2=0.42,出院时R2=0.22),表明术后早期肌酐水平更多受可量化因素影响,而后期可能受未观测变量(如个体代谢差异、"
| [1] WAN SS, CANTAROVICH M, MUCSI I, et al. Early renal function recovery and long-term graft survival in kidney transplantation. Transpl Int. 2016;29(5):619-626. [2] MOTTOLA C, GIRERD N, DUARTE K, et al. Prognostic value for long-term graft survival of estimated glomerular filtration rate and proteinuria quantified at 3 months after kidney transplantation. Clin Kidney J. 2020;13(5):791-802. [3] Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organ Tech Rep Ser. 2000;894:1-253. [4] WHO Expert Consultation. Appropriate body-mass index for asian populations and its implications for policy and intervention strategies. Lancet. 2004; 363(9403):157-163. [5] 中国肥胖问题工作组. 中国成人超重和肥胖症预防与控制指南(节录)[J]. 营养学报,2004(1):1-4. [6] KAWAI T, AUTIERI MV, SCALIA R. Adipose tissue inflammation and metabolic dysfunction in obesity. Am J Physiol Cell Physiol. 2021;320(3):C375-C391. [7] LAKKIS JI, WEIR MR. Obesity and kidney disease. Prog Cardiovasc Dis. 2018;61(2): 157-167. [8] BERNARDO DRD, CANALE D, NASCIMENTO MM, et al. The association between obesity and vitamin d deficiency modifies the progression of kidney disease after ischemia/reperfusion injury. Front Nutr. 2022;9:952028. [9] CHANG J, MUSHAILOV V, MOHAN S. Obesity and kidney transplantation. Curr Opin Organ Transplant. 2023;28(2):149-155. [10] AZHAR A, HASSAN N, TAPOLYAI M, et al. Obesity, chronic kidney disease, and kidney transplantation: an evolving relationship. Semin Nephrol. 2021;41(2): 189-200. [11] CHAN W, SMITH B, STEGALL M, et al. Obesity and metabolic syndrome in kidney transplantation: the role of dietary fructose and systemic endotoxemia. Transplantation. 2019;103(1):191-201. [12] BOIMA V, AGYEKUM AB, GANATRA K, et al. Advances in kidney disease: pathogenesis and therapeutic targets. Front Med (Lausanne). 2025;12:1526090. [13] WORKENEH B, MOORE LW, NOLTE FONG JV, et al. Successful kidney transplantation is associated with weight gain from truncal obesity and insulin resistance. J Ren Nutr. 2019;29(6):548-555. [14] LIESE J, BOTTNER N, BUTTNER S, et al. Influence of the recipient body mass index on the outcomes after kidney transplantation. Langenbecks Arch Surg. 2018; 403(1):73-82. [15] ORLIC L, MIKOLASEVIC I, JAKOPCIC I, et al. Body mass index: short- and long-term impact on kidney transplantation. Int J Clin Pract. 2015;69(11):1357-1365. [16] 钱才媛, 王殿珍, 梅童童, 等. BMI与肾移植术后早期恢复效果的关系[J]. 现代医药卫生,2022,38(5):847-849. [17] 董丽明, 江艳, 热衣汉·谢力甫, 等. 体重指数与早期移植肾功能的关系[J]. 器官移植,2015,6(4):254-257. [18] SCHROPPEL B, LEGENDRE C. Delayed kidney graft function: from mechanism to translation. Kidney Int. 2014;86(2):251-258. [19] SIEDLECKI A, IRISH W, BRENNAN DC. Delayed graft function in the kidney transplant. Am J Transplant. 2011;11(11):2279-2296. [20] CHADBAN SJ, AHN C, AXELROD DA, et al. KDIGO clinical practice guideline on the evaluation and management of candidates for kidney transplantation. Transplantation. 2020;104(4S1 Suppl 1):S11-S103. [21] CHADBAN SJ, AHN C, AXELROD DA, et al. Summary of the kidney disease: improving global outcomes (KDIGO) clinical practice guideline on the evaluation and management of candidates for kidney transplantation. Transplantation. 2020;104(4):708-714. [22] 李杨, 林俊, 王钢. 中国肾脏移植围手术期处理临床诊疗指南[J]. 器官移植, 2025,16(1):21-38. [23] 中华医学会器官移植学分会, 中国医疗保健国际交流促进会肾脏移植学分会. 中国肾脏移植长期健康管理指南(2023版)[J]. 中华器官移植杂志,2024, 45(5):283-298. [24] FIPPS DC, SINHA S, DIWAN TS, et al. Psychosocial considerations in the combined bariatric surgery and organ transplantation population: a review of the overlapping pathologies and outcomes. Curr Opin Organ Transplant. 2022;27(6): 514-522. [25] DIWAN TS, LEE TC, NAGAI S, et al. Obesity, transplantation, and bariatric surgery: an evolving solution for a growing epidemic. Am J Transplant. 2020;20(8):2143-2155. [26] GHANEM OM, PITA A, NAZZAL M, et al. Obesity, organ failure, and transplantation: a review of the role of metabolic and bariatric surgery in transplant candidates and recipients. Surg Endosc. 2024;38(8):4138-4151. [27] SAGES Guidelines Committee. SAGES guideline for clinical application of laparoscopic bariatric surgery. Surg Obes Relat Dis. 2009;5(3):387-405. [28] SCHREIBER PW, HOESSLY LD, BOGGIAN K, et al. Surgical site infections after kidney transplantation are independently associated with graft loss. Am J Transplant. 2024;24(5):795-802. [29] 中华医学会器官移植学分会, 中国医疗保健国际交流促进会肾脏移植学分会. 中国肾脏移植活体捐献供者医学评估临床指南(2023版)[J]. 中华器官移植杂志,2024,45(12):839-849. [30] 中国医师协会器官移植医师分会中华医学会器官移植学分会. 中国活体供肾移植临床指南(2016版)[J]. 器官移植,2016,7(6):417-426. [31] FELLMANN M, BALSSA L, CLEMENT E, et al. Effects of obesity on postoperative complications and graft survival after kidney transplantation. Transplant Proc. 2020;52(10):3153-3159. [32] MOLNAR MZ, KOVESDY CP, MUCSI I, et al. Higher recipient body mass index is associated with post-transplant delayed kidney graft function. Kidney Int. 2011;80(2):218-224. [33] DA SILVA IO, DE MENEZES NK, JACOBINA HD, et al. Obesity aggravates acute kidney injury resulting from ischemia and reperfusion in mice. Sci Rep. 2024; 14(1):9820. [34] NICOLETTO BB, FONSECA NKO, MANFRO RC, et al. Effects of obesity on kidney transplantation outcomes: a systematic review and meta-analysis. Transplantation. 2014;98(2):167-176. [35] LADHANI M, CRAIG JC, IRVING M, et al. Obesity and the risk of cardiovascular and all-cause mortality in chronic kidney disease: a systematic review and meta-analysis. Nephrol Dial Transplant. 2017;32(3):439-449. [36] GREGG E, JAKICIC J, BLACKBURN G, et al. Association of the magnitude of weight loss and changes in physical fitness with long-term cardiovascular disease outcomes in overweight or obese people with type 2 diabetes: a post-hoc analysis of the look AHEAD randomised clinical trial. Lancet Diabetes Endocrinol. 2016;4(11):913-921. [37] ABRAMOWICZ D, COCHAT P, CLAAS FHJ, et al. European renal best practice guideline on kidney donor and recipient evaluation and perioperative care. Nephrol Dial Transplant. 2015;30(11):1790-1797. [38] GABARRE P, PALACIOS R, PEREZ K, et al. Immunosuppressive drugs and diet interact to modify the gut microbiota and cardiovascular risk factors, and to trigger diabetes. PLoS One. 2025;20(3):e0320438. [39] CHAN W, BOSCH JA, PHILLIPS AC, et al. The associations of endotoxemia with systemic inflammation, endothelial activation, and cardiovascular outcome in kidney transplantation. J Ren Nutr. 2018;28(1):13-27. |
| [1] | Huang Zhengbo, Ou Min, Li Guoshun, Duan Fuhui, Liu Jianqi, Lou Juxiang, Zhao Yanxiu, Su Xiaoyan. Innovative application of kidney organoids in acute kidney injury [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(19): 5040-5049. |
| [2] | Chen Zan, Lei Fei, Ye Fei, Zhou Qingzhong, Yuan Hao, Zheng Lipeng, Zha Xian, Feng Daxiong. Relationship between drainage time and early efficacy after short-segment lumbar fusion [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 927-933. |
| [3] | Li Qingru, Wang Yifan, Chen Guanting, Shi Ruoyu, Zhang Linqi. Extracellular vesicles for acute kidney injury in preclinical research: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(24): 3926-3936. |
| [4] | Zhan Ying, Wu Xiaodan, Hao Shanhu. Establishment of an animal model of radioactive 131I-induced hypothyroidism in rats [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(17): 2631-2636. |
| [5] | Yang Zhiwei, Liu Junchang, Gao Xiaolin, Jiang Taimao. Relationship between tacrolimus metabolic rate and early BK virus infection after kidney transplantation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 712-716. |
| [6] | Li Qingru, Zhang Linqi, Chen Xu, Shi Ruoyu, Wang Xixi. Mesenchymal stem cells-derived extracellular vesicles in the treatment and repair of acute and chronic renal injuries [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(31): 5069-5075. |
| [7] | Xu Yuan, Niu Yulin, Yuan Zhihui, Jia Lei, Pan Guanghui. Up-regulating follicular regulatory T cells for treating antibody-mediated rejection after kidney transplantation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(26): 4118-4122. |
| [8] | Wang Xiaobo, Wang Changan, Han Jianle, Yang Qingyan, Yang Shuaiping, Yang Junwei. Influence of conversion from cyclosporine to tacrolimus on glucose metabolism and cardiovascular risk profiles in stable kidney transplant patients [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(14): 2236-2240. |
| [9] | Wu Kai, Liu Kun, Xie Lin, Lu Guanjun, Ma Shengchao, Li Guizhong, Cao Jun, Jie Yuzhen, Jiang Yideng, Hao Yinju. Mechanism of hyperhomocysteinemia induced renal injury in Cbs+/- mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(11): 1728-1732. |
| [10] | Liu Junchang, Gao Xiaolin, Jiang Taimao. Correlation of CY3A5 genetic polymorphism with concentration/dosage of tacrolimus and individualized administration of tacrolimus after kidney transplantation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(11): 1740-1744. |
| [11] | Guo Juan, Zheng Shan, Xie Hui, Hu Yahui. An analysis of pathogenic bacteria infection in 422 kidney transplant recipients [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(32): 5198-5202. |
| [12] | Liu Luhao, Fang Jiali, Zhang Lei, Li Guanghui, Xu Lu, Lai Xingqiang, Xiong Yunyi, Chen Rongxin, Ma Junjie, Chen Zheng. Clinical assessment criteria of donor pancreas transplants for simultaneous pancreas-kidney transplantation [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(26): 4157-4161. |
| [13] | Yang Jin, Zhang Meixia, Yan Pei, Cheng Qiao, Li Jianzhen . Meta-analysis of risk factors for new-onset diabetes mellitus after kidney transplantation [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(15): 2450-2460. |
| [14] | Yang Qi-shun1, Jiang Wei1, Huang Chi-bing2. Staging diagnosis and treatment for pulmonary infection after renal transplantation can improve the stability of transplanted renal functions [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(8): 1255-1260. |
| [15] | Shang Wen-jun, Wang Zhi-gang, Suo Jing-jun, Li Jin-feng, Pang Xin-lu, Feng Yong-hua, Liu Lei, Xie Hong-chang,Feng Gui-wen. Caspofungin for preventing fungal infection after kidney transplantation using donation after cardiac death donors: a prospective controlled trial [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(32): 5189-5196. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||