Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (34): 5500-5507.doi: 10.12307/2024.839
Previous Articles Next Articles
Bibliometric analysis of vertigo-related histopathology, vestibular rehabilitation, physical rehabilitation, and Chinese and Western medical treatments
Sun Yiming, Yang Xinming, Cai Liqun, Liu Aining
- Liqun Hospital of Shanghai Putuo District, Shanghai 200333, China
-
Received:2024-01-18Accepted:2024-01-25Online:2024-12-08Published:2024-03-14 -
Contact:Cai Liqun, Chief physician, Liqun Hospital of Shanghai Putuo District, Shanghai 200333, China Liu Aining, Chief physician, Liqun Hospital of Shanghai Putuo District, Shanghai 200333, China -
About author:Sun Yiming, Attending physician, Liqun Hospital of Shanghai Putuo District, Shanghai 200333, China Yang Xinming, Attending physician, Liqun Hospital of Shanghai Putuo District, Shanghai 200333, China -
Supported by:Shanghai Putuo District Clinical Special Specialty Disease Capacity Enhancement Project in 2021, No. 2021tszb01; Health Management Research Fund Project of Shanghai Society of Rehabilitation Medicine in 2023, No. 22023JGKT22
CLC Number:
Cite this article
Sun Yiming, Yang Xinming, Cai Liqun, Liu Aining. Bibliometric analysis of vertigo-related histopathology, vestibular rehabilitation, physical rehabilitation, and Chinese and Western medical treatments[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(34): 5500-5507.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
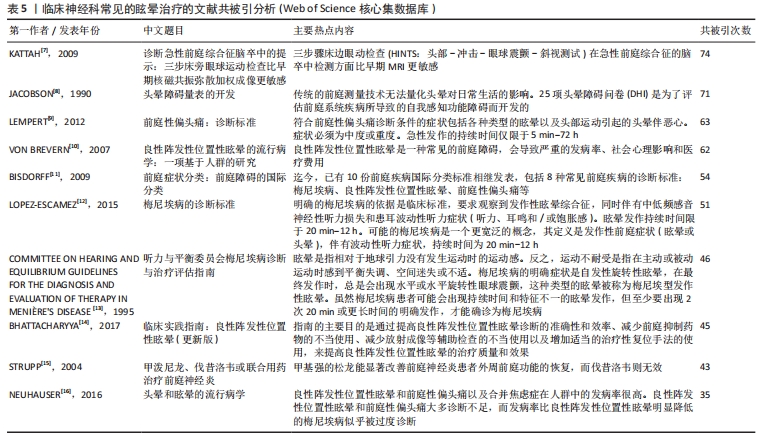
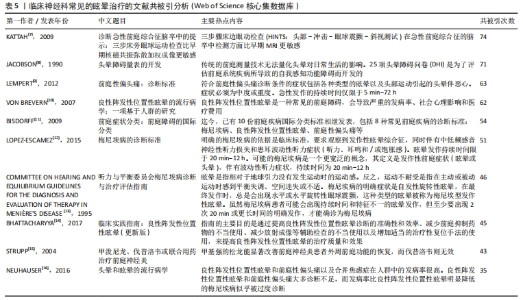
共被引次数最高的文献为KATTAH等[7]的一项横断面研究(被引74次),这项研究主要探讨了床边眼动检查在急性前庭综合征(AVS,以持续性眩晕为主要症状)中识别脑卒中的可行性,研究者对101例急性前庭综合征患者进行前瞻性横断面研究,发现正常水平头部冲击试验、方向变化性眼球震颤或斜视倾斜(垂直眼球错位)对脑卒中具有高度敏感性和特异性;斜视倾斜与脑干损伤相关,能正确预测侧脑桥缺血性脑卒中;在首次MRI扩散加权成像中,有12%的病例出现假阴性。研究结果表明,三步骤床边眼动检查(HINTS:头部-冲击-眼球震颤-斜视测试)在急性前庭综合征脑卒中检测方面比早期MRI更敏感。 其他的大部分为一些与眩晕有关的指南和标准,如头晕障碍量表(被引71次)[8]、前庭性偏头痛:诊断标准(被引63次)[9]、前庭症状分类:前庭障碍的国际分类(被引54次)[11]、梅尼埃病的诊断标准(被引51次)[12]、听力与平衡委员会梅尼埃病诊断与治疗评估指南(被引46次)[13]、临床实践指南:良性阵发性位置性眩晕(更新版)(被引45次)[14]。 此外,值得住的是,有一项关于前庭神经炎患者的临床试验(被引43次)结果表明,甲基强的松龙在治疗前庭神经炎方面具有显著效果,能显著改善患者外周前庭功能的恢复;而伐昔洛韦在该试验中未能显示出明显的治疗效果[15]。因此,对于前庭神经炎患者,使用甲基强的松龙可能是一个有效的治疗选择。 关于良性阵发性位置性眩晕,有2项流行病学研究表明,良性阵发性位置性眩晕是一种常见的前庭障碍,会导致严重的社会心理影响(被引62次)[10],其中良性阵发性位置性眩晕和前庭性偏头痛以及合并焦虑症在人群中的发病率很高(被引35次)[16]。 2.6 高被引文献分析 2.6.1 中文高被引文献分析 文章总结了万方数据库2014-2023年眩晕治疗方面的高被引文献TOP10[17-26],见表6。"
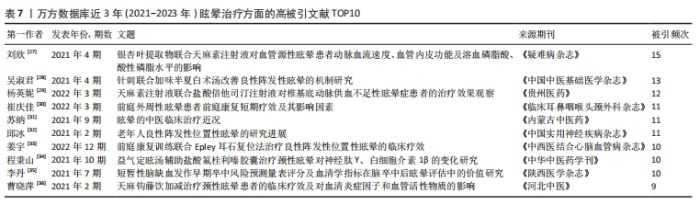
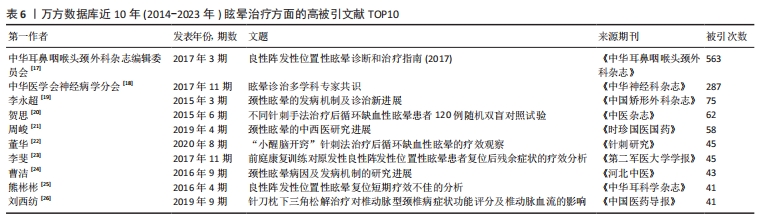

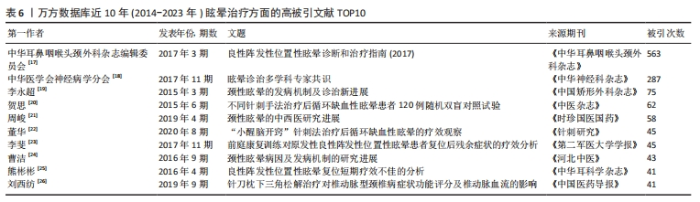
被引次数最高的文献为“良性阵发性位置性眩晕诊断和治疗指南(2017)”(被引563次)[17],其他相关指南还有“眩晕诊治多学科专家共识”(被引287次)[18],这2个眩晕相关指南为中国最权威指南,详细列举了眩晕的诊断和治疗规范标准。 最有影响力的一项临床研究主要介绍了针刺手法对后循环缺血性眩晕的疗效(被引62次) [20],该研究将120例后循环缺血性眩晕患者随机分为4组,分别采用不同的针刺手法进行治疗。结果显示,各组患者临床疗效差异无统计学意义,但不同针刺手法对眩晕症状的改善程度存在差异;其中,针刺风池3组的效果最好,可能与调节去甲肾上腺素(NE)水平有关;此外,研究还发现,不同组别的患者治疗后血浆中5-羟色胺(5-HT)、γ-氨基丁酸(GABA)、谷氨酸(Glu)水平也存在差异,这些变化可能与针刺治疗的效果有关。总之,这项研究为针刺治疗后循环缺血性眩晕提供了新的理论依据和实践指导。 此外,还有一项为期3个月随访的临床研究报道显示,“小醒脑开窍”针刺法可明显改善后循环缺血性眩晕的临床症状,其机制可能与改善椎动脉及基底动脉的血流速度,提高脑组织血液供应有关,且其治疗效果长期持续,复发率低(被引45次) [22]。还有一项临床研究研究强调了,前庭康复训练可有效缓解良性阵发性位置性眩晕复位后的残疾情况(被引45次) [23]。 进一步分析近3年的最新中国研究热点文献发现,关于眩晕的治疗方面,取得一些可喜的临床研究成果[27-36],见表7。例如,银杏叶提取物联合天麻素注射液对血管源性眩晕患者的血管功能具有改善作用(被引15次) [27],针刺联合加味半夏白术汤可能通过调节良性阵发性眩晕患者的单胺类神经递质水平改善其头晕症状(被引13次) [28],倍他司汀联合天麻素对椎基底动脉供血不足性眩晕症患者具有一定治疗效果(被引12次) [29],通过前庭康复训练联合Epley耳石复位法可有效提高良性阵发性位置性眩晕的临床疗效(被引11次) [30]。因此,近年来,中国特色药物如银杏叶提取物、天麻素、半夏白术汤治疗眩晕有一定效果,但都需要与西药(如倍他司汀)或针刺联合使用,前庭康复训练联合中医手法复位对良性阵发性位置性眩晕有一定治疗效果。"


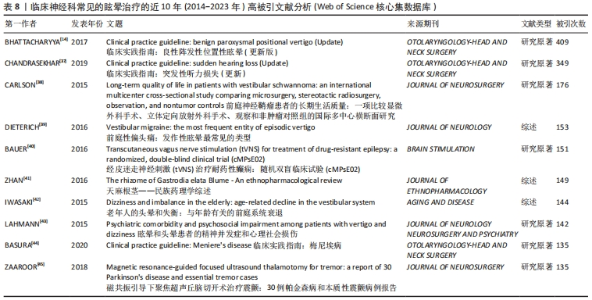
CARLSON等[38](被引176次)讨论了治疗散发性前庭神经鞘瘤的最佳方法。研究通过一系列问卷调查了接受不同治疗方法的患者的健康相关生命质量(HRQOL),并与一般人群进行了比较,对于小到中等大小的前庭神经鞘瘤应最初采取观察方法,而将干预方法留给确实出现肿瘤增长或不能通过治疗缓解症状的患者。未来评估前庭神经鞘瘤患者HRQOL的研究应优先使用经过验证的特定于疾病的测量工具,例如佩恩听神经瘤生活质量量表(PANQOL),因为一般工具在区分治疗组和肿瘤与非肿瘤对象方面存在显著限制。 LAHMANN等[43](被引142次)的一项临床研究评估患有有机性和非有机性(即不可解释的)眩晕/头晕综合征的大样本患者的精神障碍共病和心理社会功能受损,参与者包括来自一个专门的眩晕/头晕综合征多学科治疗中心的547例患者。神经学诊断发现80.8%的患者出现有机性眩晕/头晕,19.2%的患者有非有机性眩晕/头晕;在48.8%的患者中,结构化临床访谈确认了目前存在的精神障碍,最常见的是焦虑/恐怖症、心因性障碍和情感障碍;在有机性眩晕/头晕组中,42.5%的患者,特别是患有前庭突发症或前庭偏头痛的患者存在目前精神障碍;与未患精神障碍的患者相比,患有精神障碍的患者报告了更多的眩晕相关障碍、更多的抑郁、焦虑和躯体化症状,以及更低的心理生活质量;眩晕/头晕和精神共病的非有机性组合是最严重的,这应在疾病早期的诊断和治疗中予以考虑。 文章进一步分析了近3年该领域的研究热点,见表9。在2021年,有研究报道了首例因前庭神经炎而出现双面无力和麻痹的孕妇病例(被引26次)[46],这是 COVID-19感染后的表现,患者出现双侧面瘫、双下肢麻痹、眩晕、恶心、呕吐和右耳痛到急诊科就诊,说明COVID-19感染后患者可能出现前庭神经炎导致的面瘫。在2021年,有研究描述了一例感染 COVID-19 并仅有眩晕和发热症状的儿童病例[50]。该研究认为该患儿患的是 COVID-19 引起的前庭神经炎,考虑到症状的自发改善,除了中枢神经系统的自然代偿外,不需要任何治疗调整。该病例表明,对于出现眩晕的儿科患者,怀疑 COVID-19 感染非常重要。在2021年,有研究从一家土耳其三甲医院眩晕中心3年内接受前庭评估的3 400例患者中收集了203例儿童患者的数据进行回顾性分析(被引13次)[51],结果发现,良性阵发性位置性眩晕和前庭性偏头痛是最常见的小儿前庭疾病,其次是儿童良性阵发性眩晕、前庭神经炎和精神性眩晕,而梅尼埃病和中枢性眩晕在儿童中较少诊断。在2022年,巴拉尼学会前庭疾病分类委员会发布了急性单侧前庭病/前庭神经炎的诊断标准(被引22次)[47]。"

| [1] 中国医药教育协会眩晕专业委员会,中国医师协会急诊医师分会.眩晕急诊诊断与治疗指南(2021年)[J].中华急诊医学杂志,2021,30(4):402-406. [2] SAHA K. Vertigo related to central nervous system disorders. Continuum (Minneap Minn). 2021;27(2):447-467. [3] RASCOL O, HAIN TC, BREFEL C, et al. Antivertigo medications and drug-induced vertigo. A pharmacological review. Drugs. 1995;50(5):777-791. [4] VAN ECK NJ, WALTMAN L. Software survey: VOSviewer, a computer program for bibliometric mapping. Scientometrics. 2010;84(2):523-538. [5] DONTHU N, KUMAR S, MUKHERJEE D, et al. How to conduct a bibliometric analysis: an overview and guidelines. J Bus Res. 2021;133:285-296. [6] RANJBARI M, SHAMS ESFANDABADI Z, GAUTAM S, et al. Waste management beyond the COVID-19 pandemic: Bibliometric and text mining analyses. Gondwana Res. 2023;114:124-137. [7] KATTAH JC, TALKAD AV, WANG DZ, et al. HINTS to diagnose stroke in the acute vestibular syndrome: three-step bedside oculomotor examination more sensitive than early MRI diffusion-weighted imaging. Stroke. 2009; 40(11):3504-3510. [8] JACOBSON GP, NEWMAN CW. The development of the dizziness handicap inventory. Arch Otolaryngol Head Neck Surg. 1990;116(4):424-427. [9] LEMPERT T, OLESEN J, FURMAN J, et al. Vestibular migraine: diagnostic criteria. J Vestib Res. 2012;22(4):167-72. [10] VON BREVERN M, RADTKE A, LEZIUS F, et al. Epidemiology of benign paroxysmal positional vertigo: a population based study. J Neurol Neurosurg Psychiatry. 2007;78(7):710-715. [11] BISDORFF A, VON BREVERN M, LEMPERT T, et al. Classification of vestibular symptoms: towards an international classification of vestibular disorders. J Vestib Res. 2009;19(1-2):1-13. [12] LOPEZ-ESCAMEZ JA, CAREY J, CHUNG WH, et al. Diagnostic criteria for Menière’s disease. J Vestib Res. 2015;25(1):1-7. [13] COMMITTEE ON HEARING AND EQUILIBRIUM GUIDELINES FOR THE DIAGNOSIS AND EVALUATION OF THERAPY IN MENIÈRE’S DISEASE. American academy of otolaryngology-head and neck foundation, Inc. Otolaryngol Head Neck Surg. 1995;113(3):181-185. [14] BHATTACHARYYA N, GUBBELS SP, SCHWARTZ SR, et al. Clinical practice guideline: benign paroxysmal positional vertigo (Update). Otolaryngol Head Neck Surg. 2017;156(3_suppl):S1-S47. [15] STRUPP M, ZINGLER VC, ARBUSOW V, et al. Methylprednisolone, valacyclovir, or the combination for vestibular neuritis. N Engl J Med. 2004; 351(4):354-361. [16] NEUHAUSER HK. The epidemiology of dizziness and vertigo. Handb Clin Neurol. 2016;137:67-82. [17] 中华耳鼻咽喉头颈外科杂志编辑委员会,中华医学会耳鼻咽喉头颈外科学分会.良性阵发性位置性眩晕诊断和治疗指南(2017)[J].中华耳鼻咽喉头颈外科杂志,2017,52(3):173-177. [18] 中华医学会神经病学分会,中华神经科杂志编辑委员会.眩晕诊治多学科专家共识[J].中华神经科杂志,2017,50(11):805-812. [19] 李永超,彭宝淦.颈性眩晕的发病机制及诊治新进展[J].中国矫形外科杂志,2015,23(3):250-253. [20] 贺思,赵晓峰,文妍,等.不同针刺手法治疗后循环缺血性眩晕患者120例随机双盲对照试验[J].中医杂志,2015,56(6):478-482. [21] 周峻,熊振成,李文浩,等.颈性眩晕的中西医研究进展[J].时珍国医国药,2019,30(4):951-954. [22] 董华,张建明,胡伟,等.“小醒脑开窍”针刺法治疗后循环缺血性眩晕的疗效观察[J].针刺研究,2020,45(8):652-656. [23] 李斐,陈瑛,高博,等.前庭康复训练对原发性良性阵发性位置性眩晕患者复位后残余症状的疗效分析[J].第二军医大学学报,2017,38(11): 1370-1373. [24] 曹洁,齐瑞,王辉昊.颈性眩晕病因及发病机制的研究进展[J].河北中医, 2016,38(9):1416-1421, 1435. [25] 熊彬彬,赵晓明,刘劲,等.良性阵发性位置性眩晕复位短期疗效不佳的分析[J].中华耳科学杂志,2016,14(4):473-477. [26] 刘西纺,杨民毅,惠国栋,等.针刀枕下三角松解治疗对椎动脉型颈椎病症状功能评分及椎动脉血流的影响[J].中国医药导报,2019,16(9):166-169. [27] 刘欣,王晓芳,吴延佳,等.银杏叶提取物联合天麻素注射液对血管源性眩晕患者动脉血流速度、血管内皮功能及溶血磷脂酸、酸性磷脂水平的影响[J].疑难病杂志,2021,20(4):363-367. [28] 吴淑君,王宝爱,符文雄.针刺联合加味半夏白术汤改善良性阵发性眩晕的机制研究[J].中国中医基础医学杂志,2021,27(4):634-637. [29] 杨英妮,李秉纲,冯云婷.天麻素注射液联合盐酸倍他司汀注射液对椎基底动脉供血不足性眩晕症患者的治疗效果观察[J].贵州医药,2022, 46(3):389-391. [30] 崔庆佳,王蕊,闫瑾,等.前庭外周性眩晕患者前庭康复短期疗效及其影响因素[J].临床耳鼻咽喉头颈外科杂志,2022,36(3):217-221. [31] 苏纳,徐永和.眩晕的中医临床治疗近况[J].内蒙古中医药,2021,40(9): 148-151. [32] 邱冰,尹晓新.老年人良性阵发性位置性眩晕的研究进展[J].中国实用神经疾病杂志,2021,24(2):166-171. [33] 姜宇,李晶,袁颖,等.前庭康复训练联合Epley耳石复位法治疗良性阵发性位置性眩晕的临床疗效[J].中西医结合心脑血管病杂志,2022, 20(12):2290-2292. [34] 程秉山,何声萍,王妙,等.益气定眩汤辅助盐酸氟桂利嗪胶囊治疗颈性眩晕对NPY、IL-1β的变化研究[J].中华中医药学刊,2021,39(10): 101-103. [35] 李丹,杨吉睿.短暂性脑缺血发作早期卒中风险预测量表评分及血清学指标在脑卒中后眩晕评估中的价值研究[J].陕西医学杂志,2021, 50(7):864-866. [36] 曹晓萍,移军,肖章红.天麻钩藤饮加减治疗颈性眩晕患者的临床疗效及对血清炎症因子和血管活性物质的影响[J].河北中医,2021,43(2): 261-264. [37] CHANDRASEKHAR SS, TSAI DO BS, SCHWARTZ SR, et al. Clinical practice guideline: sudden hearing loss (Update). Otolaryngol Head Neck Surg. 2019;161(1_suppl): S1-S45. [38] CARLSON ML, TVEITEN OV, DRISCOLL CL, et al. Long-term quality of life in patients with vestibular schwannoma: an international multicenter cross-sectional study comparing microsurgery, stereotactic radiosurgery, observation, and nontumor controls. J Neurosurg. 2015;122(4):833-842. [39] DIETERICH M, OBERMANN M, CELEBISOY N. Vestibular migraine: the most frequent entity of episodic vertigo. J Neurol. 2016;263 Suppl 1:S82-S89. [40] BAUER S, BAIER H, BAUMGARTNER C, et al. Transcutaneous vagus nerve stimulation (tVNS) for treatment of drug-resistant epilepsy: a randomized, double-blind clinical trial (cMPsE02). Brain Stimul. 2016;9(3):356-363. [41] ZHAN HD, ZHOU HY, SUI YP, et al. The rhizome of Gastrodia elata Blume - An ethnopharmacological review. J Ethnopharmacol. 2016;189:361-385. [42] IWASAKI S, YAMASOBA T. Dizziness and imbalance in the elderly: age-related decline in the vestibular system. Aging Dis. 2014;6(1):38-47. [43] LAHMANN C, HENNINGSEN P, BRANDT T, et al. Psychiatric comorbidity and psychosocial impairment among patients with vertigo and dizziness. J Neurol Neurosurg Psychiatry. 2015;86(3):302-308. [44] BASURA GJ, ADAMS ME, MONFARED A, et al. Clinical practice guideline: ménière’s disease. Otolaryngol Head Neck Surg. 2020;162(2_suppl):S1-S55. [45] ZAAROOR M, SINAI A, GOLDSHER D, et al. Magnetic resonance-guided focused ultrasound thalamotomy for tremor: a report of 30 Parkinson’s disease and essential tremor cases. J Neurosurg. 2018;128(1):202-210. [46] AASFARA J, HAJJIJ A, BENSOUDA H, et al. A unique association of bifacial weakness, paresthesia and vestibulocochlear neuritis as post-COVID-19 manifestation in pregnant women: a case report. Pan Afr Med J. 2021;38:30. [47] STRUPP M, BISDORFF A, FURMAN J, et al. Acute unilateral vestibulopathy/vestibular neuritis: diagnostic criteria. J Vestib Res. 2022;32(5):389-406. [48] LEMOS J, STRUPP M. Central positional nystagmus: an update. J Neurol. 2022; 269(4):1851-1860. [49] MALLAMPALLI MP, RIZK HG, KHERADMAND A, et al. Care gaps and recommendations in vestibular migraine: an expert panel summit. Front Neurol. 2022;12:812678. [50] GIANNANTONIO S, SCORPECCI A, MONTEMURRI B, et al. Case of COVID-19-induced vestibular neuritis in a child. BMJ Case Rep. 2021;14(6):e242978. [51] GEDIK-SOYUYUCE O, GENCE-GUMUS Z, OZDILEK A, et al. Vestibular disorders in children: a retrospective analysis of vestibular function test findings. Int J Pediatr Otorhinolaryngol. 2021;146:110751. [52] 中华医学会,中华医学会杂志社,中华医学会全科医学分会,等.头晕/眩晕基层诊疗指南(2019年)[J].中华全科医师杂志,2020,19(3):201-216. [53] EDLOW JA, CARPENTER C, AKHTER M, et al. Guidelines for reasonable and appropriate care in the emergency department 3 (GRACE-3): acute dizziness and vertigo in the emergency department. Acad Emerg Med. 2023;30(5):442-486. [54] HAIN TC, UDDIN M. Pharmacological treatment of vertigo. CNS Drugs. 2003; 17(2):85-100. [55] MURDIN L, HUSSAIN K, SCHILDER AG. Betahistine for symptoms of vertigo. Cochrane Database Syst Rev. 2016;2016(6):CD010696. [56] CASANI AP, GUFONI M, CAPOBIANCO S. Current insights into treating vertigo in older adults. Drugs Aging. 2021;38(8):655-670. [57] 《中成药治疗优势病种临床应用指南》标准化项目组.中成药治疗眩晕相关疾病临床应用指南(2022年)[J].中国中西医结合杂志,2023, 43(10):1157-1166. |
| [1] | Wu Jing, Yao Yingce, Yang Xiaowei, Xue Boshi, Zhao Jianbin, Yang Chen, Luan Tianfeng, Zhou Zhipeng. Intervention of muscle strength training combined with neuromuscular electrical stimulation on lower limb function and biomechanical changes in patients with patellofemoral pain [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1365-1371. |
| [2] | Qi Haodong, Lu Chao, Xu Hanbo, Wang Mengfei, Hao Yangquan. Effect of diabetes mellitus on perioperative blood loss and pain after primary total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1383-1387. |
| [3] | Zhang Xihui, Li Zhengrong, Li Shineng, Xing Zengyu, Wang Jiao. Effect of rehabilitation training guided by Pro-kin balance system on proprioception and balance function of the affected knee after anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1259-1264. |
| [4] | Huang Xiarong, Hu Lizhi, Sun Guanghua, Peng Xinke, Liao Ying, Liao Yuan, Liu Jing, Yin Linwei, Zhong Peirui, Peng Ting, Zhou Jun, Qu Mengjian. Effect of electroacupuncture on the expression of P53 and P21 in articular cartilage and subchondral bone of aged rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1174-1179. |
| [5] | Liu Hanfeng, Wang Jingjing, Yu Yunsheng. Artificial exosomes in treatment of myocardial infarction: current status and prospects [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1118-1123. |
| [6] | Feng Ruiqin, Han Na, Zhang Meng, Gu Xinyi, Zhang Fengshi. Combination of 1% platelet-rich plasma and bone marrow mesenchymal stem cells improves the recovery of peripheral nerve injury [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 985-992. |
| [7] | Li Longyang, Zhang Songjiang, Zhao Xianmin, Zhou Chunguang, Gao Jianfeng. Electroacupuncture intervention on the proliferation and differentiation of hippocampal neurons and oligodendrocytes in Alzheimer’s disease model mice [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1029-1035. |
| [8] | Yin Tong, Yang Jilei, Li Yourui, Liu Zhuoran, Jiang Ming. Application of core-shell structured nanofibers in oral tissue regeneration [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 766-770. |
| [9] | Tian Xin, Liu Tao, Yang Huilin, He Fan. In vitro evaluation of sustained release Kartogenin by gelatin methacryloyl microspheres for repairing nucleus pulposus degeneration [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 724-730. |
| [10] | Zhang Ming, Wang Bin, Jia Fan, Chen Jie, Tang Wei. Application of brain-computer interface technology based on electroencephalogram in upper limb motor function rehabilitation of stroke patients [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 581-586. |
| [11] | Zhu Xi, Tao Yuhong, Huang Peng, Li Dan. A randomized controlled trial of acupuncture at Jiaji points for treatment of lumbar disc herniation under ultrasonic guidance [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(36): 5852-5857. |
| [12] | Wang Yueguang, Mu Xiaohong, Jiang Shengyuan, Deng Bowen, Kang Ximei, Su Jianguang. Correlation between early serum markers and AISA grading in patients with acute spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(34): 5494-5499. |
| [13] | Xu Yi, Deng Yubin. Exoskeleton-assisted walking rehabilitation for spinal cord injury: CiteSpace analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(33): 5403-5412. |
| [14] | Su Yuying, Li Wei, Shi Yu, Pan Changbo. Effects of different exercise interventions on symptoms and dynamic balance ability of chronic ankle instability: a systematic review and Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(32): 5217-5224. |
| [15] | Zhang Yunxin, Zhang Cunxin, Wang Qian, Xu Xinliang, Lyu Chaoliang, Ni Yong. Syringin inhibits intervertebral disc degeneration in rats [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(32): 5104-5109. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||