Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (33): 5403-5412.doi: 10.12307/2024.674
Exoskeleton-assisted walking rehabilitation for spinal cord injury: CiteSpace analysis of research hotspots
Xu Yi, Deng Yubin
- Seventh Affiliated Hospital of Sun Yat-sen University, Sun Yat-sen University (Shenzhen), Shenzhen 518107, Guangdong Province, China
-
Received:2023-09-18Accepted:2023-11-07Online:2024-11-28Published:2024-01-31 -
Contact:Deng Yubin, PhD, Professor, Seventh Affiliated Hospital of Sun Yat-sen University, Sun Yat-sen University (Shenzhen), Shenzhen 518107, Guangdong Province, China -
About author:Xu Yi, MD, PhD, Associate chief physician, Seventh Affiliated Hospital of Sun Yat-sen University, Sun Yat-sen University (Shenzhen), Shenzhen 518107, Guangdong Province, China -
Supported by:National Natural Science Foundation of China (General Program), No. 82172548 (to XY); Basic Research Free Exploration Project of Shenzhen Science and Technology Innovation Commission, No. JCYJ20180307150610733 (to XY)
CLC Number:
Cite this article
Xu Yi, Deng Yubin. Exoskeleton-assisted walking rehabilitation for spinal cord injury: CiteSpace analysis of research hotspots[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(33): 5403-5412.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
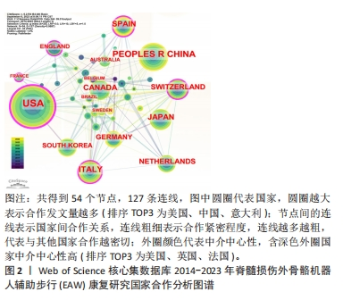
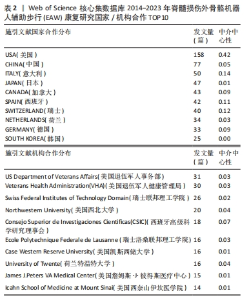
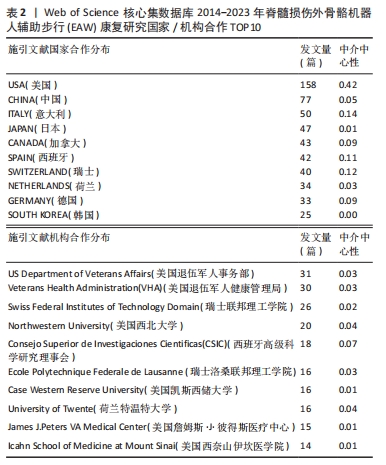
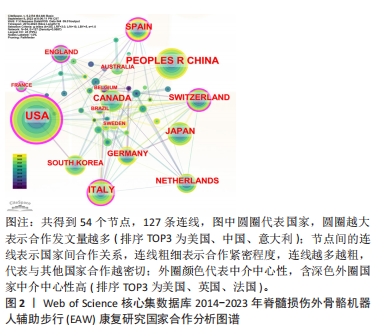
2.1.2 施引文献国家(地区)合作分析 如图2,表2所示,外骨骼机器人应用于脊髓损伤后患者步行功能研究可以看出,2014-2023 年,共有54个国家(地区)发表了该领域相关研究,合作图谱共得到54个节点,127条连线,各国间有良好合作关系。发文数量排名前5国家依次是:美国USA 158篇,中国PEOPLES R CHINA 77篇,意大利ITALY 50篇,日本JAPAN 47篇,加拿大 CANADA 43篇。中介中心性前5国家依次为:美国USA(0.42),英国ENGLAND(0.18),法国FRANCE(0.16),意大利 ITALY (0.14),瑞士SWITZERLAND(0.12)。美国的发文量及中介中心性均最高居于榜首,在此领域处于领军地位。可能由于欧美国家科学技术水平较高、起步较早、认可度高,故中介中心性也较高。中国近几年度发文量提升明显,但可能由于起步相对较晚,中介中心性仍偏低(0.05)。具体见图2。"

2.1.3 施引文献机构合作分析 如图3,表2所示,在过去近10年共有约240个机构涉及该领域研究,集中于各国大学,具有密切合作关系。发表文章数量排名前5位的机构依次为美国退伍军人事务部US Department of Veterans Affairs 31篇,美国退伍军人健康管理局Veterans Health Administration (VHA) 30篇,瑞士联邦理工学院 Swiss Federal Institutes of Technology Domain 26篇,美国西北大学 Northwestern University 20篇,西班牙国家最高科学研究委员会 Consejo Superior de Investigaciones Cientificas (CSIC)18篇 ;就中介中心性而言,排名前5位的机构依次是美国芝加哥Shirley Ryan康复中心(原芝加哥康复研究所)Shirley Ryan Ability Lab 0.08,西班牙国家最高科学研究委员会 Consejo Superior de Investigaciones Cientificas (CSIC) 0.07,意大利圣卢西亚基金会 IRCCS Santa Lucia 0.07,美国佐治亚理工学院Georgia Institute of Technology 0.05,美国西北大学 Northwestern University 0.04。与主要研究国家一致,该领域主要研究机构也以欧美国家为主,这些信息可为从事该领域研究专家后续进一步研究、深造、合作提供信息。"

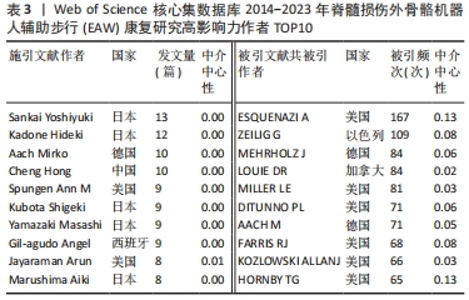
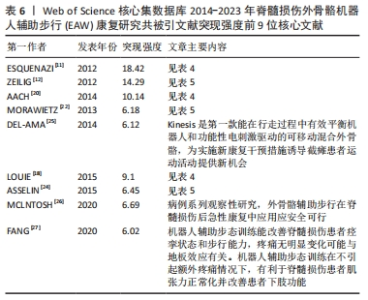
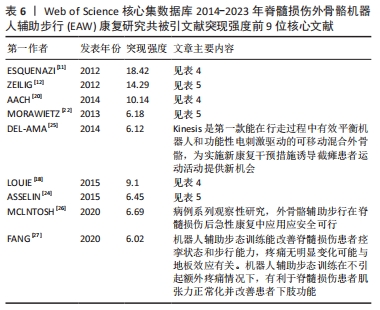
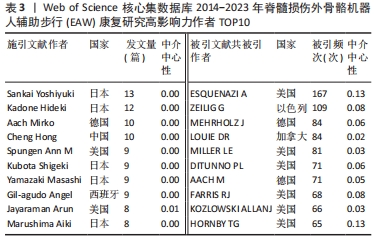
2.1.4 高影响力施引文献作者合作与被引文献作者共被引分析 如表3所示,近 10年来多名施引文献作者参与该领域研究,其中4位作者发文量在10篇以上,分别是日本筑波大学Sankai Yoshiyuki教授(13篇)、Kadone Hideki教授(12篇),德国波鸿伯格曼谢尔大学Aach Mirko教授(10篇),中国四川电子科技大学Hong Cheng教授(10篇),但综合而言,作者中介中心性较低,被引用率不高;如表3所示,近 10年被引文献被引频次排序前 5 核心共被引作者依次为美国宾夕法尼亚MossRehab & Albert Einstein医疗中心ESQUENAZI A (167 次)、以色列Chaim Sheba医疗中心ZEILIG G(109次)、德国德累斯顿医学院MEHRHOLZ J (84 次)、加拿大哥伦比亚大学LOUIE DR (84次)、美国北卡罗来纳州Miller科学咨询机构MILLER LE (81次)。被引文献中介中心性排序前 5的核心共被引作者依次为美国宾夕法尼亚MossRehab & Albert Einstein医疗中心ESQUENAZI A(0.13),美国印第安纳大学HORNBY TG (0.13),瑞士苏黎世Hocoma医学GmbH的VENEMAN JF (0.12),美国科罗拉多州恩格尔伍德克雷格医院TEFERTILLER C (0.12),瑞士苏黎世联邦理工学院RIENER R (0.11)。其中被引文献共被引频次最多、中介中心性最高作者均为来自美国Pennsylvania大学MossRehab & Albert Einstein Medical Center的Alberto Esquenazi教授,他在脊髓损伤后EAW研究领域涉及的研究主题包括评估脊髓损伤患者使用 ReWalk? 外骨骼行走系统的安全性和耐受性,评估功能性步行测量,并将其与神经脊髓水平、年龄和受伤后持续时间等相关联;并长期致力于外骨骼机器人、肉毒毒素等手段应用于各类步行功能障碍患者的相关研究[11-16]。"
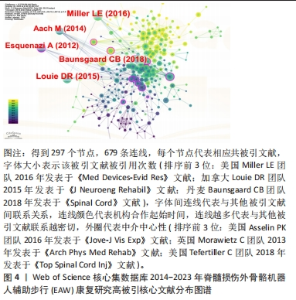
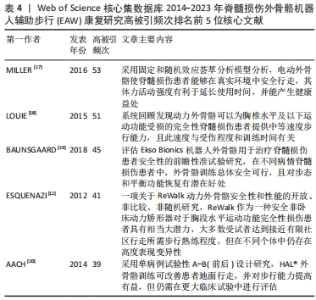
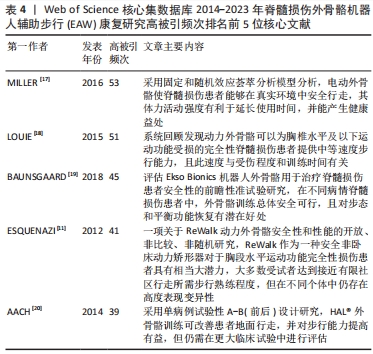
2.2 研究热点分析结果 2.2.1 被引核心文献共被引分析结果 文献共被引指1篇文献被≥2篇文献同时引用,可预测研究领域在一定时间范围内研究热点及趋势。图4可见2014-2023年间该领域的研究共涉及297篇共被引核心参考文献。共被引参考文献排名前5位的文献依次是:美国Virginia Tech大学MILLER团队[17]2016年在《Med Devices-Evid Res》发表文献,共被引次数(53次)最高,加拿大温哥华大学LOUIE团队[18]于2015年发表于《J Neuroeng Rehabil》的文献,共被引51次;丹麦Rigshospitalet脊髓损伤诊所BAUNSGAARD团队[19]2018年发表于《Spinal Cord》的文献,共被引45次;美国宾夕法尼亚MossRehab & Albert Einstein医疗中心ESQUENAZI团队[11]2012年发表于《Am J Phys Med Rehab》的文献,共被引41次;德国BG大学AACH 团队[20]2014年发表于《Spine J》的文献,共被引39次,频次前5位文献主要研究内容:脊髓损伤患者配备电动外骨骼设备真实环境中行走的安全性及优势;以及设备应用于胸椎及以下水平运动功能完全损伤的脊髓损伤患者辅助步行效果、影响因素及应用潜力等,具体见表4。"
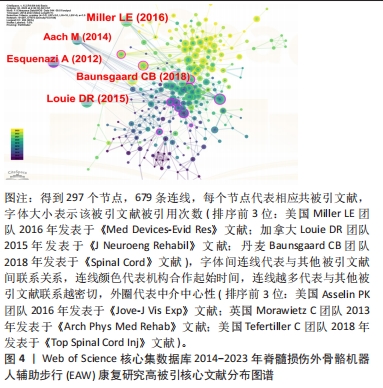
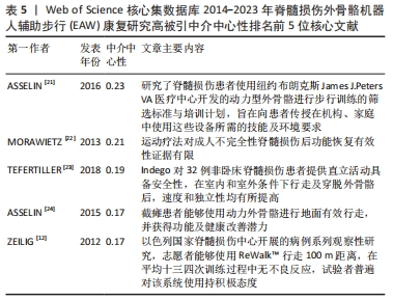
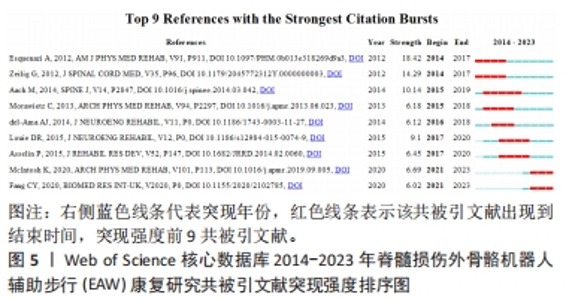
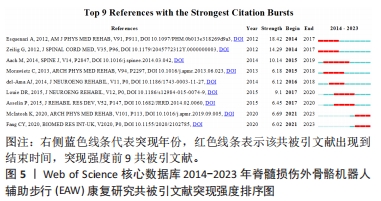
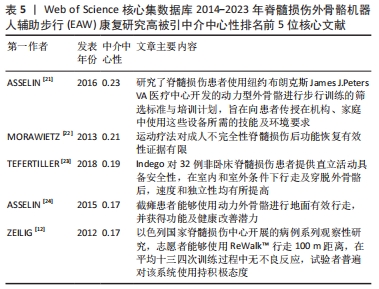
最佳中介中心性(0.23)以美国退伍军人事务部Asselin PK团队在《JOVE-J VIS EXP》发表文献“Training Persons with Spinal Cord Injury to Ambulate Using a Powered Exoskeleton”获得,他们重点研究了脊髓损伤患者使用动力型外骨骼筛选标准与培训计划[21];其他高中介中心性被引参考文献尚包括英国格拉斯哥喀里多尼亚大学 MORAWIETZ团队[22]2013年发表于《ARCH PHYS MED》文献,中介中心性0.21;美国科罗拉多州恩格尔伍德克雷格医院TEFERTILLER团队 [23]2018年发表于《 TOP SPINAL CORD INJ》文献,中介中心性0.19;美国退伍军人事务部ASSELIN团队[24]2015年发表于《J REHABIL RES DEV》文献,中介中心性 0.17;以色列Chaim Sheba医疗中心ZEILIG团队[12]2012年发表于《J SPINAL CORD MED》文献,中介中心性 0.17 ,具体见表5。"
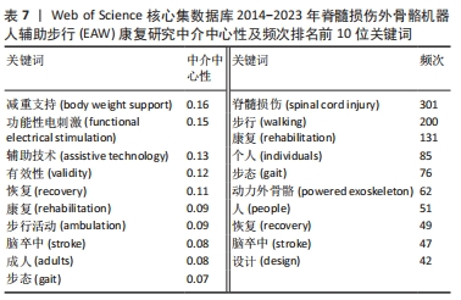
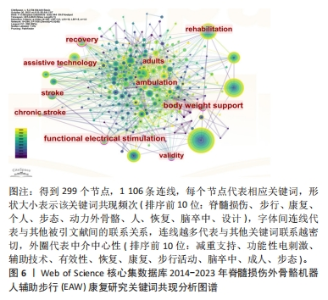
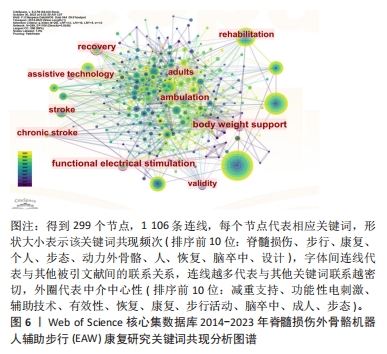
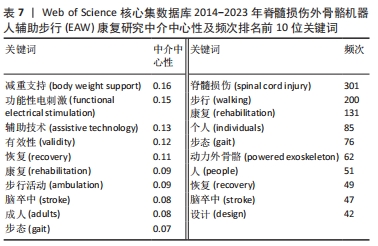
2.2.3 关键词共现分析结果 文献主要内容一般可被凝炼成关键词,故关键词共同出现次数越多则代表该领域在一定时间范围内研究主题热度越高,主要以中介中心性为衡量量化指标(0-1),数值越大影响力越大,若其≥0.1 说明中介中心性较高,如表7,图6,中介中心性排名前10的关键词依次是:body weight support (减重支持),Functional electrical stimulation (功能性电刺激),assistive technology(辅助技术),validity (有效性), recovery(恢复),rehabilitation(康复),ambulation(步行活动),stroke(脑卒中),adults(成人),gait(步态)。除去与主题相关的关键词——Spinal cord injury(脊髓损伤),walking(步行),rehabilitation(康复),共现出现频次前10的关键词尚包括Individuals (个人),gait(步态),Powered exoskeleton(动力外骨骼),people(人),recovery(恢复),stroke(脑卒中),design(设计)。"
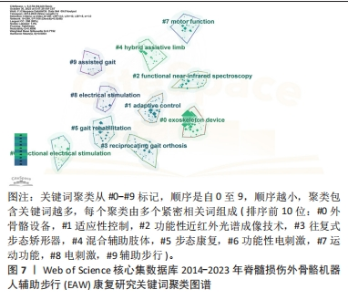
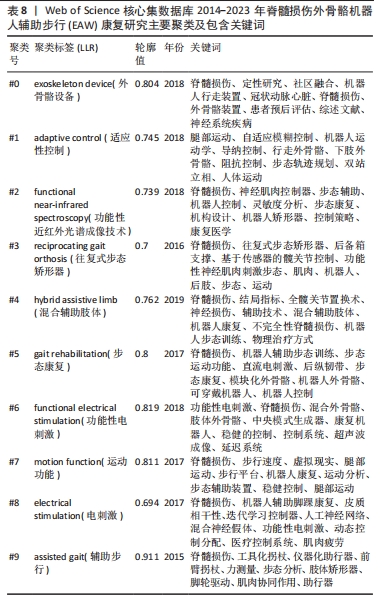
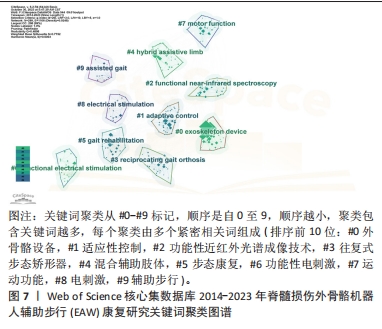
2.2.4 关键词共现聚类分析结果 关键词聚类分析是将关联密切关键词汇聚成一类,并观察一定时间范围内研究领域形成的具体研究类团(聚类号),号数越小则类团包含关键词数量越多,轮廓值则表示类团内部关键词间紧密程度,一般认为> 0.7 时聚类较成功。进一步通过对上述关键词进行对数似然比(log-likelihood ratio,LLR)聚类分析,得到聚类图7。其中,聚类模块化Q 值Modularity为0.489 8(> 0.3,表示聚类结构显著),平均轮廓S 值Silhouette 值为0.775 2(一般认为S值> 0.5聚类即合理,S值> 0.7意味聚结果令人信服),提示聚类结构显著,同质性高。如图7,排名前10的聚类与相应轮廓值分别为#0 exoskeleton device(外骨骼设备,0.804 ),#1 adaptive control(适应性控制,0.745),#2 functional near-infrared spectroscopy(功能性近红外光谱成像技术 0.739),#3 reciprocating gait orthosis (往复式步态矫形器,0.7),#4 hybrid assistive limb (混合辅助肢体,0.762),#5 gait rehabilitation(步态康复,0.8),#6 functional electrical stimulation(功能性电刺激,0.819),#7 motion function(运动功能 0.811),#8 electrical stimulation(电刺激,0.694),#9 assisted gait(辅助步行,0.911)。将上述信息进一步进行聚类列表处理,自聚类Clusters-聚类列表Summary Table中白名单Whitelist获得关键词具体相关信息,具体见表8。由聚类结果及其所含关键词可知,脊髓损伤患者步态功能康复近年研究主要聚焦于外骨骼设备技术,作用机制以适应性控制为主,既往促进步行功能改善方法还包括往复式步态矫形器、混合辅助肢体、功能性电刺激等康复工程技术,目前研究倾向联合功能性近红外光谱成像等智能高端技术。"

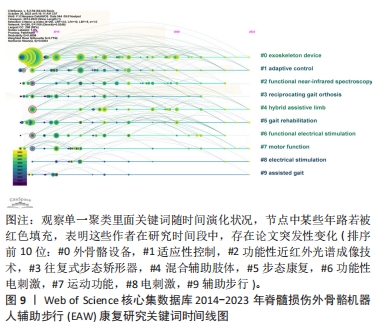
(1) 2014-2018年热点: stroke(脑卒中),2014-2017时间段针对步态异常康复机器人设备更偏重对脑卒中类患者进行尝试与研究;mobility (行走能力)与system(系统)。 (2) 2016-2018年热点:研究强调提升患者步行能力及综合系统对待病患具体问题; functional electrical stimulation (功能性电刺激),2017-2018时间段内研究偏重功能性电刺激使用对脊髓损伤患者功效。 (3)2019-2020 研究热点:逐渐转向 locomotor training(步行训练)作为干预手段改善脊髓损伤患者步行功能。 (4) 2020-2023年热点:突变热点转变为quality of life (生活质量),exercise(运动训练)、body composition(身体结构)、legged locomotion(腿部运动)等,突变系数较高且至今仍保持较高发文量,应是该领域研究热点与前沿方向,其中,尤其以quality of life 突变系数最高,可见围绕脊髓损伤患者步态康复阶段各项评估内容中,患者生活质量的重要性日益受到关注。在功能恢复中,运动训练扮演着至关重要的角色。研究人员也致力于改善机体结构,以促进康复和功能恢复。 进一步对关键词聚类进行时间线图分析,可见#0 exoskeleton device(外骨骼设备)一直是脊髓损伤患者步行功能康复研究热点与重点,尤其近几年呈现热度持续增高趋势,也是后续被持续关注目标方向;#4 hybrid assistive limb (混合辅助肢体)、#7 motion function(运动功能)也是近年研究热点聚类;相反,#3 reciprocating gait orthosis (往复式步态矫形器),#6 FES(功能性电刺激)虽在早年关注度较高,但近年呈下降趋势,具体见图9。"

| [1] YUAN S, SHI Z, CAO F, et al. Epidemiological features of spinal cord injury in china: a systematic review. Front Neurol. 2018;9:683. [2] JAZAYERI SB, MAROUFI SF, MOHAMMADI E, et al. Incidence of traumatic spinal cord injury worldwide: a systematic review, data integration, and update. World Neurosurg X. 2023;18:100171. [3] WEST CR, ALYAHYA A, LAHER I, et al. Peripheral vascular function in spinal cord injury: a systematic review. Spinal Cord. 2013;51(1):10-19. [4] KOYAMA S, TANABE S, SAITOH E, et al. Characterization of unexpected postural changes during robot-assisted gait training in paraplegic patients. Spinal Cord. 2016;54(2):120-125. [5] KHAN AS, LIVINGSTONE DC, HURD CL, et al. Retraining walking over ground in a powered exoskeleton after spinal cord injury: a prospective cohort study to examine functional gains and neuroplasticity. J Neuroeng Rehabil. 2019;16(1):145. [6] NAM KY, KIM HJ, KWON BS, et al. Robot-assisted gait training (Lokomat) improves walking function and activity in people with spinal cord injury: a systematic review. J Neuroeng Rehabil. 2017;14(1):24. [7] XIANG XN, DING MF, ZONG HY, et al. The safety and feasibility of a new rehabilitation robotic exoskeleton for assisting individuals with lower extremity motor complete lesions following spinal cord injury (SCI): an observational study. Spinal Cord. 2020;58(7):787-794. [8] TSAI CY, DELGADO AD, WEINRAUCH WJ, et al. Exoskeletal-assisted walking during acute inpatient rehabilitation leads to motor and functional improvement in persons with spinal cord injury: a pilot study. Arch Phys Med Rehabil. 2020;101(4):607-612. [9] CHEN C. Searching for intellectual turning points: progressive knowledge domain visualization. Proc Natl Acad Sci U S A. 2004;101 Suppl 1(Suppl 1): 5303-5310. [10] CHEN C, SONG M. Visualizing a field of research: a methodology of systematic scientometric reviews. PLoS One. 2019;14(10):e0223994. [11] ESQUENAZI A, TALATY M, PACKEL A, et al. The ReWalk powered exoskeleton to restore ambulatory function to individuals with thoracic-level motor-complete spinal cord injury. Am J Phys Med Rehabil. 2012; 91(11):911-921. [12] ZEILIG G, WEINGARDEN H, ZWECKER M, et al. Safety and tolerance of the ReWalk exoskeleton suit for ambulation by people with complete spinal cord injury: a pilot study. J Spinal Cord Med. 2012;35(2):96-101. [13] SALGA M, GATIN L, DELTOMBE T, et al. International recommendations to manage poststroke equinovarus foot deformity validated by a panel of experts using delphi. Arch Phys Med Rehabil. 2023;104(3):372-379. [14] ESQUENAZI A, BRASHEAR A, DELTOMBE T, et al. The effect of repeated abobotulinumtoxinA (Dysport(R)) injections on walking velocity in persons with spastic hemiparesis caused by stroke or traumatic brain injury. PM R. 2021;13(5):488-495. [15] AWAD LN, ESQUENAZI A, FRANCISCO GE, et al. The ReWalk ReStore soft robotic exosuit: a multi-site clinical trial of the safety, reliability, and feasibility of exosuit-augmented post-stroke gait rehabilitation. J Neuroeng Rehabil. 2020;17(1):80. [16] ESQUENAZI A, TALATY M. Robotics for Lower Limb Rehabilitation. Phys Med Rehabil Clin N Am. 2019;30(2):385-397. [17] MILLER LE, ZIMMERMANN AK, HERBERT WG. Clinical effectiveness and safety of powered exoskeleton-assisted walking in patients with spinal cord injury: systematic review with meta-analysis. Med Devices (Auckl). 2016;9:455-466. [18] LOUIE DR, ENG JJ, LAM T, et al. Gait speed using powered robotic exoskeletons after spinal cord injury: a systematic review and correlational study. J Neuroeng Rehabil. 2015;12:82. [19] BAUNSGAARD CB, NISSEN UV, BRUST AK, et al. Exoskeleton gait training after spinal cord injury: an exploratory study on secondary health conditions. J Rehabil Med. 2018;50(9):806-813. [20] AACH M, CRUCIGER O, SCZESNY-KAISER M, et al. Voluntary driven exoskeleton as a new tool for rehabilitation in chronic spinal cord injury: a pilot study. Spine J. 2014;14(12):2847-2853. [21] ASSELIN PK, AVEDISSIAN M, KNEZEVIC S, et al. Training persons with spinal cord injury to ambulate using a powered exoskeleton. J Vis Exp. 2016. doi: 10.3791/54071. [22] MORAWIETZ C, MOFFAT F. Effects of locomotor training after incomplete spinal cord injury: a systematic review. Arch Phys Med Rehabil. 2013;94(11): 2297-2308. [23] TEFERTILLER C, HAYS K, JONES J, et al. Initial outcomes from a multicenter study utilizing the indego powered exoskeleton in spinal cord injury. Top Spinal Cord Inj Rehabil. 2018;24(1):78-85. [24] ASSELIN P, KNEZEVIC S, KORNFELD S, et al. Heart rate and oxygen demand of powered exoskeleton-assisted walking in persons with paraplegia. J Rehabil Res Dev. 2015;52(2):147-158. [25] DEL-AMA AJ, GIL-AGUDO A, PONS JL, et al. Hybrid FES-robot cooperative control of ambulatory gait rehabilitation exoskeleton. J Neuroeng Rehabil. 2014;11:27. [26] MCINTOSH K, CHARBONNEAU R, BENSAADA Y, et al. The safety and feasibility of exoskeletal-assisted walking in acute rehabilitation after spinal cord injury. Arch Phys Med Rehabil. 2020;101(1):113-120. [27] FANG CY, TSAI JL, LI GS, et al. Effects of robot-assisted gait training in individuals with spinal cord injury: a meta-analysis. Biomed Res Int. 2020; 2020:2102785. [28] KWON SH, LEE BS, LEE HJ, et al. Energy efficiency and patient satisfaction of gait with knee-ankle-foot orthosis and robot (ReWalk)-assisted gait in patients with spinal cord injury. Ann Rehabil Med. 2020;44(2):131-141. [29] EDWARDS DJ, FORREST G, CORTES M, et al. Walking improvement in chronic incomplete spinal cord injury with exoskeleton robotic training (WISE): a randomized controlled trial. Spinal Cord. 2022;60(6):522-532. [30] OKAWARA H, TASHIRO S, SAWADA T, et al. Neurorehabilitation using a voluntary driven exoskeletal robot improves trunk function in patients with chronic spinal cord injury: a single-arm study. Neural Regen Res. 2022; 17(2):427-432. [31] KOSEKI K, TAKAHASHI K, YAMAMOTO S, et al. Use of robot-assisted ankle training in a patient with an incomplete spinal cord injury: a case report. J Funct Morphol Kinesiol. 2023;8(1):301. [32] EZAKI S, KADONE H, KUBOTA S, et al. Analysis of gait motion changes by intervention using robot suit hybrid assistive limb (HAL) in myelopathy patients after decompression surgery for ossification of posterior longitudinal ligament. Front Neurorobot. 2021;15:650118. [33] TAMBURELLA F, TAGLIAMONTE NL, PISOTTA I, et al. Neuromuscular controller embedded in a powered ankle exoskeleton: effects on gait, clinical features and subjective perspective of incomplete spinal cord injured subjects. IEEE Trans Neural Syst Rehabil Eng. 2020;28(5):1157-1167. [34] HONG E, GORMAN PH, FORREST GF, et al. Mobility skills with exoskeletal-assisted walking in persons with SCI: results from a three center randomized clinical trial. Front Robot AI. 2020;7:93. [35] JANG YC, PARK HK, HAN JY, et al. Cardiopulmonary function after robotic exoskeleton-assisted over-ground walking training of a patient with an incomplete spinal cord injury: Case report. Medicine (Baltimore). 2019; 98(50):e18286. [36] WU CH, MAO HF, HU JS, et al. The effects of gait training using powered lower limb exoskeleton robot on individuals with complete spinal cord injury. J Neuroeng Rehabil. 2018;15(1):14. [37] SUTOR TW, GHATAS MP, GOETZ LL, et al. Exoskeleton training and trans-spinal stimulation for physical activity enhancement after spinal cord injury (EXTra-SCI): an exploratory study. Front Rehabil Sci. 2022;2:789422. [38] YANG A, ASSELIN P, KNEZEVIC S, et al. Assessment of in-hospital walking velocity and level of assistance in a powered exoskeleton in persons with spinal cord injury. Top Spinal Cord Inj Rehabil. 2015;21(2):100-109. [39] GUANZIROLI E, CAZZANIGA M, COLOMBO L, et al. Assistive powered exoskeleton for complete spinal cord injury: correlations between walking ability and exoskeleton control. Eur J Phys Rehabil Med. 2019;55(2): 209-216. [40] MOLTEDO M, BACEK T, SERRIEN B, et al. Walking with a powered ankle-foot orthosis: the effects of actuation timing and stiffness level on healthy users. J Neuroeng Rehabil. 2020;17(1):98. [41] ANTONELLIS P, MOHAMMADZADEH GONABADI A, MYERS SA, et al. Metabolically efficient walking assistance using optimized timed forces at the waist. Sci Robot. 2022;7(64):eabh1925. [42] KIM HS, PARK JH, LEE HS, et al. Effects of wearable powered exoskeletal training on functional mobility, physiological health and quality of life in non-ambulatory spinal cord injury patients. J Korean Med Sci. 2021;36(12):e80. [43] TANG X, WANG X, JI X, et al. A wearable lower limb exoskeleton: reducing the energy cost of human movement. Micromachines (Basel). 2022; 13(6):900. [44] RAITHATHA R, CARRICO C, POWELL ES, et al. Non-invasive brain stimulation and robot-assisted gait training after incomplete spinal cord injury: a randomized pilot study. NeuroRehabilitation. 2016;38(1):15-25. [45] YOZBATIRAN N, KESER Z, DAVIS M, et al. Transcranial direct current stimulation (tDCS) of the primary motor cortex and robot-assisted arm training in chronic incomplete cervical spinal cord injury: a proof of concept sham-randomized clinical study. NeuroRehabilitation. 2016;39(3):401-411. [46] CUI Z, LI Y, HUANG S, et al. BCI system with lower-limb robot improves rehabilitation in spinal cord injury patients through short-term training: a pilot study. Cogn Neurodyn. 2022;16(6):1283-1301. [47] KRENN MJ, WHITE JM, STOKIC DS, et al. Neuromodulation with transcutaneous spinal stimulation reveals different groups of motor profiles during robot-guided stepping in humans with incomplete spinal cord injury. Exp Brain Res. 2023;241(2):365-382. [48] LI Y, WEI B, ZHONG Y, et al. A bibliometric analysis of global research on spinal cord injury: 1999-2019. Spinal Cord. 2022;60(4):281-287. [49] LIU S, SONG L, DAI W, et al. Worldwide productivity and research trend of publications concerning electroactive materials and spinal cord injury: a bibliometric study. Front Bioeng Biotechnol. 2023;11:1094059. [50] RODRIGUEZ-FERNANDEZ A, LOBO-PRAT J, FONT-LLAGUNES JM. Systematic review on wearable lower-limb exoskeletons for gait training in neuromuscular impairments. J Neuroeng Rehabil. 2021;18(1):22. [51] RAJASEKARAN V, LOPEZ-LARRAZ E, TRINCADO-ALONSO F, et al. Volition-adaptive control for gait training using wearable exoskeleton: preliminary tests with incomplete spinal cord injury individuals. J Neuroeng Rehabil. 2018;15(1):4. [52] WU AR. Human biomechanics perspective on robotics for gait assistance: challenges and potential solutions. Proc Biol Sci. 2021;288(1956):20211197. [53] ZHAO D, ZHANG Y, ZHENG Y, et al. Double-target neural circuit-magnetic stimulation improves motor function in spinal cord injury by attenuating astrocyte activation. Neural Regen Res. 2023;18(5):1062-1066. [54] SUTOR TW, KURA J, MATTINGLY AJ, et al. The effects of exercise and activity-based physical therapy on bone after spinal cord injury. Int J Mol Sci. 2022. doi: 10.3390/ijms23020608. [55] MICKENS MN, PERRIN P, GOLDSMITH JA, et al. Leisure-time physical activity, anthropometrics, and body composition as predictors of quality of life domains after spinal cord injury: an exploratory cross-sectional study. Neural Regen Res. 2022n;17(6):1369-1375. [56] GORACZKO A, ZUREK G, LACHOWICZ M, et al. Quality of life after spinal cord injury: a multiple case study examination of elite athletes. Int J Environ Res Public Health. 2020;17(20):7437. [57] NIZEYIMANA E, JOSEPH C, PHILLIPS J. Quality of life after traumatic spinal cord injury in a developing context: the influence of contextual factors and injury characteristics. Disabil Rehabil. 2022;44(10):2020-2026. [58] JO HJ, PEREZ MA. Corticospinal-motor neuronal plasticity promotes exercise-mediated recovery in humans with spinal cord injury. Brain. 2020; 143(5):1368-1382. [59] SANTAMARIA V, LUNA TD, AGRAWAL SK. Feasibility and tolerance of a robotic postural training to improve standing in a person with ambulatory spinal cord injury. Spinal Cord Ser Cases. 2021;7(1):94. [60] SUN T, DAI Z, MANOONPONG P. Robust and reusable self-organized locomotion of legged robots under adaptive physical and neural communications. Front Neural Circuits. 2023;17:1111285. [61] XIANG XN, ZONG HY, OU Y, et al. Exoskeleton-assisted walking improves pulmonary function and walking parameters among individuals with spinal cord injury: a randomized controlled pilot study.J Neuroeng Rehabil. 2021;18:86. [62] CHEN SJ, WANG ZB, LI YQ, et al. Safety and feasibility of a novel exoskeleton for locomotor rehabilitation of subjects with spinal cord injury: a prospective, multi-center, and cross-over clinical trial. Front Neurorobot. 2022;16:848443. [63] NISTOR-CSEPPENTO CD, GHERLE A, NEGRUT N, et al. The outcomes of robotic rehabilitation assisted devices following spinal cord injury and the prevention of secondary associated complications. Medicina (Kaunas). 2022;58(10):1447. [64] GIL-AGUDO A, MEGIA-GARCIA A, PONS JL, et al. Exoskeleton-based training improves walking independence in incomplete spinal cord injury patients: results from a randomized controlled trial. J Neuroeng Rehabil. 2023;20:36. |
| [1] |
Song Jiating, Chen Jianmin, Wang Kewen, Huang Lanying, Xu Senming, Gui Yuchang, Xu Jianwen.
Metabolomics analysis of serum and urine in patients with traumatic spinal cord injury #br#
#br#
[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(在线): 1-6.
|
| [2] | Zhou Bangyu, Li Jie, Ruan Yushang, Geng Funeng, Li Shaobo. Effects of Periplaneta americana powder on motor function and autophagic protein Beclin-1 in rats undergoing spinal cord hemisection [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1223-1228. |
| [3] | Xu Canli, He Wenxing, Wang Lei, Wu Fangting, Wang Jiahui, Duan Xuelin, Zhao Tiejian, Zhao Bin, Zheng Yang. Bibliometric analysis of researches on liver organoids [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1099-1104. |
| [4] | Sun Yukang, Song Lijuan, Wen Chunli, Ding Zhibin, Tian Hao, Ma Dong, Ma Cungen, Zhai Xiaoyan. Visualization analysis of stem cell therapy for myocardial infarction based on Web of Science in recent ten years [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1143-1148. |
| [5] | Zeng Fanzhuo, Li Yuxin, Sun Jiachen, Gu Xinyang, Wen Shan, Tian He, Mei Xifan. Efficient strategies for microglia replacement in spinal cord injury models [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1007-1014. |
| [6] | Liu Tao, Zhang Wenkai, Ma Ziqian, Zhang Yan, Chen Xueming. Riluzole interferes with the activation of NLRP3 inflammasome in microglia of rats with spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1036-1042. |
| [7] | Chen Zepeng, Hou Yonghui, Chen Shudong, Hou Yu, Lin Dingkun. Tauroursodeoxycholic acid treats spinal cord injury by reducing apoptosis of spinal cord neurons under glucose and oxygen deprivation [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 528-534. |
| [8] | Gao Yongchang, Fu Yantao, Zhao Xin, Cui Qingfeng, Zhang Zhifeng, Chen Shibin. Mechanical performance and collapse risk prediction of avascular necrosis of femoral head under walking movement [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(33): 5265-5269. |
| [9] | Yuan Yanli, Pan Yuejun, Guan Tianmin, Cheng Kai, Wang Xiangheng. Bibliometric and visual analysis of domestic and foreign scoliosis orthoses [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(33): 5396-5402. |
| [10] | Song Jiating, Chen Jianmin, Wang Kewen, Huang Lanying, Xu Senming, Gui Yuchang, Xu Jianwen. Metabolomics analysis of serum and urine in patients with traumatic spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(32): 5085-5090. |
| [11] | Zhang Yan, Zhang Wenkai, Zhang Wenxiu, Liu Tao, Ma Ziqian, Chen Xueming. Circ0005512 promotes microglia/macrophage pyroptosis after spinal cord injury in female rats [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(31): 5029-5035. |
| [12] | Teng Yilin, Xi Deshuang, Feng Yanbin, Liang Yu, Deng Hao, Zeng Gaofeng, Zong Shaohui. Indolepropionic acid inhibition of microglial cell M1 polarization for treatment of spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(31): 5010-5016. |
| [13] | Tao Guangyi, Wang Linzi, Yang Bin, Huang Junqing. Research hotspots of artificial intelligence in the field of spinal deformity: visual analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(30): 4915-4920. |
| [14] | Jiao Ziyuan, Zhuo Yue, Liang Roujun, Ding Qiangsheng, Zeng Xuejiu, Xu Ming, Zhang Hong. Electroacupuncture improves morphological structure of the detrusor muscle and bladder function in rats with spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(28): 4484-4490. |
| [15] | Zhang Zhilong, Yang Shengping, Chen Tianxin, Zhu Yuqi. Research hotspots and trends in the field of articular cartilage repair: a visualization analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(27): 4306-4311. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||