Chinese Journal of Tissue Engineering Research ›› 2025, Vol. 29 ›› Issue (1): 65-73.doi: 10.12307/2024.736
Previous Articles Next Articles
Exercise preconditioning combined with bone marrow mesenchymal stem cell transplantation for myocardial infarction in rats
Wang Zhikun1, Bai Shaoxuan2, Zhao Wei2, Wang Chenyu1
- 1Zhengzhou University of Aeronautics, Zhengzhou 450015, Henan Province, China; 2Logistics University of Chinese People’s Armed Police Forces, Tianjin 300309, China
-
Received:2023-10-26Accepted:2023-11-25Online:2025-01-08Published:2024-05-18 -
Contact:Wang Chenyu, MD, Associate professor, Zhengzhou University of Aeronautics, Zhengzhou 450015, Henan Province, China -
About author:Wang Zhikun, Master, Lecturer, Zhengzhou University of Aeronautics, Zhengzhou 450015, Henan Province, China -
Supported by:Henan Province Science and Technology Research Project, No. 232102321125 (to WCY)
CLC Number:
Cite this article
Wang Zhikun, Bai Shaoxuan, Zhao Wei, Wang Chenyu. Exercise preconditioning combined with bone marrow mesenchymal stem cell transplantation for myocardial infarction in rats[J]. Chinese Journal of Tissue Engineering Research, 2025, 29(1): 65-73.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
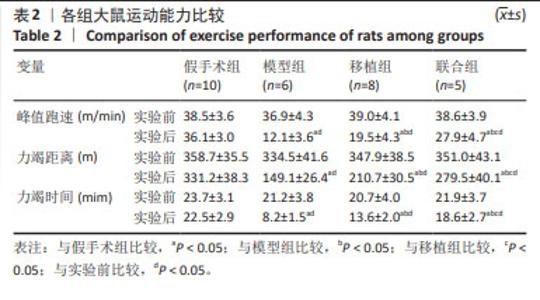
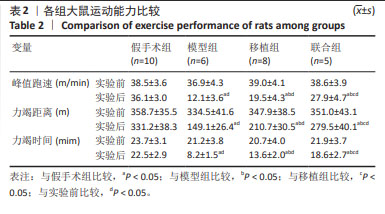
2.1 骨髓间充质干细胞鉴定结果 通过流式细胞仪测定细胞表面抗原阳性率,结果发现,CD34阳性率为1.74%(< 5%),CD90和CD44阳性率分别为98.1%和97.5%(> 95%),所检测细胞表面标志物符合大鼠骨髓间充质干细胞表面抗原表达类型,见图2。 2.2 各组大鼠运动能力比较 实验前,各组运动能力(峰值跑速、力竭距离、力竭时间)比较均无显著性差异(P > 0.05)。与实验前比较,实验后模型组、移植组和联合组运动能力均下降(P < 0.05),假手术组无显著性差异(P > 0.05);与假手术组比较,模型组运动能力降低(P < 0.05);与模型组比较,移植组和联合组运动能力升高(P < 0.05);与移植组比较,联合组运动能力各参数进一步提升(P < 0.05),见表2。 "
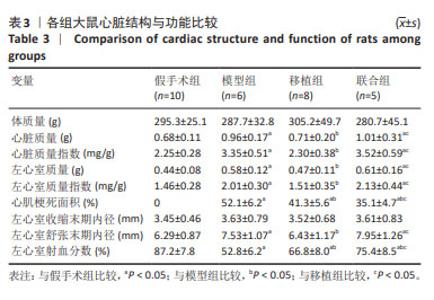
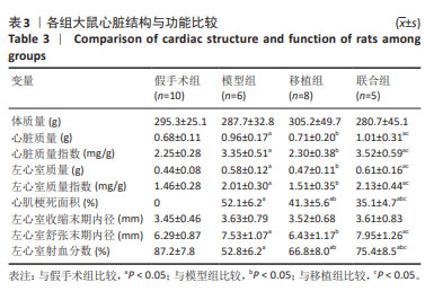
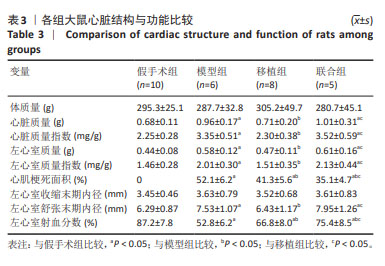
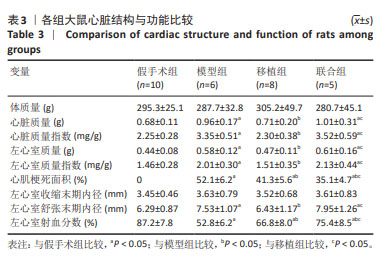
2.3 各组大鼠心脏结构、功能及左心室血液动力学比较 各组心脏结构和功能见表3。与假手术组比较,模型组心脏质量、心脏质量指数、左心室质量、左心室质量指数、心肌梗死面积、左心室舒张末期内径增加(P < 0.05),左心室射血分数降低(P < 0.05);与模型组比较,移植组心脏质量、心脏质量指数、左心室质量、左心室质量指数、心肌梗死面积、左心室舒张末期内径下降(P < 0.05),左心室射血分数升高(P < 0.05),联合组心肌梗死面积降低(P < 0.05),左心室射血分数升高(P < 0.05),心脏质量、心脏质量指数、左心室质量、左心室质量指数、左心室舒张末期内径无显著性变化(P > 0.05);与移植组比较,联合组心脏质量、心脏质量指数、左心室质量、左心室质量指数、左心室舒张末期内径、左心室射血分数升高(P < 0.05),心肌梗死面积降低(P < 0.05)。"
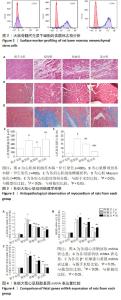
2.4 各组大鼠心肌组织病理学观察结果 心肌纵切面苏木精-伊红染色显示:假手术组心肌纤维排列整齐,胞浆染色均匀,细胞核边界清晰;模型组心肌纤维排列紊乱,可见大量中性粒细胞浸润,广泛坏死;与模型组比较,移植组和联合组上述组织病理学改变均明显减轻,见图3A。 心肌横切面苏木精-伊红染色显示:与假手术组比较,模型组心肌细胞肿大,心肌细胞横截面积较明显增加(P < 0.05);与模型组比较,移植组心肌细胞肿大明显减轻,心肌细胞横截面积显著下降(P < 0.05);与移植组比较,联合组心肌细胞横截面积升高(P < 0.05),见图3B和图3C。 心肌Masson染色显示:假手术组几乎无胶原纤维;模型组细胞间质存在大量胶原纤维并发生心肌纤维化,胶原容积分数较假手术组明显升高(P < 0.05);移植组和联合组胶原沉积明显减轻,胶原容积分数较模型组明显下降(P < 0.05);与移植组比较,联合组胶原容积分数较模型组进一步降低(P < 0.05),见图3D,E。 2.5 各组大鼠心肌胚胎基因mRNA表达量比较 与假手术组比较,模型组心房钠尿肽、脑钠肽、β-肌球蛋白重链mRNA表达量上调(P < 0.05);与模型组比较,移植组和联合组上述各胚胎基因mRNA表达量均下调(P < 0.05);与移植组比较,联合组各胚胎基因mRNA表达量进一步下降(P < 0.05),见图4。"

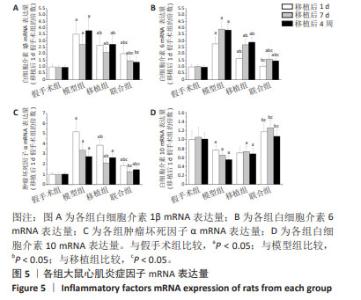
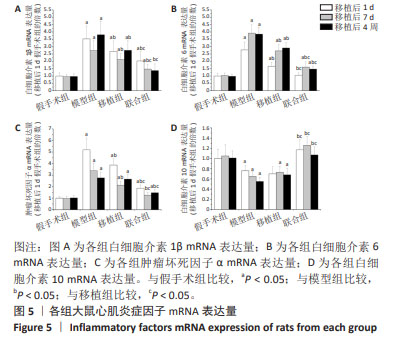
2.6 各组大鼠心肌炎症因子mRNA表达量比较 与假手术组比较,模型组白细胞介素1β、白细胞介素6、肿瘤坏死因子α mRNA表达量上调(P < 0.05),白细胞介素10 mRNA表达量下调(P < 0.05);与模型组比较,移植组白细胞介素1β、白细胞介素6、肿瘤坏死因子α(除移植后4周)mRNA表达量下调(P < 0.05),白细胞介素10 mRNA表达量无显著性变化(P > 0.05),联合组各促炎症因子表达量下调(P < 0.05),白细胞介素10 mRNA表达量上调(P < 0.05);与移植组比较,联合组各促炎症因子mRNA表达量下降(P < 0.05),白细胞介素10 mRNA表达量升高(P < 0.05),见图5。 "
| [1] 孙维兴,赵永超,赵然尊.间充质干细胞移植治疗心肌梗死:问题、症结及新突破[J].中国组织工程研究,2021,25(19):3103-3109. [2] 王文华,刘洋,吕洋,等.骨髓间充质干细胞向心肌细胞分化的研究进展[J] 华中科技大学学报(医学版),2021,50(6):811-816. [3] YAMADA Y, MINATOGUCHI S, KANAMORI H, et al. Stem cell therapy for acute myocardial infarction - focusing on the comparison between Muse cells and mesenchymal stem cells. J Cardiol. 2022; 80(1):80-87. [4] MENG H, CHENG W, WANG L, et al. Mesenchymal stem cell exosomes in the treatment of myocardial infarction: a systematic review of preclinical in vivo studies. J Cardiovasc Transl Res. 2022;15(2):317-339. [5] HICKS MR, PYLE AD. The emergence of the stem cell niche. Trends Cell Biol. 2023;33(2):112-123. [6] KHODAYARI S, KHODAYARI H, AMIRI AZ, et al. Inflammatory microenvironment of acute myocardial infarction prevents regeneration of heart with stem cells therapy. Cell Physiol Biochem. 2019;53(5): 887-909. [7] LEE CC, HIRASAWA N, GARCIA KG, et al. Stem and progenitor cell microenvironment for bone regeneration and repair. Regen Med. 2019; 14(7): 693-702. [8] LI H, HOU L. Regulation of melanocyte stem cell behavior by the niche microenvironment. Pigment Cell Melanoma Res. 2018;31(5):556-569. [9] 黄宏,邱伟,陈民佳,等.干细胞预处理及其保护机制的研究进展[J].中华损伤与修复杂志(电子版),2017,12(2):138-142. [10] QUINDRY JC, FRANKLIN BA. Exercise preconditioning as a cardioprotective phenotype. Am J Cardiol. 2021;148:8-15. [11] CHIRICO EN, DING D, MUTHUKUMARAN G, et al. Acute aerobic exercise increases exogenously infused bone marrow cell retention in the heart. Physiol Rep. 2015; 3(10):e12566. [12] 张艳,何瑞波,王庆博,等.不同负荷量有氧运动对肥胖大鼠骨骼肌炎症反应和胰岛素信号途径的影响及机制[J].中国组织工程研究,2023,27(8):1237-1244. [13] HAN BJ, CAO GY, JIA LY, et al. Cardioprotective effects of tetrahydropalmatine on acute myocardial infarction in rats. Am J Chin Med. 2022;50(7):1887-1904. [14] 李鑫辉,黄淼鑫,杜建芳,等.丹参通络解毒汤联合骨髓干细胞移植对急性心肌梗死大鼠心肌纤维化的影响及其机制[J].北京中医药大学学报,2019,42(8):655-661. [15] LAVORATO VN, DEL CARLO RJ, DA CUNHA DN, et al. Mesenchymal stem cell therapy associated with endurance exercise training: effects on the structural and functional remodeling of infarcted rat hearts. J Mol Cell Cardiol. 2016;90:111-119. [16] COSMO S, FRANCISCO JC, CUNHA RC, et al. Effect of exercise associated with stem cell transplantation on ventricular function in rats after acute myocardial infarction. Rev Bras Cir Cardiovasc. 2012;27(4):542-551. [17] DOS SANTOS L, ANTONIO EL, SOUZA AF, et al. Use of afterload hemodynamic stress as a practical method for assessing cardiac performance in rats with heart failure. Can J Physiol Pharmacol. 2010; 88(7):724-732. [18] SANTOS AA, HELBER I, FLUMIGNAN RL, et al. Doppler echocardiographic predictors of mortality in female rats after myocardial infarction. J Card Fail. 2009;15(2):163-168. [19] ALBAENI A, DAVIS JW, AHMAD M. Echocardiographic evaluation of the athlete’s heart. Echocardiography. 2021;38(6):1002-1016. [20] OLDFIELD CJ, DUHAMEL TA, DHALLA NS. Mechanisms for the transition from physiological to pathological cardiac hypertrophy. Can J Physiol Pharmacol. 2020;98(2):74-84. [21] TASHIRO H, TANAKA A, ISHII H, et al. Reduced exercise capacity and clinical outcomes following acute myocardial infarction. Heart Vessels. 2020;35(8):1044-1050. [22] SQUIRES RW, BONIKOWSKE AR. Cardiac rehabilitation for heart transplant patients: considerations for exercise training. Prog Cardiovasc Dis. 2022;70:40-48. [23] NAKAMUTA JS, DANOVIZ ME, MARQUES FL, et al. Cell therapy attenuates cardiac dysfunction post myocardial infarction: effect of timing, routes of injection and a fibrin scaffold. PLoS One. 2009;4(6): e6005. [24] 姜俣,钱海燕.间充质干细胞治疗心肌梗死的研究进展[J].基础医学与临床,2023,43(1):21-29. [25] ZHANG H, CHEN H, WANG W, et al. Cell survival and redistribution after transplantation into damaged myocardium. J Cell Mol Med. 2010;14(5):1078-1082. [26] ZHANG H, SONG P, TANG Y, et al. Injection of bone marrow mesenchymal stem cells in the borderline area of infarcted myocardium: heart status and cell distribution. J Thorac Cardiovasc Surg. 2007;134(5):1234-1240. [27] HANNA A, FRANGOGIANNIS NG. Inflammatory cytokines and chemokines as therapeutic targets in heart failure. Cardiovasc Drugs Ther. 2020;34(6):849-863. [28] 钟世根,骆杰,王志刚,等.超声靶向破碎微泡对心肌梗死犬心肌微环境的影响[J].基因组学与应用生物学,2017,36(11):4528-4533. [29] PEDERSEN BK. Anti-inflammatory effects of exercise: role in diabetes and cardiovascular disease. Eur J Clin Invest. 2017;47(8):600-611. [30] SANTOS MH, HIGUCHI MDE L, TUCCI PJ, et al. Previous exercise training increases levels of PPAR-α in long-term post-myocardial infarction in rats, which is correlated with better inflammatory response. Clinics (Sao Paulo). 2016;71(3):163-168. [31] NUNES RB, ALVES JP, KESSLER LP, et al. Aerobic exercise improves the inflammatory profile correlated with cardiac remodeling and function in chronic heart failure rats. Clinics (Sao Paulo). 2013;68(6):876-882. [32] WANG L, WEI FX, CEN JS, et al. Early administration of tumor necrosis factor-alpha antagonist promotes survival of transplanted neural stem cells and axon myelination after spinal cord injury in rats. Brain Res. 2014;1575:87-100. [33] SUZUKI K, MURTUZA B, BEAUCHAMP JR, et al. Role of interleukin-1beta in acute inflammation and graft death after cell transplantation to the heart. Circulation. 2004;110(11 Suppl 1):219-224. [34] KRISHNAMURTHY P, THAL M, VERMA S, et al. Interleukin-10 deficiency impairs bone marrow-derived endothelial progenitor cell survival and function in ischemic myocardium. Circ Res. 2011;109(11):1280-1289. [35] BOROW KM, YAROSHINSKY A, GREENBERG B, et al. Phase 3 dream-HF trial of mesenchymal precursor cells in chronic heart failure. Circ Res. 2019;125(3):265-281. |
| [1] | Yang Zhihang, Sun Zuyan, Huang Wenliang, Wan Yu, Chen Shida, Deng Jiang. Nerve growth factor promotes chondrogenic differentiation and inhibits hypertrophic differentiation of rabbit bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(7): 1336-1342. |
| [2] | Lou Guo, Zhang Min, Fu Changxi. Exercise preconditioning for eight weeks enhances therapeutic effect of adipose-derived stem cells in rats with myocardial infarction [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(7): 1363-1370. |
| [3] | Liu Qi, Li Linzhen, Li Yusheng, Jiao Hongzhuo, Yang Cheng, Zhang Juntao. Icariin-containing serum promotes chondrocyte proliferation and chondrogenic differentiation of stem cells in the co-culture system of three kinds of cells [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(7): 1371-1379. |
| [4] | Aikepaer · Aierken, Chen Xiaotao, Wufanbieke · Baheti. Osteogenesis-induced exosomes derived from human periodontal ligament stem cells promote osteogenic differentiation of human periodontal ligament stem cells in an inflammatory microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(7): 1388-1394. |
| [5] | Zhang Zhenyu, Liang Qiujian, Yang Jun, Wei Xiangyu, Jiang Jie, Huang Linke, Tan Zhen. Target of neohesperidin in treatment of osteoporosis and its effect on osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(7): 1437-1447. |
| [6] | He Bo, Chen Wen, Ma Suilu, He Zhijun, Song Yuan, Li Jinpeng, Liu Tao, Wei Xiaotao, Wang Weiwei, Xie Jing . Pathogenesis and treatment progress of flap ischemia-reperfusion injury [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(6): 1230-1238. |
| [7] | Gao Yang, Qin Hewei, Liu Dandan. ACSL4 mediates ferroptosis and its potential role in atherosclerotic cardiovascular disease [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(6): 1239-1247. |
| [8] | Sun Xianjuan, Wang Qiuhua, Zhang Jinyi, Yang Yangyang, Wang Wenshuang, Zhang Xiaoqing. Adhesion, proliferation, and vascular smooth muscle differentiation of bone marrow mesenchymal stem cells on different electrospinning membranes [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(4): 661-669. |
| [9] | Ge Xiao, Zhao Zhuangzhuang, Guo Shuyu, Xu Rongyao. HOXA10 gene-modified bone marrow mesenchymal stem cells promote bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(36): 7701-7708. |
| [10] | Zhang Xiongjinfu, Chen Yida, Cheng Xinyi, Liu Daihui, Shi Qin . Exosomes derived from bone marrow mesenchymal stem cells of young rats to reverse senescence in aged rat bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(36): 7709-7718. |
| [11] | Sima Xinli, Liu Danping, Qi Hui. Effect and mechanism of metformin-modified bone marrow mesenchymal stem cell exosomes on regulating chondrocytes [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(36): 7728-7734. |
| [12] | Yang Dingyan, Yu Zhenqiu, Yang Zhongyu. Machine learning-based analysis of neutrophil-associated potential biomarkers for acute myocardial infarction [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(36): 7909-7920. |
| [13] | Liu Lu, Zhong Chang, Yu Xin, Ren Chenyuan, Gong Yangyang, Zhou Ping, Wang Yingbin. Academic progress and clinical application of in vitro synthetic microenvironment to promote maturation of human pluripotent stem cell-derived cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(36): 7856-7862. |
| [14] | Liu Chengyuan, Guo Qianping. Differential effects of kartogenin on chondrogenic and osteogenic differentiation of rat and rabbit bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(35): 7490-7498. |
| [15] | Liu Xuan, Ding Yuqing, Xia Ruohan, Wang Xianwang, Hu Shujuan. Exercise prevention and treatment of insulin resistance: role and molecular mechanism of Keap1/nuclear factor erythroid2-related factor 2 signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(35): 7578-7588. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||