Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (34): 5565-5570.doi: 10.12307/2024.578
Previous Articles Next Articles
Spatio-temporal gait characteristics of the elderly and the risk of adverse health outcomes
Wang Chenglong1, Li Mingzhe1, Nie Mingjian2, Wang Jingjing1
- 1China Institute of Sport Science, Beijing 100061, China; 2School of Sports and Human Sciences, Beijing Sport University, Beijing 100084, China
-
Received:2023-10-24Accepted:2023-12-16Online:2024-12-08Published:2024-03-15 -
Contact:Wang Jingjing, PhD, Associate researcher, Master’s supervisor, China Institute of Sports Science, Beijing 100061, China -
About author:Wang Chenglong, Master candidate, China Institute of Sport Science, Beijing 100061, China -
Supported by:Fundamental Research Fund of China Institute of Sport Science, No. Basic 21-19 (to WJJ)
CLC Number:
Cite this article
Wang Chenglong, Li Mingzhe, Nie Mingjian, Wang Jingjing. Spatio-temporal gait characteristics of the elderly and the risk of adverse health outcomes[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(34): 5565-5570.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks

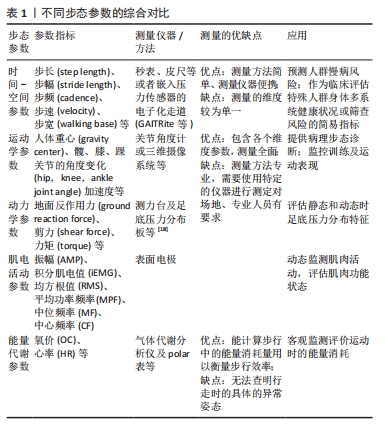
2.1 步行和步态的概述 步行(walking)是指通过双脚的交互动作移行机体的人类特征性活动,步态(gait)可以被定义为人类在行走这一活动过程中显现出来的特征,是在神经中枢命令、身体协调控制下的协同运动,它涉及下肢关节和肌肉的参与,同时也与上肢和躯干姿势有关。以正常状态步行时,人体具有身体平稳、步长适中、节奏适当的外在表现,良好的步态是人体神经系统、骨骼肌肉系统、心血管系统、视觉听觉和本体感觉等多系统相互作用的结果,其中任一环节的失调都有可能影响步态[10]。 步态参数是步态分析(gait analysis)当中用于揭示步态规律的定量分析参数,步态参数通常归为以下5类:①时间-空间参数:主要包括步速、步长、步频和步宽等,常用于临床筛查或评估特殊人群健康风险;②运动学参数:测量人体重心位置、下肢髋、膝、踝关节的角度变化和加速度等,常用于竞技体育监控运动员运动表现,也可用于提供病理性的步态诊断;③动力学参数:涉及到运动中力的变化,通常测量压力或地面反作用力等,一般用于测量和评估个体处于静态或动态时足底压力的分布特征;④肌电活动参数:包括积分肌电值、均方根值、振幅和平均功率频率等常见的测量指标,用于动态监控某块或某区域的肌肉电活动;⑤能量代谢参数:主要测量氧价和心率等,能客观监测运动过程中的能量消耗。 其中运动学参数、动力学参数、肌电活动参数和能量代谢参数的测量较为复杂,需要电子关节角度计、测力台、肌电图和气体分析仪等特定仪器,由于测量通常需要专业的实验室,且测试设备昂贵、分析过程复杂,这类参数常只应用于小样本量研究。相比较而言,时间-空间参数的测量更加便捷,传统的测量仪器只需要秒表、皮尺及能够留下“足印”的白纸和墨水,常被研究者应用于大型的横断面研究或队列研究中探究各种参数与人群健康的关系,具体步态参数的综合对比见表1。"


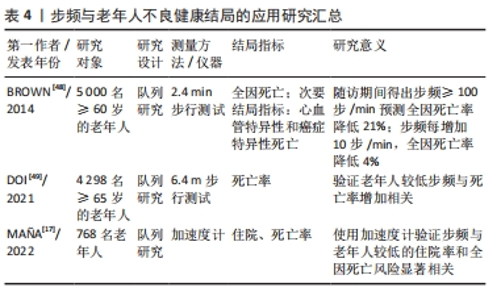
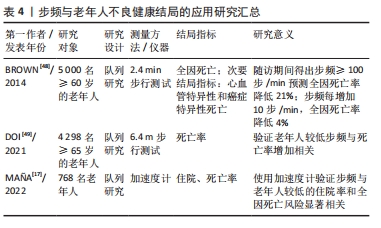
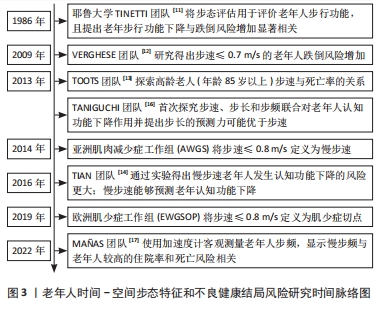
自1986年TINETTI[11]将步态评估应用于评价老年人步行功能,并提出老年人步行能力下降与跌倒风险显著相关后,相关研究领域的学者开始逐渐对步态时间-空间参数和老年人不良健康结局开展研究。初期研究者们主要集中于步速这一最具代表性也容易测量的步态参数进行研究,由于当时领域内对于老年人步速的界值没有明确的定义,因此学者们大多通过百分位数对慢步速进行划分,探索由步速百分位数分组的老年人在不良健康结局上是否出现显著性差异[12–15],直到2014年和2019年亚洲和欧洲分别发布肌少症共识才将步速≤0.8 m/s作为评定肌少症的指标之一,后续学者一般将0.8 m/s作为慢步速的界值。当步速被证明与老年人不良健康结局后,步长和步频等其他时间-空间参数也逐渐被研究者们关注[15-16],同时随着技术的发展,测量设备变得更加精细化,加速度计[17]、电子化走道等仪器的出现也使得测量结果更加准确客观。具体时间脉络见图3。"

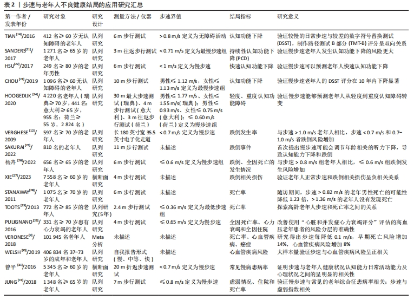
2.2 步态时间-空间参数与不良健康结局 2.2.1 步速与不良健康结局 步速即步行时的速度,通常是指习惯性步速。国内外研究表明步速与老年人健康状况相关,步速降低可能会增加老年人跌倒风险,使老年人全因死亡率上升,并且与老年人认知功能下降、心血管疾病患病风险增加等多种不良健康结局相关[18-20]。 步速与认知功能共检索到5项相关研究[14,21–24],纳入研究中多用百分位数对步速进行分组,慢步速界值在0.6-1.13 m/s,结果均表明慢步速与老年人认知功能下降相关(HR=2.90-4.58);另外,慢步速也能够预测老年人从轻度到重度认知障碍的转变[24]。1986年,耶鲁大学TINETTI[11]提出老年人移动能力下降与跌倒风险增加明显相关,后续一些学者进一步开展相关研究。步速与跌倒风险检索到4项相关研究[12,25–27],慢步速界值为0.6-1.0 m/s,研究结果表明慢步速老年人存在更高的跌倒风险(HR:1.22-1.64);此外,不良的步态也可能会调节与年龄相关听力下降对身体功能的影响,从而导致老年人更容易出现认知功能下降或跌倒事件。步速与全因死亡共检索到3项研究[13,28-29],老年人慢步速界值为0.37-1.02 m/s,研究结果均表明相较于快步速,慢步速的老年人有更高的死亡风险。相较于行走速度较慢的老年男性,步速超过0.82 m/s的老年男性死亡风险降低1.23倍,并且步速每增加1个单位(m/s),死亡率降低为2.77倍[28];类似研究结果同样在患有心力衰竭的老年人中出现[29]。步速与心血管疾病共检索到2项研究[9,30],步速每降低0.1 m/s,致命或非致命(复合)的心血管风险增加13%(HR=1.13,95%CI:1.08-1.18)[9],相较于男性,> 60岁慢步速女性患心血管疾病的风险更高[30]。除此之外,慢步速老年人患常见慢性疾病(高血压、冠心病、心脑血管病和糖尿病)比例更高[31],需要公共机构照料的风险也更高,并且步速与老年人衰弱指数也呈现出负相关关系[15]。 上述研究提示,步速作为一个简单实用的步行参数,在临床医学和公共卫生学方面有重要意义。无论是健康老年人还是患有某些疾病的老年患者,慢步速均与老年人风险结局相关。上述综述中,较为常用的衡量老年人身体健康状况的慢步速界值为0.8 m/s[14,26,32-36],但由于测量的方法、人群的年龄和种族的不同,以及地域、受测时老年人的身体健康状况等因素都会影响步速测量值,目前国际上并未对可能预示老年人发生不良结局的步速界值提出明确定义。 表2汇总了步速与老年人认知功能下降、跌倒事件、全因死亡、心血管疾病及虚弱等不良健康结局的关系。"
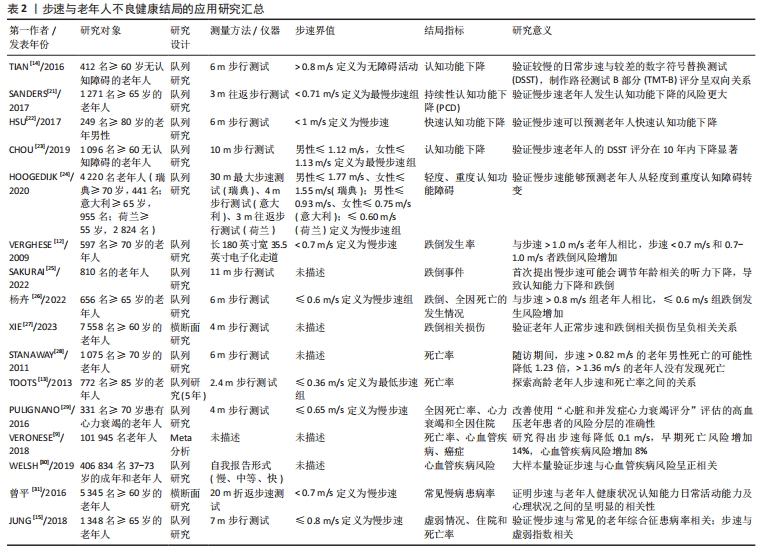

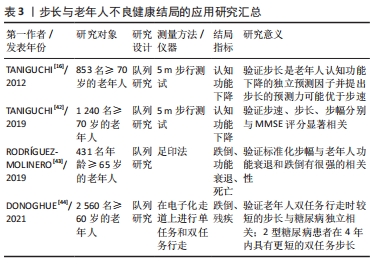
2.2.2 步长与不良健康结局 人体在行走时左右足跟(或趾尖)间的前后距离被称为步长[37],步长反映了下肢肌肉力量和关节运动能力[38-39];最大步长测试(Maximum Step Length,MSL)经常作为临床上评估平衡能力的方法[40-41]。 老年人步长(ρ=0.124,P < 0.001)及步长变异性(ρ=-0.145,P < 0.001)均与简易精神状态检查 (Mini-Mental State Examination,MMSE)得分相关联[42],不论是在最快步速状态下行走时还是日常步速状态下行走时,步长较短的老年人发生认知功能下降的可能性都要显著高于步长较长的老年人[16]。有研究探究步幅(步幅等于2倍的步长)与老年人跌倒、功能衰退和死亡的关系[43],研究发现以受试者身高标准化后的步幅< 0.52能够预测老年人未来6个月的跌倒(93%的敏感性和53%的特异性,AUC=0.72)、标准化后的步幅< 0.5能够预测老年人未来12个月的功能衰退(81%的敏感性和57%的特异性,AUC=0.67)。有研究将双任务纳入老年人步行研究中,得出老年人在进行双任务行走时,较短的步长与糖尿病独立相关[44]。另外,也有研究表明,当老年人在行走过程中面对障碍时,通常以调整步长为主规避障碍从而避免跌倒事件发生[45]。 相较步速,有关步长与老年人风险结局的研究较少。步长主要受身高和下肢长度的影响,通常来说在其他客观条件一致的情况下,个体身高与步长呈正相关。但随年龄增长,步长所呈现的下降趋势却不是由身高不同产生的,中国学者伍勰等[46]对健康老年人常速行走进行分析,按照性别和年龄分组(60-70岁组,71-80岁组)测量其步速、步长与步频,测量结果显示,男女受试者随年龄增大,3项参数均呈下降趋势,但男女对应两组身高对比无显著性差异,故得出随年龄增大带来的步长下降并不是因身高不同产生的。这项研究也证实上述研究得出的结论:步长变短反映了老年人身体功能的下降,可以作为风险结局的独立预测因子。 表3汇总了步长与老年人跌倒、功能衰退、认知功能下降及全因死亡等不良健康结局的关系。"

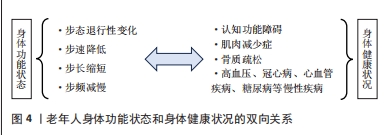
另外,峰值-30步频(peak-30 cadence,通过选择每天30个最高步频值,计算其均值,再累计所有天数的均值得出[47])也被证明与成年人全因死亡率、癌症和心血管发病率]以及痴呆相关[50-51],但研究多集中于成年人群研究,针对老年人群的相关研究较少,仅检索到1项横断面研究纳入222名60-80岁的老年人,采用三轴加速度计连续测定其7日步频,结果显示,峰值-30步频每增加10步/min,主动脉脉搏波传导速度下降0.05 m/s(95%CI:-0.09-0.01,P=0.018),提示峰值-30步频与老年人动脉僵硬程度呈负相关关系[52]。 以上研究表明老年人步态参数的变化和身体健康状况密切相关,步速降低、步长缩短、步频减慢会降低老年人健康水平,增加老年人发生不良健康结局的风险。也有部分研究发现,已经出现身体健康状况下降的老年人,其步态也会发生相应改变,认为老年人身体功能状态和健康状况两者之间存在双向相关关系。一方面,身体功能方面的下降会导致老年人日常生活能力降低,表现在老年人的活动范围减少,可自主完成的活动减少,受到外界环境刺激的程度减弱,这些又会进一步增加老年人发生超重、肥胖、认知功能障碍、骨质疏松和心血管疾病等多重慢性疾病的风险,这就让老年人再次遇到突发事件时难以通过迅速调整步态来规避风险,从而增大了老年人发生跌倒事件的概率也对应增加了全因死亡等其他不良健康结局的风险。另一方面,已经患有认知功能障碍、持续性下肢功能受限、肌肉减少症等慢病或曾经发生过跌倒、骨折等意外事件的老年人也会影响老年人与运动相关的神经肌肉活动,使其在日常行走时更加谨慎,采用慢步速、短步长的行走方式,最终也导致老年人步态发生退行性变化,见图4。"
| [1] 蔡敏,谢学勤,吴士勇.我国老年人口健康状况及卫生服务利用[J].中国卫生信息管理杂志,2021,18(1):27-34,49. [2] 刘敏,李玉茹,王健,等.不同步速条件下超重肥胖老年人步态运动学特征[J].中国老年学杂志,2022,42(13):3216-3220. [3] MIDDLETON A, FRITZ SL, LUSARDI M. Walking speed: the functional vital sign. J Aging Phys Act. 2015;23(2):314-322. [4] WALSH JA, BARKER RE, KON SSC, et al. Gait speed and adverse outcomes following hospitalised exacerbation of COPD. Eur Respir J. 2021;58(5): 2004047. [5] 王莉,于卫华.步态分析在老年人跌倒中的应用进展[J].中华护理杂志, 2016,51(3):347-351. [6] 张杰,沈通桃.步速在老年患者评估中的应用[J].国际麻醉学与复苏杂志,2020,41(12):1191-1195. [7] 吴梦余,于卫华.步行速度在老年衰弱相关不良事件中的应用进展[J].护理学报,2018,25(17):21-24. [8] 路菲,王青,杨卉.老年人步速和握力与不良健康结局关系的研究进展[J].中华老年医学杂志,2021,40(11):1444-1448. [9] VERONESE N, STUBBS B, VOLPATO S, et al. Association between gait speed with mortality, cardiovascular disease and cancer: a systematic review and meta-analysis of prospective cohort studies. J Am Med Dir Assoc. 2018;19(11):981-988.e7. [10] SNIJDERS AH, VAN DE WARRENBURG BP, GILADI N, et al. Neurological gait disorders in elderly people: clinical approach and classification. Lancet Neurol. 2007;6(1):63-74. [11] TINETTI ME. Performance-oriented assessment of mobility problems in elderly patients. J Am Geriatrs Soc. 1986;34(2):119-126. [12] VERGHESE J, HOLTZER R, LIPTON RB, et al. Quantitative gait markers and incident fall risk in older adults. Journals Gerontol A Biol Sci Med Sci. 2009;64A(8):896-901. [13] TOOTS A, ROSENDAHL E, LUNDIN-OLSSON L, et al. Usual gait speed independently predicts mortality in very old people: a population-based study. J American Med Dir Assoc. 2013;14(7):529.e1-529.e6. [14] TIAN Q, AN Y, RESNICK S M, et al. The relative temporal sequence of decline in mobility and cognition among initially unimpaired older adults: results from the baltimore longitudinal study of aging. Age Ageing. 2016;46(3): 445-451. [15] JUNG HW, JANG IY, LEE CK, et al. Usual gait speed is associated with frailty status, institutionalization, and mortality in community-dwelling rural older adults: a longitudinal analysis of the aging study of pyeongchang rural area. Clin Interv Aging. 2018;13:1079-1089. [16] TANIGUCHI Y, YOSHIDA H, FUJIWARA Y, et al. A prospective study of gait performance and subsequent cognitive decline in a general population of older Japanese. J Gerontol A Bio Sci Med Sci. 2012;67(7):796-803. [17] MAÑAS A, DEL POZO CRUZ B, EKELUND U, et al. Association of accelerometer-derived step volume and intensity with hospitalizations and mortality in older adults: a prospective cohort study. J Sport Health Sci. 2022;11(5):578-585. [18] 钱竞光,宋雅伟,叶强,等.步行动作的生物力学原理及其步态分析[J].南京体育学院学报(自然科学版),2006,5(4):1-7, 39. [19] 崔玉鹏,洪峰.表面肌电图在人体运动研究中的应用[J].首都体育学院学报,2005,17(1):102-104, 114. [20] 王桂茂,严隽陶.应用三维运动解析技术定量观测步态变化[J].中国组织工程研究与临床康复,2007,11(35):7081-7083. [21] SANDERS JB, BREMMER MA, COMIJS HC, et al. Gait speed and processing speed as clinical markers for geriatric health outcomes. Am J Geriatr Psychiatry. 2017;25(4):374-385. [22] HSU CL, LIANG CK, LIAO MC, et al. Slow gait speed as a predictor of 1-year cognitive decline in a veterans’ retirement community in southern Taiwan: The relationship between low gait speed and one-year cognitive decline. Geriatr Gerontol Int. 2017;17 Suppl 1:14-19. [23] CHOU MY, NISHITAY, NAKAGAWA T, et al. Role of gait speed and grip strength in predicting 10-year cognitive decline among community-dwelling older people. BMC Geriatr. 2019;19(1):186. [24] HOOGENDIJK EO, RIJNHART JJM, SKOOG J, et al. Gait speed as predictor of transition into cognitive impairment: findings from three longitudinal studies on aging. Exp Gerontol. 2020;129:110783. [25] SAKURAI R, KAWAI H, YANAI S, et al. Gait and age‐related hearing loss interactions on global cognition and falls. Laryngoscope. 2022;132(4): 857-863. [26] 杨卉,崔云婧,张少景,等.步速和握力对住院老年患者全因死亡和跌倒的预测价值研究[J].中国全科医学,2022,25(32):4010-4017. [27] XIE H, CHEN E, ZHANG Y. Association of walking pace and fall-related injury among Chinese older adults: data from the SAGE survey. Complementary The Clin Pract. 2023;50:101710. [28] STANAWAY FF, GNJIDIC D, BLYTH FM, et al. How fast does the Grim Reaper walk? Receiver operating characteristics curve analysis in healthy men aged 70 and over. BMJ. 2011;343:d7679. [29] PULIGNANO G, DEL SINDACO D, DI LENARDA A, et al. Incremental value of gait speed in predicting prognosis of older adults with heart failure: insights from the IMAGE-HF study. JACC Heart Fail. 2016;4(4):289-298. [30] WELSH CE, CELIS-MORALES CA, HO FK, et al. Grip strength and walking pace and cardiovascular disease risk prediction in 406,834 UK biobank participants. Mayo Clin Proc. 2020;95(5):879-888. [31] 曾平,韩怡文,庞婧,等.步速降低与老年人健康及相关状况的关系[J].中华老年医学杂志,2016,35(7):773-777. [32] LO AX, DONNELLY JP, MCGWIN G, et al. Impact of gait speed and instrumental activities of daily living on all-cause mortality in adults ≥65 years with heart failure. Am J Cardiol. 2015;115(6):797-801. [33] ODDEN MC, PERALTA CA, HAAN MN, et al. Rethinking the association of high blood pressure with mortality in elderly adults: the impact of frailty. Arch Intern Med. 2012;172(15):1162-1168. [34] LAURETANI F, RUSSO CR, BANDINELLI S, et al. Age-associated changes in skeletal muscles and their effect on mobility: an operational diagnosis of sarcopenia. J Appl Physiol. 2003;95(5):1851-1860. [35] CLEGG A, ROGERS L, YOUNG J. Diagnostic test accuracy of simple instruments for identifying frailty in community-dwelling older people: a systematic review. Age Ageing. 2015;44(1):148-152. [36] 刘莉,叶鹏, GUTIÉRREZ-MISIS A,等.西班牙老年人群的步速与高血压死亡风险的关系[J].中华高血压杂志,2015,23(5):464. [37] 赵芳,周兴龙,张振清,等.中老年人步态指标与衰老关系的研究[J].体育科学,1998,18(6):78-81. [38] LIM YP, LIN YC, PANDY MG. Effects of step length and step frequency on lower-limb muscle function in human gait. J Biomech. 2017;57:1-7. [39] BIERYLA KA, BUFFINTON C. Effects of age and step length on joint kinetics during stepping task. J Biomech. 2015;48(10):1679-1686. [40] CHO BL, SCARPACE D, ALEXANDER NB. Tests of stepping as indicators of mobility, balance, and fall risk in balance-impaired older adults. J Am Geriatr Soc. 2004;52(7):1168-1173. [41] NNODIM JO, STRASBURG D, NABOZNY M, et al. Dynamic balance and stepping versus tai chi training to improve balance and stepping in at-risk older adults. J Am Geriatr Soc. 2006;54(12):1825-1831. [42] TANIGUCHI Y, WATANABE Y, OSUKA Y, et al. Characteristics for gait parameters of community-dwelling elderly Japanese with lower cognitive function. PLoS One. 2019;14(3):e0212646. [43] RODRÍGUEZ-MOLINERO A, HERRERO-LARREA A, MIÑARRO A, et al. The spatial parameters of gait and their association with falls, functional decline and death in older adults: a prospective study. Sci Rep. 2019;9(1):8813. [44] DONOGHUE OA, LEAHY S, KENNY RA. Longitudinal associations between gait, falls, and disability in community-dwelling older adults with type II diabetes mellitus: findings from the irish longitudinal study on ageing (TILDA). J Gerontol A Bio Sci Med Sci. 2021;76(5):906-913. [45] CAETANO MJD, MENANT JC, SCHOENE D, et al. Sensorimotor and cognitive predictors of impaired gait adaptability in older people. J Gerontol A Bio Sci Med Sci. 2017,72(9):1257-1263. [46] 伍勰,陆爱云,庞军.健康老年人常速行走的步态分析[J].上海体育学院学报,2000,24(2):52-55, 64. [47] SAINT-MAURICE PF, TROIANO RP, BASSETT DR, et al. Association of daily step count and step intensity with mortality among US adults. JAMA. 2020; 323(12):1151-1160. [48] BROWN JC, HARHAY MO, HARHAY MN. Walking cadence and mortality among community-dwelling older adults. J Gen Intern Med. 2014;29(9): 1263-1269. [49] DOI T, NAKAKUBO S, TSUTSUMIMOTO K, et al. Spatiotemporal gait characteristics and risk of mortality in community-dwelling older adults. Maturitas. 2021;151:31-35. [50] DEL POZO CRUZ B, AHMADI MN, LEE IM, et al. Prospective associations of daily step counts and intensity with cancer and cardiovascular disease incidence and mortality and all-cause mortality. JAMA Intern Med. 2022; 182(11):1139-1148. [51] DEL POZO CRUZ B, AHMADI M, NAISMITH SL, et al. Association of daily step count and intensity with incident dementia in 78 430 adults living in the UK. JAMA Neurol. 2022;79(10):1059-1063. [52] CABRAL LP, FREIRE YA, BROWNE RAV, et al. Associations of steps per day and peak cadence with arterial stiffness in older adults. Exp Gerontol. 2022;157:111628. |
| [1] | Li Yongjie, Fu Shenyu, Xia Yuan, Zhang Dakuan, Liu Hongju. Correlation of knee extensor muscle strength and spatiotemporal gait parameters with peak knee flexion/adduction moment in female patients with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1354-1358. |
| [2] | Hou Zexin, Xu Benke, Dai Yuan, He Chuan, Zhang Chaoju, Li Xiaolin. Finite element analysis of the mechanism of dorsiflexion injury of wrist joint in elderly people after falls [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 886-890. |
| [3] | Zhang Zeyi, Yang Yimin, Li Wenyan, Zhang Meizhen. Effect of foot progression angle on lower extremity kinetics of knee osteoarthritis patients of different ages: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 968-975. |
| [4] | Jiang Meijiao, Zhang Junxia, Shao Yangyang, Lu Fangfang, Yin Guofu, Yang Fang. Sensitivity factor analysis of asymmetric gait quality evaluation model based on random forest algorithm [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(36): 5805-5810. |
| [5] | Dong Hongming, Li Jianping, Liu Chao, Zhang Honghao, Li Guqiang. Relationship between muscle activation characterization and fall risk in older adults during walking up and down stairs [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(34): 5419-5424. |
| [6] | Gao Yongchang, Fu Yantao, Zhao Xin, Cui Qingfeng, Zhang Zhifeng, Chen Shibin. Mechanical performance and collapse risk prediction of avascular necrosis of femoral head under walking movement [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(33): 5265-5269. |
| [7] | Lin Ying, Liao Qi, Yan Laixiu, Lai Jianhong. Risk factors of delirium after total knee arthroplasty in elderly patients and establishment of nomogram prediction model [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(33): 5340-5345. |
| [8] | Xu Yi, Deng Yubin. Exoskeleton-assisted walking rehabilitation for spinal cord injury: CiteSpace analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(33): 5403-5412. |
| [9] | He Rongzhen, Ying Lyufang, He Xingwen, Chen Chuanshun, Yin Yuesong, Zhang Kexiang, Wang Zili. Effect of ginsenoside Rg1 on muscle degeneration after massive rotator cuff injury in mice [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(32): 5136-5140. |
| [10] | Zhao Zhuoyue, Liu Jiawen, Sun Changcheng, Zhang Gaoshuai, Zhang Ying, Xu Rui. Characterization of temporal and intensity parameters of early postural adjustment phase during gait initiation in stroke patients [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(28): 4429-4435. |
| [11] | Li Zhipeng, Huan Dawei, Yuan Zhaofeng, Ding Kai, Qiu Yue, Xia Tianwei, Shen Jirong. Mid- and long-term state after total hip arthroplasty versus hemiarthroplasty for femoral neck fractures in the elderly: evaluation using propensity score matching method [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(24): 3839-3844. |
| [12] | Zhang Guohui, Tian Weifeng, Li Hua, Wang Quan, Liu Yanhui, Guan Yulong, Xiao Chunlai. A controlled trial of elastic fixation and absolute fixation for treatment of ankle fractures with lower tibiofibular instability [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(24): 3862-3866. |
| [13] | Qi Liuxin, Zhou Mian, Wang Xiangyu, Sun Wei, Wang Jiangna. Effect of support surface stability on balance in the elderly with mild cognitive impairment under different visual input conditions [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(24): 3897-3902. |
| [14] | Xu Daxing, Ji Muqiang, Tu Zesong, Xu Weipeng, Xu Weilong, Niu Wei. Constructing a risk prediction model for failure after locking plate fixation for proximal humeral fractures in the elderly by combining the deltoid tuberosity index with preoperative factors [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(21): 3299-3305. |
| [15] | Li Zhipeng, Huan Dawei, Yuan Zhaofeng, Qiu Yue, Zhang Chao, Xia Tianwei, Shen Jirong. Risk factors of postoperative mortality of femoral neck fractures in elderly patients and construction of a nomogram predictive model [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(21): 3361-3366. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||