Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (10): 1568-1574.doi: 10.12307/2024.363
Previous Articles Next Articles
Strontium ranelate-loaded sodium alginate/collagen hydrogel promotes bone defect repair in osteoarthritis
Su Kunyang, Chen Bineng, Chen Yiliang, Jin Shaofeng
- Department of Traditional Chinese Medicine Rehabilitation, 910 Hospital of Chinese People's Liberation Army Joint Logistics Support Force (Quanzhou Strait Hospital), Quanzhou 362000, Fujian Province, China
-
Received:2023-04-04Accepted:2023-05-25Online:2024-04-08Published:2023-08-19 -
Contact:Jin Shaofeng, Supervisor therapist, Department of Traditional Chinese Medicine Rehabilitation, 910 Hospital of Chinese People's Liberation Army Joint Logistics Support Force (Quanzhou Strait Hospital), Quanzhou 362000, Fujian Province, China -
About author:Su Kunyang, Supervisor therapist, Department of Traditional Chinese Medicine Rehabilitation, 910 Hospital of Chinese People's Liberation Army Joint Logistics Support Force (Quanzhou Strait Hospital), Quanzhou 362000, Fujian Province, China
CLC Number:
Cite this article
Su Kunyang, Chen Bineng, Chen Yiliang, Jin Shaofeng. Strontium ranelate-loaded sodium alginate/collagen hydrogel promotes bone defect repair in osteoarthritis[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(10): 1568-1574.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
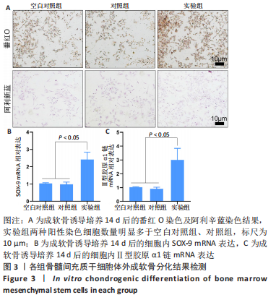
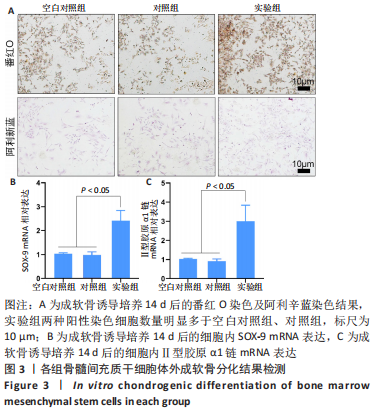
2.2.2 水凝胶对骨髓间充质干细胞体外成软骨分化的影响 番红O是一种结合多阴离子的阳离子染料,其可以与软骨基质中的多糖如硫酸软骨素、硫酸角质素等阴离子基团结合,从而使得软骨基质被染色[14]。阿利辛蓝染料可使软骨分化细胞产生的糖胺聚糖被染色,在经过核固红复染后可以使软骨分化细胞的细胞质呈现粉红色、细胞核呈现红色,从而直观地观察成软骨分化细胞的分布和含量[15-16]。 如图3A所示,番红O染色显示,相比于空白对照组及对照组,实验组阳性染色细胞数量明显增加;阿利辛蓝染色呈现了相似结果,实验组被染为红色的软骨分化细胞数量明显多于空白对照组和对照组。RT-qPCR检测显示,实验组细胞内SOX-9 mRNA的表达高于空白对照组、对照组(2.42±0.42,1.03±0.04,0.98±0.14,P < 0.05),Ⅱ型胶原α1链mRNA的表达高于空白对照组、对照组(3.01±0.84,1.02±0.04,0.91±0.11,P < 0.05),空白对照组与对照组细胞内SOX-9、Ⅱ型胶原α1链mRNA的表达比较差异均无显著性意义(P > 0.05),见图3B、C。"
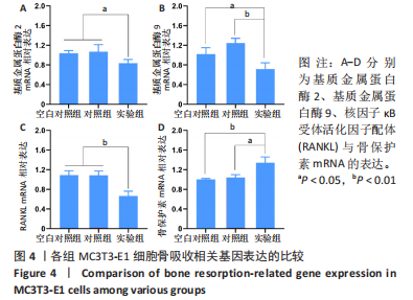
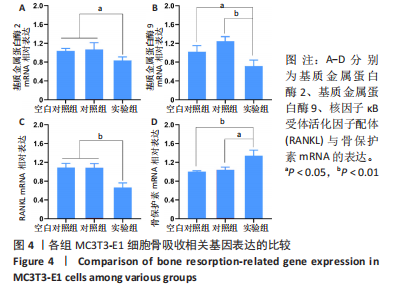
2.2.3 水凝胶对MC3T3-E1细胞骨吸收相关基因表达的影响 如图4A、B所示,实验组细胞内基质金属蛋白酶2和基质金属蛋白酶9的mRNA表达均低于空白对照组、对照组(P < 0.05或P < 0.01),空白对照组与对照组细胞内基质金属蛋白酶2和基质金属蛋白酶9的mRNA表达比较差异均无显著性意义(P > 0.05)。 如图4C、D所示,实验组细胞内RANKL的mRNA表达低于空白对照组、对照组(P < 0.01),骨保护素的mRNA表达高于空白对照组、对照组(P < 0.05或P < 0.01),空白对照组与对照组细胞内RANKL和骨保护素的mRNA表达比较差异均无显著性意义(P > 0.05)。因此这些结果表明,载雷奈酸锶海藻酸钠/胶原水凝胶可以通过增加骨保护素/RANKL比值来降低骨吸收活性。"
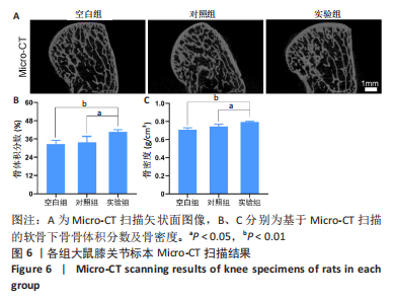
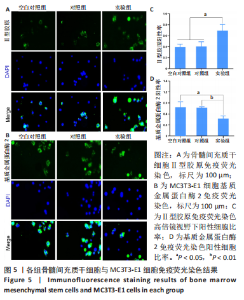
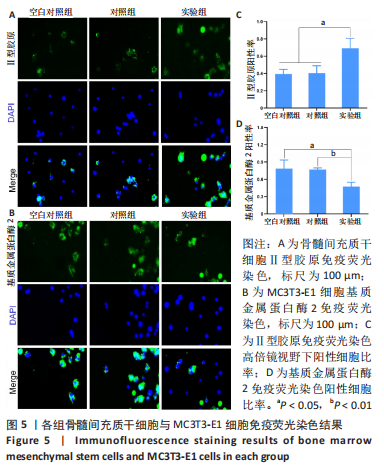
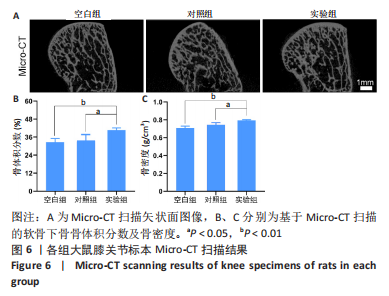
水凝胶对骨髓间充质干细胞软骨分化的影响:如图5A所示,Ⅱ型胶原呈绿色荧光,细胞核呈蓝色,实验组被染为绿色荧光的阳性细胞数量明显多于空白对照组、对照组。图5CⅡ型胶原免疫荧光染色定量分析结果显示,实验组Ⅱ型胶原阳性细胞比率(0.69±0.11)高于空白对照组(0.39±0.05)、对照组(0.40±0.08) (P < 0.05),空白对照组与对照组Ⅱ型胶原阳性细胞比率比较差异无显著性意义(P > 0.05)。 水凝胶对MC3T3-E1细胞骨吸收相关蛋白表达的影响:基质金属蛋白酶2免疫荧光染色结果显示,实验组被染为绿色荧光的阳性细胞数量明显少于空白对照组、对照组,见图5B。基质金属蛋白酶2免疫荧光染色定量分析结果显示,实验组基质金属蛋白酶2阳性细胞比率(0.47±0.07)低于空白对照组(0.78±0.15)、对照组(0.76±0.03)(P < 0.05或P < 0.01),空白对照组与对照组基质金属蛋白酶2阳性细胞比率比较差异无显著性意义(P > 0.05),见图5D。 2.3 水凝胶体内实验结果 2.3.1 实验动物数量分析 18只大鼠全部进入结果分析。 2.3.2 各组大鼠膝关节标本Micro-CT扫描 Micro-CT扫描显示,空白组和对照组大鼠膝关节软骨下骨的骨小梁结构相较于实验组显得疏松菲薄,见图6A。数据分析显示,实验组软骨下骨骨体积分数为(40.72±1.41)%,明显高于空白组的(32.56±2.56)%和对照组的(33.67±4.08)% (P < 0.05或P < 0.01),并且骨密度分析也进一步证实了实验组软骨下骨骨密度高于其他两组,空白组与对照组间骨体积分数与骨密度比较差异均无显著性意义(P > 0.05),见图6B、C。"
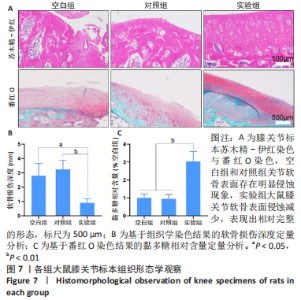
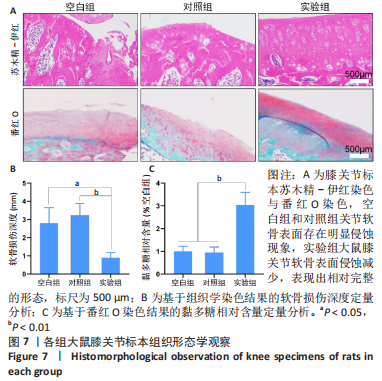
2.3.3 各组大鼠膝关节标本组织形态观察 苏木精-伊红染色和番红O染色显示,空白组和对照组大鼠膝关节软骨表面存在明显侵蚀现象,软骨面存在有裂隙和变形;实验组大鼠膝关节软骨表面侵蚀减少,表现出相对完整的形态,见图7A。组织学染色定量分析结果显示,实验组软骨侵蚀深度低于空白组、对照组[(0.91±0.28),(2.79±0.85),(3.24±0.63) mm,P < 0.05或P < 0.01],空白组与对照组间比较差异无显著性意义(P > 0.05),见图7B。番红O染色定量分析结果显示,空白组和对照组的相对黏多糖含量低于实验组(P < 0.01),空白组与对照组间比较差异无显著性意义(P > 0.05),见图7C。"

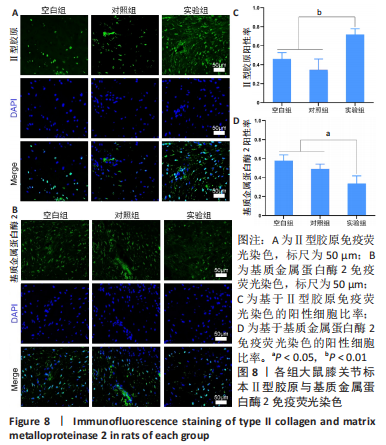
2.3.4 各组大鼠膝关节标本Ⅱ型胶原与基质金属蛋白酶2免疫荧光染色 如图8A、B所示,Ⅱ型胶原和基质金属蛋白酶2蛋白呈绿色荧光,细胞核呈蓝色荧光,与空白组和对照组相比,实验组大鼠膝关节标本Ⅱ型胶原阳性细胞数量增加、基质金属蛋白酶2阳性细胞数减少。免疫荧光染色定量分析结果显示,实验组Ⅱ型胶原阳性细胞比率高于空白组、对照组(0.71±0.06,0.46±0.06,0.35±0.12,P < 0.01),空白组与对照组比较差异无显著性意义(P > 0.05),见图8C;实验组基质金属蛋白酶2阳性细胞比率低于空白组、对照组(0.34±0.08,0.57±0.06,0.49±0.05,P < 0.05),空白组与对照组比较差异无显著性意义(P > 0.05),见图8D。"
| [1] BRANDT KD, DIEPPE P, RADIN E. Etiopathogenesis of Osteoarthritis. Med Clin North Am. 2009; 93(1):1-24. [2] MASSICOTTE F, LAJEUNESSE D, BENDERDOUR M, et al. Can altered production of interleukin-1beta, interleukin-6, transforming growth factor-beta and prostaglandin E(2) by isolated human subchondral osteoblasts identify two subgroups of osteoarthritic patients. Osteoarthritis Cartilage. 2002;10(6):491-500. [3] TELLEGEN AR, RUDNIK-JANSEN I, POURAN B, et al. Controlled release of celecoxib inhibits inflammation, bone cysts and osteophyte formation in a preclinical model of osteoarthritis. Drug Deliv. 2018;25(1):1438-1447. [4] DENG C, ZHU H, LI J, et al. Bioactive Scaffolds for Regeneration of Cartilage and Subchondral Bone Interface. Theranostics. 2018;8(7):1940-1955. [5] ZHAO CF, LI ZH, LI SJ, et al. PLGA scaffold carrying icariin to inhibit the progression of osteoarthritis in rabbits. R Soc Open Sci. 2019;6(4):181877. [6] YANG J, ZHU Y, WANG F, et al. Microfluidic liposomes-anchored microgels as extended delivery platform for treatment of osteoarthritis. Chem Eng J. 2020;400. doi.org/10.1016/j.cej.2020.126004. [7] PELLETIER JP, KAPOOR M, FAHMI H, et al. Strontium ranelate reduces the progression of experimental dog osteoarthritis by inhibiting the expression of key proteases in cartilage and of IL-1β in the synovium. Ann Rheum Dis. 2013;72(2):250-257. [8] TAT SK, PELLETIER JP, MINEAU F, et al. Strontium ranelate inhibits key factors affecting bone remodeling in human osteoarthritic subchondral bone osteoblasts. Bone. 2011;49(3):559-567. [9] WAN L, ZHANG X, WU D, et al. Application of Robot Positioning for Cannulated Screw Internal Fixation in the Treatment of Femoral Neck Fracture: Retrospective Study. JMIR Med Inform. 2021;9(1):e24164. [10] REGINSTER JY, SEEMAN E, DE VERNEJOUL MC, et al. Strontium ranelate reduces the risk of nonvertebral fractures in postmenopausal women with osteoporosis: Treatment of Peripheral Osteoporosis (TROPOS) study. J Clin Endocrinol Metab. 2005;90(5):2816-2822. [11] MEUNIER PJ, ROUX C, SEEMAN E, et al. The effects of strontium ranelate on the risk of vertebral fracture in women with postmenopausal osteoporosis. N Engl J Med. 2004;350(5):459-468. [12] HERNÁNDEZ-GONZÁLEZ AC, TÉLLEZ-JURADO L, RODRÍGUEZ-LORENZO LM. Alginate hydrogels for bone tissue engineering, from injectables to bioprinting: A review. Carbohydr Polym. 2020;229:115514. [13] MA S, ZHOU J, HUANG T, et al. Sodium alginate/collagen/stromal cell-derived factor-1 neural scaffold loaded with BMSCs promotes neurological function recovery after traumatic brain injury. Acta Biomater. 2021;131:185-197. [14] YANG YF, ZHANG JY, QIAN YX, et al. Superparamagnetic Iron Oxide is Suitable to Label Tendon Stem Cells and Track Them In Vivo with MR Imaging. Ann Biomed Eng. 2013;41(10):2109-2119. [15] IRANI S, HONARPARDAZ A, CHOUBINI N, et al. Chondro-inductive nanofibrous scaffold based gelatin/polyvinyl alcohol/chondroitin sulfate for cartilage tissue engineering. Polym Adv Technol. 2020;31(6):1395-1402. [16] HEINEMANN C, HEINEMANN S, BERNHARDT A, et al. Novel textile chitosan scaffolds promote spreading, proliferation, and differentiation of osteoblasts. Biomacromolecules. 2008;9(10):2913-2920. [17] GAO H, PAN Q, DONG W, et al. Progress in Osteochondral Regeneration with Engineering Strategies. Ann Biomed Eng. 2022;50(10):1232-1242. [18] WU J, PAN Y, YU Y, et al. Axial Compressive Loading Attenuates Early Osteoarthritis by Reducing Subchondral Bone Remodeling.Am J Sports Med. 2023;3635465231164644. doi: 10.1177/03635465231164644. [19] SU W, LIU G, LIU X, et al. Angiogenesis stimulated by elevated PDGF-BB in subchondral bone contributes to osteoarthritis development. JCI Insight. 2020;5(8):e135446. [20] CHEN Y, XU W, SHAFIQ M, et al. Injectable nanofiber microspheres modified with metal phenolic networks for effective osteoarthritis treatment. Acta Biomater. 2023;157:593-608. [21] LIAO B, DING M, WANG Y, et al. Strontium ion attenuates osteoarthritis through inhibiting senescence and enhancing autophagy in fibroblast-like synoviocytes. Mol Biol Rep. 2023; 50(2):1437-1446. [22] DING G, HE Y, SHI Y, et al. Sustained-Drug-Release, Strong, and Anti-Swelling Water-Lipid Biphasic Hydrogels Prepared via Digital Light Processing 3D Printing for Protection against Osteoarthritis: Demonstration in a Porcine Model. Adv Healthc Mater. 2023;e2203236. doi: 10.1002/adhm.202203236. [23] WANG H, LIN C, ZHANG X, et al. Mussel-Inspired Polydopamine Coating: A General Strategy To Enhance Osteogenic Differentiation and Osseointegration for Diverse Implants. ACS Appl Mater Interfaces. 2019;11(7):7615-7625. [24] FIGUEROA-PIZANO MD, VELAZ I, PENAS FJ, et al. Effect of freeze-thawing conditions for preparation of chitosan-poly (vinyl alcohol) hydrogels and drug release studies. Carbohydr Polym. 2018;195:476-485. [25] GU Z, WANG J, FU Y, et al. Smart Biomaterials for Articular Cartilage Repair and Regeneration. Adv Funct Mater. 2023;10(33):2212561. [26] 陈臻浩,赵广雷,石晶晟,等.Sox9对软骨细胞分化和基质产生的调控机制[J].复旦学报(医学版), 2019,46(6):824-828. [27] TENG B, ZHANG H, ZENG Z, et al. Application of functionalized hyaluronic acid hydrogel with the activity of regulating the behaviors of stem cells in repairing rabbit knee articular cartilage. J Biomater Appl. 2023;37(9):1617-1625. [28] YU H, LIU Y, YANG X, et al. The anti-inflammation effect of strontium ranelate on rat chondrocytes with or without IL-1 beta in vitro. Exp Ther Med. 2022; 23(3).doi:10.3892/etm.2022.11131. [29] YU DG, DING HF, MAO YQ, et al. Strontium ranelate reduces cartilage degeneration and subchondral bone remodeling in rat osteoarthritis model. Acta Pharmacol Sin. 2013;34(3):393-402. [30] HU Y, Chen X, Wang S, et al. Subchondral bone microenvironment in osteoarthritis and pain. Bone Res. 2021;9(1):20. [31] KWAN TAT S, LAJEUNESSE D, PELLETIER JP, et al. Targeting subchondral bone for treating osteoarthritis: what is the evidence? Best Pract Res Clin Rheumatol. 2010;24(1):51-70. [32] BETTICA P, CLINE G, HART DJ, et al. Evidence for increased bone resorption in patients with progressive knee osteoarthritis: longitudinal results from the Chingford study. Arthritis Rheum. 2002;46(12):3178-3184. [33] LI X, JIN L, TAN Y. Different roles of matrix metalloproteinase 2 in osteolysis of skeletal dysplasia and bone metastasis (Review). Mol Med Rep. 2021;23(1):70. [34] MARÍN-RAMOS NI, THEIN TZ, GHAGHADA KB, et al. miR-18a Inhibits BMP4 and HIF-1α Normalizing Brain Arteriovenous Malformations. Circ Res. 2020;127(9):e210-e231. [35] KOVÁCS B, VAJDA E, NAGY EE. Regulatory Effects and Interactions of the Wnt and OPG-RANKL-RANK Signaling at the Bone-Cartilage Interface in Osteoarthritis. Int J Mol Sci. 2019; 20(18):4653. [36] CHEN J, LAN Y, HE Y, et al. 99Tc-MDP-induced human osteoblast proliferation, differentiation and expression of osteoprotegerin. Mol Med Rep. 2017;16(2):1801-1809. [37] XU F, DONG Y, HUANG X, et al. Pioglitazone affects the OPG/RANKL/RANK system and increase osteoclastogenesis. Mol Med Rep. 2016;14(3):2289-2296. |
| [1] | Li Yongjie, Fu Shenyu, Xia Yuan, Zhang Dakuan, Liu Hongju. Correlation of knee extensor muscle strength and spatiotemporal gait parameters with peak knee flexion/adduction moment in female patients with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1354-1358. |
| [2] | Qi Haodong, Lu Chao, Xu Hanbo, Wang Mengfei, Hao Yangquan. Effect of diabetes mellitus on perioperative blood loss and pain after primary total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1383-1387. |
| [3] | Du Changling, Shi Hui, Zhang Shoutao, Meng Tao, Liu Dong, Li Jian, Cao Heng, Xu Chuang. Efficacy and safety of different applications of tranexamic acid in high tibial osteotomy [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1409-1413. |
| [4] | Huang Xiarong, Hu Lizhi, Sun Guanghua, Peng Xinke, Liao Ying, Liao Yuan, Liu Jing, Yin Linwei, Zhong Peirui, Peng Ting, Zhou Jun, Qu Mengjian. Effect of electroacupuncture on the expression of P53 and P21 in articular cartilage and subchondral bone of aged rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1174-1179. |
| [5] | Zhao Garida, Ren Yizhong, Han Changxu, Kong Lingyue, Jia Yanbo. Mechanism of Mongolian Medicine Erden-uril on osteoarthritis in rats [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1193-1199. |
| [6] | Li Rui, Zhang Guihong, Wang Tao, Fan Ping. Effect of ginseng polysaccharide on the expression of prostaglandin E2/6-keto-prostaglandin 1alpha in traumatic osteoarthritis model rats [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1235-1240. |
| [7] | Liu Hanfeng, Wang Jingjing, Yu Yunsheng. Artificial exosomes in treatment of myocardial infarction: current status and prospects [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1118-1123. |
| [8] | Zhang Kefan, Shi Hui. Research status and application prospect of cytokine therapy for osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 961-967. |
| [9] | Zhang Zeyi, Yang Yimin, Li Wenyan, Zhang Meizhen. Effect of foot progression angle on lower extremity kinetics of knee osteoarthritis patients of different ages: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 968-975. |
| [10] | Tian Xin, Liu Tao, Yang Huilin, He Fan. In vitro evaluation of sustained release Kartogenin by gelatin methacryloyl microspheres for repairing nucleus pulposus degeneration [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 724-730. |
| [11] | Yin Tong, Yang Jilei, Li Yourui, Liu Zhuoran, Jiang Ming. Application of core-shell structured nanofibers in oral tissue regeneration [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 766-770. |
| [12] | Shen Feiyan, Yao Jixiang, Su Shanshan, Zhao Zhongmin, Tang Weidong. Knockdown of circRNA WD repeat containing protein 1 inhibits proliferation and induces apoptosis of chondrocytes in knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 499-504. |
| [13] | Maisituremu·Heilili, Zhang Wanxia, Nijiati·Nuermuhanmode, Maimaitituxun·Tuerdi. Effect of intraarticular injection of different concentrations of ozone on condylar histology of rats with early temporomandibular joint osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 505-509. |
| [14] | Qiao Hujun, Wang Guoxiang. Evaluation of rat osteoarthritis chondrocyte models induced by interleukin-1beta [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 516-521. |
| [15] | Liu Yuhan, Fan Yujiang, Wang Qiguang. Comparison of protocols for constructing animal models of early traumatic knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 542-549. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||