Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (33): 5334-5341.doi: 10.12307/2023.762
Previous Articles Next Articles
Rougan Jiangmei Formula medicated serum inhibits activation and autophagy of human hepatic stellate cells
Tao Bonan1, Wang Yonglan1, Jiang Lu1, Zhang Zongxing1, Liu Daozhong1, Wan Xing2, Huang Debin1, Yuan Lin1
- 1Hubei Provincial Key Laboratory of Occurrence and Intervention of Rheumatic Diseases, Hubei Minzu University, Enshi 445000, Hubei Province, China; 2West China School of Preclinical Medicine and Forensic Medicine, Sichuan University, Chengdu 610064, Sichuan Province, China
-
Received:2022-09-20Accepted:2022-11-14Online:2023-11-28Published:2023-03-30 -
Contact:Yuan Lin, Associate professor, Hubei Provincial Key Laboratory of Occurrence and Intervention of Rheumatic Diseases, Hubei Minzu University, Enshi 445000, Hubei Province, China -
About author:Tao Bonan, Master candidate, Hubei Provincial Key Laboratory of Occurrence and Intervention of Rheumatic Diseases, Hubei Minzu University, Enshi 445000, Hubei Province, China -
Supported by:the National Natural Science Foundation of China, No. 82060745 (to HDB); General Project of Hubei Provincial Health Commission, No. ZY2019M076 (to YL); Science and Technology Planning Project of Enshi Prefecture Science and Technology Bureau, No. E20190001 (to YL)
CLC Number:
Cite this article
Tao Bonan, Wang Yonglan, Jiang Lu, Zhang Zongxing, Liu Daozhong, Wan Xing, Huang Debin, Yuan Lin. Rougan Jiangmei Formula medicated serum inhibits activation and autophagy of human hepatic stellate cells[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(33): 5334-5341.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
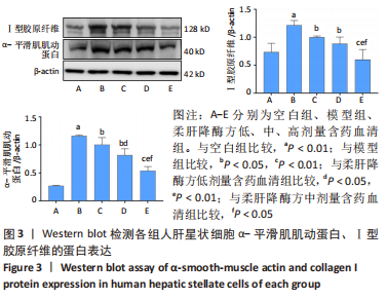
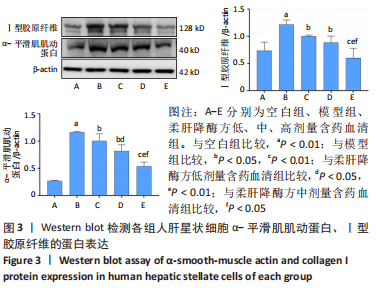
2.4 柔肝降酶方含药血清对脂多糖诱导的人肝星状细胞Ⅰ型胶原纤维、α-平滑肌肌动蛋白的蛋白表达水平的影响 Ⅰ型胶原纤维、α-平滑肌肌动蛋白是肝星状细胞活化的标志。人肝星状细胞激活是肝脏细胞外基质沉积的来源,肝星状细胞活化转化为肌成纤维细胞,表达Ⅰ型胶原纤维、α-平滑肌肌动蛋白等细胞外基质成分。与空白组相比,模型组Ⅰ型胶原纤维、α-平滑肌肌动蛋白的蛋白表达均显著升高(P < 0.01);与模型组相比,柔肝降酶方低、中、高剂量含药血清组的Ⅰ型胶原纤维、α-平滑肌肌动蛋白的蛋白表达均显著降低(P < 0.05,P < 0.01),呈剂量依赖性。与柔肝降酶方低剂量含药血清组相比,柔肝降酶方高剂量含药血清组Ⅰ型胶原纤维蛋白表达显著降低(P < 0.05),柔肝降酶方中、高剂量含药血清组α-平滑肌肌动蛋白的蛋白表达均显著降低(P < 0.05,P < 0.01);与柔肝降酶方中剂量含药血清组相比,柔肝降酶方高剂量含药血清组Ⅰ型胶原纤维、α-平滑肌肌动蛋白表达均显著降低(P < 0.05)。以上结果提示,柔肝降酶方含药血清对人肝星状细胞活化具有抑制作用,见图3。"
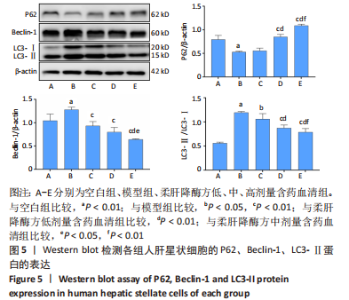
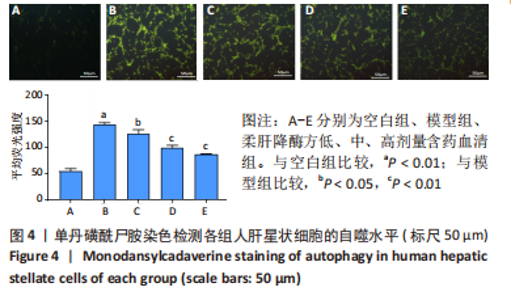
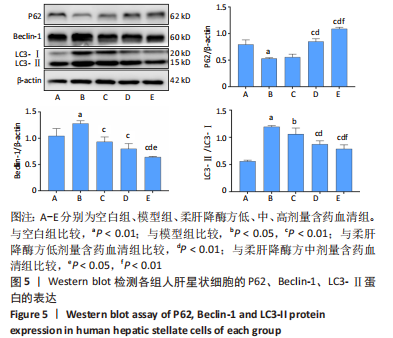
2.5.2 柔肝降酶方含药血清对人肝星状细胞自噬相关蛋白表达水平的影响 Western blot检测结果显示,与空白组相比,模型组P62蛋白表达水平显著降低(P < 0.01);与模型组相比,柔肝降酶方低剂量含药血清组P62蛋白表达水平与模型组无显著差异,柔肝降酶方中、高剂量含药血清组的P62蛋白表达水平显著升高(P < 0.01)。与空白组相比,模型组Beclin-1、LC3-Ⅱ蛋白表达水平显著升高(P < 0.01);与模型组相比,柔肝降酶方低、中、高剂量含药血清组的Beclin-1、LC3-Ⅱ蛋白表达水平显著降低(P < 0.05,P < 0.01),呈剂量依赖性。与柔肝降酶方低剂量含药血清组相比,柔肝降酶方中、高剂量含药血清组P62蛋白表达均显著升高(P < 0.01),LC3-Ⅱ蛋白表达均显著降低(P < 0.05,P < 0.01),柔肝降酶方高剂量含药血清组Beclin-1蛋白表达显著降低(P < 0.01);与柔肝降酶方中剂量含药血清组相比,柔肝降酶方高剂量含药血清组P62蛋白表达显著升高(P < 0.01),Beclin-1、LC3-Ⅱ蛋白表达水平均显著降低(P < 0.05,P < 0.01)。见图5。"
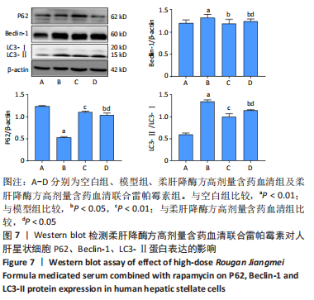
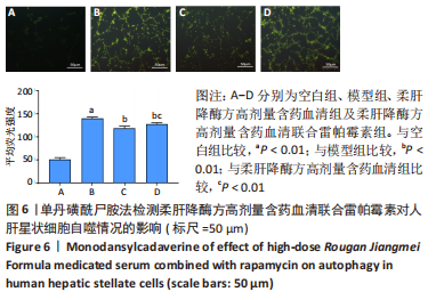
2.6.2 柔肝降酶方含药血清联合雷帕霉素对人肝星状细胞自噬相关蛋白表达的影响 Western blot检测结果显示,与空白组相比,模型组P62蛋白表达水平显著降低(P < 0.01),Beclin-1、LC3-Ⅱ蛋白表达水平显著升高(P < 0.01);与模型组相比,柔肝降酶方高剂量含药血清组、柔肝降酶方高剂量含药血清联合雷帕霉素组的P62蛋白表达水平均显著升高(P < 0.05,P < 0.01),Beclin-1、LC3-Ⅱ蛋白表达水平均显著降低(P < 0.05,P < 0.01);与柔肝降酶方高剂量含药血清组相比,柔肝降酶方高剂量含药血清联合雷帕霉素组的P62蛋白表达水平显著降低(P < 0.05),Beclin-1、LC3-Ⅱ蛋白表达水平均显著升高(P < 0.05),见图7。"

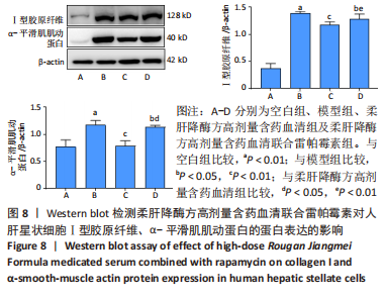
2.6.3 柔肝降酶方含药血清联合雷帕霉素对人肝星状细胞活化标志蛋白表达的影响 Western blot检测结果显示,与空白组相比,模型组Ⅰ型胶原纤维、α-平滑肌肌动蛋白的蛋白表达均显著升高(P < 0.01);与模型组相比,柔肝降酶方高剂量含药血清组、柔肝降酶方联合雷帕霉素组的Ⅰ型胶原纤维、α-平滑肌肌动蛋白的蛋白表达均显著降低(P < 0.05,P < 0.01)。与柔肝降酶方高剂量含药血清组相比,柔肝降酶方高剂量含药血清联合雷帕霉素组α-平滑肌肌动蛋白、Ⅰ型胶原纤维蛋白表达显著升高(P < 0.05,P < 0.01),见图8。以上结果提示,柔肝降酶方含药血清能够抑制自噬来减少肝星状细胞的活化。"

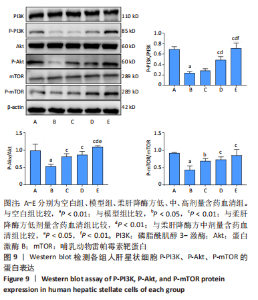
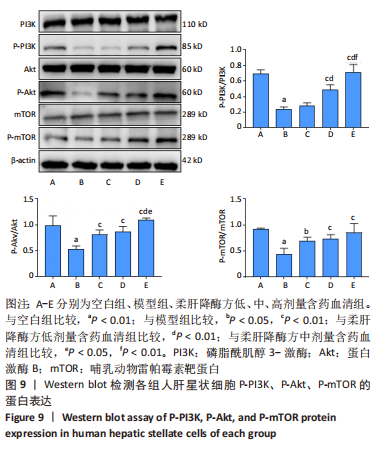
2.7 柔肝降酶方含药血清对脂多糖诱导的人肝星状细胞PI3K/Akt/mTOR信号通路的影响 2.7.1 柔肝降酶方含药血清对人肝星状细胞PI3K/Akt/mTOR信号通路的影响 Western blot检测结果显示,与空白组相比,模型组P-PI3K、P-Akt、P-mTOR蛋白表达水平显著降低(P < 0.01);与模型组相比,柔肝降酶方低、中、高剂量含药血清组的P-PI3K、P-Akt、P-mTOR蛋白表达水平均显著升高(P < 0.05,P < 0.01),呈剂量依赖性。与柔肝降酶方低剂量含药血清组相比,中、高剂量含药血清组P-PI3K蛋白表达显著升高(P < 0.01),柔肝降酶方高剂量含药血清组P-Akt蛋白表达显著升高(P < 0.05);与柔肝降酶方中剂量含药血清组相比,柔肝降酶方高剂量含药血清组P-PI3K、P-Akt蛋白表达均显著升高(P < 0.01,P < 0.05)。见图9。"
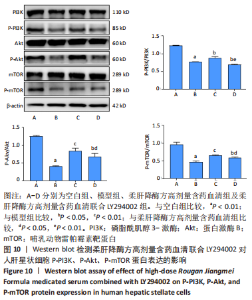
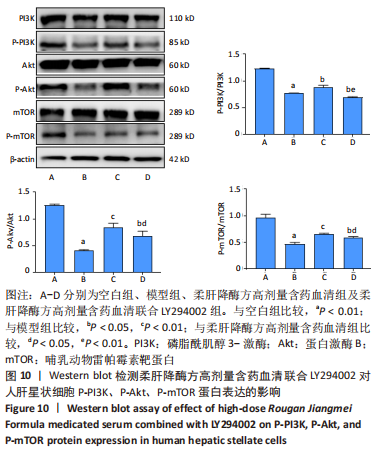
2.7.2 柔肝降酶方含药血清联合LY294002对人肝星状细胞PI3K/Akt/mTOR信号通路的影响 Western blot检测结果显示,与空白组相比,模型组P-PI3K、P-Akt、P-mTOR蛋白表达水平显著降低(P < 0.01);与模型组相比,柔肝降酶方高剂量含药血清组、柔肝降酶方高剂量含药血清联合LY294002组的P-Akt、P-mTOR蛋白表达水平显著升高(P < 0.05,P < 0.01);与柔肝降酶方高剂量含药血清组相比,柔肝降酶方高剂量含药血清联合LY294002组的p-PI3K、p-Akt、p-mTOR蛋白表达水平显著降低(P < 0.05,P < 0.01),见图10。以上结果表明,柔肝降酶方含药血清抑制人肝星状细胞自噬与活化,与PI3K/Akt/mTOR信号通路有关。"
| [1] TRAUTWEIN C, FRIEDMAN SL, SCHUPPAN D, et al. Hepatic fibrosis: Concept to treatment. J Hepatol. 2015;62(1 Suppl):S15-S24. [2] 池晓玲, 萧焕明. 病毒性肝炎防治新形势下对中医药防治肝纤维化的思考[J]. 临床肝胆病杂志,2018,34(4):694-697. [3] VERMA AK, SHARMA A, SUBRAMANIYAM N, et al. Augmenter of liver regeneration: Mitochondrial function and steatohepatitis. J Hepatol. 2022;77(5):1410-1421. [4] KRIZHANOVSKY V, YON M, DICKINS RA, et al. Senescence of activated stellate cells limits liver fibrosis. Cell. 2008;134(4):657-667. [5] LEI L, BRUNEAU A, EL MOURABIT H, et al. Portal fibroblasts with mesenchymal stem cell features form a reservoir of proliferative myofibroblasts in liver fibrosis. Hepatology. 2022;76(5):1360-1375. [6] VARGAS JNS, HAMASAKI M, KAWABATA T, et al. The mechanisms and roles of selective autophagy in mammals. Nat Rev Mol Cell Biol. 2022;1038(10):s41580-022-00542-2. [7] CHEN S, HE Z, XIE W, et al. Ginsenoside Rh2 attenuates CDAHFD-induced liver fibrosis in mice by improving intestinal microbial composition and regulating LPS-mediated autophagy. Phytomedicine. 2022;101(7):154121. [8] HOU LS, ZHANG YW, LI H, et al. The regulatory role and mechanism of autophagy in energy metabolism-related hepatic fibrosis. Pharmacol Ther. 2022;234(6):108117. [9] FUKUDA T, WADA-HIRAIKE O. The Two-Faced Role of Autophagy in Endometrial Cancer. Front Cell Dev Biol. 2022;31(10):839416. [10] WU L, ZHANG Q, MO W, et al. Quercetin prevents hepatic fibrosis by inhibiting hepatic stellate cell activation and reducing autophagy via the TGF-β1/Smads and PI3K/Akt pathways. Sci Rep. 2017;7(1):9289. [11] 张倩璐, 旷昕. 丙泊酚对转化生长因子-β1诱导肝星状细胞激活的影响及其机制[J]. 中国应用生理学杂志,2020,36(3):273-278. [12] 陈普艳, 姜锦林, 杨强. 柔肝降酶合剂对大鼠四氯化碳诱导肝损害的防治作用[J]. 世界科学技术-中医药现代化,2014,16(4):811-816. [13] 张千娥, 谢洪武, 刘福水. 柔肝降酶合剂治疗慢性乙型肝炎40例临床观察[J]. 中医杂志,2014,55(22):1929-1932. [14] 范丽丽, 陈雄, 邹忠兰, 等. 亚砷酸钠对人肝星状细胞活化及细胞外基质分泌的影响[J].中华预防医学杂志,2018,52(10):983-987. [15] 吴朕, 马微, 臧成昊, 等. 三七皂苷R1保护四氯化碳诱导肝纤维化模型大鼠的作用[J].中国组织工程研究,2020,24(26):4213-4217. [16] ZHANG D, ZHANG Y, SUN B. The Molecular Mechanisms of Liver Fibrosis and Its Potential Therapy in Application. Int J Mol Sci. 2022;23(20): 12572. [17] SCHUPPAN D, SURABATTULA R, WANG XY. Determinants of fibrosis progression and regression in NASH. J Hepatol. 2018;68(2):238-250. [18] FRIEDMAN SL, PINZANI M. Hepatic fibrosis 2022: Unmet needs and a blueprint for the future. Hepatology. 2022;75(2):473-488. [19] 徐列明, 刘平, 沈锡中, 等. 肝纤维化中西医结合诊疗指南(2019年版)[J]. 中国中西医结合杂志,2019,39(11):1286-1295. [20] SKRZYPCZAK-WIERCIOCH A, SAŁAT K. Lipopolysaccharide-Induced Model of Neuroinflammation: Mechanisms of Action, Research Application and Future Directions for Its Use. Molecules. 2022;27(17): 5481. [21] WANG T, LU Z, QU XH, et al. Chrysophanol-8-O-glucoside protects mice against acute liver injury by inhibiting autophagy in hepatic stellate cells and inflammatory response in liver-resident macrophages. Front Pharmacol. 2022;13:951521. [22] CHEN M, LIU J, YANG W, et al. Lipopolysaccharide mediates hepatic stellate cell activation by regulating autophagy and retinoic acid signaling. Autophagy. 2017;13(11):1813-1827. [23] LI J, DENG X, WANG S, et al. Resolvin D1 attenuates CCl4 Induced Liver Fibrosis by Inhibiting Autophagy-Mediated HSC activation via PI3K/Akt/mTOR Pathway. Front Pharmacol. 2021;12:792414. [24] 李佳行, 杨胜乾, 刘娟娟, 等. 连翘苷对脂多糖诱导肝脏星状细胞活化的抑制作用[J]. 第三军医大学学报,2020,42(4):342-349. [25] 杨如会, 刘丙进, 吴松泉. 淫羊藿苷通过FXR降低LPS/TLR4诱导的肝星状细胞自噬和活化[J]. 中国药学杂志,2016,51(9):708-714. [26] 刘云洁, 程玮, 李丽, 等. IRF3抑制LPS诱导肝星状细胞LX-2的炎症因子的分泌[J]. 安徽医科大学学报,2019,54(2):178-182. [27] RAVIKUMAR B, SARKAR S, DAVIES JE, et al. Regulation of mammalian autophagy in physiology and pathophysiology. Physiol Rev. 2010;90(4): 1383-1435. [28] RONG Z, ZHENG K, CHEN J, et al. Function and regulation of ULK1: From physiology to pathology. Gene. 2022;840:146772. [29] KTISTAKIS NT, TOOZE SA. Digesting the Expanding Mechanisms of Autophagy. Trends Cell Biol. 2016;26(8):624-635. [30] SHI Q, JIN X, ZHANG P, et al. SPOP mutations promote P62/SQSTM1-dependent autophagy and Nrf2 activation in prostate cancer. Cell Death Differ. 2022;29(6):1228-1239. [31] CHENG D, CHAI J, WANG H, et al. Hepatic macrophages: Key players in the development and progression of liver fibrosis. Liver Int. 2021; 41(10):2279-2294. [32] 安祯祥, 何远利, 唐东昕, 等. 扶脾柔肝颗粒对肝纤维化模型大鼠的改善作用机制研究[J]. 中国药房,2021,32(21):2587-2592. [33] MOHANASUNDARAM P, COELHO-RATO LS, MODI MK, et al. Cytoskeletal vimentin regulates cell size and autophagy through mTORC1 signaling. PLoS Biol. 2022;20(9):e3001737. [34] YOSHIDA S, PACITTO R, INOKI K, et al. Macropinocytosis, mTORC1 and cellular growth control. Cell Mol Life Sci. 2018;75(7):1227-1239. [35] WANG R, SONG F, LI S, et al. Salvianolic acid A attenuates CCl4-induced liver fibrosis by regulating the PI3K/PI3K/Akt/mTOR, Bcl-2/Bax and caspase-3/cleaved caspase-3 signaling pathways. Drug Des Devel Ther. 2019;13:1889-1900. [36] WANG H, LIU Y, WANG D, et al. The Upstream Pathway of mTOR-Mediated Autophagy in Liver Diseases. Cells. 2019;8(12):1597. [37] XIU A Y, DING Q, LI Z, et al. Doxazosin Attenuates Liver Fibrosis by Inhibiting Autophagy in Hepatic Stellate Cells via Activation of the PI3K/Akt/mTOR Signaling Pathway. Drug Des Devel Ther. 2021;15:3643-3659. [38] LEI Y, WANG Q, SHEN L, et al. MicroRNA-101 suppresses liver fibrosis by downregulating PI3K/Akt/mTOR signaling pathway. Clin Res Hepatol Gastroenterol. 2019;43(5):575-584. [39] JI D, ZHAO Q, QIN Y, et al. Germacrone improves liver fibrosis by regulating the PI3K/AKT/mTOR signalling pathway. Cell Biol Int. 2021; 45(9):1866-1875. |
| [1] | Jiang Shengyuan, Zhang Yaqi, Bi Jingxin, Zhang Chengfei, Zhang Qiue, Mu Xiaohong, Bai Huizhong, Zuo Xinwei, Liu Tonghua, Qin Lingling. Tangbikang reduces sciatic nerve oxidative stress injury in a rat model of diabetic peripheral neuropathy [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(32): 5162-5167. |
| [2] | Shi Guirong, Ren Bowen, Zhang Zhongbo, Wang Lisha, Zhang Qiwei, Shi Dongliang. Effect of Illicium henryi extract on angiogenesis in rats with osteoporotic fractures [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(31): 5028-5034. |
| [3] | Wei Qin, Amanguli·Ruze, Chen Bingxin, Zhao Ling, Zhao Banghao, Jiang Tao, Zhang Chun, Li Zhiqiang, Gao Xiaoming, Duan Mingjun. Relaxin protects myocardial microvascular endothelial cells from hypoxia-reoxygenation injury [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(28): 4519-4524. |
| [4] | Zhang Dongdong, Gu Qingyun, You Qingxin, Jin Yingxin, Zhang Jiani, Wang Haoran, Wang Fengyue, Chen Shuyue, Su Jialu, Liang Yanfeng. Effects of hydrogen sulfide in paraventricular nuclei on PI3K/Akt pathway and blood pressure in high salt-induced hypertensive rats [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(26): 4168-4174. |
| [5] | Zhang Wenjie, Zhang Yong, Shi Ming, Tang Guangjun, Shi Pengzhi, Wang Junwu, Hu Man, Wang Pingchuan, Zhang Liang. Icariin regulates apoptosis of nucleus pulposus-derived mesenchymal stem cells to repair intervertebral disc degeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(24): 3803-3809. |
| [6] | Zhong Jinglin, Cao Huimin, Pan Yaru, Jian Wenxuan, Wang Qi. Ginsenoside Rg3 protects PC12 cells against oxygen-glucose deprivation/reoxygenation-induced damage [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 177-183. |
| [7] | Ma Hongfeng, Ren Qing, Cheng Wanmin, Wang Jiguo, Meng Qingyan. Effects of Sanhuang gel on wound healing, basic fibroblast growth factor and interleukin 17 levels of auricular skin defect in rabbits [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(12): 1842-1847. |
| [8] | Zhao Jufen, Ma Rong, Cao Jia, Yu Chuanyang, Tao Xiang, Wang Jia, Wang Libin. Regulation of peroxisome proliferator-activated receptor gamma coactivator 1 beta on stemness expression in breast cancer stem cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(1): 59-65. |
| [9] | Li Weiming, Xu Qingwen, Li Yijun, Sun Yanbo, Cui Jin, Xu Pengyuan . Deep seawater promotes wound healing in diabetic mice by activating PI3K/Akt pathway [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 724-729. |
| [10] | Wu Yongli, Liu Di, Wang Duo, Liu Junwei, Ma Yuyuan. Effect of warm acupuncture on PI3K/Akt signaling pathway in articular cartilage of a rabbit knee osteoarthritis model [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(35): 5596-5601. |
| [11] | Li Zulong, Rong Zhen, Sun Hua, Jiang Ruiyuan, Zhong Xiaoting, Mo Chunmei. Mechanism underlying the effect of Fuhebeihua Recipe on the proliferation of CD133+HepG2 hepatoma stem cells and related autophagy proteins [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(31): 4988-4995. |
| [12] | Lin Bo, Chen Xinyu, Jin Qiu, Zhu Zhiman, Zhao Wenhui. Effects of miR-126-3p from adipose-derived mesenchymal stem cell released exosomes on human umbilical vein endothelial cell glucolipotoxicity [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(30): 4773-4779. |
| [13] | Mi Jianguo, Qiao Rongqin, Liu Shaojin. Bushen Jianpi Huoxue Recipe improves bone metabolism, oxidative stress, and autophagy in osteoporotic rats [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(26): 4147-4152. |
| [14] | Liu Qiqi, Liu Min, Yang Jian, Yu Ke. Lipopolysaccharide stimulates the expression of interleukin-6 and nuclear factor kappa B receptor activator ligand in mouse MLO-Y4 osteoblasts [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(20): 3121-3126. |
| [15] | Wang Wei, Tang Xiangyu, Yi Zhiqian, Liu Zhaoxu. Mechanism of osteoarthritis induced chondrocyte apoptosis and extracellular matrix degradation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(20): 3133-3140. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||