Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (2): 252-257.doi: 10.12307/2022.932
Previous Articles Next Articles
Effects of extracorporeal shock wave on the proliferation and autophagy of chondrocytes from osteoarthritis rats
Wang Huanhuan1, Wang Qing2, Tang Peng3, Zhang Rui3, Min Hongwei1, 3
- 1China Rehabilitation Research Center, School of Rehabilitation, Capital Medical University, Beijing 100068, China; 2Chinese Institute of Rehabilitation Science, Beijing 100068, China; 3Joint Disease Treatment Center, Beijing Bo’ai Hospital, China Rehabilitation Research Center, Beijing 100068, China
-
Received:2021-11-22Accepted:2021-12-22Online:2023-01-18Published:2022-06-18 -
Contact:Min Hongwei, MD, Chief physician, Professor, China Rehabilitation Research Center, School of Rehabilitation, Capital Medical University, Beijing 100068, China; Joint Disease Treatment Center, Beijing Bo’ai Hospital, China Rehabilitation Research Center, Beijing 100068, China -
About author:Wang Huanhuan, Master candidate, China Rehabilitation Research Center, School of Rehabilitation, Capital Medical University, Beijing 100068, China -
Supported by:Fundamental Research Funds for Central Public Welfare Research Institutes, No. 2019CZ-12 (to WQ)
CLC Number:
Cite this article
Wang Huanhuan, Wang Qing, Tang Peng, Zhang Rui, Min Hongwei. Effects of extracorporeal shock wave on the proliferation and autophagy of chondrocytes from osteoarthritis rats[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 252-257.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
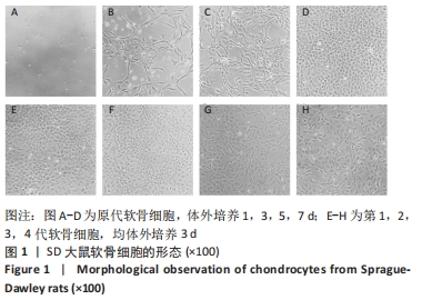
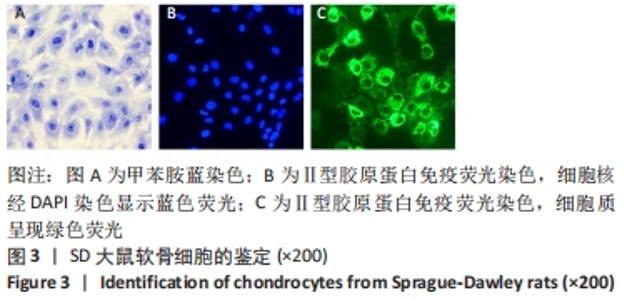
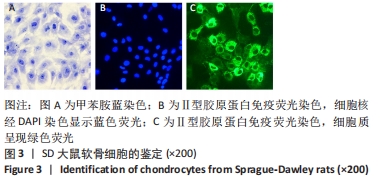
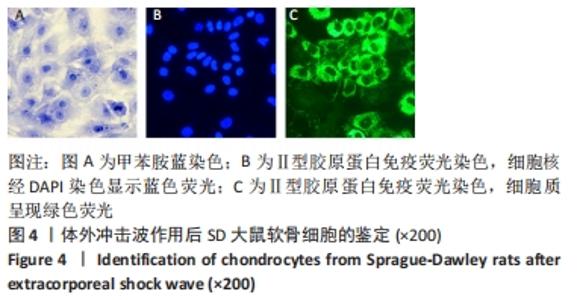
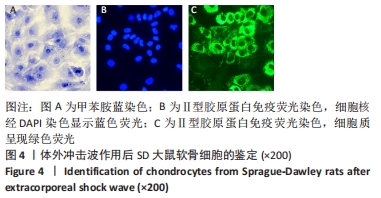
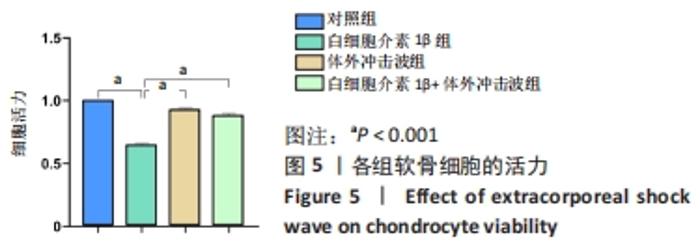
2.1 软骨细胞形态 分离培养的原代软骨细胞呈圆球形,悬浮于培养液中;接种后12 h开始贴壁,24 h后细胞逐渐展开变平,边缘出现突起,可见伪足伸出;培养3 d后大部分细胞贴壁,增殖迅速,胞核清晰,有1个或2个核仁;约7 d单层铺满整个培养皿底面,可进行传代。传代后细胞贴壁较快,约5 d即可传代,细胞呈明显铺路石状外观。 传代细胞在4代以内时,细胞形态均与原代细胞相类似,而第4代后细胞逐渐变为长梭形。传代至第4代,部分细胞变为长梭形,出现不规则形细胞,第5代后梭形细胞开始大量出现,呈纤维细胞样外观,第6代后细胞基本呈不规则形,见图1。白细胞介素1β刺激24 h后,部分软骨细胞由椭圆形或圆形逐渐变为长梭形,部分细胞膜完整性被破坏,见图2。 "
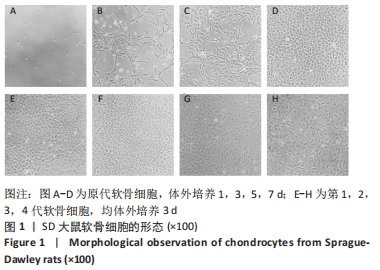
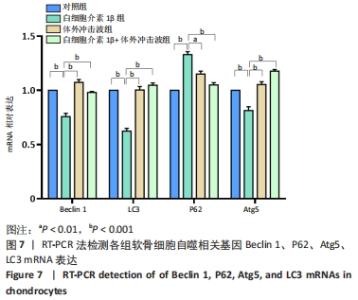
2.5 体外冲击波对软骨细胞自噬相关基因Beclin 1、P62、Atg5、LC3 mRNA表达的影响 与对照组相比,白细胞介素1β组软骨细胞Beclin 1、Atg5、LC3 mRNA表达显著下调(PBeclin 1 < 0.001,PAtg 5 < 0.001,PLC3 < 0.001),P62 mRNA表达上调(P < 0.001)。与白细胞介素1β组相比,白细胞介素1β+体外冲击波组软骨细胞的Beclin 1、Atg5、LC3 mRNA表达显著上调(PBeclin 1 < 0.001,PAtg 5 < 0.001,PLC3 < 0.001),P62 mRNA表达下调(P < 0.001),见图7。"
| [1] SHEN J, ABU-AMER Y, O’KEEFE RJ, et al. Inflammation and epigenetic regulation in osteoarthritis. Connect Tissue Res. 2017;58(1):49-63. [2] MARTEL-PELLETIER J, BARR AJ, CICUTTINI FM, et al. Osteoarthritis. Nat Rev Dis Primers. 2016;2:16072. [3] 陈浩雄,徐启良,黄竞杰,等.牛膝总皂苷体外干预膝关节炎软骨细胞增殖与凋亡的研究[J].现代中西医结合杂志,2021,30(22):2400-2404. [4] ZHOU ZB, HUANG GX, FU Q, et al. circRNA.33186 Contributes to the Pathogenesis of Osteoarthritis by Sponging miR-127-5p. Mol Ther. 2019; 27(3):531-541. [5] MURATA R, NAKAGAWA K, OHTORI S, et al. The effects of radial shock waves on gene transfer in rabbit chondrocytes in vitro. Osteoarthritis Cartilage. 2007;15(11):1275-1282. [6] MA F, LI G, YU Y, et al. MiR-33b-3p promotes chondrocyte proliferation and inhibits chondrocyte apoptosis and cartilage ECM degradation by targeting DNMT3A in osteoarthritis. Biochem Biophys Res Commun. 2019;519(2): 430-437. [7] RACANELLI AC, KIKKERS SA, CHOI AMK, et al. Autophagy and inflammation in chronic respiratory disease. Autophagy. 2018;14(2):221-232. [8] LÓPEZ DE FIGUEROA P, LOTZ MK, BLANCO FJ, et al. Autophagy activation and protection from mitochondrial dysfunction in human chondrocytes. Arthritis Rheumatol. 2015;67(4):966-976. [9] BOUDERLIQUE T, VUPPALAPATI KK, NEWTON PT, et al. Targeted deletion of Atg5 in chondrocytes promotes age-related osteoarthritis. Ann Rheum Dis. 2016;75(3):627-631. [10] LUO P, GAO F, NIU D, et al. The Role of Autophagy in Chondrocyte Metabolism and Osteoarthritis: A Comprehensive Research Review. Biomed Res Int. 2019; 2019:5171602. [11] CARAMÉS B, TANIGUCHI N, OTSUKI S, et al. Autophagy is a protective mechanism in normal cartilage, and its aging-related loss is linked with cell death and osteoarthritis. Arthritis Rheum. 2010;62(3):791-801. [12] JI Q, WANG P, HE C. Extracorporeal shockwave therapy as a novel and potential treatment for degenerative cartilage and bone disease: Osteoarthritis. A qualitative analysis of the literature. Prog Biophys Mol Biol. 2016;121(3):255-265. [13] WANG CJ. Extracorporeal shockwave therapy in musculoskeletal disorders. J Orthop Surg Res. 2012;7:11. [14] CACCHIO A, GIORDANO L, COLAFARINA O, et al. Extracorporeal shock-wave therapy compared with surgery for hypertrophic long-bone nonunions. J Bone Joint Surg Am. 2009;91(11):2589-2597. [15] WANG CJ, SUN YC, WONG T, et al. Extracorporeal shockwave therapy shows time-dependent chondroprotective effects in osteoarthritis of the knee in rats. J Surg Res. 2012;178(1):196-205. [16] WANG CJ, WENG LH, KO JY, et al. Extracorporeal shockwave therapy shows chondroprotective effects in osteoarthritic rat knee. Arch Orthop Trauma Surg. 2011;131(8):1153-1158. [17] ZHAO X, LI Y, LIN X, et al. Ozone induces autophagy in rat chondrocytes stimulated with IL-1β through the AMPK/mTOR signaling pathway. J Pain Res. 2018;11:3003-3017. [18] 孙盼盼,赵旭,林小雯,等.医用臭氧对大鼠骨关节炎软骨细胞中 PPARγ及自噬水平表达的影响[J].山东大学学报(医学版),2020,58(6):14-21. [19] QI H, JIN S, YIN C, et al. Radial extracorporeal shock wave therapy promotes osteochondral regeneration of knee joints in rabbits. Exp Ther Med. 2018; 16(4):3478-3484. [20] 綦惠,杰永生,郑蕊,等.放散式体外冲击波对软骨细胞生物学行为的影响[J].北京生物医学工程,2020,39(3):278-284. [21] LIU Q, WANG S, LIN J, et al. The burden for knee osteoarthritis among Chinese elderly: estimates from a nationally representative study. Osteoarthritis Cartilage. 2018;26(12):1636-1642. [22] NEOGI T. The epidemiology and impact of pain in osteoarthritis. Osteoarthritis Cartilage. 2013;21(9):1145-1153. [23] JOHNSON VL, HUNTER DJ. The epidemiology of osteoarthritis. Best Pract Res Clin Rheumatol. 2014;28(1):5-15. [24] MOBASHERI A, RAYMAN MP, GUALILLO O, et al. The role of metabolism in the pathogenesis of osteoarthritis. Nat Rev Rheumatol. 2017;13(5):302-311. [25] WU CW, TCHETINA EV, MWALE F, et al. Proteolysis involving matrix metalloproteinase 13 (collagenase-3) is required for chondrocyte differentiation that is associated with matrix mineralization. J Bone Miner Res. 2002;17(4):639-651. [26] MA Y, WU Y, CHEN J, et al. miR-10a-5p Promotes Chondrocyte Apoptosis in Osteoarthritis by Targeting HOXA1. Mol Ther Nucleic Acids. 2019;14:398-409. [27] GAO GC, CHENG XG, WEI QQ, et al. Long noncoding RNA MALAT-1 inhibits apoptosis and matrix metabolism disorder in interleukin-1β-induced inflammation in articular chondrocytes via the JNK signaling pathway. J Cell Biochem. 2019;120(10):17167-17179. [28] ROMEO P, LAVANGA V, PAGANI D, et al. Extracorporeal shock wave therapy in musculoskeletal disorders: a review. Med Princ Pract. 2014;23(1):7-13. [29] SCHMITZ C, CSÁSZÁR NB, MILZ S, et al. Efficacy and safety of extracorporeal shock wave therapy for orthopedic conditions: a systematic review on studies listed in the PEDro database. Br Med Bull. 2015;116(1):115-138. [30] 高宏梁,周新华,吴猛,等.低能量体外冲击波对膝骨关节炎大鼠软骨细胞凋亡的影响[J].中国现代医生,2018,56(1):32-35. [31] KIM YH, BANG JI, SON HJ, et al. Protective effects of extracorporeal shockwave on rat chondrocytes and temporomandibular joint osteoarthritis; preclinical evaluation with in vivo99mTc-HDP SPECT and ex vivo micro-CT. Osteoarthritis Cartilage. 2019;27(11):1692-1701. [32] NOTARNICOLA A, IANNONE F, MACCAGNANO G, et al. Chondrocytes treated with different shock wave devices. Muscles Ligaments Tendons J. 2017;7(1):152-156. [33] VETRANO M, RANIERI D, NANNI M, et al. Hyaluronic Acid (HA), Platelet-Rich Plasm and Extracorporeal Shock Wave Therapy (ESWT) promote human chondrocyte regeneration in vitro and ESWT-mediated increase of CD44 expression enhances their susceptibility to HA treatment. PLoS One. 2019;14(6):e0218740. [34] CHENG NT, MENG H, MA LF, et al. Role of autophagy in the progression of osteoarthritis: The autophagy inhibitor, 3-methyladenine, aggravates the severity of experimental osteoarthritis. Int J Mol Med. 2017;39(5):1224-1232. [35] CARAMÉS B, HASEGAWA A, TANIGUCHI N, et al. Autophagy activation by rapamycin reduces severity of experimental osteoarthritis. Ann Rheum Dis. 2012;71(4):575-581. [36] SALMINEN A, KAARNIRANTA K, KAUPPINEN A. Beclin 1 interactome controls the crosstalk between apoptosis, autophagy and inflammasome activation: impact on the aging process. Ageing Res Rev. 2013;12(2):520-534. [37] LONG M, LI X, LI L, et al. Multifunctional p62 Effects Underlie Diverse Metabolic Diseases. Trends Endocrinol Metab. 2017;28(11):818-830. [38] LAHUERTA M, AGUADO C, SÁNCHEZ-MARTÍN P, et al. Degradation of altered mitochondria by autophagy is impaired in Lafora disease. FEBS J. 2018;285(11):2071-2090. [39] SCHAAF MB, KEULERS TG, VOOIJS MA, et al. LC3/GABARAP family proteins: autophagy-(un)related functions. FASEB J. 2016;30(12):3961-3978. [40] 孙明帅,范重山,李凯杰,等.骨关节炎中软骨细胞自噬的作用及其靶向治疗[J].中国组织工程研究,2021,25(35):5688-5693. [41] 杜汉承.雷诺嗪联合血栓通胶囊对糖尿病大鼠心肌缺血再灌注损伤过程中细胞自噬及心肌核因子-κB、人磷酸化Akt蛋白、IP7水平的影响[J].中国药物经济学,2020,15(9):39-43. [42] 唐琴,朱海鹏,郭卫中,等.锌对THP-1细胞自噬、NF-κB通路活化及产生白细胞介素23的影响[J].免疫学杂志,2018,34(4):319-325. [43] DU L, SHEN T, LIU B, et al. Shock Wave Therapy Promotes Cardiomyocyte Autophagy and Survival during Hypoxia. Cell Physiol Biochem. 2017;42(2):673-684. [44] QIU Q, SHEN T, YU X, et al. Cardiac Shock Wave Therapy Alleviates Hypoxia/Reoxygenation-Induced Myocardial Necroptosis by Modulating Autophagy. Biomed Res Int. 2021;2021:8880179. [45] LONG Q, LI X, HE H, et al. Autophagy activation protects shock wave induced renal tubular epithelial cell apoptosis may through modulation of Akt/ GSK-3β pathway. Int J Biol Sci. 2016;12(12):1461-1471. [46] ZHU GQ, JEON SH, BAE WJ, et al. Efficient Promotion of Autophagy and Angiogenesis Using Mesenchymal Stem Cell Therapy Enhanced by the Low-Energy Shock Waves in the Treatment of Erectile Dysfunction. Stem Cells Int. 2018;2018:1302672. |
| [1] | Sun Kexin, Zeng Jinshi, Li Jia, Jiang Haiyue, Liu Xia. Mechanical stimulation enhances matrix formation of three-dimensional bioprinted cartilage constructs [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(在线): 1-7. |
| [2] | Chen Jingqiao, Li Ying, Meng Maohua, Xu Xingxing, Wang Qinying, Wang Huan, Lu Jing, Shu Jiayu, Dong Qiang. Research progress in platelet-rich fibrin in stomatology [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 441-446. |
| [3] | Zong Mingrui, Liu Haiyan, Li Bing, Wu Xiuping. Application of carboxymethyl chitosan in tissue engineering of stomatology [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 447-452. |
| [4] | Zhang Hui, Wang Jiayang, Wang Qian, Gan Hongquan, Wang Zhiqiang. Effects of hyaluronic acid combined with domestic porous tantalum on chondrocyte function under the dynamic environment [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 339-345. |
| [5] | Liu Huan, Li Han, Ma Yunhao, Zhong Weijian, Ma Guowu. Osteogenic capacity of partially demineralized dentin particles in the maxillary sinus lift [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 354-359. |
| [6] | Wang Junxiang, Sun Jiangwei, Bai Bujiafu·Yellisi, Wang Zhaoxin, Nijati·Turson. Effect of three abutment materials on bone stress around maxillary angle implant under dynamic loading [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 398-405. |
| [7] | Ning Ziwen, Wang Xu, Shi Zhengliang, Qin Yihua, Wang Guoliang, Jia Di, Wang Yang, Li Yanlin. Meniscal injury repair methods for non-blood supply area [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 420-426. |
| [8] | Dai Xianglin, Zhang Wenfeng, Yao Xijun, Shang Jiaqi, Huang Qiujin, Ren Yifan, Deng Jiupeng. Barium titanate/polylactic acid piezoelectric composite film affects adhesion, proliferation, and osteogenic differentiation of MC3T3-E1 cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 367-373. |
| [9] | Shui Xiaoping, Li Chunying, Li Mingjuan, Li Shunchang, Sun Junzhi, Su Quansheng. Effects of aerobic and resistance exercise on antioxidant stress index and brain-derived neurotrophic factor expression in the hippocampus of type 2 diabetic rats [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 264-269. |
| [10] | Li Mingxiu, Wang Xuan, Yang Jie, Li Yi. An osteoarthritis model in vitro: characteristics and new design idea [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 300-306. |
| [11] | Liu Yinghong, Yi Yating. Mechanism and implication of angiogenesis in osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 307-313. |
| [12] | Zhang Jie, Tian Ai. Advances in the signaling pathway of M2 macrophages involved in bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 314-321. |
| [13] | Lin Shi, Yuan Jiayao, Lin Xiancan, Yang Binbin, Wu Jianjun, Dongzhi Zhuoma, Tang Zijia, Yang Zhijie, Wan Lei, Huang Hongxing. Diagnostic value of peripheral blood interferon-gamma and monocyte chemoattractant protein-1 in postmenopausal osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 165-170. |
| [14] | Chen Xiaosi, Tan Xiaoyan, Liu Tianfeng, Han Dengpeng, Wei Bo, Hu Zibing, Wu Shaoke. Effects of asiatic acid on biomechanical properties, trabecular area and Runx2 protein in osteoporotic rats [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 246-251. |
| [15] | Zhang Weiye, Zhan Jiawen, Zhu Liguo, Wang Shangquan, Chen Ming, Wei Xu, Feng Minshan, Yu Jie, Han Tao, Cai Chuhao, Zhou Shuaiqi, Shao Chenchen. Effect of nucleus pulposus cells-derived exosomes under cyclic mechanical tension on endplate chondrocytes [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 223-229. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||