Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (27): 4283-4288.doi: 10.12307/2021.183
Previous Articles Next Articles
Establishment and validation of a finite element model of sacral lumbarization in adolescents
Wu Xuehai, Wang Xing, Zhang Shaojie, Xu Xuebin, Shi Jun, Wang Tieying, Li Zhijun
- 1Department of Orthopedics, Chifeng City Second Hospital, Chifeng 024000, Inner Mongolia Autonomous Region, China; 2Human Anatomy Teaching and Research,
3Physiology Teaching Laboratory, Basic Medical College of Inner Mongolia Medical University, Hohhot 010110, Inner Mongolia Autonomous Region, China
-
Received:2020-05-19Revised:2020-05-20Accepted:2020-10-16Online:2021-09-28Published:2021-04-10 -
Contact:Li Zhijun, Master, Professor, Doctoral supervisor, Human Anatomy Teaching and Research, Basic Medical College of Inner Mongolia Medical University, Hohhot 010110, Inner Mongolia Autonomous Region, China Wang Tieying, Chief physician, Department of Orthopedics, Chifeng City Second Hospital, Chifeng 024000, Inner Mongolia Autonomous Region, China -
About author:Wu Xuehai, Master, Attending physician, Department of Orthopedics, Chifeng City Second Hospital, Chifeng 024000, Inner Mongolia Autonomous Region, China Wang Xing, Doctoral candidate, Lecturer, Human Anatomy Teaching and Research, Basic Medical College of Inner Mongolia Medical University, Hohhot 010110, Inner Mongolia Autonomous Region, China -
Supported by:the National Natural Science Foundation of China, No. 81860382 (to WX), No. 81860383, 81560348 (to LZJ), No. 81660358 (to ZSJ); the Natural Science Foundation of Inner Mongolia Autonomous Region, No. 2020MS03061 (to WX), No. 2019MS08017 (to ZSJ); the Science and Technology Development Program of Inner Mongolia Autonomous Region, No. 2019GG158 (to WX); the Science and Technology Project of Inner Mongolia Medical University, No. YKD2017KJBW009 (to WX), No. 2015YKDKJBW03 (to ZSJ)
CLC Number:
Cite this article
Wu Xuehai, Wang Xing, Zhang Shaojie, Xu Xuebin, Shi Jun, Wang Tieying, Li Zhijun. Establishment and validation of a finite element model of sacral lumbarization in adolescents[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(27): 4283-4288.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
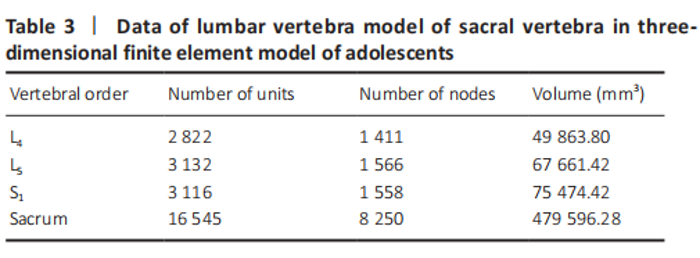

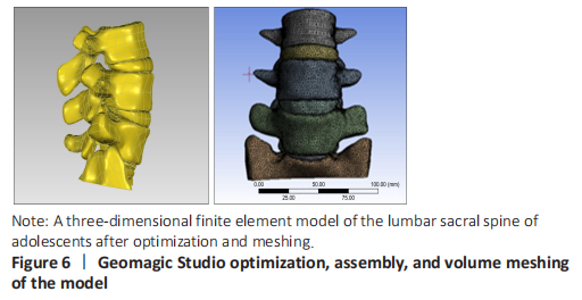
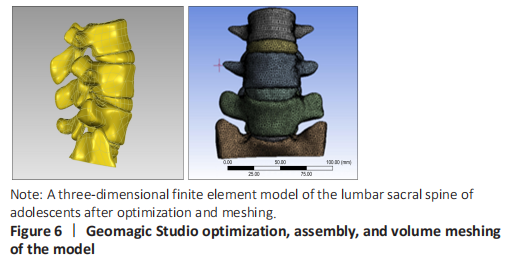
A three-dimensional finite element model of lumbar sacral vertebrae was established In this study, a three-dimensional finite element model of lumbar sacral vertebrae in adolescents was established based on the data of patients with lumbar sacral vertebrae, including 22 815 elements and 12 785 nodes (Table 3). The model is highly simulated, the geometric structure is good, the appearance of the model is close to the structure of sacral lumbar data, and has a high degree of reduction (Table 3 and Figure 6)."

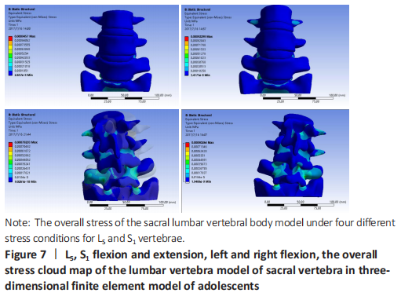
Stress analysis of lumbar vertebrae of sacral vertebrae under different working conditions in three-dimensional finite element model of adolescents When the torque of 2 N·mm was applied to the lumbar vertebra finite element model of sacral vertebrae, the stresses of L5 and S1 under lumbar vertebrae of sacral vertebrae were as follows: during flexion, the stress was mainly concentrated in the facet joint of S1Unix 2, followed by the posterior structure of each vertebra. During the extension, the stress was mainly concentrated in the S1ax 2 facet joint, and decreased in turn from S1 to upward, which was basically consistent with the flexion movement. In the left and right side flexion, the stress is mainly concentrated in the S1hip 2 facet joint, followed by the superior articular process of S1, and decreases upward from S1. For the symmetry of human body development, the stress and strain of the model under the right bending condition is the same as that of the left bending. In the axial torsion of the left and right sides, the stress is greater in the anterior part of the C2-3 vertebral body, and the stress is also obvious in the facet joint and pedicle of the opposite side of the vertebral body. For L5 and S1 vertebrae, the maximum stress appeared in the inferior articular process of the vertebrae under flexion and extension, followed by the isthmus of the pedicle of the vertebrae, and in the condition of left and right lateral bending, the maximum stress appeared in the inferior articular process of the vertebrae, followed by the superior articular process of the vertebrae, and then in the isthmus of the pedicle of the vertebrae (Figure 7)."
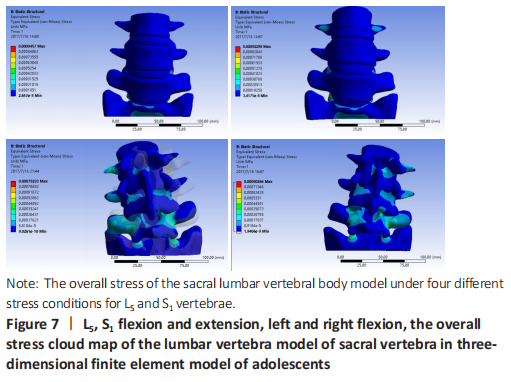
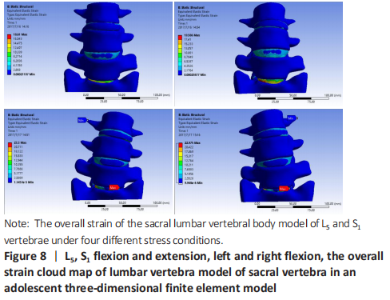
Strain and displacement analysis of lumbar vertebrae of sacral vertebrae under different working conditions in adolescents three-dimensional finite element model In the stress analysis of the model, the maximum strain was located in the intervertebral disc tissue under different working conditions, and the strain law was that S1 decreased upward, and the maximum displacement was located at the anterior upper edge of L4 during flexion. Under the left bending condition, the maximum strain of the model was S1Scan2, and there was little difference in stress between L4-5 and L5/S1 (Figure 7). To analyze the displacement changes of the model under different working conditions, during flexion and extension, the maximum displacement is located at the upper edge of L4, and the displacement decreases successively from L4 to the sacrum. Under the condition of left and right side bending, the maximum displacement is located at the front and upper edge of L4, and the displacement decreases successively from L4 to downward (Figure 8)."
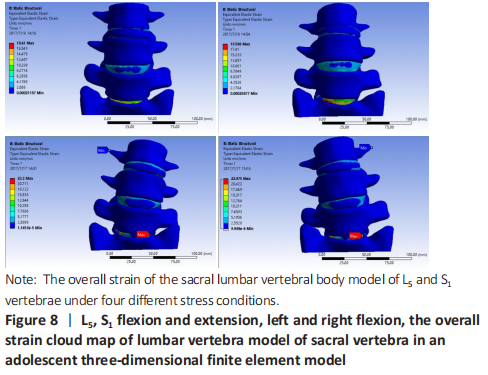
| [1] MITRA R, CARLISLE M. Bertolotti’s syndrome: a case report. Pain Pract. 2009;9(2): 152-154. [2] LV YP, Lin W, Ma XM. The localization of iliolumbar ligaments in lumbar column segmentation. Fangshe Xue Shijian. 2016;31(11):1080-1083. [3] JANCUSKA JM, SPIVAK JM, BENDO JA. A Review of Symptomatic Lumbosacral Transitional Vertebrae: Bertolotti’s Syndrome. Int J Spine Surg. 2015;9:42. [4] ZHAO S. Imaging study of percutaneous intervertebral foramen approach in lumbosacral 1. Suzhou: Suzhou University. 2015. [5] GONG H, SLUNSKY P, KLASS LG, et al. Brunnberg L. Prevalence of lumbosacral transitional vertebrae in dogs in Berlin. Pol J Vet Sci. 2020;23(2):261-265. [6] SEKHARAPPA V, AMRITANAND R, KRISHNAN V, et al. Lumbosacral transition vertebra: prevalence and its significance. Asian Spine J. 2014;8(1):51-58. [7] TANG M, YANG XF, YANG SW, et al. Lumbosacral transitional vertebra in a population-based study of 5860 individuals: prevalence and relationship to low back pain. Eur J Radiol. 2014;83(9):1679-1682. [8] MAHATO NK, DHASON R, RAM DR. Quantifying Range of Motion and Stress Patterns at the Transitional Lumbosacral Junction: Pilot Study Using a Computational Model for Load-Bearing at Accessory L5-S1 Articulation. Int J Spine Surg. 2019;13(1):17-23. [9] MAHATO NK. Trabecular bone structure in lumbosacral transitional vertebrae: distribution and densities across sagittal vertebral body segments. Spine J. 2013 Aug;13(8):932-937. [10] JARAMILLO HE, GÓMEZ L, GARCÍA JJ. A finite element model of the L4-L5-S1 human spine segment including the heterogeneity and anisotropy of the discs. Acta Bioeng Biomech. 2015;17(2):15-24. [11] LIN ZY, XIE YS, XIE PS, et al. Construction and accuracy test of lumbar intelligent medical image modeling system. Zhongguo Linchuang Jiepou Xue Zazhi. 2020; 38(4):444-449. [12] SHIRAZI-ADL A, AHMED AM, SHRIVASTAVA SC. Mechanical response of a lumbar motion segment in axial torque alone and combined with compression. Spine (Phila Pa 1976). 1986;11(9):914-927. [13] SCHMIDT H, HEUER F, DRUMM J, et al. Application of a calibration method provides more realistic results for a finite element model of a lumbar spinal segment. Clin Biomech (Bristol, Avon). 2007;22(4):377-384. [14] LIU YK, RAY G, HIRSCH C. The resistance of the lumbar spine to direct shear. Orthop Clin North Am. 1975;6(1):33-49. [15] HU Y, XIE H, YANG SH. Utilization of three- dimensional finite element method in spinal biomechanics. Yiyong Shengwu Lixue. 2006;21(3):246-250. [16] TOKGOZ N, UCAR M, ERDOGAN AB, et al. Are spinal or paraspinal anatomic markers helpful for vertebral numbering and diagnosing lumbosacral transitional vertebrae?. Korean J Radiol. 2014;15(2):258-266. [17] GIRDLER S, CHO B, MIKHAIL CM, et al. Emerging Techniques in Diagnostic Imaging for Idiopathic Scoliosis in Children and Adolescents: A Review of the Literature. World Neurosurg. 2020;136:128-135. [18] JANCUSKA JM, SPIVAK JM, BENDO JA. A Review of Symptomatic Lumbosacral Transitional Vertebrae: Bertolotti’s Syndrome. Int J Spine Surg. 2015;9:42. [19] MAHATO NK. Implications of structural variations in the human sacrum: why is an anatomical classification crucial?. Surg Radiol Anat. 2016;38(8):947-954. [20] LUOMA K, VEHMAS T, KERTTULA L, et al. Chronic low back pain in relation to Modic changes, bony endplate lesions, and disc degeneration in a prospective MRI study. Eur Spine J. 2016;25(9):2873-2881. [21] HOU LS, BAI XD, GE F, et al. Castellvi’s classification type-Ⅱa lumbarization combined with L5-S2 disc herniation: a case report. Dier Junyi Daxue Xuebao. 2018;39(10):1177-1179. [22] HANHIVAARA J, MÄÄTTÄ JH, NIINIMÄKI J, et al. Lumbosacral transitional vertebrae are associated with lumbar degeneration: retrospective evaluation of 3855 consecutive abdominal CT scans. Eur Radiol. 2020;30(6):3409-3416. [23] DANG L, CHEN ZQ LIU XG, et al. Etiology of lumbar disc herniation in adolescents: excessive load on the lumbar spine and aberrant configurations of the lumbosacral region. Zhongguo Jizhu Jisui Zazhi. 2015;25(11):991-996. [24] FUJIWARA A, TAMAI K, KURIHASHI A, et al. Relationship between morphology of iliolumbar ligament and lower lumbar disc degeneration. J Spinal Disord. 1999; 12(4):348-352. [25] AHN SS, CHIN DK, KIM SH, et al. The Clinical Significance of Lumbosacral Transitional Vertebrae on the Surgical Outcomes of Lumbar Discectomy: A Retrospective Cohort Study of Young Adults. World Neurosurg. 2017;99:745-750. [26] BERLEMANN U, JESZENSZKY DJ, BÜHLER DW, et al. Facet joint remodeling in degenerative spondylolisthesis: an investigation of joint orientation and tropism. Eur Spine J. 1998;7(5):376-380. [27] HAMMERBERG KW. New concepts on the pathogenesis and classification of spondylolisthesis. Spine (Phila Pa 1976). 2005;30(6 Suppl):S4-S11. [28] JIANG HC, WANG JX, YANG XD, et al. Analysis of the related factors of lumbar spondylolysis. Zhongguo Linchuang Jiepou Xue Zazhi. 2019;37(5):583-585,589. [29] KANEMATSU R, HANAKITA J, TAKAHASHI T, et al. Extraforaminal entrapment of the fifth lumbar spinal nerve by nearthrosis in patients with lumbosacral transitional vertebrae. Eur Spine J. 2020;29(9):2215-2221. [30] ALBANO D, MESSINA C, GAMBINO A, et al. Segmented lordotic angles to assess lumbosacral transitional vertebra on EOS. Eur Spine J. 2020;29(10):2470-2476. |
| [1] | Wang Jianping, Zhang Xiaohui, Yu Jinwei, Wei Shaoliang, Zhang Xinmin, Xu Xingxin, Qu Haijun. Application of knee joint motion analysis in machanism based on three-dimensional image registration and coordinate transformation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(在线): 1-5. |
| [2] | Xu Xinzhong, Wu Zhonghan, Yu Shuisheng, Zhao Yao, Xu Chungui, Zhang Xin, Zheng Meige, Jing Juehua. Biomechanical analysis of different ways of inserting Steinmann Pins into the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1313-1317. |
| [3] | Wei Guoqiang, Li Yunfeng, Wang Yi, Niu Xiaofen, Che Lifang, Wang Haiyan, Li Zhijun, Shi Guopeng, Bai Ling, Mo Kai, Zhang Chenchen, Xu Yangyang, Li Xiaohe. Biomechanical analysis of non-uniform material femur under different loads [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1318-1322. |
| [4] | Zhang Yufang, Lü Meng, Mei Zhao. Construction and verification of a full spine biomechanical model of adolescent scoliosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1351-1356. |
| [5] | Zhang Jichao, Dong Yuefu, Mou Zhifang, Zhang Zhen, Li Bingyan, Xu Xiangjun, Li Jiayi, Ren Meng, Dong Wanpeng. Finite element analysis of biomechanical changes in the osteoarthritis knee joint in different gait flexion angles [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1357-1361. |
| [6] | Bai Zixing, Cao Xuhan, Sun Chengyi, Yang Yanjun, Chen Si, Wen Jianmin, Lin Xinxiao, Sun Weidong. Construction and biomechanical analysis of ankle joint finite element model in gait cycle [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1362-1366. |
| [7] | Liu Feng, Feng Yi. Finite element analysis of different Kirschner wire tension bands on transverse patella fractures during gait cycle [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1367-1371. |
| [8] | Song Yuxin, Zhang Tongtong, Niu Jianxiong, Wang Zengping, Wen Jie, Zhang Qunli, Xue Wen, Liu Lin. Precise screw placement of 3D printing model and orthopedic robot in spinal deformity [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 904-907. |
| [9] | Duan Chao, Shang Xiaoqiang, Duan Xianglin, Yang Ping, Tao Shengxiang. Stability of patellar claw versus loop plate combined with patellar claw for the treatment of comminuted fractures of the lower pole of the patella [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 934-937. |
| [10] | Li Guijun, Fang Xiaohui, Kong Weifeng, Yuan Xiaoqing, Jin Rongzhong, Yang Jun. Finite element analysis of the treatment of hallux valgus deformity by microplate combined with super strong suture elastic fixation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 938-942. |
| [11] | Liu Dongcheng, Zhao Jijun, Zhou Zihong, Wu Zhaofeng, Yu Yinghao, Chen Yuhao, Feng Dehong. Comparison of different reference methods for force line correction in open wedge high tibial osteotomy [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 827-831. |
| [12] | Wen Mingtao, Liang Xuezhen, Li Jiacheng, Xu Bo, Li Gang. Mechanical stability of Sanders II type calcaneal fractures fixed by two internal fixation methods [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 838-842. |
| [13] | Wang Hailong, Li Long, Maihemuti·Yakufu, Chen Hongtao, Liu Xu, Yilihamu·Tuoheti. Finite element analysis of stress distribution of acetabular prosthesis in the Lewinnek safety zone [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 843-847. |
| [14] | Huang Hao, Hong Song, Wa Qingde. Finite element analysis of the effect of femoral component rotation on patellofemoral joint contact pressure in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 848-852. |
| [15] | Zheng Yongze, Zheng Liqin, He Xingpeng, Chen Xinmin, Li Musheng, Li Pengfei, Lin Ziling. Extended finite element modeling analysis of femoral neck fracture based on ABAQUS software [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 853-857. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||